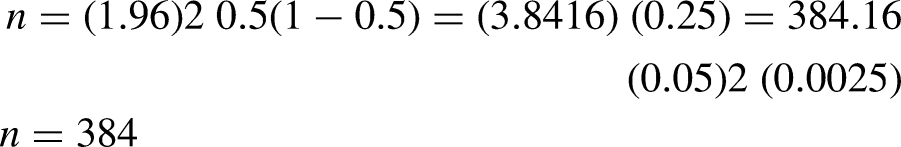Abstract
Background
Continuous Professional Development (CPD) programs are crucial for enhancing the quality of healthcare delivery. The presence of incompetent and unskilled healthcare professionals is not satisfactory. This study aimed to evaluate nurses’ engagement in CPD programs and identify the barriers affecting this engagement.
Methods
A mixed-methods approach, combining quantitative and qualitative cross-sectional studies, was employed from April 1 to 30, 2022. The quantitative component involved 271 randomly selected nurses, while nine key informants were purposively chosen for qualitative analysis. Data were collected using a structured self-administered questionnaire with a content validity index of 0.91 and an interview guide. Ethical guidelines were strictly followed. Quantitative data were entered into Epi-data version 3.1 and analyzed with SPSS version 25.0. Descriptive statistics described participant characteristics, while chi-square tests and logistic regression analyses assessed the relationships between independent and outcome variables, with significance set at p < 0.05 and goodness-of-fit evaluated by the Hosmer–Lemeshow test (>0.05). Qualitative data were analyzed using manual exploratory descriptive methods and thematic analysis.
Results
Of the 271 nurses, 262 (96.7%) participated, with a median age of 28 years. The overall CPD engagement rate was 34.4%. Factors influencing CPD engagement included financial constraints (adjusted odds ratio [AOR] = 3.1, 95% CI: 1.28–7.52), lack of access to CPD information (AOR = 0.3, 95% CI: 0.12–0.76), time constraints due to family commitments (AOR = 3.35, 95% CI: 1.08–10.34), and insufficient CPD resources (AOR = 0.15, 95% CI: 0.03–0.742). Qualitative findings revealed low CPD engagement levels, insufficient financial support, reluctance to self-finance training, the positive impact of diverse training mediums, and barriers related to nurses’ attitudes and the availability of training.
Conclusion
Nurses’ engagement in CPD is notably low. Financial and time constraints, along with limited access to information and resources, significantly hinder participation in CPD activities.
Introduction
Background
Continuing Professional Development (CPD) in nursing is defined as a lifelong process involving active participation in learning activities that help develop and maintain competencies, enhance professional practice, and support career goals (Hakvoort et al. 2022). Continuous Professional Development is crucial for verifying that healthcare workers can deliver safe, effective, timely, and patient-centered care in increasingly complex healthcare environments (Nsemo et al. 2013; World Health Organization, 2013).
Ensuring high-quality healthcare is a global priority, with patient safety being paramount for providing excellent health services (Nwogbe and Haliso, 2020; World Health Organization, 2017). To maintain quality healthcare services, meet patient satisfaction, and address societal needs, the healthcare system must adapt to ongoing challenges (Onyango, 2013). Nurses, being at the forefront of healthcare delivery, must engage in CPD to ensure the quality of care (Ingwu et al., 2019). Engagement in work was found to be influenced by a strong sense of coherence and the use of approach coping strategies (Van der Colff & Rothmann, 2009).
In Africa, CPD engagement among nurses is notably low (Mosol et al., 2017), and inadequate participation in CPD contributes to substandard healthcare, especially in developing countries (Nwogbe and Haliso, 2020). Basic nursing education alone is insufficient to address the complex demands of modern healthcare.
Governments are responsible for safeguarding public health through high-quality healthcare systems (Arinze-Onyia et al. 2018). Although the Federal Ministry of Health of Ethiopia is in the early stages of implementing a mandatory CPD system, where healthcare providers must earn Continuing Education Units annually for license renewal, there is limited information about nurses’ engagement in CPD activities in Ethiopia. This study aims to evaluate nurses’ engagement in CPD programs and identify barriers to their participation.
