Abstract
Near-infrared fluorescence (NIRF) imaging has great potential for studying physiological and pathophysiological processes noninvasively in several locations of the body. In this study, we evaluated the feasibility of NIRF imaging to visualize fluorescent compounds within the brains of live mice commonly used in brain research. To simulate the presence of a molecular NIRF reporter agent at the site of a lesion, we developed a new in vivo phantom model wherein capsules containing different amounts of an NIRF dye (Cy5.5) were stereotactically implanted deep into the left hemispheres of living mice. To precisely locate the implanted capsules, magnetic resonance imaging (MRI) was performed. Fluorescence reflectance imaging (FRI) and transillumination fluorescence imaging (TFI) were conducted to analyze and compare sensitivity and target-to-background ratios of the two methods. The sensitivities of FRI and TFI to background fluorescence from circulating dye was tested by imaging fluorescent capsules in mice intravenously injected with increasing amounts of long-circulating Cy5.5-dextran. The results show that capsules containing dye amounts as low as 10−12 mol can be detected. TFI yielded significantly higher target-to-background ratios than FRI at 10−11 mol (
Keywords
Introduction
In recent years, numerous near-infrared fluorescence (NIRF) reporters have been designed and successfully used for noninvasive NIRF imaging of biological processes in a variety of small-animal disease models including cancer [1], cardiovascular diseases [2], and arthritis [3]. NIRF imaging offers several advantages: It sensitively detects low amounts of fluorochrome, uses nonionizing radiation, requires relatively simple instrumentation, is inexpensive and rapid, and allows for high-throughput imaging of animals. Not surprisingly, a number of NIRF imaging devices with different setups, modes of data collection, and features have now become available and have been tested for small-animal imaging purposes. The majority of these systems are based on so-called planar fluorescence imaging. To access the distribution of fluorescent probes using planar imaging systems in vivo, the animal is illuminated with light tuned to the excitation wavelength of the fluorescent reporter agent. The fluorescence light is then detected with a highly sensitive charge-coupled device (CCD) camera equipped with appropriate filters to discriminate fluorescence from excitation light. The light source and the detector can be either on the same side of the animal (fluorescence reflectance imaging [FRI]) or on opposite sides (transillumination fluorescence imaging [TFI]). More complex tomographic systems (fluorescence-mediated tomography [FMT]) have also recently emerged. In these systems, light is coupled sequentially to the object at different locations for a fixed position of the detectors, thus delivering 3-D reconstructions of the fluorochrome distribution in an object and data for quantitative analysis [4–6].
Although NIRF imaging has great potential for studying physiological and pathophysiological processes in the brain, including brain tumors, stroke, or neurodegenerative diseases, the number of approaches using noninvasive NIRF imaging to evaluate biological events within the brain of live animals is currently limited [7,8]. When applying the method to animal models of brain diseases, one faces various methodological challenges: Due to photon absorption in tissue, the depth of the fluorescent object nonlinearly decreases the number of excitation photons reaching the fluorochrome and the number of fluorescent photons reaching the detector. Thus, the detection limit of the method is reduced compared to observations of fluorescent sources at the surface of the animal. The successive attenuation of photons by several tissue layers of different vascularization and composition such as the scalp, the skull, and the meninges leads to distortion of the fluorescence signal. Furthermore, the demand for high specificity of a systemically administered fluorescent reporter is increased because the tissue surrounding the brain is highly vascularized, which may result in increased background fluorescence from circulating or unbound extravascular probe. Adding to these issues, many brain disease models can only use pigmented mice with fur, further reducing the number of photons that can be detected [4].
