Abstract
Maxillofacial injuries are increasing in frequency due to increasing reliance on road transportation and increasing socioeconomic activities. The primary management of most of the maxillofacial traumas is closed reduction with maxillomandibular/intermaxillary fixation (IMF). But owing to the advantages offered by open reduction and internal fixation it has become more popular nowadays. This article includes a case report and literature review regarding the necessity of IMF after open reduction and internal fixation.
Introduction
Maxillofacial injuries are increasing in frequency due to increasing reliance on road transportation and increasing socioeconomic activities. Maxillofacial region involves soft and hard tissues forming the face extending from frontal bone superiorly to the mandible inferiorly. Trauma to the facial region causes injuries to skeletal components, dentition, as well as soft tissues of the face.
The primary management of most of the maxillofacial traumas is closed reduction with maxillomandibular fixation (MMF)/intermaxillary fixation (IMF). Even though lot of evolution occurred in the treatment of maxillomandibular fractures from ancient Egypt times, concept remained the same in immobilization of the jaw bone. IMF is basically tying the teeth of fractured jaw to that of the stable one.
With recent advancements and developments in health sector, it has become possible to provide early and definitive treatment for majority of patients. Owing to the advantages of open reduction and fixation over closed reduction like early return to function and better patient acceptance, it has become an integral part especially in the management of mandibular fractures.
Patients usually deny long-term IMF as there is gingival trauma, difficulty in maintaining oral hygiene, and delayed temporomandibular joint (TMJ) discomfort. In addition to optimal bone healing, restoration of premorbid occlusion is one of the primary goals of open reduction and internal fixation (ORIF). Many surgeons recommend maintaining postoperative MMF to hold the mandible in correct position against occlusal forces.
Case Report
A 24-year-old male patient reported to trauma emergency unit with history of road traffic accident 1 day before. There was no history of loss of consciousness or vomiting. Upon examination, patient’s Glasgow Coma Scale was full and he showed laceration in lower lip, b/l circumorbital ecchymosis, and b/l subconjunctival hemorrhage (Figure 1). Intraoral examination revealed step deformity between 34,35 and between 43,44 and vestibular tenderness in relation to 25,26,27 region. NCCT face with 3D reconstruction was done and patient was diagnosed as a case of b/l Bilateral body of mandible and left zygomatic complex (Figure 2).
Preoperative Clinical Photograph.
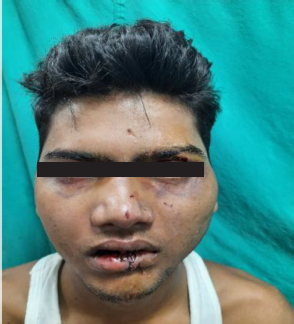
Preoperative 3D CT.
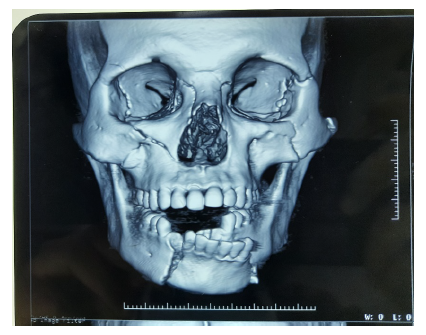
Upper and lower arch bar was tied and IMF was done as a primary management. ORIF was done with 1.2/1.5/2.0 mm Ti miniplate nonlocking system under LA (Figure 3). Postoperatively, IMF was released and patient was advised to take semisolid/liquid diet for 1 week.
Postoperative OPG.
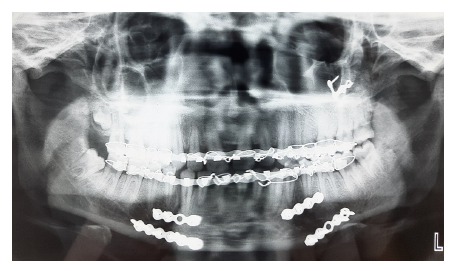
Patient was recalled after 1 week. Oral hygiene maintenance was good and there were no signs of infection. But his occlusion status was not as satisfactory as that was achieved intraoperatively (Figure 4). Again IMF was done for further 2 weeks (Figure 5). After 2 weeks, follow-up was done, occlusion was satisfactory, and soft tissue healing also got completed (Figure 6).
