Abstract
Objective:
To compare the symptoms and function of patients with psychosis who have ceased using substances to those who have psychosis but do not have a history of substance use.
Method:
The databases EMBASE, MEDLINE and PsycINFO were searched for peer-reviewed publications in English reporting the characteristics of patients with psychotic illness who had stopped using substances and those who had never used substances. The searches yielded 20 articles that met the inclusion criteria. Four key outcome variables – positive symptoms, negative symptoms, depression and global function – and four other outcome measures reported in five or more studies were examined using meta-analysis.
Results:
Former substance-using patients were significantly younger than non-substance-using patients and were more likely to be male, but did not differ in age at onset of psychosis or in their level of education. There were no significant differences between former substance users and non-substance users in ratings of positive symptoms, negative symptoms, depression or global function. Among first-episode patients there was a trend towards former substance users having less severe depressive symptoms than non-substance users. In contrast, among non-first-episode patients, former substance users had significantly more depressive symptoms than non-substance users. In studies rated as being of higher quality, former substance users had significantly less severe positive symptoms than non-substance users.
Conclusion:
The absence of significant differences between the two groups suggests that a history of substance use is not a poor prognostic indicator for patients who are able to stop using substances.
Introduction
The association between psychosis and substance use has been extensively studied. High rates of substance use, in particular the use of cannabis, have been found in both cross-sectional (Kavanagh et al., 2004; McMillan et al., 2009; Morgan et al., 2011; Regier et al., 1990) and prospective (Henquet et al., 2005; Moore et al., 2007) population-based studies of people with psychotic disorders. There are many studies showing that patients with psychosis who use substances have a worse outcome than non-users (Barnes et al., 2006; Hambrecht and Hafner, 1996b; Korver et al., 2010; Mauri et al., 2006; Pencer and Addington, 2003; Peters et al., 2009; Sorbara et al., 2003; Talamo et al., 2006; Wade et al., 2006, 2007). Substance-using patients with schizophrenia are less likely to take medication, are more likely to relapse (Novick et al., 2010; Perkins et al., 2008; Turkington et al., 2009) and are more likely to commit an act of violence (Elbogen and Johnson, 2009; Fazel et al., 2009; Yee et al., 2011) than non-substance users.
It is generally assumed that the poor prognosis of substance users with psychosis is due to the direct effect of substance use. However, it is not feasible to test whether substance use causes or exacerbates psychosis using a randomised trial. Moreover, there are several other non-causal explanations for the observed association between substance use and worse outcome. One possible explanation is the existence of a shared vulnerability for both psychosis and substance use, which might result in patients with more severe symptoms being more likely to use substances (Hirvonen and Hietala, 2011; Mullin et al., 2012). Another possibility is that substance abuse brings forward the age at onset of psychosis, which prevents patients from achieving developmental milestones and affects their social performance (Large et al., 2011). Patients with more severe symptoms might also use substances as a form of self- medication for either symptoms of psychosis, side effects of medication or for associated anxiety or depression (Gregg et al., 2007; Swendsen et al., 2011). Hence, the observed differences in outcomes between substance-using and non-substance-using patients with psychosis might be due to co-variation with a third factor or a consequence of the illness itself, rather than the detrimental effects of substance use.
In a recent meta-analysis, we showed that current substance users with psychosis had more severe positive symptoms, more severe depressive symptoms and greater social disability than those with psychosis who had previously used substances (referred to in this paper as former substance users) (Mullin et al., 2012). These results support the view that the association between substance use and a poor prognosis is due to substance use, but do not exclude other possibilities, such as more severe psychosis being a cause of ongoing substance use. If it were the case that more severe psychosis is a cause of substance use, then former substance users would be expected to have more severe symptoms than those who have never used substances (non-substance users in this paper). Alternatively, if the level of symptoms of former substance users were similar to those of non-substance users, then more severe illness could be regarded as unlikely to be a cause of substance use. It is also possible that former substance users with psychosis might have better outcomes than non-substance users because substance use might precipitate psychosis in a group of people who are not otherwise predisposed and who recover after they stop using substances.
In the course of conducting our previous meta-analysis comparing the characteristics of current and former substance users with psychosis (Mullin et al., 2012), we did not locate any individual studies or meta-analyses that had the aim of comparing the characteristics of former substance users with non-substance users. The lack of primary research might be due to the low proportion of former substance users among samples of patients with psychosis, so that individual studies lacked the statistical power to detect differences between former substance users and non-substance users. A lack of statistical power in primary research can be overcome by meta-analysis.
We considered that former substance users with psychosis would be likely to have more severe symptoms than non-substance users because: (i) patients might experience ongoing effects of substance use after cessation of substances; (ii) substance use by patients with psychosis might reflect a pre-existing vulnerability to use substances that is also associated with more severe symptoms; and (iii) patients with more severe psychotic symptoms might be more likely to use substances in an attempt to alleviate symptoms or the side effects associated with more treatment.
We report a systematic review and meta-analysis to compare the symptoms and function of former substance users and non-substance users with psychotic illness. The specific null hypotheses were that groups of former substance users and non-substance users with a psychotic illness would not differ in ratings of the key outcomes of: (i) positive symptoms; (ii) negative symptoms; (iii) depressive symptoms; and (iv) global function.
Methods
The methods were based on the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Liberati et al., 2009).
Searches
Systematic searches of the electronic databases EMBASE, MEDLINE and PsycINFO were conducted for publications in English comparing the characteristics of patients with a psychotic illness who reported any use of a psychoactive substance (other than tobacco and caffeine) with the characteristics of patients with a psychotic illness who had no history of substance use (Figure 1). All papers that appeared likely to include data were examined in full text because the abstracts proved to be an unreliable guide as to whether the papers met the inclusion criteria of separately reporting on former substance users and non-substance users. The electronic search results were supplemented with a manual search of the reference lists of: (i) included studies; (ii) a recent systematic narrative review of substance use and outcome in first-episode psychosis (Wisdom et al., 2011); and (iii) a recent meta-analysis comparing the characteristics of former and current substance users (Mullin et al., 2012).
