Abstract
Medical education has evolved over time toward a model which integrates clinical medicine with the basic sciences. More recently, medical education has put an emphasis on outcome-based education. Other areas of health care education have had a similar emphasis which can provide models to inform a new model for medical education. The Roseman University of Health Sciences has developed and implemented a model based on underlying tenets of mastery learning since 1999. The model has been implemented in pharmacy, nursing, and dental education. It was conceived as an integration of 6 key points which reinforce each other and interrelate to support learning. The model has been modified for application to medical education in support of medical education’s outcome-based emphasis and to address the educational demands of the changing environment of the practice of medicine.
Background
Medical school curriculum and treatment have evolved since the latter 19th century, when medical educators began to rethink the educational process, rejecting memorization and moving toward problem solving and critical thinking. Abraham Flexner’s
1
report to the Carnegie Foundation for the Advancement of Teaching furthered the process by emphasizing the scientific basis of the practice of medicine. Integration of clinical medicine and the basic sciences slowly evolved. In 1993, the Association of American Medical Colleges published its
Subsequently, outcomes were emphasized, stressing student acquisition of knowledge and clinical performance over the structure of the curriculum. The Medical School Outcome Project3,4 and the movement to competencies were key drivers. More recently, the Physician Competency Reference Set 5 and the Core Entrustable Professional Activities project 6 have driven the outcomes/student performance aspect of undergraduate medical education curricular development efforts. Medical schools began altering their approach to teaching. One example was the shift to earlier patient experience.
The challenge for medical schools remains delivery of a curriculum, within the context of a constantly growing core knowledge base, the development of leadership, communication and professional skills, as well as to maximize the student’s education, foster their short and long-term learning, and produce lifelong learners with a passion for their career.
The Physician in the 21st Century
The issue
The changing climate of health care has placed practicing physicians in time-limited and productivity-driven environments, with compensation tied to seeing more patients. Forces from society, government, and the marketplace have decreased autonomy in the decision making of physicians within their scope of practice, in turn pressuring changes in the education of these physicians. This potentially results in a compromise of provision of the level of patient care for which they were trained. Increasing utilization of nurse practitioners and physician assistants, as well as patients assuming more responsibility for their care, should in theory allow physicians the opportunity to provide the care at a higher and more thorough level. These changes in role, combined with outside pressures, direct changes in the future physician’s professional identity and skill set. Team-based care, where the physician is the captain of the team and manages quality aligned with the goals of the Institute for Healthcare Improvement’s Triple Aim, 7 appears to be the direction toward which education should be aimed.
It is imperative that medical training programs at the undergraduate and graduate medical education levels incorporate and emphasize the concepts of problem solving, critical thinking and the tools for quality improvement, high value health care, and population management. Ideal training sites for the physicians of tomorrow must emphasize interdisciplinary teamwork in the care of their patients.
The solution
Prior to and most recently in 2013, the American Medical Association’s (AMA) Accelerating Change in Medical Education
8
consortium focused an initiative, outlined in an AMA paper entitled
Develop new methods for measuring and assessing key competencies for physicians at all training levels to create more flexible, individualized learning plans;
Promote exemplary methods to achieve patient safety, performance improvement, and patient-centered team care;
Improve understanding of the health care system and health care financing in medical training;
Optimize the learning environment.
The model
The “Roseman University 6-Point Mastery Learning Model” was developed to facilitate the learning and training of pharmacists and integrates 6 key tenets which reinforce each other and interrelate to support training. It has been successfully applied to educational programs in nursing, dentistry, and business administration. We believe this model can be successfully adapted to medical education (Figure 1).

“The Roseman University Health Sciences Model.”
The model has as its basis the concept that educational progress is determined through regularly spaced testing of a single skill or a body of knowledge before proceeding to the next skill or body of knowledge. Assessment is ongoing and continuous until achievement of 90% score. Content is designed in attainable blocks of knowledge to be mastered. Classrooms and learning environment are designed to maximize interaction of students and faculty. Curriculum is delivered using active and interactive learning methods. Relevant experiential and clinical activities are included early in the curriculum.
