Abstract
Background
It is increasingly important to create longitudinal advocacy education opportunities starting as early as medical school to train physicians capable of handling the complexities of the social determinants of health that they will encounter in their communities. This is a brief overview of the journey of medical students in developing an interdisciplinary, longitudinal advocacy curriculum at the University of New Mexico School of Medicine (UNM SOM).
Methods
The Healthcare Advocacy Initiative of New Mexico (HAINM) has disseminated information on the significance and structure of health policy in New Mexico through various educational opportunities by communicating with state representatives, community advocates, law students, professors, and professional advocacy organizations. To analyze the significance of these experiences, a survey was conducted at the capstone event.
Results
Pre- and post-test survey responses from the interprofessional “Med/Law/Psych Day 2025” event were analyzed using Wilcoxon signed-rank tests. Two events were found to be statistically significant (developing a plan to change policy related to healthcare issues and teaching other peers advocacy skills) with P < .05 and .04, respectively. Differences in survey data collected before and after the interprofessional advocacy event demonstrate that a majority of respondents reported a mild to moderate increase in proficiency after attending the event.
Discussion
HAINM has become a hub for a continuous medical advocacy curriculum that is available to medical students through all 4 years of training. This provides interested students with a solid foundation, a skill set, and a network to pursue interprofessional advocacy work successfully.
Keywords
Introduction
Understanding the physician as an advocate becomes apparent at each level of healthcare; socioeconomic and cultural disparities from patient to patient, fragmented health teams and systems that reduce clinical productivity, and political decisions that can consequently leave some with less than equitable access.1–3 Becoming an advocate for one's patients may also improve medical professionals’ barriers that come about navigating care in a complex healthcare landscape. 4 A crucial aspect of early engagement of medical students in health policy is ensuring that institutional leaders in health education are committed to emphasizing the advocate role of all physicians, regardless of specialty, and the foundational role they play in communities through research, engagement, and quality improvement. 5 Currently, structured global or public health programs are present at approximately 39% of US allopathic and osteopathic medical schools. There is little standardization in program structure or requirements, and most programs are internally administered. 6 Most US medical schools offer at least one advocacy-related course. Still, these are predominantly elective rather than required, and may focus on health policy, population health, public health/epidemiology, or specific populations such as children or persons with low socioeconomic status. 7 Medical curricula are densely packed, making it difficult to allocate time for advocacy training without displacing other required content. This is consistently cited as a major barrier to both undergraduate and graduate advocacy medical education. 8 Communication between organizations that address social and legal needs outside of the healthcare system with medical professionals who are involved in patient advocacy offers a solution to barriers which hinder social progress on account of limited ability to coordinate and plan among involved parties, often due to differences in administrative structure, informal agreements, and lack of resources. 9
Our goal is to foster the above collaboration through a comprehensive, longitudinal health advocacy curriculum available to all medical students throughout their 4 years of undergraduate medical education rooted in collaboration with other healthcare professionals and community organizations. The Healthcare Advocacy Initiative of New Mexico (HAINM) was created to enhance advocacy training available for health science professionals and law students. There are several components to HAINM, such as a longitudinal curriculum, regular lunch seminars with community stakeholders, and legislative session educational opportunities. In addition, we host our annual capstone event, “Med/Law/Psych Day,” an interprofessional educational event for medical, legal, psychology, and public health students to engage in cased-based learning on multidisciplinary teams and share interdisciplinary research. This event highlights the importance of interprofessional communication in managing complex socioeconomic factors that act as barriers to patients receiving quality, holistic healthcare.
Methods
Members of HAINM are encouraged to dialogue with local lawmakers about their professional experiences through mentored educational opportunities at the legislative session. To this end, medical students at the University of New Mexico (UNM) can elect to attend legislative sessions at the State Capitol through a shadowing experience with a state lobbyist from the New Mexico Academy of Family Physicians (NMFAP) through a program called the “Student of the Day” experience; here students gained exposure to the legislative process and role of lobbyists in communicating the legislative priorities of a greater medical society, in addition to learning how to visit legislators’ offices to advocate for or against bills of interest. Additionally, UNM and Burrell College medical students collaborated with the New Mexico Medical Society (NMMS) to attend the annual “White Coat Day” at the legislative session, hosted by physicians across NM experienced in health advocacy; here students were encouraged to engage with key community stakeholders, including leaders of local nonprofits and grassroots organizations, judges, state representatives, public defenders, education deans, and members of legislative committees.
