Abstract
Second to symptoms, health-related quality of life (HRQOL) is one of the most widely used outcomes in schizophrenia research studies. The World Health Organization (WHO) defined HRQOL as an ‘individual's perception of their position in life in the context of the culture and value systems where they live and in relation to their goals, expectations, standards, and concern’ [1]. Conceptually, HRQOL is considered a patient-centred construct reflecting patient satisfaction with life in the context of sustained disability, and the risk residing in treatment [2,3]. To identify the determinant of HRQOL, researchers have attempted to predict HRQOL from clinical variables [4–6], psychosocial variables (such as personality traits or perceived stigma) [7], or both. A number of studies seem to suggest that symptom reductions may not be sufficient in bringing about meaningful change in HRQOL unless other issues, such as poor self-esteem and internalized stigma, are addressed [6]. Recently, a meta-analytical study found that self-reported HRQOL were only modestly related to symptoms [8]. In contrast, a growing body of research has shown that a large percentage of variance in HRQOL was related to a host of disease-independent factors, including autonomy, self-esteem, and perceived stigma [9–12]. Similarly, studies on the effectiveness of psychosocial training also found that patients’ progress in QOL was independent of improvement of symptoms [13]. Thus, this evidence seems to support the possible existence of a patient-oriented QOL model that links patient self-factors with their subjective well-being, largely independent of psychiatric symptoms.
In this regard, many researchers have recognized the term ‘recovery’ from the patient movement conveying a meaning similar to the concept of HRQOL [14,15]. Not only do both concepts reflect patients’ holistic perspectives on various life domains [14], but they also emphasize the development of human potentials to meet the demands in fulfilling personal goals and social roles [16]. Still, very few (if any) empirical studies tested the association between the two concepts. Mindful of that, the authors were interested to explore whether the broadly accepted recovery components from the patient movement are related to HRQOL reported from patients with schizophrenia spectrum disorders. Specifically, the aim of the study was to answer the following questions: (i) what is the strength of association between HRQOL and different recovery components; (ii) given that the strength of the associations is sufficiently large, in what way can we hypothesize a structural model to explain HRQOL based on relevant recovery components; and (iii) to what extent is the variance of HRQOL accounted for by a good-fit structural model.
In the present study we used the definition proposed by the Substance Abuse and Mental Health Services Administration (SAMHSA) National Consensus Statement on Mental Health Recovery [17] to operationalize the concept of recovery. A standardized measure of HRQOL, the WHO Quality of Life Inventory (WHO-QOL-BREF-Hong Kong), was used to indicate subjects’ HRQOL rating. A number of structural models showing the intercorrelations between recovery components and WHOQOL-BREF were hypothesized, and the statistical significance of each regression path was tested using structural equation modelling (SEM) analysis.
US National Consensus Statement on Mental Health Recovery
The US National Consensus Statement on Mental Health Recovery was proposed by SAMHSA as key guiding principles to enhance mental health recovery. According to the statement, mental health recovery is defined as ‘a journey of healing and transformation that enables a person to live a meaningful life in a community of his or her choice while striving to achieve his or her full potential’ [17]. The statement identifies 10 recovery components as essential mediators of recovery: (i) enhancing personal control and the self-determination of patients; (ii) implementation of person-centred treatment to enhance recovery; (iii) empowerment; (iv) enhancement of holistic well-being in mental, spiritual, and social domains; (v) awareness of the non-linear nature of recovery and recognition that positive change is possible for patients; (vi) implementing strength-based intervention, such as building resilience; (vii) strengthening patient-peer support among individuals with mental disorders; (viii) promoting respect at a personal level and eliminating stigma from society; (ix) encouraging patients to bear responsibility in recovery and personal health care; and (x) instillation of hope for recovery. These 10 recovery components were measured on 12 psychometric scales in the present study (Table 1). The preliminary hypothesis was that all 12 variables would be positively correlated to WHOQOL-BREF. We also noted, however, that the subjects with a Chinese cultural mindset may interpret the importance of each recovery component differently to their Western counterparts. For instance, Chan et al. and Hsiao et al. noted that the Western principle of recovery based on autonomy and independence may not fit the needs of Chinese patients, who have a concept of self embedded in collectivist Confucian values [18,19]. Therefore, the second objective of the presents study was to determine whether the recovery principles proposed by SAMHSA are significantly correlated with HRQOL of Hong Kong Chinese patients.
Psychometric scales used in canonical correlation analysis (n=201)
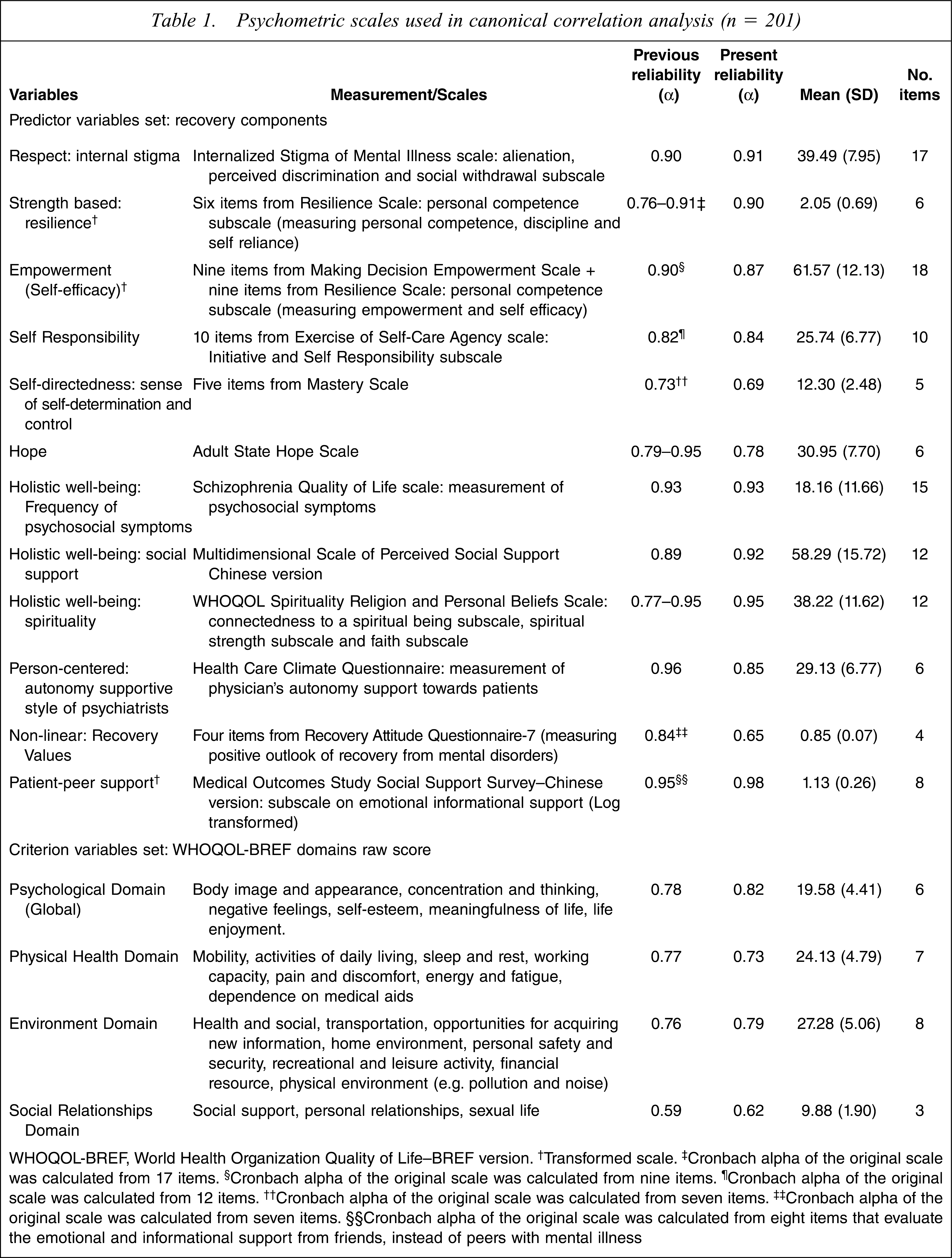
WHOQOL-BREF, World Health Organization Quality of Life–BREF version. †Transformed scale. ‡Cronbach alpha of the original scale was calculated from 17 items. §Cronbach alpha of the original scale was calculated from nine items. ¶Cronbach alpha of the original scale was calculated from 12 items. ††Cronbach alpha of the original scale was calculated from seven items. ‡‡Cronbach alpha of the original scale was calculated from seven items. §§Cronbach alpha of the original scale was calculated from eight items that evaluate the emotional and informational support from friends, instead of peers with mental illness
Method
Sample