Through consensual discussion, a task force of faculty in the College of Medicine developed medicine-specific definitions or interpretations of the 6 tenets of the Roseman model. These can in turn guide development and implementation of the curriculum. The medicine-specific definitions are an extension of the Roseman University definitions: the inherent flexibility of the model will allow the medical curriculum to be delivered to meet the needs of the profession just as it has done with the Roseman programs in pharmacy, nursing, dental medicine, and business administration. The flexibility of the model allows the planned medical curriculum to meet medical school accreditation body requirements for outcome-based education:
Block curriculum and assessment encourage students to focus on the medically relevant material and keeps track of their progress toward mastery as content is mapped to course objectives, program objectives, and physician competencies.
Students will be held to a high level of competence achievement in key curricula objectives.
The learning environment will maximize interaction with peers and faculty while being rich in early and continuous experiential involvement.
A comparison of the definitions of these tenets is shown in Table 1.
Comparative definitions.

We feel it is important to highlight that this active and collaborative learning model will promote the development of new skills in students and prepare them to practice medicine in the 21st century. Advocating for health care, engaging with the community, and partnering with the patient are among the fundamentals emphasized throughout the collaborative interactive curriculum (Figure 2).

Condensed Definition.
Implementation and Expected Outcomes
The implementation of a curriculum requires many things including identification of workforce and financial resources, with continued administrative oversight during all phases of development and implementation.
The tenets of our model provide the framework for faculty development.
The College of Medicine model curriculum supports students as they strive to reach specific levels of achievement based on the Physician Reference Competency Set (PCRS). 5 The PCRS was used by our faculty to develop our overarching program objectives and measurable outcomes. The 6-point learning model curriculum includes clearly identified specific content, integrated across and between blocks. The block approach supports a deeper understanding by focusing content. The model assures attention to the learning environment and its impact on teaching and learning.
One aspect of the learning environment is that physical space is optimized to favor faculty and student interactions, supported by appropriate technology. Progress is measured against specific standards of knowledge, attitudes, and skills with shared understanding of levels of attainment required. Integration of content is enhanced through early experiential learning in the clinical settings of our longitudinal courses. Students will have the opportunity to apply classroom learning to experiences of patient care, physician role, and the business of health care. The model provides support for a variety of instructional methods relevant to medical education and practice, allowing for deeper understanding of key concepts and their application. Interaction among students, faculty, and other professionals (interprofessional education), another aspect of the learning environment, serves to increase student engagement and encourages ongoing self-assessment.
Assessment, as formal tracking of learning, is integrated in the curriculum and becomes an additional tool to develop and demonstrate mastery of the content and its application. By extension, assessment supports student progress and enhances the educational process. When multiple-choice examination questions are administered, students will take the examination individually and then as a group. This allows the examination to become a learning tool, with team-teaching emphasized. In addition, it represents early application of the principles (competency domain) of practice-based learning and improvement.
Based on the implementation of our curriculum, a series of measurable outcomes related to the objectives developed for both the preclerkship and clerkship years will be achievable in the 6-point learning model. The curriculum provides for an increased focus and deeper understanding of content with provision for application, integration, and independent learning in an environment that encourages interaction, insight, and self-assessment. We believe this framework may support the application of the current medical education trend related to the principles of the entrustable professional activities. 6
Discussion
Medical education has been challenged to revise its traditional lecture base to better prepare physicians for practice in the changed health care environment of the 21st century. Numerous approaches have been advanced to address this challenge including emphases on active learning, interprofessional education, teamwork, problem solving, and competency assessment. The application of this 6-point learning model provides an integrated approach to incorporating these educational priorities and new methodologies to our medical curriculum. It is also an opportunity to
A rigorous 90% pass score is central to the model. It encourages students to achieve a high level of proficiency in specific content at a specific time in their educational path: the expectation is that the student will attain the equivalent of an “A” grade to progress, rather than progressing as a “B” or “C” student. In Roseman University’s current programs, a consequence of the 90% pass score is that student remediation rates while enrolled in their program are relatively high, varying from 36% to 52%.