Along with events like those above, a more longitudinal asynchronous advocacy curriculum, named the Community of Healthcare Advocates (CHA), is available to first year medical students on an opt-in, extracurricular, application-based process at UNM for completion over 4 years of their training (Figure 1). As a member of CHA, students must complete various assignments including a combination of lectures and activities, such as conducting community needs assessments, participating in service projects, writing opinion editorials, attending state committee meetings, and lobbying legislators. Lastly, our capstone event, the “Med/Law/Psych Day” is an educational conference for individuals interested in the interprofessional intersections between medicine, law, and psychology in healthcare, with attendees from UNM undergraduate, graduate, health science, and law campuses. Case-based learning was facilitated by preceptors from each discipline who were recruited and included UNM School of Medicine faculty, forensic psychologists, community physicians, UNM School of Law faculty, community attorneys, district court judges, and UNM board of regents members. Conference attendees were randomly and evenly distributed into 8 to 10 participants per group with 3 to 5 preceptors per group representing each of the 3 disciplines of medicine, law, and psychology. Small group discussion and case-based learning were utilized to teach both students and professionals how to collaborate in mitigating complex socioeconomic, political, and psychological barriers that prevent patients from fully accessing healthcare. This stimulates the type of collaboration that occurs in medical-legal partnerships. 10

Objectives for learning in the Community of Health Advocacy year 1 curriculum.
Data Collection
IRB approval (Study 25-232) was obtained to send a pre- and post-event Likert scale survey to each of the participants of “Med/Law/Psych Day 2025” via the RedCap surveying system. 11 Pre-/post-test questions were implemented to assess if the event increased interest in healthcare advocacy and competency in pursuing advocacy initiatives in one's future career. Those who attended the event in its entirety and who voluntarily consented and completed the survey were included in the survey response analysis. Additionally, participants were asked to qualitatively identify the role of public health professionals in upholding social accountability, an approach toward building accountability that holds healthcare professionals to a standard of care that addresses the complexities of their patients’ life circumstances. 2 The survey used in the study is novel, and is being pilot tested at this event. Ongoing use of this survey in subsequent events will ensue.
Data Analysis
Likert scale and free text responses evaluated individual interest and competency.
We assessed competency before and after attending the event, using the Wilcoxon signed-rank test to evaluate differences in responses before and after participation in the event. A histogram of differences was created for each before-and-after question to determine whether participation tended to increase, decrease, or have no effect on competency and confidence. Biases may be present, but mitigation has ensued by pre- and postsurveying methods within the same day of the event to reflect the value of the event on the professionals’ advocacy endeavors.
Results
There were on average 25 to 35 attendees from the UNM Health Sciences Center at each educational session. Approximately 20 medical students participated in “Student of the Day 2025,” and 30 medical students participated in the “2025 White Coat Day,” marking the most significant turnout of medical students at the New Mexico Roundhouse in its history.
Notably, student participation was key in the design and advocacy of instating the Behavioral Health Reform & Investment Act, which established a $100 million fund to reform state behavioral health services using the Sequential Intercept Model. 12 Additionally, with the help of student testimony and mobilization, HAINM contributed to the opposition of a scope of practice bill that would be detrimental to providing quality healthcare services to medically underserved areas of New Mexico. 13
In our analysis of “Med/Law/Psych Day 2025,” 14 survey responses were voluntarily received and analyzed. A distribution of respondents can be found in Figure 2. Two pre-/post-test competency events were found to be statistically significant (developing a plan to change policy related to healthcare issues, teaching other peers advocacy skills) with P < .05 and .04, respectively. Differences in survey data collected before and after the interprofessional advocacy event demonstrate a mild to moderate increase in proficiency following attendance at the event (Figure 3). A summary of P-values for each before/after question assessed is included in Table 1. The average Likert rating scores of interest in incorporating advocacy and health policy work into an individual's profession (1 being “No interest” to 5 being “Strong Interest”) were assessed through 4 questions, with an average rating of 4.20 ± 0.12. The average Likert rating scores of competency in incorporating advocacy and health policy work into an individual's profession were assessed through 4 questions, of which average ratings were 4.45 ± 0.00634. Regarding interprofessional collaboration, an average score of 4.71 ± 0.726 was reported when respondents were asked if the event inspired them to pursue more interprofessional collaboration efforts regarding healthcare advocacy and/or policy in their future career. An average score of 4.57 ± 0.935 was reported when respondents were asked if the event “helped me learn more about other students and professionals in their respective medical, legal, and psychological/psychiatric professions.”
