Abstract
Abstract
Face, has always been the point of attraction in a person’s physique, any disfigurement of that, caused either due to any sort of trauma or by animal attack, would lead to not only functional impairment but also severe psychological disturbance. The reasons for these injuries may vary from one country to another and even within the same country. Injuries due to bear mauling are most commonly seen in rural areas, but in developing countries like ours, stripping the wildlife of their natural habitation brings them close to more populated areas in the search of food. Increase in tourism may be another cause of these types of injuries. We herein report a rare presentation of bear maul injury in adult patient in maxillofacial region, and the purpose of this clinical report is to discuss the increase in incidence of such injuries and its subsequent management.
Introduction
Love of life is next to love of our own faces —Shushrut (600 BC)
Face, has always been the point of attraction in a person’s physique, any disfigurement of that, caused either due to any sort of trauma or by animal attack would lead to not only functional impairment but also severe psychological disturbance. For this reason, any such grievous injury demands rapid and skillful management. The incidence as well as etiological factors vary between different countries and within the country itself depending upon various socioeconomic, cultural, and environmental factors. Mauling is the lesser evil for the cause of these injuries with a range of 1.2% to 2.3%. 1 Among these cases, injuries caused by bear mauling have a much higher incidence 2 of 51.2%, although bear mauling injuries are rarely reported. Most common sites which are involved in mauling by bear is face (80.57%) followed by head (54.67%). 3 Following a facial bite wound, unforeseeable infections (13%-30%) that can occur as a result of primary bacterial invasion and management of extensive soft tissue defect represent the main challenge in the management of such injuries. 4 Hence, the foremost goal of maxillofacial reconstruction should be directed towards addressing the esthetic and functional problems of the patient. The purpose of this clinical report is to discuss a case of rarely occurring maul injury by a bear and its management.
Case Report
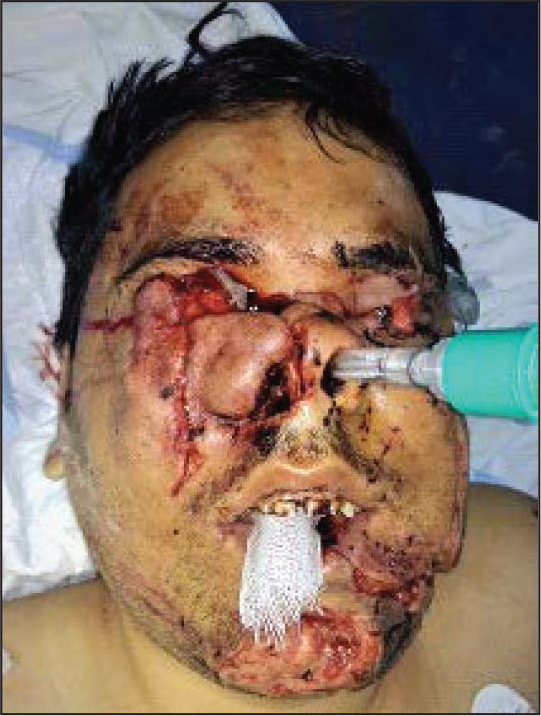
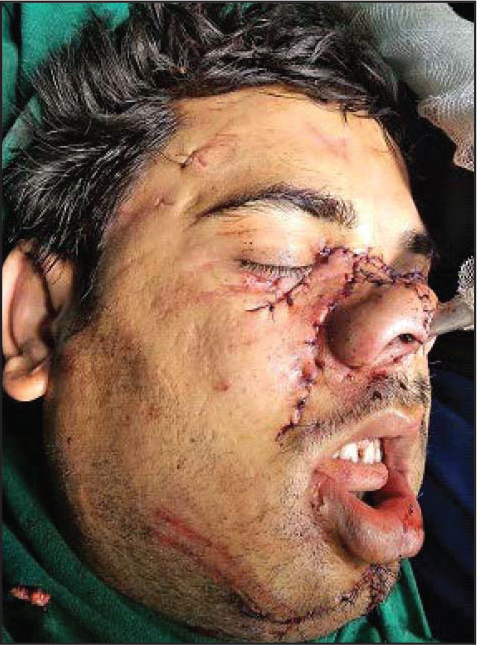
A male patient of 35 years of age presented in the emergency department (ER) of a private hospital in Kashipur on January 30, 2019, with the history of attack by a bear on the same afternoon around 2 pm while grazing cattle in the jungle, after which there was severe bleeding from oral cavity and face in association with severe lacerations on maxillofacial region (Figures 1 and 2). A single episode of vomiting after arrival of the patient in hospital was witnessed. No history of seizure attack or neurological deficits was eminent.
