Abstract
Study Design
Case Report.
Objective
To present a case of a previous complicated mandibular orthognathic surgery that aimed to setback the mandible in a female cleft lip and palate (CLP) patient, which led to bone necrosis on one side with subsequent severe mandibular deviation and facial asymmetry. We additionally reviewed the previous reports of similar complications, the pathophysiology and the factors that could lead to this dreadful result.
Method
A 27-year-old female patient presented with a severe dentofacial deformity secondary to a complicated bilateral sagittal split ramus osteotomy performed five years earlier, which resulted in aseptic bone necrosis on the right side. The patient had marked mandibular deviation, chin and midface retrusion and a pronounced occlusal discrepancy. Imaging demonstrated a bony defect at the right mandibular angle with a superiorly displaced proximal segment. Deviation of the mandible was corrected first by performing vertical ramus subsigmoid osteotomy (RSO) on the left side. The right bone defect was then reconstructed with a reconstruction plate and bone grafting. Maxillary and chin advancement was performed at a second stage.
Results
On follow-up, the patient shows a significant improvement in facial esthetics and mandibular symmetry and is currently under orthodontic management to enhance the occlusal relationship.
Conclusion
Bone necrosis is a rare but dreaded problem in orthognathic surgery. Minimizing the musculo-periosteal dissection and competent execution of the bone osteotomy is substantially effective in reducing the risk of bone ischemia and necrosis.
Keywords
Introduction
Orthognathic surgery is the standard method for treating a wide range of congenital, developmental, and acquired dentofacial deformities. These deformities have deleterious effects on the orofacial esthetics and function and are often associated with a negative impact on the patients’ psychosocial life and mental health. 1 The goal is to reposition the jawbones for harmonious facial aesthetics, normal oral and facial functions and improve patients’ overall quality of life. Surgeons should pursue these goals and reduce the risk of complications through thorough patient assessment and careful preoperative planning. According to a review by Panula et al., a variety of complications can occur during surgery or the postoperative period, such as hemorrhage and sensorineural deficits as the most serious and frequent complications, respectively. Additional to less common problems such as those related to the temporomandibular joint (TMJ), condyle position, relapse and infection. 2 Postoperative loss of hard and soft tissue is another rare but deleterious complication reported following maxillary or mandibular surgeries and typically attributed to vascular compromise. 3 In the modern practice of mandibular orthognathic surgery, this incident is rarely encountered and often secondary to genioplasty and ramus subsigmoid osteotomy (RSO).4,5,6 To our knowledge, no cases of avascular bone necrosis following sagittal split osteotomy (SSO) have been reported for three decades. 7 That is mainly due to the advancements and modifications in the surgical procedure that led to improvement in the healing process, and the greater understanding of the significance of conservative reflection of soft tissues on the perfusion of bone fragments.8,9 In this article, we present a case of complicated orthognathic surgery that aimed to setback the mandible in a female cleft lip and palate (CLP) patient, which led to bone necrosis on one side with subsequent severe mandibular deviation and facial asymmetry. We also reviewed the previous reports of avascular necrosis secondary to SSO, the pathophysiology, and the factors that could lead to this dreadful complication.
