Abstract
Study design:
A finite element method used to virtually analyze the distribution of stresses in human mandible.
Objective:
The aim of this study was to evaluate the distribution of stresses in 1 customized and 2 non-customized plates used in simulated procedures of mandibular advancement and rigid fixation after bilateral sagittal split osteotomy of the mandibular ramus.
Methods:
The model used was obtained from a tomograph of an 18-year-old patient, and the simulation involved advancing the mandibular body by 4.75 mm. The plates used were Osteomed, double-row medium; Stryker, standard straight; and Traumec, custom-machined double straight. Virtual models of the mandible and the installed plates were generated and submitted to finite element analysis. Two 100-N loads, 1 anterior and 1 posterior, were applied perpendicular to the occlusal plane.
Results:
In the Osteomed and Traumec plate models, the stress peaks occurred near the separation zone of the mandible, adjacent to the connections. In the Stryker plate model, the stress peak occurred in the region between the screws.
Conclusions:
The Stryker plate was associated with the lowest risk of compromising bone repair, followed by the Traumec and Osteomed plates. Stress concentration was related to plate length and to the existence of a connection between the upper and lower portions of the fixation used.
Introduction
The bilateral sagittal split osteotomy (BSSO) of the mandible modified by Hunsuck/Epker is a technique routinely applied in orthognathic surgery for the surgical treatment of mandibular deficiency or asymmetry (separately or together with maxillary deformities) by mandibular advancement. 1 Although modifications of this technique have been introduced over the years, 2 interfragmentary instability of the fixation was replaced by risk of exposure, infection and palpation of the plate and screw fixation systems are some problems related to this technique. Improved rigidity of plate fixation required anatomical alignment of the fracture fragments. 3
A systematic review of fixation stability with different methods of BSSO for mandibular advancement found no significant difference among bicortical screws, titanium plates and screws, and resorbable screws during clinical follow-ups of up to 1.5 years. 4 However, higher relapse rates were found in the long term among patients treated with bicortical screws (2.0% to 50.3%) versus titanium miniplates (1.5% to 8.9%). Mandibular advancements in the 6 to 7+ mm range predisposed patients to horizontal relapse. 4
