Abstract
A 1.5-year-old captive female Dama wallaby (Macropus eugenii) died after a 3-month period of progressive weight loss, anorexia, bloat, and diarrhea. Histopathologic examination revealed numerous Entamoeba histolytica trophozoites within the gastric mucosa and, less frequently, gastric submucosa and submucosal vessels. Immunofluorescent antibody testing confirmed the identity of the trophozoites as E. histolytica. The trophozoites were associated with mild glandular epithelial necrosis, mucosal erosions, and lymphoplasmacytic inflammation. E. histolytica most commonly causes necrotizing and ulcerative colitis in humans and captive nonhuman primates, and it causes necrotizing and ulcerative gastritis in nonhuman primates with sacculated stomachs adapted for leaf fermentation. Rare cases of gastric amebiasis also have been been reported in captive macropods, which also have complex sacculated stomachs. To our knowledge, this is the first report confirming E. histolytica as the cause of gastric amebiasis in a wallaby. The zoonotic potential of this infection in macropods is uncertain.
Entamoeba histolytica is a parasitic ameba whose trophozoites can cause necrotizing and ulcerative colitis and hepatic abscesses in humans and captive nonhuman primates. 1 , 5 , 15 The outcome of infection can vary tremendously from an unapparent carrier state to severe clinical manifestations, depending on the virulence of the strain of E. histolytica, host species, host nutritional status, host immune status, host intestinal microflora, and the presence of concurrent intestinal pathogens. 14 , 15 The life cycle is direct, and the typical source of infection is drinking water or food contaminated with infectious cysts. Excystation occurs in the colon, and the excysted amebae develop into trophozoites that usually reside in the colonic lumen but can invade the mucosa. The trophozoites also can invade mural blood vessels and lymphatics in the colon and spread to other organs, most commonly the liver. The invasive trophozoites are often associated with extensive necrosis in the colon and liver that is likely due to a combination of factors, including stimulation of inflammatory mediator production by host cells, neutrophil infiltration of affected tissues, cysteine protease production by the trophozoites, and induction of host cell apoptosis by the trophozoites. 14 Although E. histolytica most frequently affects humans and nonhuman primates, it also can cause necrotizing and ulcerative colitis in dogs and cats. 3 , 7 , 13 , 18 The source of infection for both captive nonhuman primates and companion animals is thought to be cysts shed from a human carrier, and in at least one case an infected dog was observed to drink water routinely from a toilet bowl. 18 Infected nonhuman primates can shed infectious cysts and transmit the disease to humans, although infected dogs rarely shed infectious cysts and are therefore of less concern to public health. 3 , 15 , 18
Erosive and ulcerative gastritis due to E. histolytica infection in colobus monkeys and a silver-leafed monkey has been described. 4 , 10 These primate species are leaf eaters with a complex, sacculated stomach adapted for fermentation. Presumably, the higher gastric pH of 5.0–6.7 in these monkeys allows E. histolytica excystation to occur in the stomach, and gastric amebiasis ensues. 10 Macropods also have a complex, sacculated stomach adapted for fermentation that is similar to the stomachs of leaf-eating monkeys. 9 The pH of the sacculated portion of the macropod stomach has been reported to range from 4.6 to 8.0 and from 5.6 to 6.5. 6 , 16 Rare cases of gastric amebiasis have been reported in captive macropods, and in one case E. histolytica was suspected. 2 , 8 , 12
A 1.5-year-old captive female Dama wallaby (Macropus eugenii) died after 3 months of progressive weight loss, anorexia, bloat, and diarrhea. The wallaby was housed in an outside pen with another wallaby. Both were born and raised in captivity. The wallabies were kept on a farm with numerous other wallabies and kangaroos. The penmate also had developed similar clinical signs and had died previously, but a necropsy had not been performed. Sulfa drugs and amprolium had been administered to the wallaby, but they had not resulted in any clinical improvement. Necropsy examination revealed poor body condition and a fluid-filled gastrointestinal tract. Multiple sections of the gastrointestinal tract and other viscera were submitted for histopathologic evaluation. In multiple sections of the stomach, numerous E. histolytica trophozoites had invaded the mucosa and displaced the gastric glands (Fig. 1). The trophozoites were approximately 15–50 μm in length and round, oval, or ameboid. The trophozoites had abundant, vacuolated, lightly basophilic cytoplasm, which occasionally contained phagocytosed plant material. Nuclei were slightly eccentric with peripheral chromatin, and in some a small central endosome was present (Fig. 2). Periodic acid–Schiff-positive granules were present in some trophozoites. The organisms had multifocally invaded the muscularis mucosa and also were present within the submucosa and rarely in the submucosal blood vessels and lymphatics (Fig. 3). Gastric gland epithelial cell necrosis was rarely present, and the mucosal epithelium overlying the invading trophozoites was eroded. Small numbers of lymphocytes, plasma cells, and neutrophils also were present among the trophozoites within the gastric mucosa. Trophozoites were not detected within other tissues submitted from the wallaby, including liver and colon. Indirect immunofluorescent antibody testing, as described, was performed using rabbit antiserum against E. histolytica, Acanthamoeba castellanii, Balamuthia mandrillaris, and Naegleria fowleri. 11 , 17 The trophozoites within the stomach exhibited positive immunofluorescence with the rabbit E. histolytica antiserum only (Fig. 4).
