Abstract
Study Design:
Case Report
Objective:
To present a patient with long-standing TMJ dislocation and pseudoarthrosis in the temporal bone treated with orthognathic surgery and unilateral joint replacement.
Method:
The patient, a 52-year-old female, came to our department to treat facial asymmetry and oral rehabilitation. The patient reported early facial trauma at 7 years old showing partial edentoulism, dental occlusion class III and a 19 mm mandibular midline deviation. Cone beam computed tomography showed the left TMJ in long-standing dislocation into the fossa temporalis, creating a new articular fossa in the temporal bone and adaptation of the hard and soft tissue.
Results:
Orthognathic surgery and TMJ replacement using a patient-specific implant and dental rehabilitation were planned; surgery was performed with no complications, and the 1-year follow-up showed that this treatment was a good option for long-standing TMJ dislocation.
Conclusion:
The long-term TMJ dislocation can be successfully treated by TMJ replacement using a patient-specific implant to obtain facial balance and oral function and avoid relapse.
Introduction
TMJ dislocation occurs when the mandibular condylar is out of the glenoid fossa. Recurrent TMJ dislocation is related to a benign condition; however, difficulties in terms of function and aesthetics can be observed. 1 Usually, recurrent TMJ dislocation shows a descriptive image observed by computed tomography or nuclear magnetic resonance, an open bite, difficulties with mandible stability and acute pain during condylar movement. 2
Recurrent TMJ dislocation presents as a condition when the condyle is in the anterior area of the eminence and returns to the glenoid fossa with some frequency. 3 However, long-term or permanent TMJ dislocation is not common and can be observed as a permanent position of the condyle in the anterior area of the articular eminence. 4 Causes such as facial trauma or long-standing oral intubation have been reported.
Long-term TMJ dislocation can be related to the adaptation of the mandibular muscles, the stable position obtained before long-term dislocation of the TMJ, the vascular and nervous adaptation of the area and the long-term position of the entire dental and skeletal component; in terms of treatment, no consensus is reported. 5