Review of Literature
Importance of CPD for Healthcare Systems
Continuing Professional Development is essential for improving healthcare quality by enhancing nurses’ knowledge and skills, which leads to better patient outcomes. It directly impacts nurses’ career satisfaction, promoting retention and recruitment, while ensuring sustained professional competence beyond initial education (Chong et al., 2014; World Health Organization, 2013). Continuous Professional Development fosters accountability and up-to-date care, recognized by governing bodies and healthcare organizations. Additionally, it improves nurses’ knowledge, ethical attitudes, and interpersonal skills, contributing to better patient care and elevating the status of the nursing profession (Sharma Pant & Poudel Panthi, 2018).
Modes of CPD Delivery
Continuous Professional Development can be categorized into three main types: statutory training, which is required for legal compliance (e.g., health and safety); mandatory training, which is essential for specific job roles (e.g., hand hygiene); and developmental training, which can be formal or informal and supports individual or workforce growth. Learning formats for CPD include traditional classroom-based sessions, workshops, and seminars, as well as online learning (e-learning), which offers flexibility through webinars, online courses, and recorded lectures, though it requires internet access (Giri et al., 2012; Gitonga & Muriuki, 2014; Ross et al., 2013).
Engagement of Nurses in CPD Programs
Nurses must remain competent and adapt to advancements in healthcare, and CPD plays a vital role in helping them meet these evolving demands while contributing to evidence-based practice. By fostering lifelong learning, CPD enables nurses to continuously enhance their skills and deliver safe, patient-centered care (Chong et al., 2014; Giri et al., 2012).
Barriers to CPD Participation
Barriers to CPD participation include various challenges such as lack of time, funding, staff shortages, and heavy workloads, which hinder nurses from engaging in professional development. Organizational barriers such as the absence of CPD policies, guidelines, and coordination, along with personal barriers such as time constraints, family commitments, and financial concerns, also limit participation. To address these issues, recommended solutions include hiring more nurses, developing clear CPD policies, and providing both financial and organizational support to facilitate CPD activities (Katsikitis et al., 2013; Pillay, 2017).
Objectives
General
To investigate engagement in continuing professional development programs and its barriers among nurses in a selected health care setting of Addis Ababa, Ethiopia.
Specific
To determine the level of nurse's engagement in continuing professional development programs
To identify barriers which impact nurses’ engagement in continuing professional development programs
To explore nurses’ perception toward engagement in continuing professional development programs.
Method and Material
Study Area, Study Design, and Period
An institution-based mixed approach cross-sectional study was conducted in Addis Ababa, the capital city of Ethiopia, and the headquarters of the United Nations Economic Commission for Africa (Abnet, 2022).
The study was conducted in the two CPD training accredited hospitals: Minilik II and St. Peter Specialized Hospital hospitals; from April 1 to April 30, 2022.
Study Population, Recruitment Procedure, and Sample Size
All nurses working in the two randomly selected hospitals were included for the quantitative section, and nine key informants from: the Ethiopian Nursing Association, nursing director of St. Peters specialized hospital and Minilik II hospital, nongovernmental organization (NGO) like the Ethiopian nursing association, Ministry of Health, Addis Ababa Regional Health Bureau were included in the in-depth interview. To recruit the study participants for the quantitative study, we first proportionally allocated the calculated sample size to the two randomly selected hospitals based on the total population of nurses working in the hospitals. Then, list of nurses was obtained from the nursing director's office, and simple random sampling method was used to enroll 271 participants. Newly employed nurses with experience of three months or less were excluded. Nine key informants were purposively recruited and interviewed in the qualitative study.