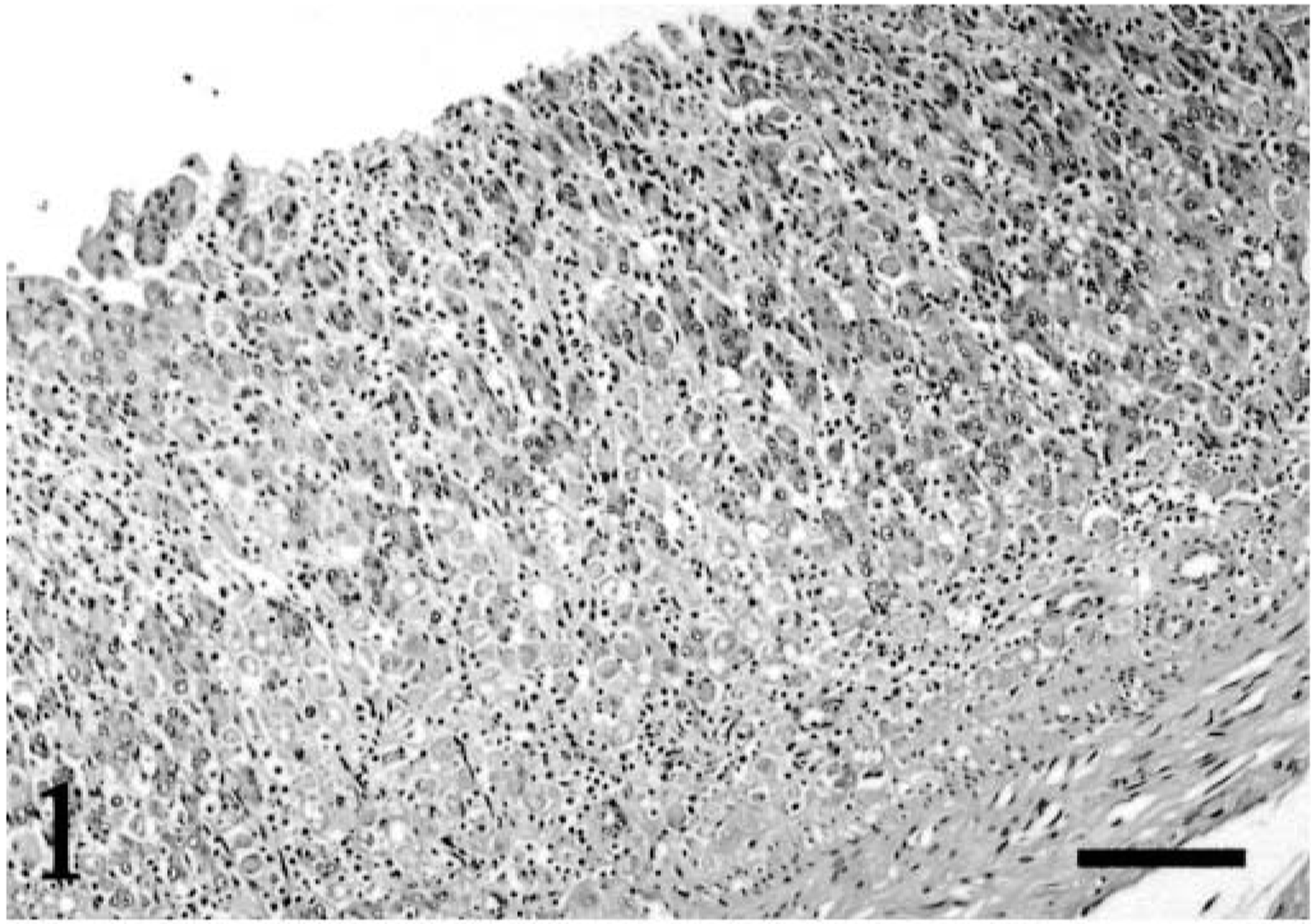
Stomach; Dama wallaby. Gastric glands are displaced by numerous E. histolytica trophozoites and inflammatory cells. The mucosal epithelium is eroded. HE. Bar = 100 μm.