The aim of this article is to show the treatment of a patient after 45 years of permanent dislocation and pseudoarthrosis of the mandibular condyle into the fossa temporalis after facial trauma at 7 years of age using a TMJ prosthesis to address the functional and aesthetic condition.
Case Report
The patient, a 52-year-old female, was treated in the Department of Oral and Maxillofacial Surgery at the A.G.P. Hospital (Lautaro, Chile), complaining of malocclusion and pain in the left cranial and temporomandibular areas.
Clinically, significant facial asymmetry was observed (Figure 1A), with a 15 mm chin deviation from the midline and class III facial condition (Figure 1B and C); tooth loss was confirmed, including long-term difficulties with a removable dental prosthesis (Figure 1D and E). Medical records showed facial trauma at 7 years old with no treatment. The mouth opening was 35 mm and was painful at the final stage of the forced movement of the mandible.
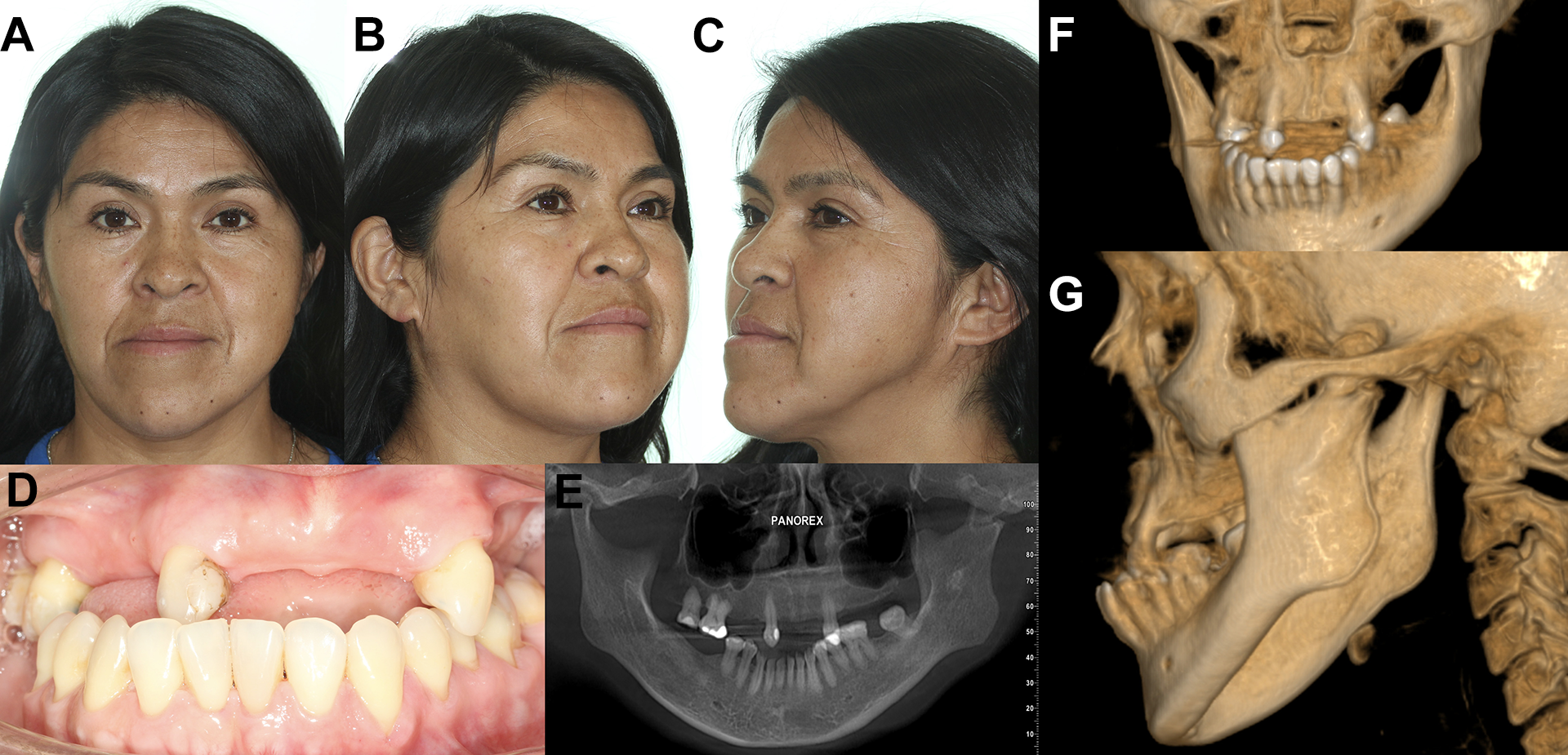
A, Frontal view showing midline deviation. B, ¾ right view showing the mandibular line contour and regular position if the mandible. C, ¾ left view showing the mandibular contour modified and the mandibular angle in the front of the ear. D, Dental occlusion with the midline deviation. E, Orthopantomography showing dental treatments in the past and normal condition of the dento-alveolar unit. F, Prognathism and midline deviation of the mandible and volume differences in the angle and mandibular position. G, Left mandibular condyle in the fossa temporalis with a neoarthrosis in the temporal bone.
Computed tomography showed a midline deviation (Figure 1F) and the real cause of facial asymmetry related to the permanent movement of the condylar/ramus unit into the fossa temporalis out of the glenoid fossa (Figure 1G). The condyle was present, developing a new fossa, i.e. pseudoarthrosis, in the temporal bone medial to the left zygomatic arch, showing an adaptation of this anatomical site to function for more than 40 years. Right TMJ showed no deformity and function with no pain or complications.
