Abstract
BACKGROUND:
Previous studies have demonstrated that platelets play an important role in growth, invasion, and angiogenesis of a variety of tumors. Nevertheless, the prognostic role of platelet indices in hepatocellular carcinoma (HCC) has not been explored. The aim of this study was to explore the association between platelet indices and prognosis in HCC.
METHOD:
A total of 260 patients with HCC between January 2009 and December 2015 were retrospectively analyzed. The optimal platelet distribution width (PDW) cutoff value is identified by the receiver operating characteristic curve (ROC) curve. The relationship between PDW and clinicopathological features was assessed. The prognostic effects of PDW were assessed by using the Kaplan-Meier method and Cox regression model.
RESULT:
Elevated PDW level was significantly associated with portal hypertension, vascular invasion, and Child-Pugh grade. In addition, survival curve indicates that patients with high PDW levels have a worse prognosis than patients with low PDW levels (
CONCLUSION:
Elevated PDW may be a novel marker for predicting the prognosis of HCC, but further research is needed to validate our conclusions.
Introduction
Hepatocellular carcinoma (HCC) is one of the common malignant diseases worldwide, and the incidence rate is increasing year by year [1]. Surgical resection and liver transplantation (LT) are currently effective ways to treat HCC [2]. Despite the improvement of diagnosis and treatment of HCC, its five-year overall survival rate is still very poor. Therefore, identifying a novel and valuable tumor markers is critical for improving cancer management.
Recently, researchers have discovered the important role of platelets in tumor progression and metastasis [3]. Activation of platelets can facilitate cancer cell proliferation, invasion, and angiogenesis. High platelet counts are associated with poor prognosis in numerous cancers, including renal cell carcinoma [4], lung cancer [5], colorectal cancer [6], pancreatic cancer [7], renal cortical malignancy [8], breast cancer [9], ovarian cancer [10], bladder cancer [11], and endometrial cancer [12]. Nevertheless, total platelet count is depended on the consumption and production of platelets. Due to the normal compensatory mechanism of the body, normal platelet counts can mask the existence of hypercoagulable states and pro-inflammatory tumor phenotypes [13].
Platelet distribution width (PDW) reflects changes in platelet size. Mean platelet volume (MPV) is an index which reflects activation of platelet. They are associated with the prognosis of a variety of tumors, including colorectal cancer [14], invasive bladder cancer [15], esophageal cancer [16], pancreatic cancer [17], breast cancer [18], melanoma [19], nasopharyngeal cancer [20], etc. Both PDW and MPV are easy-to-detect indicators in routine blood tests, and their prognostic role in hepatocellular carcinoma has not been explored. Therefore, the aim of this study was to explore the prognostic significance of platelet indices in HCC patients.
Basic characteristic of the HCC patients
Basic characteristic of the HCC patients
Notes: HCC: hepatocellular carcinoma.