In this study, we wanted to explore the feasibility of applying noninvasive NIRF imaging to visualize biological processes in animal models of brain diseases. To simulate the presence of an accumulating fluorescent molecular reporter at the site of a lesion, we developed a new in vivo phantom model wherein capsules containing different amounts of an NIR fluorochrome (Cy5.5) were implanted into the left hemispheres of live C57Bl6 mice, a pigmented mouse strain that is commonly used in brain research [9]. This in vivo phantom offers the advantage in that it preserves the complex optical properties of living tissue. By varying the concentration of the contrast agent in the capsule, the sensitivity of FRI and TFI to detect a fluorochrome in the brain of mice was evaluated. Target-to-background ratios were calculated to compare the two modes of data collection. The sensitivity of planar NIRF imaging to background fluorescence was tested by injecting the mice intravenously with a long-circulating NIRF compound (Cy5.5-dextran).
Materials and Methods
Generation of Fluorescent Capsules
Translucent polyethylene tubes with an outer diameter of 0.61 mm and an inner diameter of 0.26 mm (SIMS Portex Ltd, Kent, UK) were filled with varying concentrations of a Cy5.5-dextran solution (MW = 70 kDa, Nanocs, New York, NY). The tubes were cut into 2-mm pieces, for a net volume of 0.106 μL. The pieces were then thermically sealed. Capsules containing 10−11, 10−12, or 10−13 mol Cy5.5, corresponding to a concentration of 10−4, 10−5, and 10−6 M, respectively, were stereotactically implanted deep into the brain of live mice.
Animals
Fifteen adult male C57Bl6 mice weighing 18–20 g (Bundesinstitut fuer Risikoforschung, Berlin, Germany) were used. The animals were housed under standard conditions with food and water available ad libitum. All procedures were in accordance with German animal welfare laws and approved under the animal research license G0229/05.
In Vivo Implantation of Capsule
During the implantation and imaging procedure, the mice were anaesthetized by injecting a
Experimental Design
For assessing the detection limit of the NIRF imaging system using the in vivo phantom, capsules of 10−11 (
Magnetic Resonance Imaging
MRI was performed on a dedicated animal scanner (7 T Bruker scanner, Pharmascan 70/16 AS, Bruker Bio-spin, Ettlingen, Germany) with a 16-cm horizontal bore magnet and a 9-cm (inner diameter) shielded gradient with a maximum strength of 300 mT/m. For imaging the mouse brain, a T1-weighted 2-D turbo spin-echo sequence was used (TR 1000 msec, TEeff 13.2 msec, four averages, total scan time 8 min 30 sec). Ten coronal and sagittal slices with a slice thickness of 0.7 mm were positioned to cover the brain region of interest (ROI). The field of view (FOV) was 2.84 × 2.84 cm and the matrix was 256 × 256 resulting in an in-plane resolution of 111 μm.
Fluorescence Reflectance Imaging and Transillumination Fluorescence Imaging
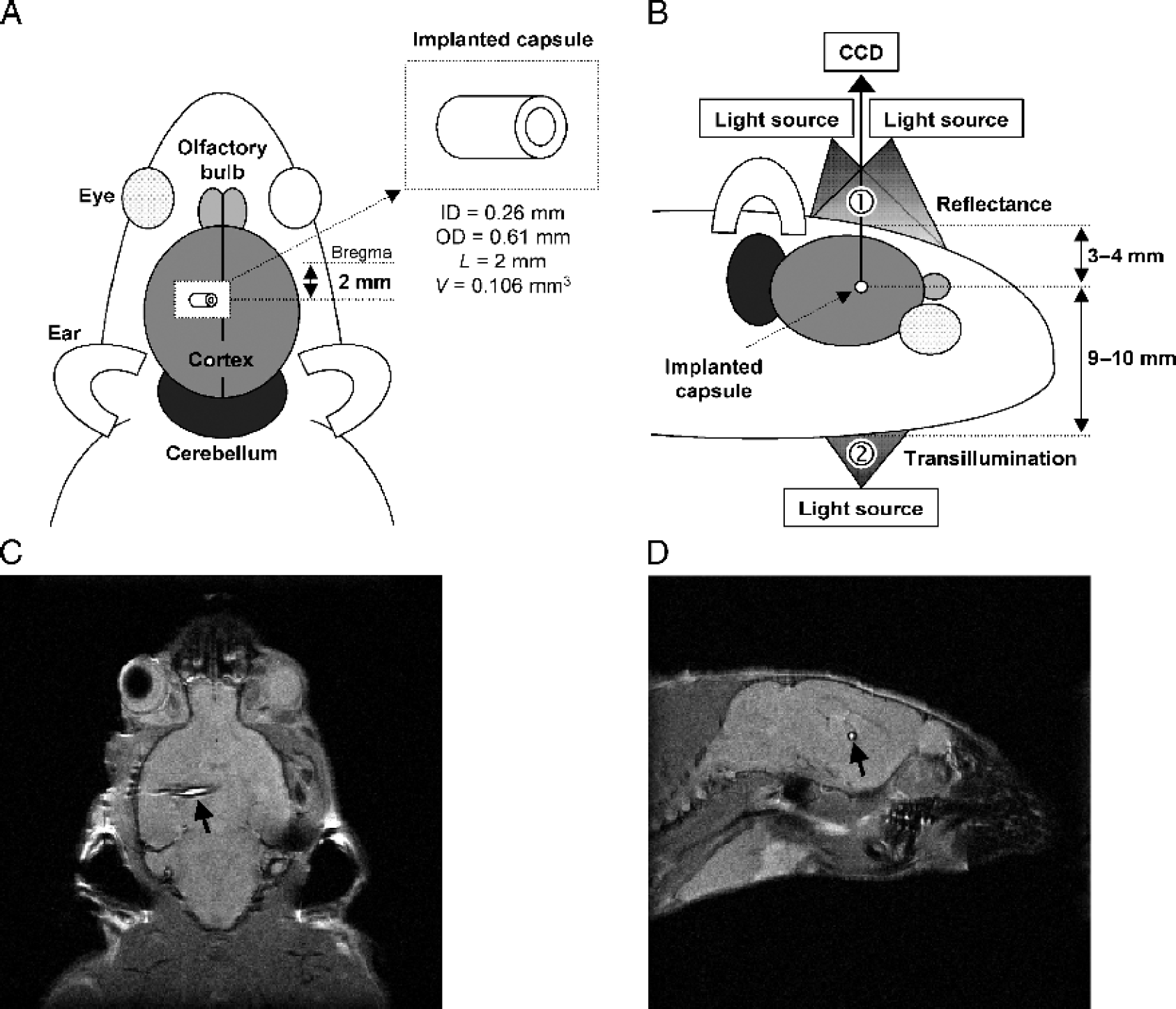
