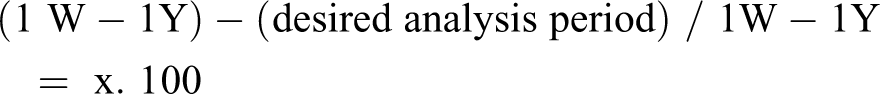Abstract
The purpose of this retrospective study was to determine postoperative volume differences associated with orthognathic surgery after controlling for time, gender, age, and side of face. Three-dimensional (3D) photographs of 10 patients submitted to simultaneous Le Fort I + Bilateral Sagittal Split osteotomies were analyzed. The images were obtained using a Vectra® M3 device (Canfield, NJ, USA) and were captured postoperatively, at 1 week (1S), 1 month (1M), 2 months (2M), 6 months, (6M) and 1 year (1A). The photo taken at 1A was used as the basis of comparison for the other photos (1S, 1M, 2M, and 6M). Greatest facial volume was observed at 1 week after surgery (42.54 cm3, SD = 29.71 cm3), with men in this period showing higher values (60.20 cm3, SD = 36.75 cm3) than women (30.76 cm3, SD = 19.04 cm3). The most extensive facial volume reduction occurred between the first week and the first month; postoperatively (52.1%). No significant difference was found between age and side groups.
Introduction
Orthognathic surgery is a highly complex procedure and has been widely used worldwide in the treatment of dental and skeletal deformities. Patients are generally very anxious and apprehensive about the effects of orthognathic surgery on their face and day-to-day activities, especially in the immediate postoperative period. Understanding and clarifying patients’ preoperative questions is essential for a successful treatment. 1 Patients undergoing orthognathic surgery are more likely to rate their experience as positive if accurate information is provided prior to the surgical procedure. 2 Additionally, the surgeon who provides accurate information regarding the surgical sequelae and recovery period will positively influence the patient’s perception of the success of the surgery and the psychological impact of the postoperative experience. 3
The most common sequelae of orthognathic surgery include pain, edema, nausea and vomiting, trismus, and negative social and functional interference. 4 Most of these symptoms usually disappear around the first postoperative week, except for facial edema. 5 Precisely quantifying the extent and duration of postoperative edema is important in the treatment of patients who will undergo orthognathic surgery, especially those who are very anxious to know when the end result will be achieved. 3
Different techniques have been proposed for measuring postoperative edema. The use of magnetic resonance imaging or cone beam computed tomography (CBCT) is not justifiable for long-term studies due to the high cost and exposure of the patient to high levels of ionizing radiation. 3 Fortunately, recent advances in three-dimensional imaging technology have provided the oral and maxillofacial surgeon a powerful tool for obtaining quick, accurate, and non-invasive images of the face. 6 The three-dimensional photo (3D photo), also called stereophotogrammetry, captures the face in milliseconds with its real texture, colors, and scales. 7 Moreover, the images have a high level of accuracy, precision, and reliability comparable to CBCT. 8 –10
Therefore, this study aimed to retrospectively evaluate the changes in the facial volume of patients undergoing bimaxillary orthognathic surgery using 3D photo.
Materials and Methods
This study was approved by the ethics committee of the School of Dentistry of Ribeirão Preto, University of São Paulo, Brazil, process number of the Certificate of Presentation for Ethical Consideration (CAAE - Certificado de Apresentação para Consideração Ética, in Portugueses language): 60734016.1.0000.5419.
Sampling Criteria
A retrospective study analyzed the medical records of all patients who underwent orthognathic surgery at the Residency Training Program in Oral and Maxillofacial Surgery at School of Dentistry of Ribeirão Preto (hereafter ROMS), from August 2013 to August 2015.
The criteria for inclusion in the study were: skeletally mature patients who underwent orthognathic surgery following the same therapeutic protocol, consisting of concomitant Le Fort I osteotomy and bilateral sagittal split osteotomy (BSSO), use of miniplates and self-tapping screws of 1.5 and 2.0 mm in the conventional system for internal fixation, osteotomies performed applying reciprocating saws and chisels, bone movements at any planes (AP, vertical, and transversal) up to 8 mm, presence in regularly scheduled postoperative follow-ups, and having the 3D images taken on each follow-up. In addition, the exclusion criteria were: patients with some healthy conditions that interfere with the bone physiology (i.e. osteoporosis, hyperparathyroidism) or cause soft tissue swelling (i.e. endothelial dysfunction), patients taking any medication in a regular basis that interfere with the bone or soft tissue physiology (i.e. bisphosphonates, corticosteroids), previous history of orthognathic surgery, patients submitted to mentoplasty or segmental surgery, occurrence of undesirable fractures during the procedure, need for additional trans or postoperative surgical procedure (inferior alveolar nerve lateralization, biomaterial or bone graft placement, dental implant, removal of miniplates and/or screws, correction of nasal septum deviation, etc.), occurrence of any postoperative complication (i.e. infection, hematoma, internal fixation failure), use of maxillo-mandibular immobilization in the postoperative period, use of additional instruments during the osteotomies in addition to reciprocating saw and chisels (i.e. piezoelectric tips), and use of medication different from the established protocol. Data were collected based on age, sex, operation time required, type of malocclusion according to Angle classification, and the movements applied in each plane (AP, vertical, and transversal) in millimeters (mm).
Method
Clinical Methodology
Every patient referred for orthognathic surgery underwent a thorough anamnesis, a rigorous clinical examination, and an analysis of orthodontic documentation, which necessarily included recent plaster models, panoramic radiographs, and lateral and frontal cephalograms.
Surgical Methodology
The surgical procedures were performed under general anesthesia in the hospitals attended by the ROMS. Surgical procedures were always performed by a faculty member and a senior resident. The patients were submitted to nasotracheal intubation in the horizontal dorsal decubitus position. According to the anesthetic protocol, 2 g of Cefazolin Sodium and 10 mg of Dexamethasone were administered intravenously as antibiotic and antiemetic prophylaxis, respectively.
The surgical procedure consisted in the infiltration of an anesthetic solution containing 2% lidocaine and epinephrine IU along the mucobuccal fold of the maxilla. With the aid of a dissecting tip mounted on an electrocautery, the maxillary access was made with a lower vestibular incision, approximately 4 mm from the mucobuccal fold, from the first molar on one side to the contralateral first molar. After the mucoperiosteal detachment and the subsequent exposure of the bone surface of the maxilla and the nasal cavity, with the aid of reciprocating saw and chisels, a Le Fort type I osteotomy was performed, followed by downfracture. The maxillo-mandibular immobilization was obtained interposing the intermediate surgical guide and the maxilla was then fixed with conventional 1.5 mm plates and self-tapping screws. After that, an anesthetic solution was infiltrated containing 2% lidocaine and epinephrine 1:200.000 IU on the oblique ridge and the mandible was accessed with a linear incision to the mandibular ramus. After adequate exposure, the BSSO was obtained; this step was repeated bilaterally. The fracture and mobilization of the fragments were then obtained on both sides and, immediately after, the maxillo-mandibular immobilization was achieved. This osteotomy was fixed with the conventional 2.0 mm system, using only 1 straight plate fixed on each side with four 5 mm self-tapping screws. After this, the maxillo-mandibular immobilization was removed, the occlusion was checked, and soft tissue synthesis was performed with absorbable polyglactin 910-based 4-0 diameter suture yarn.
