Abstract
Purpose:
The present study aims to report the reoperation of an unsuccessful orthognathic surgery with the use of heterogeneous graft and hybrid rigid internal fixation.
Case Report:
We report the case of V.M.S., a 19-year-old female patient with the main complaint of “crooked chin.” The patient revealed that she previously underwent two operations that were conducted by a different team. The first surgery was carried out to correct the dentofacial deformity, while the second one was intended to eliminate a postoperative infection. After a detailed anamnesis, facial analysis, cephalometric analysis with tomography, and examination of gypsum models, we observed mandibular left-handedness and vertical maxillary excess on the right side. In addition to these previously reported problems, there was a nonunion in the region of the sagittal fracture of the left jaw.
Results:
The patient underwent surgery to correct dentofacial deformity using the Le Fort I maxillary osteotomy technique and bilateral sagittal osteotomy with hybrid rigid internal fixation plus mentoplasty.
Conclusion:
Six months following the procedure and orthodontic completion, the patient has a satisfactory occlusion and stability of nonunion without the laterognathism in the skeletal and soft tissue profile.
Introduction
Orthognathic surgery is a suitable procedure for the correction of dentofacial deformities. Its main benefits are the improvement of aesthetics and facial pattern, improvement of masticatory function, and amelioration of facial asymmetries. Such cross-sectional asymmetries are common mainly in the mandible and are frequently directed to the left side. 1 They are usually being treated with bilateral sagittal osteotomy with or without a combination of other osteotomies such as Le Fort I and mentoplasty.
One of the greatest challenges for correcting transverse asymmetries is the adaptation of the bone to be moved, so that it is in the planned position without interference from the bones that will not be moved, 2 maintaining the stability of the movement and the occlusion after the surgical procedure. The greater the discrepancy presented, the greater the difficulty for bone repositioning, which could lead to problems in the immediate and late postoperative periods such as nerve damage, anticlockwise rotation of the proximal fragment, severe secondary bleeding, edema, recurrence, unsatisfactory occlusal outcome, 3 –6 vascular impairment, failure of the inferior alveolar nerve, condylar resorption, removal of osteosynthesis material, 3 fixation, 6 and psychological problems. 7
The sagittal osteotomy technique of the mandible is one of the most commonly used treatment methods for asymmetries as it obtains a three-dimensional displacement of the manipulated bone. Nevertheless, the patient may present complications due to severe facial deformities, transoperative difficulties, operator inexperience, and incorrect use of a fastening material. 3 This failure in the fixation material may be potentiated by the lack of support tissue for its fixation. It can hamper its use and lead to a reduced area of contact between the operated stumps. It may also cause instability that can result in problems of the bone repair process such as infection, malunion, osteomyelitis, tissue dehiscence, and nonunion. 8
Of the problems listed, an infection of the mandible following an orthognathic surgery is an unlikely complication, 3,6 present from 0% to 18% of cases when antibiotics are used in the trans- and postoperative periods. However, when this postoperative complication occurs in a severe manner and a procedure is deemed necessary, the following tasks are required to be performed: a more aggressive debridement or bone grafting, and even both. In any case, a new surgery should be performed. 6
This case report aims to present an unsuccessful orthognathic surgery that aimed to correct laterognathism, which developed into an infectious process in the mandible and led to a nonunion in the fracture line of the sagittal osteotomy. It will also discuss the main problems encountered when treating asymmetries, infectious process, and nonunion in orthognathic surgeries.
Case Report
The present study reports the case of a 19-year-old woman, M.S.M., who was referred to the Maxillofacial Surgery Department of the School of Dentistry of Bauru, University of Sao Paulo, with the main complaint of “crooked chin.” This study followed the Declaration of Helsinki on medical protocol and ethics and the regional Ethical Review Board of the University approved the study.