The soft tissue response and its stability depend on the surgical procedure itself, and on the technique and materials used. 5 A higher frequency of fractures has been observed for bent plates, and these fractures have been found to occur at the mandibular angle, possibly owing to the large areas undergoing stress, and to stress accumulation in the plate regions where adaptations were required. 6 Reconstruction plates do not fracture exclusively by excessive bending during surgical placement; fractures also occur due to stress concentration in the mandible. This added reason has led to proposed changes and adjustments to plate morphology. 7 Three-dimensional plates have been found to present higher fracture site stability than conventional plates, particularly between the upper and lower portions of the fracture. 8 Ramos et al. 9 also observed that customized plates displayed better stress distribution than their non-customized counterparts.
Thus, the aim of this study was to identify the areas of stress and evaluate the risk of fracture in customized versus non-customized plates used for mandibular advancement surgery. The hypothesis studied was that the customized plate would present lower levels of stress, and better stress distribution in the plate body and in the fixation screws than the non-customized plates.
Materials and Methods
This study was approved by the local Ethics Committee (number # 2018/020).
A three-dimensional model of the mandible was constructed from a tomograph of an 18-year-old male patient, the same tomographic image used in the study conducted by Ramos et al. 9 This patient had a complete dentition, except for the third molars, a Class II skeletal malocclusion, and pronounced mandibular retrusion, which indicated mandibular advancement surgery. Computer software (Dolphin v.11.7, Chatsworth, CA, USA) was used to import the CT scan and perform surgical planning (Figures 1A and 1B). This planning revealed that 4.75 mm of mandibular advancement would be required to correct the skeletal deformity. This measurement was selected considering an average of programmed advances of up to 5 mm. 10
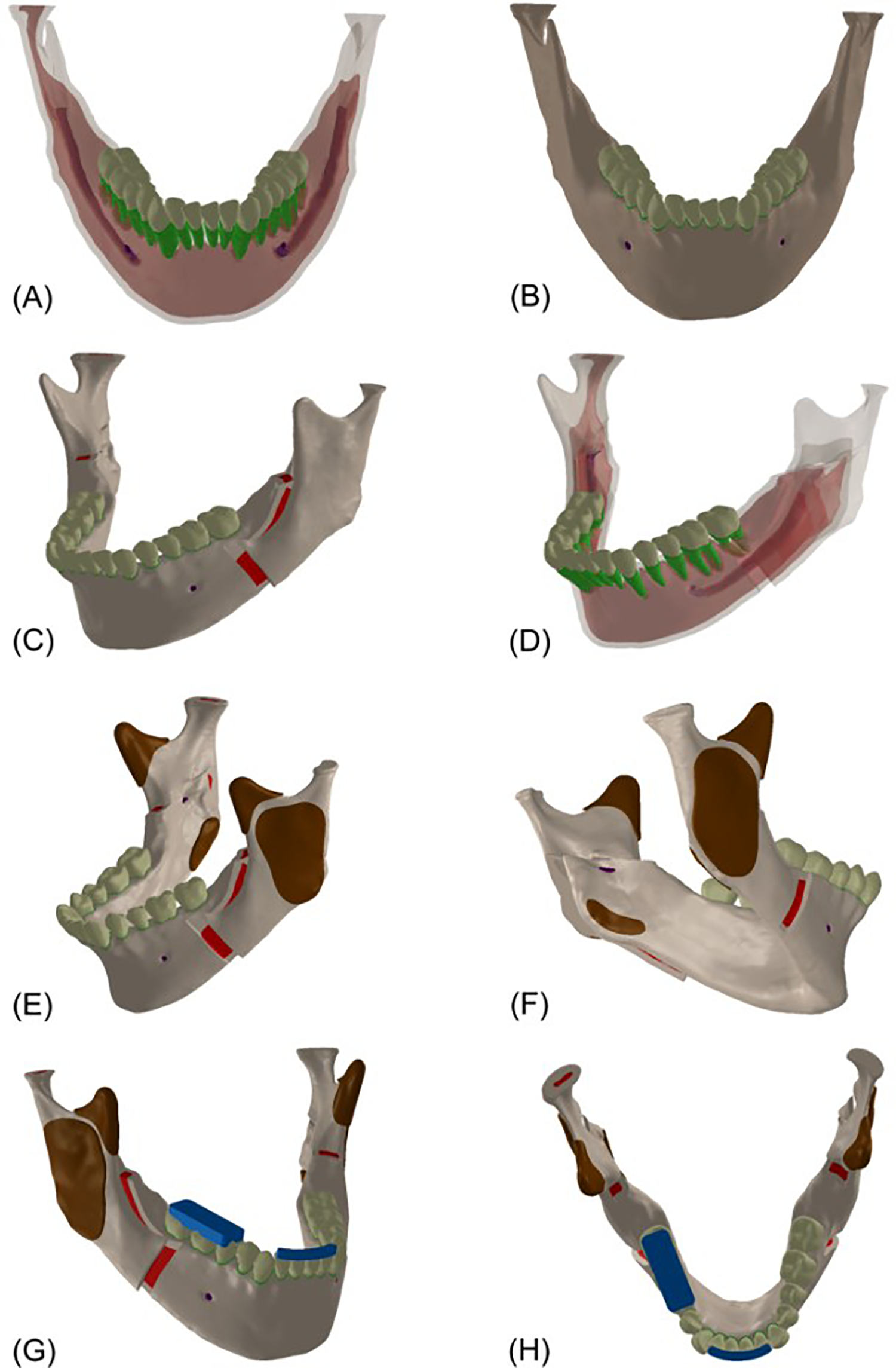
(A) View of the mandibular model reconstructed from a tomographic image. B) Semi-transparent bone to allow visualization of internal structures. (C) Anterior lateral view of the cut demonstrating the proposed mandibular advancement. (D) View through bone transparency. (E) Structures used to simulate muscle support, and mandibular advancement on the left side. (F) Structures used to simulate muscle support, and mandibular advancement on the right side. (G) Frontal view of structures used to standardize load application; occlusal view of structures used to standardize load application.
The mandible image was then processed to allow its digital reconstruction in a 3D model and editing of virtual models using CAD software (SolidWorks 2015, Dassault Systemes, Solidworks Corps, Waltham, MA, USA), in which geometrical changes were made, required for finite element mesh generation.
