Abstract
Immediate obturation of the patient undergoing maxillectomy who is not undergoing formal autologous reconstruction is important for immediate form and function of the patient. Exophytic tumors, that are large in dimension can make pre-operative obturator formation challenging. Traditional methods of obturator fabrication involve a physical or digital impression. Preoperative virtual surgical planning for tumor resection and reconstruction using free tissue transfer has become a mainstay in head and neck reconstruction. We describe a variation of this for a patient unable to undergo free tissue transfer where the authors used preoperative virtual surgical planning and CAD/CAM technologies to perform tumor resection, and fabricated an obturator based on the CT imaging alone.
Introduction
Immediate reconstruction is extremely important for the form and function of the maxillectomy patient. 1 Despite this, not all patients are ideal candidates for immediate free tissue reconstruction. Obturator reconstruction has been shown to give patients good quality of life and function. 2 Traditional methods of obturator fabrication involve a physical or digital impression. Large and exophytic tumors may make impressions by either methods challenging. Virtual surgical planning (VSP) and three-dimensional (3-D) printing have become standard in the treatment of the complex head and neck cancer patient. These technologies have led to improved outcomes, decreased surgical time, and increased precision. 3,4 Despite the advances in VSP and 3-D printing, there are no reported cases of these technologies being utilized to fabricate an interim maxillary obturator for a post ablative defect when traditional impression techniques are not feasible. We present a case of a female with a rapidly expanding tumor of the maxilla, prohibiting traditional obturator fabrication techniques, who was not eligible for immediate free tissue transfer, in which an immediate surgical obturator was created from only CT data.
Report of a Case
84-year-old female with compromised medical history was referred to the Oral and Maxillofacial Surgery (OMFS) Clinic at the University of Illinois at Chicago (UIC) with a speckled erythroleukoplakic lesion of the anterior maxilla with significant bone loss and pain with mastication and speaking. At the consultation appointment an incisional biopsy was obtained and the patient was sent for a formal malignancy workup. The biopsy returned as sarcomatoid squamous cell carcinoma of the maxilla. When the patient presented for review of pathology and treatment discussion, the tumor had significantly increased in size (Figure 1). After thorough discussion with the family and consideration for the patient’s multiple comorbidities, the decision was made to perform a curative ablation of the maxillary lesion and reconstruction with a surgical obturator. The fungating lesion of the anterior maxilla made a traditional alginate impression impossible. Digital impressions were attempted with Trios 3D scanner (3Shape A/S, Copenhagen, Denmark) however the lesion distorted the ability to obtain an accurate scan of the anterior maxilla and depth of the maxillary vestibule. The decision was made to fabricate a 3-D printed surgical obturator based off the preoperative CT scan. A standard CT face with fine cuts (0.5 mm) was obtained. A virtual surgical planning session was completed with 3D systems (3D Systems, Inc, Littleton, CO) and predictive surgical resection was undertaken (Figure 2). The surgical resection was planned for 1 cm margins as per standard technique for squamous cell carcinoma. A virtual obturator was then fabricated to the post-resection defect (Figure 3). Stereolithic models and the obturator were then printed by 3D systems based on the virtual surgical plan (Figure 4). The obturator was composed of acrylic and epoxy photopolymers, which is biocompatible and approved to be in tissue contact for greater than 30 days.
