Abstract
Objective:
To analyze how technical assistants benefit diagnostic medical sonography settings by improving efficiency and patient care.
Materials & Methods:
Credentialed obstetric sonographers who currently work in maternal fetal medicine were surveyed. Closed-ended and open-ended questions were used to examine effectiveness, usefulness, and overall satisfaction with the technical assistant position. In addition, quantitative methods were used to compare the time efficiency of technical assistants with medical assistants in obstetric settings.
Results:
The majority of sonographers and providers view technical assistants in a positive manner and indicated that the existence of the technical assistant role improved clinic flow. When compared with studies regarding medical assistant efficiency, this study showed shorter wait times for patients.
Conclusion:
The data supports that the presence of a technical assistant in clinic increases the overall efficiency of the clinic, which could allow providers to see more patients and reduce wait times for critical appointments. This could also lead to a more cost-effective system, especially when compared to alternative options such as hiring more providers or sonographers. These findings should encourage obstetric and gynecological sonography clinics to implement trained technical assistants to address clinic inefficiency, sonographer burnout, and sonographer and practitioner satisfaction.
A technical assistant (TA) provides support in administrative tasks and patient care for diagnostic medical sonographers. This position was created by BB Imaging, a mobile ultrasound company that provides services to clinics across Texas, Oklahoma, Kansas, and Missouri. The company specializes in maternal fetal medicine (MFM). The TA role was the first position implemented to serve as support for the sonographers at these clinics. The role came about after a time study was conducted. This study showed that 60% of the sonographer’s time was spent scanning (defined as the time holding the transducer) while the other 40% was spent on administrative tasks. These administrative tasks included triaging, reporting, invoicing, and setting up and turning over patient rooms. The TA role arose to address the administrative support the sonographers were lacking. By delegating the administrative tasks, leadership noticed clinics were scheduling more patients each day, charting errors were reduced, and billing and collection turnaround quickened.
TAs typically hold a bachelor’s degree or are enrolled to obtain that degree. Many want a career in health care and hope to gain experience in clinics and with patients. They are the first team member to arrive at the clinic and set up the patient rooms for the day. They triage patients, complete invoices, assist sonographers in completing patient reports, clean rooms, and input patient information between scans. Job duties vary at each clinic, depending on if it is a remote or central location. Remote clinics are in less populated areas and use telemedicine to communicate with the physician, while central clinics are in urban centers and typically have a physician on-site. At remote clinics, the TA acts as part of the front desk team by checking patients in and out, gathering necessary paperwork, ordering supplies, answering calls, and scheduling patients. Typically, these clinics are staffed with a minimum of one sonographer and one TA, and they serve patients that otherwise could not be seen at a larger, more distant facility.
It is important to note that while the role of a TA may closely mimic the role of a medical assistant in a primary care facility, the TA position does not require a medical certification or even previous health care experience. Medical assistants are generally found in primary care settings, and the position requires a certification. 1 Like TAs, medical assistants are used to decrease provider burnout, lower costs, and increase patient satisfaction. They aid in documentation, triaging, patient counseling, and identifying and contacting patients for preventative care. 1 In some clinics, a medical assistant will aid in minor procedures and physical exams and perform phlebotomy. Their roles at each clinic can vary greatly depending on the clinic and physician the medical assistant is working with. 1 For a TA, prior knowledge of medical terminology or experience in a health care setting is beneficial, but a successful TA has effective professional communication, attention to detail, critical thinking skills, and possesses strong computer literacy. During training, the TA will be taught applicable medical terminology, patient health information collection, triaging, and specific obstetric charting procedures. To aid in charting, the TA will view the incoming images and fill out information such as fetal and placental position in the report. This report is always verified by the sonographer before completion, but the assistance of a TA reduces the initial input time. Combining these soft skills and specific in-clinic sonography training forms the unique TA position. It is important to note that while this study is specific to MFM, TAs are trained for all sonography modalities.