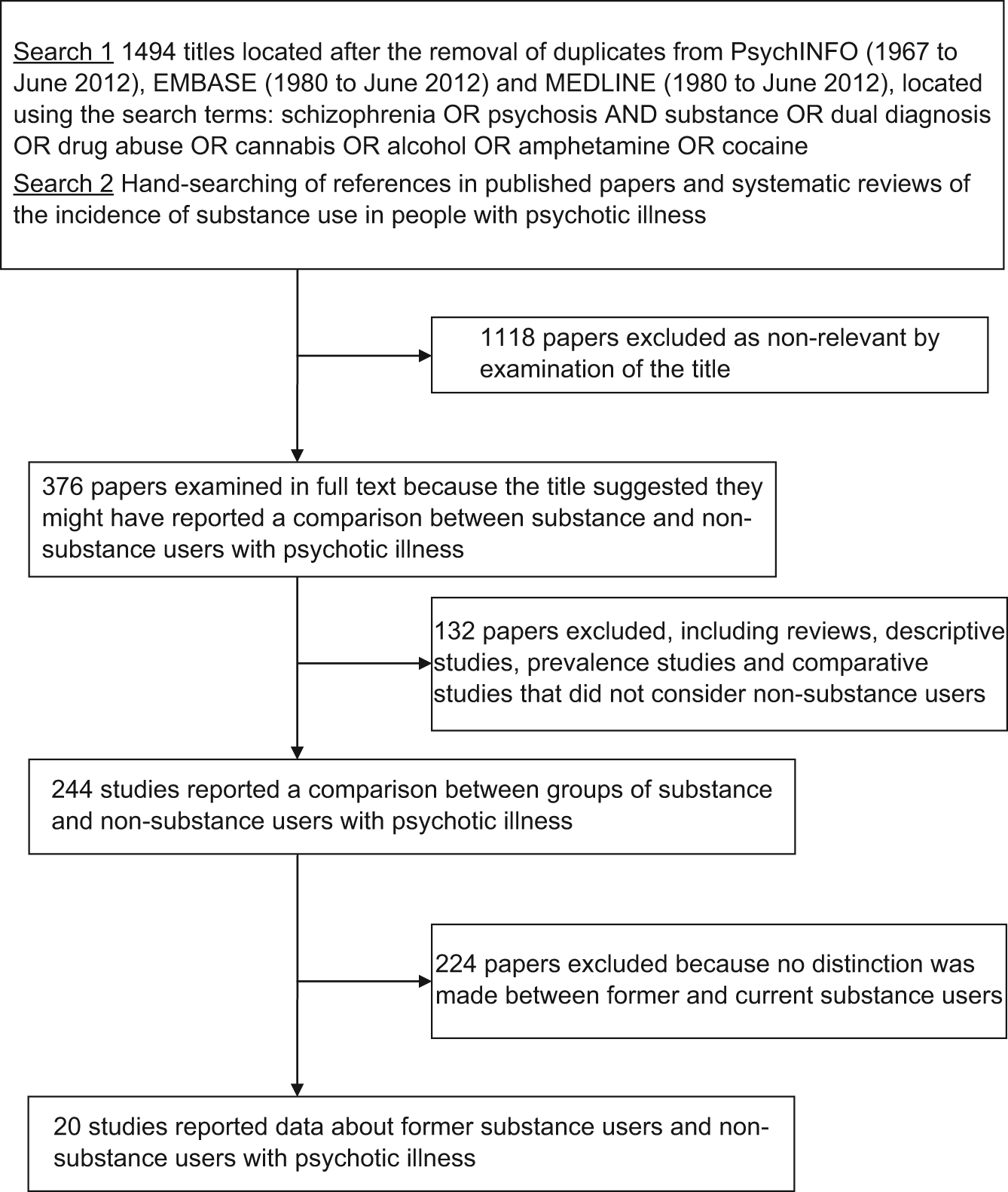
Flow chart of search strategies and results.
Definitions and coding of substance use and symptoms
Psychosis was defined as a schizophrenia-related psychosis, including patients with first-episode psychosis, schizophrenia and schizoaffective disorder, delusional disorder and affective psychosis. Studies of patients with bipolar disorder alone were not included because of the likelihood of the inclusion of patients with non-psychotic conditions. Studies of drug-induced psychosis were excluded.
The studies that met the inclusion criteria used a range of definitions of substance use. However, in all the studies, the level of substance use was considered to be clinically significant and in many studies the threshold for inclusion was the diagnosis of a substance use disorder. We included studies that considered the use of any form of psychoactive substance, including alcohol, cannabis, stimulants and other drugs, as well as studies that specifically examined cannabis use. None of the studies used tobacco smoking or caffeine use to define psychoactive substance use. We included cross-sectional studies reporting substance-use histories and longitudinal studies reporting cohorts of substance-using and non-substance-using patients in whom symptoms were measured at baseline and re-assessed at a later date.
Substance use and measures of illness severity were expressed as positive scores. A positive effect size indicated more severe symptoms in former substance users. For measures of global function, a negative effect size indicated reduced function among former substance users.
Data extraction
KM, PG and ML independently extracted the following data:
diagnostic criteria of included patients, the substances examined, and the number of former substance-using and non-substance-using patients;
demographic data for both groups – age, age at onset of psychosis, sex and the level of education;
measures of the three key symptom outcomes – positive psychotic symptoms, negative symptoms and symptoms of depression;
measures of global function (including employment);
other outcomes – total symptom scores, numbers of hospital admissions, self-harm, episodes of violence and convictions for non-violent offences.
Assessment of study quality
The quality of the methods of each study was rated using an eight-point scale (see data supplement, Table DS1). Studies of patients with schizophrenia-related psychosis were regarded as being of greater quality than those examining a mix of affective and non-affective psychoses because differences in the prognosis between the two diagnostic groups might obscure the effect of ceasing substances. Studies examining consecutive presentations and those with a participation rate of over 50% were also regarded as being of higher quality. Studies with a larger sample of former substance users (n ≥ 25) were regarded as being of higher quality because of the reduced probability of chance findings. Longitudinal studies were also considered to be of higher quality because those studies were in a better position to confirm cessation of substances and measure the benefits of giving up. The scale also accorded a point for using structured methods for establishing the history of substance use, the diagnosis of psychosis and measuring outcome. Studies with a score of 6 or more were classified as being of higher quality.