The patient’s medical history was negative for any underlying disease or contraindication for orthognathic surgery. Results of the physical examination revealed that the mandible has deviated to the left and the right jaw was exceeded. Findings from the intrabuccal examination showed that the patient had an open bite on the right side and crossbite on the left side. When the dynamic inspection of the mandible was performed, mobility was observed in the region of the left mandibular angle with painful symptomatology. The patient reported bilateral alveolar nerve paresthesia after the first surgery.
When asked about the history of a recent trauma in the region, the patient reported having undergone two previous orthognathic surgeries that were performed by another Maxillofacial service. According to the patient, the first proposed surgery was performed to correct the laterognathism (Figure 1) with the plan of a Le Fort I-type osteotomy to impact the maxilla and a sagittal osteotomy to correct the asymmetry. After the first surgery (Figure 2), the patient developed an infection in the region of the left mandibular angle in the sagittal osteotomy line. Upon returning to the group that performed the first surgery, a second surgical procedure was recommended to treat the infectious process. The patient underwent a second surgery to clear the infection (Figure 3), and an exchange of the synthesis material was performed.
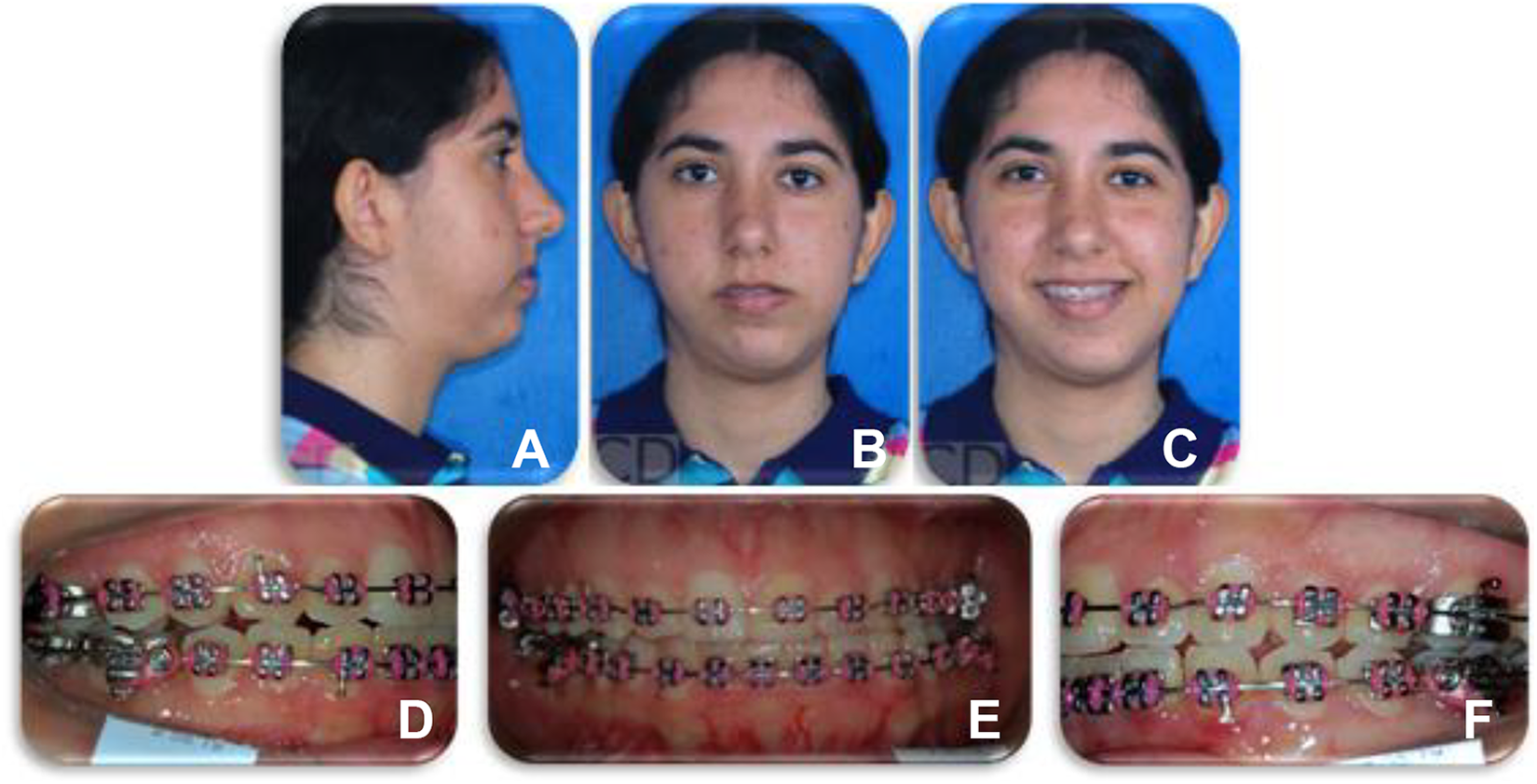
Initial photos of the patient before the first orthognathic surgery: (A) right face, (B) frontal face where a left mandibular deviation is noted, (C) frontal view of the patient’s smile, (D) occlusal view of the right side, (E) frontal, and (F) left side.
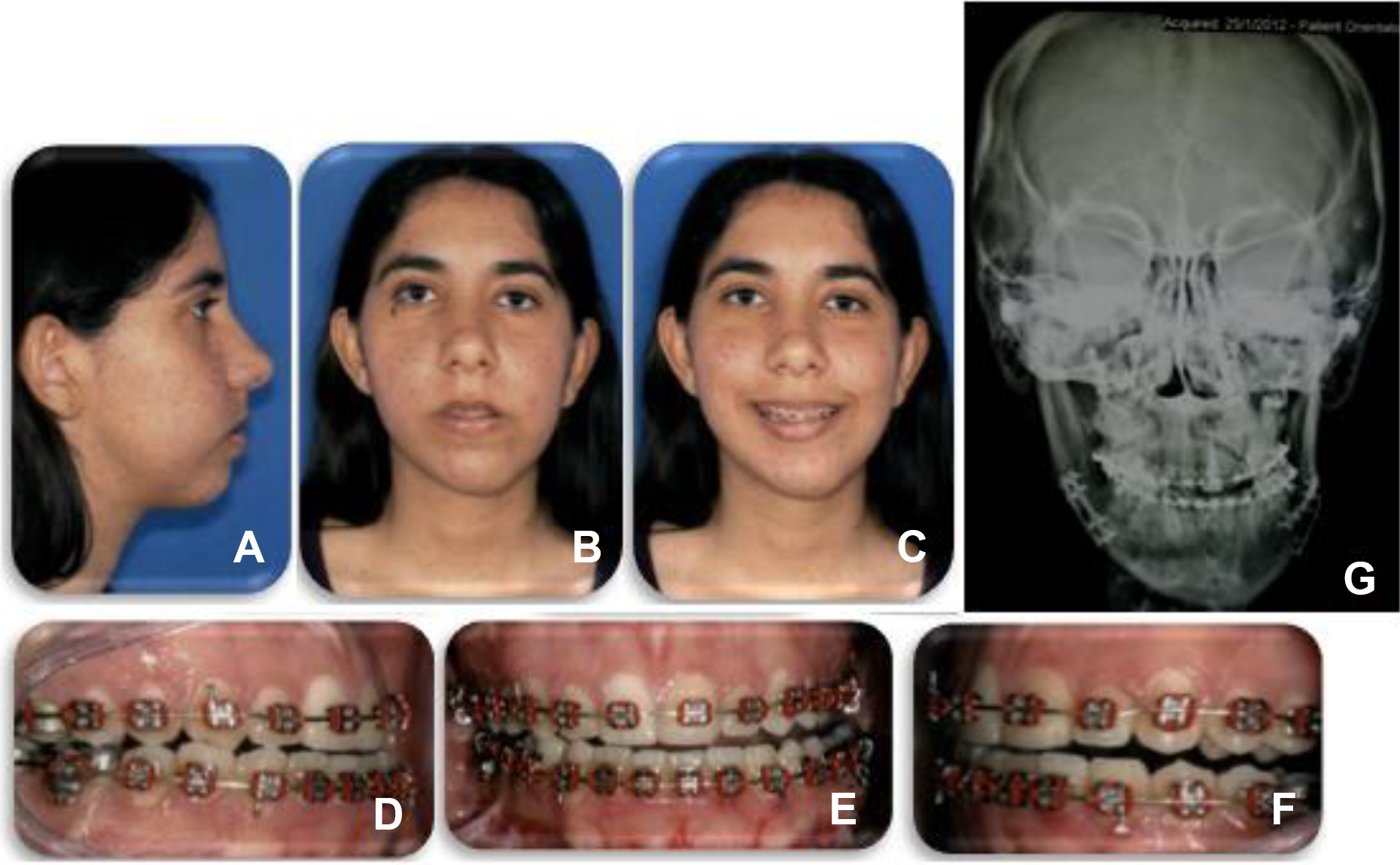
Result of the first orthognathic surgery, where in the face: (A) lateral right, (B) frontal with lip at rest, and (C) smiling it is still possible to observe the mandibular deviation to the left. (D) View of the occlusion of the patient in the postoperative period of the first orthognathic surgery showing in the right lateral photo posterior crossbite, (E) mean line deviation in frontal norm, and (F) open bite on the left side. (G) Posteroanterior radiography showing the plates and screws of the first orthognathic surgery. Still observed is the deviation of the mandible to the left side.