Orthognathic surgery and TMJ replacement were proposed to obtain facial symmetry and a new position and function of the face. A patient-specific implant (PSI) for the left TMJ was designed (Artfix
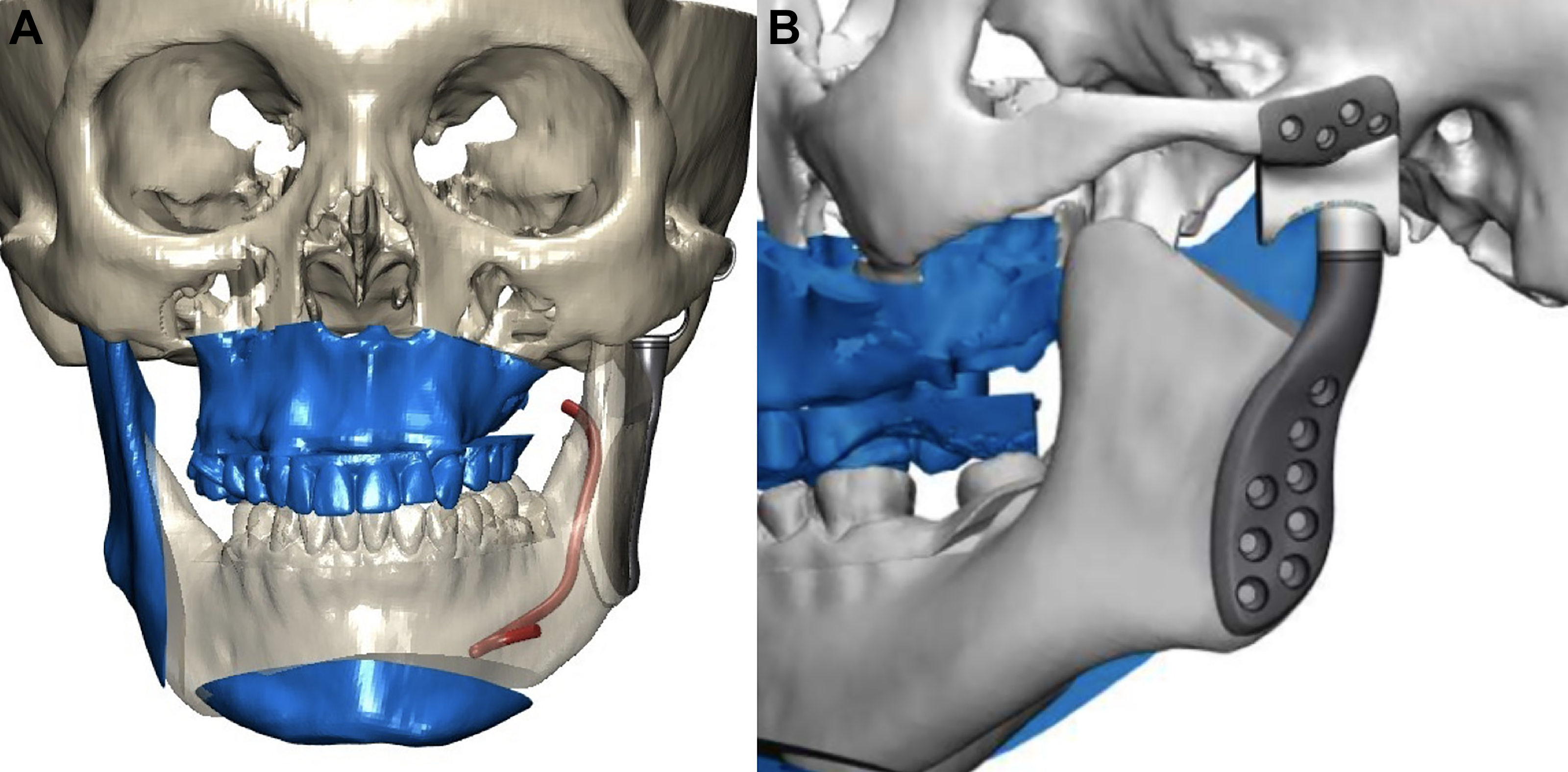
A, 3D plan with the bimaxillary orthognathic surgery. B, TMJ prosthesis design and the new position of the mandible on the left side.
Surgery was performed using 2-step condylectomy by the classical preauricular approach in the left condyle and extended to obtain good visibility of the zygomatic arch; the ramus was exposed by the submandibular approach.
The initial trauma followed by growth caused the left condyle which had developed a pseudoarthrosis to adherent to the temporal bone by fibrotic tissue. Hence, a high condylectomy was performed with Piezoelectric system (Piezotome®, Satelec, France) and the upper fragment (6 mm) left in situ.
A second osteotomy was performed in the lower area of the condylar neck to remove the condylar neck; the coronoid process was maintained, and the mobilization of the ramus was obtained with no problems.
The anatomical area of the glenoid fossa was prepared to install the template of the fossa component; after confirming the correct position, the definitive fossa component was installed and fixed in the proper position using a 2.0 mm screw.
On the right side, a sagittal split osteotomy (SSO) was performed, and mobilization of the mandible was obtained. Maxillomandibular fixation was done using an intermediary dental splint printed previously to obtain a forward movement of 9 mm on the right side and to create rotation of the mandible to the left side; the right osteotomy was fixed using a 2.0 system, and then the condylar component was fixed on the left mandibular ramus.