Postoperative Orientation
Patients were discharged the day after surgery, with postoperative recommendations and prescription. The first postoperative follow-up was scheduled for 7 days after surgery. The prescription consisted of 500 mg of Amoxicillin every 6 hours for 7 days, 100 mg of Ketoprofen every 8 hours for 3 days, and 500 mg of Dipyrone every 6 hours in case of pain, all orally. The diet consisted of liquid for 4 weeks, a pasty diet for another 2 weeks, and, after this period, the patient was instructed to return to their routine diet, avoiding foods that required intense chewing (peanuts, nuts, barbecue, among others) for another 2 months.
Postoperative Follow-ups and Guidelines
On the first postoperative follow-up, all instructions were confirmed, all questions were answered, and the patient was reassessed clinically and radiographically (panoramic radiography, frontal and lateral cephalograms). Following ROMS protocol, after this follow-up, the patients were scheduled to return at 1 month, 2 months, 6 months, and 1 year after their orthognathic surgery.
The ROMS’s protocol demands annual follow-ups of all orthognathic surgery patients, with the last one before discharge set at 5 years after surgery. In all these annual returns, 3D images were taken; however this study evaluated only images of the first postoperative year.
Capturing Photos
Also following our protocol, the 3D images were obtained in the Stomatognathic System Electromyography Research Laboratory (LAPESE) and were taken on all patient returns, i.e.: at 1 week after the procedure (1 W) 1 month (1 M), 2 months (2 M), 6 months (6 M), and 1 year (1Y), the latter being used as baseline. Although a preoperative 3D image was also taken, it was not included in this study. The images were captured using a Vectra® M3 [(Canfield, NJ, USA), (Figure 1)]. The capture system has a geometric resolution of 1.2 mm (triangle edge length), a capture time of 3.5 milliseconds, on-board modular intelligent flash units, stereophotogrammetry technology, floor stand, and a Dell® computer (Dell Computadores do Brasil Ltda., RS, Brazil) with a flat screen. The associated software included were: Face Sculptor®, RBX® image processor, VECTRA® 3D Analysis Module, Mirror® Photo File® and Mirror,® Photo Tools® (Canfield, NJ, USA).

Vectra® M3 device with capture system with a geometric resolution of 1.2 mm (triangle edge length), a capture time of 3.5 millisecond, on-board modular intelligent flash units, stereophotogrammetry technology, floor stand, stool.
Protocol for Marking Landmarks
The establishment of facial landmarks for marking and recording measurements/distances was based on previous studies. 11 Farkas 12 suggested marking 50 landmarks. This study uses 32 of the reference points on Farkas list, 12 with the addition of reference points Cheek - Chk [r], Chk [l], introduced by Ferrario et al., 11 and Gnation (Gn). The landmarks and their abbreviations used in this study were Trichion (Tr), Glabella (G), Nasion (N), Pronasale (Prn), Columella (C), Subnasale (Sn), Labiale superius (Ls), Stomion (Sto), Labiale inferius (Li), Sublabiale (Sl), Pogonion (Pg), Gnation (Gn), Mento (Me), Cheilion (Ch[r] Ch[l]), Exocanthion (Ex[r] Ex[l]), Endocanthion (En[r] En[l]), Frontotemporale (Ft[r] Ft[l]), Cheek (Chk[r] Chk[l]), Orbitale (Or[r] Or[l]), Zygion (Zy[r] Zy[l]), Alare (Al[r] Al[l]), Crista philtri (Cph[r] Cph[l]), Tragion (T[r] T[l]), Gonion (Go[r] Go[l]).
The landmarks were marked with Make-B eyeliner (O Boticário®, SP, Brazil), and this procedure was performed by the same operator on all patients studied.
Before marking the landmarks, each patient used a headband in order to hold back the hair and keep the area clear. A sterile gauze soaked in 70% alcohol was systematically wiped over each patient’s face in order to cleanse the skin of impurities, oiliness, and makeup.
Digital Marking of Landmarks
In order to digitally acquire each of the points marked on the patient’s face, a procedure was adopted and standardized, whereby the image was enlarged so that the point occupied the entire computer screen, which allowed the central region of the point to be selected. The purpose of this procedure was to decrease the chances of the digital marking not being at the center of the point and its standardization minimized possible variations in the results (Figure 2).
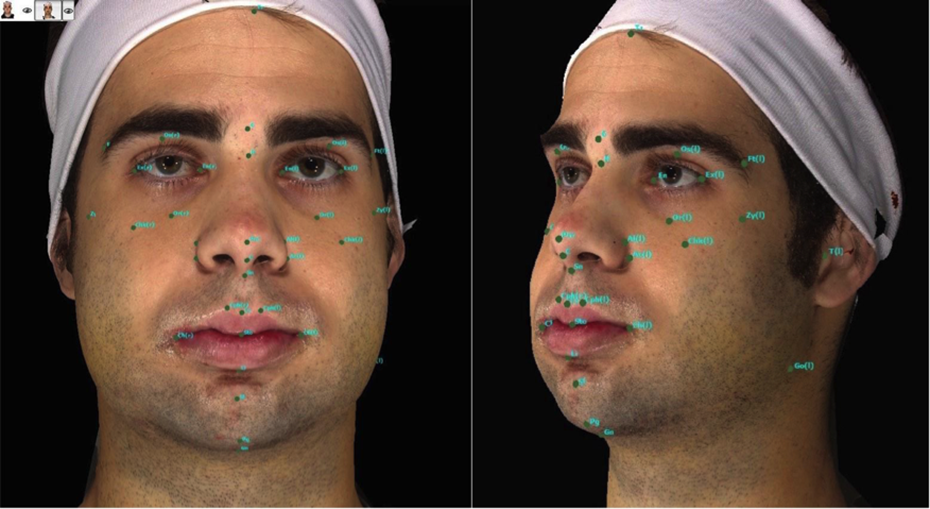
Patient at 1 postoperative week (1 W), showing the digitally marked points based on the previous manual marking.
Selection of the Area to be Calculated
After all the images had been duly marked, a single evaluator selected the points and calculated the areas measured. The points used to determine the areas to be measured were: T [r], Zy [r], Or [r], N, Or [l], Zy [l], T [l], Go [l] Me, Go [r], T [r] (Figure 3), for measurement of the whole face. The points marked to select the right side of the face were: T [r], Zy [r], Or [r], N, Prn, Al [r], Ac [r], Sn, Ls, Sto, Li, Sl, Pg, Gn, Me, Go [r]. For the left side of the face, the points marked to select the area were: T [l], Zy [l], Or [l], N, Prn, Al [l], Ac [l], Sn, Ls, Sto, Li, Sl, Pg, Gn, Me, Go [l] (Figure 4). Volume change was obtained by overlaying the images of periods 1 W, 1 M, 2 M, and 6 M with that of the final period 1Y, and calculating the difference between them in a process we have denominated Subtraction (Figures 5 and 6). The surface area was generated including all soft tissue of the middle and lower third of the face, excluding the nasal cavity only in unilateral measurements. The volume difference was expressed in cubic centimeters (cm3).