Meta-analysis
Meta-analysis was performed using a random effects model because of differences between the studies in the diagnostic inclusion criteria, stage of psychotic illness and the definition of key variables. A random effects model only requires that definitions be consistently applied within each study. Variables reported in fewer than five studies were excluded from the meta-analysis because the random effects model selected for this analysis lacks the statistical power to detect potentially significant effect sizes when the number of studies is small (Borenstein et al., 2009).
The statistical power of a random effects meta-analysis was considered on an a priori basis using assumptions based on our earlier meta-analysis of the symptoms of current and former substance users and the method described by Borenstein and associates (Borenstein et al., 2009). We estimated that a random effects meta-analysis of 15 studies, each with a sample size of approximately 25 subjects in each group, where between-study heterogeneity was high, would have an 80% chance of detecting a small standardised mean difference (SMD) of 0.3 at a level of significance of 0.05. The power of the study would be increased if there were more than 15 studies, if the included studies had a larger mean sample size, if the heterogeneity was low or if the true difference between the groups was larger than a SMD of 0.3.
Comprehensive Meta-Analysis (Version 2; Biostat, Englewood, NJ, USA) was used to convert all continuous data into a SMD and was also used to calculate pooled effect sizes, to assess heterogeneity and to assess the possibility of publication bias. Categorical data was analysed using meta-analysis of odds ratios (OR). Between-study heterogeneity was assessed with I-squared statistics. Between-study heterogeneity was classified as low if I-squared was below 25, moderate for I-squares between 25 and 50, and high if I-squared was above 50 (Higgins et al., 2003). Between-subgroup heterogeneity in effect size was examined using Q-value statistics and a significance level of 0.05. The possibility of publication bias was examined using funnel plots.
Subgroup analysis to investigate between-study heterogeneity
Three subgroup analyses were performed to explore between-study heterogeneity that might have arisen from:
differences between the studies that grouped patients according to a history of the abuse of any substance, or cannabis alone;
whether the studies were conducted in cohorts of patients with first-episode psychosis or among patients with a more established illness; and
differences in overall study quality.
Results
Searches, data extraction and selection of variables for meta-analysis
The electronic searches and the hand searches of references identified 376 potentially relevant papers identified by their title. KM and ML examined all of the papers in full text (Figure 1). Twenty papers met the inclusion criteria (Table 1). There were disagreements in 17 of 724 data points (2.3%) extracted independently by KM and PG. ML performed a third independent data extraction, and the remaining discrepancies were resolved by re-examination of the data by ML.
Included studies reporting the characteristics of former substance-using and non-substance-using patients with psychosis.
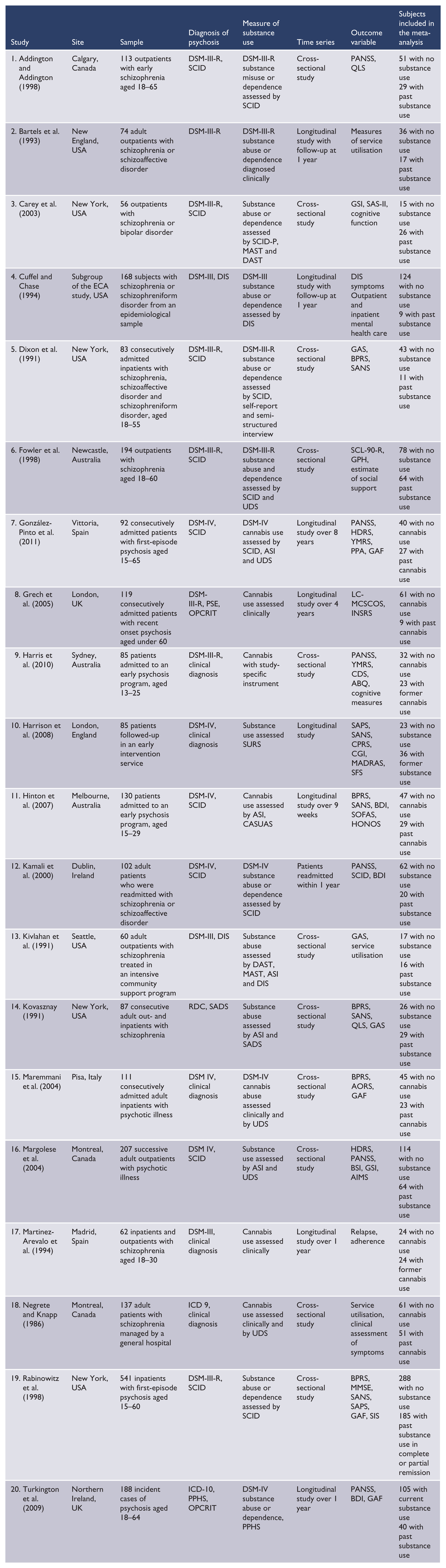
ABQ: aggressive behaviour questionnaire; AORS: overt aggression rating scale; ASI: addiction severity index; BDI: Beck depression inventory; BPRS: brief psychiatric rating scale; BSI: brief symptom inventory; CASUAS: cannabis and substance use assessment schedule; CDS: Calgary depression scale; CPRS: comprehensive psychopathological rating scale; DAST: drug abuse screening test; DIS: diagnostic interview schedule; DSM: Diagnostic and Statistical Manual; ECA: epidemiologic catchment area; GAF: global assessment of function scale; GAS: global assessment scale; GSI: global severity index; HDRS: Hamilton depression rating scale; HoNOS: health of the nation outcome scale; LC-MCSCOS: life chart from the multi-centre study on the course and outcome of schizophrenia; MADRAS: Montgomery–Asberg depression rating scale; MAST: Michigan alcoholism screening test; OPCRIT: operational criteria for psychotic illness; PANSS: positive and negative symptom scale; PPA: Phillips pre-morbid adjustment scale; PPHS: psychiatric and personal history schedule; PSE: present state examination; QLS: quality of life scale; RDC: research diagnostic criteria; SADS: schedule for affective disorders and schizophrenia; SANS: scale for the assessment of negative symptoms; SAPS: scale for assessment of Positive symptoms; SCID: structured clinical interview for DSM-IV; SCL-90-R: symptom checklist 90–revised; SOFAS: social and occupational function scale; SURS: substance use rating scale; UDS: urine drug screen; YMRS: Young mania rating scale. AIMS: Abnormal Involuntary Movement Scale; ICD: International Classification of Diseases; MMSE: Mini Mental State Examination; GPH: Global Personal Hopefulness scale; SIS: Structured Interview for Schizotypy; SFS: Social Functioning Scale; INSRS: Iager Negative Symptom Rating Scale; SAS: Social Assessment Scale; CGI ; Clinician Global Impression scale.