From two participating psychiatric outpatient clinics in Hong Kong, 201 patients aged 18–60 years were recruited. Only patients who were diagnosed with schizophrenia, schizophreniform, or schizoaffective disorder were recruited for the study. After a complete description of the study to participants, written consent was obtained from the individuals. All participants who consented to participate were screened with the Capacity to report subjective quality of life (CapQOL) inventory to ensure their competence in answering questions on QOL [20]. Finally, 55% of the eligible subjects who met the inclusion criteria agreed to participate in the study. Prior to data collection, ethics approval was obtained from both the ethics committees of the Hospital Authority and the university involved.
Quality of Life measures
Subjects’ quality of life was measured using the WHOQOL-BREF(HK). The instrument has well-established reliability and validity among Chinese people with schizophrenia. WHOQOL perception among people with schizophrenia was found to be negatively correlated with symptoms measured on the Brief Psychiatric Ratings Scale [18,21]. The WHOQOL-BREF(HK) consisted of 26 questions from the global version (WHOQOL-BREF) and two national items from the WHOQOL-100(HK). The two items were related to ‘satisfaction in eating’ and ‘feeling of being respected and accepted’ and were grouped under the psychological domain of the instrument. The 28-item WHOQOL-BREF(HK) yielded four domain scores that reflect subjects’ HRQOL in the areas of physical health, psychological health, social relationships, and environmental satisfaction.
Recovery component measures
Twelve psychometric instruments were used to measure patients’ recovery as defined by the SAMHSA statement. The internal consistency for each scale in previous studies and the present study are shown in Table 1. Perceived respect was measured by alienation, perceived discrimination, and the social withdrawal subscale of the Internalized Stigma of Mental Illness (ISMI) scale. The validity and reliability of the ISMI are well established to reflect the subjective experience of stigma among populations with mental disorders, with a test–retest reliability coefficient of 0.90 [22]. Strength of patients was assessed on a 17-item, personal competence subscale of the Resilience Scale (RS) [23]. Empowerment was measured by a nine-item, self-esteem self-efficacy subscale of the Making Decision Empowerment scale (MDES) [24]. The scale was developed to assess level of empowerment. The MDES has been validated in US and Swedish patient samples, with good validity and reliability [25]. The self-efficacy, self-esteem subscale that was applied to measure the psychological aspect of empowerment has demonstrated strong stability across cultures. Personal responsibility was measured by the initiative and self-responsibility subscale of the Exercise of Self Care Agency (ESCA) scale [26]. The subscale, which is composed of 12 items, measured subjects’ sense of responsibility towards self-care. The ESCA scale has been validated in previous studies and has demonstrated satisfactory reliability and validity among general population [27].
Sense of self-determination was measured on the seven-item Mastery Scale (MS) [28]: a scale that assesses perceived ability to exercise control in the daily course of life. The MS has demonstrated good validity and reliability among subjects with severe mental disorders [29,30]. Hope was assessed on the Adult State Hope Scale (ASHS), a six-item measure of hope specific to accomplishing goals. The measure demonstrates good internal consistency in the US population [31]. Person-centred treatment was measured by the Health Care Climate Questionnaire (HCCQ), a scale that assesses the level of autonomy support that patients received from psychiatrists. Autonomy support is defined as a style of interaction between a clinician and a patient by which the patient's initiatives were encouraged, and their viewpoints were acknowledged by the clinicians reacting responsively to their concerns and offering free choices to meet their needs. The scale, which consists of six items, demonstrated good internal consistency and predictive validity in previous studies [32].
Adherence to a non-linear concept of the recovery process was measured on the Recovery Attitude Questionnaire (RAQ-7). The RAQ-7 was developed from patient groups with the aim of measuring patient compliance to recovery values. Internal consistency and test–retest reliability of the RAQ-7 have met conventionally accepted standards in US samples [33]. The RAQ-7 originally consisted of seven items but, when pilot tested among Hong Kong Chinese subjects, who held different recovery beliefs, the internal consistency of the scale dropped to 0.56. In view of that, two items with low corrected item-total correlation were deleted from the scale, and Cronbach alpha was raised to 0.63. Patient-peer support was measured by the Emotional Informational Support Scale of the Medical Outcome Study Social Support Survey Chinese version (EISS-MOS-SSS-C) [34]. The original scale was modified to measure the peer support that subjects received from other patients. Subjects were asked to recall any acquaintances with mental illness with whom they could easily get along. If ‘patient-peer(s)’ did exist, subjects were asked to rate on an eight-item scale that measured the emotional and informational support they received from their peer(s). Summation score from the EISS ranged from 8 to 40, with the lowest score indicating the absence of peer support. For subjects who reported not having any patient-peers, the minimum value was automatically imputed.
Holistic well-being was assessed in three areas: psychosocial symptoms (emotional well-being), social support (community well-being), and spirituality. Frequency of psychosocial symptoms was measured on the 15-item psychosocial subscale of the Schizophrenia Quality of Life Scale (SQLS) [35]. The subscale has demonstrated excellent internal reliability and validity among people with schizophrenia. Social support was measured on the Multidimensional Scale of Perceived Social Support–Chinese version (MSPSS-C), a 12-item scale indicating perceived social support from friends and family members [36]. Spirituality was measured on the WHOQOL Spirituality Religion and Personal Belief Scale (WHOQOL-SRPB-HK). Among the eight facets of the WHOQOL-SRPB-HK, three (connectedness to spiritual beings, spiritual strength, and faith subscales) were selected for the present study because only these three provide a pure measure of subjects’ spirituality, uncontaminated by mental health conditions [37]. These four-item subscales have demonstrated excellent reliability and validity with internal consistency coefficient between 0.77 and 0.95 [38].