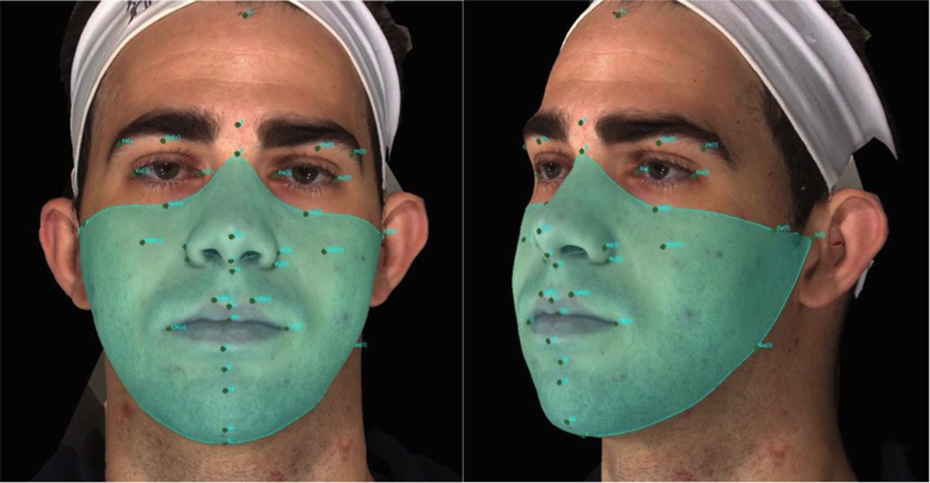
Patient at 1 postoperative year (1Y), showing the total area selected by points: T [r], Zy [r], Or [r], N, Or [l], Zy [l], T [l], Go [l], Me, Go [r], T [r].
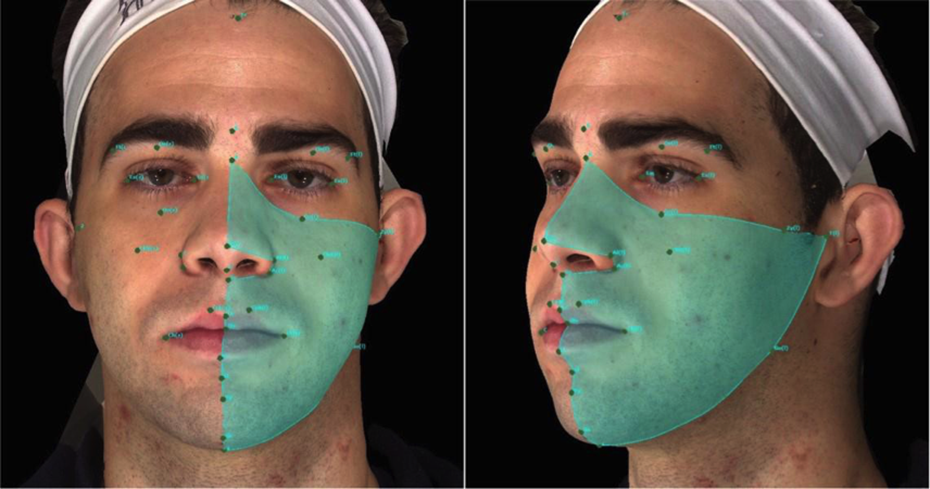
Patient at 1 postoperative year (1Y), showing the area on the left side selected by points: T [l], Zy [l], Or [l], N, Prn, Al [l], Ac [l], Sn, Ls, Sto, Li, Sl, Pg, Gn, Me, Go [l], T [l].
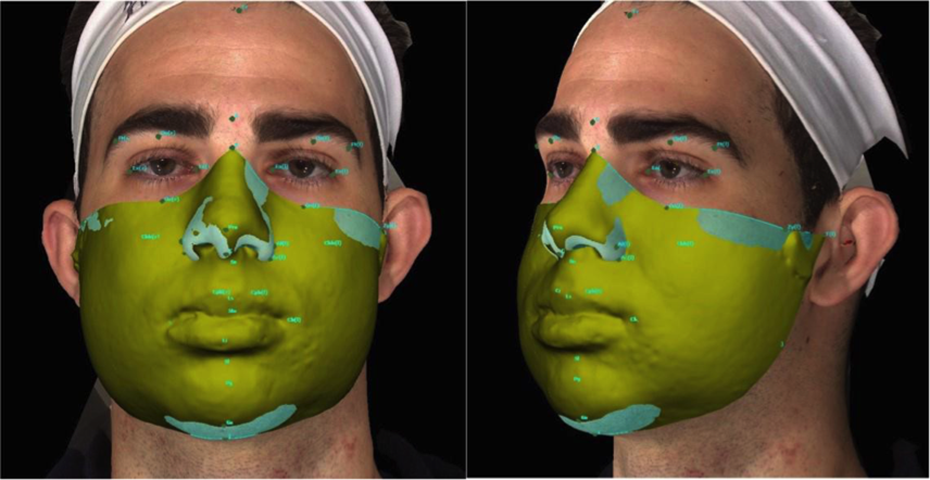
Overlay of 3D photos from periods 1 W and 1Y in order to subtract the total volumes between these 2 periods (1W–1Y).
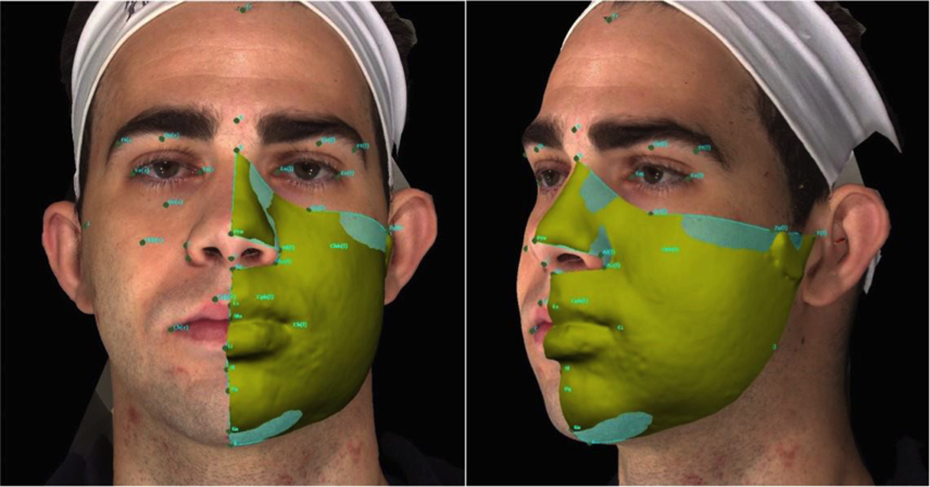
Overlay of 3D photos from periods 1 W and 1Y in order to subtract the volume of the left side of the face between these 2 periods (1W–1Y).