Sampling and Sample Size
The sample size was determined based on single population proportion formula, considering prevalence of 0.5 since no similar study was found in the study area (Moore, McCabe, & Craig, 2012):
Data Collection Instruments and Process
A standardized pretested self-administered data collection instrument was used to gather information from participants for the quantitative study. The self-administered data collection instrument for the quantitative study was adapted from similar studies conducted elsewhere (Davids 2007; Onyango, 2013; Owaka, 2014), while an in-depth interview guide for the qualitative study was developed from literatures conducted elsewhere (Mnguni, 2018). The instrument was evaluated for content validity by experts. Content validity was done among seven experts with content validity index of 0.91 to check its ability to test the question in study. The content validity indexes were done among seven experts; the result was 0.91. The instrument was pretested among 14 (5%) nurses at Yekatit 12 Hospital. Two data collectors were recruited and trained on the purpose, goals, and significance of the study, data collection strategies, and interviewing techniques. The quantitative instrument constituted questions about sociodemographic characteristics of nurses, Nurses level of understanding on CPD concept, and nurses’ engagement on CPD activities. However, the qualitative section focused on the barriers for engagement on CPD. The data collection process was carried out by trained nurses. The questionnaire included all relevant variables to meet the objective of the study. Each questionnaire was checked for completeness by the assigned supervisor and primary investigator on daily basis.
The qualitative data were gathered through face-to-face in-depth interviews using semistructured open-ended and probing questions interview guide. To ensure the validity of the interview guide, it underwent a critical review process by two experts in the field. To ensure the reliability and trustworthiness of the data, interviews were guided by interview questions based on a comprehensive literature review, and field notes were made during the interview. Two independent researchers analyzed the data and verbal and nonverbal data were recorded and interpreted. Besides, quotations were also presented to elaborate each theme and subtheme, and an external expert. Inconsistencies were resolved through discussions.
Operational Definition
Continuous Professional Development engagement was measured when nurses engaged in both formal and informal teaching and learning activities, which involves interactive learning or training activities such as in-service training, short refresher courses, coaching of trainees, conferences, seminars and workshops and general reading, or informal CPD activities which are less structured educational program activities within the past 12 months of this study.
Data Processing and Analysis
Data were cleaned and entered into Epi-data version 3.1 and analyzed using SPSS version 25.0. Cross-tabulation was done in order to determine the sample characteristics. Descriptive statistics were used to describe characteristics and displayed using tables, figures, and text. Logistic regression analysis was used to examine the factors associated with independent and outcome variables. All variables with p < 0.25 in bivariable regression analysis were included into the multivariable regression model for analysis. Goodness-of-fit was checked by the Hosmer–Lemeshow test (>0.05). Finally, statistical significance was declared at p < 0.05.
The qualitative data used a thematic analysis following verbatim transcription of audio records, transcribed and translated from the local language “Amharic to English,” then the data Coded and categorized, themes were generated, and four themes and subthemes were emerged.
Qualitative Approach
Study Design
This study employed a qualitative, exploratory, and descriptive approach to delve into nurses’ engagement in CPD activities and to identify barriers that impede this involvement.
Sampling Technique
The study included nine purposively selected key informants who possessed nursing backgrounds and held leadership roles within the Ethiopian Nursing Association, nursing directors from St. Peter's Specialized Hospital, Menelik II Hospital, various NGOs, the Ministry of Health, and the Addis Ababa Regional Health Bureau. The ages of the key informants ranged from 29 to 42 years, and the sample size was established based on the principle of data saturation.
Inclusion Criteria
Nurses in leadership positions with relevant responsibilities related to CPD in the selected study settings were eligible to participate.
Data Collection Tools and Procedure
The principal investigator, a female MSc candidate in Adult Health Nursing with previous data collection experience, conducted face-to-face in-depth interviews. To mitigate any potential bias, only she conducted the interviews. The interview guide was pilot-tested with head nurses to ensure clarity and relevance. Key informants were briefed on the study's objectives and scope prior to the interviews. The questions focused on participants’ perspectives on nurses’ engagement in CPD, the educational programs available, barriers to participation, and recommendations for enhancing CPD implementation. Verbal consent was obtained before the interviews, which lasted approximately 20–25 min, were conducted in the participants’ offices for their convenience. The data collection process involved audio recording and taking field notes during the interviews. The recorded data were manually transcribed verbatim, translated, and coded by the principal investigator, resulting in four emerging themes.
