Abstract
The relationship between violence and psychosis remains a subject of considerable debate [1]. Although serious violence by patients with established psychotic illness is relatively uncommon [2], recently published studies reported that the first episode of psychosis (FEP) may be a period of greatly increased risk for lethal violence [3–5]. Studies that have examined rates of aggression in FEP have found that between 12% and 39% of FEP patients commit an act of aggression by the time of first presentation [6–15]. Methodological issues, however, have created considerable confusion in this area.
The importance of considering less serious and more serious forms of aggression by patients in separate categories was noted by the Macarthur Violence Risk Assessment Study [2] and has been recognized in several studies in FEP [8–11]. Serious aggression, defined as any physical assault causing an injury, assault with a weapon or any sexual assault, may have different associations than less serious aggression. For example, Milton et al. found that serious aggression was associated with treatment delay whereas less serious aggression was not [9], and both Steinert et al. and Milton et al. reported a larger number of incidents of less serious aggression after treatment compared to incidents of more serious aggression, which remained stable or declined in the post-treatment period [8, 9]. Furthermore, even the forms of aggression described as serious in studies of FEP would not necessarily result in serious criminal charges and rarely resulted in serious injuries. Steinert et al. reported that only one of 138 FEP patients inflicted severe injuries in a single assault, although 22 inflicted minor injuries [8].
The measurement of violence and aggression is complex. The definition of violence may limit the population studied. Some studies have excluded verbal aggression, restricting the definition to acts of physical aggression despite the distress that verbal aggression can cause [6,7,11,12]. In contrast, very serious violence (serious assault or murder) is frequently diverted into the criminal justice system and not observed in surveys that are restricted to the mental health system [4]. Prevalence rates of aggression have been estimated, over very different periods of time, to vary from as little as 2 weeks [11] to lifelong [10]. Cross-sectional research or studies limited to a brief period run the risk of not observing rare acts of serious violence [11], whereas research that uses a lifelong history of aggression [10] may not be able to examine the relationship of psychosis and aggression because all past episodes of aggression are conflated prior to the onset of psychosis.
The method of obtaining data about aggression affects the quality of the information. Self-report obviously requires the disclosure of behaviours that are not only socially undesirable, but may have both legal and medico-legal consequences, with detention in the forensic or psychiatric system being at issue. But it can detect violence that may otherwise go unreported because informant sources are unaware of the acts. Surveys that depend upon relatives’ report need to fully survey the range of possible aggression to include both the less serious acts of aggression highlighted by Steadman et al. [2], as well as the more severe acts of aggression that may trigger referral to mental health services or hospitalizations. Research dependent upon aggression reported in medical records [8] or criminal records [16] risks an underreporting of aggression. This is not limited to less serious aggression. In one study of people convicted of homicide in the United Kingdom, 22 of 42 previous convictions for violence were not recorded in the medical records of mentally ill offenders [17].
The method of ascertaining the relevant population is also important. Population-based surveys are unable to examine less serious aggression because they are dependent upon databases recording significant violence such as criminal record registers [16]. Epidemiological surveys are limited in the detail that they can enquire about regarding violence [7,12,14]. For example surveys using the Psychiatric and Personal History Schedule (PPHS) [18] include a single question regarding physical assault, but this is the basis for the investigation of the relationship of aggression to mental illness. Community-based studies using multiple sources of information are thought to have a greater likelihood of accurately determining both the rates of aggression in the population and the determinants of that behaviour [2]. The restriction of studies to a specific diagnosis such as schizophrenia [6–8] also limits the generalizability of results to FEP. This is despite the instability of diagnosis at this time [19].
Past studies that have reported rates of aggression in FEP and examined the clinical associations have identified associations with substance abuse [7–9,11,12], the positive symptoms of psychosis [6,7,10], manic symptoms [12], male gender [8,9,12], forensic history [7,9,12] and young age [7,9,12]. Three studies identified a possible association between violence and treatment delay [6, 9, 10], although two other studies did not find this association [12, 20]. None of the studies, however, examined the association between neuropsychological variables and aggression, despite the likelihood of a relationship between cognitive deficits and aggression. Most studies have reported the association between an omnibus measure of substance abuse but few have reported the association between the abuse of specific substances and aggressive behaviour during FEP.
In the present study we re-examined the factors that have been found to be associated with violence in other studies of aggression in FEP. These include young age, male gender, psychotic and manic symptoms, diagnosis, a history of criminal convictions and substance abuse. We were particularly interested in a possible association between prolonged duration of undiagnosed psychosis (DUP) and aggressive behaviour, and the role of the abuse of alcohol, cannabis and stimulant drugs on both serious and less serious forms of self- and informant-reported aggression. We also examined the relationship between aspects of cognitive function and aggression, with the a priori hypothesis that there would be an association between impairment in executive function and aggression.