Reduction of Facial Volume
The percentage of volume reduction was obtained by the formula proposed by Kau et al. 13 :
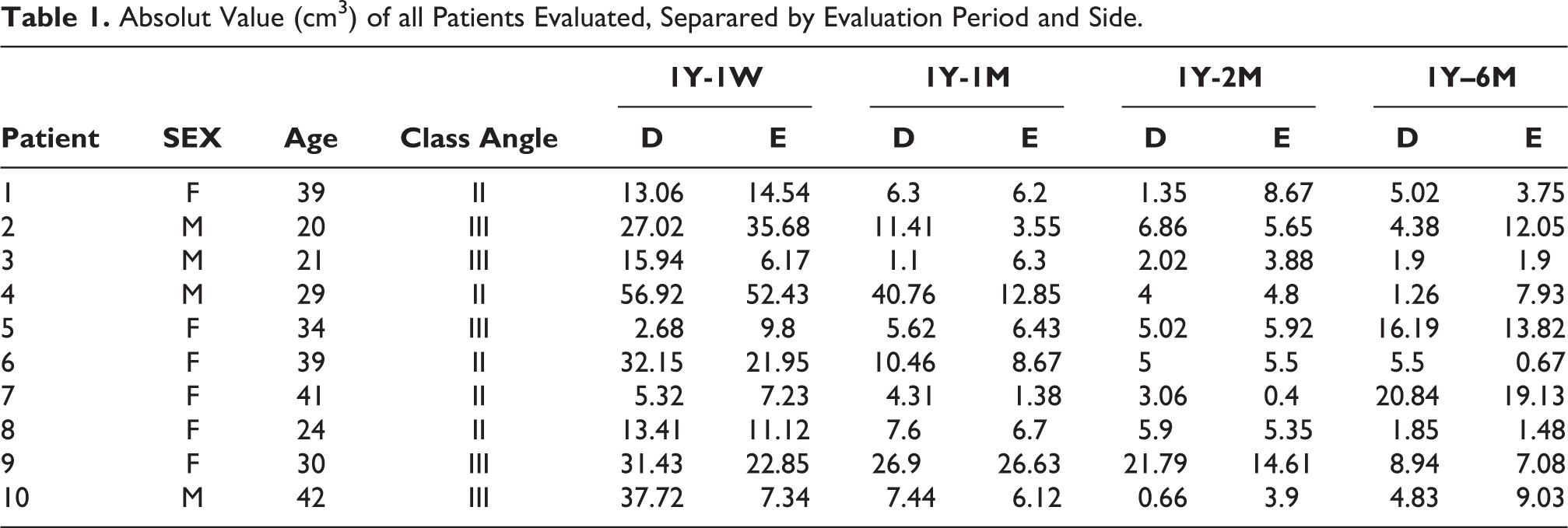
Therefore, the mean value of 1W–1Y (Table 1) was considered as a 100% reduction in face volume. Thus the percentage corresponding to the average values of 1M–1Y; 2M–1Y; 6M–1Y could be found.
Absolut Value (cm3) of all Patients Evaluated, Separared by Evaluation Period and Side.
Statistical Methodology
Initially the data were presented through descriptive measures such as mean, standard deviation, minimum, median, and maximum. All comparisons between sex, age, time, and face side were analyzed using the linear regression model with mixed effects (random and fixed effects). Linear models of mixed effects are used in the analysis of data in which responses are grouped (more than 1 measure for the same individual) and the assumption of independence between observations in the same group is not adequate. 14 For the comparisons, the orthogonal contrasts post-test was used. All graphs presented were made using R software, version 3.2.1 (Bell Laboratories®, NJ, USA) and the analyses using SAS 9.0 (SAS Institute Inc.®, NC, USA). A significance level of 5% was adopted for all comparisons.
Results
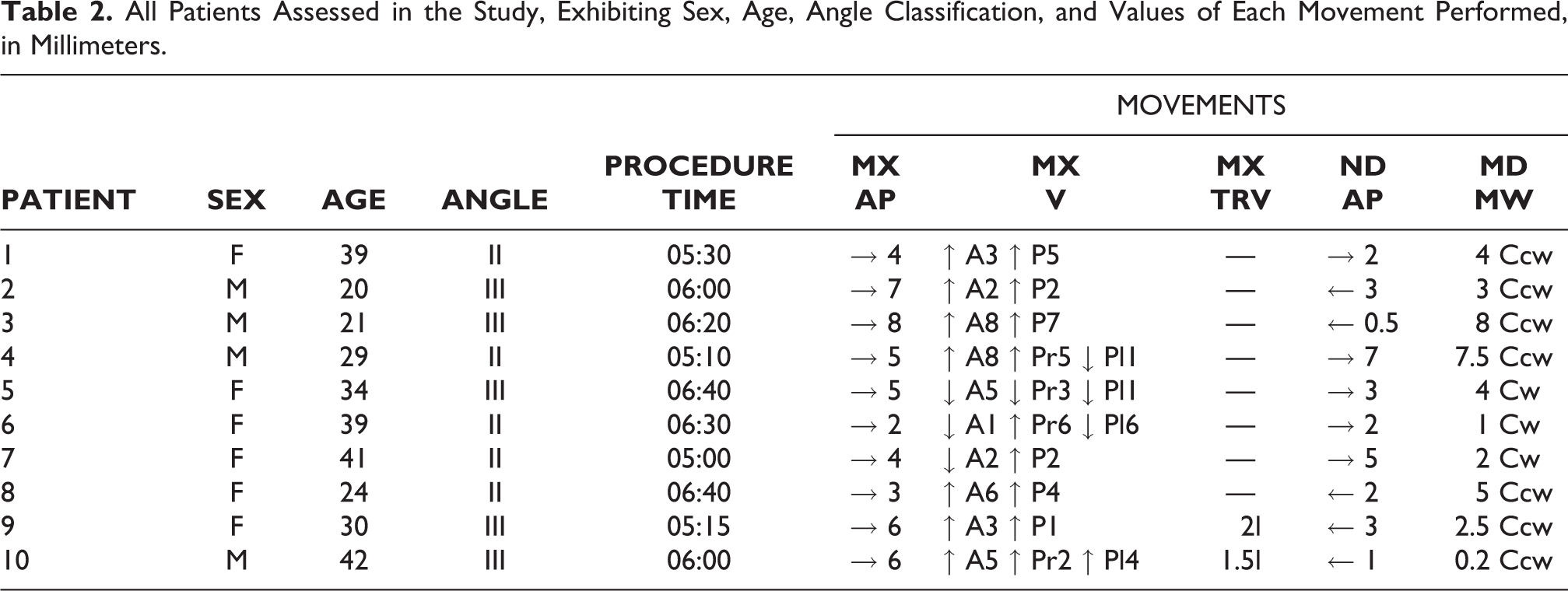
Of the 70 medical records of orthognathic surgeries available for the period of this study, 10 met the inclusion/exclusion criteria previously mentioned and, therefore, were selected. Of the 10 patients, 6 were women (60%) and 4 were men (40%). Age ranged from 20 to 42 years old, with an average of 31.9 years old. According to the Angle Classification, 5 were Class II patients (50%) and 5 Class III (50%) (Table 1). The movements applied in the maxilla were: in the anterior-posterior (AP) plane consisted in advancement and ranged from 2 to 8 mm, in the vertical plane consisted in upward movements ranged from 1 to 8 mm in anterior maxilla and from 1 to 7 mm in the posterior, and the transversal plane was restricted to maxillary midline correction, which ranged from 0 mm to 2 mm. The movements applied in the mandible were: in the AP plane ranged from 3 mm of backward movement to 7 mm of forward movement, while the anterior mandible rotation varied from 0.2 to 8 mm of counter clockwise movement and 2 from 4 mm of clockwise movement. The total time to perform the surgical procedure ranged from 5.0 to 6.40 hours, with a mean of 5.785 hours (Table 2).