The mandible model was virtually segmented according to the technique of BSSO of the ramus. 11 After segmentation, the rami were repositioned 4.75 mm posteriorly, sliding them parallel to and in contact with the osteotomy surface of the central portion of the mandible (Figures 1C and 1D).
The support zone of the mandible was standardized by creating structures in the insertion regions of the temporal, masseter and medial pterygoid muscles (Figures 1E and 1F). Two structures were also created to standardize the area of load application, one in the anterior region and the other in the posterior region (Figures 1G and 1 H).
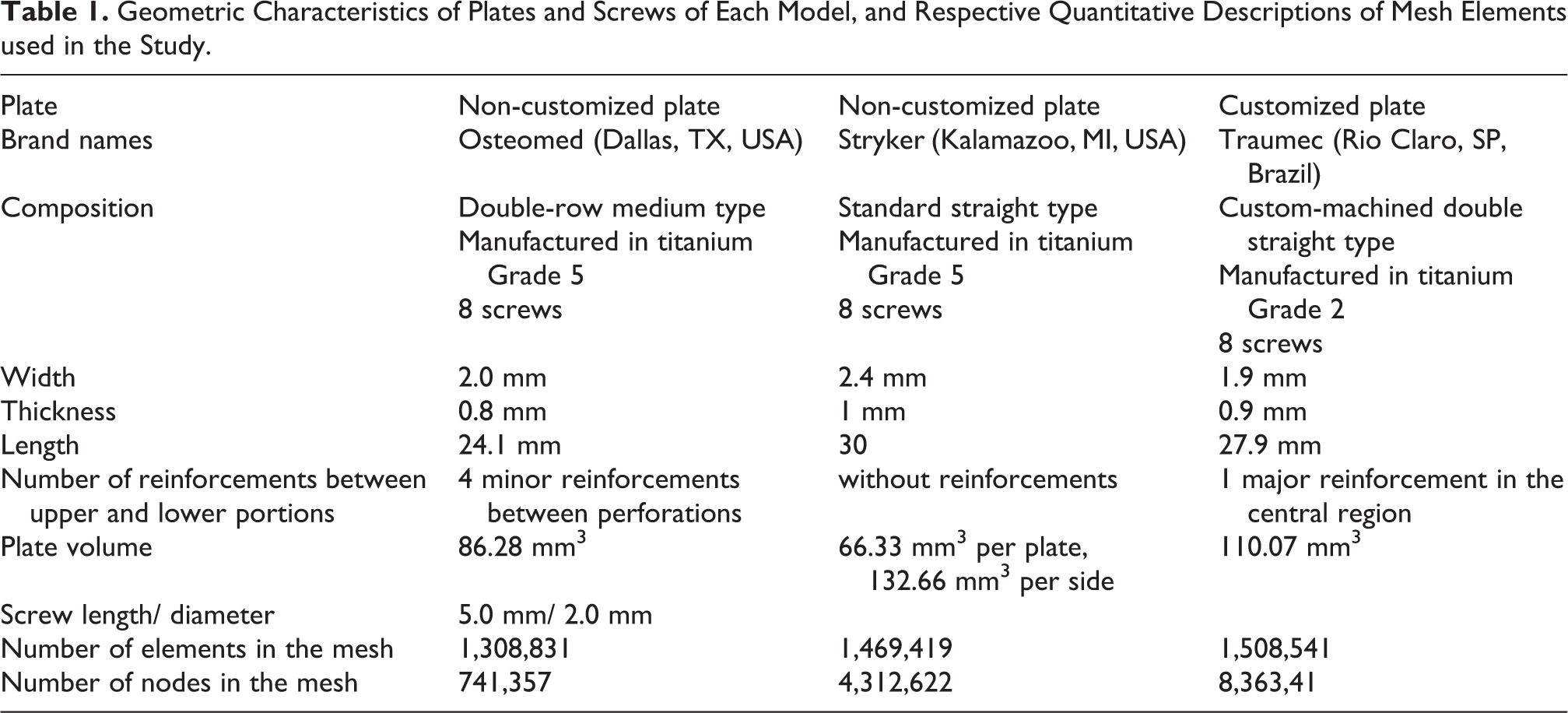
Two non-customized plates (Osteomed, Dallas, TX, USA; and Stryker, Kalamazoo, MI, USA) and 1 customized plate (Traumec Health Technology, Rio Claro, SP, Brazil) were virtually reconstructed for use in the present study (Figure 2). In this virtual reconstruction, the plates were acquired and analyzed using digital calipers (Litz Professional, Germany) and a digital microscope (B008, Supereyes, Shenxhen D&F, Bantian Village, China), under 10X to 500X magnification, and using the manufacturer’s proprietary software. Detailed analysis and measurement of the plates (Table 1) enabled reconstruction of the models using the Solidworks program.

Plates evaluated in the study: Osteomed, double-row medium (Osteomed, Dallas, TX, USA); Stryker, standard straight (Kalamazoo, MI, USA); and Traumec, custom-machined double straight (Traumec Health Technology, Rio Claro, SP, Brazil).
Geometric Characteristics of Plates and Screws of Each Model, and Respective Quantitative Descriptions of Mesh Elements used in the Study.
All the models were then exported from Solidworks software to finite elements simulation software (Ansys Workbench V15; Ansys, Canonsburg, PA, USA). All the structures were considered isotropic, homogeneous and linearly elastic. This process resulted in the creation of elements and nodes of a finite element mesh, thus enabling accurate analysis of the stresses involved (Table 1).
A virtual model including mandible and installed plate was created for each of the plate types studied to analyze their biomechanical performance, considering the associated impact and/or deformation that would occur after the mandibular advancement procedure. The plates were installed in the buccal region of the molars, following the recommendations of their respective manufacturers. The Osteomed, Stryker and Traumec plates (Figure 3) were fixed to the mandible with 8 screws. Since the length of the non-customized plates is preset by their respective manufacturers, some bending was simulated to allow their adaptation to the 4.75-mm simulated advancement used in this study. The number of screws and the distance between them were predetermined by the manufacturer.
