Abstract
Objectives:
Liposomes are reported as penetration enhancers for dermal and transdermal delivery. However, little is known about their percutaneous penetration and as to at which level they deliver encapsulated drugs. The penetration of multilamellar vesicles (MLVs) and small unilamellar vesicles (SUVs), in comparison to one of their lipid components, was investigated.
Methods:
Using the fluorescent lipid, Lissamine Rhodamine B-PE (R), as a constituent, MLV and SUV liposomes were prepared, tested, and R, MLV, or SUV were applied in vivo on the back of hairless mice. Absorption of each was evaluated at the levels of stratum corneum, living skin, and blood by fluorometry.
Results:
Penetration of the lipid R in stratum corneum in the nonliposomal form exceeded that in the liposomal form and only R penetrates the living skin in a statistically significant manner. No statistical significant absorption into blood was observed with either form.
Conclusions:
Liposomes size did not play an important role in penetration to stratum corneum. The lipid constituent in the nonliposomal form penetrated at higher rates into stratum corneum and living skin. Even though these liposomes entered stratum corneum, they were not significantly absorbed into viable skin or blood.
Keywords
Introduction
The use of beneficial liposomes as drug carriers is established. 1,2 These vesicles, usually made by amphiphilic phospholipids, can control the release of hydrophilic and lipophilic substances. 3,4 They increase therapeutic and decrease side effects of potent drugs. 2,5 –7 Drugs encapsulation within alters their pharmacokinetics, 8 and changes on liposome surface can enhance drug targeting. Liposomes have been used in medical applications as agents in “passive tumor targeting,” “vaccine adjuvants,” “sustained release depot at point of injection,” “anti-infective agents,” carriers for “targeting regional lymph nodes,” and “gene vehicles.” 6,9 –16
Over recent decades, they have been intensively studied as carriers for dermal and transdermal administration. Molecules encapsulated in liposomes are better absorbed in skin, compared to conventional formulations. 17 In cosmetology, liposomes are used with vitamins such as α-tocopherol and ascorbic acid, and also with lipids and humectans. 17 Many drugs encapsulated in liposomes such as corticosteroids, anesthetics, retinoids, interferons, methotrexatre, nonsteroidal anti-inflammatories, antibiotics, antifungals, and photosensitizers have been tested in skin. 18 –24 As an example, topical cutaneous application of triamcinolone acetonide in liposomes showed an increased absorption into epidermis compared to a decrease in the thalamic region, a site responsible for adverse effects.
However, few studies demonstrate the manner by which liposomes penetrate. Effects on stratum corneum utilizing freeze fracture electron microscopy and small angle X-ray scattering 18,19 concluded that there are two types of liposome skin interaction. First, adsorption and fusion of vesicles on skin surface, and second is impaired barrier function within the stratum corneum caused by liposomes. Deformable liposomes like ethosomes, transferosomes, or ultradeformable liposomes are able to deliver active ingredients into deeper skin layers. 20,21,25,26 The main cause for their higher penetration is their deformability, which, according to some investigators, could facilitate penetration through stratum corneum intercellular spaces. Nevertheless, studying skin localization of ultradeformable liposomes with confocal laser microscopy revealed that the major penetration pathway was transfollicular and not stratum corneum. 25 With ethosomes, using the same technique, the thermodynamic state of the liposome was a more important factor for penetration than flexibility. 22 A similar study concluded that the liquid crystalline state associated with unsaturated lipids was the most important feature for liposome penetration. 23 Conventional liposomes seem unable to penetrate deeply and remain confined to stratum corneum. 24,27 –29
Especially in vivo, it is not clear how deeply liposomes themselves penetrate, as most studies were performed in vitro with the static cell model. 24,27 –29 There is no study comparing the penetration of liposomes themselves in vivo or in vitro or in comparison to a lipid constituent of them. Two liposomes formulations, multilamellar vesicles (MLVs) and small unilamellar vesicles (SUVs) and one of the lipid components, the fluorescent Lissamine rhodamine B sulfonyl-PE, were applied to skin to compare their penetration quantitatively and evaluate their ability to enter into stratum corneum, viable skin, and blood.