All Patients Assessed in the Study, Exhibiting Sex, Age, Angle Classification, and Values of Each Movement Performed, in Millimeters.
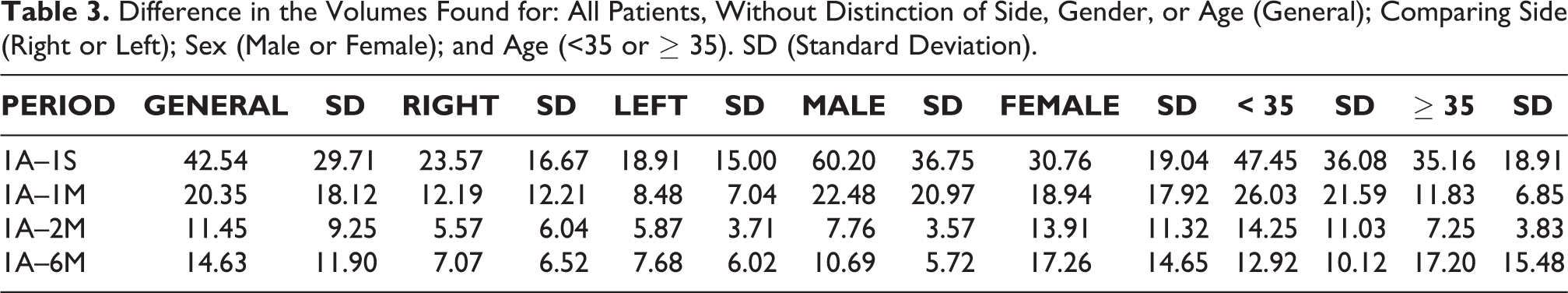
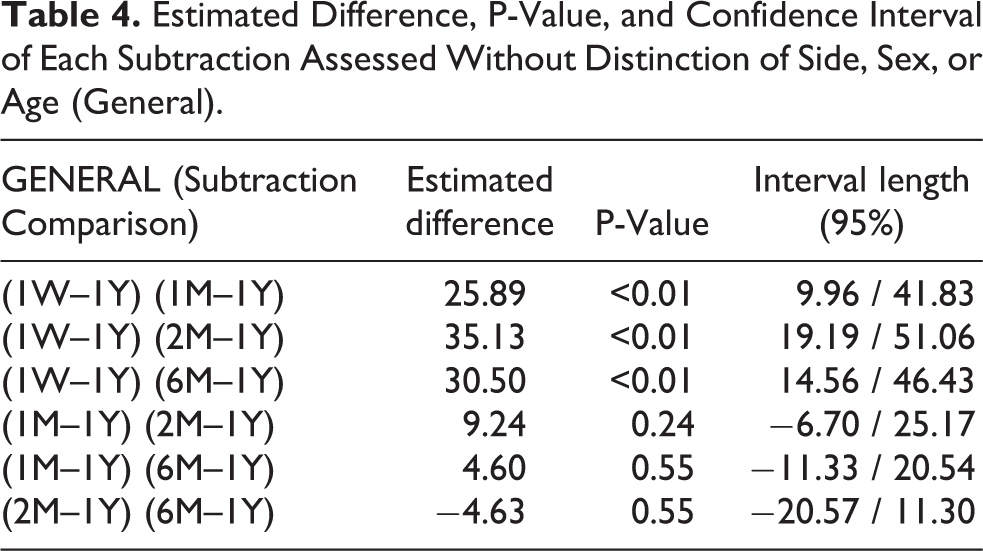
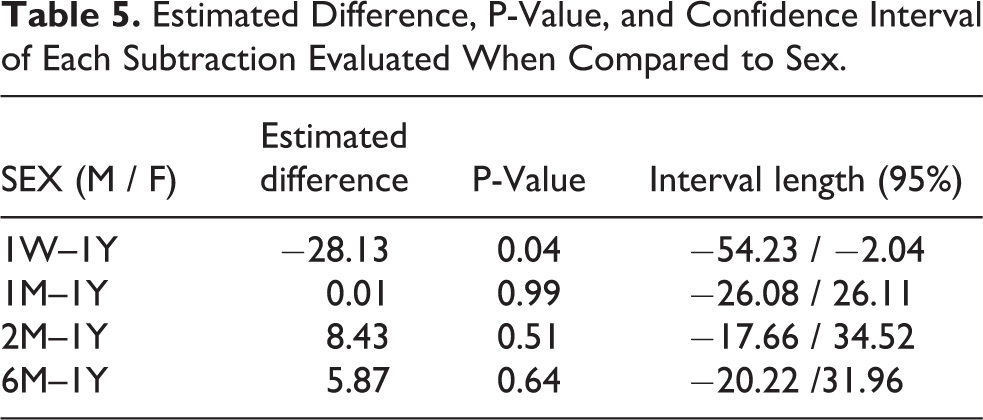
Analyzing face volume differences of all patients as a group (General), we observed that the value obtained in the subtraction 1W–1Y, (42.54 cm3, SD = 29.71 cm3) presented a statistically significant difference when compared to the other subtractions, 1M–1Y (20.35 cm3, SD = 18.12 cm3), 2M–1Y (11.45 cm3, SD = 9.25 cm3) and 6M–1Y (14.63 cm3, SD =11.90 cm3)—Table 3. However, when these subtractions were compared to each other, no statistically significant difference was observed, even though they presented decreasing values (Table 4). However, the analysis of the variable sex produced some additional differences (Figure 7). In the subtraction 1W–1Y, men had a volume difference of 60.20 cm3 (SD = 36.75 cm3), while women presented 30.76 cm3 (SD = 19.04 cm3). This was the only subtraction with a statistically significant difference between the sexes. In the subtraction 1M–1Y, men and women presented, respectively, 22.48 cm3 (SD = 20.97 cm3) and 18.94 cm3 (SD = 17.92 cm3). In 2M–1Y, men had 7.76 cm3 (SD = 3.57 cm3) and women had 13.91 cm3 (SD = 11.32 cm3). Comparing the final subtraction, 6M–1Y, men and women presented, respectively, 10.69 cm3 (SD = 5.72 cm3) and 17.26 cm3 (DP = 14.65 cm3) (Tables 3 and 5).
