Abstract
Gender differences in schizophrenia have received ample attention over recent decades. Consistently reported gender differences in schizophrenia include age at onset, clinical presentation, course, social functioning, therapeutic alliance, and treatment response [1–5]. It should be noted, however, that evidence to support reported gender differences is still preliminary because schizophrenia is a heterogenous disorder, possibly determined by a host of biological and sociocultural factors [5–7]. As a result, findings obtained in Caucasian patient populations may not be applicable to other ethnic groups in different sociocultural settings.
In the past two decades, quality of life (QOL) has been gaining attention as an important outcome measure in psychiatric practice because it could give a comprehensive view of the effectiveness of pharmacotherapeutic and psychosocial interventions [8]. A number of factors, including sociodemographic characteristics [9], psychotic and depressive symptoms [10–12], drug-induced side-effects [13], and length of illness [14] are all related to poor QOL in schizophrenia. There is preliminary evidence of cross-cultural or ethnic differences in the QOL of psychiatric patients [15], and it is likely that findings reported from Western countries do not apply to patients with different ethnic and cultural backgrounds. To the best of our knowledge, no study in China has addressed gender in schizophrenia and its relationship with QOL using standardized assessment methods.
The aim of the present study was therefore to examine (i) gender differences with regard to sociodemographic and clinical characteristics in schizophrenia outpatients in two major Chinese cities, Beijing and Hong Kong; and (ii) the association between gender and QOL in schizophrenia patients. In view of earlier findings [6,7,15], we hypothesized that gender differences in one or more sociodemographic or clinical characteristics would exist in Chinese schizophrenia patients. We also expected that female patients would have a better QOL than their male counterparts.
Schizophrenia outpatients deserve special attention because they account for >90% of the whole schizophrenia patient population in China, comprising approximately 5 million outpatients [16].
Methods
Settings and subjects
The present study was part of a large-scale project on QOL in schizophrenia outpatients in China. A detailed description of the study design and data collection has been reported elsewhere [17]. Briefly, subjects in Hong Kong were randomly selected from the schizophrenia patients who attended the outpatient department (OPD) of a university-affiliated general hospital serving a population of approximately 800 000. Their Beijing counterparts, matched according to gender, age, age at onset and length of illness, were recruited from schizophrenia patients who attended the Adult Psychiatric OPD at Beijing Anding Hospital, a teaching psychiatric hospital serving a population of approximately 3 000 000 in Beijing.
Patients who met the following inclusion criteria were invited to participate in the study: (i) diagnosis of schizophrenia according to DSM-IV; (ii) age between 18 and 60 years; (iii) length of illness ≥5 years; and (iv) being outpatients who had been clinically stable for ≥3 months before recruitment [18]. The exclusion criteria were: (i) history of or ongoing major chronic medical or neurological condition(s); and (ii) past or current significant drug/alcohol abuse other than nicotine.
The course of recruitment was as follows: (i) at the Hong Kong site, all schizophrenia patients meeting the study criteria were identified with the computerized Chart Management System (CMS) by the principal author before their attendance at the OPD; (ii) subjects were randomly selected from the total number of eligible patients and invited to participate in the study; (iii) in Beijing, once schizophrenia patients registered at the OPD of Anding Hospital, their medical records were screened to establish eligibility for the study, and the first patient who matched a previously unmatched Hong Kong counterpart was invited to participate; and (iv) the principal author spent 2 months alternatively in Hong Kong and Beijing selecting, recruiting, and assessing the subjects.
The study protocol was approved by the Joint Chinese University of Hong Kong and New Territories East Cluster Clinical Research Ethics Committee in Hong Kong and the Human Research and Ethics Committee of Beijing Anding Hospital. Written consent was obtained from all subjects.
Data collection
The principal author assessed all subjects throughout the study and conducted interviews on the day that the subjects attended the OPD. Sociodemographic and clinical data were extracted from medical notes and confirmed during the interview.
Assessment tools and procedures
Psychotic symptoms were measured with the Brief Psychiatric Rating Scale [19]. The following three mean symptom scores of the scale were used: (i) positive (conceptual disorganization, suspiciousness, hallucinatory behavior, and unusual thought content); (ii) negative (emotional withdrawal, motor retardation, blunted affect, and disorientation) [20]; and (iii) anxiety and tension [10]. The 17-item Hamilton Depression Rating Scale was used to assess the severity of depressive symptoms [21]. Extrapyramidal side-effects (EPS) were evaluated with the Simpson–Angus Scale of Extrapyramidal Symptoms [22] and the Barnes Akathisia Rating Scale [23]. The sum scores of these scales were entered into the statistical analysis [24].