Materials and methods
Materials
Lissamine rhodamine B sulfonyl-PE (phosphatidyl ethanolamine) was purchased from Avanti (California, Alabaster, USA), 1,2 dilmyristoyl-sn-glycero-3-phosphocholine (DMPC) from Limhamnsgardens alle (Larodan AB, Sweden), sodium chloride solution 0.9% from Cooper (Athens, Greece), chloroform and HPLC grade methanol from Lab-Scan (Analytical Sciences, Dublin, Ireland), and γ-hydroxybuturic acid from Sigma-Aldrich Chemicals Co (Taufkirchen Germany, USA).
Plastic vials to collect blood were purchased from Logo Silicone (acetoxy; Pioneer, Quezon, Philippines), opaque plates, solid black 96-well with lid for fluorescence measurements from Corning Costar® Incorporate (New York, USA), and Millex® 0.22 and 13 mm syringe-driven filters from Millipore (Bedford, Massachusetts, USA). Water was of HPLC grade and obtained from Labconco® WaterPro PS (Kansas City, Missouri, USA).
Animals
Animal care was performed according to the guidelines established by the European Council Directive. Experimental procedure was approved by the National Peripheral Veterinary Authority. Forty female hairless SKH-hr1 mice aged 3–5 months were studied. All mice originated from the breeding stock of the School of Pharmacy Small Animal Laboratory (Licence: EL 25 BIO 06). Animal room was kept at 24°C ± 1°C, 45% humidity, and illuminated by yellow fluorescent tubes in a 12-h cycle of light and dark (switched on at 8:00 and off at 20:00). These lamps do not emit measurable ultraviolet radiation. Mice had unrestricted continuous access to solid pellets (Keramaris SA, Greece) and freshwater. They were divided into four groups: (1) MLV, (2) SUV, (3) Lissamine rhodamine B, and (4) control mice.
MLV liposomes and SUVs preparation
DMPC and Lissamine rhodamine B-PE were dissolved in chloroform in a round-bottomed flask and dried in a rotary evaporator (R-114; Buchi, Switzerland) at 37°C, under pressure, to form a thin film on the flask. The film was hydrated with 0.9% sodium chloride solution. MLV liposomes were formed by vortexing for 5 min (MS1 minishaker Vortex, IKA, Connecticut, USA). The final concentrations were 10 mg/ml for DMPC and 91.5 μg/ml for Lissamine rhodamine PE.
SUV liposomes were prepared from the MLVs by reducing vesicles to the smallest possible size. This procedure imparts energy at a high level. Suspension of MLVs was transferred to a round-bottomed tube with straight sides and a diameter slightly greater than that of the probe. The vessel was immersed in a cooling bath and nitrogen inserted to avoid excessive heat and lipid oxidation, respectively. Total sonication time of 30 min to1 h was sufficient to make a clear suspension. During sonication (Probe-Sonicator Dr. Hielscher; Gmbh, Germany) either an amplitude of 60% and cycle 1 for 30 s or an amplitude of 100% and cycle 0.5 for 1 min was used to avoid overheating. After sonication, liposomes were left in the water bath (B-480; Buchi) for approximately 1.5 h at a temperature of 37°C—above their transition temperature. Finally, the liposome suspension was centrifuged (Sorvall Ultra Pro 80, Newtown, USA) at 20,000 r/min at 4°C for 20 min to sediment undispersed lipids and MLVs and to remove particles of titanium released from the probe.
Skin application
Liposomes and Lissamine rhodamine (91.5 μg/ml) were applied to 10 animals and 10 others served as control. Plexiglass rings of 2 cm2 were attached with silicon glue to the lower back and 400 μl (18.3 μg/cm2) of liposome or lipid suspension were applied for 3 h. At the end of application time, blood was collected after killing the mice in EDTA-coated tubes. Six tape strips (3M invisible tape) removed stratum corneum at the application site. Living skin and subcutaneous fat biopsies were collected from the area were MLVs, SUVs, and Lissamine rhodamine were applied.