With the exception of the MSPSS-C, WHOQOL-SRPB-HK, and MOS-SSS-C, all scales were translated directly from English to Cantonese by an experienced linguist. All Chinese items were pilot tested among patients with schizophrenia to ensure that their proper meaning was understandable to subjects. The internal consistency of each scale was cross-checked in the pilot stage before being applied in the main study. The research team then discussed and modified items to ensure the accuracy in the meaning of each question. To improve the validity of translated question items, confirmatory factory analyses (CFAs) were conducted on the data collected from the main study prior to performing SEM analysis. Unidimensionality of each recovery variable was supported in the CFAs.
Sample characteristics
The sample consisted of 107 male and 97 female subjects with a mean age of 42 years (SD = 9.15). More than 60% of the subjects had never been married; around one-third (29%) were currently married, and <10% had been previously married. More than half (56%) had attained senior high school education or beyond. More than three-quarters (78%) were residing with family members; <20% were living alone, and 5% were living in hostels. Close to one-third (32%) of the subjects were unemployed, while another one-third (32%) were currently employed in a competitive job. The rest were working in sheltered workshops, working as homemakers, or retired. The mean age at disease onset was 25 years (SD = 7.72), and the mean duration of untreated psychosis (DUP) was approximately 1 year (SD = 3.03). Approximately one-third of the subjects had engaged in some form of social welfare services during the 12 months preceding the interview.
Statistical analysis
Prior to the main analysis, item analysis was performed on each scale measuring recovery components. Question items showing an item-total correlation of <0.30 were excluded from the analysis [39]. Two items from the ESCA scale, two items from the MS and three items from RAQ-7 were excluded from analysis. The impact of exclusion was minimal but, given that three items had low item-total correlation on the RAQ-7, the notion of ‘non-linear recovery values’ may not be applicable to present Chinese sample. Variables demonstrating considerable overlap in multicollinearity diagnosis were reanalysed using principal component analysis (PCA) to identify their unique components and grouped under the respective recovery components for further analysis. To improve linearity, transformations were performed on variables showing extreme skewness or kurtosis before performing the multivariate analysis.
Analyses were conducted in two stages. In the first stage, canonical correlation analysis (CCA) was applied to define the nature of relationship between recovery components (RC) as a set of predictors and the WHOQOL-BREF(HK) domains as a set of criterion variables. RC(s) attained to canonical loading (within-set, variable–variate correlations) of >0.30 in magnitude were considered important in their association with the WHOQOL-BREF. Such RC(s) were admitted to further analysis. In the second stage, hypothesized structural models were tested for overall model fitness using SEM. The best-fit model with the highest percentage of predicted variance in WHOQOL was selected for final interpretation. All SEM statistics were estimated using the maximum likelihood method in AMOS 6.0 (SPSS, Chicago, IL, USA); other statistical analyses were conducted using SPSS version 15.0 (SPSS, Chicago, IL, USA).
In SEM, the fit between data and model was evaluated using comparative fit index (CFI), Tucker–Lewis index (TLI), standardized root mean square residual (SRMR), root mean square error of approximation (RMSEA), and normed χ2 (χ2/df). Because all models were over-identified and the sample size was moderately large, χ2 test tended to falsely reject the exact fit hypothesis between the data and model, thus making it unsuitable as a criterion for judging overall model fitness. Models were therefore considered as having adequate fit if CFI and TLI ≥0.90, SRMS < 0.08, RMSEA < 0.10 and 1 ≤ χ2/df ≤ 5 [40].
Hypothesized structural models
A recent study by Bjorkman and Svensson showed that 67% of the variance in QOL can be explained by social network, psychosocial functioning, and internalized stigma [41]. Although no concrete evidence showed the direction of causality between the three concepts, some studies suggested that the perception of stigma is a mediator between negative social experience and QOL [42]. Others found that internal stigma contributes to hopelessness, contraction in social network, and poor self-esteem among patients with schizophrenia, resulting in negative recovery outcomes [43–45]. Although the exact causal pathways between perceived stigma and psychosocial symptoms and social support remain unclear, one possible explanation is that psychosocial symptoms and internal stigma affect the expectation of patients in receiving support from others (including services), hence predisposing them towards withdrawal from supportive networks. In view of this, a simple model was initially proposed to explain HRQOL: a model in which psychosocial symptom (B) contributes to internal stigma (C), and both (B) and (C) contribute to the latent variable WHOQOL-BREF (A) through perceived support (F). In the model, both (B) and (C) are also directly associated with WHOQOL-BREF (A). We named this simple model (with variables A, B, C, and F) the baseline model.
The capability approach to quality of life proposed that QOL can be construed in terms of personal agency, apart from being conceptualized as personal well-being. According to the theory, patients’ personal agency can be actualized only through a supportive social environment in which opportunities are available with expectation (hope) being lifted to a reasonable level, and personal capacities being developed without hindrances [46,47]. Based on this concept, Hopper developed a recovery framework for patients with mental disorders. In his framework, four facilitating elements of recovery were delineated: (i) renewed sense of hope, (ii) regaining social competence through mitigation of psychosocial symptoms, (iii) reconnecting with supportive network, and (iv) rebuilding a functional sense of self or a healthy self-sense of self-agency [46]. In accordance with this theory, we grouped 11 recovery component variables under four constructs and used these as building blocks for structural models. The constructs are outlined as follows: (i) psychosocial symptoms (SQLS) (variable B); (ii) personal agency, defined as patients’ perceived ability to perform intentional self-directed action [31] (latent variable D) (the latent variable is manifested in four observable domains, including self-esteem and self-efficacy (MDES), responsibility in self-care (ESCA), resilience (RS), and sense of mastery in daily setting (MS); (iii) optimism (latent variable E), manifested as motivational hope and general hope (motivational hope refers to the positive expectation that drives a person towards achieving goals (ASHS) [48], whereas general hope refers to a sense of possibility that recovery is possible (RAQ-7); and (iv) perceived support (latent variable F), manifested in four observable variables, including social support from friends and family (MSPSS-C), emotional support from patient-peers (EISS-MOS-SSS-C), autonomy support from clinicians (HCCQ), and spiritual support derived from spirituality (WHOQOL-SRPB-HK).
Derived from the capability framework, we proposed that a higher level of social competence (fewer psychosocial symptoms, B) is associated with a higher level of perceived support (F), which leads to an elevated sense of optimism (E), resulting in the realization of personal agency that contributes to a higher level of HRQOL in patients. On top of this pathway (B→F→E→D→A), we overlaid the baseline model and hypothesized a final model (Figure 1). In between the baseline model and the final model, we also hypothesized a reduced model with the following pathway: B→F→E→D→A, which we referred to as the capability model.