Results
Quantitative Findings
Sociodemographic Characteristics of Participants in Addis Ababa Selected Hospitals
A total of 271 nurses with a response rate of (262) 96.7% were included in the study. Of the total participants, 168 (64.1%) were aged between 20 and 29 years old, with median age of 28 years old (IQ at 25 to IQ at 75). More than half 147 (56.1%) were males. One hundred thirty-six (51.9%) of participants were unmarried. One hundred eight (41.2%) of participants were reported to have earned monthly income between 4610 and 6192 ETB, with a mean of 6871.03 ETB and a median of 7035.50 ETB. One hundred thirty-one (50.0%) of participants had experience of 5–10 years with a mean year of 5.64 and +3.81 SD. Two hundred thirteen (81.3%) of participants had a bachelor of degree, and 214 (81.7%) were a comprehensive nursing (Table 1).
Sociodemographic Characteristics of Nurses at Addis Ababa Selected Public Hospital, Addis Ababa, Ethiopia (n = 262).

ETB: Ethiopian Birr.
Nurses Engagement in CPD
Ninety (34.35%) among the 262 participants reported they ever participated in CPD training, of which 47 (52.3%) received the training in past one month, 21 (23.3%) one to two years ago, 13 (14.4%), in the past one to six months. Concerning their reason for participation in the training, 22 (24.4%) said to advance their qualification, 19 (21.1%) to renew their license. About half 132 (50.4%) participants reported the work in a hospital offering in-service training for nurses (Table 2).
Nurses Engagement in Continuous Professional Development in Addis Ababa Selected Public Hospital, Addis Ababa, Ethiopia (n = 262).

Significant at p < 0.05.
Engagement of CPD among Nurses
Of the total participants, 172 (65.6%) were not engaged in at least one CPD through their career while, 90 (34.4%) were participated on CPD activities (Figure 1).

Engagement of nurses on CPD at Addis Ababa Selected Public Hospitals, Addis Ababa, Ethiopia. (n = 262). CPD: Continuing Professional Development.
Figure 1 shows 34.35% of nurses working in public hospitals in Addis Ababa ever participated in CPD programs.
Nurses Reason for Decrease in CPD Engagement
Factors affecting engagement of nurses on CPD: Lack of interest was 30.5%, lack of time due to heavy workload 37.8%, staff shortage 22.5%, lack of finance were 45.4%,failure of administration to organize off duty 42.4%, lack of information on available CPD sessions was 17.9%, lack of time due to family commitments 19.8%, lack of role models at work was 40.5%, unavailability of interesting CPD activities 14.5%, lack of encouragement 16.4%, irrelevant topic selection 11.8%, and lack of CPD activities 21.4% (Table 3).
Nurses Reasons for Decreased CPD Engagement into Addis Ababa Selected Public Hospital, Addis Ababa, Ethiopia (n = 262).

CPD: Continuing Professional Development. Significant at p < 0.05.
Factors Associated with CPD Engagement
In order to identify the extent of factors affecting the engagement of nurses on CPD, a binary logistic regression model was used. Variables that had a p-value <0.25 on bivariate analysis; lack of interest, lack of time due to heavy workload, lack of finance, failure of administration to organize off duty, lack of information on available CPD sessions, lack of time due to family commitments, lack of role models at work, lack of encouragement, and lack of CPD resources, had checked. In the multivariable logistic regression, only lack of finance, lack of information on available CPD sessions, lack of time due to family commitments, and lack of CPD resources remained statistically significant with engagement on CPD.