Closed and open mouth stability were revised in the TMJ prosthesis (Figure 3A); the close fit position of the ramus was confirmed (Figure 3B). Maxillary osteotomy was performed with forward and rotational movement of a 1-piece Le Fort I osteotomy. No complications, such as bleeding, were observed during the surgery.
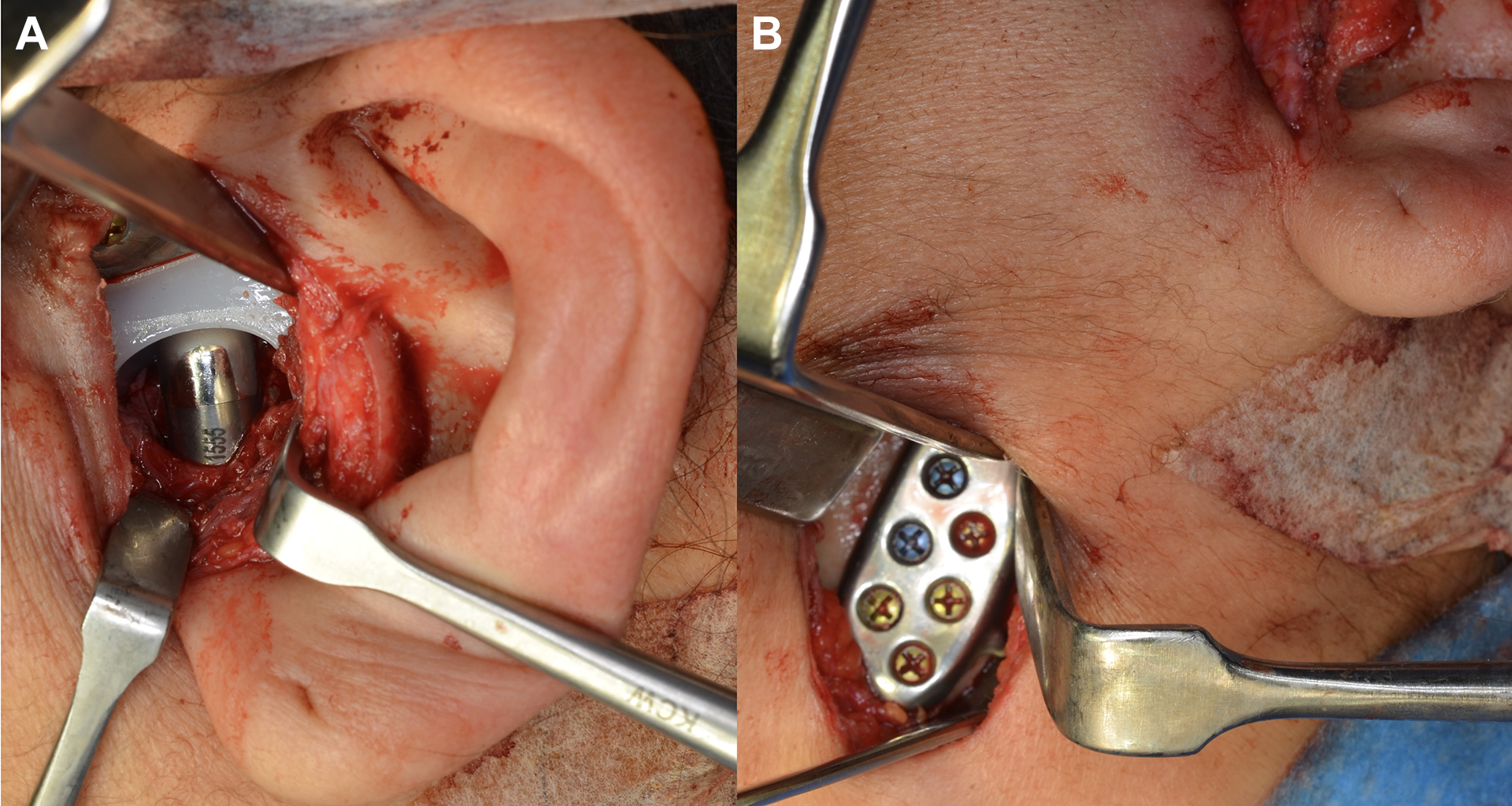
A, Condylar component in movement in the open mouth position. B, Condylar component position from the submandibular approach.