Method
Sample and measures
Consecutive patients (n = 224) presenting to all public health services with FEP in the defined catchment of Western Sydney (estimated to be 950 000 people) during a 2 year period were asked to participate in a multi-modal investigation of FEP [21, 22]. Because of the nature of the catchment, the paucity of private sector services and the development of local early intervention services this is likely to be highly representative of the total number of young people who became psychotic in this catchment area over this period.
All subjects were aged between 13 and 25 years at the time of recruitment. Of the 120 who did not take part, 48 refused to give consent, 11 refused all services, 16 could not be traced, eight moved out of area, seven were working full time and refused to come in for the project and 30 did not meet inclusion criteria, leaving 104 subjects. Those who declined to take part were older (χ2 = 6.703, df=1, p = 0.01) but did not differ on gender. A further 10 subjects were withdrawn from the study due to clinical concerns.
Clinical assessments included the Positive and Negative Syndrome Scale (PANSS) [23], the Young Mania Rating Scale (YMRS) [24], the Calgary Depression Scale [25] and purpose-designed instruments for recording substance abuse and aggression.
Aggression was assessed in an interview with both the patient and their relatives using a purpose-designed semi-structured scale: the Aggressive Behaviour Questionnaire (ABQ) [26]. The questionnaire was administered as part of the clinical interview performed by study psychiatrists (AH, JB, JA). Both subject and relative/carer were interviewed and the rating scored on the basis of the more severe behaviour described by either subject or relative/carer. This scale rates the frequency of 10 aggressive behaviours including shouting, verbal threats, physical aggression to a person, use of a weapon, inappropriate sexual behaviour, sexual assault, damage to property, fire setting, harm to animals and self-harm in the 3 months prior to recruitment and at any time in the past.
All subjects were assessed using a comprehensive battery of age-appropriate neuropsychological tests. The test battery was devised with reference to other studies in this group [27, 28], and to cover the domains of neurocognitive deficit observed in first-episode schizophrenia [29]. The tests included a full-scale IQ (FSIQ; the Wechsler Adult Intelligence Scale 3rd edition or the Wechsler Intelligence Scale for Children 3rd Edition), the Wisconsin Card-Sorting Task (WCST; categories and perseverative errors), Connor's Continuous Performance Task (CPT), the Rey Auditory Verbal Learning Test, the Wechsler Memory Scale or Children's Memory Scale, the Controlled Oral Word Association Test, the Trail-Making Tests and the Wide Range Achievement Test third edition (WRAT3) [30]. All tests were administered by masters level or higher psychologists and neuropsychologists and were conducted in the same order for all subjects.
The subject interviews were all conducted in the same order, with subject consent and clinical interview preceding neuropsychological assessment. The neuropsychological assessment was generally conducted within 1–2 days of the clinical interview. The maximum time elapsed between interview and neuropsychological assessment was 14 days.
Approval to conduct the study was obtained from Sydney West Area Health Service Human Research Ethics Committee and the University of Sydney Human Research Ethics Committee.
Psychometric properties of the ABQ
The internal reliability of the ABQ was examined using Cronbach's alpha. A two-step cluster analysis of the ratings of 10 aggressive behaviours was performed. Log likelihood was used as the distance measure using auto-clustering to minimize the ratio of distance measures. This cluster analysis formed the basis of further analysis of the cohort.
Univariate statistics
Univariate continuous variables were compared with a Student's t-test. Categorical variables were examined using a Pearson χ2 if there were more than five subjects in all cells or a Fisher's exact test if there were fewer than five subjects in any cell. The DUP was transformed using Ln(DUP+1 month) because the distribution of DUP was severely right skewed [31]. All the measures of cognitive function were Z score transformed [22] and the CPT and WCST error scores were inverted such that a higher score indicated better performance for all tasks.
Multivariate statistics
Manual step-forwards entry of variables that are known to be associated with aggression was performed. The results of this were confirmed using automated step-backward and automated step-forwards multiple logistic regression analysis with the same findings in each three analyses. A receiver operating curve (ROC) was calculated using the variables that were found to have an independent association with serious aggression. All analyses were performed using SPSS for Windows version 15.0 (SPSS, Chicago, IL, USA).
Results
The study has been described in detail elsewhere [21]. The subjects were young (mean age=18.5±3.2 years) and predominantly male (65.1%). The patients had an average 10.7 years of schooling (±2.0 years). The majority (70.3%) were admitted to hospital for treatment of psychotic illness, while the remaining patients were treated in the community. Subjects were diagnosed with the following disorders: the schizophrenia group, consisting of schizophrenia (44.7%), schizophreniform (10.6%), and schizoaffective (1.2%); the affective group, made up of bipolar disorder (15.4%) and major depression with psychotic features (4.7%); and the other psychoses, including substance-induced psychotic disorder (12.9%), psychosis not otherwise specified (5.9%), and brief psychotic disorder (4.7%).
