Abstract
A patient case is provided that required debridement for a postoperative infection, following Achilles tendon rupture surgery, without tendon defect reconstruction. The tendon repair process in the defect was serially evaluated using sonography. Healing began in a doughnut-shaped pattern from the margins, where the paratenon-derived cells remained, and tendon continuity was restored, 4 weeks after debridement. At this point, the cast was switched to an Achilles tendon boot and full weight-bearing was allowed. The repair then progressed toward the center, and the tendon tissue completely replaced the defect at 16 weeks, which allowed the patient to gradually return to daily and sports activities, while wearing regular shoes. A longitudinal sonographic evaluation clarified the repair mechanism after debridement for postoperative Achilles tendon infection, with a large defect. It was also valuable for determining a safe postoperative treatment regimen.
Achilles tendon surgery carries a 2% to 3% risk of postoperative infection, 1 with steroid use, smoking, and diabetes identified as associated risk factors. 2 Postoperative infection of the Achilles tendon often necessitates tendon transfer or free flap surgery. 3 Recently, less invasive approaches have been reported, in which only the infected Achilles tendon is thoroughly debrided, and the remaining paratenon and fascia are sutured together. 4 The defect in the Achilles tendon following debridement is then filled postoperatively with fibrous tissue at 28 weeks 4 ; however, the process of tendon repair in these cases remains unknown, as a large defect in the Achilles tendon can be associated with poorer clinical outcomes during rehabilitation. 5 Therefore, it is essential to establish objective criteria to ensure the safe progression of rehabilitation.
Case Report
A 44-year-old man experienced discomfort in his right calf during a basketball game. He visited a nearby orthopedic clinic and underwent magnetic resonance imaging (MRI), examination, which revealed an Achilles tendon rupture. The patient was referred to the local hospital for surgery. Additionally, he had a history of autoimmune hepatitis and was taking 7.5 mg of prednisolone.
The Achilles tendon was evaluated using LOGIQ E10 ultrasound equipment system (GE Healthcare, Chicago, Illinois). and a L2-9-D, high-frequency linear transducer. The sonographic gain and depth were set to 60 dB and 4 cm, respectively. The focus was automatically maintained across the entire image, eliminating the need for focal zone adjustment. The patient was placed in the prone position, with the affected foot hanging off the end of the examination table, in a natural plantarflexed position. The acquisition and interpretation of sonographic images were performed by a single board-certified orthopedic surgeon, with over 5 years of experience in musculoskeletal sonography. The long-axis sonographic view showed that the ruptured area appeared hypoechoic (See Figure 1). This result was confirmed with a sagittal view, short tau inversion recovery, MRI image that showed a high-signal intensity area at the site of tendon rupture (See Figure 2). An open Achilles tendon repair was performed.
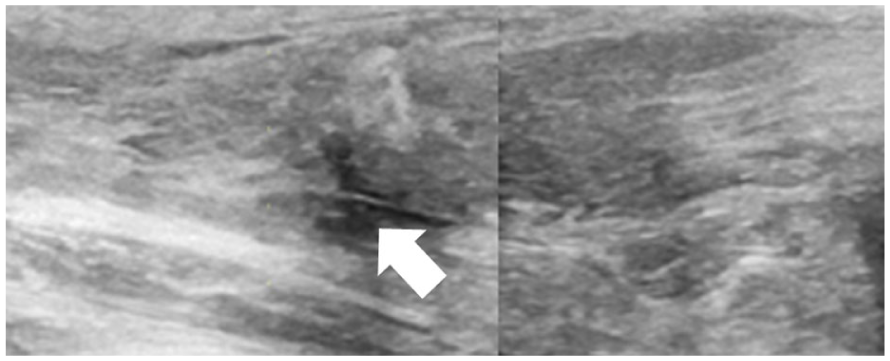
A long-axis sonographic view is provided of an Achilles tendon rupture. The arrow indicates the area of the ruptured Achilles tendon.