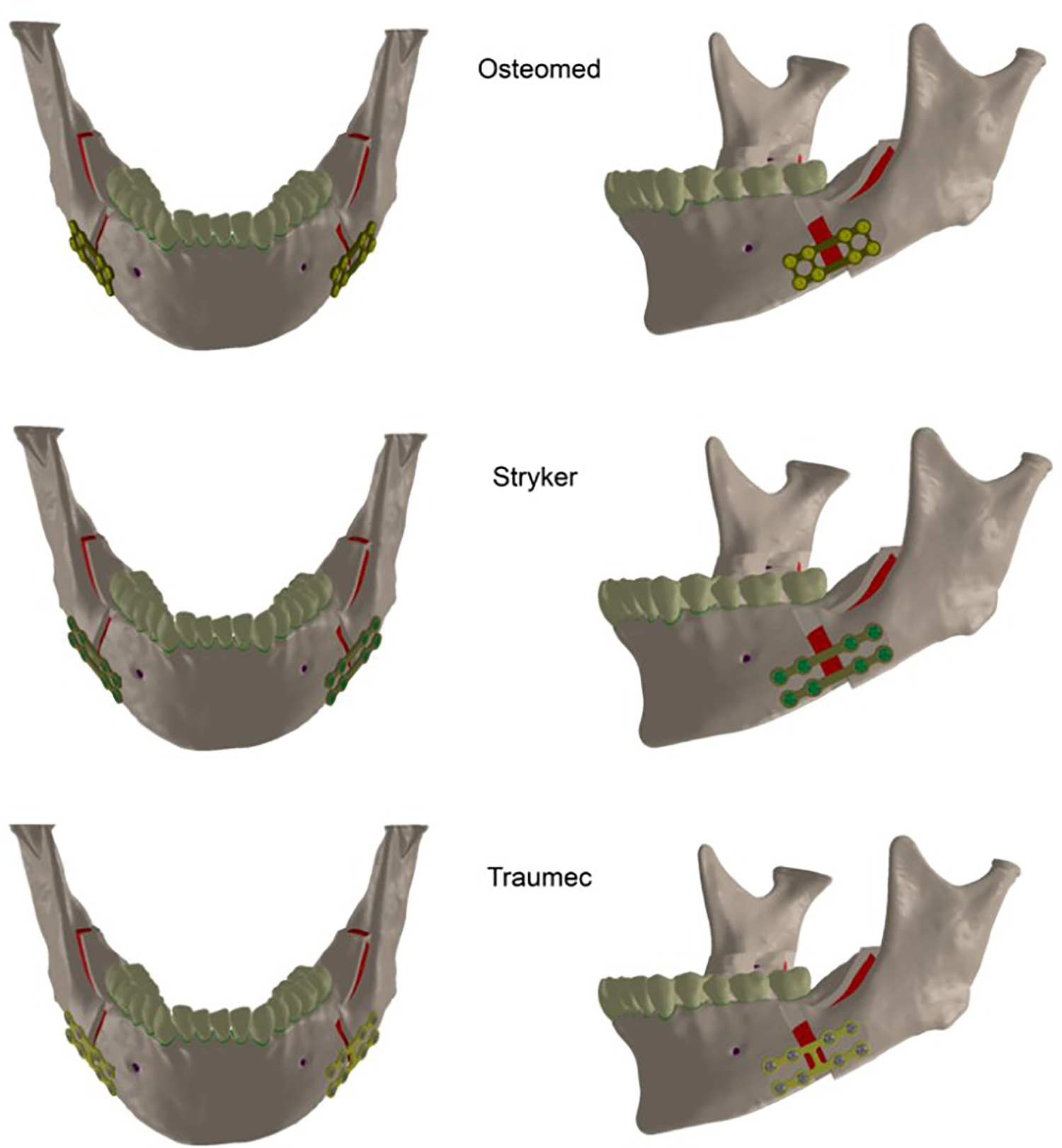
Frontal and lateral views of the models analyzed in the study.
Data on the Poisson coefficient and modulus of elasticity pertaining to these materials (Table 2) were fed into the modeling software in order to calculate the stresses on the structures of the plates and the bone.
Mechanical Properties of the Materials Considered in the Study Simulations.
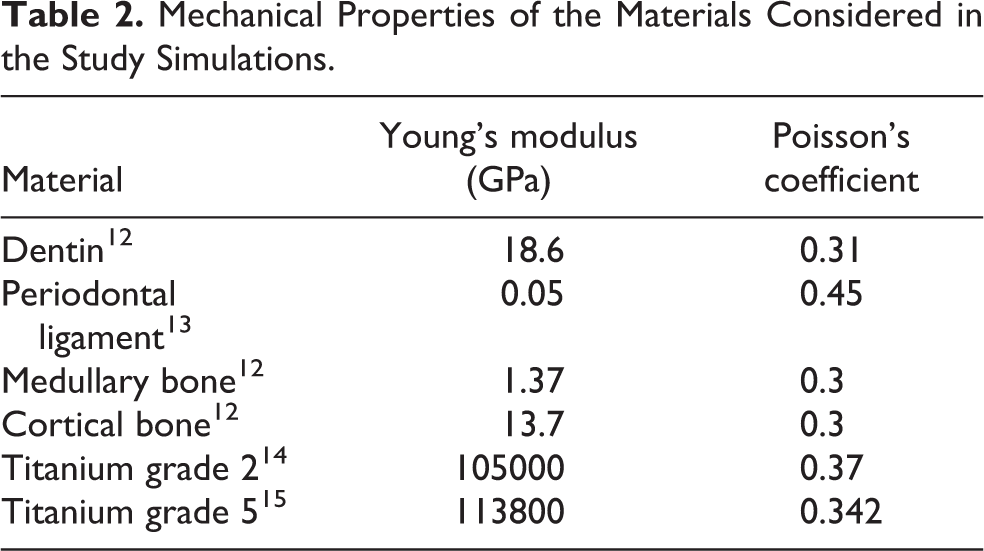
The contacts between teeth were configured as frictional, with a friction coefficient of 0.2, 16 to simulate the contact between their saliva-lubricated enamels. The contact between screws and bone and between plates and bone were configured using a friction coefficient of 0.3 to simulate a non-osseointegrated titanium condition. 17 The contact between the sectioned segments was configured as frictional, with a friction coefficient of 0.372, 18 based on the same coefficient observed between tibial bones sectioned with an oscillating saw.
Although friction coefficients can vary according to several factors, such as surface roughness, cutting instrument, quantity and quality of lubricants (exudate or saliva), among others, the values cited in the literature were used for simplification purposes. All the other contacts were defined as contacts that did not allow separation or slip. The simulations were nonlinear in relation to contact. Rigid supports were added in the regions of muscle insertion.