The odds of engaged nurses on CPD were 3 [adjusted odds ratio, AOR = 3.10, 95% CI (1.28–7.52)] times higher among nurses on lack of finance compared to those who had not. In addition, nurses with lack of information on available CPD sessions were 0.3 [AOR = 0.30, 95% CI (0.12–0.76)] times higher odds of having engaged on CPD than those counterparts. Moreover, nurses on lack of time due to family commitments were 3.3 [AOR = 3.35, 95% CI (1.08–10.34)] times more likely engaged on CPD compared to those nurses who had not. The odds of engaged nurses on CPD were 0.15 [AOR = 0.15, 95% CI (0.03–0.742)] times higher among nurses on lack of CPD resources activities compared to those who had not (Table 4).
Bivariable and Multivariable Logistic Regression on Factors Affecting the Engagement of Nurses on CPD at Addis Ababa Selected Public Hospital, Addis Ababa, Ethiopia (n = 262).

AOR: adjusted odds ratio; COR: crude odds ratio; CI: confidence interval; CPD: Continuing Professional Development.
* p-value significant at <0.05.
Qualitative Findings
Sociodemographic Characteristics of Participants
A total of nine key informants with mean age of 36.55 ± 1.96 SD ranging from 29 to 42 years were interviewed. Seven of the key informants were Masters of Science degree holders, and two were Doctoral degree holders. The key informants were intentionally chosen, assuming they could provide valuable information due to the connection between their work and the topic. Regarding their recruitment sector, two were from Ministry of Health, two from Addis Ababa Regional Health Bureau, two from NGO, two from hospital nursing directors, and one from Ethiopian Nursing Association.
The key informants were questioned regarding their perspectives on the significance of CPD for nurses, the current level of nurses’ participation in CPD within the country, the enforcement of CPD initiatives, and the obstacles to effective implementation. Audio-recorded data were, transcribed, translated condensed, and coded. Unit meanings were categorized under sub units and four themes, including low levels of CPD engagement of nurses, lack of financial support and nurse's willingness to pay for own training, medium of training improved CPD engagement, and nurses’ Attitude and training availability as barriers to CPD engagement with subclasses were emerged,
Theme I: Low levels of CPD engagement of nurses: Participants expressed that nurses’ engagement is very low especially before the commencement of mandatory CPD programs. PA1: e…m “compared to the number of nurses and the dispersion of the health personnel throughout the country, their participation, and engagement was very minimal….” PA 2: “…Before the implementation of mandatory CPD, it seemed as if it would not be implemented at all, but now there are improvements though it is not enough….” PA 8: It was a big opportunity for all our staff to work in an institution with accredited CPD training center. Continuous trainings are carried out in our institution and nurses are benefited, but still way behind…”
Incentive Motivated CPD Engagement
Participants perceived that nurses were eagerly participating in in-service training previously because they were earning incentives, but now, the scenario has been changed and they engaging on CPD programs for renewal of their working license, hence they are required to pay for trainings. PA5: “…Previously nurses were involved in training only to get the incentives but, currently the health professionals start engaging in training which does not have an incentive for them. Especially when we see the data we get from ENA, there is a big difference in the engagement of nurses after the commencement of mandatory CPD….” PA6: “…. Previously nurses were not happy when the training was prepared in Addis Ababa by just considering the amount of money they earn. They were only interested when the training was prepared outside Addis Ababa as they would get more incentive. But after the implementation of the CPD program, nurses started asking the nursing directorate to facilitate training for them. They start using the training to renew their license and to update their knowledge….”
Themes II: Lack of financial support and nurse's willingness to pay for own training
Participants’ expressed that, nurses believe and willingness to pay for CPD training services rendered to them shall be covered by institutions, and not by them. Participant from the regional health bureau stated it as:
PA 4: “…. Health professionals were not willing to pay for their own training…”
Another participant from Ethiopian nursing association stated:
PA5: “…. Currently paid training is expensive for most health professionals….”
Some of the participants mentioned that lack of financial support is the main challenge to provide training at the cost of their institution.