Case Presentation
A 27-year-old female patient presented to the Oral and Maxillofacial Clinic at our institute with facial asymmetry and mandibular deviation. The current complaint occurred following a mandibular orthognathic surgery performed at another hospital five years ago. According to the patient records, the surgeon had attempted to treat the skeletal cl III discrepancy and setback the lower jaw by SSO procedure. An orthopantomogram following the initial surgery demonstrates evidence of bone separation distally at the angle of the mandible with a non-rigid fixation of proximal and distal bone segments by interosseous and intermaxillary wiring (Figure 1). The mandibular deviation occurred within two months afterward, following the release of the jaw immobilization. The patient reported numbness affecting the lower lip on the right side while denied any history of purulent discharge, swelling, or pain during the postoperative period. In a second procedure, debridement of the right surgical site was performed, through a cutaneous incision. The medical history was negative for relevant medical diseases, and surgeries for the CLP repair and alveolar bone grafting were carried out earlier in life. Orthopantomogram of the patient following the initial surgical intervention.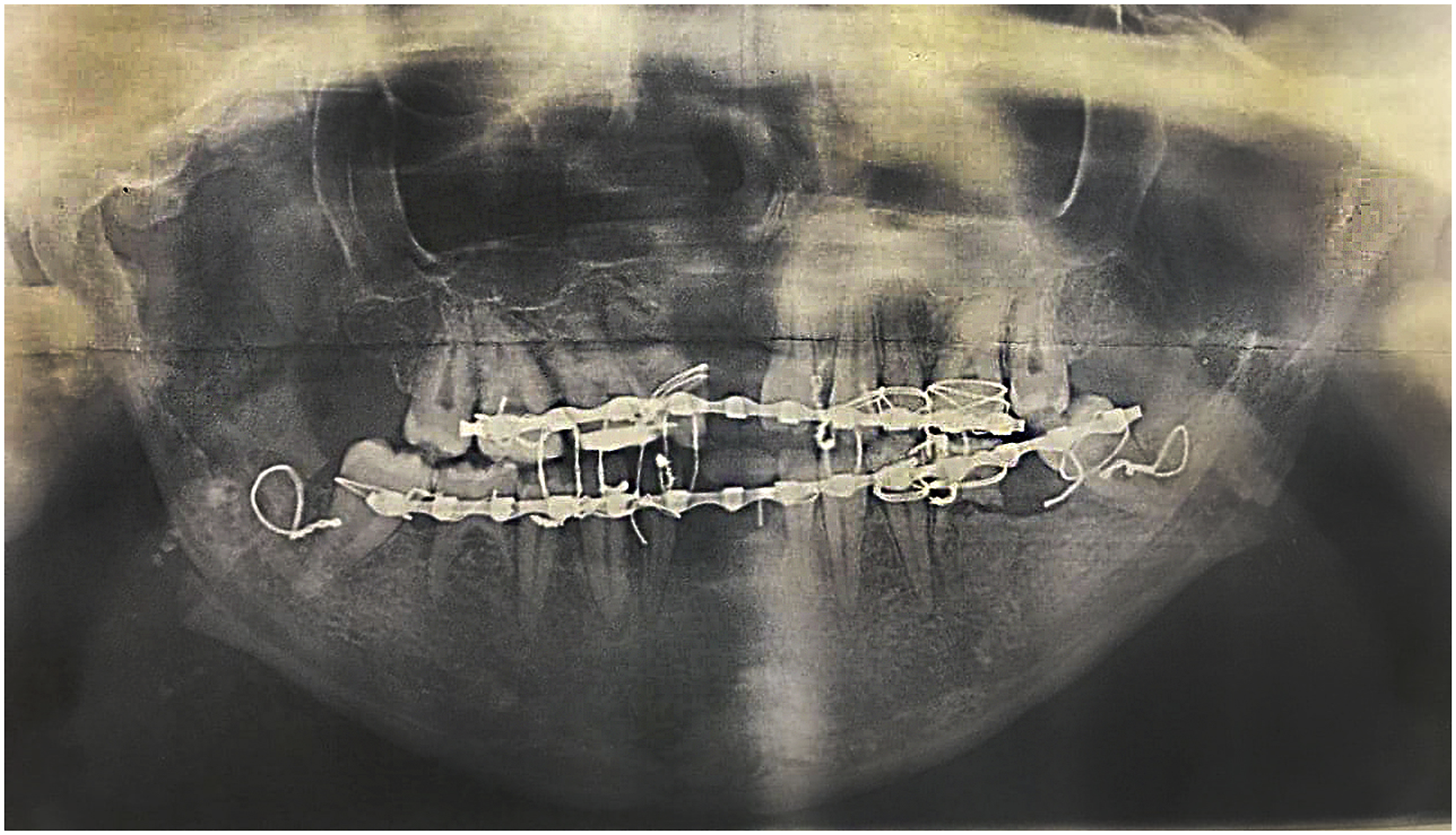
Clinical evaluation revealed a shift of the mandible toward the right side with significant retrogenia, and lip incompetence. The midface showed marked retrusion with poor lip support. A significant occlusal discrepancy was evident, complicated by the cleft discrepancy, the jaw deviation, and the missing dentition. Computed tomography (CT) scan demonstrates the extent of the skeletal discrepancy, in addition to the discontinuity defect at the right mandibular angle, with bone resorption involving the displaced proximal segment (Figure 2). The clinical and radiographic appearance of the patient demonstrating the extent of the dentofacial and skeletal deformity.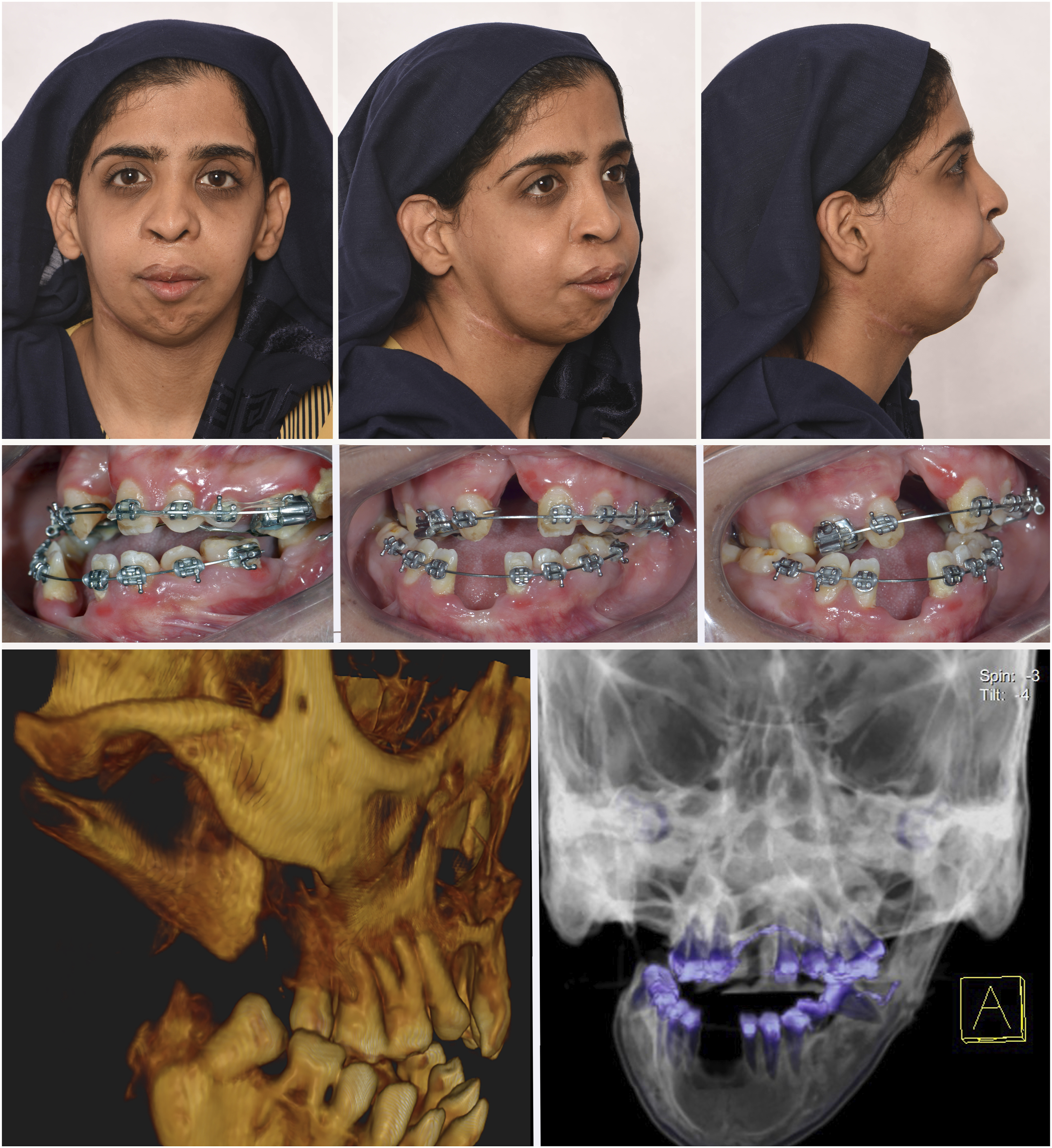
We planned to correct the lower jaw deviation first, by performing RSO on the left side and reconstructing the discontinuity defect with bone grafting and reconstruction plate. Maxillary Lefort I advancement and genioplasty were planned to be performed at a second stage.