For NIRF imaging, we used a system developed by our group whereby FRI and TFI can be performed without having to move the animal: Light from a TEC-cooled laser diode emitting at 682 nm with a maximum power of 350 mW (Roithner Lasertechnik, Vienna, Austria) was coupled to an optical switch (LightTech Fiber-optics Inc, San Leandro, CA) to facilitate convenient switching between FRI and TFI. The laser power behind the switch was kept constant to 40 mW. The light was directed into a dark chamber by optical fiber bundles (diameter 0.5 mm, Loptek, Berlin, Germany). For FRI, the light was coupled into two fibers and the object (the heads of the mice from above) was illuminated by two overlapping light cones with a circle diameter of about 4 cm at an object distance of about 10 cm. Illumination inhomogeneities in the field of view were below 10%. For TFI, the light fiber was directly coupled to the throat of the animal (Figure 1). In both settings, the emitted fluorescence light was detected by using a back-illuminated nitrogen-cooled CCD camera (Vers Array 512, 512 × 512, Roper Scientific Inc., Duluth, GA) equipped with a focusing lens system (Nikkor macro lens,
Data Processing and Image Analysis
Data processing and analysis was accomplished using customized routines in Matlab 6.5 software (The Mathworks, Inc., Natick, MA). The offset due to readout noise was removed by an automatic baseline correction prior to analysis. All images were normalized to the acquisition time, thus returning counts per second. To correct for superficial fluorescence from dust and for cosmic rays, the top hat image (top-hat filtering, structuring element circle with a diameter of 4 pixels) was subtracted from each image. In a second step of analysis, images were corrected for illumination inhomogeneities by dividing the fluorescence image by the image that was recorded without blocking the excitation light. ROI analyses, using Matlab software, were performed with rectangular ROIs manually selected over the right and left hemisphere of the mouse brain. In each ROI, the average value over all pixels of the normalized image was calculated. To minimize user variability, ROIs were selected by three skilled scientists and showed no significant differences between users. Target-to-background ratios were calculated by dividing the ROI values of the left hemisphere by the ROI values of the right hemisphere. For statistical comparison of the target-to-background ratios, an unpaired Student's
Results
Characterization of the In Vivo Phantom Model
The properties of the in vivo phantom model are illustrated in Figure 1. The capsules could be exactly positioned with high reproducibility. The deviation of the intended implantation depth and distance from the midline was less than 0.5 mm, as determined by MRI. The whole procedure (surgery, injections, imaging) was well tolerated by the anesthetized animals. No hemorrhages as a result of the implantation procedure were observed. No animals had to be excluded from the study.