The ABQ was completed in 85 of 94 subjects; nine subjects without ABQ ratings were excluded from the analysis. There were six missing data cells with respect to five subjects (four subjects failed to complete all the cognitive tests and one subject had a missing MRS score). Missing values for these subjects were replaced with the mean of that variable.
The internal reliability of the ABQ was good (Cronbach's α = 0.728). Cluster analysis identified two distinct clusters after 13 iterations. The first cluster, termed ‘no aggressive behaviour’ (NAB), contained the majority of subjects (n = 48), some of whom were recorded as shouting and exhibiting evidence of self-harm (items 1,10) but not other aggressive behaviours (Table 1). The second cluster, ‘any aggressive behaviour’ (AAB), contained the 37 patients, or 43.5% of the sample, who exhibited any other form of threatening and aggressive behaviour (items 2–9) in the 3 months before presentation (Table 2).
Aggressive behaviour† in 85 first-episode psychosis patients
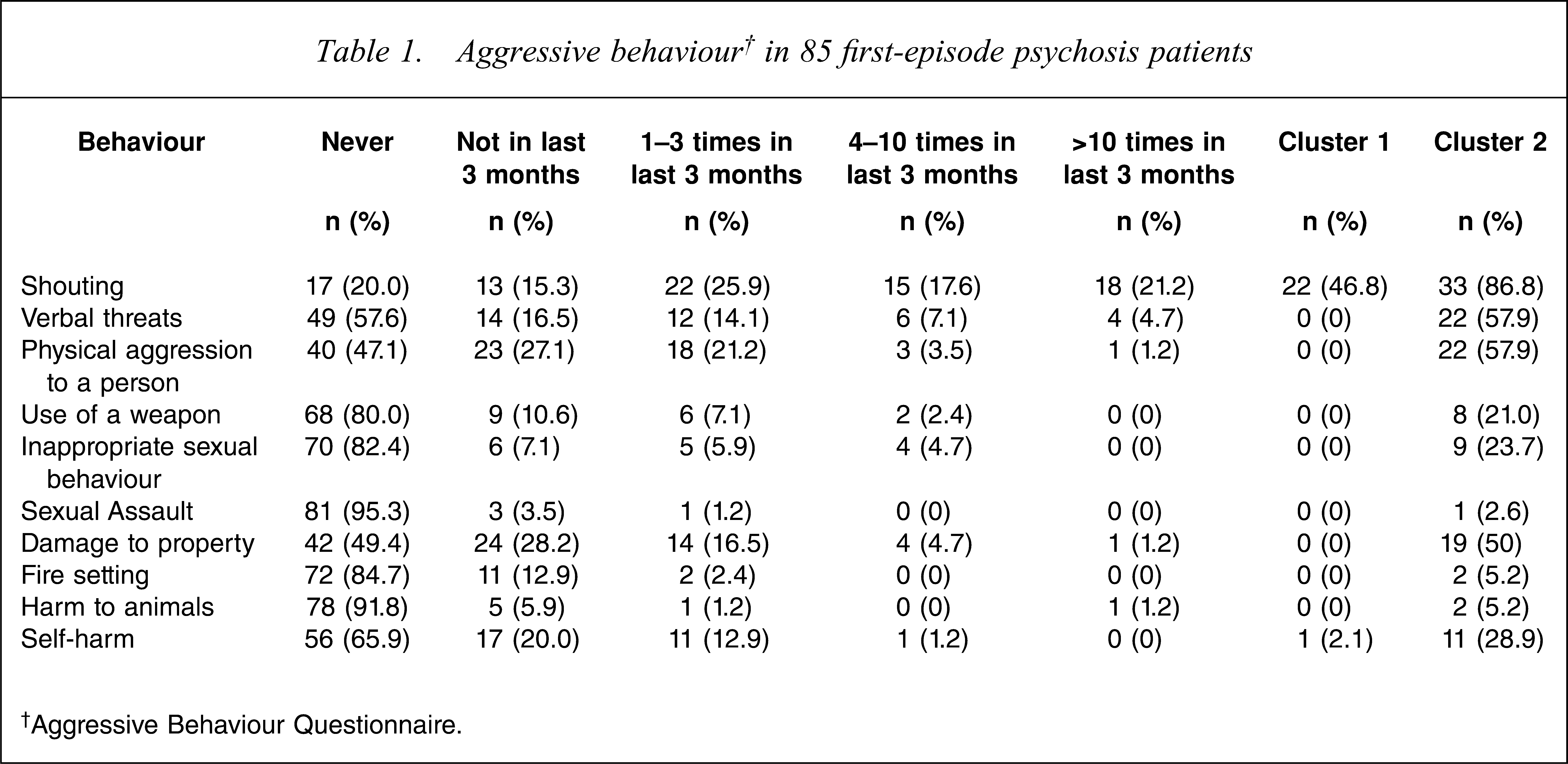
†Aggressive Behaviour Questionnaire.