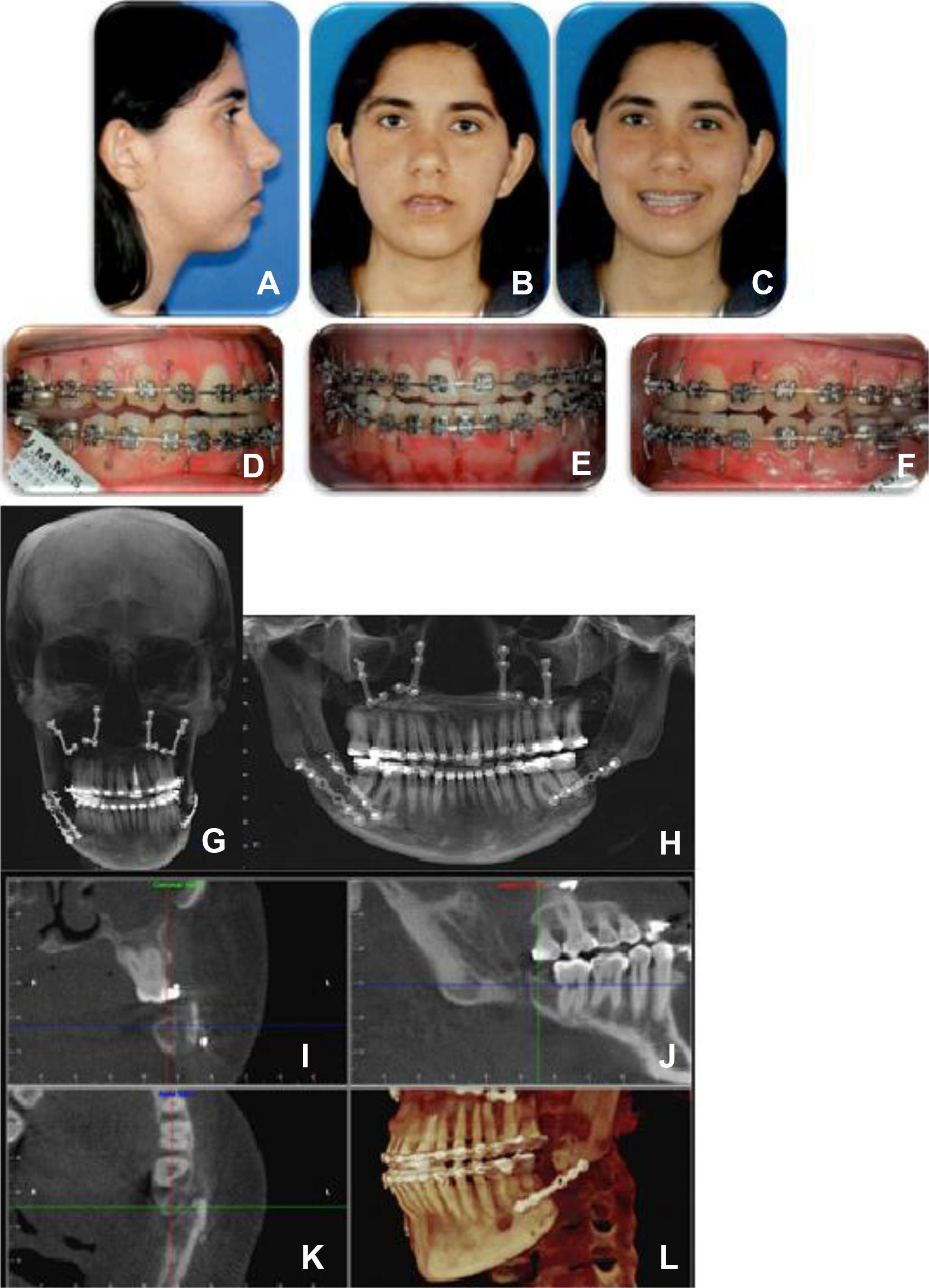
Result of the second orthognathic surgery with the photos of (A) face of the patient in right lateral norm, (B) front view with the lip at rest, and (C) with smile. Still observed is the deviation of the mandible to the left side. (D) Occlusal view of the right side with open bite, (E) bite on top in the anterior region, and (F) crossbite on the left side. (G) Computed tomography showing an image suggestive of nonunion of mandibular stumps after a sagittal osteotomy of the left jaw, with the use of a single plaque for fixation of the osteotomy. (H) Panoramic view, (I) coronal, (J) sagittal, (K) axial, and (L) three-dimensional reconstruction.
After the second procedure, the patient still presented left side laterognathism and reported chewing discomfort, especially in the left jaw region. Our team was asked for all the documentation for the preoperative period, such as facial analysis, cephalometric analysis with computed tomography, and examination of gypsum models with mandibular left-handedness, and vertical maxillary excess on the right. In addition to these previously reported problems, a nonunion image of the left-sided sagittal osteotomy was observed at the tomographic examination using a single 2.0-mm system board.
After documentation review and virtual planning performed on Dolphin 3D software (Version Dolphin Imaging 11.95), a third orthognathic surgery was proposed to correct the two problems: the facial deformity and nonunion. The proposed techniques to be used were as follows: Le Fort I-type osteotomy in the maxilla to correct the vertical excess, a new bilateral sagittal osteotomy of the mandible using the hybrid fixation technique and one plate with bicortical screws placed at the base of the mandible, and a mentoplasty that had not yet been performed. To perform the surgery, a guide was made to assist in the new positioning of the jaws, minimizing the possibility of error in the final occlusal positioning of the case. Meanwhile, the patient revived treatment for paresthesia with Whitening Laser II DMC (São Carlos–SP, Brazil), with gallium arsenide and aluminum (GaAIAs) active medium, with infrared emission of λ = 808 nm, with a power of 100 mW in 10 sessions, one session per week for 10 weeks.