Segmentation of CT DICOM data was performed using Mimics (Materialise, Leuven, BE) and converted to a 3D model. Additionally, the plaster models scanned individually, and in the planned final occlusion using a 3D scanner. Freeform plus (Geomagic, 3d Systems, USA; 2019) was used for VSP. The jaws osteotomies were designed, and the mandibular shift was then corrected by aligning the dentate segment of the lower jaw with the maxilla in the final occlusion. Correction of the maxillary position then followed according to the plan in the three dimensions. A mirror image was generated and used as a guide for repositioning the displaced proximal segment of the mandible and reconstruction of the discontinuity defect on the right side. Surgical wafers were finally designed and fabricated. (Figure 3). Virtual surgical planning.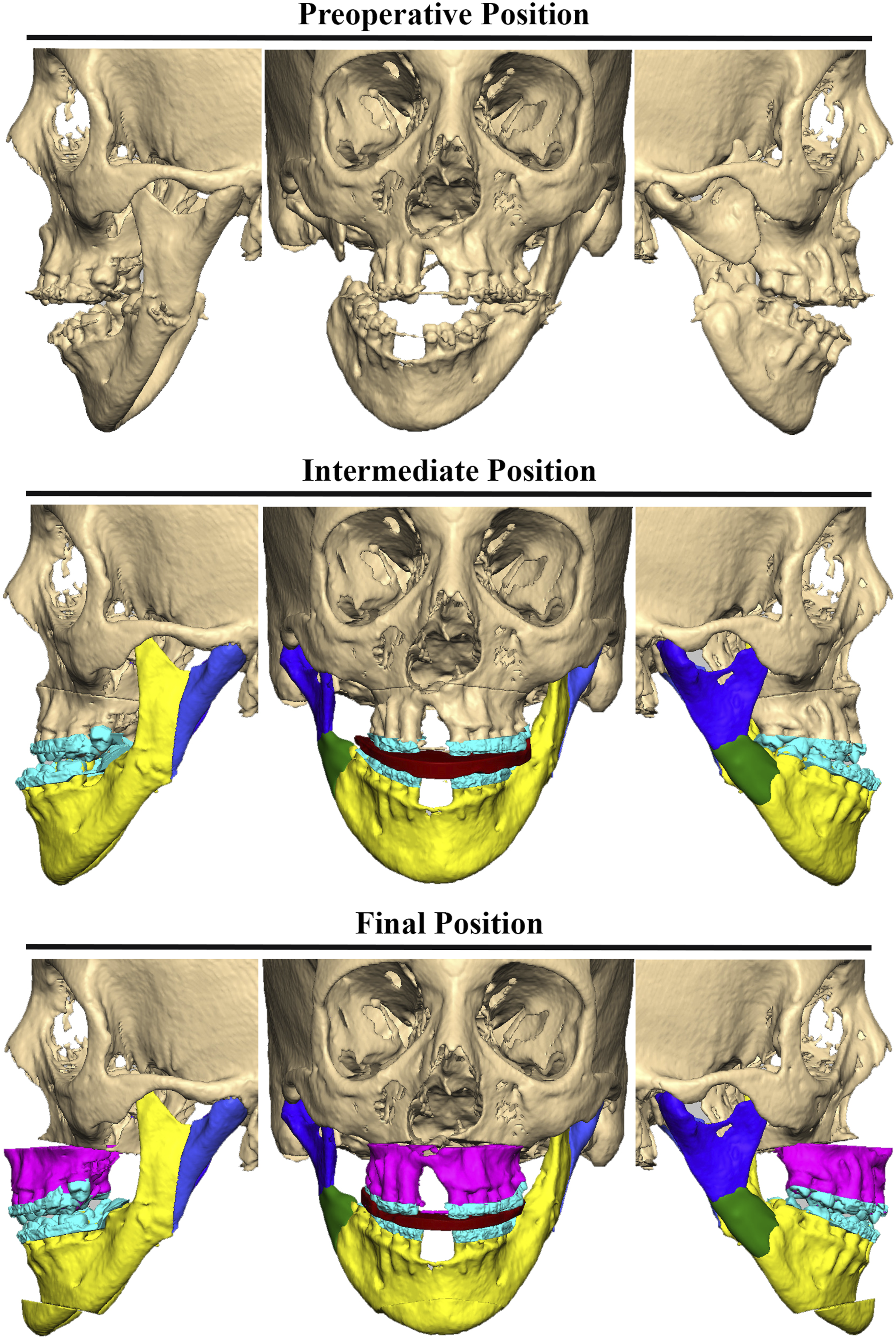
A submandibular incision was used to gain access to the mandibular defect on the right side and exposure of the proximal and distal bone stumps with excision of the surrounding fibrous tissue. Left RSO was then performed and the mandible secured in position guided by the intermediate wafer. A prebent reconstruction plate with a non-vascularized block of iliac bone graft was applied to the defect. Lefort I advancement with bone graft augmentation of the alveolar cleft defect and genioplasty were performed at a second stage 3 months later. (Figure 4) The surgical procedure. A: reconstruction of the right discontinuity defect with load-bearing plate and bone grafting. B: Lefort I advancement with augmentation of the bone defect sites using bone graft and platelet-rich fibrin.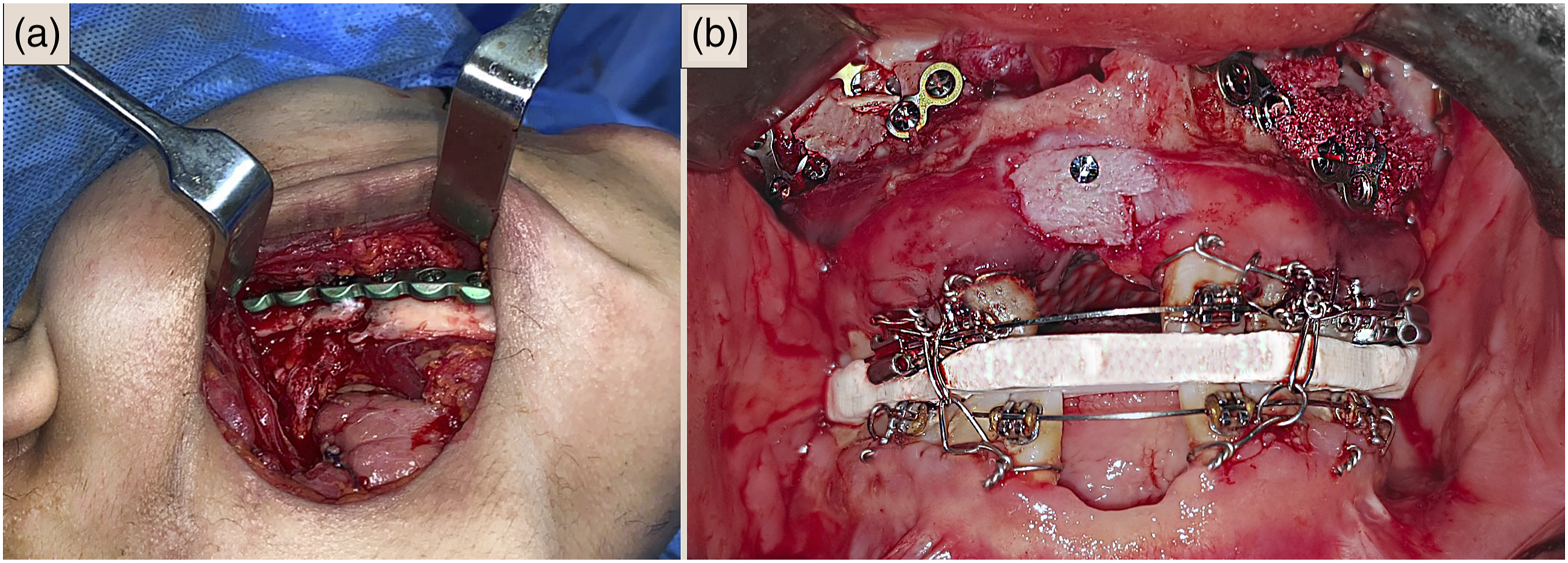