Characteristics of group displaying any aggression in the last 3 months
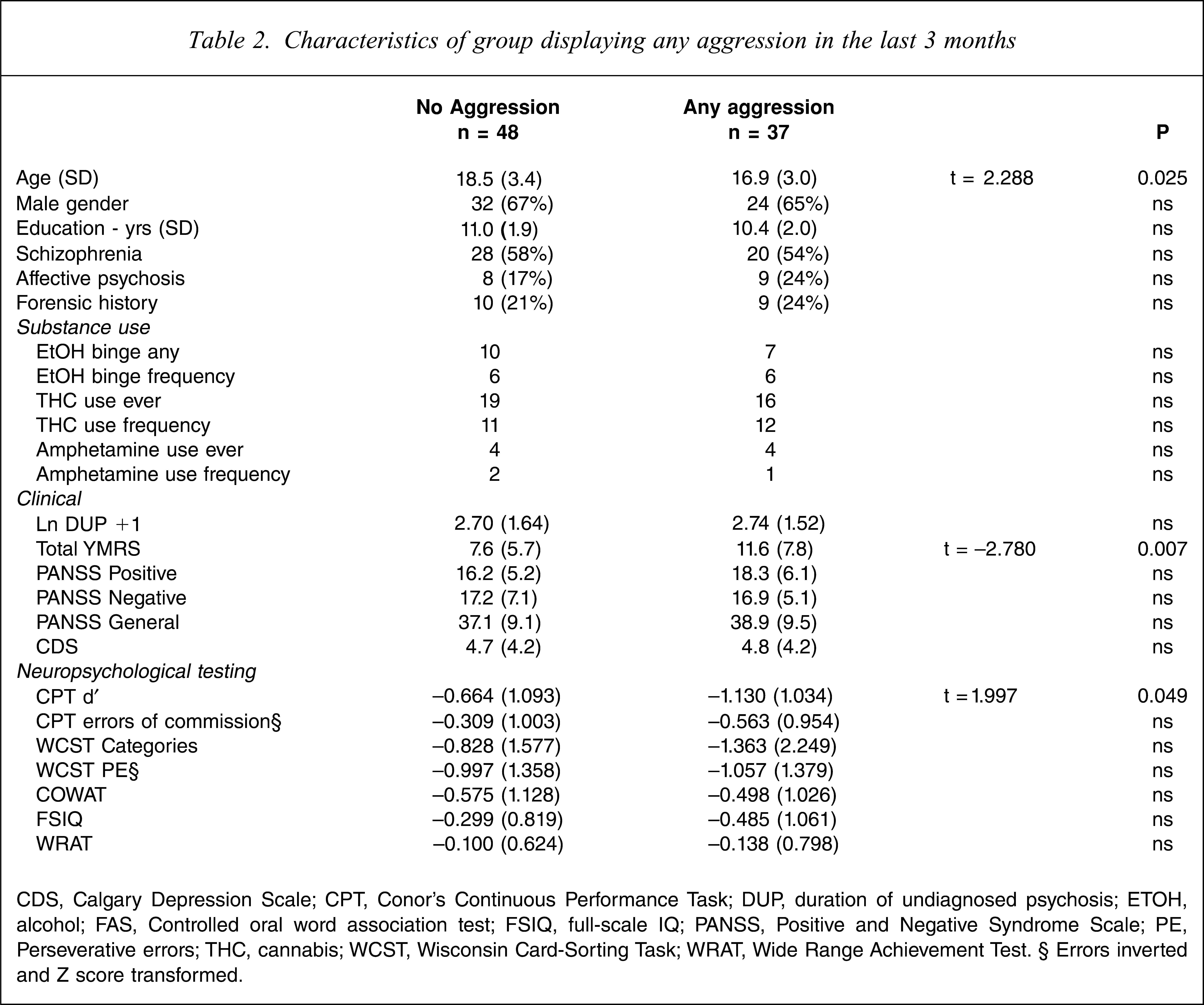
CDS, Calgary Depression Scale; CPT, Conor's Continuous Performance Task; DUP, duration of undiagnosed psychosis; ETOH, alcohol; FAS, Controlled oral word association test; FSIQ, full-scale IQ; PANSS, Positive and Negative Syndrome Scale; PE, Perseverative errors; THC, cannabis; WCST, Wisconsin Card-Sorting Task; WRAT, Wide Range Achievement Test. § Errors inverted and Z score transformed.