The main focus of the surgery was nonunion of the mandible. After access and detachment of the flap in the region of the left mandibular angle, the area was accessed, and a large amount of fibrous tissue was removed until the mandibular stumps were visible. These were then released by removing the synthesis material. After the maxillomandibular block, with a surgical wafer, a proximal follow-up was conducted with the condyle resting in the glenoid cavity, and the mandible fixation was performed using the hybrid technique. The residual gap in the mandible was filled using Bio-Oss Collagen (Geistlich Pharma AG, Wolhusen, Switzerland), and the tissues were sutured in the muscular and mucosal planes using absorbable suture yarn 3-0 and 4-0, respectively (Polyglactin 910; Ethicon, Johnson & Johnson, São Paulo, Brazil).
Six months after the procedure and orthodontic completion, the patient presented a satisfactory occlusion and stability of nonunion (Figure 4) without laterognathism in the skeletal and soft tissue profile that characterized the face of the patient.
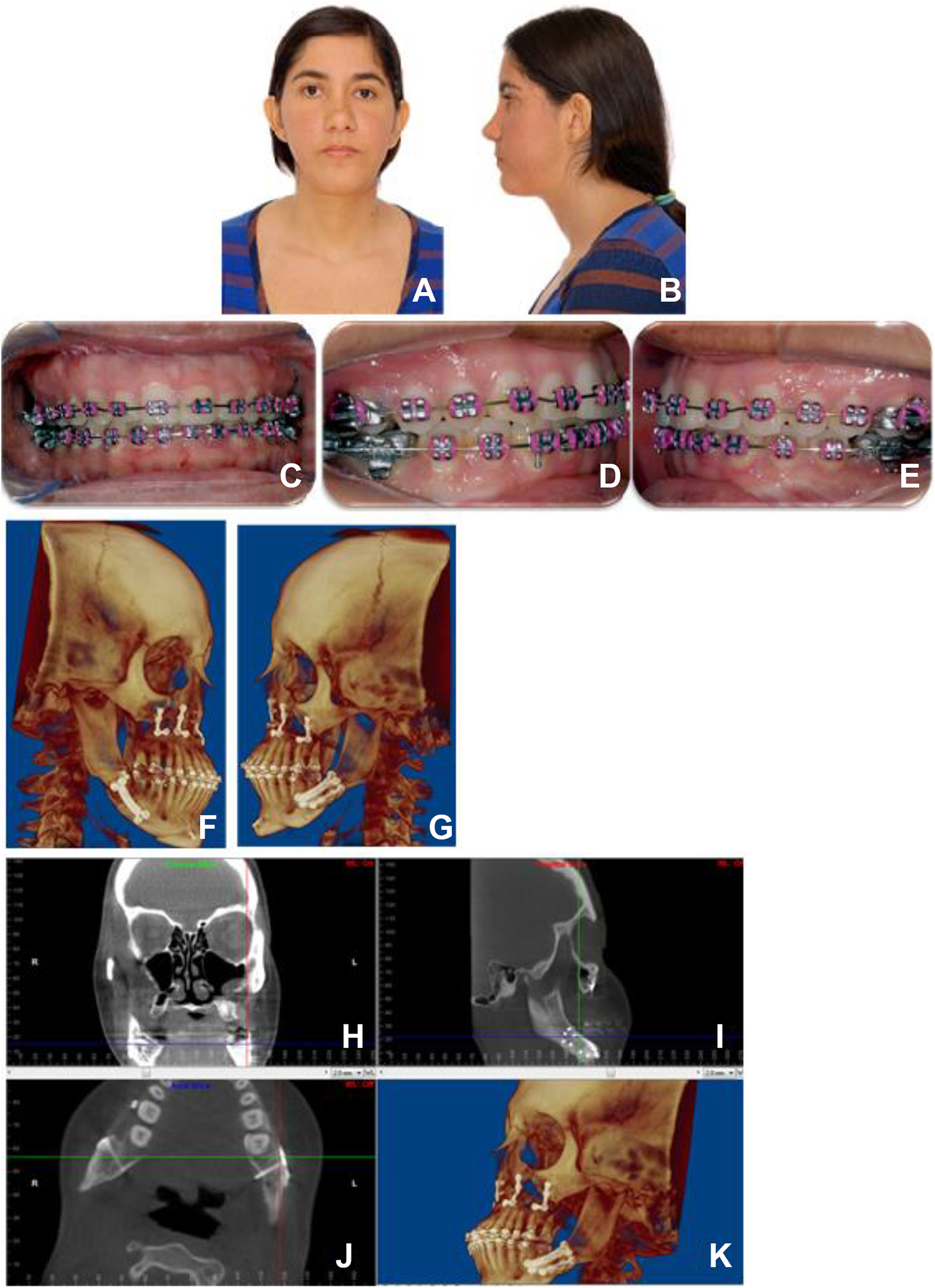
View (A) frontal and (B) left lateral of the patient’s face after the third orthognathic surgery, without the mandibular deviation to the left. Occlusal view of the occlusion after the third orthognathic surgery, (C) frontal view, (D) right lateral, and (E) left lateral. Computed tomography with three-dimensional reconstruction in (F) right lateral view and (G) left showing the fixation materials used for the treatment of mandibular nonunion on the left side. (H) Coronal view of computed tomography, (I) sagittal view, (J) nonunion fixation in mandible using the hybrid fixation technique, (K) three-dimensional tomographic reconstruction showing the result of the third orthognathic with the nonunion treatment using Bio-Oss Collagen and the hybrid fixation technique.
Discussion