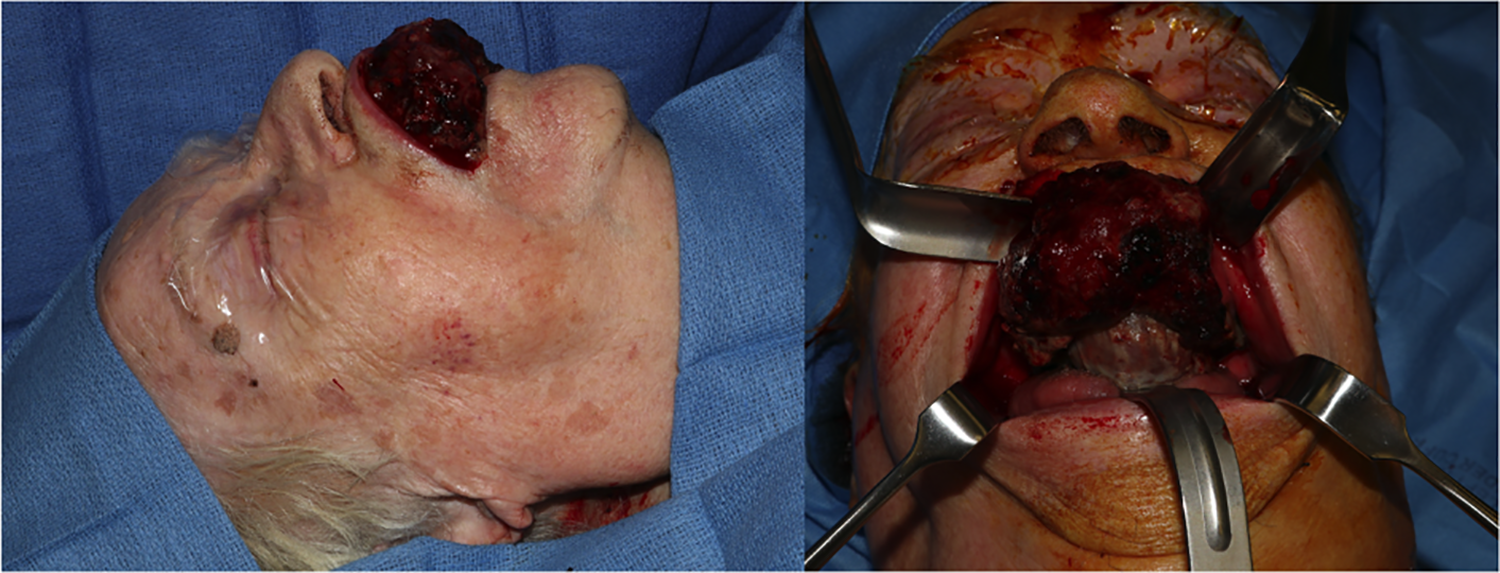
Lesion at time of surgery.
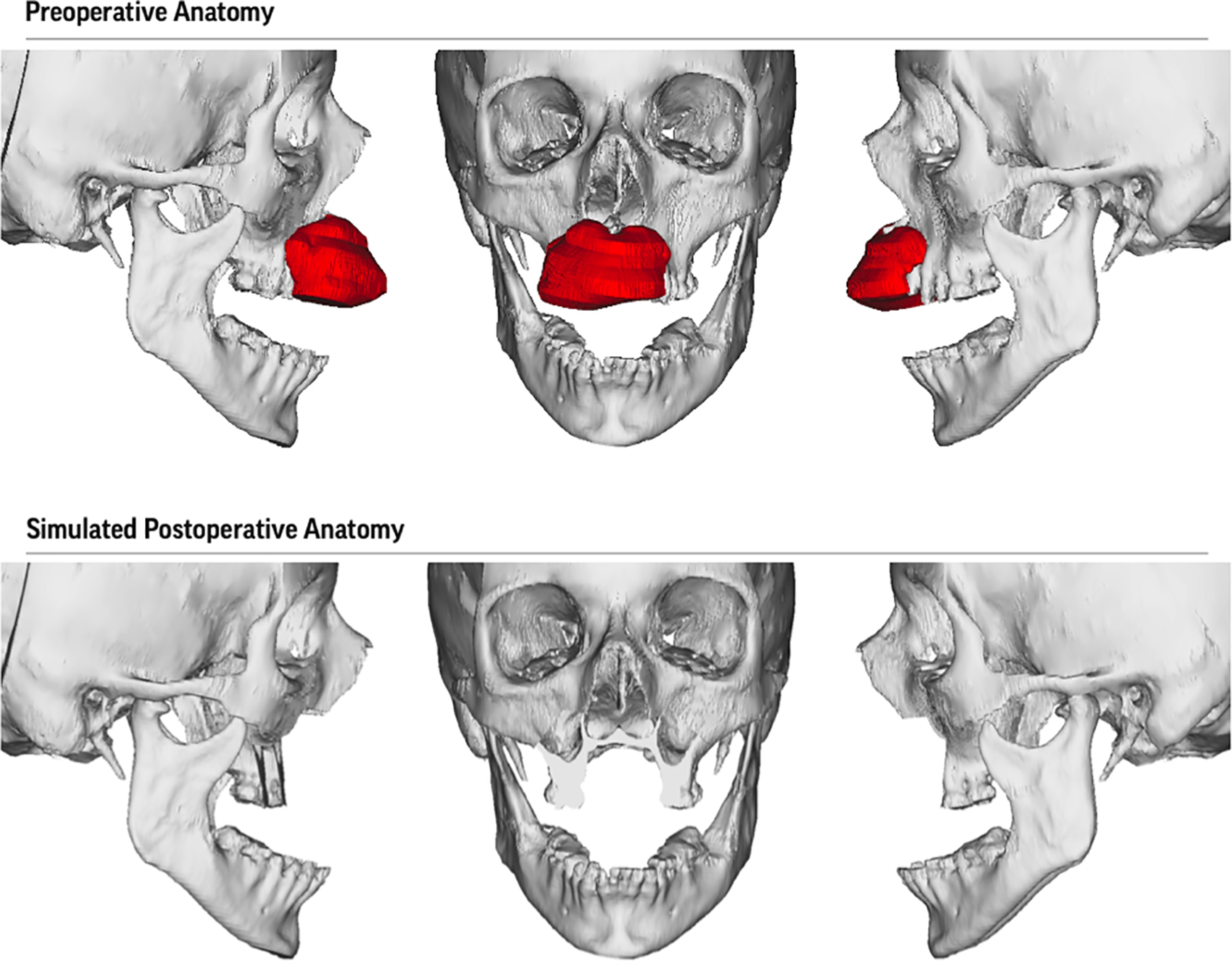