The basic parameters of the patients included in the study are presented in Table 1. A total of 260 patients were incorporated in the study between January 2009 and December 2015. The average age was 50.1
The PDW value ranges from 8.2 to 21.6. In the light of the receiver operating characteristic (ROC) curve, 12.9 was identified as the optimal cutoff value of PDW. And the sensitivity and specificity of PDW in OS were 64.3% and 69.7%, respectively (Fig. 1A). Patients were then separated into two groups based on the cutoff value: patients with high PDW values and patients with low PDW values. Among them, 173 patients had PDW
A. Optimal cutoff value for the PDW was identified by ROC curve. B. Kaplan-Meier analysis of OS in HCC patients according to PDW groups. Notes: ROC: receiver operating characteristic curve; OS: overall survival; HCC: hepatocellular carcinoma.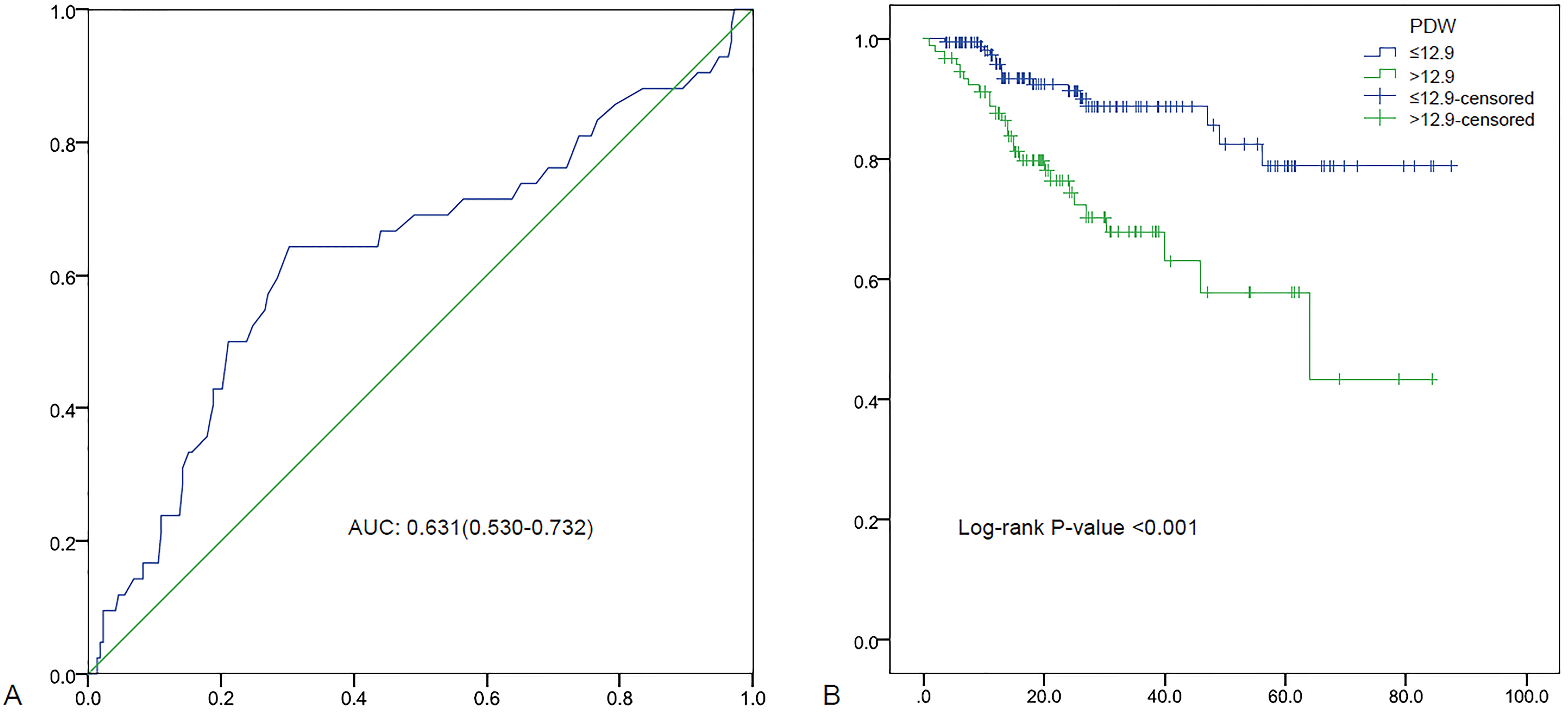
Relationship between PDW and clinicopathological features of patients with HCC
Note: Bold represents
Baseline parameters of patients with hepatocellular carcinoma based on PDW levels
Note: Bold represents
Univariate and multivariate analyses of parameters in HCC patients
Note: Bold represents
The relationship between PDW and clinicopathological features and blood parameters are presented in Tables 2 and 3. No statistical difference were found in age, gender, hepatitis B surface antigen, anti-HBV treatment, tumor diameter, tumor number, alpha-fetoprotein (AFP), Barcelona Clinic Liver Cancer (BCLC) stage, tumor differentiation, gamma-glutamyl transpeptidase (GGT), albumin (ALB), lymphocyte to monocyte ratio (LMR), and neutrophil to lymphocyte ratio (NLR) between the high PDW group and the low PDW group. Nevertheless, there were significantly statistical differences between the two groups in portal hypertension, vascular invasion, Child-Pugh grade, prothrombin time (PT), fibrinogen (Fib), total bilirubin (TB), platelet (PLT), MPV, and platelet to lymphocyte ratio (PLR).
Spearman correlation analysis showed that PDW was positively correlated with PT (
Kaplan-Meier method was utilized to analyze the prognosis of patients in the high PDW group and low PDW group. The results of the survival analysis are presented in Fig. 1B. Compared with patients in the low PDW group, the 5-year overall survival (OS) rate was poor in patients with high PDW group (90.5% versus 71.7%,
As shown in Table 4, in univariate regression analysis, age, tumor diameter, alpha-fetoprotein, vascular invasion, BCLC stage, Fib, GGT, PDW, NLR, PLR, and LMR were all significantly correlated with OS. No other clinical pathological features and blood parameters were found to be significantly correlated with OS. The statistically significant factors of univariate regression analysis were then put in multivariate regression analysis. Multivariate regression analysis showed that alpha-fetoprotein, GGT, and PDW were independent prognostic factors in patients with hepatocellular carcinoma.
As far as we know, this is the first time to explore the prognostic role of PDW in hepatocellular carcinoma patients and its correlation with clinicopathological features. In this study, we found that PDW is correlated with overall survival in HCC patients and is an independent prognostic factor affecting the prognosis of patients with hepatocellular carcinoma.