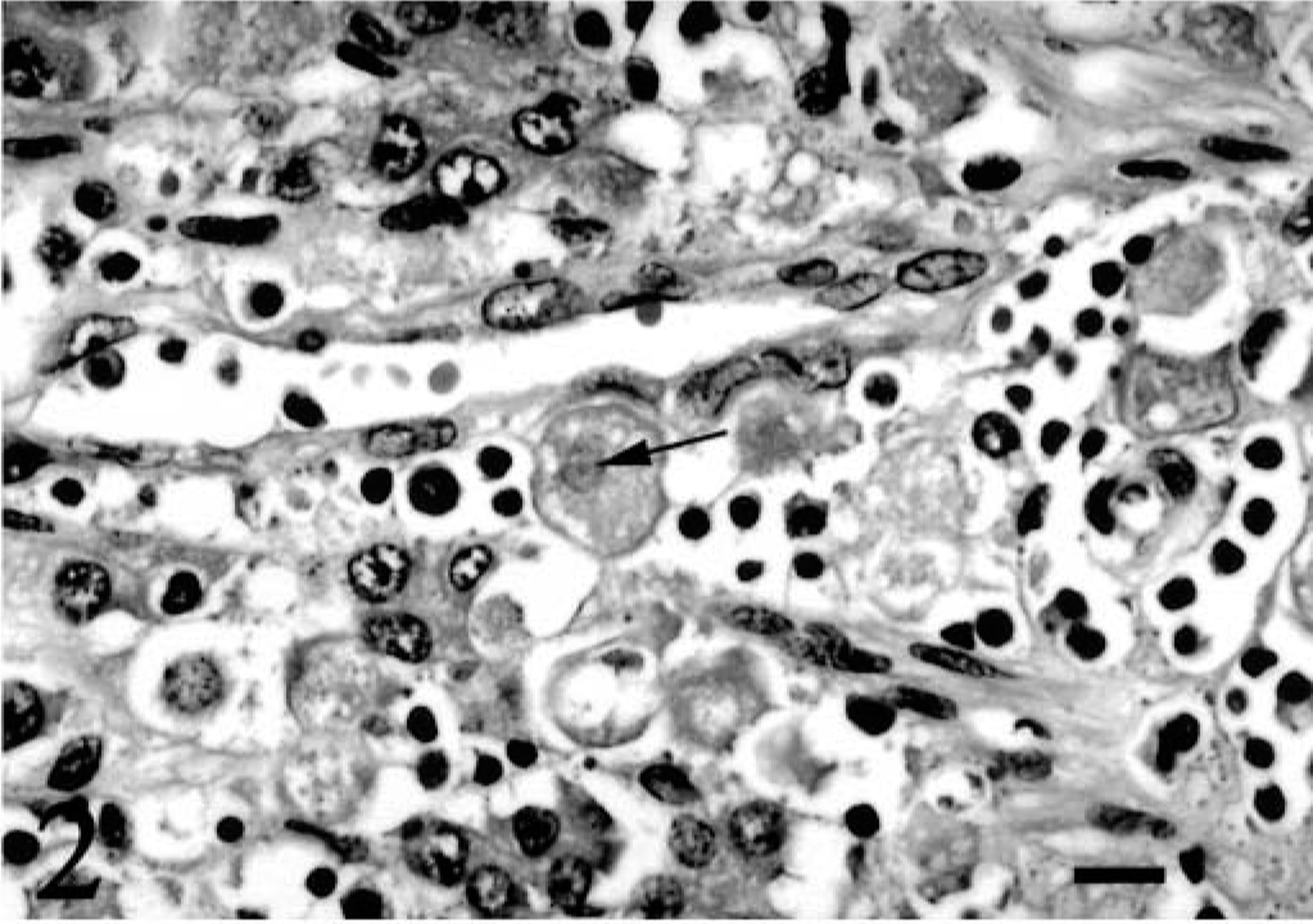
Stomach; Dama wallaby. E. histolytica trophozoites within the gastric lamina propria have abundant vacuolated cytoplasm. A small central endosome is present in the nucleus of one trophozoite (arrow). HE. Bar = 10 μm.
