Abstract
Study Design:
Biomechanical in vitro study. Mandibular advancement after sagittal split ramus osteotomy (SSRO) is a common procedure in orthognathic surgery. Several fixation methods are used for stabilization of SSRO.
Objective:
The aim of this study was to compare a new fixation method (gridplate) with more contemporary applied methods of fixation.
Material and Methods:
In this study, 50 polyurethane hemimandibles with a prefabricated SSRO were used as specimens. All hemimandibles were advanced by 8 mm and divided into 5 groups with different fixation methods: (A) one 4-hole miniplate with 4 monocortical screws; (B) two 4-hole miniplates with 8 monocortical screws; (C) one 4-hole miniplate with 4 monocortical screws and 1 bicortical screw in the retromolar area (hybrid method); (D) 3 bicortical screws in an inverted-L pattern; and (E) one 8-hole gridplate with 8 monocortical screws. Loads in newtons were recorded at displacements of the mandibular incisive edge at 1 mm, 3 mm and 5 mm.
Results:
Fixation with 3 bicortical screws and the gridplate presented the most stability, followed by two 4-hole miniplates. Fixation with the hybrid method or the single miniplate showed the least stability.
Conclusion:
According to the results of this study, the 8-hole gridplate design appears a sufficient fixation method regarding stabilization of SSRO with larger mandibular advancement.
Introduction
Sagittal split ramus osteotomy (SSRO) with advancement of the mandible is nowadays a routine orthognathic surgical procedure and has a wide array of indications, such as for the correction of skeletofacial discrepancies and/or class II malocclusion. 1 It could also function as an effective treatment for patients with obstructive sleep apnea (OSA). In the latter case, the SSRO is frequently combined with a Le Fort 1 osteotomy with advancement and rotation of the occlusal plane, commonly referred to as maxillomandibular advancement surgery (MMA). 2,3
There is a wide range of rigid internal fixation methods for stabilization of SSRO, namely bicortical screws, miniplates with monocortical screws or a combination of both techniques (hybrid). 4 In the current literature there are different perspectives regarding preferences for each fixation technique. These preferences are based on different considerations such as handling, predictability, occurrence of complications, possibility of relapse, cost-effectiveness, length of advancement and rigidity. 4 –7
With regard to the length of mandibular advancement and rigidity, it is acknowledged that larger mandibular advancements (i.e. >6-7 mm) using contemporary fixation methods are more prone to postoperative instability. 5,8 The rigidity of fixation methods has also been investigated in a number of biomechanical evaluation studies. 9 –12 Regarding mandibular advancements up to 10 mm, the use of 3 titanium bicortical screws placed in an inverted-L pattern has presented the most stability. 4,13,14 However, in the case of extremely large advancements (i.e. >15 mm), 2 titanium miniplates presented more stability than 3 titanium bicortical screws in an inverted-L pattern. 13
Two miniplates can also be connected with each other, which is known as a “gridplate.” It is thought that connecting the 2 miniplates could provide additional stability. 4,15,16 A gridplate may also be useful in minimizing post-operative instability in the case of larger mandibular advancements. In the recent literature, various new designs of gridplates have been compared with other fixation methods. 15 –17 The use of in vitro biomechanical research for these comparisons has yielded fundamental knowledge regarding the mechanical characteristics of the newly designed fixation material. The aim of this study was to evaluate the stability of a newly designed gridplate in comparison with other commonly used fixation techniques for the stabilization of SSRO after mandibular advancement of 8 mm.