This study sought to analyze the efficiency of TAs at BB Imaging by collecting insight from sonographers and physicians working in the industry. It also provided data on the impact that the TA position has on clinic effectiveness.
Materials and Methods
The data gathered to understand the role of a TA is a mixed-method study. Qualitative data was gathered through physician and sonographer surveys, while quantitative information came from detailed time studies. This information was collected from sonographers with experience ranging from 5 to 30 years.
Survey Data
An obstetric sonographer, as well as one of the coauthors, designed a survey to send to sonographers who work closely with TAs. 1 A member of the administrative team collaborated with the physicians to obtain their input. 2 The sonographer survey was composed of four open-ended questions and four closed-ended questions while the practitioner survey consisted of three open-ended questions. All closed-ended questions and open-ended questions are reported here.
Participants were invited to share their input in the survey through company e-mail. The survey link remained open for 3 weeks. The data were collected through the online survey tool SurveyMonkey. The survey participants consisted of 18 diagnostic medical sonographers, credentialed in obstetrics, who worked for BB Imaging, in Central Texas.
The questions solicited information on the view of TA roles from the perspective of their sonographer colleagues. These questions are presented in Table 1.
Questions Asked to Sonographers About Their View of Technical Assistants.

Abbreviation: TA, technical assistant.
Time-Study Data
To obtain a greater quantitative understanding of the impact a TA has on the efficiency of an obstetric clinic, information on appointment times was collected using past charts and scheduling information. Data from 100 sonograms performed in Central Texas were collected, including new patient anatomy imaging, new patient anatomy and fetal echocardiography, and primary fetal echocardiography. The dates of the examinations range from August 2019 to February 2020. The imaging studies were pulled from five clinics, one of which was a remote clinic and four central clinics. Remote clinics are clinics where only the TA and sonographer are present. The TA provides administrative support at this clinic, and telemedicine is used to communicate with the provider. Central clinics typically have a provider and an administrative team on site. They will often have nurses, and occasionally medical assistants present as well. This provides a holistic view of the most common exams performed and includes times with new patient paperwork.
Patient check-in and check-out times were monitored by eClincialWorks. This common clinical software system allowed researchers to obtain the total time of an appointment, including check-in, vitals, the sonogram, the physician’s consult, and check-out. Viewpoint, the dictation systems for the clinics studied, allowed researchers to calculate the length of the sonogram itself. Ultimately, accurate times for check-in to the start of the exam, exam length, and end of the exam to check-out were found. For this study, the focus is on the time from check in to start of the exam, total time in clinic, and the end of the exam to check-out.
To understand the implications of this data, the results are compared with similar studies which calculated the average wait time in similar clinics.
Results
Sonographer Opinions
Sonographers were asked an open-ended question about their views on the role of a TA when patients are present and when they are not. Sonographers agreed that the TA is very versatile and spends time in an administrative position and interact with patients. They help set up and wrap up for the day to allow sonographers to focus on their exams and charts. TAs maintain a clean and organized exam room while attending to the patient and sonographer needs. Sonographers also stated that TAs are essential in gathering patient information and setting the sonographer up for success.
Participants were asked what additional roles they would like to see TAs perform. From the survey, 55.56% of sonographers responded with not applicable or none. Others suggested TAs should take on a larger role in creating and implementing new ideas to improve clinic flow. They also suggested TAs assist more in patient exam reports.
Of the sonographers participating in this survey, 33.33% and 61.11% stated having a TA in the clinic helped with the overall efficiency a lot or a great amount, respectively, as compared with the 5.56% that believed the position only helped a little. These numbers are presented in Figure 1.