A second analysis was based on the comparison of 23 subjects, or 27% of the sample, who exhibited serious aggressive behaviour (SAB), with the remaining 62 subjects, who were grouped in a ‘non-serious aggressive behaviour’ (N-SAB) category (Table 2). Serious aggression was defined, on an a priori basis using the definitions in the Macarthur Violence Risk Assessment Study [2], as actual physical aggression against another person (item 3), used a weapon (item 4) or had committed a sexual assault (item 6). In the present study 23 of 85 (27.5%) FEP patients were reported to have had at least one incident of SAB in the 3 months before presentation. AAB was reported in (43.5%) of patients (Table 3).
Serious aggression in the last 3 months-all 85 subjects
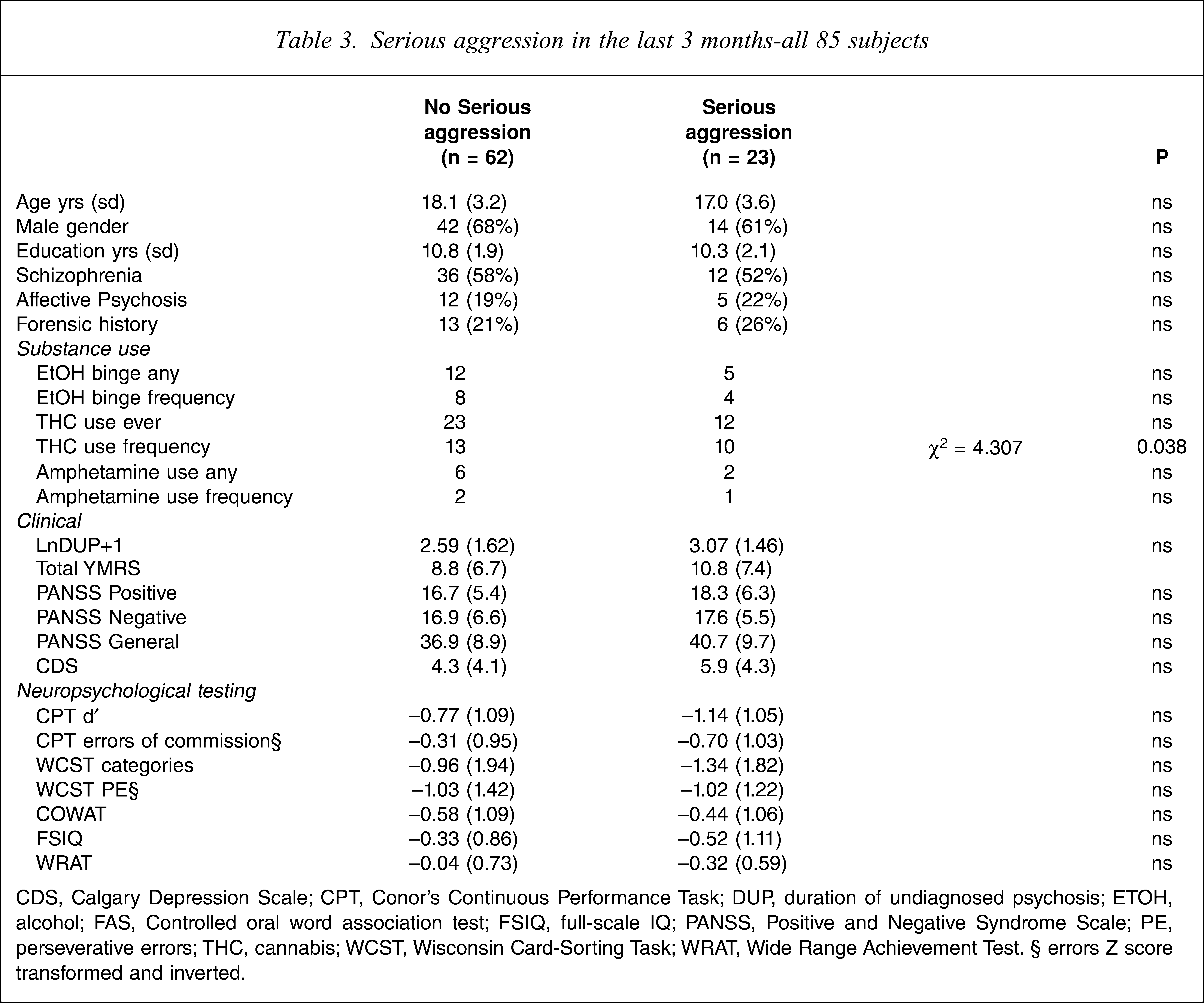
CDS, Calgary Depression Scale; CPT, Conor's Continuous Performance Task; DUP, duration of undiagnosed psychosis; ETOH, alcohol; FAS, Controlled oral word association test; FSIQ, full-scale IQ; PANSS, Positive and Negative Syndrome Scale; PE, perseverative errors; THC, cannabis; WCST, Wisconsin Card-Sorting Task; WRAT, Wide Range Achievement Test. § errors Z score transformed and inverted.