Sample preparation
Methanol was added to the blood samples in a ratio of 1:1 v/w, mixed for 1 min (vortex minishaker MS1, IKA, Connecticut, USA), and centrifuged at 8°C for 30 min at 10,000 r/min (Universal 32R; Hettich, Zentrifugen, Germany). Supernatant mixture of serum with methanol was obtained and filtered (Millex-GV). Skin was sectioned in pieces of about 1–2 mm2 with surgical scissors and transferred to the homogenizer tube; 1.5 ml of methanol was added to the skin and homogenized on ice for 15–20 min with a Black & Decker homozenizer (DNJ52 H29; Black & Decker, Towson, Maryland, USA). Solution was centrifuged and filtered in the conditions similar to blood. Tape strips were taken in pairs; 1.5 ml of methanol was added to two strips, vortexed for 3 min, and sonicated (Transonic T460/h; Elma, Metrolab, UK) for 1 min.
Fluorometry
FluoStar Galaxy (BMG; Lab-technologies, Ortenberg, Germany) was used for fluorescence measurements. Two hundred microliters of each sample were introduced into the wells of Costar plates 96 (Costar). Fluorescence was measured using an excitation filter at 555 nm and an emission filter at 613 nm. The calibration curve for Lissamine rhodamine using a range of concentrations from 0.000438 to 0.2 μg/ml is shown in Figure 1. The lower Lissamine rhodamine concentration that could be measured with this method was 0.0004 μg/ml. For Lissamine rhodamine concentrations, appropriate higher dilutions of 0.2 μg/ml were done.
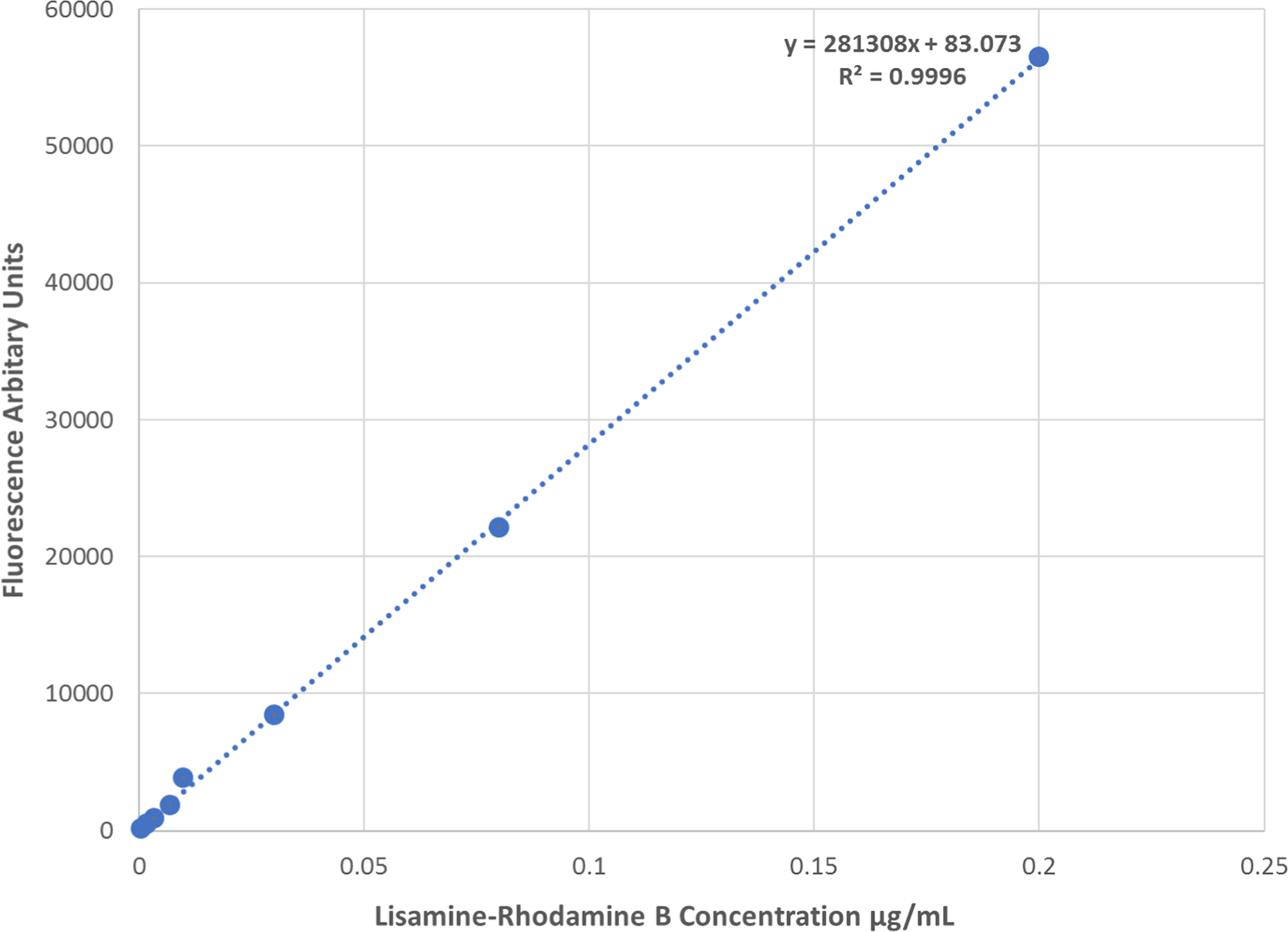
Lissamine rhodamine calibration curve. The lower Lissamine rhodamine concentration that could be measured with this method is 0.0004 μg/ml.