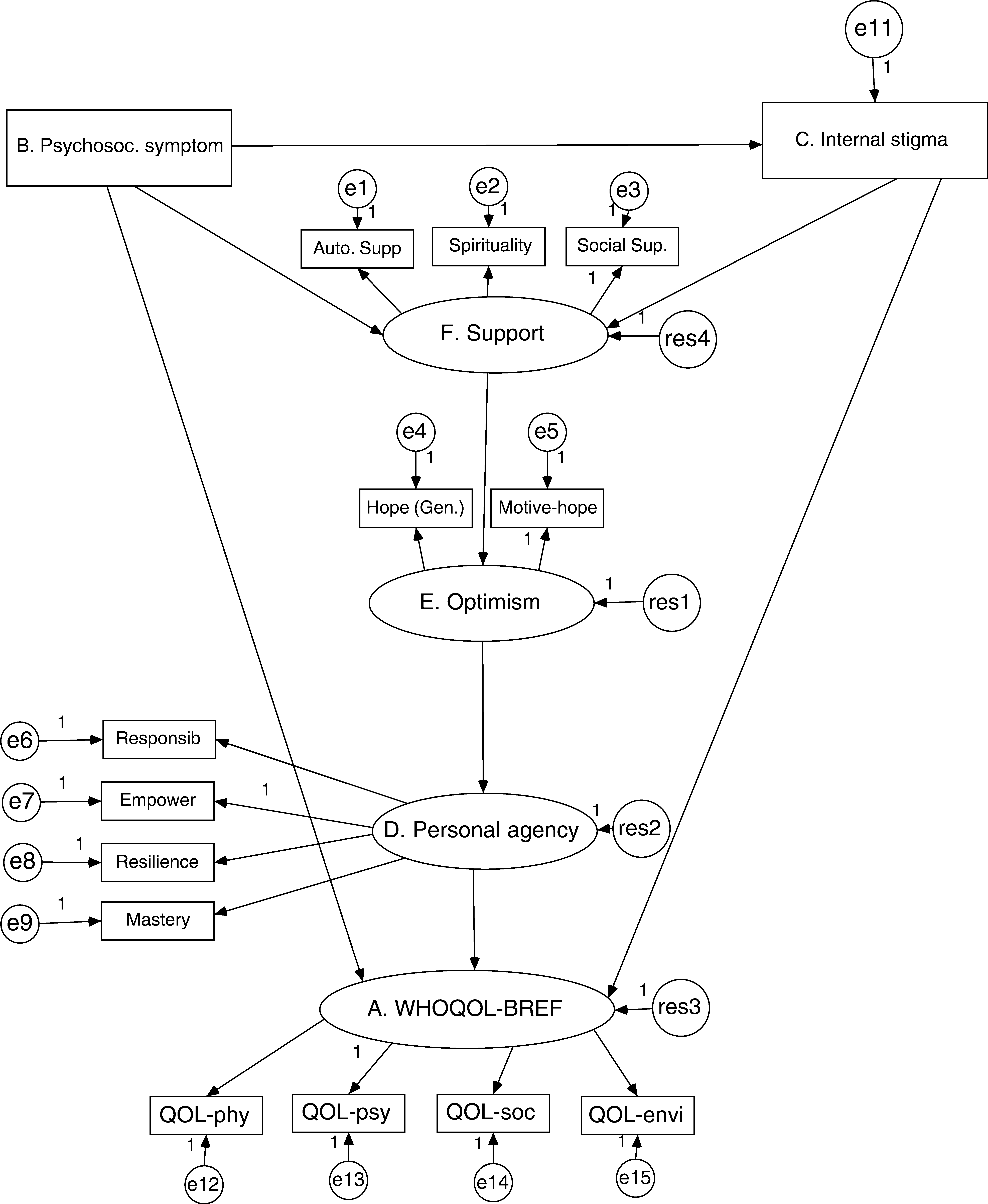
Hypothesized structural model 3. QOL, quality of life; WHOQOL-BREF, World Health Organization Quality of Life–BREF version.
Results
Pre-analysis: item and principal component analysis
Low corrected item-total correlation were observed in items measuring Self-responsibility (ESCA-ISR, α = 0.81), Self-direction (MS, α = 0.66), and Non-linear recovery attitude (RAQ-7, α = 0.56). After dropping these items, the internal consistency (α) of these scales rose to 0.84, 0.69, and 0.65, respectively. Internal consistency (α) of the remaining RC variables ranged from 0.78 to 0.98, demonstrating good internal consistency.
Multicollinearity between variables was checked using SPSS COL-LINEARITY DIAGNOSTIC procedures. The test indicated a large amount of shared variance between the Resilience scale and Empowerment scale. Upon closer examination of the question items, the investigator found many similar items across the two scales. Therefore, PCA was applied to regroup items according to the underlying factor structure [49]. Preliminary results from the scree plot showed two underlying factors from the 26 items. With a sample size of 204, a cut-off loading of 0.40 was used for item-scale selection [50]. Upon subsequent inspection of item loading, the two factors were labelled the 18-item Empowerment Scale (composed of nine MDES-SESE items and nine RS-PC items) and the six-item Resilience Scale (made up of six RS-PC items). Two items with loadings below the cut-off in both components were excluded from both factors. Skewness and kurtosis were inspected again with appropriate transformation applied to reduce deviation from normality. The two new scales showing satisfactory internal consistency (a = 0.77 and 0.92) were then entered into CCA with nine other RC variables. The descriptive statistics of the scales applied in multivariate analysis are presented in Table 1.
Stage I: canonical correlation analysis of recovery components and WHOQOL-BREF
Table 2 lists the correlation matrix of all variables used in CCA. Normality was confirmed in the distributions of all variables, except MOS-SSS-C (patient-peer support); thus, MOS-SSS-C was logarithmically transformed to reduce skewness.