10
However, the assessment-reassessment remediation cycle gives the student the opportunity to achieve this high level of performance that is a core tenet of the model. Remediation is a key component of competency-based education and is presented as a positive opportunity to develop a deeper understanding of the material. The cycle also helps to fulfill one of the expected criteria for mastery learning as defined in the
The structure of the curriculum (Figure 3) for the years 1 and 2 is used here to illustrate that it provides the elements to implement the College of Medicine 6-point learning model. The model has applicability as well for students in years 3 and 4 with their near-complete immersion in the clinical settings. The inherent flexibility of the model is seen through certain hexagons being differentially emphasized and or interpreted at different periods of the program. For example, in the third and fourth years, the early “experiential learning” hexagon recedes in importance, and the “classroom as teacher” hexagon becomes the inpatient and outpatient clinical experience sites. The “assessment as learning” hexagon is one that remains constant in its emphasis across the 4 years. A variety of methods will be used within the model to measure level-appropriate performance in early patient exposure in years 1 and 2 and clerkship settings in years 3 and 4. The application of these tenets adjusts from more cognitive to more clinical content. Programmatic evaluation of the 6-point learning model using the Kirkpatrick Evaluation Model will allow us to monitor the model’s effectiveness in achieving the high level of proficiency of professional and educational competencies (ie, problem solving, critical thinking, self-directed learning, and knowledge to meet the expectations of the workplace).
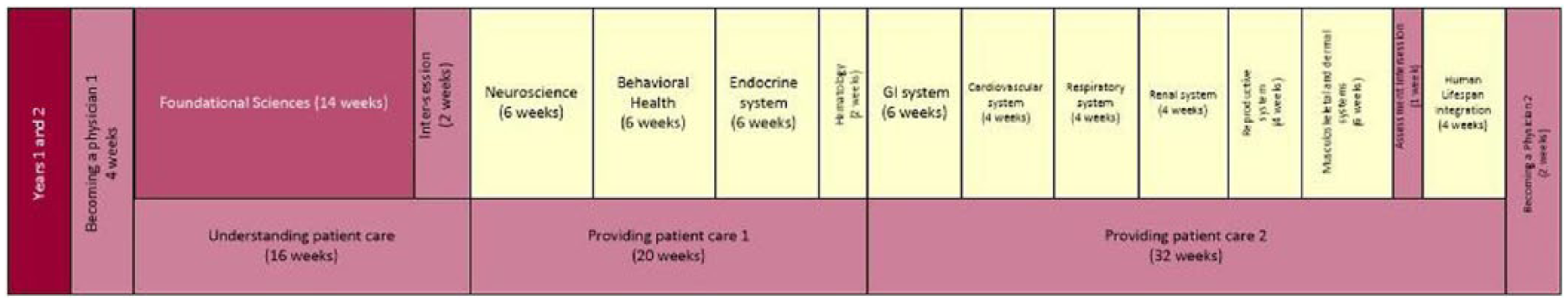
Proposed years 1 and 2 integrated curriculum.
Figure 3 illustrates the curricular plan to have integration of the biomedical sciences, coordination with a series of clinical experiences, and early exposure to patients. The content of the organ system being taught is referred in the longitudinal course and complements and enhances the students’ understanding of the concepts of clinical experiences.
The 6-point learning model adds the dimension of collaboration, active learning, and early consistent involvement in patient care over time to the aspects of its mastery learning components. The early experiential learning will allow for the competency domains of professionalism, communication, and leadership to be introduced early and in a consistent fashion. The model strives to apply components of mastery learning to the content of medical education as well as the development of physician identity and professionalism to its medical students, with the goal of graduating proficient, confident medical doctors who will relate effectively to peers, patients, and the community.
Conclusions
The underlying principles of mastery learning were adapted by the Roseman University in developing a curriculum for its health sciences colleges. With the creation of the Roseman University College of Medicine, this approach is further modified to meet the needs of a medical school’s educational program. The College of Medicine 6-point learning model, as implemented in the college, will address the need to educate students for the changing environment of the practice of medicine while providing them with the medical knowledge, skills, and attitude to continue their development and career in medicine. This model adds important aspects of mastery learning to medical education. Although not rigidly adherent to the model of mastery learning proposed in the series in
Footnotes
Acknowledgements
The authors thank Anne Marie DeMarco Rehm Administrative Assistant, Office of Academic Affairs, Roseman University Health Sciences College of Medicine. This manuscript was prepared by the Roseman University Health Sciences College of Medicine Mastery Learning Task Force.
Declaration of conflicting interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Author Contributions
JL and JR served as co-primary authors. The additional authors were involved in the task force, development of the content that served as the basis for the paper and editing of the final document.