The 20 studies reported a total of 2024 patients, of whom 1292 (63.8%) patients were non-substance users (mean sample size of 64.6 per study, standard deviation (SD) 61.2) and 732 (36.2%) were former substance users (mean of 36.6 per study, SD 38.3). Current substance users were not considered in this study.
Most studies used well-established measures of illness severity:
6 used the Positive and Negative Syndrome Scale;
5 used the Brief Psychiatric Rating Scale;
2 used the Scale for the Assessment of Positive Symptoms;
5 used the Scale for the Assessment of Negative Symptoms;
3 used the Beck Depression Inventory;
2 used the Hamilton Depression Rating Scale (see Table 1 for details).
Most of the studies comparing former substance users with non-substance users were cross-sectional in design. A smaller number provided some longitudinal data after a period of follow-up (González-Pinto et al., 2009; Turkington et al., 2009). No study reported repeated measures of symptoms before and after the cessation of substance use. Of the studies that reported data measured at more than one point in time, the data after the longest period of follow-up were used. Hence, the meta-analysis can be considered to be of cross-sectional data.
A total of 13 variables were reported in five or more studies. These included five demographic or diagnostic variables (age, age at onset of psychosis, sex, years of education, proportion with a schizophrenia-related psychosis), four key outcome measures (positive symptoms, negative symptoms, depressive symptoms and global function) and four other outcomes (total symptom scores, a history of self-harm, episodes of violence or criminal convictions and the number of hospital admissions).