MLV liposomes size
MLVs’ size was measured by “MASTERSIZER” (Malvern Instruments Ltd, Worcestershire, UK). A small quantity of the MLV liposomes was introduced, with stirring, in a solution of 0.9% sodium chloride. The instrument’s optical unit captured the actual scattering pattern from the field of particles and converts it to particle size.
This technique cannot be applied for the evaluation of SUV liposomes.
Data analysis
Average and standard deviation of the Lissamine rhodamine concentration in the stratum corneum and residual skin were calculated for each animal group. Analysis of variance single factor with a 0.05 significance level was applied on data in order to reveal the differences in average concentration of each group and skin layer.
Results
Size of MLVs
The mean particle size for the MLVs was 1.23 μm, and the distribution of MLVs was as follows: 10% <1.09 μm, 20% <1.22 μm, 50% <1.81 μm, 80% <3.26 μm, and 90% <4.10 μm. Two weeks later, the mean particle size increased to 8.18 μm.
Stratum corneum penetration
Penetration of Lissamine rhodamine B in stratum corneum with MLV and SUV liposomal form and in the nonliposomal one is shown in Figure 2. It is expressed as per micrometer, as the mean thickness of stratum corneum in hairless mice was previously evaluated at 10 μm. 30 Penetration of the lipid is nonstatistically significant (p = 0.4) only with comparison between the groups treated with MLV and SUV liposomes. In all other group comparisons, there is statistically significant (p < 0.006) difference in the means of Lissamine rhodamine B concentration. The nonliposomal penetration of lipid in stratum corneum exceeded that in the liposomal form.
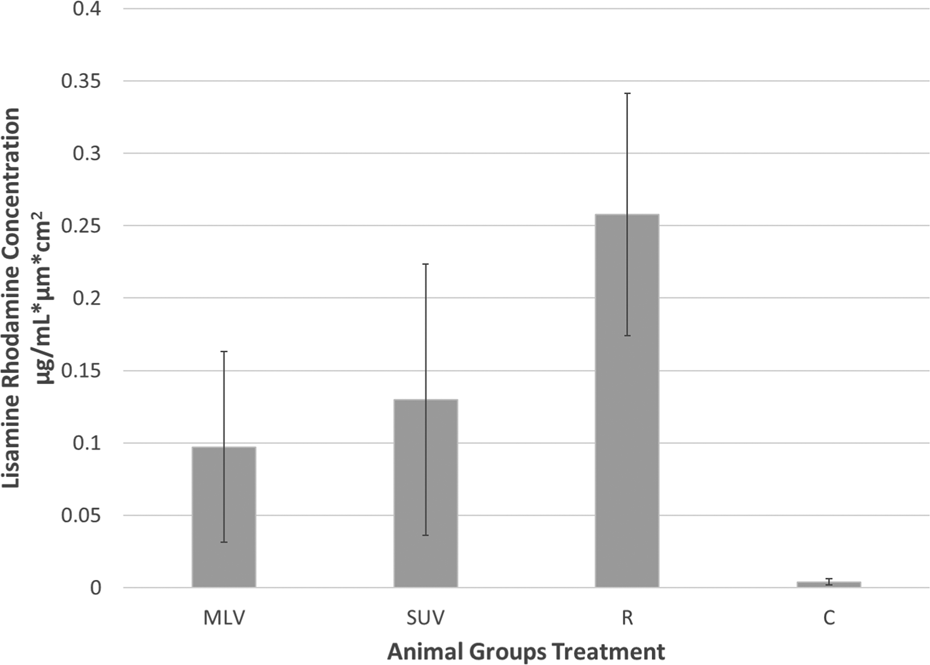
Lissamine rhodamine concentration in stratum corneum. Penetration of lipid in SC in the nonliposomal form exceeded than in liposomal. MLV and SUV liposomes do penetrate in stratum corneum. MLV: multilamellar vesicle; SUVs: small unilamellar vesicle.