Two years postoperatively, the patient is currently showing a significant improvement in facial symmetry and overall appearance. However, an open bite developed subsequently on follow-up, which is currently under orthodontic management. The orthopantomogram demonstrates enhanced jaw relationship and mandibular positioning. (Figure 5). The main scope of our surgery was to initially correct the severe skeletal discrepancy and improve the patient’s quality of life. However, further interventions regarding orthodontic optimization of occlusion, prosthetic rehabilitation and soft tissue esthetic surgeries are required to enhance the result. The postoperative clinical and radiographic appearance of the patient.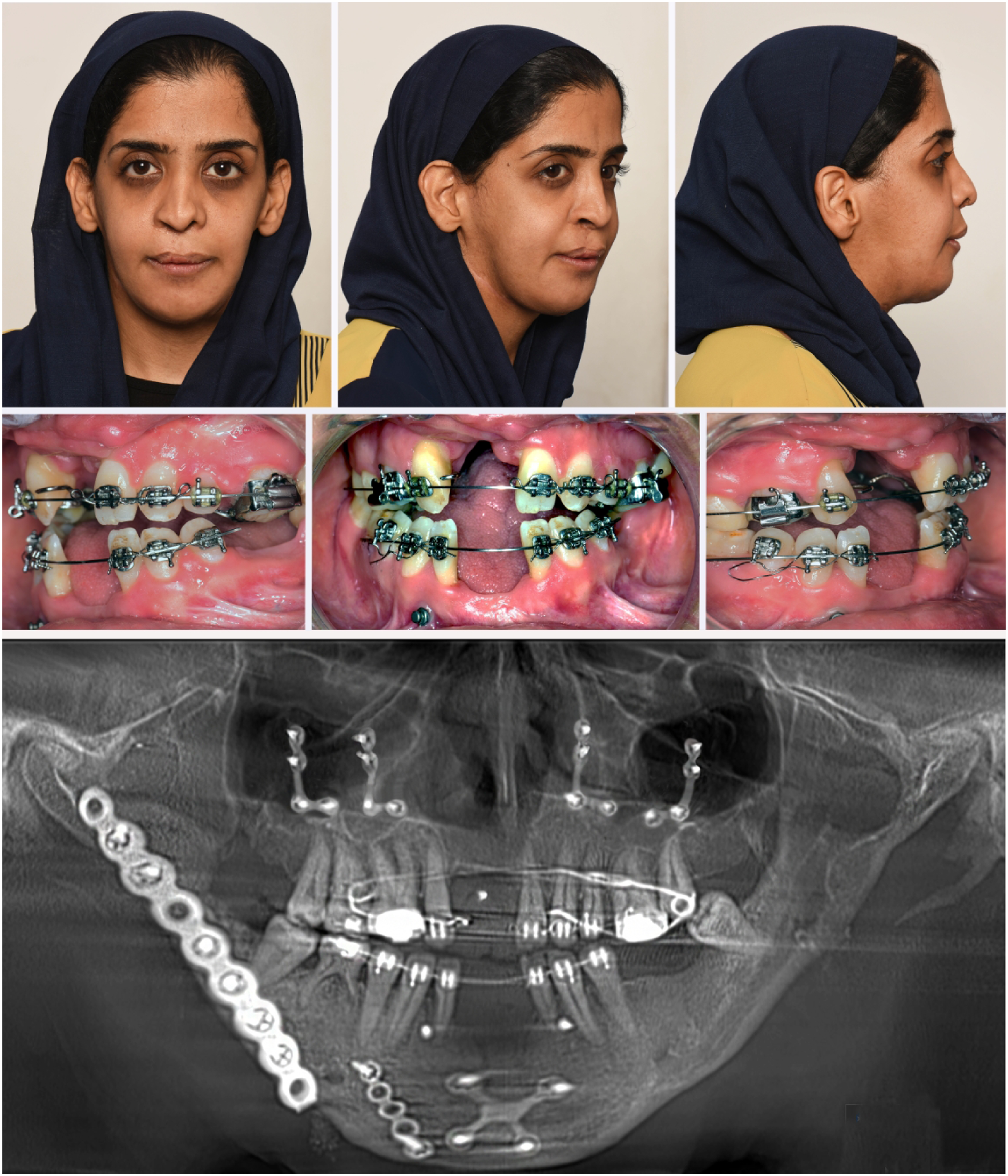
Discussion
In this article, we reported a case of a complicated corrective jaw surgery performed previously to setback the mandible in a CLP patient and resulted in compromised healing and necrosis of bone segment on one side with subsequent severe jaw deviation. Among several types of bone osteotomies, SSO is the most versatile and commonly performed procedure for correcting the lower jaw discrepancies. 10 However, in this case, the initial surgery aimed to setback the mandible to treat the cl III skeletal malformation in a CLP patient, a procedure that usually bears various dentofacial esthetic and functional problems, and does not address the hypoplasia in the midface. 11 Moreover, the complication that followed added a considerable adverse impact on the patient’s condition, which necessitated prompt management.
Necrosis and loss of bone segments following SSO is a not frequently encountered but detrimental problem that has been attributed mainly to vascular compromise of the osteotomized segments. 