Correlation matrix of predictor and criterion variables used in canonical correlation analysis (n = 201)
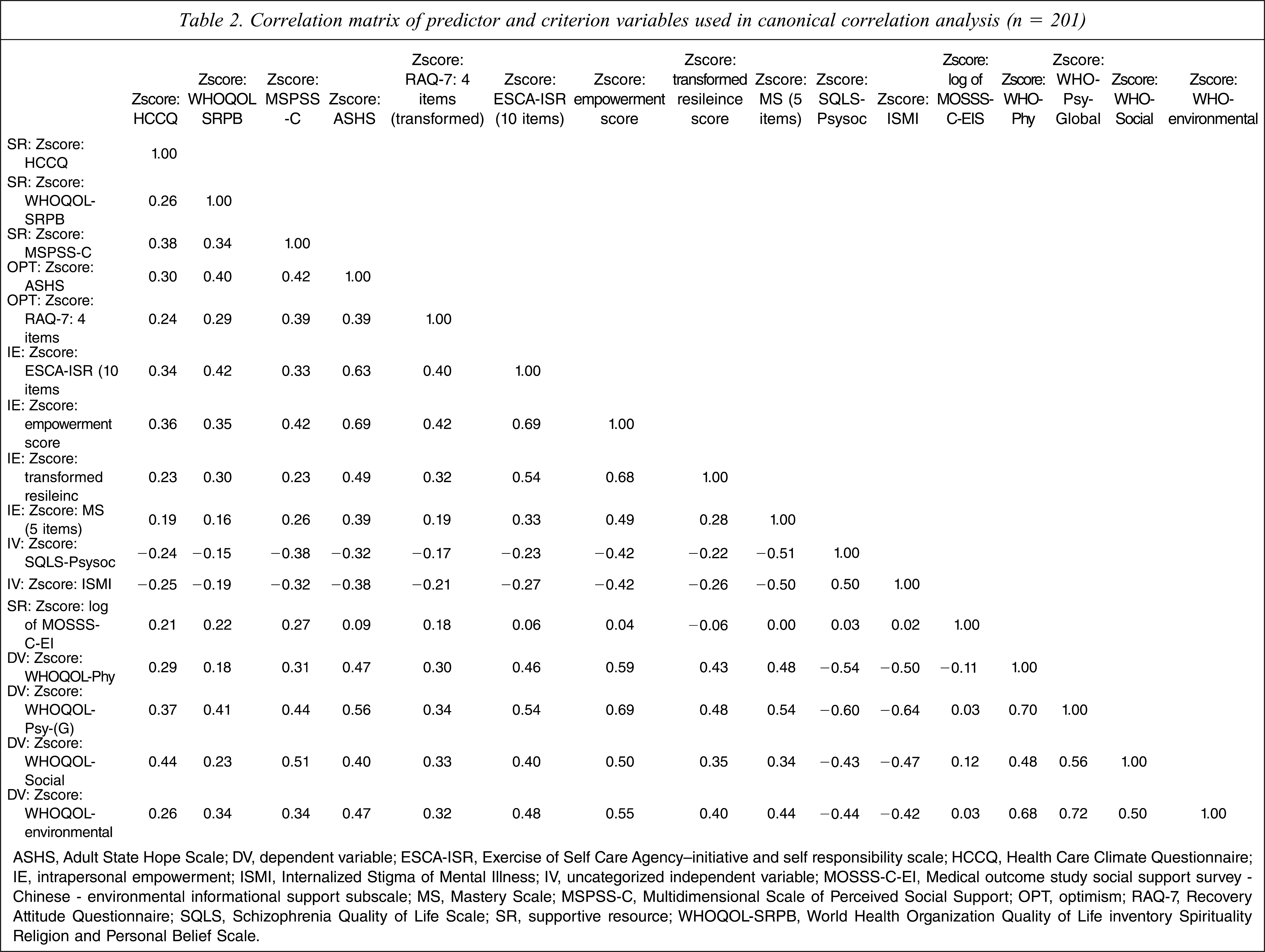
ASHS, Adult State Hope Scale; DV, dependent variable; ESCA-ISR, Exercise of Self Care Agency–initiative and self responsibility scale; HCCQ, Health Care Climate Questionnaire; IE, intrapersonal empowerment; ISMI, Internalized Stigma of Mental Illness; IV, uncategorized independent variable; MOSSS-C-EI, Medical outcome study social support survey - Chinese - environmental informational support subscale; MS, Mastery Scale; MSPSS-C, Multidimensional Scale of Perceived Social Support; OPT, optimism; RAQ-7, Recovery Attitude Questionnaire; SQLS, Schizophrenia Quality of Life Scale; SR, supportive resource; WHOQOL-SRPB, World Health Organization Quality of Life inventory Spirituality Religion and Personal Belief Scale.
CCA was performed using the 12 RC variables to predict WHOQOL domain scores. The analysis produced four functions with overlapping variance (squared canonical correlations, Rc 2) of 0.76, 0.15, 0.11, and 0.04 for each successive function. Collectively, the full model across all functions was statistically significant using Wilks’ λ = 0.18 criterion (F(48,714.68) = 8.37, p < 0.001).
The dimension reduction analysis tested the hierarchal arrangement of functions for statistical significance. The full model (including functions 1–4) was statistically significant (χ2(48) = 328.96, p < 0.001). With the first canonical correlation removed, functions 2–4 were also significant (χ2(33) = 59.90, p < 0.01). Function 3 and 4, however, did not explain a significant amount of shared variance between the variable sets (χ2(20) = 29.64, p = 0.08; χ2(9) = 7.55, p = 0.58). To conclude, only the first two functions accounted for the significant relationship between the predictor set and criterion set (Table 3).
Predicting quality of life from recovery components using canonical correlation analysis
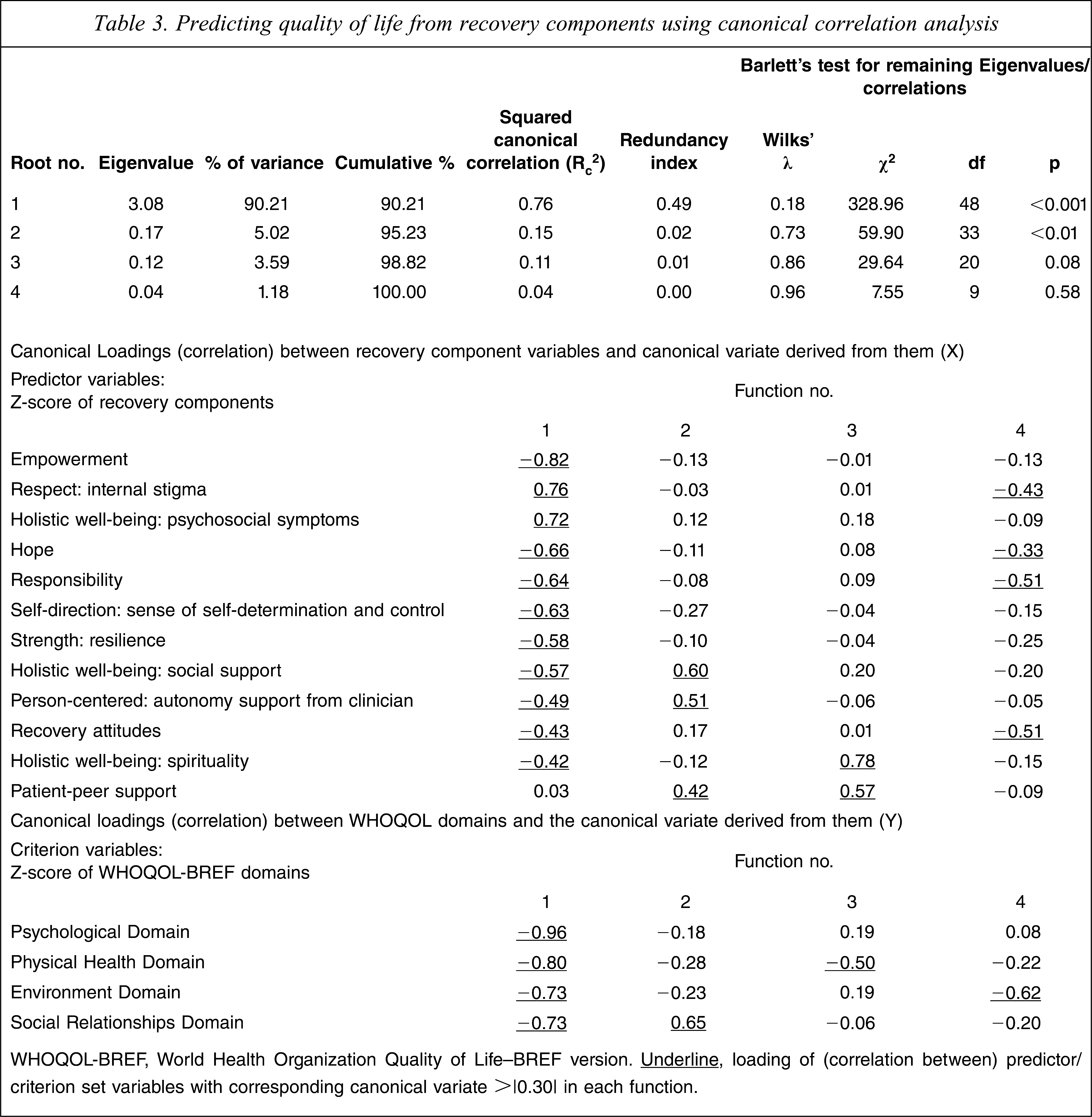
WHOQOL-BREF, World Health Organization Quality of Life–BREF version.