Two loading patterns were applied to each model (Figure 4). In the first pattern (posterior), the load was applied in the region of teeth 45, 46 and 47. In the second pattern (anterior), the load was applied in the region of teeth 42, 41, 31 and 32. Both loads had an intensity of 100 N and a vector perpendicular to the occlusal plane. Figure 4 shows images of the antagonist structures with their respective load vectors.
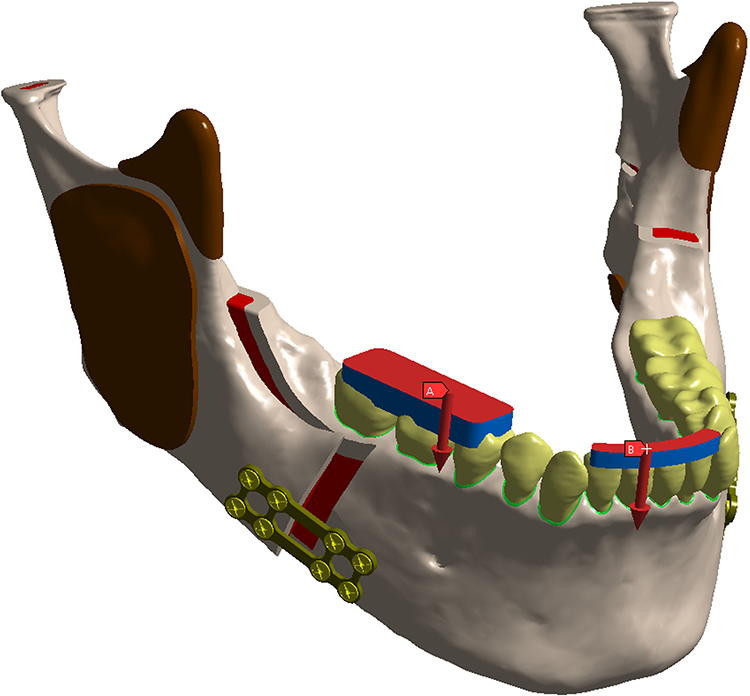
View of antagonist structures with loading vectors. (A) Posterior load. (B) Anterior load.
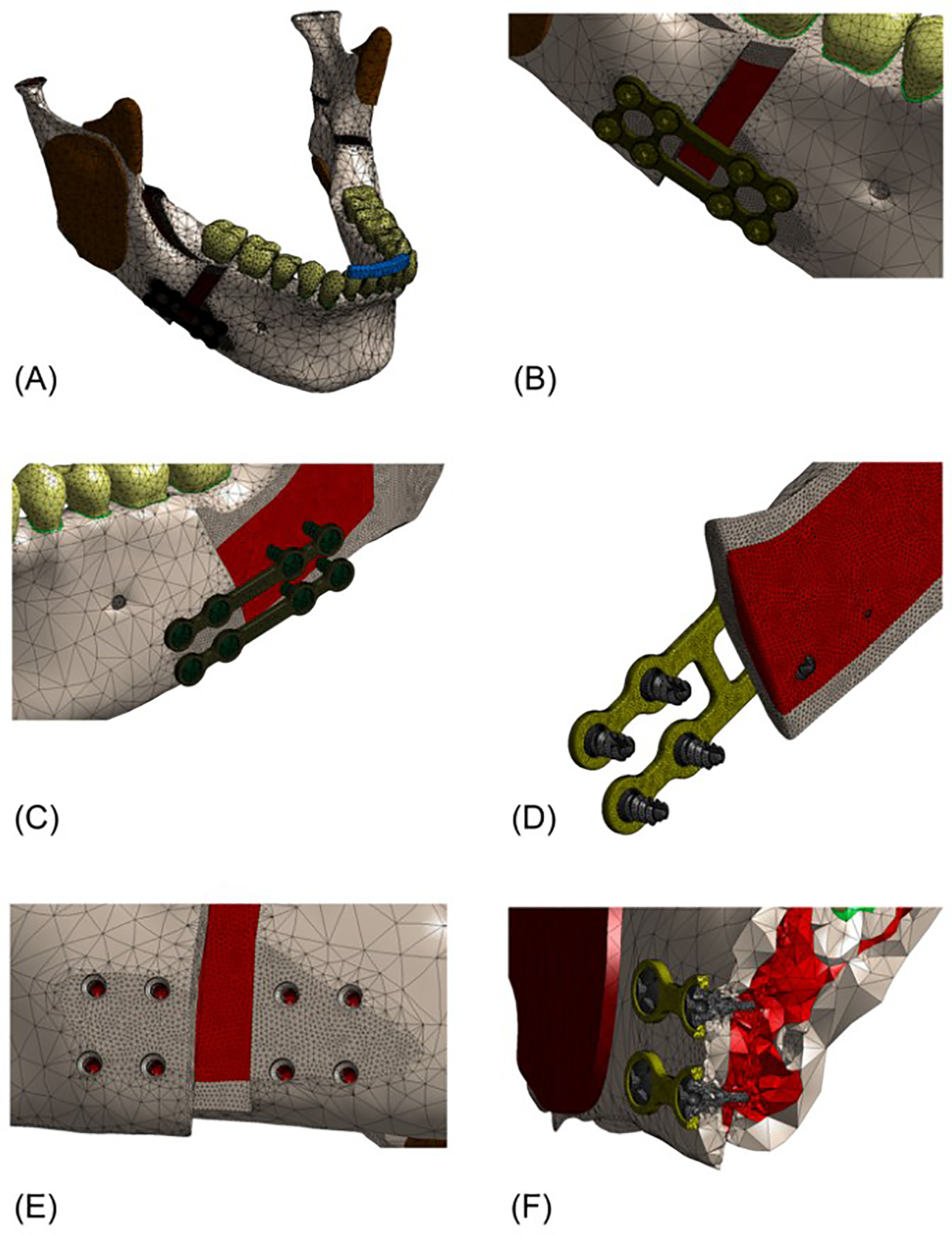
Discretization of the model, which is the transformation of a solid model into a mesh of nodes and elements, was performed to enable analysis by the finite element method. The mesh was generated and validated through a mesh refinement process, where convergence of the results was verified, and the number of nodes and elements was gradually increased (Figure 5).