3 Several authors investigated the impact of the SSO and other mandibular osteotomies on the bone blood supply in animals.8,12,13,14 Their studies have delineated the significance of judicious stripping of the periosteum and pterygomassetric sling off the proximal segment of the mandible on the bone viability. Grammer et al. studied the vascular response after SSO in 11 adult Macaca monkeys and proved that the procedure had resulted in a crucial reduction in the blood flow to a portion of the proximal segment below the horizontal cut that is adequate to result in bone ischemia. 8 In that regard, it has been hypothesized that it may typically take days before the revascularization of the devitalized bone to occur, and the perfusion remains inadequate postoperatively to prevent avascular necrosis. Therefore, a more conservative modification of the SSO has been proposed, entails less soft tissue stripping from the proximal segment, enhancing the bone perfusion and decreasing the postoperative bone loss. 9
In modern practice, reports of necrosis of large bone segments following SSO are scarce in the literature. Behrman, MacIntosh and Martis have reported cases of bone necrosis affecting the proximal segment after SSO with a variable degree of severity during the postoperative period.4,15,16 Lanigan and West have also reported a case of aseptic necrosis of a large segment of bone following SSO extending from the first molar and involving most of the ramus without significant clinical signs and symptoms suggestive of the extensive underlying process. 7
In general, the relationship between ischemic bone necrosis and the presence of infection after orthognathic surgery varies in the literature. Bone sequestration secondary to ischemic necrosis forms the most significant factor that may predispose to infection postoperatively. 16 However, inexplicably, aseptic necrosis of large bone segments with no clinical signs of infection or osteomyelitis has also been reported. 7 Overall, infection after orthognathic surgery is an extremely rare occurrence, even with the absence of prophylactic antibacterial, with most cases usually occur following the mandibular surgery.16,17