Methods
In this in vitro biomechanical study, 50 identical, left-sided polyurethane hemimandibles were used for loading tests. In all hemimandibles a standardized SSRO was performed by the manufacturer (Nacional Ossos, Jaù, Sao Paulo, Brazil), mimicking the technique described by Epker. 18 The hemimandibles were allocated among 5 fixation groups with 10 hemimandibles each. A specific configuration of titanium material was used for each group: (A) one 4-hole miniplate with 4 monocortical screws; (B) two 4-hole miniplates with 8 monocortical screws; (C) one 4-hole miniplate with 4 monocortical screws and 1 bicortical screw in the retromolar area (hybrid technique); (D) 3 bicortical screws in an inverted-L pattern; and (E) one 8-hole gridplate with 8 monocortical screws (Figure 1). All fixation materials were manufactured by KLS Martin Group (Tüttlingen, Germany). The miniplates and screw materials were from the 2.0 mm system. The monocortical screws were 6 mm and the bicortical screws were 13 mm in length. All miniplates, including the gridplate, were equal in length and 1.0 mm thick. For fixation of the SSRO, the distal segment of the mandible was advanced in a linear direction, resulting in an 8 mm gap between the proximal and distal segments of the hemimandible.

Five configurations of fixation methods in polyurethane hemimandibles with 8 mm linear mandibular advancements: (A) one 4-hole miniplate with 4 monocortical screws; (B) two 4-hole miniplates with 8 monocortical screws; (C) one 4-hole miniplate with 4 monocortical screws and 1 bicortical screw in the retromolar area; (D) 3 bicortical screws in an inverted-L pattern; and (E) one 8-hole gridplate with 8 monocortical screws. Each group contained 10 polyurethane samples.
To standardize placement of the fixation materials and the length of mandibular advancement, a drill jig custom-made according to the method of Kuik et al. was used. 13 Using the jig for guidance, the hemimandibles were predrilled. All plates and screws were bent and fixated by one investigator (KK). Loading tests were carried out using an Instron universal testing machine (6022, High Wycombe, UK). The proximal part of the hemimandible was fixated at the condylar and ramus region in a resin jig with a metal support structure (Figure 2). Vertical loading, at a speed of 1 mm/min, was applied on the incisal edge of the hemimandibles. Loads in newton were recorded at displacements of the incisal edge at 1 mm, 3 mm and 5 mm, respectively. All hemimandibles were used only once for testing. After the loading tests of up to 5 mm, the sample and fixation material were assessed macroscopically for fractures.

Experimental set-up. The polyurethane hemimandible was fixed at the condylar and ramus part in a resin jig within a metal support structure. Vertical compressive forces were applied on the mandibular incisal edge by an Instron 6022 testing machine.
Data were analyzed using the Statistical Package for the Social Sciences (SPSS, version 25, IBM, Chicago, IL, USA). Means and standard deviations were derived from the results for all 3 lengths of displacement. Using the Kolgomorov-Smirnov test, normality of distribution was determined for all groups. Means and standard deviations of the groups were compared for statistically significant differences using analysis of variance (ANOVA) and the Tukey test. Significance was set at the α level of 0.05.
Results
As shown in Figure 3, at 1 mm displacement, the group with 3 bicortical screws yielded the strongest fixation method, followed by the gridplate group, the 2 miniplates group and the hybrid group. The single miniplate group yielded the least stability (P < 0.01). The results for the 3 bicortical screws fixation group differed significantly from those obtained with the gridplate (P = 0.012). The significance of the difference between the gridplate group and the 2 miniplates group was P = 0.032. All statistical differences between the other groups were P < 0.01.