Lateral view of the areas where the highest stress levels were observed on the screws, on the side where the highest stress peaks were observed (right side).
All the models were then resolved using a personal computer running Windows 7 (64-bit), with an Intel I7 920 processor and 24 Gb of RAM. The graphical and numerical plotting of the data was recorded, evaluated and compared. Quantitative analysis of the images was performed to allow observation of color gradients correlated to a numerical scale, containing the minimum and maximum values of each color indicative of the level of stress on each region, expressed in megapascal (MPa).
Results
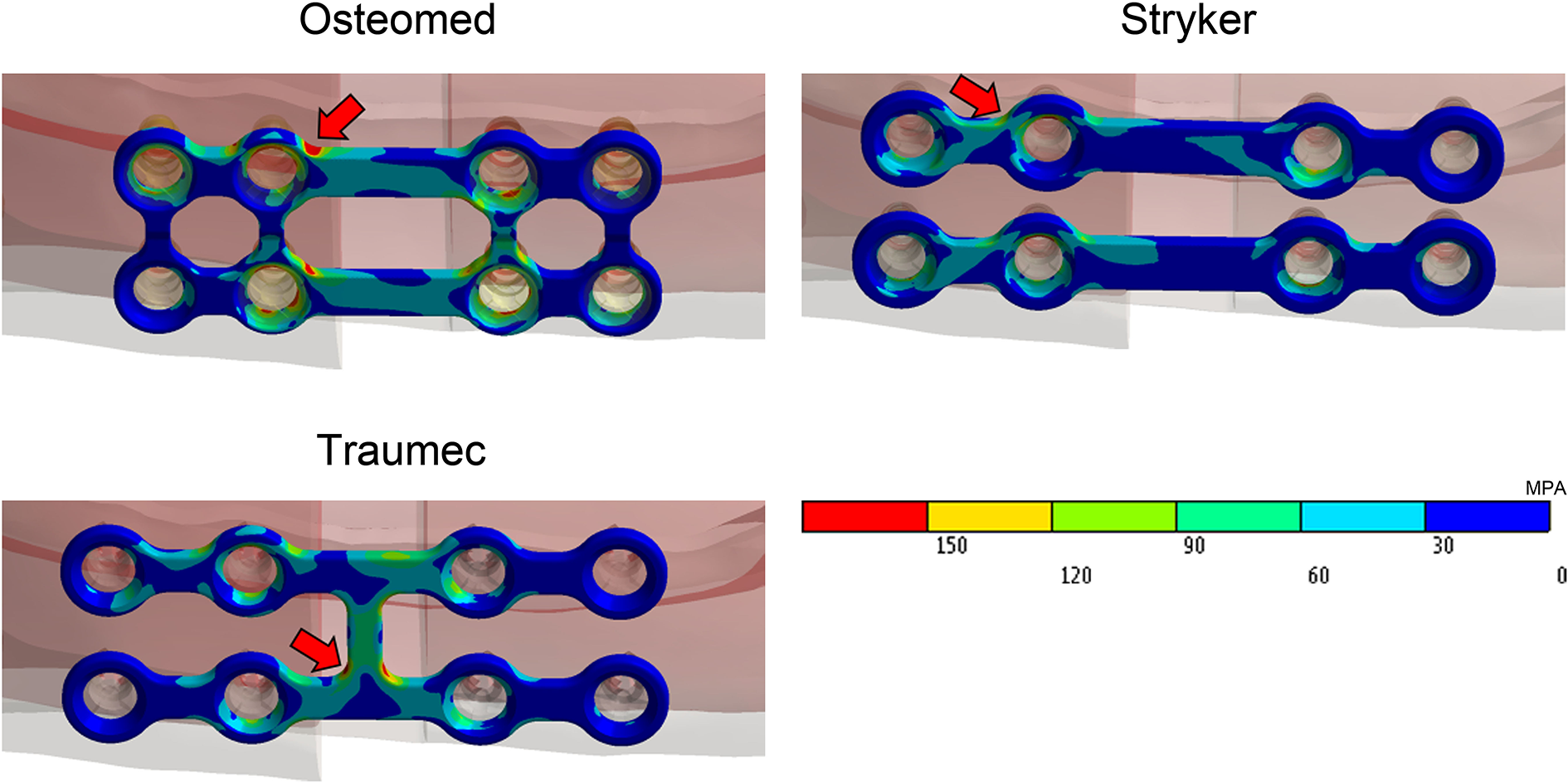
The stress peaks on the plates whose upper and lower portions are connected (Osteomed and Traumec) occurred near the separation zone of the mandible, and in the regions adjacent to the connections (Figure 6). The peak on the Stryker plate, whose upper and lower parts are not connected, occurred in the region between the screws.