PA6: “…. There is no financial support from any other partner organization….”
Some participants mentioned that a limited organization was providing support.
PA 8: “…. There is no financial or technical support from any organizations except the ENA….”
Minimal Partner Collaboration to Solve Financial Challenges
To solve this financial problem, some of the institutions are working with different supporting partners. PA 8: “…. To solve this problem, currently we are working in collaboration with ENA and give the opportunity for the nurses to get online training and certification from there….”
Themes III: Medium of training improved CPD engagement: The participants stated that access and reachability of CPD program was a challenge that hinder nurses’ engagement in training programs. The use of different medium of training mechanisms recently introduced has improved nurses’ engagement on CPD activities. PA7: “…Currently, electronic software applications funded by partner organization WACA are available for training through mobile telephone. we are providing online training for almost all health professionals and mainly for nurses. According to our data, more than 1000 individuals are using the application every month, and since the beginning approximately 60,000 individuals were registered, and about 20,000 nurses successfully completed the training and collected their certificate online. The cost of face to face training is also subsidized for members of Ethiopian Nursing Association ….”
“emm…. We are also in provision of on-site training for nurses by traveling to their own working area….”
PA2: “…. CPD is provided in two ways; one as a category 1: face to face training and online training is incorporated on which certificate is provided after the completion of the training. The other category 2: a day to day activity of the health professional in his working setup which can maintain & develop the knowledge of them continuously. Because category 2 has no certification, most health professionals don’t consider it as a CPD activity. However, currently MoH is focusing on category 2 as implementation guideline….”
Another participant similarly emphasized on lack of awareness of the nurses toward other CPD training modalities apart from face to face and online training, stating: PA5: “…. Most health professionals only think about the modality of face-to-face training and online training. They are not familiar with other kinds of CPD activities like engagement on research work, participation in conferences, seminars, and meetings….”
Another participant (Nursing director from one of the study hospitals) stated that in-service training facilitated by employer institutions is other options. The participant mentioned that; PA8: “…. We have a CPD facilitating committee under the Nursing directorate which is called Capacity building Committee. So, this committee works on the capacity building through different mechanisms: Formal training, peer training on case team, nursing round, grand nursing round which we started recently and with collaboration with ENA, provide online training….”
Themes IV: Nurses’ Attitude and training availability as CPD barriers Engagement:
Study some participants perceived that: nurses’ attitude toward CPD engagement and limited number of trainings available were the main barriers. PA6: “…Attitude of the nurses is the challenging problem. Everyone dislike it to be regulated as it is intended, rather, they just want to be free as it was in the previous days. They were unhappy to engage in the training, unless the enforcement was in place….” PA9: “…. There was a very big misunderstanding of the nurses. Previously health professionals don’t think CPD is important for their carrier as well as their clients, thus they don’t want to engage in trainings. Despite its mandatories, several nurses are unhappy and complaining about it….” PA1: “…Access to accredited CPD training centers, shortage of trained personnel who can train nurses are challenges to nurses CPD engagement, I believe. To date, there are only 115 CPD providers, and 35 accredited CPD centers all over the country. Further, most of the CPD centers are found in and nearby the capital city, and the number of trainers is unproportionate to the total number of nurses in the country. ….”
Another participant stated lack of infrastructure like access to internet service is also major problem hindering nurses CPD engagement. The participant stated this as: PA2: “…. Access of infrastructures required to provide CPD, like internet is one among the main barriers, especially to those nurses residing outside Addis Ababa. CPD providers’ coverage all over the country, and weak initiation of CPD providers halt nurses to engage to the expected level….”
Participants again stated, topic selection, and absence of ownership of CPD programs impeding nurses CPD engagement. PA7: “…. CPD programs were uncontrolled, disorganized, without ownership and nurses engage in trainings just for the sake of certification even if the topic is not related with their scope of practice….”
