Abstract
BACKGROUND:
Ovarian cancer (OC) is one of the most malignant gynecological cancers. Platelets play a profound role in cancer growth and metastasis. Platelet distribution width (PDW) is an indicator of platelet activation and is altered in malignancies. However, the prognostic value of PDW in OC remains unclear. This present study aimed to investigate the predictive significance of PDW in OC.
METHODS:
221 OC patients, between January 2013 and December 2013, were included in this study. The correlations between PDW and clinicopathological features were analyzed. Kaplan-Meier method and Cox regression were used to evaluate the prognostic impact of PDW.
RESULTS:
Of the 221 patients, increased PDW levels were observed in 163 (73.6%) patients. Kaplan-Meier analysis revealed that higher PDW levels were associated with poor progression-free survival and overall survival (both
CONCLUSION:
Higher PDW levels predict poor prognosis in patients with OC. Elevated PDW may be a novel target for therapy.
Introduction
Ovarian cancer (OC), one of the most malignant gynecological cancers, is more diagnosed at an advanced stage and has poor prognosis [1, 2]. Despite the development of therapeutic strategies and surgical techniques, the long-term survival of OC patients remains poor. Therefore, the identification of new biomarkers is urgently needed in patients with OC.
Platelets play a recognized role in various stages of cancer growth and metastasis [3]. Thrombocytosis typically suggests a poorer prognosis in various types of cancer, such as pancreatic, gastric, colorectal, endometrial, and ovarian cancer [4, 5, 6, 7, 8]. Tumor cells in the circulatory system tend to attract new platelets, thus facilitating tumor cell adhesion, arrest, and metastasis [9]. Tumor cell adhesion of platelets and their activation is a crucial step for tumor cell survival within the blood circulatory system [10].
A platelet index known as platelet distribution width (PDW) indicates variation in platelet size and can aid in diagnosing thrombocytopenia [11]. Increased PDW levels have been linked to a poor prognosis in a variety of tumors, such as gastric cancer, non-small cell lung cancer, breast cancer, laryngeal cancer, hepatocellular carcinoma, and melanoma [12, 13, 14, 15, 16]. However, the relationship between preoperative PDW levels and survival in OC has not been investigated.
The aim of this study was to evaluate the potential prognostic role of PDW in OC patients.
Materials and methods
Patient characteristics
This retrospective review was drawn from a database of OC patients managed through Harbin Medical University Cancer Hospital between January 2013 and December 2013. Two hundred and eighty patients meeting all of the following requirements were eligible for enrollment: (1) diagnosis of OC was confirmed by histology; (2) untreated before diagnosis. Patients were excluded if they had hematological disorders (
Standard demographic and clinicopathological data were collected from the patients’ records in hospital. For all participants in the study, venous peripheral blood samples were collected at admission. All patients were clinically staged according to the International Federation of Gynecology and Obstetrics (FIGO) system. Platelet indices were determined with an automated hematological analyzer (Sysmex XE-2100, Kobe, Japan). The normal range for PDW in our hospital was 11–17%. Survival data were obtained through follow-up. Progression-free survival (PFS) was defined as the time from the day of surgery to the first event (relapse, metastasis or death from any cause) or last follow-up. Overall survival (OS) was defined as the interval from the date of diagnosis to death or last follow-up.