VSP rendering of tumor and resection plan.
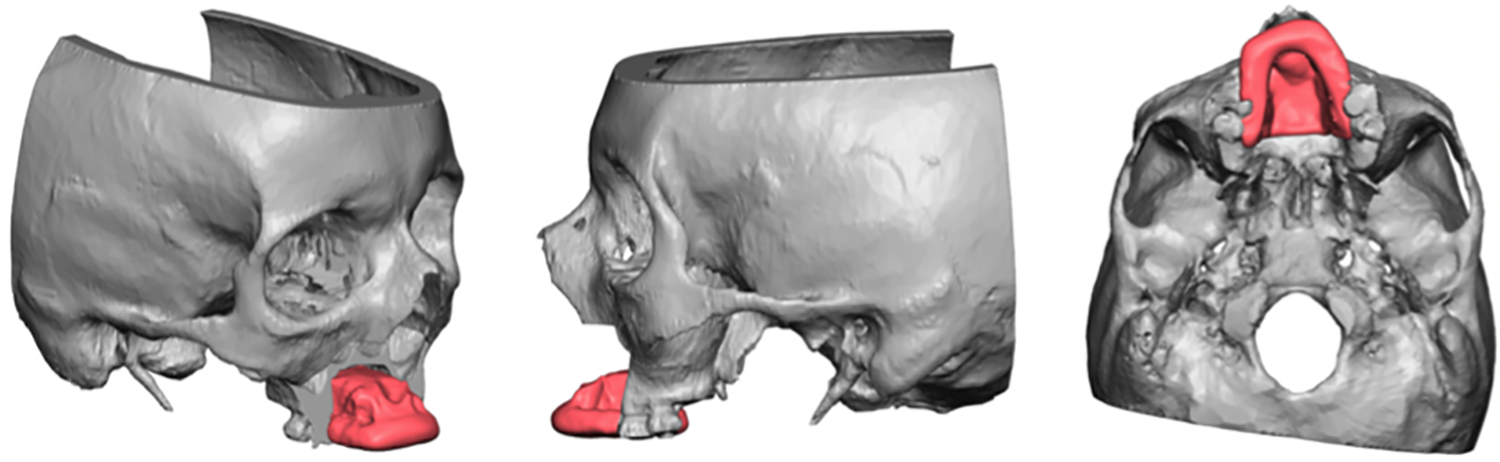
VSP plan for surgical obturator.