Living skin absorption
Only the Lissamine rhodamine B in the nonliposomal form penetrated viable skin in a statistically significant manner (p < 0.00008). Lipids in the MLV and SUV liposomes did not penetrate living skin in a statistically significant way (p > 0.5). Comparative absorption of the Lissamine rhodamine B in liposomal and nonliposomal form is shown in Figure 3. It is expressed per micrometer. Depth of the residual epidermis, dermis, and subcutis was previously estimated in mean about 540 μm. 30 Figures 2 and 3 show higher penetration of lipid (Lissamine rhodamine B) into stratum corneum and viable skin.
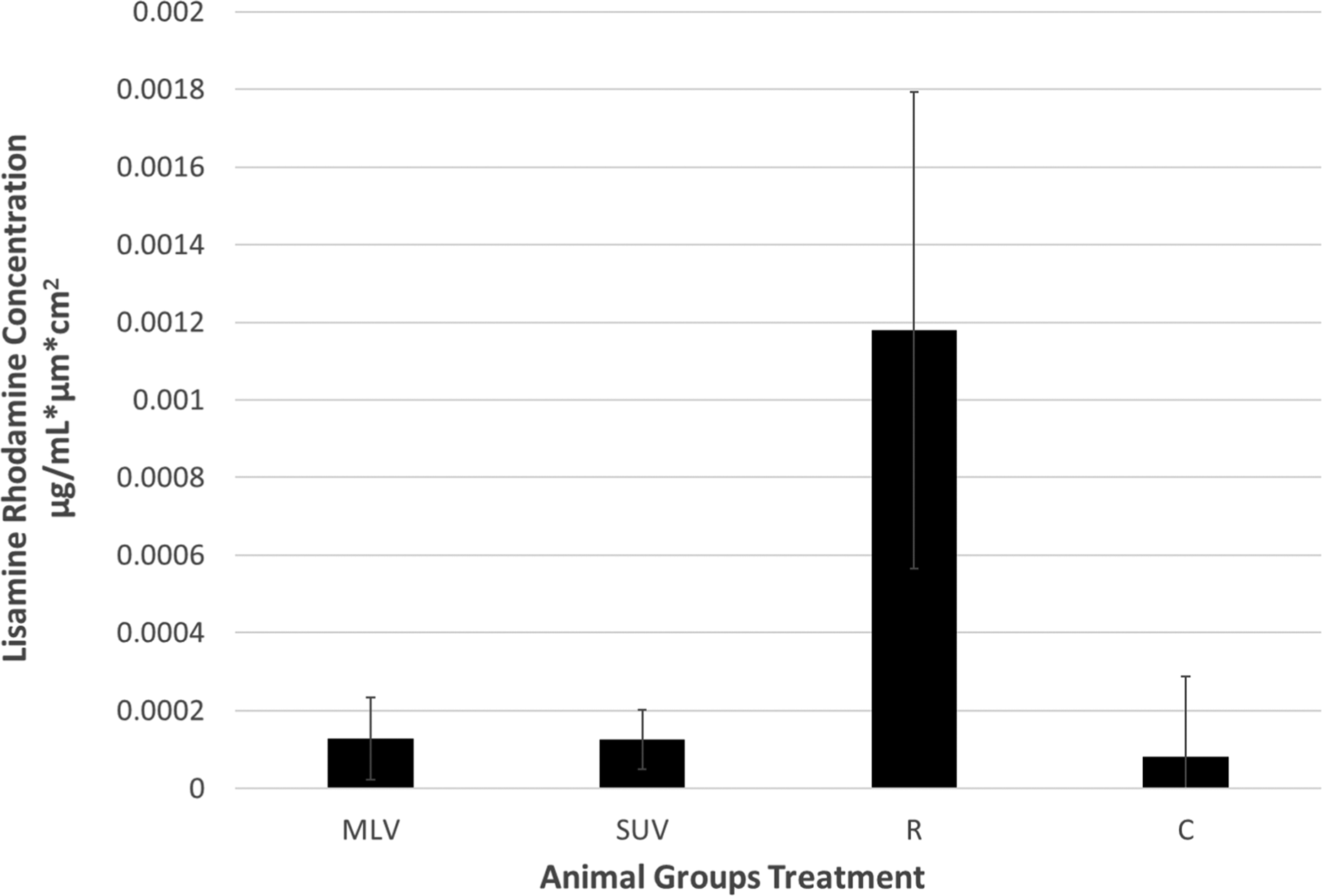
Lissamine rhodamine concentration in skin. MLV and SUV liposomes did not significantly absorbed in viable skin. MLV: multilamellar vesicle; SUV: small unilamellar vesicle.