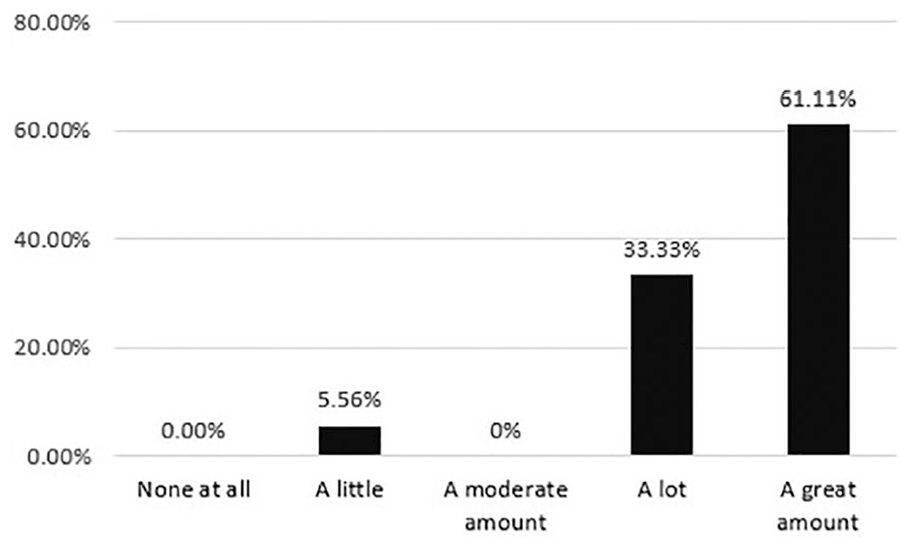
Sonographer opinion of how much the technical assistant aids in the efficiency of the clinic.
An open-ended question asking what words come to mind when thinking of the TA model supports this finding with 11 of 18 participants including “helpful” and 3 of 18 stating “efficiency” in their response. Other common responses were “time-saving” and “hard-working.”
Figure 2 shows the responses of sonographer opinions on if having a TA present helps decrease sonographer burnout, with 72.22% of the participants choosing strongly agree or agree, and 27.78% responding they neither agree nor disagree.
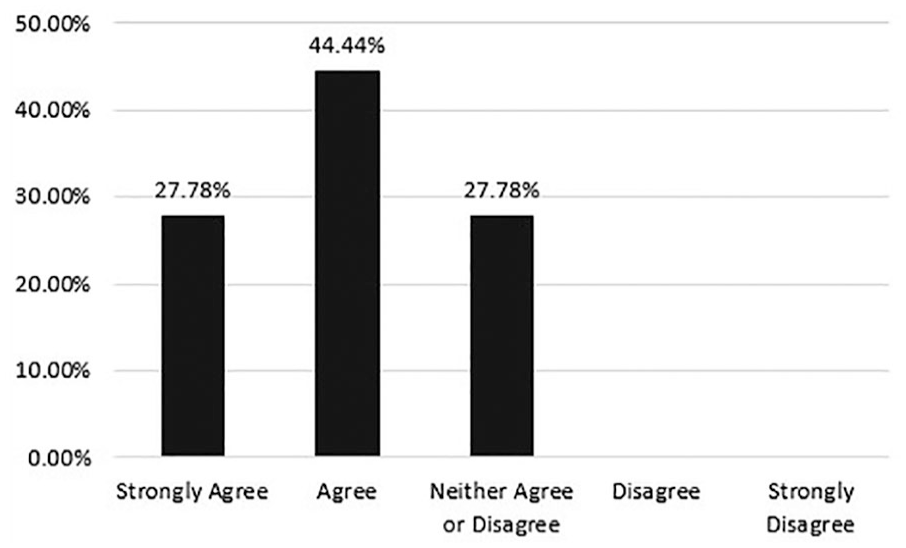
Sonographer opinion of how much a technical assistant reduces sonographer burnout.
When asked what characteristics make the best TA, common responses included hardworking, friendly, attentive, quick learner, self-starter, organized, and helpful. Sonographers agreed TAs are vital to the clinic running smoothly, especially in stressful situations that require flexibility. The sonographers also rely on TAs to complete exam documentation quickly and thoroughly.
Sonographer Satisfaction
Two of the eight survey questions explored the satisfaction of sonographers with the TA model. Participants were asked how satisfied they are with the current responsibilities of the TA. Of the 18 surveyed, 88.89% stated they are either very satisfied or satisfied with the TA’s current role, while 11.11% stated they are neither satisfied nor unsatisfied, as shown in Figure 3.