Detection Limit of FRI and TFI
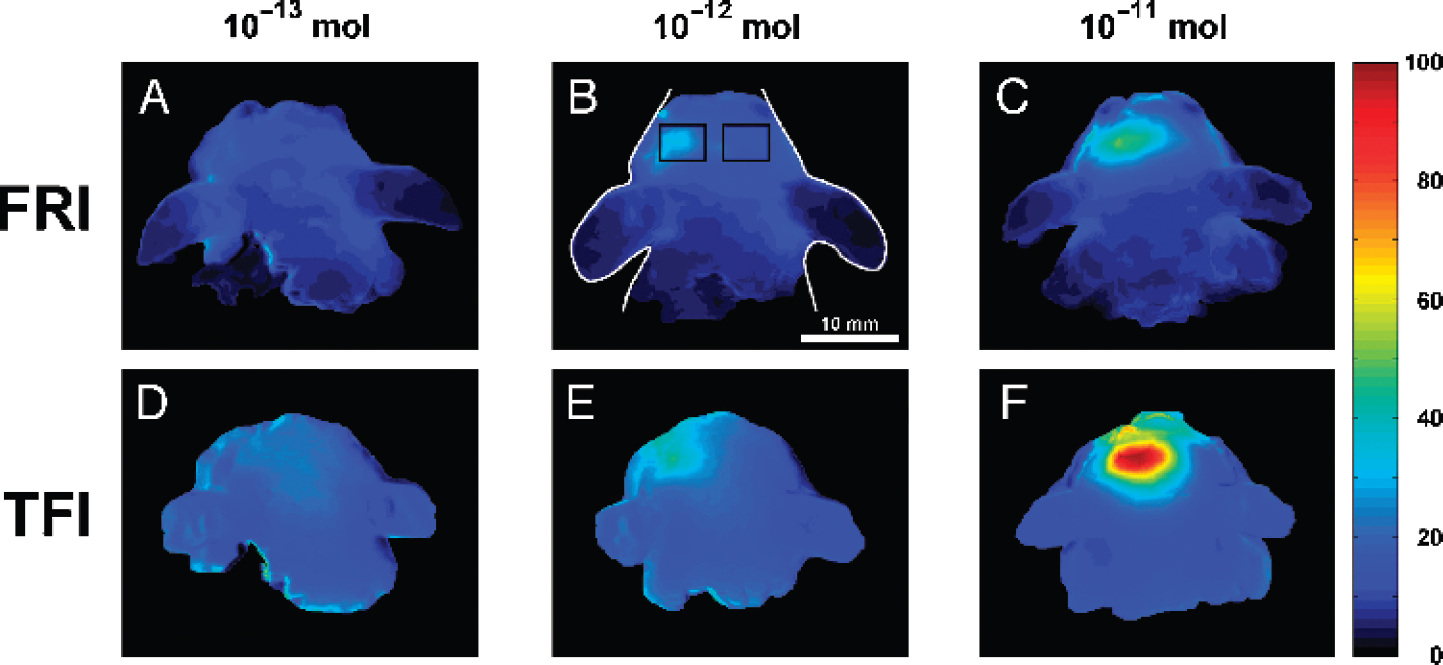
Figure 2 shows typical color-coded NIRF images (FRI and TFI) of the heads of mice implanted with capsules containing different amounts of NIRF dye (10−13, 10−12, and 10−11 mol Cy5.5). The fluorescent capsules with the lowest dye amount (10−13 mol) could not be detected with either FRI or TFI. The capsules containing 10−12 and 10−11 mol NIRF dye could be clearly identified with FRI and TFI.