We propose that a confluence of several factors relevant to the anatomy of our patient’s mandible and the surgical techniques of the initial intervention had resulted in the incidence of this complication. The ramus is excessively thin in the bucco-lingual dimension with a low volume of cancellous bone, in addition to a diminished posterior height and reduced depth from the apices of the molars to the inferior border. Those features pose a considerable challenge to favorably split the buccal and lingual cortices without resulting in unwanted fractures of bone segments. That might explain the unusual pattern of the ramus split following the initial surgery (Figure 1), which involved complete bone separation through the angle of the mandible with the lack of overlap between the proximal and distal segments. Several studies have highlighted the influence of bone thickness and height of the posterior mandible on the split pattern and the incidence of operative complications.18-21 It was found that a slender and thin mandible with short ramus height and body depth carries a higher risk of unfavorable fractures.18,21 The biggest concern about bad split in these cases emerges from the compromised bone contact and extensive periosteal dissection that is necessary for the fragment salvage and fixation, resulting in an increased risk of bone ischemia and sequestration. 22
Additionally, unscrutinized soft tissue reflection from the small and short ramus is another critical factor in the pathophysiology of bone devitalization and necrosis. It carries a high risk of stripping a considerable surface area of bone from its musculo-periosteal coverage and hence interrupting most of its blood supply.