QOL is defined as ‘an individual's perception of one's position in life in relation to goals, expectations, standards and concerns in the context of the culture and value systems in which one lives’ [25]. It was assessed with the Hong Kong and mainland Chinese versions of the World Health Organization Quality of Life Schedule–Brief [26] in Hong Kong and Beijing, respectively. The two QOL schedules are nearly identical, and both cover four domains: physical and psychological health, social relationships, and environmental factors. Doses of antipsychotic drugs (AP) were converted to chlorpromazine equivalents [27]. A suicide attempt was defined as ‘a self-destructive act carried out with at least some intent to end one's life’ [28].
To check the consistency of the principal author's ratings, before the study an interrater reliability exercise of all rating instruments was conducted involving another qualified psychiatrist on 20 randomly selected schizophrenia patients. The intra-class correlation coefficients (ICC) for all instruments tested were >0.75.
Statistical analysis
The data were analysed using SPSS 13.0 for Windows (SPSS, Chicago, IL, USA). The comparison between the two genders with respect to sociodemographic and clinical characteristics was performed using independent sample t-test, Mann–Whitney U-test, and χ2 test as appropriate. Multiple logistic regression analysis was used to adjust for relevant covariates and to determine the independent correlates of gender. Gender was the dependent variable, and the independent variables included age, marital and employment status, education level, monthly income, age at onset, length of illness, number of admissions, lifetime suicide attempts, severity of psychopathology, drug-induced EPS, and depressive symptoms, taking typical APs only, atypical APs only, doses of APs, and each domain of QOL. The one-sample Kolmogorov–Smirnov test was used to check the normality of distribution for the continuous variables. The level of significance was set at 0.05 (two-tailed).