Patient Reported to Emergency Department
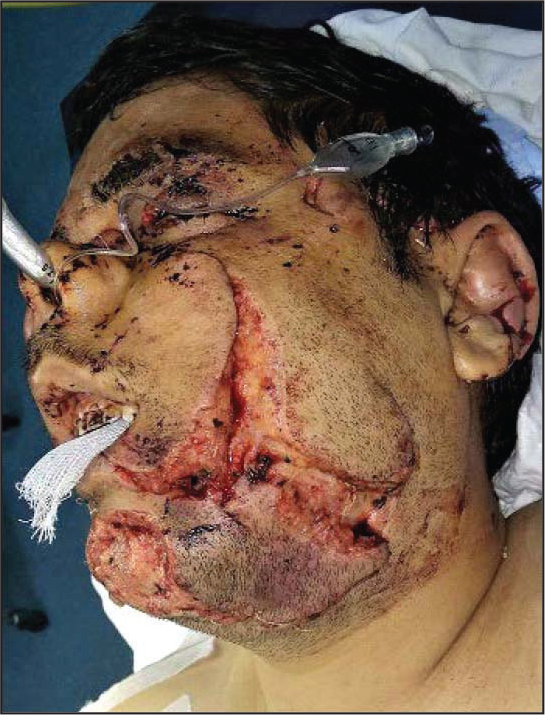
Intraoperative picture
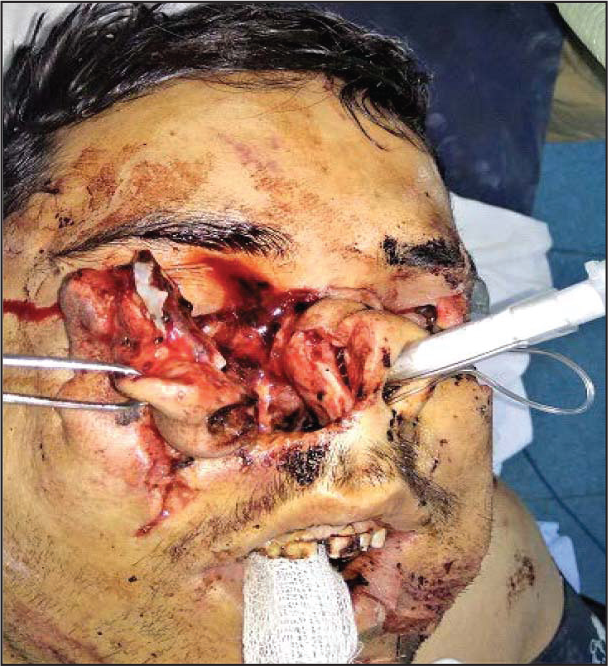
On local examination, there was laceration present below the right eye sparing the globe extending mediolaterally from the bridge of nose laterally involving the lower eyelid and running over the zygomatic bone exposing whole of the nasal structures. The skin covering this defect was hanging lose laterally including part of nasal septum (Figure 3). Further examination revealed that left upper eyelid was also lacerated and there were de-gloving injuries in upper and lower vestibule as well as in lower half of the face. Fractured segments were evident over the left body of mandible resulting in occlusal derangement and were delirious at presentation. On ear examination, laceration of left pinna was noted. Patient also sustained minor lacerations over his left temporal region and left upper limb which were sutured in a primary health center in his place. Investigations like noncontrast computed tomography (NCCT) brain with bony window and 3D face showed fracture of the left mandibular body (Figure 4). Soft tissue swelling was noted involving almost the whole face. All the required basic investigations including chest X-ray, cervical spine, and ECG were normal.