Difference in the Volumes Found for: All Patients, Without Distinction of Side, Gender, or Age (General); Comparing Side (Right or Left); Sex (Male or Female); and Age (<35 or ≥ 35). SD (Standard Deviation).
Estimated Difference, P-Value, and Confidence Interval of Each Subtraction Assessed Without Distinction of Side, Sex, or Age (General).
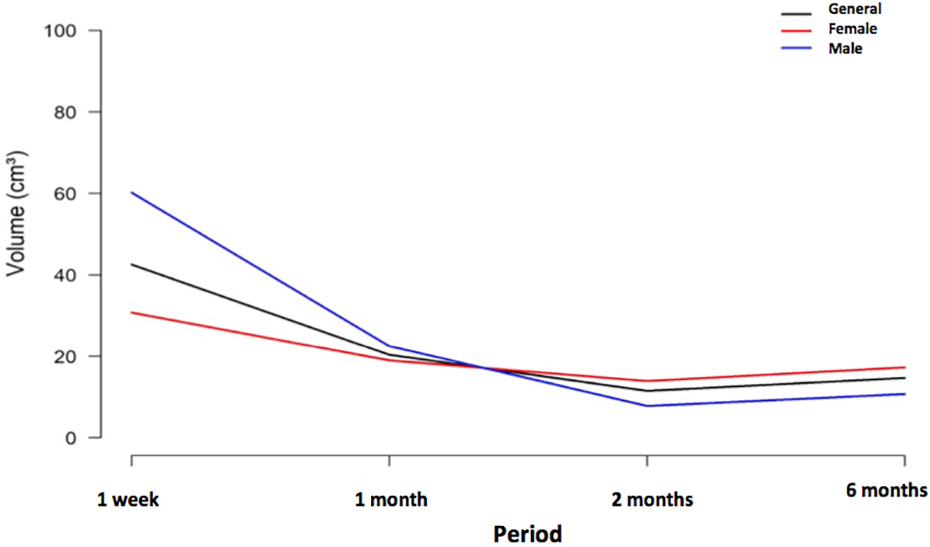
Face volume variation in patients who underwent orthognathic surgery regarding the general and sex values. The values were achieved subtracting the periods of 1 W, 1 M, 2 M, and 6 M to 1Y.
Estimated Difference, P-Value, and Confidence Interval of Each Subtraction Evaluated When Compared to Sex.
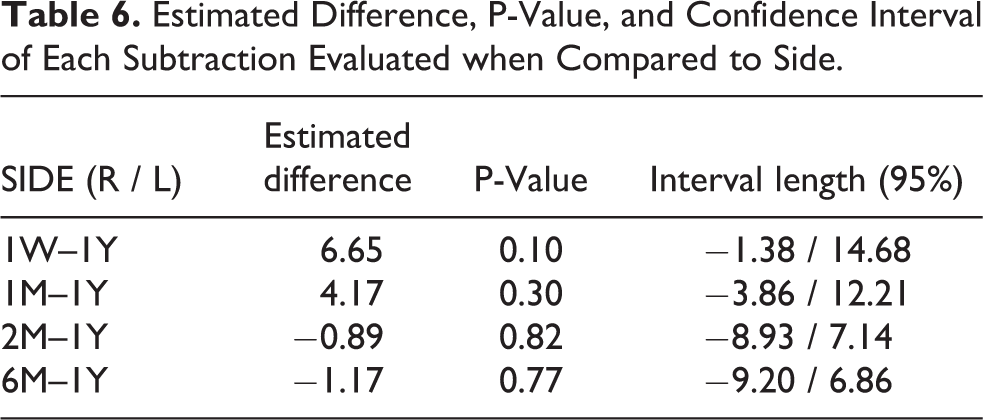
On analyzing the separately operated sides, we observed that, in the subtractions 1W–1Y and 1M–1Y, the right side presented, respectively, 23.57 cm3 (SD = 16.67 cm3) and 12.19 cm3 (SD = 12.21 cm3), while the left presented 18.91 cm3 (SD = 15.00 cm3) and 8.48 cm3 (SD = 7.04 cm3). The following values of subtractions for both sides remained similar (Tables 3 and 6, Figure 8), and showed no statistically significant difference.
Estimated Difference, P-Value, and Confidence Interval of Each Subtraction Evaluated when Compared to Side.
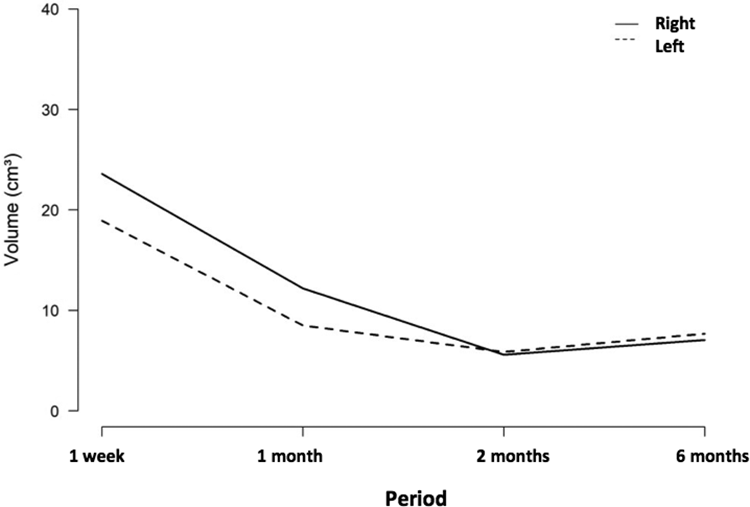
Differences in face volume at the left and right sides in women and men who underwent orthognathic surgery. The values were achieved subtracting the periods of 1 W, 1 M, 2 M, and 6 M to 1Y.