Lipid rhodamine concentration per micrometer in nonliposomal form is about 370 times higher in stratum corneum (Figure 2) than in viable skin (Figure 3). Figure 4 shows the comparative total SC penetration and skin absorption for liposomes and nonlipids.
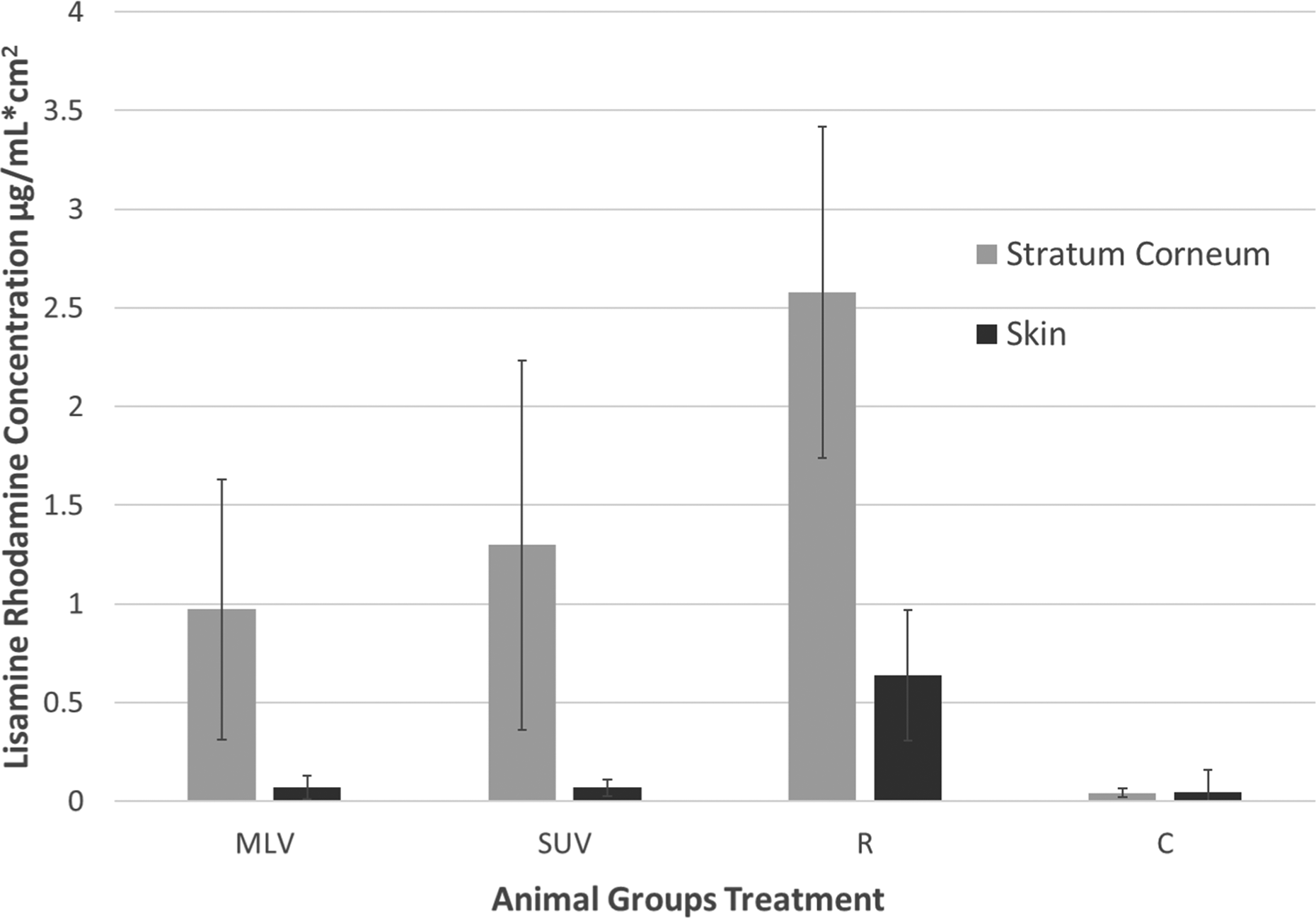
Lissamine rhodamine total stratum corneum penetration and skin absorption. Only Lissamine rhodamine in nonliposomal form is significantly absorbed in viable skin.