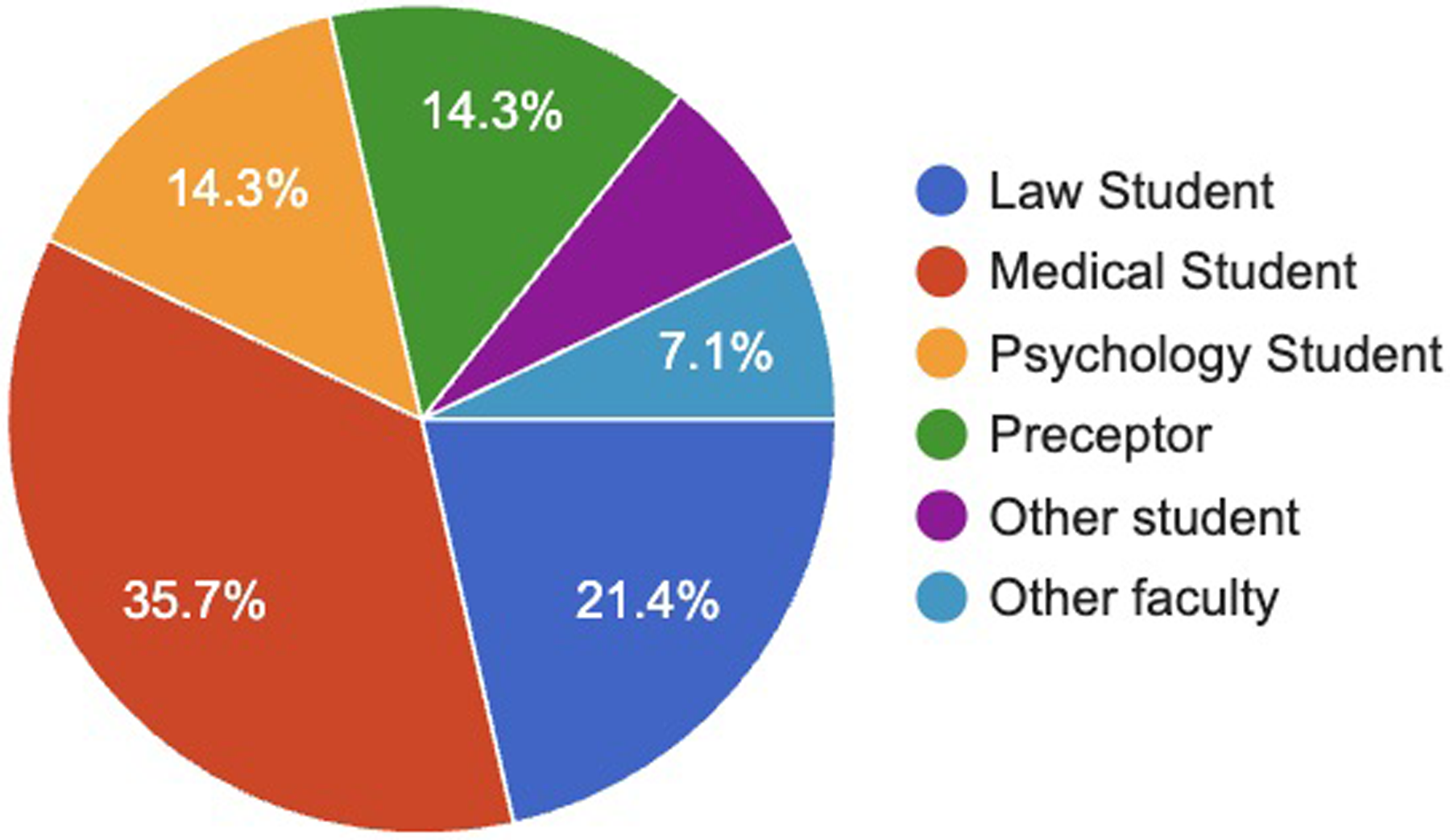
Student and professional representation at the “Med/Law/Psych Day” event.