Optimized cut-off was determined for PDW using standard ROC curve analysis.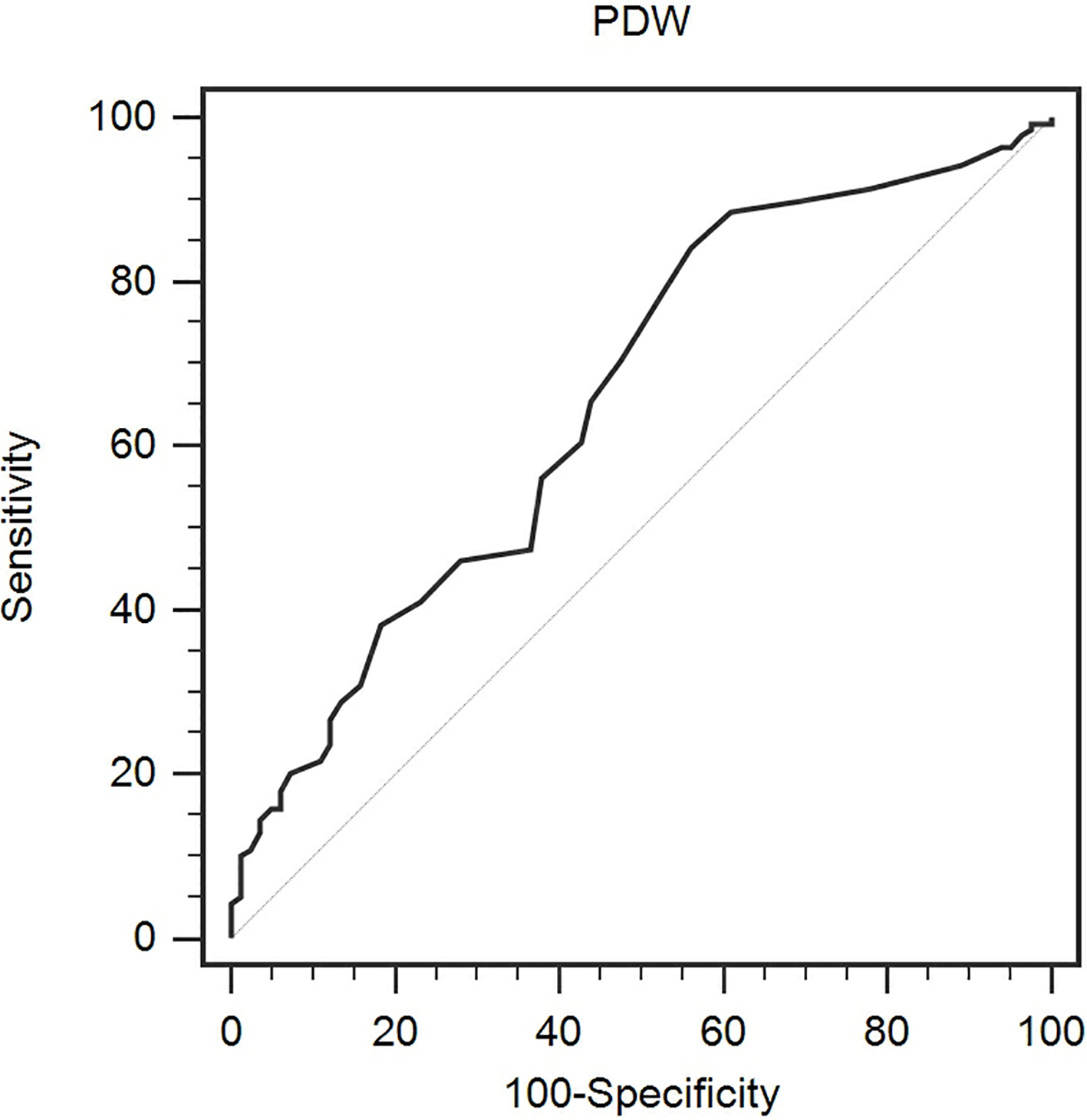
Informed consent was obtained from all participants, and this study was approved by the Ethics Committee of Harbin Medical University Cancer Hospital.
All statistical tests were performed in the software of SPSS (version 25.0, SPSS Inc., Chicago, IL, USA). Data are presented as percentages or mean
Results
Among the 221 patients, the mean age was 53.7
According to the ROC curve analysis, we identified that the optimal cut-off value of 16.5 for PDW had a 84.2% sensitivity and 51.7% specificity for survival rate (AUC
The associations between PDW levels and baseline clinicopathological characteristics were presented in Tables 1 and 2. There was no significant association between PDW levels and age, tumor size, ascites, CA125, histological grade, histological type, lymph node metastasis, and FIGO stage.