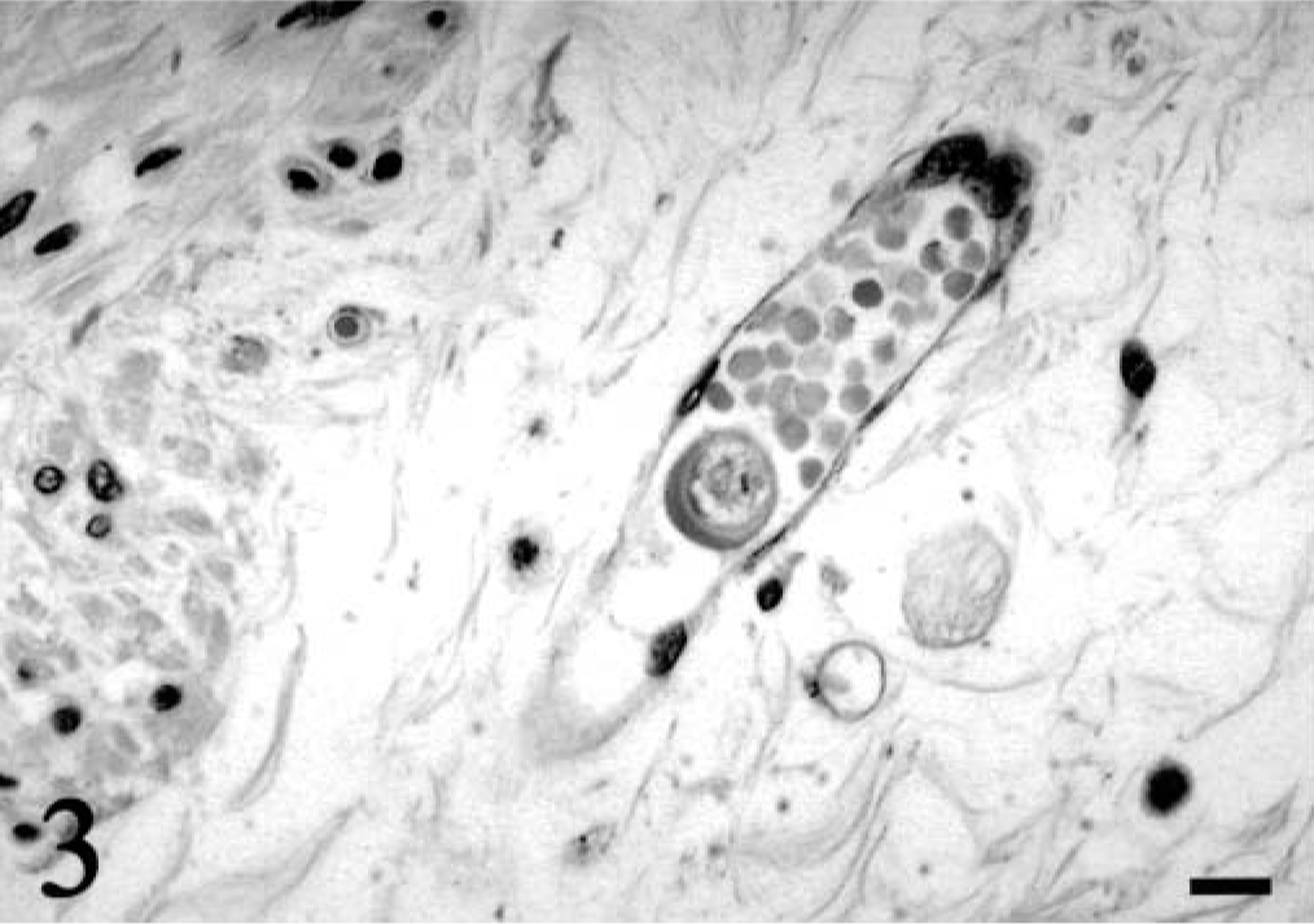
Stomach; Dama wallaby. A single E. histolytica trophozoite is present within the lumen of a submucosal blood vessel. HE. Bar = 10 μm.