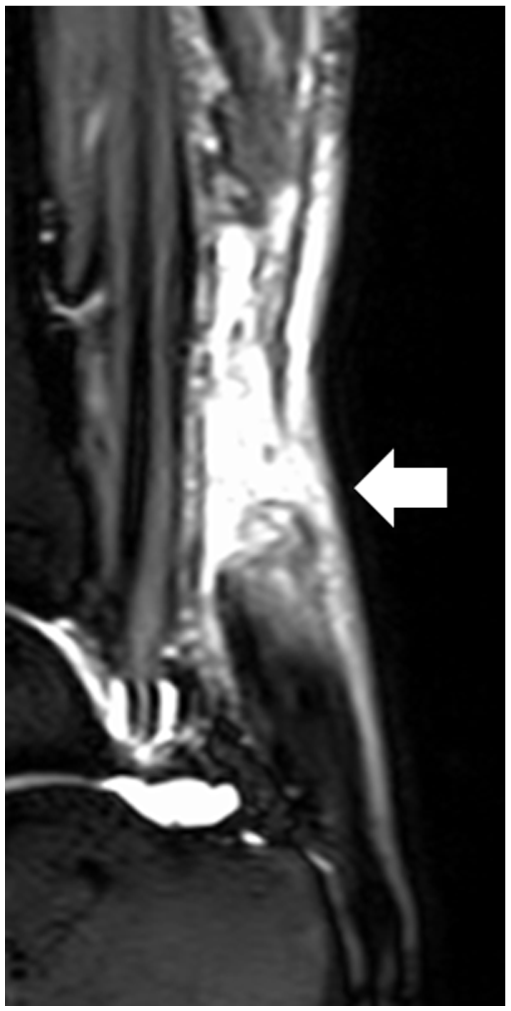
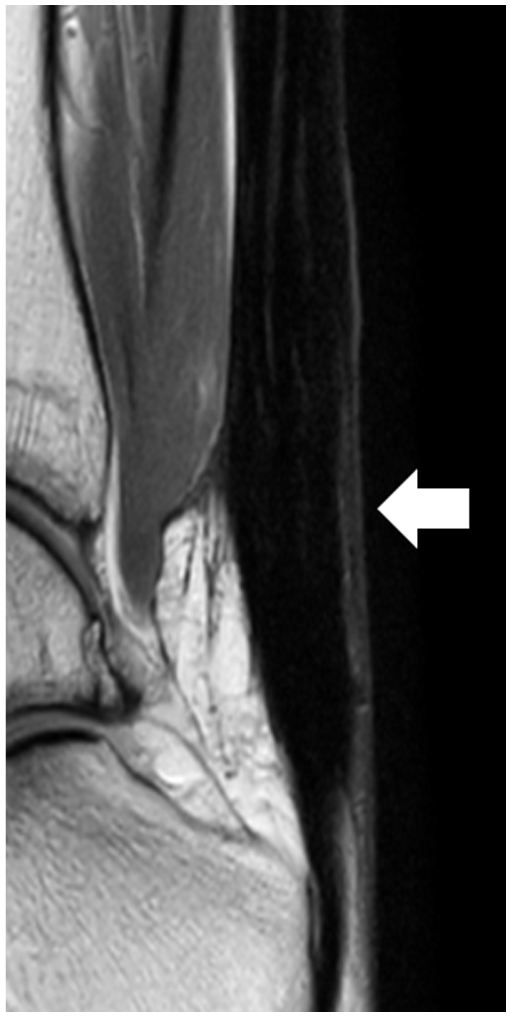
A sagittal, short tau inversion recovery MRI view is provided of an Achilles tendon rupture. The arrow indicates the area of the ruptured Achilles tendon.
Four weeks postoperatively, dehiscence of the surgical incision and purulent discharge were observed (See Figure 3A). The patient was admitted to the hospital with a diagnosis of postoperative infection, after Achilles tendon repair, and underwent emergency surgery. The infected Achilles tendon was exposed using an incision made during the previous surgery (See Figure 3B). All suture materials were removed, and the infected Achilles tendon was thoroughly debrided, leaving a 2.5 cm defect (See Figure 3C). The wound was closed by suturing the crural fascia and paratenon together.