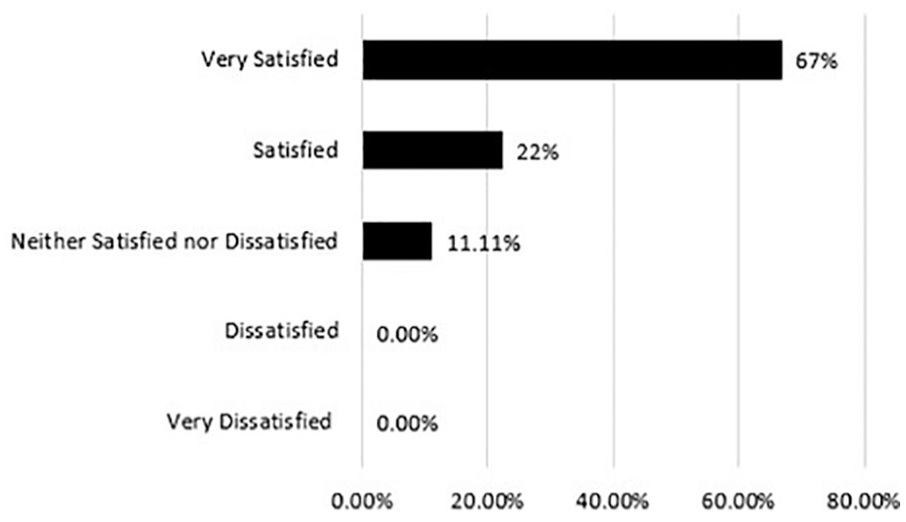
Sonographer satisfaction with the Technical Assistant model.
Additionally, sonographers were asked, “If applicable, how would you rate your experience when working without a technical assistant?” 22.22% of participants said this was not applicable to them. Of the remaining participants, the majority (38.89%) stated it was difficult or very difficult working without a TA. 16.67% said neither easy nor difficult and 16.67% said easy or very easy, although this does not account for whether the clinic is remote or, a central clinic would have additional support staff. The data of those who have worked without a TA are shown in Figure 4.
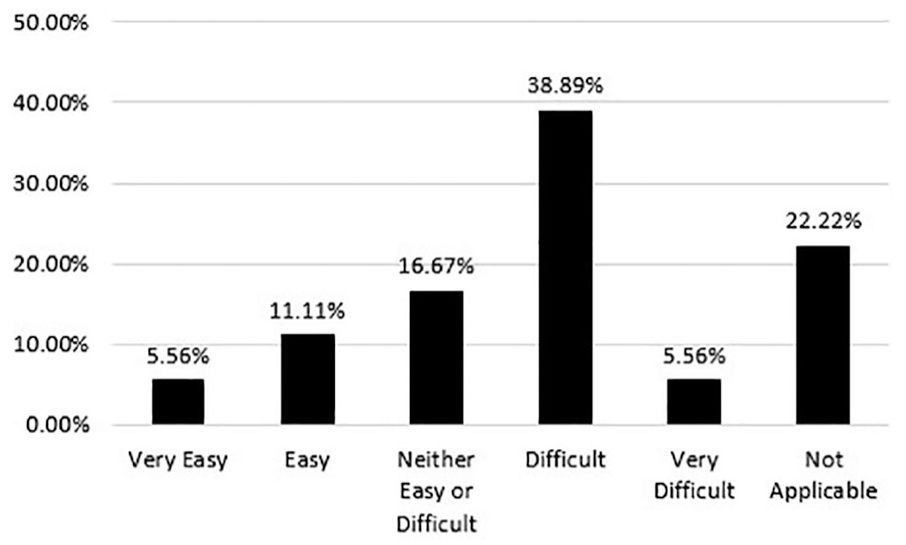
Sonographer’s experience working without a technical assistant.