Results
Two hundred and ninety-eight patients in Hong Kong and 288 patients in Beijing were invited to participate in the study. Forty-three patients in Hong Kong and 38 in Beijing declined to take part. There was no significant difference between those who participated and those who declined to take part in the study in terms of age, gender, age at onset, or length of illness. The two samples in Hong Kong and Beijing were combined because they were both drawn from a population of clinically stable outpatients and were matched according to basic sociodemographic and clinical variables. There were 251 male and 254 female patients in the combined sample.
Table 1 lists the sociodemographic and clinical characteristics of the whole sample and those for men and women separately, providing a comparison between the genders with regard to sociodemographic and clinical data and QOL. More male patients were employed and they had a significantly higher monthly income and took higher doses of antipsychotic drugs than the female patients.
Subject characteristics
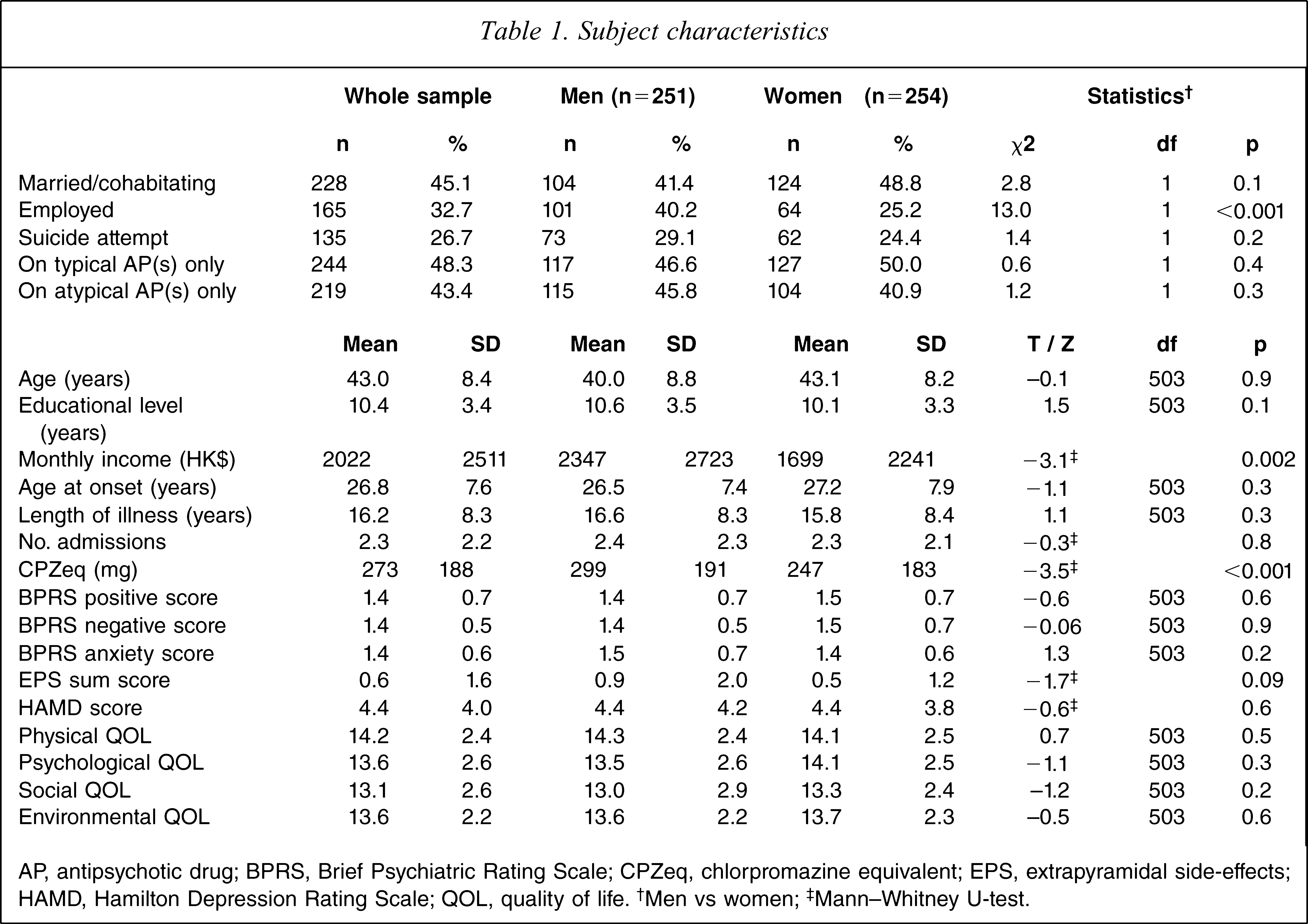
AP, antipsychotic drug; BPRS, Brief Psychiatric Rating Scale; CPZeq, chlorpromazine equivalent; EPS, extrapyramidal side-effects; HAMD, Hamilton Depression Rating Scale; QOL, quality of life. †Men vs women; ‡Mann–Whitney U-test.
On multiple logistic regression analysis, being employed, a higher dose of antipsychotic drugs, more severe EPS, and a higher score on the physical QOL were independently associated with male gender (Table 2).
Factors associated with gender on multiple logistic regression†
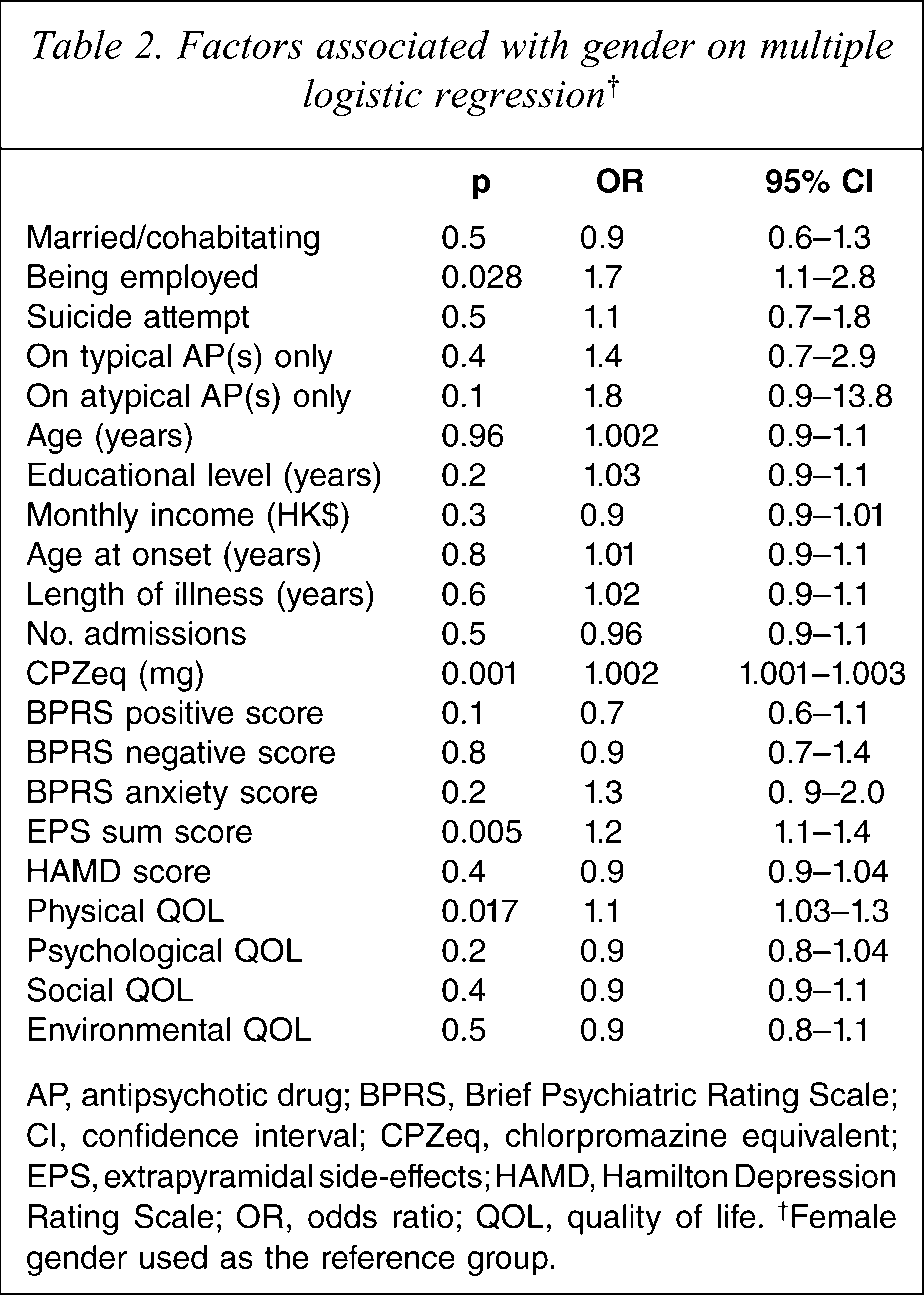