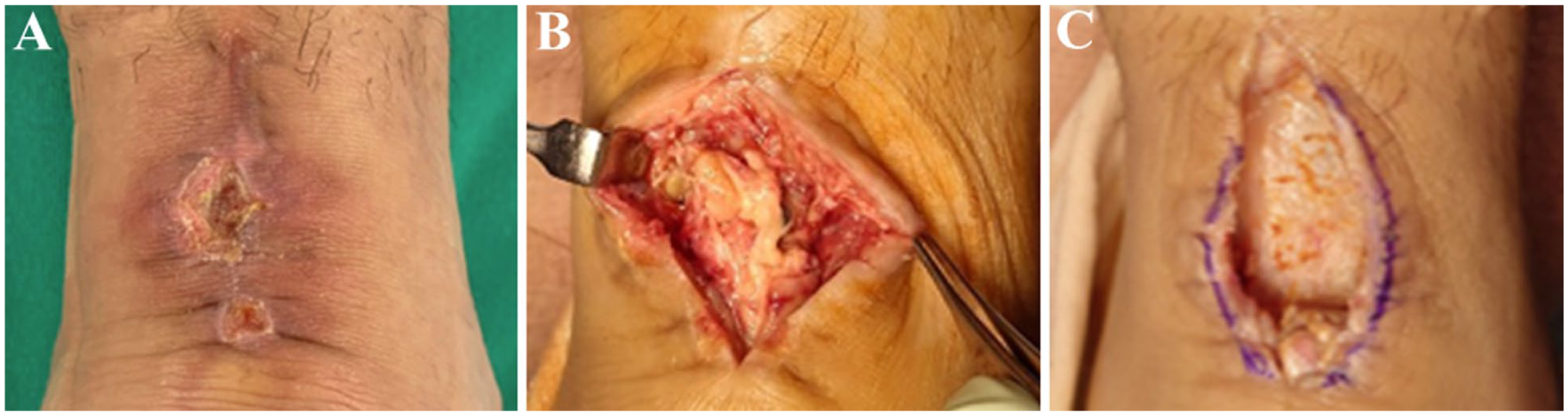
Documentation of a postoperative infection of the Achilles tendon and intraoperative findings are provided. (A) A wound dehiscence is observed at 4 weeks postoperatively. (B) An intraoperative view is provided that shows the infected Achilles tendon. (C) An intraoperative view is also provided after debridement, that demonstrates a tissue defect.
Postoperatively, the ankle was immobilized in a non-weight-bearing cast, with maximum plantar flexion. A short-axis sonographic view was taken 4 weeks after debridement, which showed doughnut-shaped scar tissue, forming from the outer margin of the tendon defect (See Figure 4A). The sonographic long-axis view confirmed the continuity of the proximal and distal tendon stumps (See Figure 4B). At this time, the cast was converted to an Achilles tendon boot, with wedged heel pads, and full weight-bearing was allowed. Subsequently, a sonogram was performed every 1 to 2 weeks that confirmed that the defect area was being filled (See Figure 4C and D), and the heel height of the Achilles tendon boot was gradually lowered. At 16 weeks postoperatively, the defect was filled with repaired tissue (See Figures 4E and F), and he returned to daily activities with regular shoes. At 20 weeks postoperatively, the patient was able to perform 20 single-heel raises and successfully returned to sports. At 48 weeks postoperatively, sonography confirmed a fibrillar pattern over the entire length of the Achilles tendon, indicating satisfactory repair (See Figure 4G and H). A proton-weighted MRI sagittal view depicted the tendon with a homogeneous low signal (See Figure 5). The Achilles tendon Total Rupture Score improved from 3 points preoperatively to 92 out of 100 points.
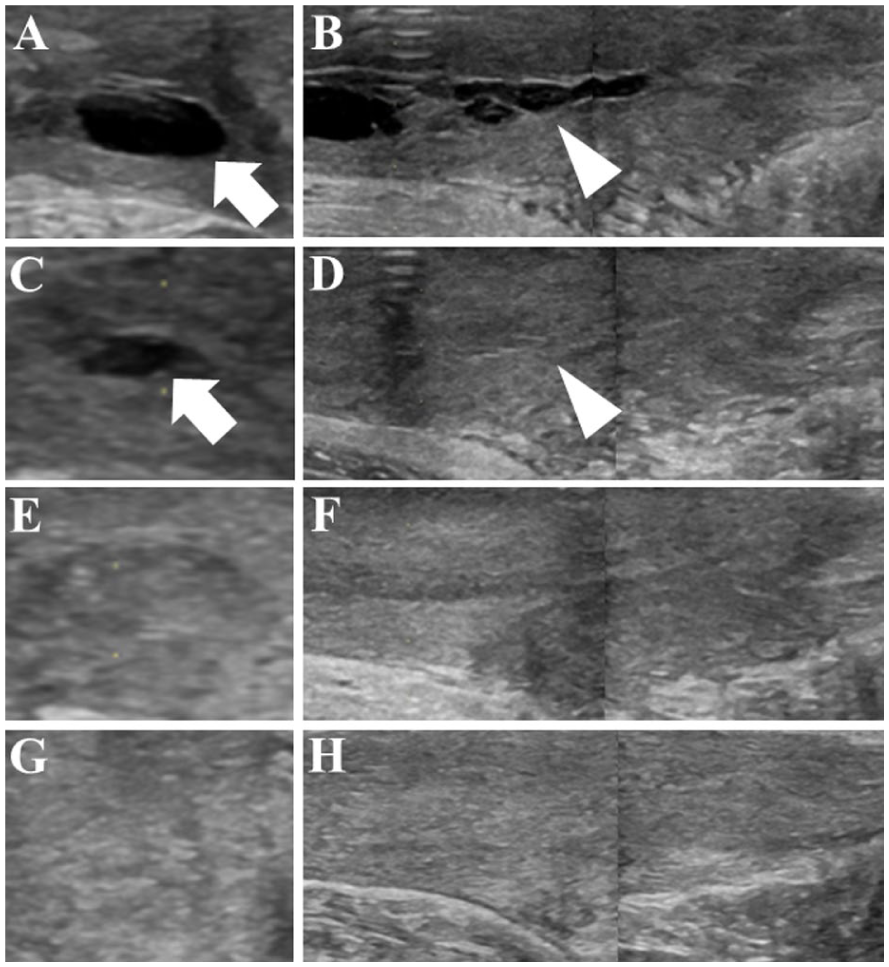
Sonographic images of the repair process of tissue defects in the Achilles tendon debridement. (A) The sonographic short-axis view is provided of the Achilles tendon. (B) The sonographic long-axis view is also provided of the Achilles tendon. These images were taken 4 weeks after debridement. The arrow and arrowhead indicate the defect after debridement. Scar tissue formed around the defect and connected the proximal and distal stumps. (C) The sonographic short-axis view is provided of the Achilles tendon. (D) The sonographic long-axis view is also provided of the Achilles tendon. These images were taken 8 weeks after debridement. The arrow and arrowhead indicate that scar tissue has proliferated and the defect area has decreased. (E) The sonographic short-axis view is provided of the Achilles tendon. D. The sonographic long-axis view is also provided of the Achilles tendon. These images were taken at 16 weeks after debridement. The defect is filled with scar tissue. (G) The sonographic short-axis view is provided of the Achilles tendon. (H) The sonographic long-axis view is also provided of the Achilles tendon at 48 weeks after debridement. A fibrillar pattern is noted that covers the entire length of the Achilles tendon.
A proton-weighted MRI sagittal view is provided that was taken 48 weeks after debridement. The arrow indicates the tendon with a homogeneous low signal radiowave.
Discussion