In Figure 3, the results of the ROI analysis are illustrated by giving the target-to-background ratios. These were calculated by dividing the ROI values of the left hemisphere by the corresponding ROI values of the right hemisphere. The target-to-background ratios of the mice with capsules containing 10−13 mol are approximately 1 for both FRI and TFI. These values are significantly different (

Sensitivity to Background Fluorescence
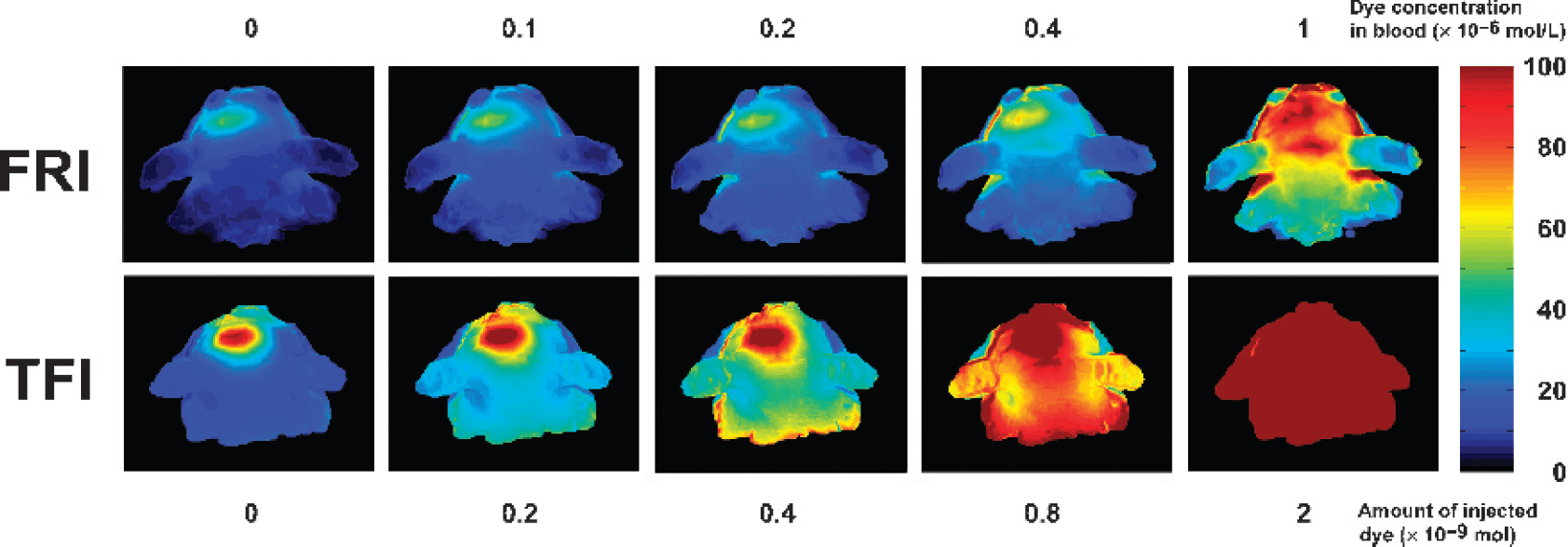
Figures 4 and 5 demonstrate an inverse relation between decreasing target-to-background ratios of mice with implanted NIRF dye capsules and increasing values of background fluorescence. This increase in background fluorescence was simulated by multiple intravenous injections of a long-circulating NIRF compound (Cy5.5-dextran) administered in incremental amounts of (0, 0.2, 0.4, 0.8, 2, 3.6, and 5.2) × 10−9 mol. Assuming a total blood volume of 2 mL per mouse, this corresponds to a blood concentration of (0, 0.1, 0.2, 0.4, 1, 1.8, and 2.6) × 10−6 mol/L, respectively. Figure 4 shows typical FRI (top) and TFI (bottom) images of an animal with an implanted capsule containing 10−11 mol Cy5.5 Scaling was maintained as in Figure 2 to allow for direct comparison. The images on the left were acquired before the injections. From left to right, the amount of dye in blood was increased. At a dye concentration of 0.4 × 10−6 mol/L, the capsule was still visible. When the dye concentration in blood was increased up to 1 × 10−6 mol/L, the capsules could no longer be detected. In Figure 5, the results of the ROI analysis are illustrated. The target-to-background ratios of TFI decrease with increasing dye concentrations, approximating a value of 1.