AP, antipsychotic drug; BPRS, Brief Psychiatric Rating Scale; CI, confidence interval; CPZeq, chlorpromazine equivalent; EPS, extrapyramidal side-effects; HAMD, Hamilton Depression Rating Scale; OR, odds ratio; QOL, quality of life. †Female gender used as the reference group.
Discussion
To the best of our knowledge, this was the first study to investigate the association of gender and QOL in Chinese schizophrenia patients.
The first hypothesis was supported by the results. There were differences between the two sexes in terms of employment status, monthly income, doses of APs and severity of EPS. Over recent decades it has been consistently reported that men with schizophrenia have an earlier age at onset than women [3,29–31]. Several biological mechanisms for this gender difference have been proposed, including sex-linked genetic mechanisms [32], the neuroprotective effect of estrogens [33], and the increased vulnerability of the male brain due to slower maturation [34]. In the present study male patients had an earlier age at onset than female patients, but the difference did not reach a statistically significant level. The discrepancy between our results and those of the mainstream literature could be due to the following reasons. First, the age at onset of schizophrenia is likely to be influenced by both biological and social factors [5,35]. Consequently, differences in the sociocultural environment between Caucasian and Chinese populations could explain the difference in findings. Second, there is evidence that men have an earlier age at onset only in the 15–25 year age group, whereas equal numbers of men and women fall ill between the ages of 25 and 35. After the age of 35 more women are diagnosed with schizophrenia [36]. In the present sample the mean age at onset was 26.5 years in men and 27.2 years in women in the age range of 25–35 years, supporting Castle's findings [36]. The relationship between gender and age at onset needs to be further explored in different ethnic groups and sociocultural contexts.