A debridement was performed for a postoperative Achilles tendon infection and conducted short-interval longitudinal observations of the resulting defect, thereby elucidating the tendon repair process through diagnostic imaging. Furthermore, by using sonographic images as objective indicators, it was possible to safely carry out his postoperative rehabilitation. It is likely novel that sonography was used to monitor large defects, after debridement, over short intervals of time. This case demonstrates the use of sonographic imaging as an objective indicator in postoperative rehabilitation.
In patients who underwent debridement, for postoperative Achilles tendon infections, it was possible to sonographically observe the resolving Achilles tendon defect, over short intervals of time. A previous study evaluated the Achilles tendon healing process in patients with Achilles tendon rupture, using MRI and sonography. In that study patients were imaged at postoperative intervals of 6, 12, and 24 months. 6 Serial observations, of the defect, were conducted every 1 to 2 weeks and showed a doughnut-shaped appearance of iso-echoic fibrous tissue. 6 To visualize this change, the transducer angulation was adjusted to avoid anisotropy and the use of hard acoustic couplant was helpful.
In the current patient case, favorable clinical results were achieved by advancing rehabilitation while referring to the sonographic images of tissue repair. Various rehabilitation protocols exist following Achilles tendon rupture repair, with some approaches emphasizing early weight-bearing and range-of-motion exercises. However, tendon elongation can occur in the early postoperative period, which may cause muscle weakness, range of motion limitations, and persistent functional impairment. 7 Therefore, rehabilitation needs to be conducted at the appropriate time. The use of sonographic findings as objective indicators of Achilles tendon repair is valuable in guiding the progression of rehabilitation.
The study patient was retreated with 7.5 mg oral steroids for autoimmune hepatitis. Steroids may impair tendon healing and decrease the mechanical strength of tendon tissue. 8 However, the specific steroid dose and duration that clearly delays Achilles tendon healing remains unclear. The steroid dose in the current patient case was relatively low, and the Achilles tendon defect was filled 16 weeks postoperatively, a finding that matches previous reporting. 5 These observations suggest that oral steroid dose may have had minimal influence on Achilles tendon healing, in this patient.
Conclusion
The defect resulting from debridement for postoperative infection, of the Achilles tendon, was evaluated with sonography, over a short time interval, thereby elucidating its repair process through imaging. Furthermore, sonographic images were provided as objective indicators for safely proceeding with rehabilitation after debridement. In the future, it will be necessary to gather more published cases to evaluate the detailed course of Achilles tendon repair after debridement.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval
Ethical approval for this study was waived by the research ethics committee of the Graduate School of Medicine, Chiba University, because it was considered a case report and all patient information was de-identified.
Informed Consent
Written informed consent was obtained from the subject(s) before the release of the report for review.