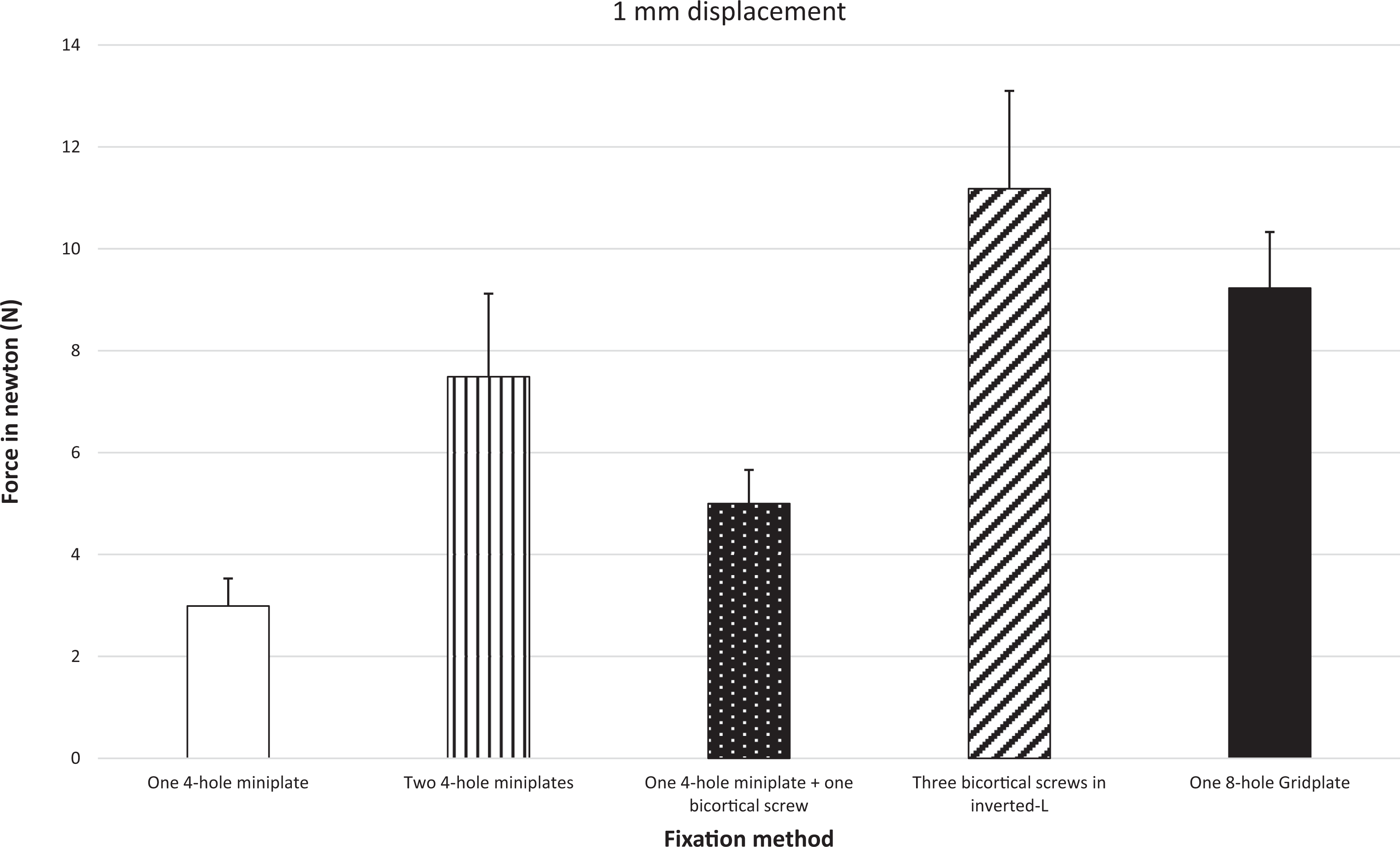
Mechanical resistance using vertical loading measured in newton at 1 mm displacement. One-way ANOVA post hoc Tukey test. Differences in the content of the bars indicate significant differences between bars (P < 0.05). The error bars represent 1 standard deviation.
At 3 mm displacement, the groups with 3 bicortical screws and the gridplate did not differ significantly (P = 0.712). Both groups were significantly the most stable methods of fixation (Figure 4). Fixation with 2 miniplates was less stable than both groups; however, the use of 2 miniplates was more stable than the single miniplate group and the hybrid group. The results obtained from the single miniplate group were not significantly different from those obtained from the hybrid group (P = 0.108). All significant differences between groups were P < 0.01.