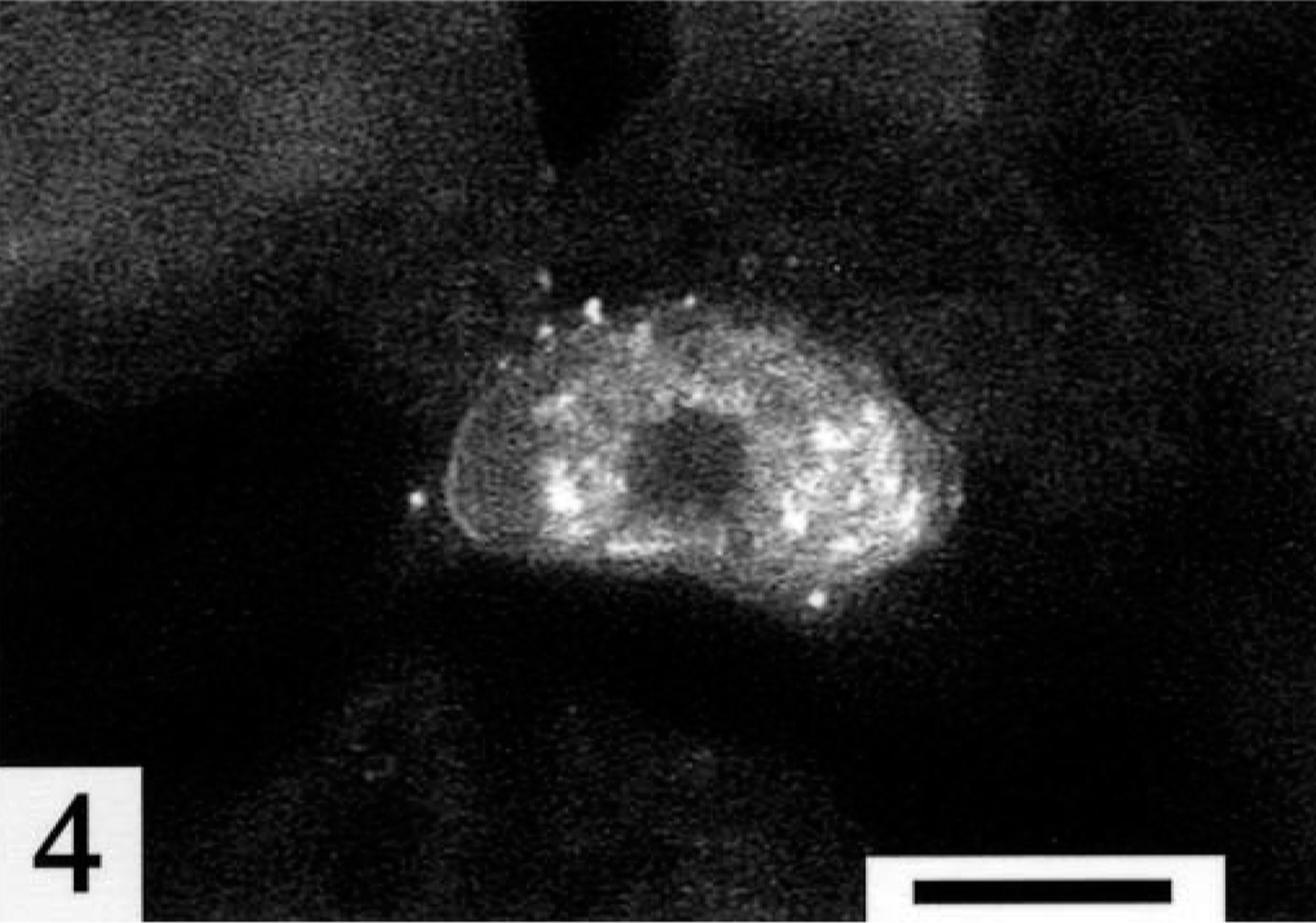
Stomach; Dama wallaby. An E. histolytica trophozoite exhibits positive immunofluorescent staining. Fluorescein-conjugated antirabbit IgG with polyclonal antiserum raised against E. histolytica trophozoites and cysts. Bar = 10 μm.
Amebiasis due to E. histolytica is most frequent in captive nonhuman primates, is occasionally found in companion animals, and is likely associated with extensive contact with human carriers. Captive propagation of macropods increases contact between humans and these animals. This captive wallaby most likely acquired infectious cysts from a human carrier. Alternatively, although its penmate was not necropsied, the similar clinical presentation suggests that the penmate also may have acquired amebiasis from a human carrier and may have been the source of the infectious cysts in this wallaby. Because macropods have a sacculated stomach, the manifestation of the infection as gastric amebiasis, which is similar to the infection in colobus and silver-leafed monkeys, is not surprising. The zoonotic potential of this infection in wallabies is uncertain. During an outbreak in colobus monkeys, an animal keeper developed amebiasis, presumably acquired from the monkeys. 4 In one report of gastric amebiasis in two captive wallaroos, cysts were detected in feces from the infected animals and the other macropods in contact with them. 12 Transmission from infected macropods to humans may be possible. Gastric amebiasis due to E. histolytica should be considered as a potentially zoonotic cause of gastrointestinal disease in captive macropods.