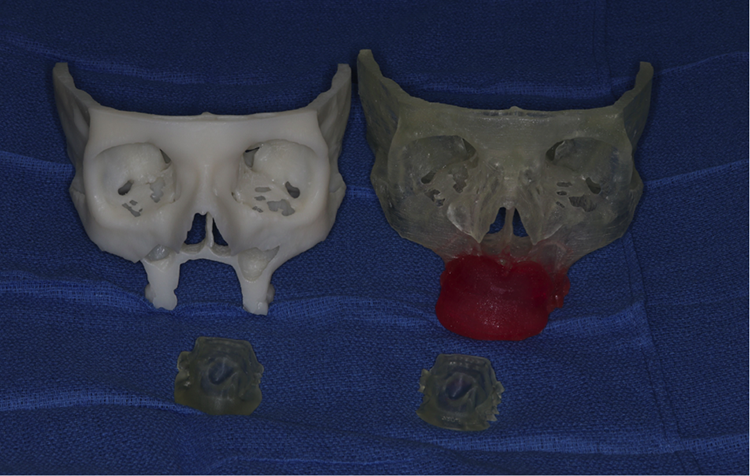
Stereolithic models and stents.
The patient was then taken to the operating room, where a tracheostomy was performed to stabilize the airway. An anterior maxillectomy was completed according to the virtual surgical plan, since no tissue reconstruction was being planned, no cutting guides were utilized. A traditional alginate impression was taken at this time for fabrication of a traditional dental obturator. The obturator was sterilized by soaking the prothesis in betadine. The prefabricated interim obturator was then seated with minimal adjustment required (Figure 5). An alginate impression was taken for formal obturator fabrication. The defect was relined with coe-soft and the obturator was secured with a 16 mm 2.0 mm screw (Stryker-Leibinger, Freiburg, Germany) to the residual palate. The obturator was also wired to the remaining posterior dentition bilaterally.
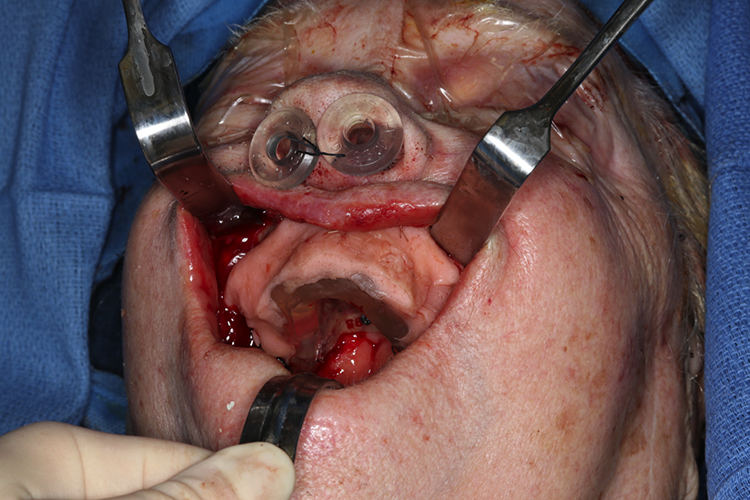
Stent in place.
After decannulation the patient was able to tolerate PO and phonate well with the interim obturator in place. She was discharged home after an uneventful hospital course. The patient returned for follow up 3 weeks post op where the interim obturator was removed and replaced with a traditional obturator fabricated by maxillofacial prosthetic department from the intraoperative impression. An adequate dental prothesis was able to be made from the impression, negating the need for a 3d printed obturator. The 3d printed surgical obturator was left in place until the traditional obturator could be placed to help prevent tissue contraction. The formal obturator was placed to allow for dental rehabilitation and better function for the patient. Minimal adjustments were needed to the final prothesis.
Discussion
Large and exophytic tumors of the maxillectomy traditionally have required packing of wounds and delayed obturator placement when tissue transfer is not used. Immediate rehabilitation is always preferred. Obturation has shown a benefit to the quality of life, form, and function of these patients. 2 Ideally surgical obturators are fabricated preoperatively and require minimal intraoperative adjustments. However, to fabricate these obturators, either digital or physical impressions must be taken. 5
Virtual surgical planning has fundamentally changed the field of oral and maxillofacial surgery, allowing completion of complex surgeries with decreased operating time 6 and more precision 7 than ever before. Virtual surgical planning and Stereolithic printing is an evolving technology. Using a combination of these techniques we were able to create a surgical obturator preoperatively where before these techniques this would not have been possible. This allows for less time in the operating room and allows for immediate return of patient’s form and function. There is new evidence that a combination of MRI and CT data may provide an even more accurate image and allow for increased accuracy for the resection and reconstruction. 8
This case shows that an adequate obturator can be created using just CT data and VSP without an impression.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