Seven of the 20 studies reported on cannabis users and 13 used the broader definition of any substance use. Seven studies were conducted among patients in first-episode psychosis. Eight studies were rated as being of higher quality, defined as a score of more than 6 out of 8 on our quality assessment scale. Every study had at least two features indicating study quality and no study was excluded from the meta-analysis because of quality concerns (see data supplement, Table DS1). There were 15 studies reporting on positive symptoms but fewer studies reporting negative symptoms (n = 10), depressive symptoms (n = 9) or measures of global function (n = 9).
Results of the main meta-analysis
There were no significant differences between former substance users and non-substance users in the four key variables of positive symptoms, negative symptoms, depressive symptoms or global function (Table 2).
Comparison of the characteristics of former substance users and non-substance users with psychosis.
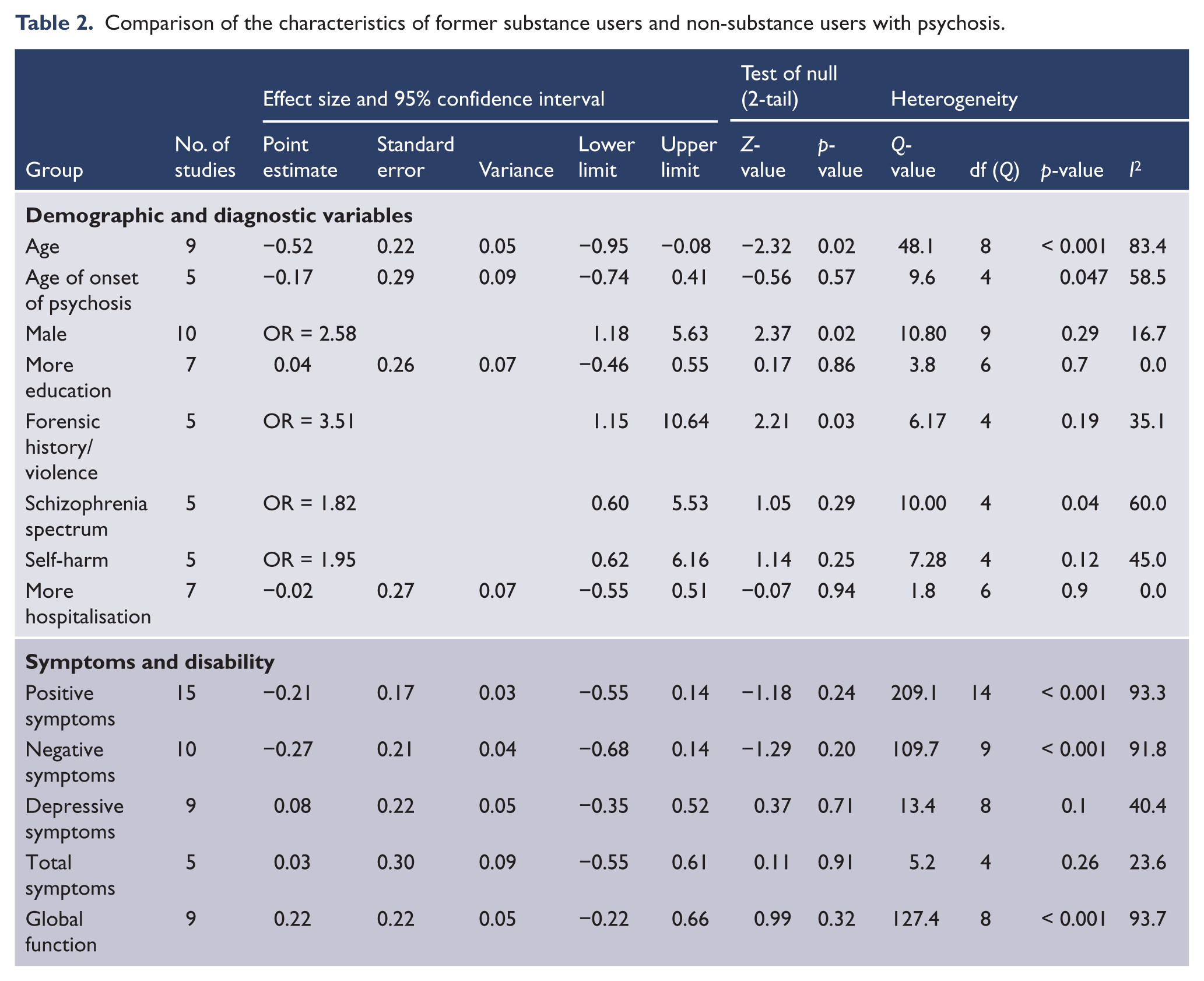
Former substance users were significantly younger, were more likely to be male and were more likely to have had a history of criminal convictions or a history of violence than non-substance users. There were no significant differences between former substance users and non- substance users in the proportions of patients with a schizophrenia-related psychosis, age at onset of psychosis or years of education. There were no significant differences in the number of hospital admissions or in the frequency of self-harm between former substance users and non-substance users (Table 2; further details in data supplement, Table DS2). In the main analyses that included all of the available studies, there were non-significant trends towards former substance users having less severe positive symptoms, less severe negative symptoms and better global function than non-substance-using patients. There was no suggestion of a difference in depressive symptoms between former and non-substance users.
Investigation of between-study heterogeneity
There was a high degree of between-study heterogeneity in the effect sizes for positive symptoms, negative symptoms and global function, confirming the decision to use a random effects model in the meta-analysis. Between-study heterogeneity in the effect size for depression was rated as moderate.