The ratio of the lifetime suicide attempts – an important risk factor for completed suicide [37,38] – between women and men in the present study was 0.8, considerably lower than the figure of 2.7 found in the general Chinese population [39]. This discrepancy is compatible with the fact that the prevalence of and gender ratio in suicidal behavior and completed suicide are different between the general population and schizophrenia patients [38–40]. In a retrospective survey, 9156 schizophrenia patients were followed up for 17 years after their first admission in Denmark [40]. The female/male suicide ratio was 0.7, very similar to the ratio of suicide attempts found in the present study.
Women with schizophrenia have been found to have better social functioning and more post-hospitalization employment than their male counterparts [1,2,41]. In the present study, however, more men were found to be employed. The attitudes of Chinese society towards women with psychiatric disorders might be behind this surprising finding. In China, men are traditionally regarded as the ‘pillar’ of the family. Their role is to take full responsibility to support the whole family. Most women with schizophrenia, even if they are clinically stable and have better social functioning than male patients, are expected to stay at home as housewives. In addition, Chinese women with psychiatric disorders suffer from more severe discrimination when applying for jobs than men [42]. All of these factors could lead to a lower rate of employment and lower monthly income in women with schizophrenia.
The male patients in the present study took higher doses of antipsychotic drugs and experienced more severe EPS than the female patients, confirming most [43–45] but not all [46] previous findings. In addition to the variables controlled in the present study, other factors that could play a role in determining antipsychotic doses, treatment responses, and side-effects such as genetics, height, weight, lean muscle–fat ratio, diet, exercise, smoking, alcohol abuse, and use of concomitant medication [1] were not included. Therefore, the relationships between gender with antipsychotic doses and side-effects need to be further explored.
Women with schizophrenia have been reported to have better social functioning, more employment, less severe psychopathology, fewer and shorter hospitalizations, more benign courses of the disease, more favourable outcomes, and fewer criminal records [1,2,41,47,48]. Consequently, we hypothesized that female schizophrenia patients would have a better QOL than their male counterparts. The results, however, did not support this hypothesis. There was no significant difference between the two genders in any of the QOL domains on univariate analysis, but female patients had a lower score in the physical domain after adjusting for sociodemographic and clinical variables. This result suggests that there might be an independent association between gender and QOL in schizophrenia, although female gender has never been reported as an independent negative factor in any of the theoretical models of QOL in psychiatry [49–54]. According to the distress/protection QOL model [54], QOL is the outcome of an interaction between protective and distressing factors. Although most illness-related factors are more favourable to female schizophrenia patients than their male counterparts [1,2,41,47,48], their QOL was worse in the present study, suggesting that distressing factors must be negatively influencing it: this unexpected finding needs confirmation. We speculate that relatively more severe discrimination towards women with schizophrenia in Chinese society might contribute to their lower QOL.
The strengths of the present study were its large, random, and diagnostically homogeneous sample. The results should be interpreted with caution, however, because of the following methodological limitations. First, only chronic and clinically stable schizophrenia patients were included and those with a history of or ongoing major medical or neurological conditions, and past or current drug/alcohol abuse were excluded. Therefore the results may not be applicable to patients in different stages of the disorder. Second, some factors might have led to selection bias using the current recruitment strategy. For example, in Hong Kong schizophrenia patients in better economic condition are more likely to attend private psychiatrists for more convenient service provision, while the stigma attached to schizophrenia might have prevented some patients from attending outpatient clinics in both sites. Third, previous studies in the West indicated that some more variables such as premorbid functioning and family support had significant influence on QOL [55–57], therefore more relevant factors should be investigated in future studies. Finally, the severity of psychotic symptoms of patients who refused to participate in the study could not be assessed because they did not sign the consent form. Therefore, the possibility cannot be excluded that the participants represented a less or more severely disabled subgroup of schizophrenia patients.
In conclusion, gender differences with regard to sociodemographic and clinical characteristics in Chinese schizophrenia patients are not entirely consistent with the results reported in Western settings. In contrast to the generally held view based on Western studies, Chinese female schizophrenia patients do not seem to have a better QOL, and, even in the physical aspect of QOL, they fare worse than their male counterparts.
Footnotes
Acknowledgements
This study was supported by grants from the National Natural Science Foundation of China (No. 30800367), the Beijing Nova Program of the Beijing Municipal Science and Technology Commission (No. 2008B59), and a Direct Grant for Research from the Chinese University of Hong Kong (Project No. 2041454).