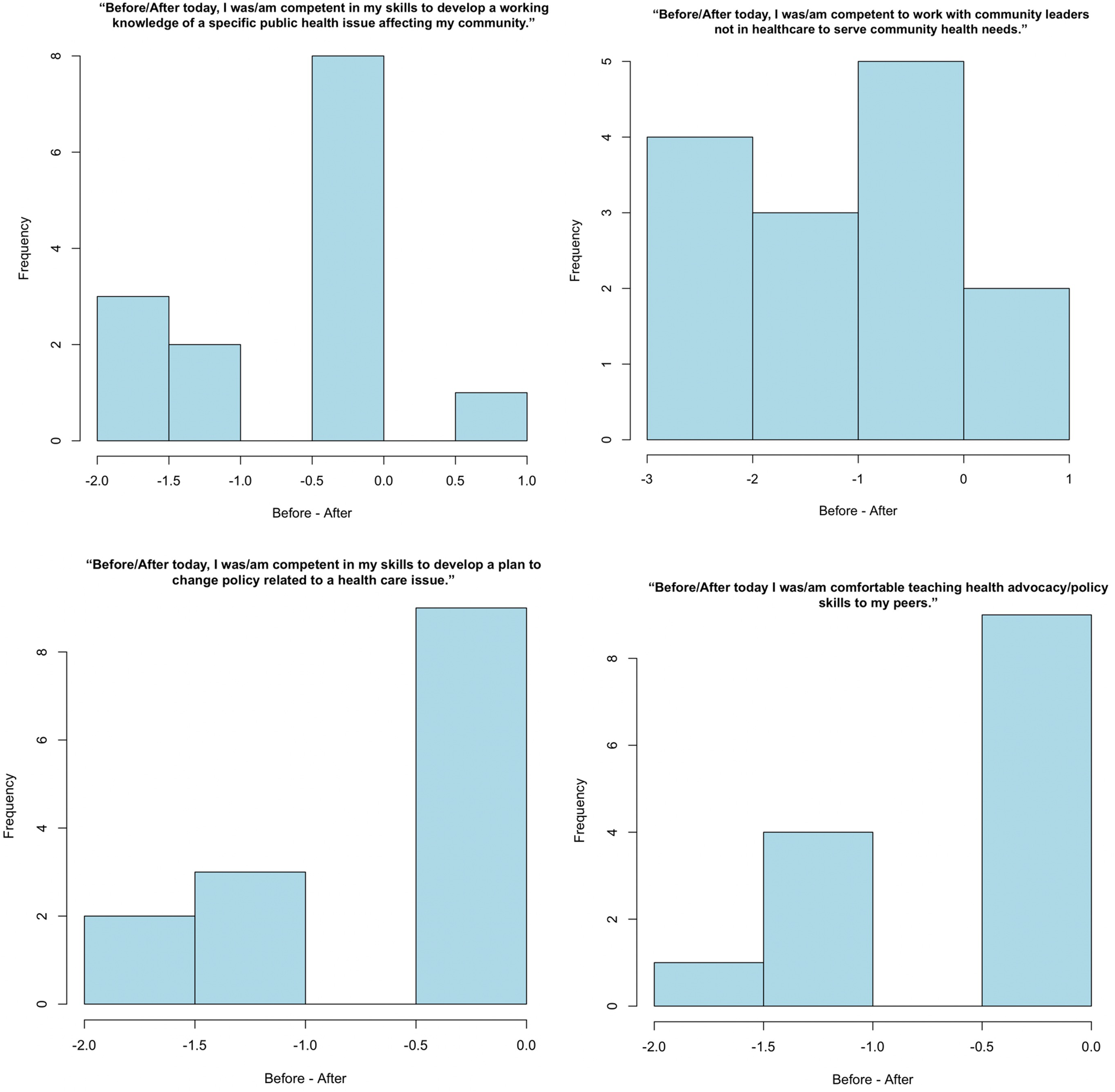
Historiographical differences between the 4 before/after questions. Negative differences are associated with an increase in competency when measuring before-after for all rankings on the x-axis and frequency of the response on the y-axis.
Wilcoxon signed-rank test comparing competency according to the following questions and associated p-values.

In response to an open-ended question on the survey based on the theme of a health professional's role in social accountability, one individual said, “I believe it is the duty of public service professionals to participate and lead their communities in social accountability. If any real headway is to be made in addressing the physician shortage and health crisis in New Mexico (NM), public service professionals must step up as leaders to enact upstream change. What's more, it is vital that interdisciplinary public service professionals work together to create such change. We need each other.” Another said, “Public service professionals earn credibility and respect for their participation in the communities they work with. These roles inherently require professionals to take social accountability in order to enact real change.”