Univariate statistics suggested that younger patients and those with elevated scores in the total mania scale were more likely to be in the AAB group. Logistic regression found that the total mania score and the age were both independent predictors of aggressive behaviour (Table 4).
Any aggression, multiple logistic regression, backward step†

WCST, Wisconsin Card-Sorting Test. †Included after 23 steps, χ2 = 14.91, df = 3, p = 0.002. ‡Confirmed in step forward model.
The use of cannabis with a frequency of more than fourfold in the previous month was the only factor that was found to be associated with serious aggression (Table 2). Using multiple logistic regression a higher rate of errors of commission on the CPT was independently associated with serious aggression (Table 5). This association was not apparent in the univariate measures because of the surprising finding that patients who smoked marijuana regularly had a lower overall rate of errors of commission on the CPT. This was thought to be an incidental finding because cannabis smokers were also older and had higher FSIQ and WRAT scores.
Serious aggression, multiple logistic regression, backward step†
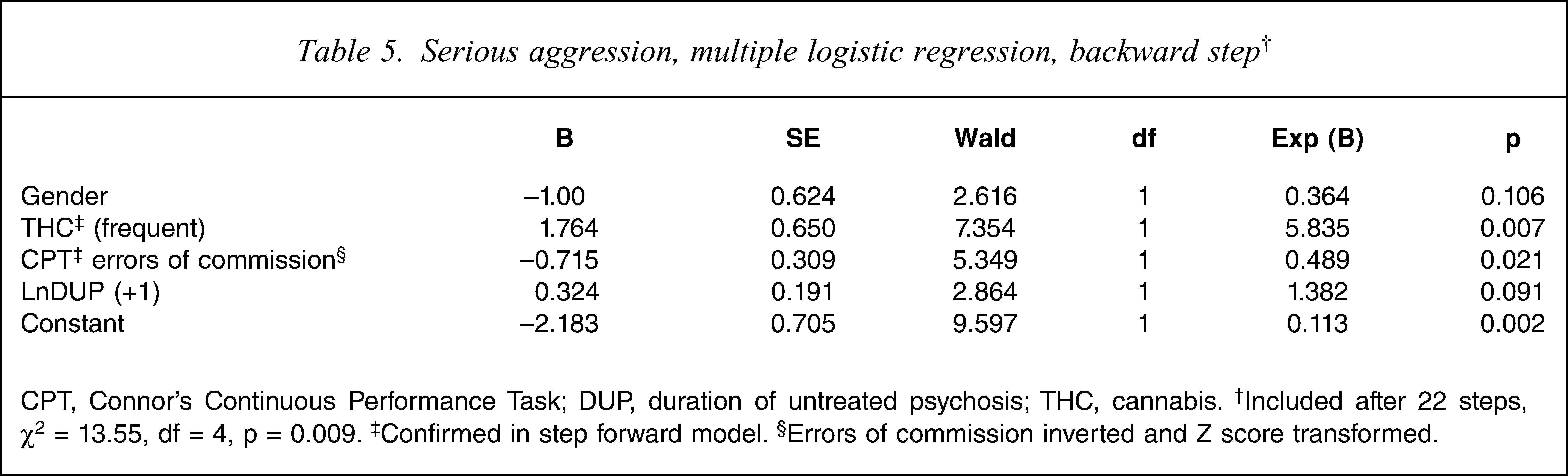
CPT, Connor's Continuous Performance Task; DUP, duration of untreated psychosis; THC, cannabis. †Included after 22 steps, χ2 = 13.55, df = 4, p = 0.009. ‡Confirmed in step forward model. §Errors of commission inverted and Z score transformed.
An ROC (Figure 1) was calculated using regular cannabis use, CPT errors of commission, gender and Ln(DUP+1) as predictor variables for serious aggression. DUP and gender were included because they trended towards significance in the regression analysis. The area under the ROC was 0.745 (SE = 0.066, asymptotic significance = 0.001, asymptotic 95% confidence interval = 0.615–0.875).