The correlations between PDW levels and clinical parameters in OC patients
The correlations between PDW levels and clinical parameters in OC patients
The correlations between PDW levels and clinical parameters in OC patients
Data are expressed as means (SD). WBC, white blood cell; BMI, body mass index.
After a follow-up of 60 months, 117 (71.8%) patients had died, and 22 (37.9%) patients remained alive at the end of study. Patients with high PDW levels exhibited significantly shorter OS and PFS compared to those with low PDW levels (for OS, 28.2% vs. 62.1%,
Kaplan-Meier analysis of progression-free survival in OC patients.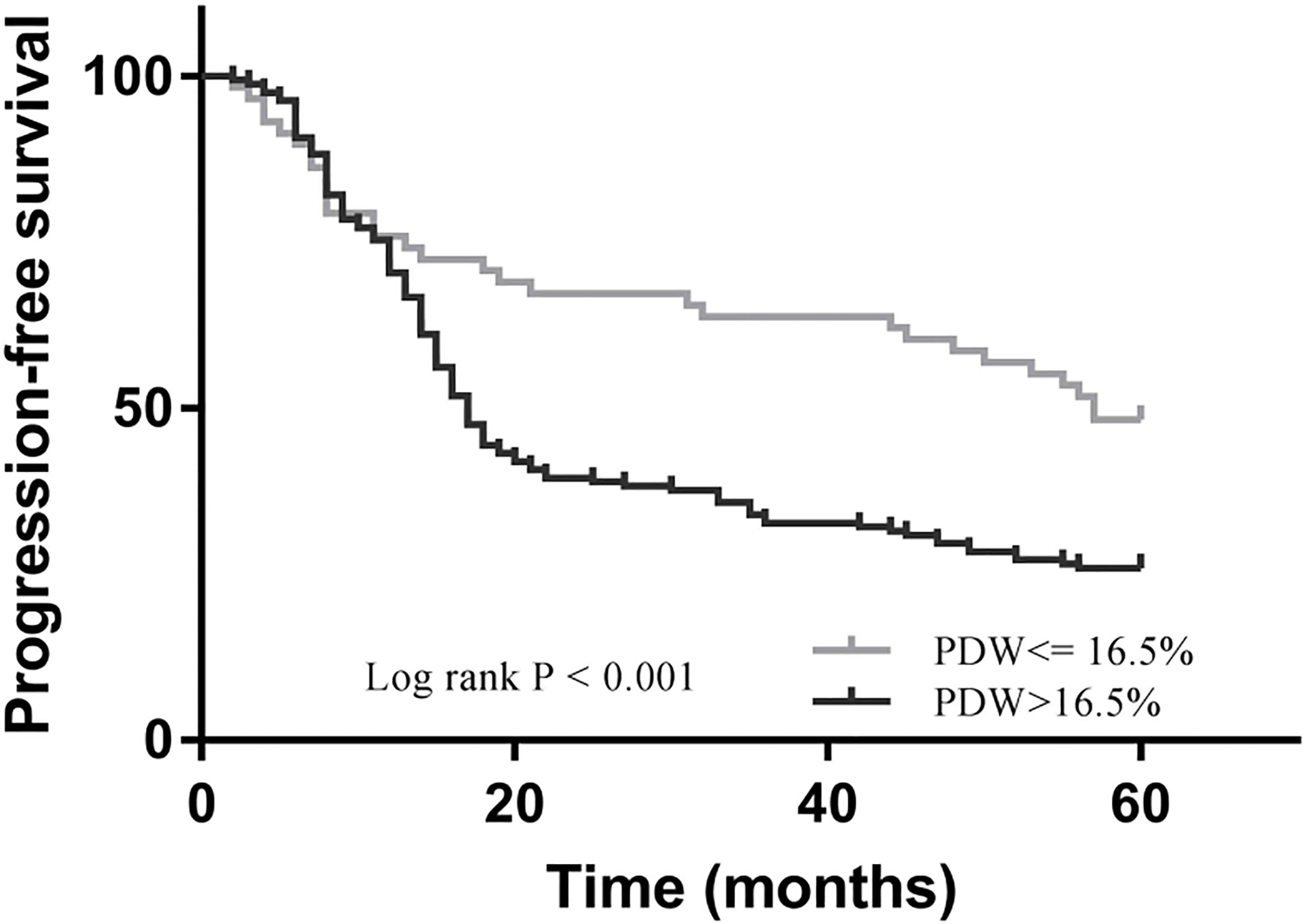
Cox univariate and multivariate proportional regression analyses were performed for the potential risk factors for OS. In univariate analyses, ascites, lymph node metastasis, higher FIGO stage, and high PDW levels were significantly associated with a shorter OS (Table 3). In multivariate analysis, lymph node metastasis, higher FIGO stage, and high PDW levels were independent predictive factors of a shorter OS (Table 4). Patients with high PDW levels had a hazard ratio (HR) of 2.820, [95% confidence interval (CI): 1.776–4.476,
Univariate analyses of factors associated with overall survival in OC patients
Multivariate analyses of factors associated with overall survival in OC patients
The present study revealed that OC patients with high PDW levels exhibited lower OS and PFS rate. It is the first time that high PDW levels were reported to contribute to worse OC prognosis.