The percentage of variance in Table 3 showed that the first function explained 90.21% of the total variance extracted in all functions, while the second function explained only 5.02% of the total variance extracted. The redundancy index, which is analogous to R2 in multiple regression, offers a more realistic estimate of predictive ability in canonical relationships. Under the first canonical function, the redundancy index indicated that 49% of the variance in WHOQOL-BREF domains was accounted for by the variance in RC variable set. Under the second function, however, the redundancy index showed that only 2% of the variance in WHOQOL-BREF was explicable by the variance in the predictor set. Conclusively, only the first canonical solution was highly relevant in explaining the association between predictors and criterion. Interpretation of the second canonical solution was not supported.
First canonical solution
Using a cut-off of 0.30 for canonical loadings, RC variables correlating with the first canonical variate in the predictor side (variate X) were as follows: empowerment (R = −0.82), internal stigma (R = 0.76), psychosocial symptoms (R = 0.72), hope (R = −0.66), responsibility (R = −0.64), sense of self-determination and control (R = −0.63), (reflect and square root of) resilience (R = −0.58), social support (R = −0.57), autonomy support (R = −0.49), (reflect and log of) recovery attitude (R = −0.43), and spirituality (R = −0.42). (Logarithm of) patient-peer support was weakly correlated with the first canonical variate (R = 0.03) on the predictor side. Hence, the present results did not support the hypothesis that patient-peers are associated with the WHOQOL-BREF. All other predictors were associated with a canonical variate representing an overall deterioration in patient HRQOL (variate Y), signified by its negative correlations with physical health (R = −0.80), psychological health (R = −0.96), social relationships (R = −0.73), and environmental satisfaction (R= −0.73; Table 3).
Stage II: structural equation modelling of hypothesized models
A summary of model fitness for the three, hypothesized models is presented in Table 4. According to the results only model 3 (final model) attained adequate fit and explained the highest percentage of variance in WHOQOL-BREF (80.7%). Hence, it was selected as the best-fit model for final presentation. Detailed inspection showed that all parameters (path coefficients) in the final model were significant at the p < 0.001 level.
Summary of model fit with percentage of variance explained for recovery in different hypothesized models
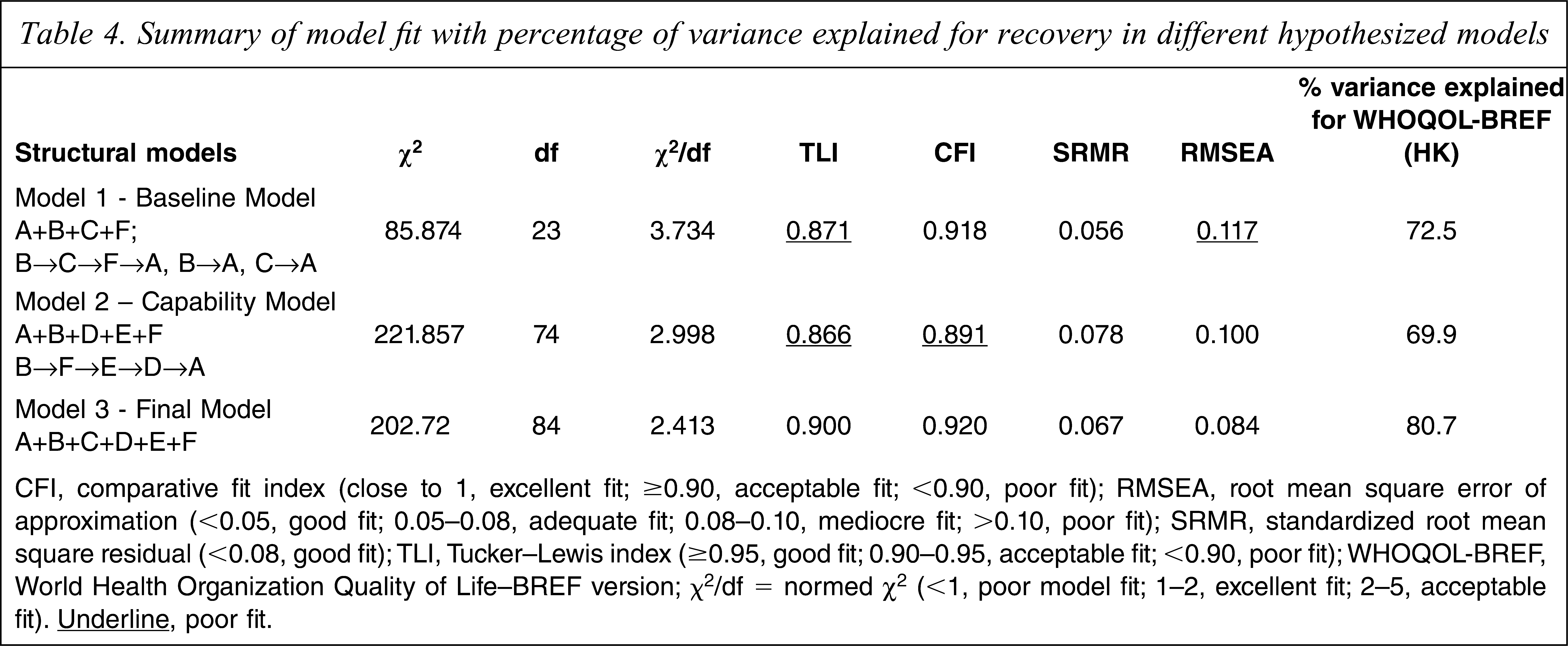
CFI, comparative fit index (close to 1, excellent fit; ≥0.90, acceptable fit; <0.90, poor fit); RMSEA, root mean square error of approximation (<0.05, good fit; 0.05–0.08, adequate fit; 0.08–0.10, mediocre fit; >0.10, poor fit); SRMR, standardized root mean square residual (<0.08, good fit); TLI, Tucker–Lewis index (≥0.95, good fit; 0.90–0.95, acceptable fit; <0.90, poor fit); WHOQOL-BREF, World Health Organization Quality of Life–BREF version; χ2/df = normed χ2 (<1, poor model fit; 1–2, excellent fit; 2–5, acceptable fit).