Postoperative Occlusion After 1 Week Without IMF.
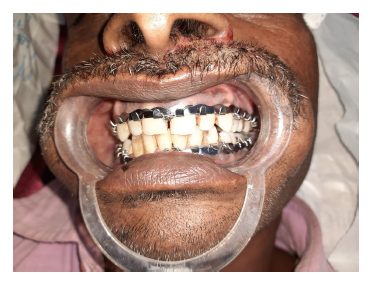
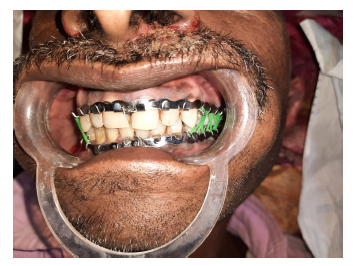
Occlusion Attained With IMF After 1 Week During Follow-Up.
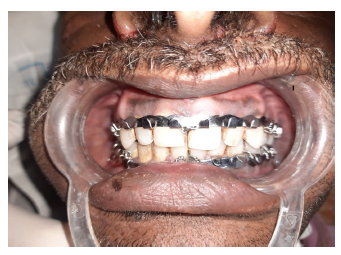
Two Weeks Postoperatively Both Occlusion and Healing Satisfactory.
Discussion
Many surgeons prefer postoperative IMF for varying periods of time depending upon the type of fractures. In clinical practice, it is not uncommon to find minor occlusal discrepancies even after ORIF of simple undisplaced fractures. Severe masticatory pull, loosening of IMF while placing the screws, and TMJ positioning are the commonly blamed factors for malocclusion post internal fixation.
In a prospective study conducted by Chritah et al, 1 it was found that when using 2.0-mm locking miniplates for mandibular fractures, it is possible to reduce the period of postoperative IMF from 2 weeks to 1 week due to the greater stability of LMP system.
Pradeep et al 2 concluded by saying that miniplate fixation of mandibular fractures along the Champy’s lines of ideal osteosynthesis is practically semirigid and provides a functional stability. During the early postoperative period, there is a chance for displacement of the fracture segments if subjected to strong external forces, because of the semirigid nature of this fixation. Hence, supplemental IMF for a brief period (2 weeks) following miniplate fixation secures the reduction of fracture fragments that is achieved intraoperatively.
Various studies also show no difference of outcome even if no IMF secured postoperatively. Dimitroulis 3 proposed that there is no need of IMF either intraoperatively or in the postoperative period in the management of mandibular angle fractures. They also concluded that by discarding the use of IMF not only helps improve patient comfort but also reduces the operating time by up to 1 h and accelerates discharge times by up to half a day.
According to a study conducted by Pradeep et al, 2 postoperative malocclusion can be due to severe masticatory pull, loosening of IMF while placing the screws, TMJ positioning, improper placement of IMF intraoperatively, and inability to assess proper occlusion due to partial edentulousness and premorbid malocclusion. IMF for 1 week postoperatively yielded better results in their study.
In another original investigation conducted by Saman et al, 4 it was concluded that the surgical dictum of maintaining postoperative MMF for all trauma patients after ORIF of the mandible may not be of advantage in the treatment of dentate patients with noncomminuted symphyseal, parasymphyseal, or angle fractures. They were of the opinion that plating according to Champy’s 5 line of osteosynthesis provides sufficient stability to counteract the stresses exerted by masticatory muscles.
The rationale for use of postoperative IMF includes use of guiding elastics to correct minor occlusal discrepancies and improved bone healing. In certain complicated fractures like subcondylar, displaced condylar, and comminuted fractures, the use of postoperative IMF may actually result in better results.
Apart from the problems faced by the patient after IMF, there are certain other disadvantages like complication in bone healing secondary to osteopenia and changes in local venous pH, and prolonged intermaxillary fixation may lead to weakness and atrophy of the masseter and temporalis.
Conclusion
Although moving toward no wire fixation is need of the hour, there is still no other options left other than placing IMF if postoperatively minor occlusal discrepancies occur. Most of the studies suggest that postoperative IMF for a period of 7 days yielded less occlusal discrepancies when compared to study group with early mandibular mobilization.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Statement of Informed Consent and Ethical Approval
Necessary ethical clearances and informed consent was received and obtained respectively before initiating the study from all participants.