Thrombocytosis is associated with poor prognosis in several cancers, such as lung, ovarian, endometrial, rectal, kidney, gastric, pancreatic, and breast cancer. Moreover, increased platelet count was observed in OC and was associated with shorter survival time. A meta-analysis revealed that thrombocytosis before treatment predicts poor prognosis in OC patients [17]. Moreover, elevated platelets were correlated with positive second-look laparotomy results and disease progression in OC [18]. Aspirin and P2Y12 inhibition abrogate platelet-induced OC cell invasion [19]. Platelets facilitate cancer progression and metastasis by promoting angiogenesis and tumor cell proliferation at distant sites [20]. Since platelets have critical physiological roles, it is suggested to target cancer-specific platelet-activating factors, rather than targeting platelets [21]. Recent studies revealed that platelet-derived endothelial cell growth factors and activated receptors might be useful biomarkers in terms of progression, chemotherapy resistance, and recurrence of OC [22, 23, 24, 25, 26]. Further research confirmed that platelet transforming growth factor
Kaplan-Meier analysis of overall survival in OC patients.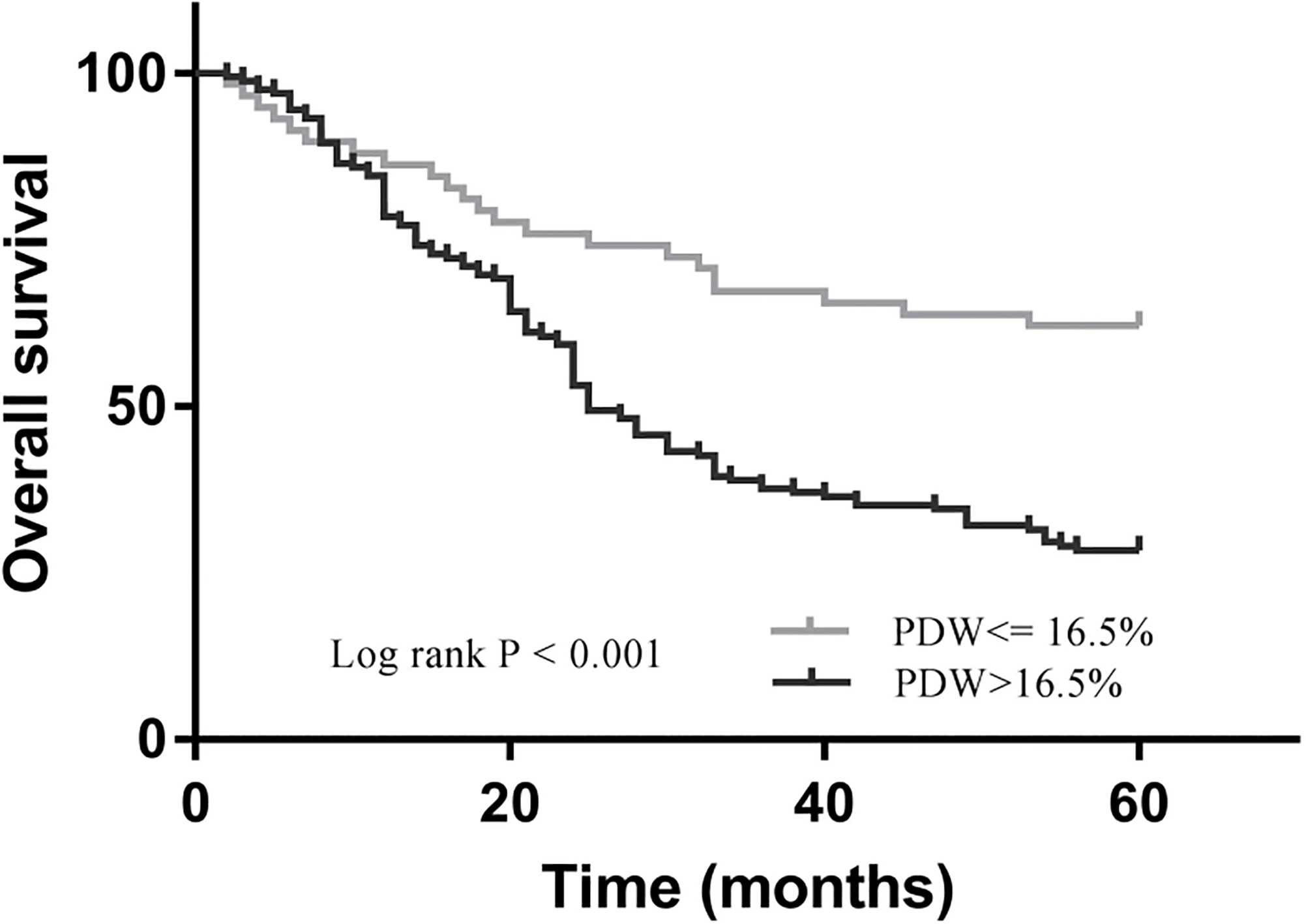
The mechanisms affecting the association between PDW and survival are unclear. Dysfunction of bone marrow cells (including megakaryocytes) may contribute to elevated PDW levels. PDW is a quantification of platelet heterogeneity resulting from heterogeneous demarcation of megakaryocytes [28]. Some studies showed that several cytokines, such as interleukin-6 (IL-6), granulocytes colony stimulating factor (G-CSF) and