Sources of between-study heterogeneity were examined by three sub-group analyses: (i) first-episode versus previously treated patients; (ii) cannabis use versus other substance use; and (iii) higher-quality studies versus other studies. Tests of publication bias such as the fail-safe N and trim and fill tests were not indicated because the findings were not statistically significant.
Subgroup analysis of studies of cannabis users, first-episode patients and of higher-quality studies
There were no significant differences between former cannabis users and former users of any substance in the effect size for positive, negative and depressive symptoms, and for measures of global function as assessed by the contribution to between-study heterogeneity (Table 3).
Comparison of former and non-substance users with psychosis according to use of cannabis versus any substance use.
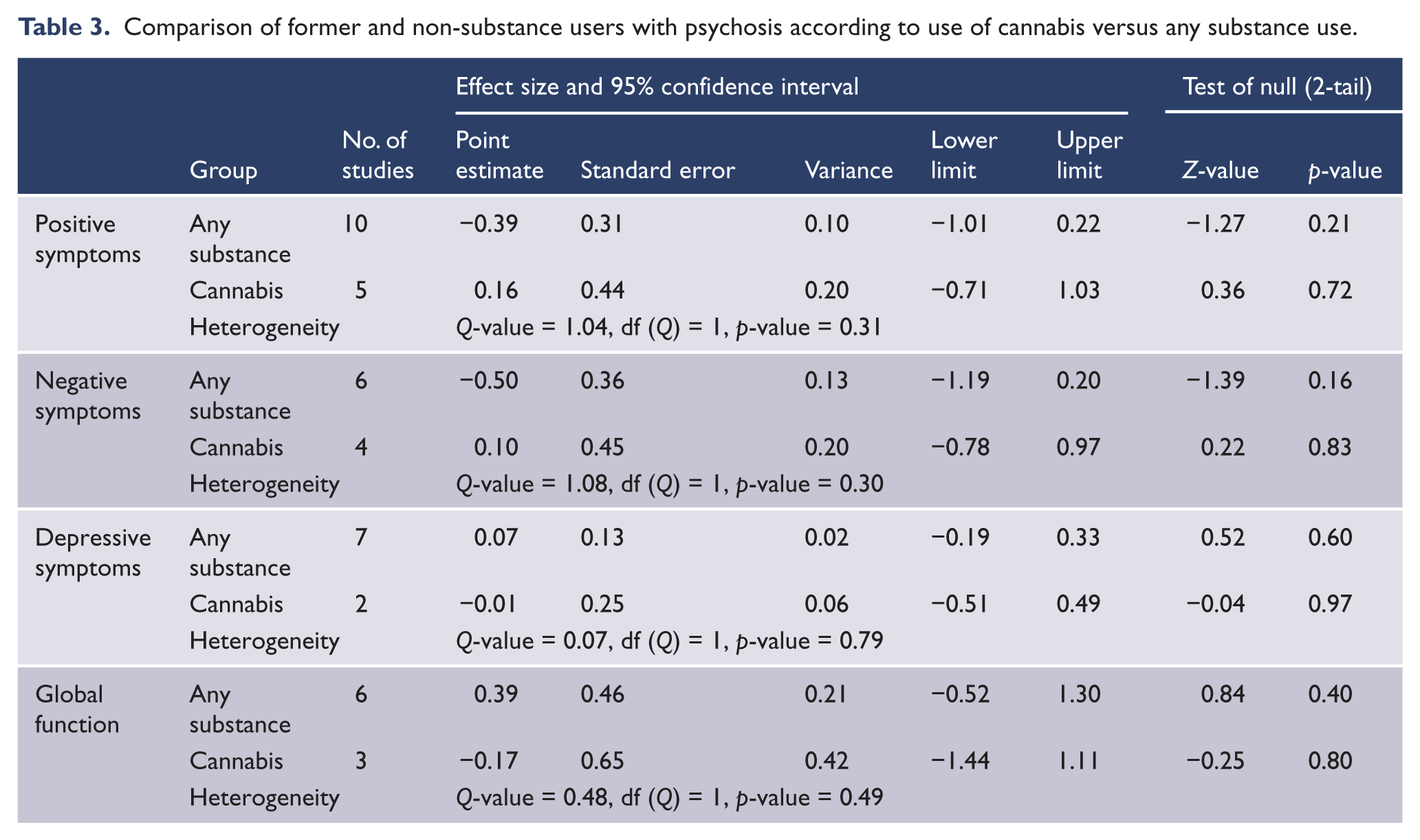
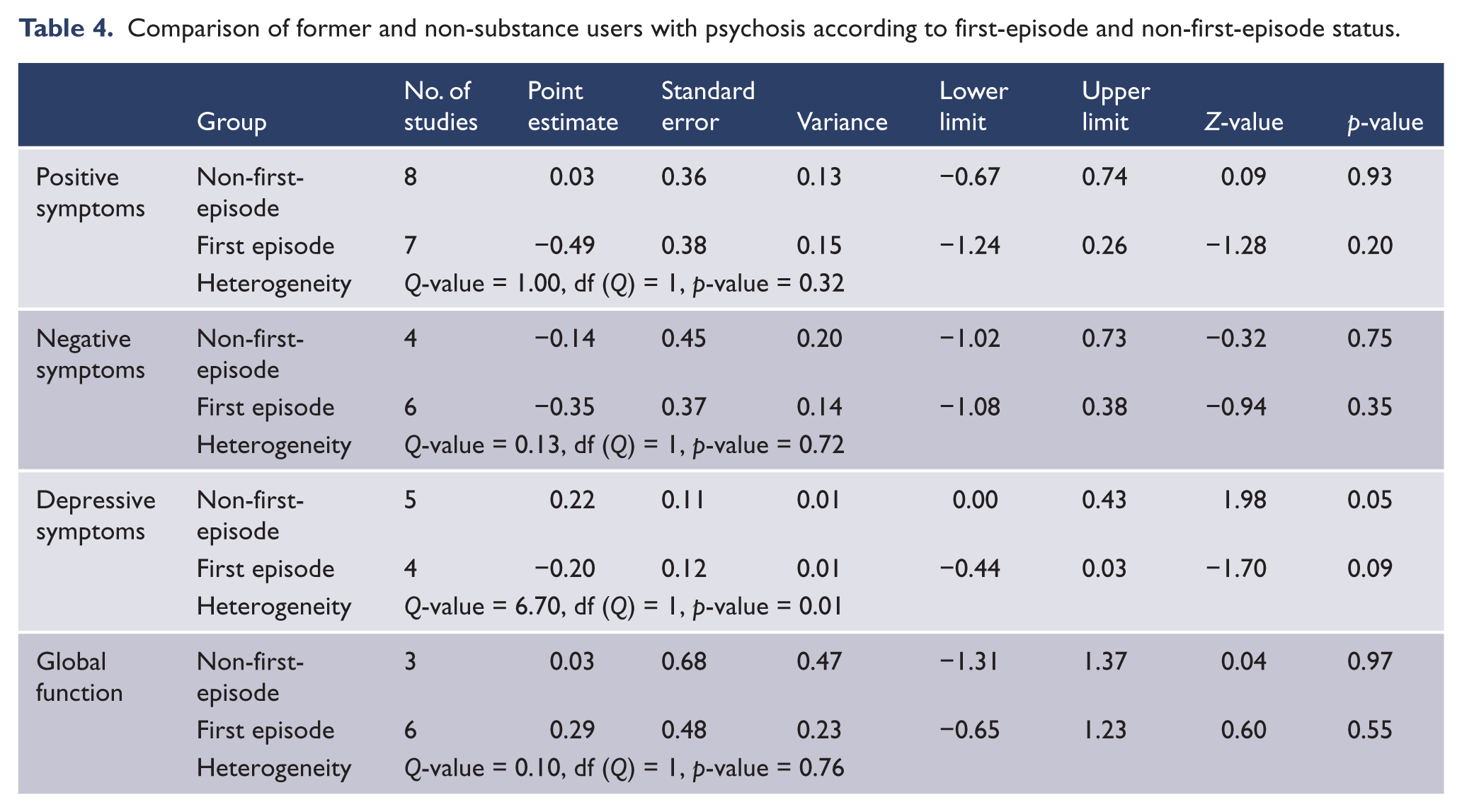
The subgroup of studies of first-episode psychosis patients (n = 7) made no significant contribution to the between-study heterogeneity of the effect size for positive symptoms, negative symptoms or global function. Non-first-episode patients who were former substance users had significantly more depressive symptoms than non-substance users. By contrast there was a trend towards first-episode patients who were former substance users having fewer depressive symptoms than first-episode patients who were non-substance users. First-episode status made a statistically significant contribution to the observed heterogeneity of the effect size for symptoms of depression, indicating a significant differential effect of giving up substances between first-episode patients and non-first-episode patients (Table 4).
Comparison of former and non-substance users with psychosis according to first-episode and non-first-episode status.