The objective of this work was to report an unsuccessful case of laterognathism operation, which developed into an infectious process in the mandible leading to a nonunion. Planning the surgical correction of skeletal deformities is complex and requires some parameters of facial analysis and surgical standards to be performed. This is because in some cases, the planned movements may become unstable because of their amplitude and can lead to limit the application of the synthesis material or even, in certain situations, the difficulty of the repair process of the osteotomies performed.
Orthognathic surgery is widely used to correct congenital abnormalities and acquired dentofacial discrepancies. However, its complications in extreme cases are life-threatening. 3 In addition, there are several other factors that can affect the frequency and type of complication, including surgery site, chosen approach, clinical nature of the surgery, surgery time, wound contamination, patient psychological pattern, postoperative care, and skill of the surgeon. 9,10
Predicting these complications requires a better understanding of how to manage them and avoid their occurrence. A surgical procedure may present a lower probability of failure. When a complication arises, despite precautions, appropriate treatment should be given to ensure a good prognosis. 10 In this case, the treatment performed was focused on the infection and the exchange of the mandible fixation technique without the use of thick profile plates or with the use of a maxillomandibular block and a grafting material to contribute to the fracture repair process.
Sagittal bilateral osteotomies allow the distal segment of the mandible to be repositioned in the three spatial planes, and the transverse deviation of the facial midline can thus be corrected. The adaptation of the segments to obtain a good bone contact may be necessary. This is one of the most challenging surgical procedures, in both its planning and its implementation, which may have implications for long-term postoperative stability, generating some iatrogenic effects such as sensory impairment and paresthesia. 2 In this case, the main complaint of the patient in her first surgery was accentuated laterognathism, which was not resolved even after two orthognathic surgeries and was only corrected after the third surgery using the mentoplasty technique.