macrophage colony stimulating factor (M-CSF), could regulate megakaryocytic maturation, platelet production and platelet size [29]. IL-6 promotes tumor angiogenesis, and G-CSF and M-CSF stimulate megakaryopoiesis and subsequent thrombopoiesis in cancer [30, 31]. These data are also consistent with the current knowledge that antiplatelet therapy is considered to be a part of cancer adjuvant therapy [32].
PDW is an early indicator of activated platelets and tests for PDW are available in any clinical practice. The present study revealed the prognostic role of PDW in OC patients. PDW could be assessed in routine clinical practice with minimal extra cost, and may help clinicians to quickly identify patients at high risk.
Some limitations should be considered when interpreting the results. Firstly, there is no evidence for mechanistic explanation in our study. Thus, further investigations are needed to explore the exact mechanism of PDW in OC. Secondly, this was a single-center retrospective study, so multicentric prospective studies are needed to reduce selection bias. Finally, because our study only includes Chinese participants, our findings may not extend to different ethnic groups.
In conclusion, higher PDW levels predict poor prognosis in patients with ovarian cancer. Elevated PDW may be a novel target for therapy.
Footnotes
Acknowledgments
This work was supported by grants from the Harbin Medical University Cancer Hospital (JJZD2017-05) and from Nn10 program of Harbin Medical University Cancer Hospital.
Conflict of interest
The authors declare that they have no conflict of interests.