Recovery-oriented explanatory model for health-related quality of life
The indexes of model fit for the final model were good (χ2/df = 2.41, CFI= 0.92, TLI = 0.90, SRMS = 0.07, RMSEA = 0.84), indicating that the model provides a reasonable fit to the data. In addition to internal stigma and psychosocial symptoms, personal agency also had a significant direct effect on WHOQOL-BREF. The size of the direct effect that personal agency had on WHOQOL-BREF was larger (β = 0.58, p < 0.001) than that of internal stigma (β = −0.24, β < 0.001) and psychosocial symptoms (β = −0.29, p < 0.001; Figure 2). When considering the size of total effects (direct effect and indirect effect combined), however, psychosocial symptoms had an influence on WHOQOL-BREF (total β = −0.64) greater than that of personal agency (total β = 0.58). The total effect that optimism had on WHOQOL-BREF (total β = 0.54) was comparable to that of personal agency, while the size of the total effect for perceived support on WHOQOL-BREF (total β = 0.47) was slightly higher than that of internal stigma (total β = −0.42; Table 5).
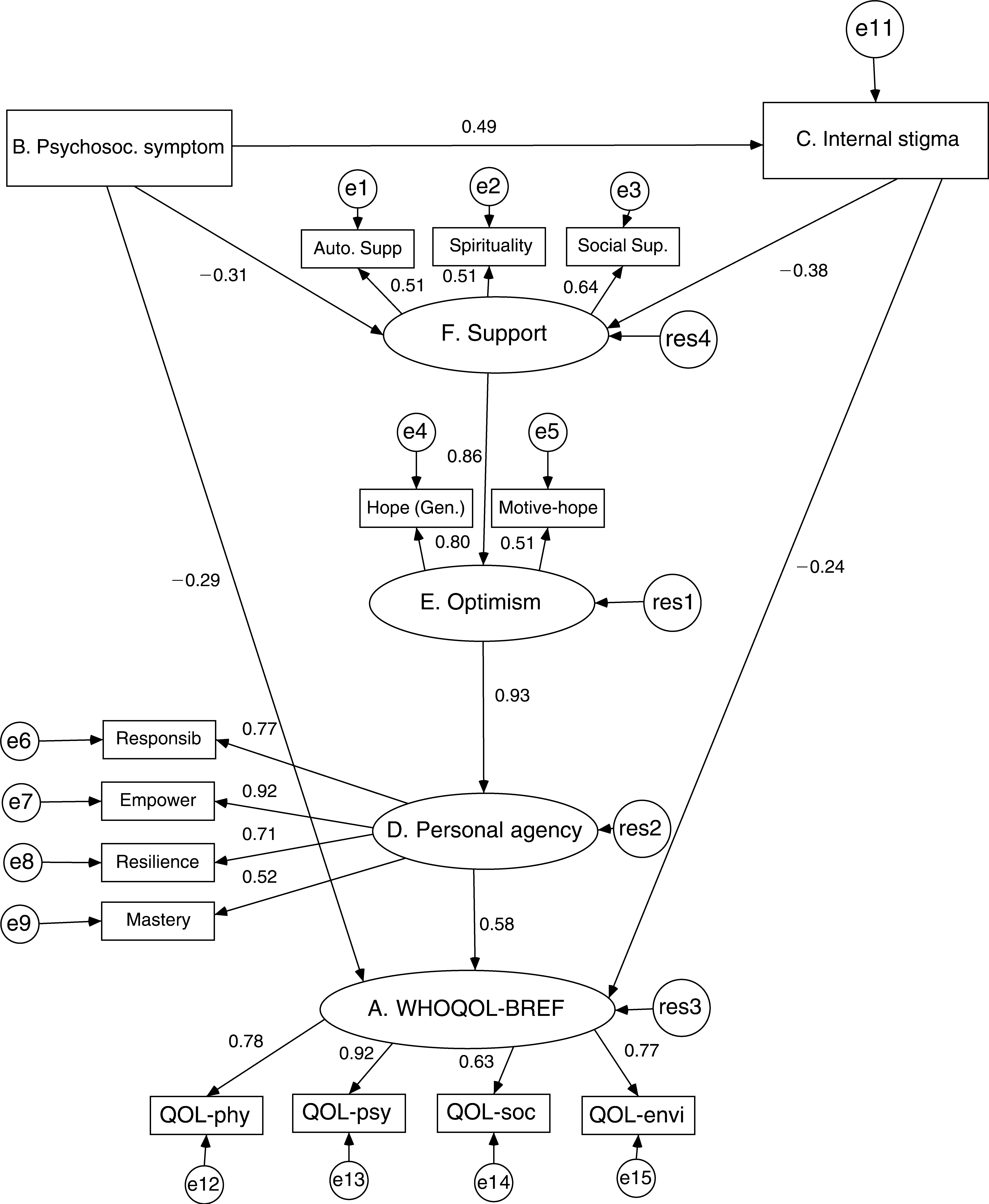
Final structural model with standardized parameter estimate. QOL, quality of life; WHOQOL-BREF, World Health Organization Quality of Life–BREF version.