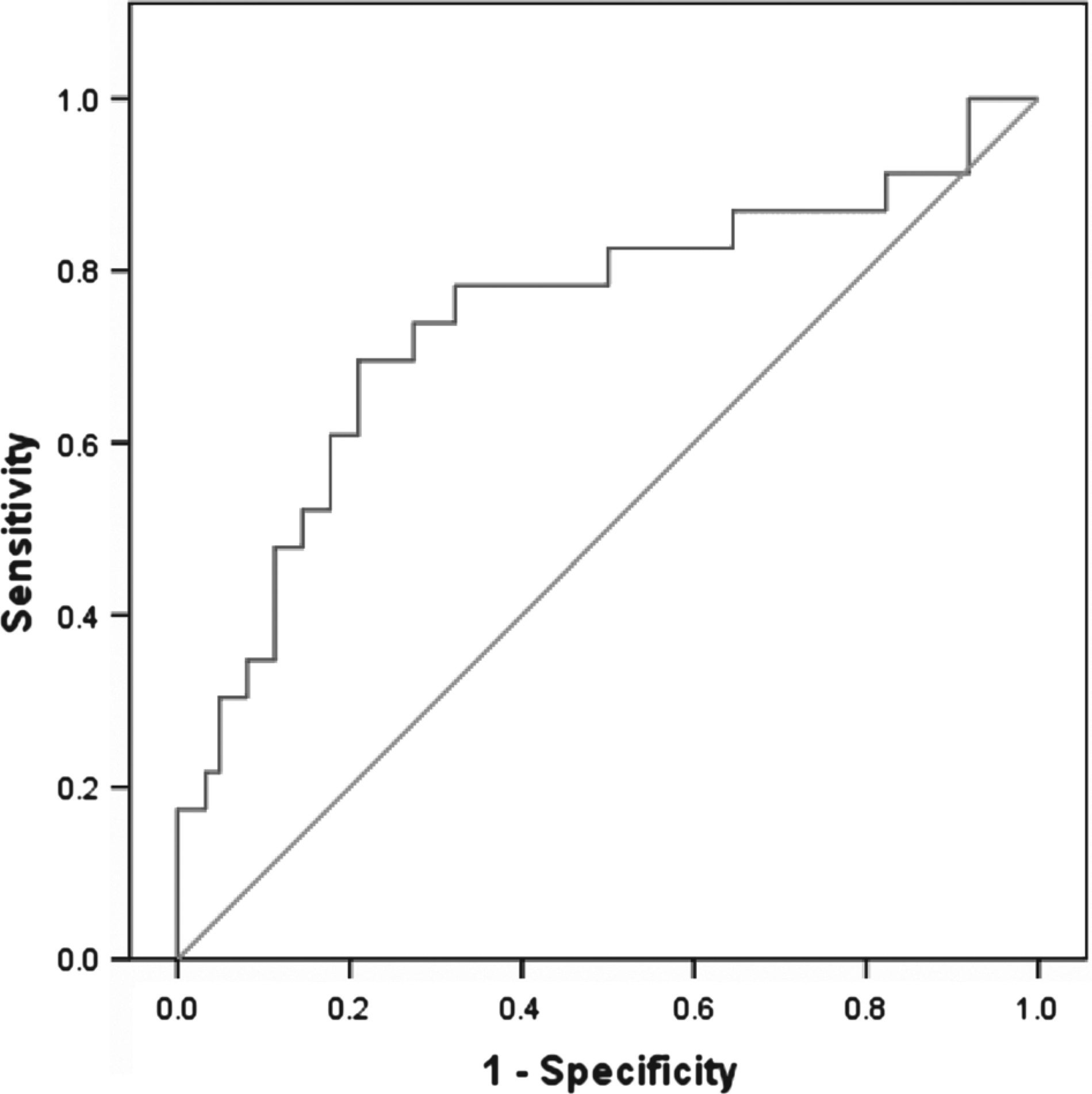
Receiver operating curve calculated using regular cannabis use, Connor's Continuous Performance Task errors of commission, gender and Ln(DUP+1) as predictor variables for serious aggression. DUP, duration of undiagnosed psychosis.
Discussion
The present study is a reminder of the high level of aggressive behaviour of FEP patients prior to treatment. The proportion of patients reported to have aggressive behaviour (43.5%) was higher than had been reported in other studies, possibly because the patients were younger or they were asked about a wider range of aggressive behaviours and a corroborative interview was used. Interviews with relatives in general may identify more aggressive incidents than interviews with the patients themselves [32].
The range of methods to establish a history of aggression would be expected to produce different results. Even studies using responses recorded on the PPHS [18], which was developed as part of the Determinants of Outcome of Severe Mental Disorder (DOSMeD) study [7,9,12,14], appear to differ in the specific questions used to determine if a subject had been aggressive or violent. We could not discern, however, underreporting or over-reporting of aggression from the various methods.
Although the rate of events classified as serious violence was high, there were no instances of violence that resulted in serious physical injury or may have led to a serious criminal charge. The absence of any episodes of very serious violence in FEP series has been noted elsewhere, and in the present series may be due to the relatively small sample size and the low base rate of very serious violence in general. A more concerning explanation is that most FEP patients are taken into secure custody after episodes of very serious violence and are hence excluded from this kind of study. In a study of homicide during psychosis illness, over a 15 year period that included the 2½ years in which these patients were recruited, there were seven FEP patients from the western Sydney area that committed homicide [4]. There were at least as many serious non-lethal assaults by FEP patients who were remanded directly to custody (Nielssen O: unpublished data, 2008). However, in our study, no association was seen between a forensic history and aggression.