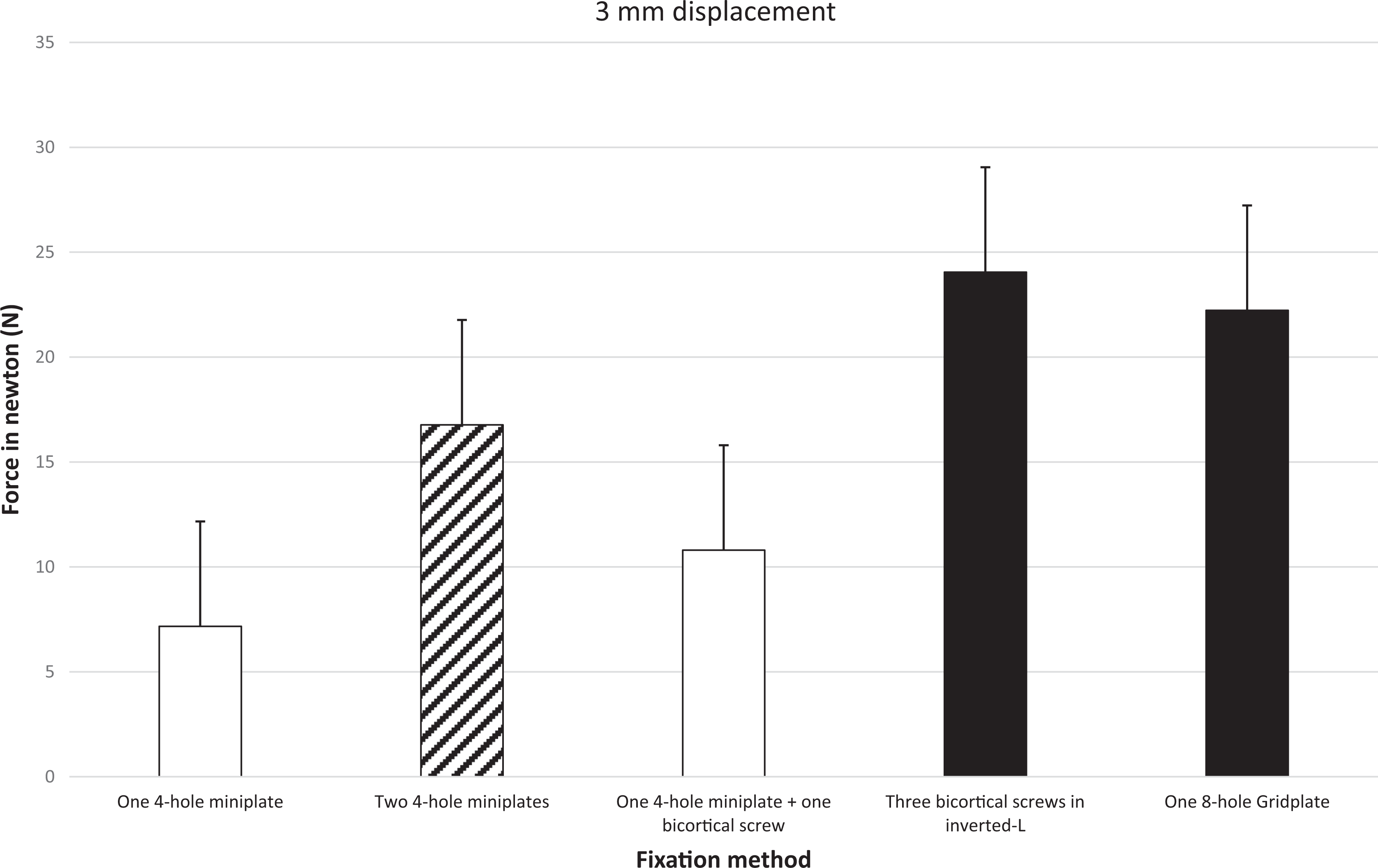
Mechanical resistance using vertical loading measured in newton at 3 mm displacement. One-way ANOVA post hoc Tukey test. Differences in the content of the bars indicate significant differences between bars (P < 0.05). The error bars represent 1 standard deviation.
As shown in Figure 5, at 5 mm displacement, the groups with 3 bicortical screws and the gridplate did not differ significantly (P = 0.615). Both groups presented the most stability, followed by the 2 miniplates group. The single miniplate group and the hybrid group were shown to be the least stable fixation groups. There was no significant difference between the single miniplate group and the hybrid group (P = 0.079). The results obtained from the 2 miniplates group differed significantly from those obtained from the hybrid group (P = 0.016). All significant differences between other groups were P < 0.01.