Platelets are the main cells active in hemostasis and thrombosis, and play important roles in various physiological and pathophysiological processes of the body, including immune response, inflammation, and angiogenesis. Moreover, platelets also play a crucial role in tumor growth and metastasis [3]. PDW, as an essential parameter of platelet activation, plays an important role in the prognosis of various tumors. For example, PDW has been demonstrated to be a prognostic risk factor in laryngeal cancer [21], colorectal cancer [22], thyroid cancer [23], nasopharyngeal carcinoma [20] and melanoma [19], but Cui’s study found that PDW is a protective factor for the prognosis of non-small cell lung cancer [24]. Consistent with most literatures, our study found elevated PDW is an independent risk factor for prognosis in patients with hepatocellular carcinoma. These contradictory results may be explained by different tumor types, the small sample size, and selective bias. Therefore, it is necessary to conduct large-scale multi-center studies for verification.
The mechanisms that explain the relationship between PDW and the prognosis of patients with hepatocellular carcinoma are rarely elucidated. Dysfunction of bone marrow megakaryocytes may result in a change in the PDW value of the measure of platelet heterogeneity [25]. Studies have shown that macrophage colony-stimulating factor (M-CSF), granulocyte colony-stimulating factor (G-CSF) and interleukin-6 (IL-6) can regulate megakaryocyte maturation, platelet size and platelet production [26]. G-CSF and M-CSF secreted by cancer cells can facilitate megakaryocyte production and subsequent platelet production in tumor micro-environment [27]. Besides, IL-6, as an important pro-inflammatory cytokine in the tumor microenvironment, has been found to be abnormally elevated in almost all types of tumors. Studies have shown that IL-6 promotes tumor progression by regulating cell proliferation, apoptosis, metabolism, survival, angiogenesis and metastasis [28]. In addition, a potential mechanism is that platelets can facilitate a hypercoagulable state in the tumor microenvironment [3]. Activation of platelets can enable cancer cells to encompass themselves with platelets and escape the body’s immune defense attacks [29].
At the same time, there are some limitations in our research. First, we did not deeply study the exact molecular mechanism of PDW affecting the prognosis of HCC patients. Second, the patients we included in our study were all Chinese, and whether the results were applicable to other races remains to be verified. Third, the number of patients incorporated in the study is quite small, and the statistical power is weak. Subsequent large-sample data is required for verification. Fourth, some patients have short follow-up time and may have an influence on overall outcomes. Finally, this is a single-center study that requires multiple centers to further verify the reliability of the results.
In conclusion, elevated PDW levels can serve as a biomarker for poor prognosis in hepatocellular carcinoma, and further research is needed to elucidate the exact mechanism of PDW in hepatocellular carcinoma. This easy-to-detect and inexpensive marker may play a significant role in clinical decisions in the future.
Patients and methods
Study population
This retrospective study included 260 cases of hepatocellular carcinoma diagnosed between January 2009 and December 2015 in The Third Affiliated Hospital of Sun Yat Sen University. The inclusion criteria for this study were: (1) All patients underwent radical resection of liver cancer; (2) Postoperative pathology confirmed hepatocellular carcinoma; (3) No extrahepatic metastasis; (4) no treatment with radiotherapy or chemotherapy before surgery. Preoperative severe systemic diseases such as hematopoietic diseases, other malignant tumors, autoimmune diseases, coronary heart disease, high blood pressure, etc. will be excluded from the study. Early morning fasting venous blood samples were collected within 1 week prior to surgery. When there are multiple tumors, the diameter of the tumor is the sum of the diameter of multiple tumors. BCLC staging was used to identify the clinical stage of hepatocellular carcinoma. The study was authorized by the Ethics Committee of The Third Affiliated Hospital of Sun Yat Sen University, and all patients who participated in the study signed informed consent. Abdominal ultrasonography, chest X-ray examination and routine monitoring of serum AFP levels were performed every 3 to 6 months after surgical resection. The OS is defined as the time interval between the day of surgery and the day of death or the last follow-up.
Statistical analysis
SPSS software version 22.0 (IBM, Chicago, IL, USA) was used to conduct statistical analysis. The best cutoff values for age, PT, Fib, TB, GGT, ALB, platelet indices, NLR, PLR, LMR were determined by using the ROC curve. The statistical description of the categorical variables is shown as a percentage of the number, while the statistical description of the continuous variables is presented using the mean
Footnotes
Acknowledgments
This work was funded by the National Natural Science Foundation of China (project number: 81670517). At the same time, I would like to thank the Third Hospital of Sun Yat-sen University for providing the data of HCC patients.
Conflict of interest
The authors declare that they have no competing interests.
Supplementary data
Spearman correlation between PDW and other haematological indicators Notes: PDW: Platelet distribution width, PT: prothrombin time, Fib: fibrinogen, MPV: Mean platelet volume, PLT: platelet, TB: bilirubin.