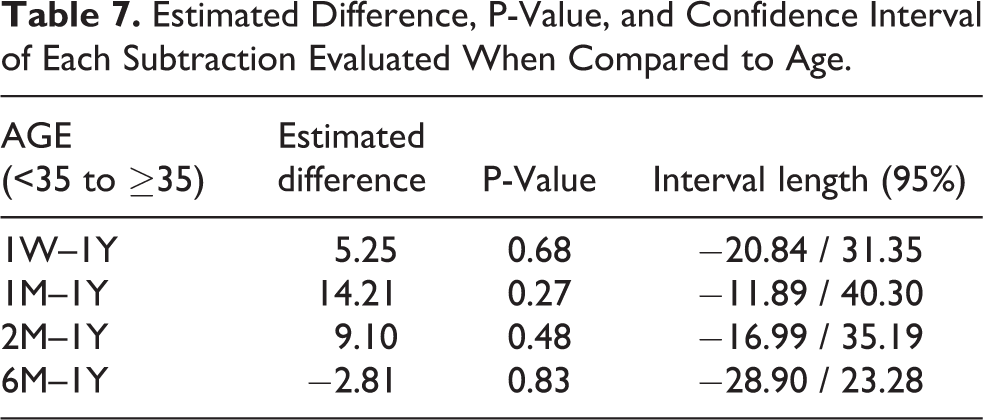
When the influence of age was analyzed, the facial volume at the subtraction 1W–1Y of the group <35 years was 47.45 cm3 (SD = 36.08 cm3) and the group ≥ 35 years was 35.16 cm3 (DP = 18.91 cm3). In 1M–1Y, the values of the groups <35 years and ≥ 35 years were, respectively, 26.03 cm3 (SD = 21.59 cm3) and 11.83 cm3 (SD = 6.85 cm3). In the subtraction 2M–1Y, the values of the groups <35 years and ≥35 years were, respectively, 14.25 cm3 (SD = 11.03 cm3) and 7.25 cm3 (SD = 3.83 cm3). Finally, in 6M–1Y, the values of the groups <35 years and ≥35 years were, respectively, 12.92 cm3 (DP = 10.12 cm3) and 17.20 cm3 (DP = 15.48 cm3). No statistically significant difference was observed in any of the above-mentioned subtractions (Tables 3 and 7, Figure 9).
Estimated Difference, P-Value, and Confidence Interval of Each Subtraction Evaluated When Compared to Age.
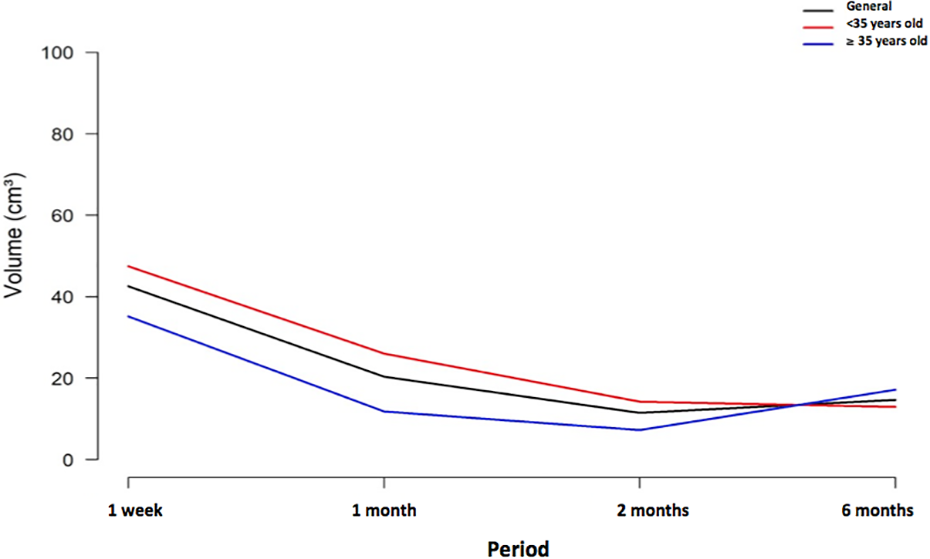
Face volume variation in patients who underwent orthognathic surgery, regarding the general and age (<35 and ≥35) values. The values were achieved subtracting the periods of 1 W, 1 M, 2 M, and 6 M to 1Y.
The facial volume reductions in the subtractions 1M–1A, 2M–1A, and 6M–1A were, respectively, 52.1%, 73%, and 65.6%. Clearly the most intense facial volume reduction occurred during the first postoperative month.
Discussion
Orthognathic surgery generates a variety of expectations not only in patients but also in their relatives, and these expectations, in turn, raise questions, many of which arise from doubts about the surgical procedure itself, and how this procedure will affect the postoperative period. Additionally, patients and families need information in order to adjust their day-to-day activities to the demands of the surgery. Kiyak et al., 1 observed
that the pre-surgical expectations of potential problems reported by the patients were important predictors of reports of postoperative experiences of dissatisfaction and mood alteration up to 2 years after the surgical procedure. Moreover, subjective information about the postoperative period provided by patients has been used as an indicator of success of surgical treatment. 15 Therefore, it is important to inform the patient as much as possible about what may occur in the postoperative period, answering, if possible, all their inquiries. In addition, patients with significant improvement in functional capacity and of quality of life experienced high levels of discomfort and functional limitation soon after the surgical procedure. 16 Communication between patient and surgeon is essential for obtaining satisfactory surgical results.1 However, preoperative counseling depends on the accuracy of the data in the recovery period and the realistic expectations regarding the return to preoperative health, as well as their day-to-day activities. 17
The convalescence period is complex and requires solving postoperative sequelae such as nausea, edema, discomfort, and pain, resulting in the return of oral functions and the day-to-day activities. 17 One of the most frequent questions asked by the patients is when the “swelling” will disappear so they can return to their day-to-day activities, such as their work and studies. Changes in the soft tissue after orthognathic surgery, including postoperative edema, are of great interest to both the surgeon and the patient. 18 Phillips et al. 17 observed that 75% of the patients reported little or no difficulty related to edema after 22 days of the surgical procedure. Therefore, 25% of the patients reported significant difficulties related to edema, of which 10% reported to be a substantial interference. After 30 days, the total percentage of patients reporting difficulties dropped to 3%. However, it is important to note that this study was based on information provided subjectively by the patients through a questionnaire, i.e. the data demonstrated the patients’ perception regarding facial volume regression and not objective measures obtained by the professional. This study demonstrated that, in subtraction 1M–1Y, there was a 52.17% reduction compared to the initial subtraction (1W–1Y). Kau et al. 13 observed a 70.51% reduction of the initial volume 1 month after orthognathic surgery, while van der Vlis et al. 3 observed a 50% reduction after 3 weeks. The most significant reduction in our study occurred after the first postoperative month, similar to the results observed by Kau et al. 13 and van der Vlis et al. 3 Nonetheless, it was also observed that 34.39% of the volume in the 1W–1Y subtraction was still present in 6M–1Y. Van der Vlis et al. 3 observed 11% of the initial volume after 6 months; however, it is important to emphasize that the authors included different types of osteotomies and that only 6 patients had been submitted to simultaneous Le Fort I and sagittal split osteotomies. It is important to highlight that Kau et al. 13 used the laser to obtain the images, whereas van der Vlis et al. 3 used 3D stereophotogrammetry. Compared to the use of laser, the 3D image has the advantage of providing speed both in image acquisition and processing. 3 By using laser scanner to get the image, the right and left sides are scanned with an average speed of 7.5 seconds. 13 These images are connected and the scan distortions are corrected by the computer program and are also manually corrected by the operator, and then the analysis layer is generated. 3 In the 3D image, the system captures the image of the face at once, accurately and with the actual surface texture of the patient’s soft tissues in 3.5 milliseconds, without any interference of the operator. 19 The speed and complete capture of the images makes the 3D image an ideal research tool for evaluation of the facial contour and volume changes, with minimum inconvenience for the patient. 7
Yamamoto et al., 18 used the 6-month period as a reference for evaluation, justifying that no statistically significant difference in facial volume was observed between 5 and 6 months postoperatively. However, van der Vlis et al. 3 found that approximately 11.2% of the initial volume increase was present at 6 months postoperatively and that this volume continued to decrease with statistically significance up to 12 months postoperatively. Similarly to van der Vlis et al., 3 we observed a variation of the facial volume until the end of the study, i.e. up to 12 months postoperatively.