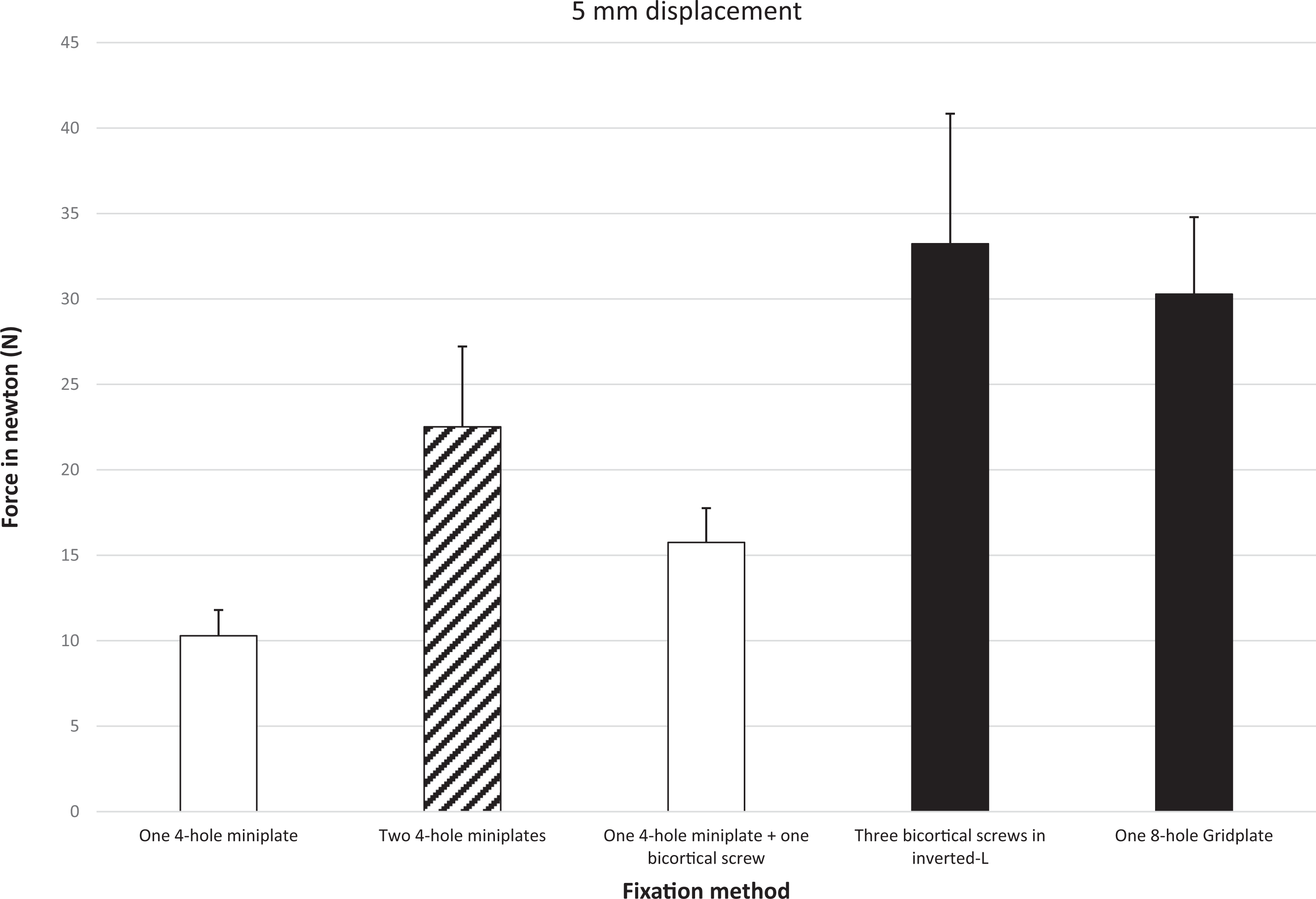
Mechanical resistance using vertical loading measured in newton at 5 mm displacement. One-way ANOVA post hoc Tukey test. Differences in the content of the bars indicate significant differences between bars (P < 0.05). The error bars represent 1 standard deviation.