Variables
AUC
95% CI
PDW
0.631
0.530–0.732
PT
0.424
0.328–0.519
0.118
Fib
0.626
0.528–0.724
MPV
0.513
0.411–0.615
0.787
PLT
0.518
0.420–0.615
0.715
TB
0.494
0.399–0.589
0.901
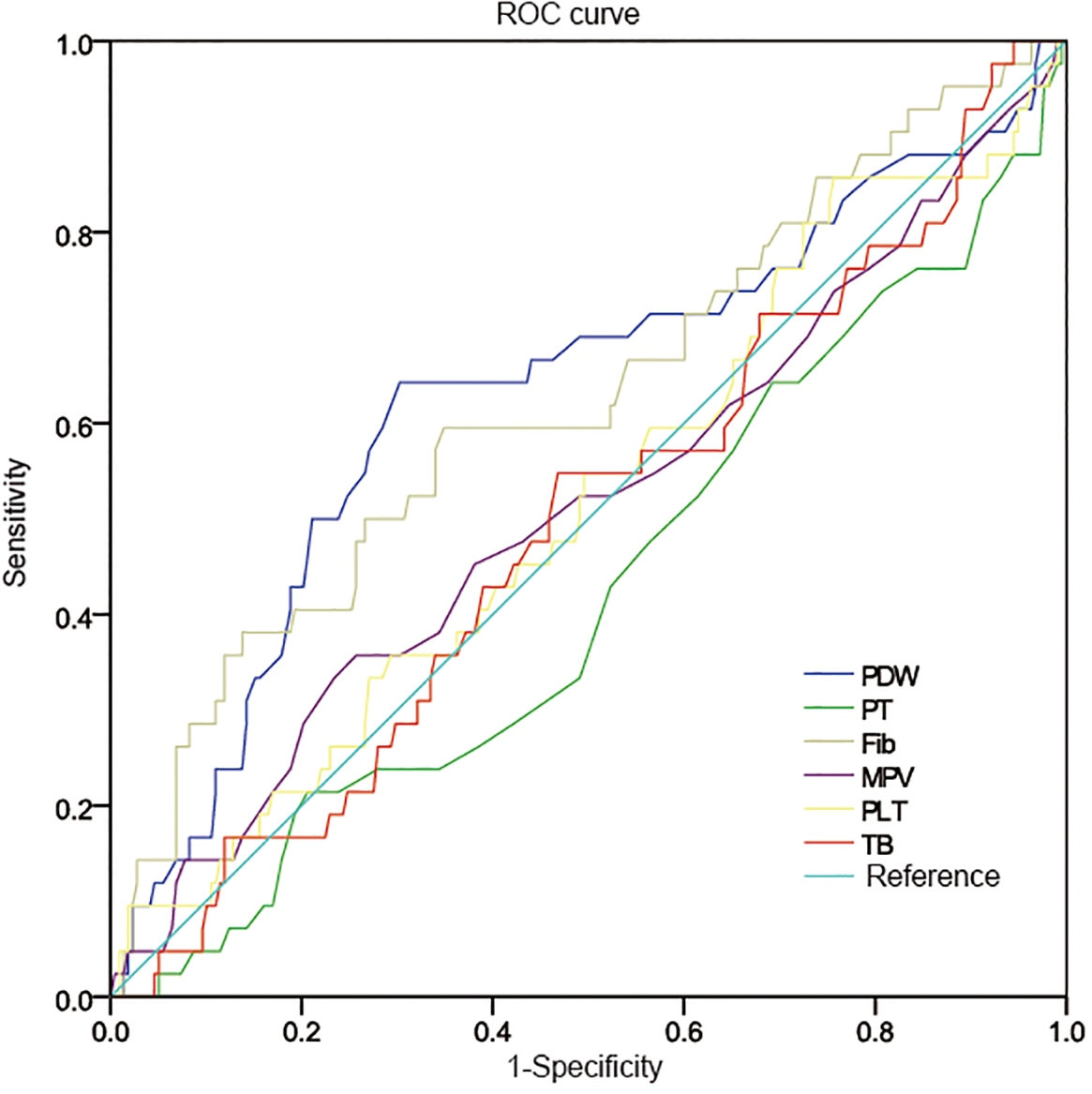
ROC analyses for haematological indicators Notes: AUC: the areas under the curve, CI: confidence interval, PDW: Platelet distribution width, PT: prothrombin time, Fib: fibrinogen, MPV: Mean platelet volume, PLT: platelet, TB: bilirubin.
Variables
PDW
Spearman correlation
PT
0.222
Fib
0.249
MPV
0.869
PLT
0.386
TB
0.144
ROC curve for haematological indicators. Notes: PDW: Platelet distribution width, PT: prothrombin time, Fib: fibrinogen, MPV: Mean platelet volume, PLT: platelet, TB: bilirubin.