Practitioner Opinions and Satisfaction
Three practitioners were interviewed in person, over the phone, or through e-mail. Two of the participants were physicians, specializing in obstetrics and gynecology, and one was a telemedicine nurse and clinical manager. All these practitioners regularly worked with a TA. All practitioners responded that they are satisfied with the TA role, with one stating “it helps us tremendously.” All participants agreed that the TA position adds efficiency and makes the day go smoother. The practitioners were asked what additional responsibilities they would like to see the TA assume. One participant stated there were no other responsibilities needed at the moment. Additional responses included Technical assistants could take charge of any duties associated with the telemedicine set up and inquire if there are any short-term or long-term changes that need to be implemented. They could ask if there is anything they can do to make the day go smoother on our end and communicate those updates to all parties to maximize team communication. At certain clinics, technical assistants should focus more on rooming patients and maximizing room usage than front-desk duties. They should prioritize keeping the behind-the-scenes of the clinic running as efficiently as possible.
When asked to comment on any differences in working at a clinic with a TA as compared to a clinic without a TA, two of the participants stated they did not notice a significant difference between clinics with or without a TA. One participant noted that the TA performs similar duties to medical assistants at the other clinics in which they worked. They also noticed that TAs do not perform a first trimester fingerstick for a blood sample, like a medical assistant, but this was not a problem. Another practitioner noted that clinical flow is smoother when a TA is present and allows for more efficiency.
Finally, practitioners were asked what characteristics make the best TA. Answers included [They have] an energetic and positive attitude. They interact with everyone in the clinic, so when that positivity spreads it makes for a pleasant day. A great TA shows initiative, has effective communication skills, and is a critical thinker. [My] top priority is efficiency, and the TA role can make a big impact in that regard. A great TA would be bubbly, friendly, willing to jump in and learn new things and help out at any time. They would also ask management before initiating any new processes. Communicate well and work as part of a team with [our] employees.
Time Study Results
The time study results echoed the majority of the responses from sonographers and physicians. Using the TA model, new patients waited an average of 18 minutes to be seen by a sonographer and total time spent in clinic averaged 77 minutes across all clinics studied. In the rural clinic studied, the average wait time per new patient was 10 minutes and the total average time spent in clinic was 76 minutes. In central clinics, the new patient wait time was averaged at 11 minutes and the average total time in clinic was 77 minutes. These results are compared with various time studies in similar clinical settings.
Discussion
This study offers important insight into the potential impacts of a TA on clinic effectiveness and sonographer satisfaction, in a MFM sonography setting. However, there are some limitations to note. The qualitative data was gathered from a small sample of sonographers and physicians only in a MFM setting. Additionally, the time study was a limited sample, including a relatively small number of scans at a few high-risk obstetric clinics, in Central Texas. It is suggested these findings provide the groundwork for other sonography clinics to implement the TA position and perform similar research before the results can be applied to the field of obstetrics at large.
The role of a TA mimics that of a medical assistant, although more obstetrics and gynecology knowledge is necessary. There are several commonalities between a TA and a medical assistant. TAs and medical assistants perform both administrative and clinical roles. 2 Despite the similarities, TAs do not require specific certifications, and their role is specific to sonography. The potential impact of the TA can be compared to that of a medical assistant in primary care clinics. Many studies have discussed the benefits of medical assistants, specifically for their cost effectiveness and efficiency by facilitating patient flow and impact on increasing patient satisfaction through shorter wait times. 3 One study, in particular, sought to find what combination of practitioners would yield the least amount of wait time between patients. They were able to reach their goal with scheduling changes and the addition of a medical assistant. 4
Waiting to see a provider can be a common obstacle in health care, but women waiting to see an OB/GYN have the longest wait time when compared to other specialties. These patients wait an average of almost 24 days before seeing an OB/GYN practitioner. 5 These providers see a limited number of patients per day. One way to increase that number is to decrease time spent in clinic, which could potentially lead to decreased wait times and higher patient satisfaction. One article surveyed common causes of patient dissatisfaction and found two major patient concerns were wait times and perception of cleanliness in the clinic. 6 A TA can address both these issues by taking over exam room cleaning duties to ensure cleanliness while allowing the sonographers more time to complete the ultrasound exam.