The present study confirmed previously observed associations between aggression and age, manic behaviour, and cannabis abuse. Male gender and prolonged DUP, which were significantly associated with aggression in other studies, only trended towards significance in the present cohort. We found no association between positive symptoms, lower educational attainment and lack of insight and aggression. The association between ratings on the YMRS and aggression did not persist when examined again with the SAB group. Nor was there an association between diagnostic group and aggression. Because we used the PANSS as the major measure of psychopathology we were not able to comment on the relationship between the content of delusional beliefs and aggressive behaviour. We also found no association between alcohol use and aggression, although an association had been reported in studies from Britain or Ireland, which have similar patterns of alcohol use to Australia [9, 11, 12]. The lack of correlation between amphetamine use and violence may reflect the low rate of the use of amphetamine and other stimulant drugs in this relatively young group of patients. It is likely that the young age of the sample also contributed to the lack of an association between a forensic history and aggression.
An important finding of the present study was the association between low levels of regular cannabis use and more serious violence. Although there is substantial evidence for causal associations between cannabis use and psychosis [33] and psychosis and violence [34], there are few studies that specifically examine the association between cannabis use and violence. The conventional wisdom is that cannabis has a calming effect and makes violence less likely [35], a belief that is also held by many patients who continue to use cannabis against medical advice. But cannabis use has been shown to be an independent predictor of violence at a community level [36]; also, patients with chronic schizophrenia who use cannabis are more likely to be violent [37, 38].
It is not clear that cannabis use itself is a direct cause of violence, or whether people who use cannabis are violent as a result of a third factor such as a personality type, or if cannabis dependence is an indirect cause of violence as a result of criminal association or crime to obtain money for the drug. A proposed mechanism by which cannabis use increased the likelihood of aggressive behaviour is its effect on the go/no go functions of the brain, which are usually attributed to the anterior cingulate and lateral pre-frontal cortex [39] and play a role in inhibiting behaviour. These are impaired in people who abuse cannabis [40]. The more aggressive patients were more likely to use cannabis and made more errors of commission on the CPT, which has been conceptualized as a test of impulse control. Hence the results of the present study are consistent with the hypothesis that cannabis use increases the risk of violence by reducing inhibition.
The finding that regular cannabis use and errors of commission on CPT were associated with serious aggression should alert clinicians to the risk posed by these patients. When combined with male gender and longer DUP it was able to predict incidents of serious violence, with an area under the ROC that is greater than that of the actuarial instrument derived from a large study of patients who had previously received treatment [41].
Personality could be another important factor influencing aggression, but this was not formally assessed in the diagnostic workup in the present study. The definitive diagnosis of personality disorder in a young population of psychotic individuals is problematic due to conceptual, diagnostic and definitional difficulties. In assessing personality in a cohort with an average age of 18.5 years one needs to distinguish between the developmental deviance often seen in schizophrenia and personality disorders [42–44], the shared genetic predisposition within the schizotypal spectrum of disorders [45] and the shared effects of life stressors such as childhood trauma [46]. Nevertheless, an increase in antisocial behaviour is seen in young people who go on to develop schizophrenia [47]. Although the presence of a forensic history of any sort did not distinguish between groups, a small proportion of the present subjects (classified in the SAB group) had exhibited actions prior to the past 3 months such as sexual assault (3.5%) or harm to animals (5.9%) that would suggest that they had a premorbid antisocial personality disorder. Further work would be assisted by examining specifically for antisocial personality and more generally for a diagnosis of personality disorder despite the difficulties outlined.
The present study was limited by its relatively small sample size, its dependence upon a community sample that may have excluded subjects already detained in the forensic system and its lack of a non-psychiatric control group. The sample was, however, drawn from the broad community of Western Sydney; was not limited to those admitted to hospital; and included a broad range of psychotic disorders. The ABQ, although a new instrument, appears to be psychometrically sound and is specifically designed to measure a wide range of serious and less serious aggressive behaviour on the basis of both self and informant report. As such it is a considerable advance upon instruments, such as the PPHS [18], used in other studies. Further testing of the ABQ, however, including comparison with other established instruments, is required in other populations of people with psychosis to further define its role in measuring aggression and to fully confirm its reliability and validity.
The main clinical and public health messages from the present study are to emphasize the level of aggression seen in young people with their first diagnosis of psychosis, remind the clinician of the significance of poor impulse control in this population and to underline the danger that even moderate cannabis use poses to families of early psychosis patients and to mental health workers. In turn this suggests the need to pay special attention to the assessment of aggression at this stage of the illness; emphasizes the usefulness of neuropsychological assessment of young people with psychosis; and underlines the importance of addressing impulse control problems and cannabis abuse in our management of these young people.
Footnotes
Acknowledgements
We would like to thank Dr Karen Byth for her assistance with the analysis; Dr Mark Kneebone and Dr Sandy Bremner for their help in originally developing the ABQ; and Sara Lucas and Diane Fitzgerald for data collection and entry.