Discussion
NIRF imaging using fluorescent reporters is a promising technology for visualizing biological events noninvasively in small animals and potentially in clinical settings. In this context, our study demonstrates that fluorescent dyes within the brain of live pigmented mice can be detected with high sensitivity using NIRF imaging. Amounts as low as 10−12 mol can be visualized. This data is valuable for target selection in molecular imaging approaches in brain diseases. Given that the capsules can be precisely positioned and localized by MRI and because quantitative amounts of other signal molecules can also be included in the capsules, the presented phantom model might also provide a tool to evaluate and directly compare detection limits and sensitivity to background of other imaging modalities such as MRI or nuclear imaging methods. Moreover, the model can provide helpful data on how precisely signals can be located by diverse imaging systems and assist in the development of algorithms for image reconstruction in tomographic systems.
Several studies have previously used tubes filled with solutions of a fluorophore as phantoms to evaluate fluorescence imaging devices [10–12]. Fluorescent tubes have also been implanted into mice to account for the optical properties of tissue surrounding the fluorescent source [13,14]. In none of these studies were fluorescent objects implanted into the brains of live mice. The ability to detect a fluorescent object in vivo with an NIRF system depends on a number of parameters such as the spatial resolution of the imaging system, the depth of the fluorescent source, its dimensions, the amount of fluorescent molecules present, and the optical properties of the surrounding tissue. Therefore, these studies cannot be directly compared with ours.
Schulz et al. [13] inserted 40-mm-long glass tubes with a diameter of 2 mm (equal to a concentration of 2 × 10−6 mol/L) into the esophagus of euthanized mice. They showed that a fluorescent source in deep tissue layers can be located in a quantitative manner by using a tomographic fluorescence imaging system [13]. In a recent paper published by Graves et al. [14], fluorescent tubes filled with Cy5.5 dye (8 mm length, 1.5 mm inner diameter, 6 μL volume, fluorophore amounts in the range of 10−12 mol) were implanted subcutaneously into live nude mice to probe the performance of a tomographic NIRF imaging system. The paper demonstrates that superficially implanted capsules can be detected with quantitative accuracy [14]. In our study, capsules containing 10−12 mol Cy5.5 dye implanted deep into the brains of live pigmented mice can be clearly identified with FRI and TFI (see Figures 2 and 3). As shown in Figure 3, we observed a significant reduction of fluorescence yield when the amount of dye in the capsule was increased from 10−12 to 10−11 mol. A 10-fold increase leads to an increase in fluorescence intensity of about 2-fold in vivo as determined by analysis of fluorescence intensities in the region of the implanted capsules. This effect was also observed with solutions of the Cy5.5 dye in polyethene tubes (data not shown) and may likely be explained by quenching and reabsorption effects. Thus, when increasing the amount of dye in the capsule concentration from 10−12 to 10−11 mol, the target-to-background ratios are increasing only by 2. Nevertheless, when fluorochrome concentrations are equal to or less than 1 × 10−6 mol/L, the response of the NIRF imaging system is linear. The nonlinearity of the response at the highest concentration is solely due to quenching effects. Use of larger capsules to increase the amount of fluorochrome at lower dye concentrations to avoid quenching and reabsorption effects significantly increases the risk of compromising important brain and vital body functions and the risk of hemorrhage.