There were no visible fractures in the samples and in the titanium material after mechanical loading at all 3 distances.
Discussion
Development of new osteosynthesis material is an ongoing process and is aimed at expanding the SSRO fixation options in order to find a fixation method with the most ideal characteristics. Currently used fixation materials have some drawbacks. The use of bicortical screws is associated with an extraoral approach and the chance of neurovascular bundle damage and scarring. 6 Also, the bicortical screw technique is less forgiving in its use with regard to the correction of improper condylar seating. 6,19 This in contrast to the application of miniplates in which correction of the condylar seating requires only repositioning of the monocortical screws at the distal (tooth-bearing) aspect of the osteotomy. 19 Conversely, less-rigid fixation with a single miniplate could result in fixation failure in some of cases. 20 Although the use of thicker plates results in more rigidity, this could also lead to bothersome palpability of the hardware. 7 The use of multiple miniplates also adds to stability. 13,15 However, this increases the hardware costs and placement is not always feasible because of the lack of available bone surface. For this reason, the use of an increased number of plates is also associated with an increased risk for plate removal following orthognathic surgery. 21 Therefore, in the development of new fixation material all strengths and weaknesses should be considered.
In this in vitro study, biomechanical loading tests were used to assess the rigidity of different fixation methods. The limitations of biomechanical studies are well known and have often been described. 4,14 Biomechanical studies are simplified theoretical models of reality. 4 However biomechanical research serves an important function for testing the rigidity of osteosynthesis material, due to the possibility of testing under standardized conditions. Furthermore, the rigidity of new fixation methods can be compared in a safe experimental set-up with commonly used rigid internal fixation methods. That is why, similar to our study, other studies have also utilized the in vitro biomechanical method in order to test the mechanical resistance of new osteosynthesis materials. 11,14 –16 In this study we simplified the model to an hemimandible and used a cantilevered beam model in mimicking masticatory function. Other biomechanical studies have used whole polyurethane mandibular replicas, in which more complex biomechanical models were used in mimicking masticatory function. 4,12,16 Although the strive for closer proximity to human anatomy in these models could be encouraged, the results of all biomechanical studies cannot directly be extrapolated to clinical circumstances. As of a financial perspective, the costs for materials in biomechanical research with complete mandibles would be doubled with the same number of samples.
The results observed in this study should be approached with a certain amount of caution in application in clinical circumstances. In this biomechanical study incisal bite forces are simulated in an in vitro setting. Previous clinical studies have measured occlusal and/or incisal forces shortly after mandibular surgical treatment. 22,23 Harada et al. observed mean occlusal forces of 66.5 newton in patients, 2 weeks after SSRO with a mandibular setback. 22 Ellis et al. measured incisal forces in patients treated with open reduction internal fixation after a mandibular angle fracture. After 1 week, the average incisal bite force was 62.7 N and after 6 weeks 120.5 N. 23 The resultant forces in this biomechanical study are lower in comparison with data of the earlier mentioned clinical studies. This could be explained by the cantilevered beam model and the absence of soft tissue and muscles in this in vitro experimental set-up.
Earlier, an alternative gridplate design has been compared in a biomechanical set-up with various other fixation methods, such as 2 miniplates, a single miniplate or the hybrid method. 15,17 The gridplate design in these studies comprised 2 miniplates with 1 vertical connecting bar between both, which was positioned at the proximal screw holes closest to the osteotomy site. None of the other tested fixation methods presented significantly better rigidity compared with the gridplate. 15,17 However, in comparison with 2 separate miniplates, the use of a gridplate did not increase rigidity. 15,17 In contrast to these studies, the present study shows that the gridplate presented significantly more rigidity than 2 separate miniplates. This difference is probably explained by the specific design of our gridplate. The plate used in this study did have 2 vertical connecting bars. In addition, these bars linking both miniplates were in a symmetrical, middle position, dividing the ends of the miniplates into equal lengths. It is hypothesized that this feature results in a more equal stress distribution. However, this can only be theorized and is without supporting results from a finite element analysis study. 24,25
In the biomechanical in vitro study by Sener et al, 16 2 gridplate designs were compared with a fixation with 2 miniplates. An oblique connection added to 2 miniplates (Z-shaped miniplate) was significantly stronger than 2 unconnected miniplates. The addition of 2 vertical connecting bars at the ends of this Z-shaped design did not result in more stability. 16 In contrast to our study, these studies did not compare this with a fixation method using 3 bicortical screws in an inverted-L pattern, which is considered to be the “gold standard” regarding rigidity in mandibular advancements of up to 10 mm. 4,15 –17 Because of this classification, the authors feel that when focusing on stability, a 3 bicortical screws fixation should always be used as a benchmark and control when evaluating new methods of fixation.