Systemic absorption
Figure 5 shows Lissamine rhodamine blood concentration. No statistical difference in average concentration of Lissamine rhodamine was observed between the animal groups.
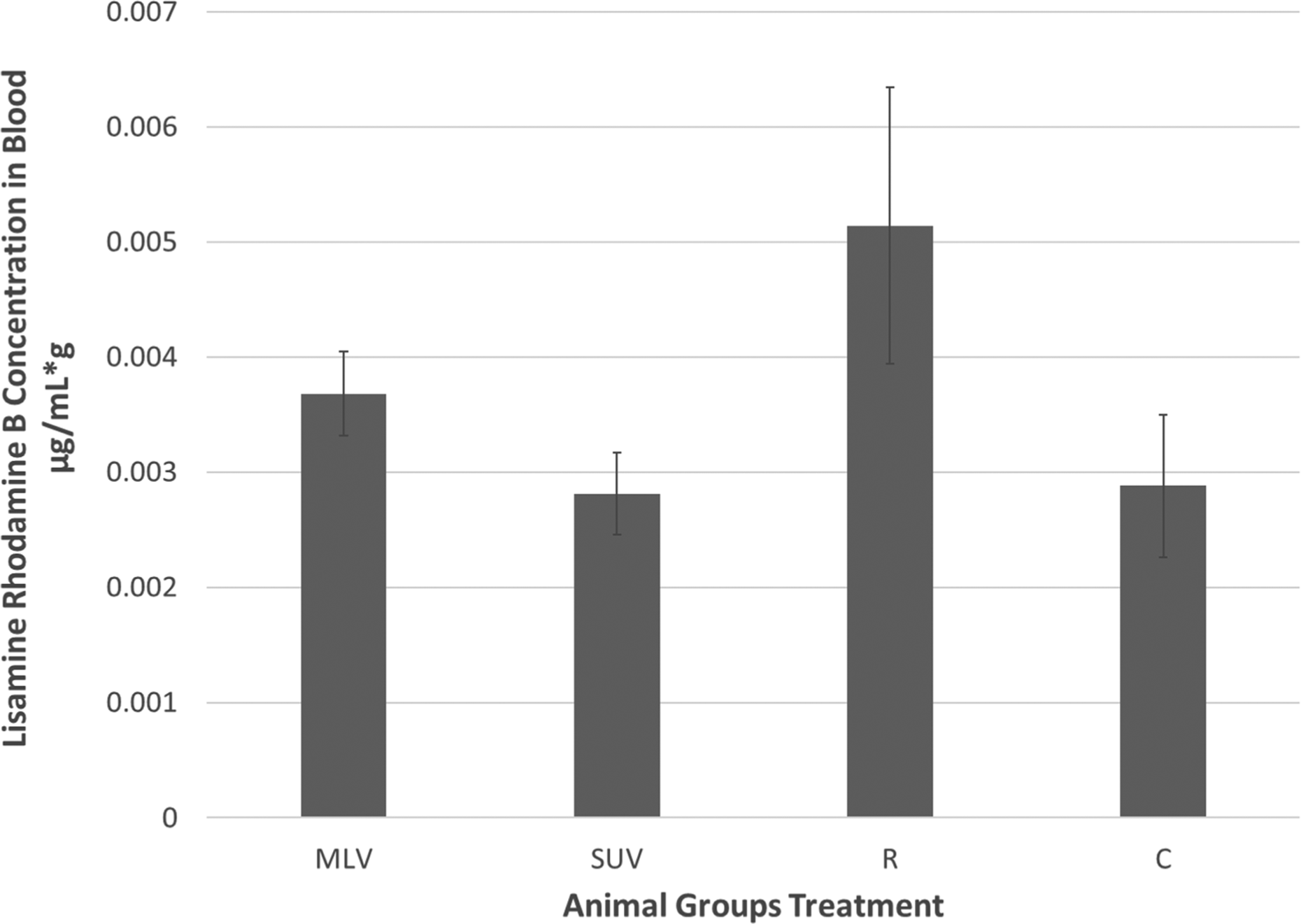
Lissamine rhodamine concentration in blood. Practically, no Lissamine rhodamine was detected in the blood.