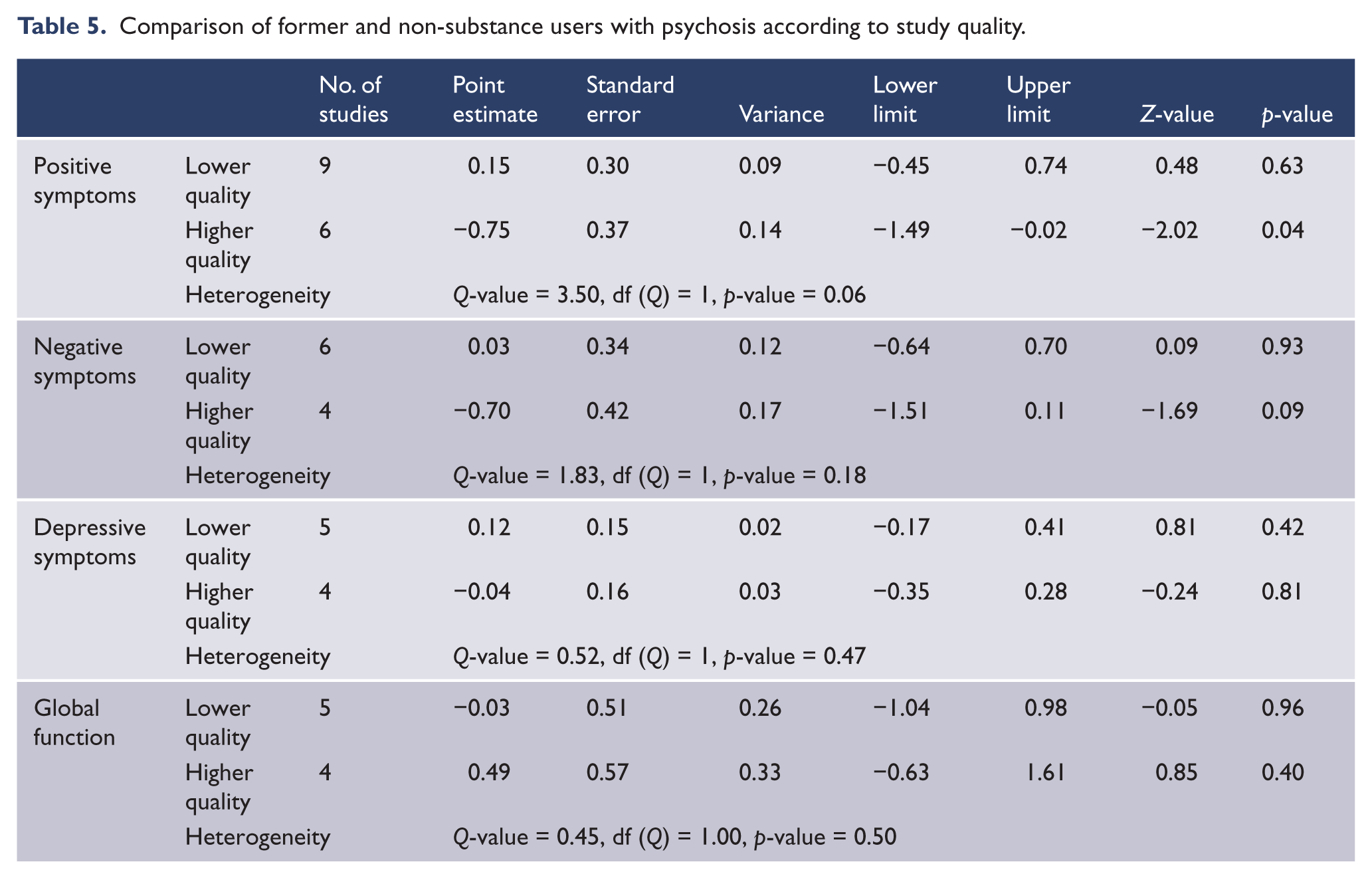
In higher-quality studies (n = 6), former substance users had significantly fewer positive symptoms than non-substance users and there was a statistical trend suggesting that study quality contributed to between-study heterogeneity in the effect size with respect to positive symptoms. There was a trend towards former substance users having less severe negative symptoms in the meta-analysis of studies of higher quality. The effect size heterogeneity in measures of negative symptoms, depressive symptoms and global function were not explained by ratings of study quality (Table 5).
Comparison of former and non-substance users with psychosis according to study quality.
Discussion
The finding of the main analyses in this study was that we were unable to demonstrate differences between former substance users with psychotic illness and non-substance users in ratings of positive symptoms, negative symptoms, depressive symptoms and global function. However, the sub-analyses of the higher-quality studies found that former substance users have significantly fewer positive symptoms than non-substance users and the sub-analysis of first-episode psychosis patients found that former substance users had fewer depressive symptoms than non-substance users.
The results of this study add to the findings of our earlier study, which found that current substance users had more severe symptoms and worse global function than former substance users (Mullin et al., 2012). The lack of significant differences between former substance users and non-substance users suggests that patients who are able to cease substance use can expect to recover to the same overall level of symptoms and global function as patients with psychosis who have never used substances. This adds support to the hypothesis that the worse outcomes of substance users with psychosis are related to continued use of substances, rather than the substance-use being due to the patient having a more severe psychotic illness. The findings do not support the suggestion of the existence of a shared vulnerability to both substance-use and more severe psychosis, nor does the study support the suggestion that patients with more severe psychosis are more likely to use substances as a form of ‘self medication’. However, neither of these explanations can be dismissed on the basis of our findings. Although the sub-group analyses suggest that some patients with psychosis who give up substance use might have fewer positive symptoms and less depression, the findings also suggest that giving up substances after developing psychotic illness may not be sufficient, at least in the short term, to bring about a remission of symptoms in many patients, including among first-episode psychosis patients. One limitation of the study was that much of the primary data was cross-sectional and later improvements in former substance users might have been missed. It is also possible that subjects who ceased substance use and recovered were lost to follow-up in the longitudinal studies, resulting in a bias away from a finding of less severe symptoms among former substance users.
The failure to detect a significant difference between former substance users and non-substance users does not exclude the possibility that such a difference exists because the variables we examined in the main analysis of 15 studies that reported measures of positive symptoms did not have the statistical power to detect small effect sizes of less than a SMD of 0.3. However, the lack of a discernible difference might not have been due to the magnitude of the effect size, and instead might have been a result of the lower quality methodology of some studies, because the sub-analysis of a small number of higher-quality studies did find that former substance users had fewer positive symptoms. Hence, another meta-analysis performed when more studies of higher quality are available might find significant differences between former substance users and non-substance users with psychosis. Moreover, a meta-analysis performed when more primary research is available might have the statistical power to detect differences in negative symptoms, depressive symptoms and global function between groups of former and non-substance-using patients.