Figures 2 and 3 also show that TFI yielded a significantly higher target-to-background ratio than FRI at 10−11 mol, favoring the use of TFI as the mode of data acquisition when imaging the brain. This observation was recently made by Ntziachristos et al. [12] in phantoms and in in vivo mouse measurements using a different planar imaging setting. There might be several explanations for this phenomenon: Due to imperfections in blocking interference filters [15], the FRI technique leads to an excessive amount of excitation photons directly reflected on the skin towards the detector. When illuminating the head of a mouse from below, as in the TFI setting, the amount of excitation photons reaching the detector located above the head is significantly lower because of the long path of the photons through the absorbing tissue. Additionally, because the fluence impinging on the top of the head is significantly higher in the FRI setting, an enhanced autofluorescence signal from the endogenous chromophores in the skin is to be expected, thus reducing the contrast.
Graves et al. [14] tested the sensitivity of a tomographic system to background fluorescence by a single intravenous injection of 1 nmol Cy5.5-labeled annexin V in nude mice that were implanted with fluorescent tubes. They found that the sensitivity to background fluorescence can be counteracted by mathematical correction of the measured fluorescence intensities [14]. Substraction methods were also proposed by Gao et al. [16] as a promising approach to adaptively correct for background effects in a tomographic system. In our study, we probed the sensitivity of a planar NIRF imaging system to background fluorescence by subsequent intravenous injections of up to 5.2 × 10−9 mol of a long-circulating dye (Cy5.5-labeled dextran). One hour after a single dye injection, we found an overall dye loss from blood of about 10%, as estimated by the measurement of blood samples and the loss of signal intensity over the right hemisphere of the mice without a fluorescent capsule (data not shown). This loss might be due to the renal excretion of low molecular weight components in the injected solution or due to slight extravasation of the compound. Figures 4 and 5 show that relatively low background fluorescence (dye concentration in blood of 1 × 10−6 mol/L) can extinguish the signal. This means that given a blood volume of 2 mL per mouse, approximately 1% of the injected amount of a long-circulating fluorescent reporter must be accumulated at a target volume of about 0.1 mm3 in our system. From a different point of view, the concentration of dye in blood must be less than about 0.5% of the concentration at the target. However, these numbers are a low estimate due to the observed quenching effects within the capsule at 10−11 mol. The blood volume in the brain and in the surrounding tissue is comparatively high [17]. Therefore, the pharmacokinetic properties of the imaging agents must be carefully considered in fluorescence imaging approaches of targets within the brain. Compounds with a short blood half-life are preferably more suitable than long-circulating contrast agents. So-called activatable or “smart” imaging agents, which show almost no signal in their injected state and a high increase in signal intensity (activation) upon target interaction [18], seem to be a good choice. Furthermore, tomographic imaging systems might be less sensitive to background fluorescence than planar imaging systems [14].
In conclusion, highly sensitive detection of fluorochromes within brains of live mice can be attained with appropriate noninvasive NIRF imaging systems, encouraging imaging approaches in animal models of brain diseases with NIRF molecular reporters.
Footnotes
Abbreviations
Acknowledgments
We kindly acknowledge the technical assistance of Susanne Mueller from the Berlin NeuroImaging Center (BNIC), Charité Universitaetsmedizin, Berlin, Germany, in performing excellent MR images. RB and JK were funded by the Europaeischer Fond fuer regionale Entwicklung (EFRE). JS was supported by the Bundesministerium für Bildung und Wissenschaft in the Berlin NeuroImaging Center, and UD by the Herrman and Lilly Schilling Foundation.