Views of the meshes of the different models (the mesh was refined in important areas). (A, B, C) Mandibular advancement region and respective discretization areas. (D, E, F) Discretization and greater number of nodes in the area relevant to the study.
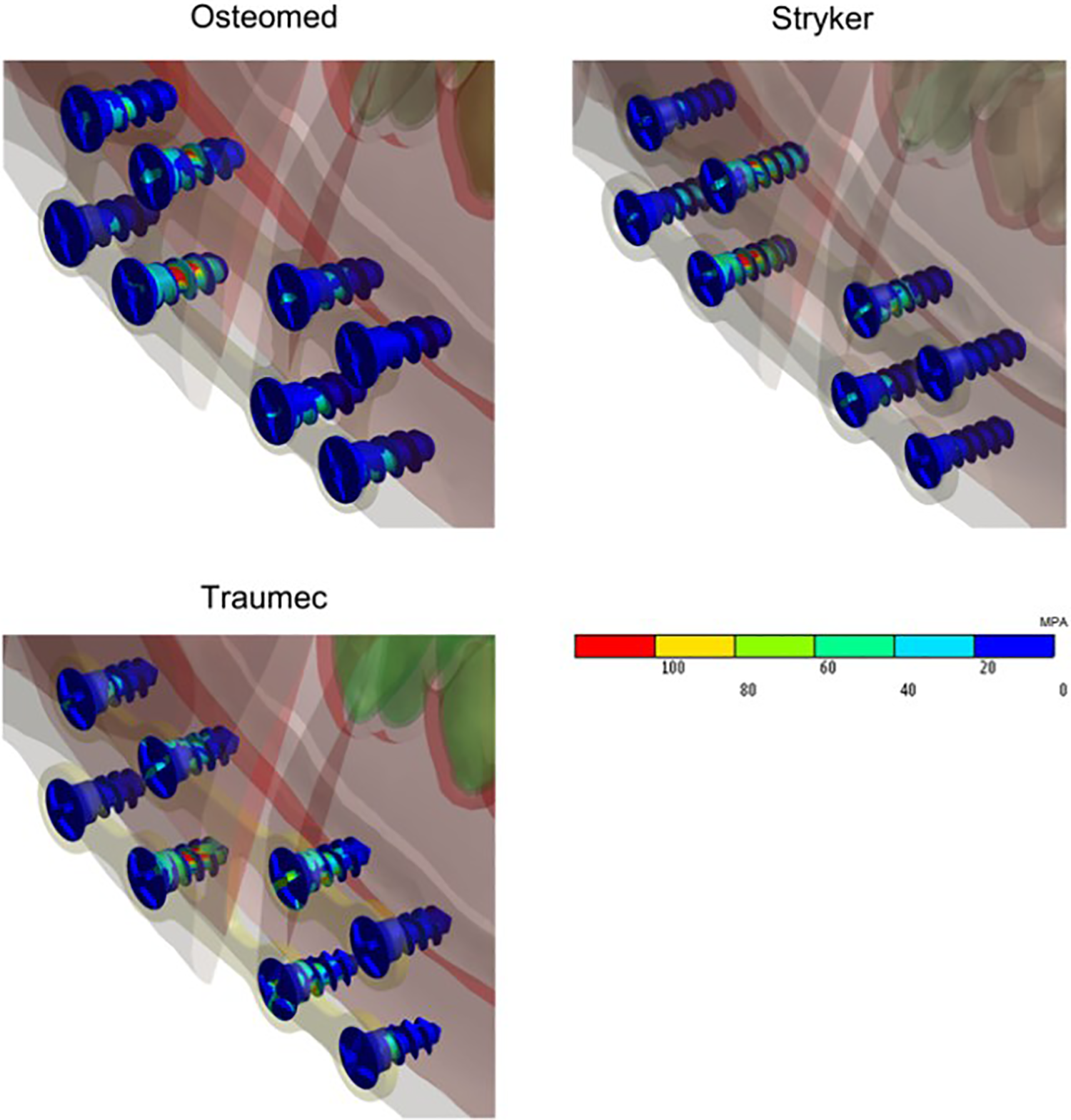
Qualitatively, there was a greater accumulation of stress in the screws closer to the separation zone between body and ramus (Figure 7). Regarding the screws furthest from the separation zone, there was greater stress accumulation on the Osteomed plate, intermediate stress accumulation on the Traumec plate, and lower stress accumulation on the Stryker plate. Stress accumulation on the sharp angles of the plates in contact with the screws was disregarded (Table 3), considering that deformation of these angles causes only local rounding of the neoformed bone, without structural risks to the plate.
Results for plates on the side where the highest stress levels were observed (right side). Arrows indicate where the stress peaks described in Table 3 occurred.