The gridplate design presented in this study is a ready-made plate which comes in a standardized size and needs to be adapted (pre)operatively for proper fitting in each individual case. Its use is limited by the extent of mandibular advancement. In the case of mandibular advancement beyond 10-11 mm, other fixation methods need to be considered. In a biomechanical study regarding stabilization of SSRO with a 10 mm mandibular advancement, Sigua-Rodriguez et al 14 used a customized 3D titanium miniplate, which could also be considered an 8-hole gridplate. This customized plate presented mechanical resistance results comparable to those of the 3 bicortical screws fixation and the 2 miniplates fixation methods. 14 The use of customized CAD/CAM plates could be a resourceful option for the development of new plate designs and for patient-specific treatments, such as in the case of extremely large mandibular advancement. 14,26 However, the cost of this patient-specific technique is currently at least 10 times as much as that of the use of standardized, off-the-shelf plates. 26 Besides, until now there has been no evidence that a customized CAD/CAM plate provides additional stability when compared with 2 miniplates fixation or 3 bicortical screws in an inverted-L pattern. 14 Large mandibular advancements as part of MMA surgery are commonly required in OSA patients. 2,3 Therefore, the authors suggest that a ready-made, larger version of the gridplate design like the one tested in the present study should be produced.
Proximity between plates could also be of importance with respect to fixation rigidity. It has been theorized that a larger distance between miniplates results in more rigidity. 27 This variable was taken into account by using the same drill holes in the custom-made jig for screw positioning of the two 4-hole miniplates and the gridplate, resulting in similar (vertical) proximity between both types of miniplate.
In this study, the hybrid method resulted in less favorable results regarding its rigidity in comparison with other methods. In the case of similar or larger mandibular advancements, comparable results have been observed in other studies. 13,14,15 According to the results of the present study, it might not be very effective in clinical cases of larger mandibular advancements to add only 1 bicortical screw in the retromolar area next to a 4-hole single miniplate fixation. Instead, the authors suggest adding a second miniplate if more rigidity is required during the immediate postoperative period.
Regarding ease of handling during operative treatment, the authors believe that a single miniplate requires less surgical experience than the use of other fixations methods. Also, readjustments can be carried out with more ease than the use of 2 miniplates, a gridplate or bicortical screws. With regard to correction of improper condylar seating, readjustment of a gridplate or 2 miniplates could result in difficulties for buccal cortical screw placement, especially in relation with the mental nerve. Also, in the case of the gridplate design a more experienced surgeon might probably reduce the amount of unwanted plate bending before fixation. As mentioned before, the use of bicortical screws is less suitable for correction and requires in large advancements sufficient lingual bony overlap. With regard to the inferior alveolar nerve, its position has to be considered, especially placement of a screw in het mandibular lower cortex.
Based on the results of this study, it can be concluded that the gridplate design presented here shows mechanical fixation resistance comparable with that of 3 bicortical screws in an inverted-L pattern. Moreover, the 8-hole gridplate shows more stability compared with two 4-hole miniplates, one 4-hole miniplate or a hybrid method. In this biomechanical study, this gridplate design showed itself to be a sufficient fixation method for stabilization of SSRO in a linear mandibular advancement of 8 mm.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Screws and miniplates were donated by KLS Martin Group. KLS Martin Group did not have influence on the study design, writing of the manuscript or decision to submit the manuscript.