A literature review found wait times to be one of the most influential factors in patient satisfaction, even when considering the cost of treatment. 7 Another article indicated that waiting times and the environment patients are in can negatively impact a patient’s experience, with wait time ranked as the least satisfying aspect of patient experience. 8 In addition, the longer the patients spend waiting to be seen, the more negative the overall clinical experience is rated. 8
In a study where the most important aspect of patient satisfaction was being called into their appointment on time, the average wait time was calculated to be 51.6 minutes. The third highest cause of this large wait time was sonographer tasks in between patients. 9 The TA can remedy this by performing some of these tasks, such as collect patient history or begin charting, while the sonographer is with a patient. Ultimately, more sonographers were introduced to solve this problem, and all patients were seen within the set goal of 30 minutes. 9 Since the average hourly pay of a sonographer is $34.41 in Texas, when compared to hiring a TA at $11 to $13 an hour, hiring more sonographers is much less cost-effective and still has a much higher wait time than the average time of 18 minutes in a clinic with a TA. 10
Shipman and Sinsky addressed the concerns of cost-effectiveness when trying to increase clinic efficiency. One of the most cost-effective options for increasing clinic flow was hiring a medical assistant. 11 This allowed the practitioner to focus more on visits while the medical assistant maintained communication between all parties and handled medial tasks. One clinic in the study found this saved the physician 30 minutes a day, allowing them to see more patients. 11
When addressing sonographer burnout, one study breaks down the pressure of sonographers to perform more examinations per day, without considering non-imaging tasks or rest. 12 They reference a study by Stewart et al 13 that found 37% of the sonographer’s time was spent with non-imaging tasks such as room cleanup and data entry. This dramatic split of sonographer time is important when it comes to preventing burnout. Burnout is a concern for health care workers and occurs when constant stress makes it unattainable to meet work demands. There are several sources of burnout, including high work demand and emotional cases. 14 TAs could be utilized to combat burnout due to high work demand by addressing non-imaging tasks. This could allow sonographers more time to interact with patients.
Finally, one study in an obstetrics and gynecology clinic with a medical assistant was compared to time study results from this research. The comparison study’s initial times were used rather than the times recorded after the author’s recommendations were implemented. In addition, the collected data only showed new patient information because the TA plays a vital role with new patient paperwork and patient history. Therefore, established or quick visits were not compared. In their study, new patients averaged 21.5 minutes to be seen by a sonographer and an average of 108.39 minutes total in the clinic, as compared to 18 minutes and 77 minutes in this study, respectively. 15 An additional study showed similar time discrepancies with 34 minutes as the average wait time and 169 minutes for the average total visit time. Even after interventions, such as more appointments, better computer access, and outpatient appointments, the average time for both wait time and total visit time only decreased by 1 minute. 16 This indicates that a TA could increase clinic efficiency by decreasing patient wait times when compared with similar obstetric sonography clinics.
Conclusion
The research conducted supports the theory that patients spend less time in MFM clinics when there is a TA present. In addition to medical assistant duties, TAs can aid in sonographer charting to allow information to reach the physician more quickly. The research also suggests that implementing a TA role in sonography can increase clinic efficiency by lessening sonographer burnout, as well as increasing sonographer, and practitioner satisfaction. TAs can provide a more cost-effective option than alternative solutions. While study is limited to MFM settings, TAs can be utilized across other sonography specialties, further research is suggested.
Footnotes
Acknowledgements
The authors thank Ben Buentipo, MS, RDMS, Co-Founder of BB Imaging and Consulting, Molly Siemens, RDMS, RVT, Mollie Morgan, Mandi Bowen, BS, RDMS, RVT, Geena Buentipo, Amanda Fraraccio, Jessica Kennedy, and Bella Mullen-Wright-Crowe.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