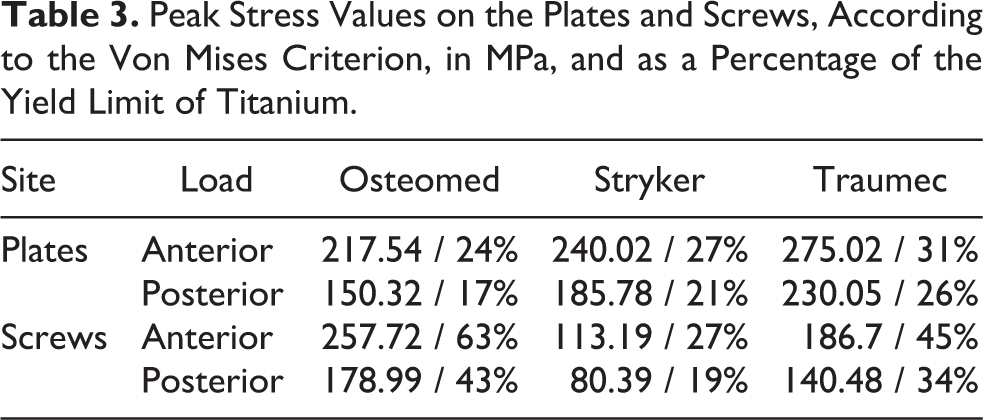
Peak Stress Values on the Plates and Screws, According to the Von Mises Criterion, in MPa, and as a Percentage of the Yield Limit of Titanium.
Discussion
In a customized plate, no bending is required for its adaptation to the anatomical shape of the mandible and the bone segment, prior to installation. This customization considerably minimizes the stress areas. 9 Besides the use of customized plates reduces the surgical time, it may also improve the stability of bone fixation since it may decrease the tension in the osteotomized mandibular stumps and in the plates due to multiple folds to seek the correct adaptation of them to the bone surface. On the other hand, non-customized plates very rarely fit the anatomy of the mandibular bone or bone segment perfectly, thus increasing stress areas. The bending occasionally required involves application of tensile forces to the titanium. By applying this force to the plate, stress is not transferred to the adjacent bone; however, it may lead to increased risk of plate fracture. 19
The characteristics of each plate regarding design and number and location of screws influenced the observed stress values (Figures 6 a). This study intended to compare a customized plate with commercial plates, which present different designs for the mandibular advancement surgery. Respecting the technical specifications of the non-customized plates—size, thickness and width—this study tried to evaluate a customized plate that could be of easy manufacturing, even though it made it difficult to compare some results. All the plates require grade 2 titanium for their production, which made them similar to each other in composition, although differences are in fact related to the design features. This suggests that the location of peaks is related to these connections, possibly indicating that the best design for minimizing the area subjected to stress peaks is that of the Stryker plate. The results shown in Table 1 seem to indicate that greater thickness and no connection (as in the Stryker plate) favors better stress distribution, although more studies are needed to confirm this hypothesis.
It is assumed that the space between the fixation points of the plate is inversely proportional to its flexural strength, and that there are differences between plate and bone regarding their intrinsic rigidity. 20 The connection between upper and lower portions is associated with a reduction in the difference between left and right sides, in regard to plate deformation, and provides improved plate-to-bone fixation. However, it can also lead to much greater areas of stress concentration than those associated with plates whose upper and lower portions are not connected.
It was noted that the screws closest to the zone of separation between body and ramus underwent higher stress accumulation, which can be explained by the greater tendency of these segments to separate in that region; thus, stress concentration is higher closer to the osteotomy site. Since stress is calculated by dividing the force by the area considered, 21 it follows that the larger the area of distribution, the lower the stress peak in this area. The screws farthest from the zone of separation between body and ramus underwent the lowest stresses. As for the screws farthest from the separation zone, it was observed that stress concentration was highest for the Osteomed plate, intermediate for the Traumec plate, and smallest for the Stryker plate; this difference may be related to plate length and to whether or not the upper and lower portions of the fixation are connected. However, more studies are needed to evaluate the mechanism underlying the observed stress distribution differences among screws.
For small to moderate linear mandibular advancement, the results obtained in this study showed that Stryker non-customized plate presented better performance than Osteomed (non-customized) and Traumec (customized) plates. This result suggests that the avoidance of folds for the correct adaptation of the plate to the bone, its thickness, and the greater length reduced the tensions generated nearly to the osteotomy region when using Stryker plate. Further research is needed to show whether similar results would be obtained with nonlinear advances and/ or greater advances. However, the universal applicability is that contrarily to what was expected, the customized plate did not present any advantage in relation to the stability compared to the commercial available Stryker plate. Even decreasing the surgical time and, therefore, reducing complications associated with greater tissue detachment and also reducing the edema, the customized plate did not present an effective advantage concerning the postoperative stability of the mandibular stumps and, therefore, Stryker plate (straight with 4-holes) presents an advantage when compared to double-row plates (Osteomed and Traumec).
Based on the results of the present study, the hypothesis that customized plates would exhibit less stress and better stress distribution on the plate body and fixation screws than non-customized plates was rejected. The models submitted to the conditions of this study involved a single masticatory act, and presented similar performance regarding mandible stabilization. However, in a clinical scenario, the plates would be subjected to thousands of cycles and episodes of high masticatory loads (such as cases when patients might bite down on a stone in the food or on hard food, or even when parafunction is involved). In this scenario, use of the Stryker plate seems to offer a lower risk of impaired bone healing, followed by use of the Traumec and Osteomed plates for a small to moderate mandibular advancement.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