Intraoperative picture
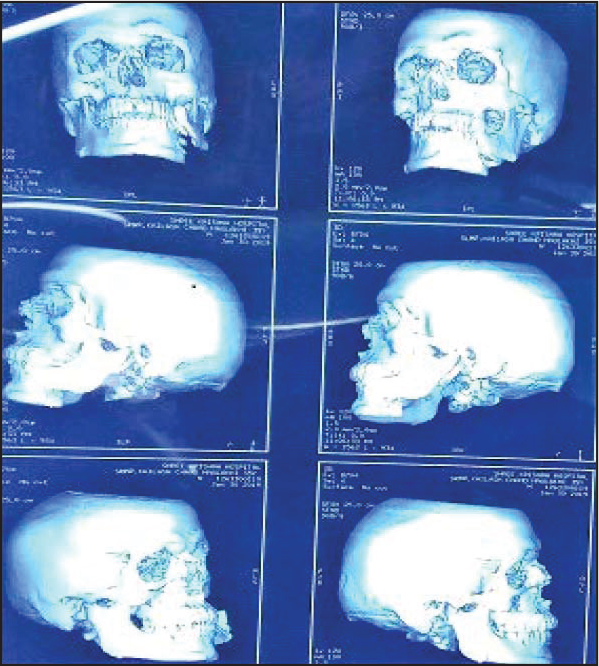
Preoperative CT scan
Immediate Post Operative Picture
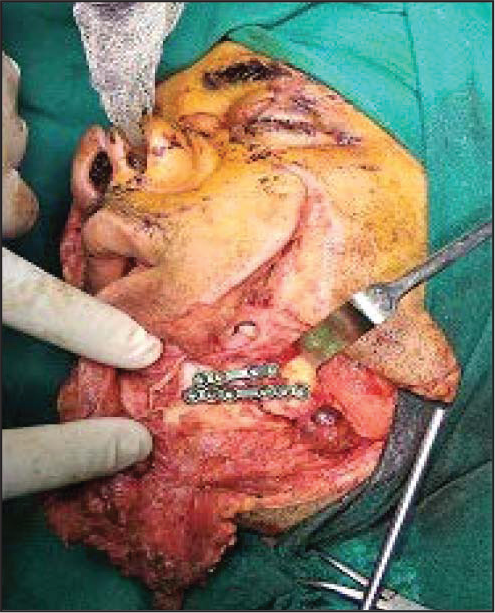
Intraoperative Picture After Fixation
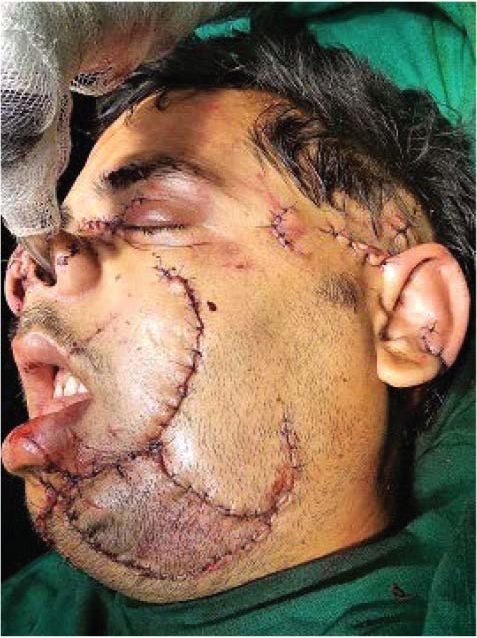
Immediate Post Operative Picture
Management
Based on the above presentation in the ER, the case was treated following a basic protocol as explained below:
After maintaining the airway, breathing, and circulation, bleeding was arrested. Tetanus prophylaxis (intra-muscular gluteal region) and rabies vaccine (four dose regimen, intra-muscular deltoid region) were given to the patient in first sitting. One unit of whole blood was transfused in ER. Under general anesthesia after copious irrigation with normal saline and wound debridement, fracture of body of mandible was reduced and stabilized using 2.5 mm titanium miniplates (Figure 5). Human rabies immunoglobulin (20 IU/kg body weight) was locally infiltrated in wound before closure.
11
Intraoral layer-wise closure of the wound was done with 4-0 vicryl suture. After the adequate approximation of deep structures extra oral wound closure was done using 4.0 prolene sutures (Figures 6 and 7). A course of antibiotic (piperacillin/tazobactam 4.5 gm IV thrice daily, amikacin 500 mg IV twice daily, metronidazole 100 ml IV thrice daily) and anti-inflammatory was prescribed for a week.
Discussion
Injuries due to bear mauling are most commonly seen in rural areas, but in developing countries like ours, stripping the wildlife of their natural habitation brings them close to more populated areas in the search of food. 5 Increase in tourism may be another cause for these type of injuries. 6 The distinguishable feature of injuries due to bear mauling are combination of cutting, penetrating, and crushing (due to powerful slaps) type of injuries. 7 Mud, grass, and other contaminating foreign materials are forced into the wound when such injuries occur; therefore, vigorous irrigation and removal of these contaminating agents are of utmost importance.7,8
Due to contamination with unique poly-microflora (most common species—Pasteurella), facial bite wounds are considered complex type of injuries but show a low rate of infection because of rich blood supply in the area,3,9 According to the report published by Kunimoto et al, 10 they have seen aerobic gram negative bacilli and enterococcus from their cases but they also supported the presence of anaerobes in bear maul injuries. Therefore, it is always better to administer broad spectrum antibiotics. Other factors that must be considered in the management of such injuries are bite location, time until wound management, type of wound, host factors, and local wound care.7,8,10
In our case report, the subject was attacked in jungle while cattle were grazing, so this gives an idea that the bear might have attacked the patient as a defensive measure. Wound sustained by the subject involved the head and neck region and this is in accordance with previously documented reports. Complications common after bear mauling are psychiatric complications and post-traumatic stress disorders such as depression, cognitive difficulties, and anxiety, but none of these complications were noticed in this case.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