Anatomical references of soft tissues have been identified and described for 3D image analysis and have showed excellent reliability and validity. 10,19,20
Areas that are not affected by the surgical procedure are fundamental as reference for overlapping the images. 21 Rana et al. 21 used the forehead, ears, and the root of the nose. We used in our study several points located in the upper third, therefore, that were not affected by the surgical procedure. In addition, the references were first marked on the patients’ faces and then transferred to the computer program, which further improved the accuracy of the measurements. The facial expression at the time of imaging is an important factor, since different facial expressions can significantly influence the calculation of the difference in volume. 21 Similarly to Rana et al.’s study, 21 for standardization in the image acquisition, patients were instructed to keep their faces relaxed, comfortable, and neutral, without expressions. In addition, the device used in our study was provided with a fixed mirror and the patient was instructed to look in this mirror into his own eyes. It is not appropriate to compare pre and postoperative images as Tozzi et al. did, 22 as the orthognathic surgery substantially alters the bone bases and, consequently, the soft tissues that cover them. For this reason, we used only the images obtained after the surgical procedure and used the last 12-month period as a reference to evaluate the previous periods. It is important to emphasize why we use the term “assessment of facial volume” and not only “edema evaluation”. We believe that changes in face volume after orthognathic surgery are mainly the result of facial edema, but not exclusively. This variation of facial volume is also resulting from other phenomena such as, for example, leakage of blood to the interstitium in the immediate postoperative period, bone remodeling, and adaptation of the soft tissue in the postoperative period, as well as variation of weight throughout the postoperative period.
In relation to the variable sex, we observed that there was a statistically significant difference between men and women in the subtraction 1W–1Y. In the analysis of this subtraction, men presented values above the general average, while women presented values below the average. However, from the subtraction 1M–1Y, no statistically significant differences were observed in any of the analyses; nevertheless, we observed a more significant decrease in men. We can say that, after 1M–1Y, the variation of facial volume of the analyzed areas remained stable in women, while in men there was still an observable decrease until 2M–1Y. Therefore, the volumetric variations found in women throughout the experimental period were less pronounced than those found in men. Unfortunately the scientific literature is sparse on the analysis of the differences in facial volume alterations in men and women submitted to orthognathic surgery. Van der Vlis et al. 3 did not observe a statistically significant difference in facial volume between men and women, but of the 49 patients included in their study, only 6 were submitted to simultaneous Le Fort I and bilateral sagittal split osteotomies. It is well established that the sexual hormones play an important role in tissue repair. 23 Estrogen increases the number of neutrophils in the bloodstream and, in high doses, decreases the production of proinflammatory cytokines, such as IL-1, IL-2, and Tumor Necrosis Factor. 24 Testosterone has the opposite effect, since it reduces the production of kinases and leukotrienes in neutrophils. 25 Therefore, it is reasonable to assume that this different hormonal, genetic, and environmental interaction between men and women had influence, at least in part, on the results observed in the present study. Nonetheless, more studies with larger sample are necessary to determine if this result is a normal response to the surgical procedure or is just a tendency.
No statistically significant difference was observed when the right and left sides were compared. All surgical procedures were performed by experienced surgeons and by residents in their third and final year of residency. They each operated 1 side of both the Le Fort I and the bilateral sagittal split osteotomies. The professionals were not responsible for any specific side, with no restriction on operating both sides of the jaw in the same procedure. Therefore, we cannot include professional experience as a variable capable of influencing the result.
When the influence of age on postoperative volume change in the subtraction 1W–1Y was analyzed, it was found that patients under 35 had absolute values higher than the general average and higher than patients at age 35 or over; however no statistically significant differences were observed. The patients’ ages ranged from 20 to 55 years of age, so we can assume that patients were in different biological and behavioral stages. Younger patients present a more rapid and intense immune system response when compared to older patients. 26 Additionally, especially after the age of 30, the concentration of sex steroidal hormones declines rapidly in women and more gradually in men. 26 As previously mentioned, in relation to the sex factor, sex steroidal hormones influence the tissue repair process. It is also plausible to suggest that patients aged 35 or older are more mature and socially stable patients, from whom it would be reasonable to expect greater collaboration with postoperative recommendations (diet, rest, respect for medication schedules, etc.) as compared with younger patients. It is also interesting to note that, although there was no statistically significant difference, a change in behavior occurred from 2M–1Y to 6M–1Y. Between these subtractions, while facial volume increased in patients ≥ 35 years of age, in patients <35 years it continued to decrease.
Our inclusion and exclusion criteria were rigorous in order to make our sample as standardized and reliable as possible, but it significantly limited the number of patients. During the investigated period we found out that 16 patients were submitted exclusively to the osteotomies type Le Fort I and BSSO, with movement limit up to 8 millimeters. Nonetheless, 6 patients were excluded because the piezoelectric instrument was applied during the osteotomy and 2 of the same patients were also excluded due to a bad split during the BSSO osteotomy. Although van der Vlis et al. 3 claim that their sample is larger than previous studies, it is important to note that patients exclusively undergoing bimaxillary surgery were only 6 (12%) of the 49 patients analyzed, and the authors did not mention the type of instruments used during osteotomies. Another important difference is that we use corticoid only in the trans-operative period, whereas van der Vlis et al. 3 used in the pre and postoperative periods. Similarly to Phillips et al.’s study, 17 in our study the patients were operated by an OMS’s teacher and 1 senior resident, all the patients were under orthodontic appliances in place, and internal fixation with plates and screws were applied; however the authors applied the intermaxillary fixation in the postoperative period while we did only during the surgical procedure. Some systemic abnormalities that may cause volume increase in the face such as congestive heart failure, renal or hepatic failure, or even endothelial dysfunction were one of the exclusion criteria of our study. Patients with these alterations should not be included in studies to evaluate volume changes after surgical procedures in the face. 21
The study was to a certain extent limited by our difficulty in obtaining a larger sample of patients who had undergone orthognathic surgery under more homogeneous conditions. Thus, despite the strict inclusion and exclusion criteria, some heterogeneity was still observed. Based on the methodology used in the present study, it is possible to conclude that the largest facial volume was observed 1 week after the orthognathic surgery, and only in this period men had higher values than women, and the most significant volume reduction occurred between the first week and the first month (52.17%).
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was partly financed by the Coordination for Improvement of Higher Education Personnel—Brazil (CAPES—“Coordenação de Aperfeiçoamento de Pessoal de Nível Superior”, in Portuguese language)—Finance Code 001.