Another common and significant complication in the postoperative period is the failure to fix the osteotomy in the mandible, which usually results from technical difficulty during surgery or incorrect use of the synthesis material. This may be problematic if it is not recognized early in the postoperative period because it is likely to result in malocclusion, nonunion, and potentially rotation and resorption of the proximal segment. The surgical correction may become much more technically difficult. 6 In the case presented in the first surgeries, a single 2.0-mm system board with monocortical screws was used. It was associated with an infectious process, which was developed by the patient during the postoperative period and led to nonunion of the mandible. To treat this patient, the hybrid fixation technique was used. 11 A 2.0-mm system board fixed with monocortical screws and two bicortical screws was utilized, increasing the stability of the fracture. The ability to correctly fix the fractured segments at the time of surgery may facilitate bone repair postoperatively and reduce the possibility of bone segment displacement. The excessive shearing produced by the compressive action of the masseter muscle to the osteotomy line can transform the mandibular form in the postoperative period. Therefore, osteosynthesis should be performed bicortically, especially in patients who have undergone overcorrection. 11
After surgery, some degree of postoperative discomfort is expected. Some patients may experience extreme pain, swelling, bruising, and infection. 6 One of the most frequent complications after bilateral sagittal osteotomy is the sensorineural disturbance of the inferior alveolar nerve, with an incidence of 9% to 85%. Many factors can affect this incident, including the age of the patients, the magnitude of the mandibular movement, the degree of manipulation of the nerve during surgery, surgeon’s skill and experience, method, and moment of the sensorineural evaluation in the postoperative period. 12 The patient in the case reported had some complications but did not present any sensory deficits or paresthesia in the postoperative period. Painful symptomatology and discomfort during chewing on the left side of the mandible were noticed, besides mobility in the mandibular angle.
Bone repair after orthognathic surgery is associated with few complications. However, wound infection remains an occasional problem. Generally, the prevalence of infection after maxillary and mandibular osteotomies is low, and the reported infection rate may vary from 1% to 33%. Numerous factors are believed to influence these rates, including age, duration of surgery, type of procedure, and prophylactic use of antibiotics. 13
Inadequate repair of large mandibular defects may affect the stability and support of soft tissues at the lower edge of the mandible. The correction of dento-skeletal deformities is often associated with large vertical and sagittal maxillomandibular movements satisfying the functional and aesthetic results. 14
The normal process of fracture repair is divided into four temporal phases: inflammatory, chondrogenic, osteogenic, and remodeling. Each one is repaired by tissue differentiation. The normal repair is bone union, in which the end of a fractured bone is joined by a new bone tissue, with anatomical reduction and fixation, resulting in the restoration of function and prevention of deformities. 15
Most negative results can be prevented or corrected, but probably, the most challenging of them all is nonunion treatment. Patients who develop this complication often suffer from infection, pain, and trismus at some point during treatment. The infection affects bone repair, thereby reducing oxygenation and providing a proliferation of fibroblasts with delayed osteoblast and osteoclastic activity. The formation of fibrous tissue thus predominates over bone deposition and leads to fibrous attachment. The site of most nonunion is in the mandibular body. This is known as the site of high complications because the mandible has less blood supply than the maxilla. 16 The patient operated in this case presented infection and nonunion at the angle of the left jaw. In the third surgery that aimed to correct the deformities and complications, a large amount of fibrous tissue was removed at the site where the bone repair was to be performed, requiring a xenogenous bone graft to fill the gap.
The use of Bio-Oss Collagen as a grafting material occurred because of its ease of manipulation and the possibility of greater adhesion to osteotomized stumps, facilitating its modeling and stability after the placement of the flap. Other works have already used Bio-Oss as a filling material in cases of maxillary segmentation 17 and in sagittal mandible osteotomies, 14 with similar results found in this case.
Once nonunion has occurred, treatment should be individualized. The infection is treated by drainage, debridement, and stabilization of the mandible with rigid or external/internal fixation. If a defect develops, it can be treated with a bone graft. 16
The failure of orthognathic surgery is caused not only by surgical complications but also by several factors. Thus, adequate diagnosis followed by proper orthodontic and surgical planning is necessary. An orthodontist should perform adequate orthodontic planning to obtain the correct occlusion relationship after surgery. 18
Six months following the procedure and orthodontic completion, the patient presented a satisfactory occlusion and stability of the nonunion without the laterognathism in the skeletal and soft tissue profile that characterized the face of the patient.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