Stability and facial symmetry were confirmed using computed tomography (Figure 4A), and the new position of the TMJ replacement was observed with no problems (Figure 4B and C). Follow-up was carried out using oral and facial manual therapy and a new dental prosthesis.
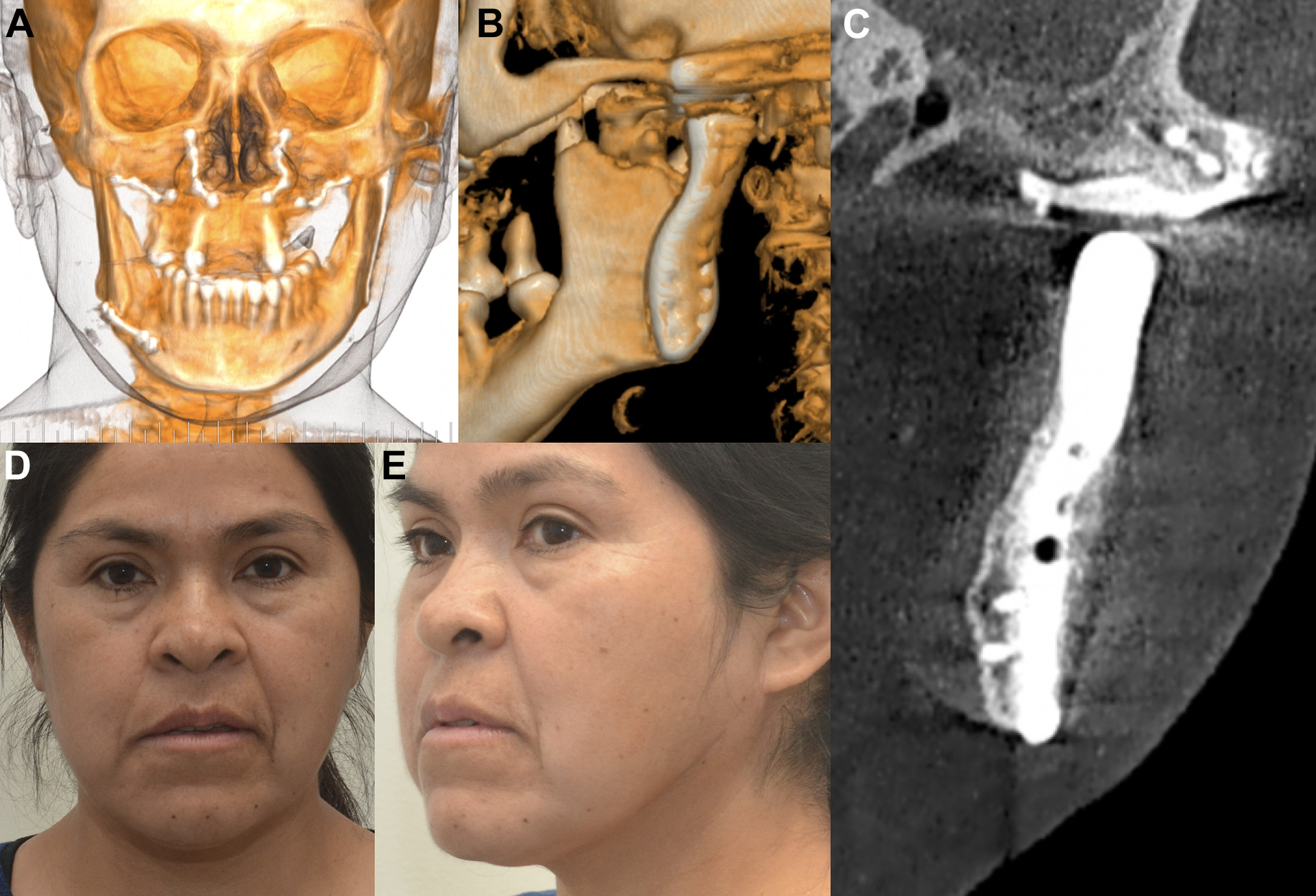
A, Six months of follow-up showing a good position of the TMJ after surgery. B, Six months of follow-up showing adaptation of the TMJ in the fossa and the condylar unit. C, The fossa component showing stability and fit position. D, Facial balance and stability after 1 year of follow-up. D, ¾ view after 1 year of follow-up showing good relations in terms of mandibular contour and angle.
After 1 year of follow-up, the patient showed symmetry, stability and regular function in mandibular movement, good dental occlusion and a TMJ condition free of pain (Figure 4D and E).