Discussion
HAINM demonstrates measurable success in exemplifying the impact and value of interprofessional collaboration on health advocacy education and training. In particular, the data gathered from “Med/Law/Psych Day 2025” highlights the efficacy of a single interprofessional health advocacy event on health professional students’ confidence in their ability to develop a plan to change policy related to healthcare issues and to teach other peers advocacy skills. Given the busy schedules of medical students and their sparse time for extracurriculars, it is reassuring that attendance at even just one HAINM event solidifies that HAINM is meeting its goals of providing students with the knowledge, skills, opportunities, and confidence to pursue health advocacy as budding physicians. In one such initiative, Belkowitz et al described a novel curriculum designed to (1) teach medical students about engaging in community needs assessments, (2) expose them to adjunct careers in health policy, and (3) assess their interest and skills in health advocacy. There was no significant difference in reports of interest between the intervention and control groups; however, reports of skill in community outreach, assessment, and engagement in healthcare policy improved in the curricular intervention. 14 The parallel success of other medical advocacy education initiatives underscores these findings in residency advocacy education, where participants did not receive any formal advocacy training in medical school. A study found that residents who completed the 3 week George Washington University (GWU) Residency Fellowship in Health Policy experienced marked increases in their self-reported knowledge of health policy, likelihood of teaching peers about health policy, and intention to pursue additional health policy education in the future. 15 HAINM uniquely demonstrates that healthcare advocacy training in the forms of both curriculum and community outreach can be quite effective early on in medical training, perhaps preparing medical students with the tools they need to actively engage in issues of advocacy throughout their entire careers.
Conclusion
The next steps to build on the pillars of advocacy, communication, and education are to develop pathways from learning to action. In addition to incorporation of advocacy into future career practice, we anticipate furthering long-lasting collaborative initiatives with community stakeholders to ensure the continuity of advocacy training for future healthcare, legal, and professional students. In addition, we will continue ongoing surveying methods to highlight the strengths of advocacy medical education, serving as a compass for creating ACGME-certified advocacy curriculum competencies in the future.
Supplemental Material
sj-docx-1-mde-10.1177_23821205251400427 - Supplemental material for Interdisciplinary Solidarity: Advancing Medical Student Education in Healthcare Advocacy
Supplemental material, sj-docx-1-mde-10.1177_23821205251400427 for Interdisciplinary Solidarity: Advancing Medical Student Education in Healthcare Advocacy by Natasha Dark, Luke Chao, Mia Lobitz, Luke Sanchez, Lauren Anderson, Hannah Herring, Ahmed Raihane and Amy Clithero-Eridon in Journal of Medical Education and Curricular Development
Supplemental Material
sj-pdf-3-mde-10.1177_23821205251400427 - Supplemental material for Interdisciplinary Solidarity: Advancing Medical Student Education in Healthcare Advocacy
Supplemental material, sj-pdf-3-mde-10.1177_23821205251400427 for Interdisciplinary Solidarity: Advancing Medical Student Education in Healthcare Advocacy by Natasha Dark, Luke Chao, Mia Lobitz, Luke Sanchez, Lauren Anderson, Hannah Herring, Ahmed Raihane and Amy Clithero-Eridon in Journal of Medical Education and Curricular Development
Footnotes
Ethical Considerations
Ethical approval was not required.
Consent to Participate
Consent to participate in this surveying technique as described in our methodology was obtained by each participant via written consent signature. The consent form was validated by our institution's IRB (25-232).
Consent for Publication
Informed consent for publication was provided by the participant(s) or a legally authorized representative.
Author Contribution
ND was involved in conceptualization, data curation, formal analysis, investigation, methodology, project administration, resources, writing—original draft, and writing—review & editing; LC and LS in conceptualization, methodology, project administration, resources, and writing—review & editing; ML in methodology, project administration, resources, writing—original draft, and writing—review & editing; AR, HH, and LA in writing—original draft and Writing—review & editing; and AC-E in supervision and funding acquisition. All the authors have read and approved this manuscript. The requirements for authorship have been met, and each author believes that the manuscript represents their honest work.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Center for Advancing Translational Sciences (grant number UL1TR001449).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