Total, direct and indirect effects of independent variables on WHOQOL-BREF in the final model
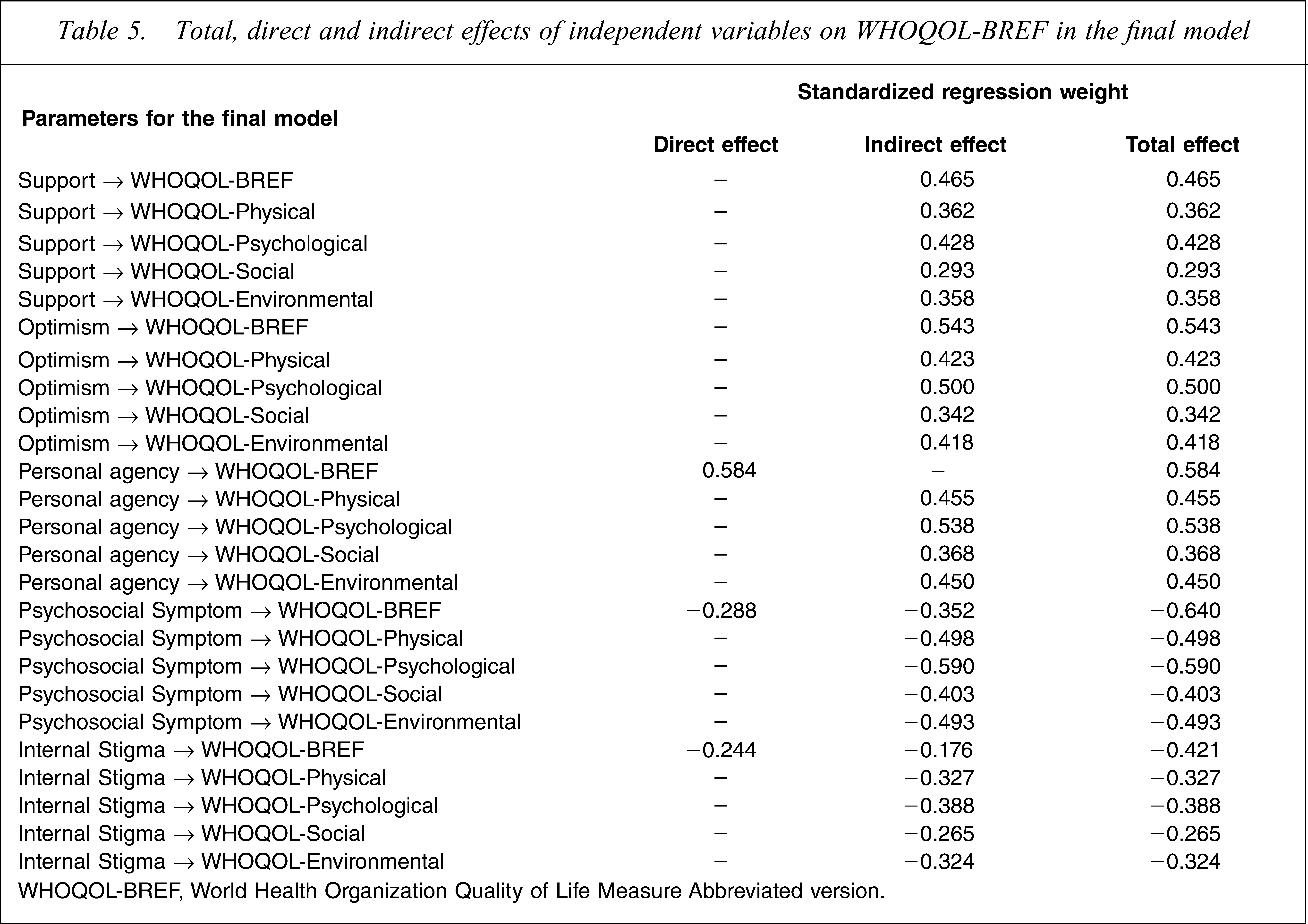
WHOQOL-BREF, World Health Organization Quality of Life Measure Abbreviated version.
Discussion
In the first stage of the analysis, the results supported the hypothesis that all recovery components from the SAM-HSA consensus statement – except patient-peer support – contribute to improvements of HRQOL. It proved that most recovery components proposed in the West were highly correlated with HRQOL perceived in Hong Kong Chinese patients. Nonetheless, the lack of association between patient-peer support and HRQOL deserves further explanation. Prevailing social stigma towards people with schizophrenia has caused subjects to conceal their identity in their daily interaction with strangers. Consequently, patients were also hindered from establishing supportive companionship among themselves unless they were already engaged in rehabilitation services. Because only one-third of the present sample had been engaged in any kind of services, the opportunity for the present subjects to build meaningful relationships with other patients is restricted. As noted, one-third of the present subjects employed in the open market were not service users themselves, but they enjoyed more opportunities for interaction with people from normal society. In comparison, interaction with patient-peers may be perceived as less attractive, unimportant, or even undesirable given their primary concern to shake off the mentally ill identity. Because of the interplay between these factors, the present results were confounded and did not support the original hypothesis.
The first model showed that psychosocial symptoms, internal stigma, and perceived support alone were able to explain more than 73% of the variance in WHOQOL-BREF. Although this simple psychosocial model sounds reasonable, it was rejected based on poor fit criteria. The second model, which explained WHOQOL-BREF based on psychosocial symptoms, perceived support, optimism, and personal agency, also failed to fit the empirical data well. The final model, based on nine SAMSHA recovery components, provided a better fit for empirical reality than the previous two models. The model offers new empirical evidence for the relationship between recovery components and HRQOL impairment in people suffering from schizophrenia. Second to psychosocial symptoms, personal agency plays a substantial role in improving HRQOL. Optimism, which was considered an essential ingredient in the recovery process, also played a significant role in improving patient HRQOL. This finding reinforces the growing evidence that personal agencies or perceived control play a crucial role in raising HRQOL [51–54]. Surprisingly, the model also showed that perceived support has a smaller effect on HRQOL, compared with personal agency. Thus, the suggestion that Chinese patients need more intensive social support rather than development of self-agency (such as mastery and autonomy) needs to be further scrutinized in future studies.
To conclude, the present findings confirm the role that personal agency plays in the HRQOL of Chinese patients with schizophrenia. In addition to that, the study draws attention to the potential benefits of hope-inspiring programmes and mastery-based intervention in improving the quality of life of community dwellers [18,55]. In concordance with other studies, the present results show that Chinese patients’ HRQOL is also significantly determined by personal factors, such as resilience, autonomy, perceived personal control, and stigma [7,9,10,54,56,57]. Therefore, a holistic intervention should aim at upgrading psychological quality in addition to improving psychosocial functioning. Finally, by providing a preliminary empirical validation of the nine recovery components proposed by SAMHSA, the final model can be used as the foundation for further development of a recovery-measuring instrument in Chinese patient communities.
Limitations
The present sample of 204 subjects was modest in size but large enough for testing a structural regression model with 11 observable predictors The WHOQOL-BREF profile of subjects in the present study was similar to that of other local outpatient studies, which supported the generalizability of the findings [21]. Pre-interview screening was carried out to ensure that subjects possessed the necessary cognitive ability to answer QOL questions: those who were chronically ill were excluded. Hence, statistical inferences cannot be comfortably drawn in respect to those at the lowest end of the recovery spectrum, especially those who are under long-term hospitalization.
Drafted as a statement of principles, recovery and its components have been defined with broad meanings under the SAMHSA national consensus statement. For example, holistic recovery was defined as a construct that encompasses all aspects of life, including housing, employment, education and so on. Strength-based intervention was defined as an intervention that enhanced resilience, coping capacities, personal potential, and self-worth [17]. These all-embracing concepts make delineation impossible by methods other than deploying a large number of indicators. Constrained by the small sample size, we only operationalized the recovery components in a sense possibly narrower than originally proposed. Other limitations included the use of sub-scales that have been taken out of parent instruments to measure recovery components, and the exclusion of items with low item-total correlation to the instrument. Although some of the modified instruments had not been validated among Chinese people with schizophrenia, the use of CFA in pre-analysis ensured the unidimensionality and reliability of each instrument. Nonetheless, readers should note that the instrument for measuring non-linear recovery values may not be completely valid in the present Chinese sample, hence the association between this recovery component and WHOQOL-BREF should be interpreted with caution.
Footnotes
Acknowledgements
This paper is based on the doctoral work of the first author.