Discussion
Size increase of MLV liposomes 2 weeks after preparation reveals that their aggregation into large particles. For this reason, only fresh MLVs were used. No such results were obtained for SUVs (20–50nm), as their size was insufficient for accurate measurements.
MLVs and SUVs present similar ability to penetrate into stratum corneum (Figure 2). Difference in penetration can be seen between the two liposome types and the lipid form, suggesting that the barrier function of stratum corneum is important for liposomes. However, by comparing control group and liposome groups, it is understood that the penetration MLVs and SUVs into stratum corneum is a significant and remarkable.
The study by Aggarwal and Goindi using confocal laser scanning colorimetry visualized liposome penetration in human skin in vitro. 24 Liposomes penetrated stratum corneum at different depths. Most penetrated to upper stratum corneum layers. Only liposomes containing dioleoylphosphatidylethanolamine (DOPE) penetrated into deeper stratum corneum. Roding and Artmann studied in vivo in pigs the absorption of an oligolamellar negatively charged liposome-containing soya phospholipids using different concentrations and application times. 28 The liposome penetrated mainly into the stratum corneum, while it was found 200 times lower in epidermis and almost 800 and 10,000 times lower, respectively, in dermis and subcutis. The study by Lasch et al. using fluoromicography in vitro to visualize the penetration of intact liposomes concluded that they did not penetrate deeper stratum corneum. 29
In accordance with the obtained data from literature, liposomes penetrate in significant amounts into stratum corneum. Their lipid components do penetrate in much higher rates in both stratum corneum and viable skin (Figures 2 and 3).
For these MLV and SUV liposomes, size did not play an important role in the penetration rate and the ability to penetrate into stratum corneum and viable skin (Figures 2 and 3).
The in vivo experiments showed that the liposomes are unable to pass through stratum corneum. A question to be answered is whether other types of liposomes like the deformable have this ability, as some data suggest that only skin appendages 25 do so. In an in vitro assay, the fact of enhanced penetration of liposomal ibuprofen in relation to a commercial formulation could be due to the simultaneous use of surfactants as penetration enhancers is explained by the authors as the transformation of liposome vesicle structure into planar. 29
Neither lipid nor MLV and SUV liposomes are systemically absorbed in blood (Figure 5). Even though nonstatistically significant, much higher mean concentration of Lissamine rhodamine B-PE in nonliposomal form was observed.
How do the liposomes act on skin? Do they penetrate and, if so, which types? Do they act as slow releasers of active ingredients entering stratum disjunctum, as they are more compact than the stratum compactum? Do they act as depots on skin surface? Are they impeded to penetrate hydrophilic media like viable epidermis and dermis? These questions must be clarified using in vivo skin models, as the vitro assays may not always represent reality. 31 Study limitations includes that is realized in mice and non in humans and even though fluorescence determination is considered as highly sensitive method, another type of analysis as chemiluminescence could be more appropriate. Future experiments could include comparative studies between different liposome types and long application times examining the possibility of liposomes acting as slow drug releasers.
Teaching point
Even though conventional liposomes are more or less widely used in topical skin preparations, especially cosmetics, our results do not confirm significant contribution to their pharmacological performance.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