The main limitation of the study was that former substance users were more likely to be younger and male than non-substance users. This lack of matching was unlikely to have resulted in our failure to find that former substance users had more severe illness than non-substance users, because younger age and being male are associated with a poorer prognosis for psychotic disorders (Abel et al., 2010; Riecher-Rössler and Häfner, 2000). It follows that the larger number of younger people and males in the former substance-using groups might have biased the study away from finding that former substance users have a better prognosis than non-substance users.
A further limitation to the findings stems from differences in the definitions of ‘substance use’ used in the primary research included in this study. It is possible that the between-study heterogeneity in the outcomes was due to differences in the definitions of the types or amounts of substances used. For example, the direction of the effect sizes suggested that former cannabis users had non-significantly more positive and negative symptoms when compared to non-cannabis users, while former users of any substance tended to have less severe positive and negative symptoms than substance non-users. This trend might have been due to former cannabis users continuing or commencing the use of other substances, or because their use of cannabis had a lasting effect on the course of their psychotic illness. We were also unable to differentiate the effects of alcohol from other drugs. None of the primary research reported on the symptoms of former and non-alcohol users. Hence, it is possible that differences in the proportions of former alcohol users between studies might account for the observed between-study heterogeneity in symptoms and global function if giving up alcohol is associated with more symptomatic improvement than giving up other substances.
Despite these limitations, the findings of this study provide evidence that the symptoms and disability of patients with psychosis who stop using substances are no worse than those who have never used substances, which in turn suggests that current, rather than past substance use contributes to the severity of symptoms. When ratings of depression are considered, the findings suggest that becoming abstinent from substances early in the first episode of psychosis is likely to have a greater benefit than giving up later in the course of illness. Although the findings of this study do not support the ‘self-medication’ hypothesis as a major cause of substance use in psychosis, it is also possible some former substance users might have used substances to alleviate the effect of symptoms when they were untreated, or may have been more unwell than non-users when they were using substances (Hambrecht and Hafner, 1996a). Finally, the results do not exclude the possibility that patients with more severe illness are generally less able to stop substance use.
The findings of the study support the need to assist substance-using patients to stop or reduce their substance use. However, there is currently little evidence that any specific treatment programs for substance use, particularly use of cannabis, can bring about sustained abstinence among patients with psychotic disorders (Baker et al., 2010). In our earlier meta-analysis, we found that there are similar numbers of current and former substance users (Mullin et al., 2012) and in the studies included in this meta-analysis there was about one former substance user for every two non-substance users. The observation that many patients stop using substances soon after diagnosis and the disappointing results of interventions aimed at reducing substance use in the remaining patients is something of a paradox, which might be explained by the rational decision of many patients to heed the medical advice to stop using substances before they are considered for recruitment into trials of treatment for substance use. Alternatively, patients with more significant substance use might be less likely to be recruited into clinical studies, such as the studies included in our meta-analysis, leaving patients who had less difficulty ceasing substance use as the subjects in published studies. Hence, it is possible either that the results of substance cessation trials might be disappointing because of selection bias towards patients who have difficulty giving up substances, or that naturalistic studies are more likely to include patients who are able to cease substance use. Furthermore, substance-using patients who give up substance use and improve significantly may be lost to follow-up. Nevertheless, even if the natural history of substance use in psychosis is better than intervention studies suggest, patients with psychosis who do not stop substances despite medical advice present a significant therapeutic challenge.
This study and our earlier meta-analysis comparing current and former substance users suggest that (i) giving up substances can improve the symptoms and global function of patients with psychosis, and (ii) the level of improvement brings the patients who give up to a degree of symptoms and global functioning that is similar to patients with psychosis who have never used substances. The meta-analysis and most of the primary research in this area has the limitation of being both naturalistic and cross-sectional in its sampling of patient characteristics. However, the results are similar to those of three recent studies that did not meet our inclusion criteria, but looked at the association between the level of substance use and the severity of psychotic and other symptoms over time using a longitudinal design with repeated measures of outcome (Barrowclough et al., 2011; Faber et al., 2012; van Dijk et al., 2012). These studies all examined the effect of cannabis use over time in cohorts of patients with psychosis. None of the studies were able to demonstrate that reduced or increased substance use had an impact on positive symptoms, although two studies suggested that ongoing cannabis use was associated with poorer social function (Barrowclough et al., 2011; Faber et al., 2012) and one of the studies found that cannabis users were more likely to be readmitted to hospital (van Dijk et al., 2012). The absence of improvement in symptoms after the reduction in cannabis use in these longitudinal studies is broadly consistent with the results of this study and those of our previous meta-analysis of current and former substance users (Mullin et al., 2012). It is not clear whether existing studies are unable to detect the benefits of cannabis cessation because of the replacement of cannabis with substances such as alcohol or stimulants, or whether the adverse effects of cannabis persist after ceasing the drug.
While it may be that stopping substance use, in particular cannabis use, might not bring about rapid or dramatic improvements in symptoms or global function, a particular focus on cannabis use in the early phases of psychotic illness is certainly warranted because of the compelling evidence that cannabis use is associated with an increased incidence of psychosis (Moore et al., 2007) and an earlier onset of psychotic illness (Compton et al., 2009; Large et al., 2011). Reducing substance use among patients identified as being at high-risk of developing psychosis, as well as those in first-episode psychosis, could reduce the incidence and improve the course of psychotic illness. The treatment of substance use among patients with psychosis should be regarded as a key element of psychosis treatment programs, with a similar status to the initiation and maintenance of treatment with antipsychotic medication and psychosocial treatments to overcome social disability. The development of effective treatments for substance abuse in people with psychosis should remain a priority in psychosis research.
Footnotes
Authors’ contribution
Dr Large has full access to all the data and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Large; acquisition of data: Gupta, Harris, Large, Mullin; statistical analysis: Large; interpretation of data: Gupta, Harris, Large, Nielssen, Mullin; drafting of the manuscript: Gupta, Large, Nielssen; critical revision of the manuscript for important intellectual content: Harris, Nielssen; administrative, technical, or material: Large; study supervision: Large.
Online supplemental information
Table DS1 and Table DS2.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Declaration of interest
The authors report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