The lack of rigid fixation is almost associated with increased morbidity of the procedure, carries a tremendous adverse impact on the healing process, and increases the possibility of infection, sequestration, non-union or mal-union. 17 The non-rigid immobilization had unfavorably promoted the mobility of bone segments at the osteotomy/fracture site, adversely interfering with the revascularization and bone consolidation.
Consequently, the short, thin, and unfavorably osteotomized proximal segment of the mandible devitalized and underwent ischemic necrosis, which provoked and augmented by the reflection of the surrounding soft tissue attachment.
Owing to the severe dentofacial esthetic and functional disturbance, prompt management was planned to be provided to our patient. The preoperative orthodontic preparation aimed primarily to perform teeth alignment and jaw accommodation to create a stable occlusion for the surgery, while the definitive management planned to be performed postoperatively to correct the severe dental arch deformity.
The use of VSP provided an additional valuable tool to understand the deformity and plan the surgical procedure. Correction of the mandibular deviation was planned first to recreate a stable reference for the subsequent maxillary repositioning. It is usually helpful to plan correction of the jaw with the largest discrepancy and midline shift first and reestablish a centric occlusion. 10 Ramus subsigmoid osteotomy was performed on the left side, followed by the defect reconstruction on the right by a prebent load-bearing plate and bone graft, with the application of IMF. Performing RSO is a viable and safe procedure in the correction of jaw asymmetries and rotation, especially in revision cases. It allows jaw mobilization without approaching the previous surgical site and decreases injury of the inferior alveolar nerve. Although rigid internal fixation has been described in RSO, IMF is still valid and considered the standard of care in these cases. 23 That entailed performing surgical intervention in two stages, with the maxillary advancement and genioplasty were performed at a second stage, after healing of the mandibular surgical site and the release of the immobilization.
Two years postoperatively, the patient now shows significant enhancement in facial esthetics and mandibular symmetry with improved occlusal relationship, and overall quality of life. However, further definitive orthodontic management and prosthetic rehabilitation still required to enhance the patient’s occlusion.
Conclusion
Orthognathic surgery is considered an elective intervention and most of the time carried out only for esthetics reasons. Therefore, the surgeon must understand the specific need of each patient and work to reduce the risk of complications through a comprehensive diagnostic process and accurate planning. Avascular necrosis of the bone segment after orthognathic surgery is a rare but dreaded problem and requires a thorough knowledge of the risk factors to minimize the incidence and efficient team collaboration for proper management. Following the basic surgical principles by minimizing the musculo-periosteal dissection followed by competent execution of the bone osteotomy are substantially effective in reducing the risk of bone ischemia and necrosis.
Footnotes
Acknowledgments
The authors would like to thank Dr. Sargon shazo and Dr. Abdulaziz Muayad for their vast contribution in management of the case, and Dr. Esraa Hassan for the valuable support in writing the article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