Discussion
TMJ dislocation is associated with poor function in the facial and oral status and is usually related to pain. Recurrent TMJ dislocation is associated with bone and soft tissue remodeling, with a morphological adaptation to obtain function under this condition. 6
Treatment for recurrent TMJ dislocation is to obtain stability and function of the TMJ, aiming for normal function and to prevent recurrence. 3,6 A recent clinical review 6 included a summary of 235 patients published in 15 articles between 2007 and 2016; the surgical treatments were disc plication, eminectomy or orthognathic surgery. Condylectomy is another technique used for this disease. 3
Eminectomy is the most common process to treat this condition, showing low morbidity, TMJ stability, lower pain during function and dental stability. 1,2 Long-term dislocation, however, is another entity showing stable function out of the regular anatomical limit of the TMJ; for this reason, long-term TMJ dislocation needs different treatment than recurrent TMJ dislocation. 5,7 In this case, the long period of time under TMJ pseudoarthrosis created a new facial and dental position, which was complex to treat using the routine surgical approach.
A recent report 5 showed that long-standing TMJ dislocation could develop into pseudoarthrosis of the TMJ, showing adaptation and some movement of the mandible to permit stomatognathic function. In the present case, pseudoarthrosis was presented, with a new cavity in the temporal bone showing the adaptability and capacity of the structure to achieve function using a new anatomical position. In this case, fibrous tissue will probably be observed in the articular layer replacing the fibrocartilage. 8
The aim of treating long-standing TMJ dislocation is to reduce the condyle, obtain appropriate function, balance facial conditions and stable oral rehabilitation to avoid relapse and complications. 8 For this reason, TMJ replacement was the choice in this case. In the initial stage of long-standing TMJ dislocation, eminectomy, 4 condilectomy 8 and discectomy 7 can be considered. In the later stage of long-term dislocation, however, a more aggressive technique has to be performed considering the full condition of the patient 5 ; in this case, the aim was to achieve facial symmetry, facial balance, proper dental occlusion and relief of pain.
Lee et al 9 showed a 5-month prolonged bilateral TMJ dislocation treated by mandibulotomy in the midline to obtain independent movement of each condyle and to obtain a secure position of the condyle, showing stability after 2 years; the same strategy was used by Rattan et al 10 in patients with 3 months of TMJ dislocation, showing stability as well. Gholami et al 11 reported 3 patients with mandibular dislocation for more than 4 months, using discectomy as the surgical strategy.
In a clinical series with long-standing TMJ dislocation and medical compromised in patients over 70 y.o., 7 eminectomy was successful in 5 patients, and combined discectomy or condylectomy was included for 11 patients, showing two patients with incomplete reduction. Incomplete reduction could be related to the time involved in permanent TMJ dislocation and soft and hard tissue adaptation. Moreover, in long-standing TMJ dislocation cases, dental occlusion is one of the key factors affecting the stability of surgically assisted TMJ reduction and could be difficult in long-term edentoulism or malocclusion, as shown in the present case.
In this case, the new position of the condyle created a pseudojoint with strong fibrous tissue. For that reason, the intraoperative decision was to maintain the upper 6 mm of the condylar head in the same anatomical area using a high condylectomy. Complications could be related to infection of the area or foreign body reaction; however, there were no post-operative complications for example infections resulting from the surgery of from the implant noted.
Güven 5 observed pseudoarthrosis as a possibility in long-term TMJ dislocation, showing an edentulous 85 years old patient with 18 months of TMJ dislocations and an 80 years old patient with TMJ dislocation for 14 months. In the present report, we show a patient with 45 years of TMJ dislocation created by a complex facial trauma at 7 years old; the patient grew and developed facial asymmetry, type III dental occlusion and adaptation of the new TMJ, showing a new fossa in the temporal bone. In this case, no psychiatric or medical comorbidity was observed, and full-face rehabilitation using TMJ replacement, orthognathic surgery and later dental rehabilitation could be planned. Other technical options, such as conservative surgical treatment based on condylectomy or eminectomy, were considered, but long-standing dislocation, the requirement for full-face reconstruction and proper dental occlusion were key factors supporting this treatment.
It is possible to conclude that long-term TMJ dislocation can be successfully treated by TMJ replacement using a patient-specific implant to obtain facial balance and oral function and avoid relapse.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