Discussion
Continuous Professional Development programs are designed to ensure the competence of healthcare workers (Hakvoort et al. 2022; Nsemo et al. 2013; World Health Organization, 2013). Globally, the quality of healthcare is a major concern, with evidence showing that unsafe and poor-quality care can lead to significant morbidity and mortality. Continuous education is crucial for addressing many safety-related health concerns. Continuous Professional Development is widely used to enhance professional competence and ensure best practices (Badu-Nyarko, 2015; Nsemo et al. 2013; Nwogbe and Haliso, 2020). This study aimed to assess nurses’ engagement in CPD programs and identify barriers to their participation.
The study found that 34.35% of nurses reported participating in CPD activities. This figure is similar to a study in eastern Ethiopia, where 32.97% of participants engaged in CPD, and a study in Lagos, Nigeria (Nwogbe and Haliso, 2020; Yadeta et al., 2024). However, a Kenyan study reported a higher engagement rate of 63.6% a decade ago, though recent engagement has significantly declined (Onyango, 2013). In contrast, studies in Nigeria and Malaysia have reported higher CPD engagement rates among nurses (Chong et al., 2014; Nsemo et al. 2013). A study by Yadeta et al. also highlighted a strong perception regarding the need for CPD among nurses (Adane & Asgedom, 2024; Yadeta et al., 2024). Variations in findings may be due to differences in policies and guidelines across institutions.
In-depth interviews revealed that nurses exhibit low CPD engagement, particularly before mandatory programs, primarily because they believe institutions should cover training costs, leading to reluctance to self-finance. The introduction of various training mediums has improved accessibility and participation, although negative attitudes and limited training availability continue to hinder effective CPD engagement. This aligns with findings from a meta-analysis conducted at Stockholm University (Beckett, 2020; Mlambo, Silén & McGrath, 2021).
Factors negatively impacting CPD engagement include financial constraints, lack of information about available trainings, time constraints related to family commitments, and insufficient resources. In our study, 54.5% of participants cited financial constraints as a major reason for not engaging in CPD, a finding supported by key informants who noted a lack of financial support, reluctance to pay for training, and the absence of supporting organizations. These findings are consistent with studies from South Africa, India, and Western Kenya, where financial difficulties were reported as barriers to CPD engagement (Baloyi and Jarvis, 2020; Pillay, 2017; Macaden et al. 2017; Mosol, 2017). This finding was further supported by a study conducted in the Casablanca-Settat Region of Morocco in 2021, which identified work overload, organizational challenges, unsuitable schedules, unmet needs of nursing staff, and the absence of supportive measures as barriers to CPD engagement (Lhbibani et al., 2021).
Lack of information about CPD sessions was positively associated with engagement (p < 0.011), with 82.1% of participants acknowledging this issue, aligning with findings from South Africa (Maggie Nyelisani & Luhalima 2023). Time constraints related to family commitments also emerged as a barrier, consistent with studies from Nigeria (Cecilia, 2022; Pillay, 2017). However, the availability of online options has provided more time-convenient opportunities for CPD. A qualitative study among perioperative nurses in Ethiopia revealed that limited access to ongoing in-service perioperative training and problematic staffing policies hindered nurses’ ability to fully utilize and share the knowledge gained from CPD training (Abebe, Bender & Pittini, 2018). However, this was not the case in our study.
The study found a significant relationship between nurses’ professional level and CPD engagement, consistent with a study in Iran (Khademi et al. 2021), though it differed from findings in Kenya (Onyango, 2013). This discrepancy may be due to variations in sample sizes. Additionally, formal education was the primary method used by more than half of the participants to advance their professional standards, aligning with a study in India where 66% of nurses attended courses for further education (Das et al. 2019).
Key informants also noted that nurses often resist regulated practices, a finding not supported by a study in India (Uba 2019). The difference may be attributed to varying levels of understanding of CPD benefits and institutional efforts to encourage participation.
Limitation
The limitations of this study include limited similar studies were found during literature review in the area. Secondly, this is an institutional study included only two public hospitals, but not health centers, and private health care institutions. These limitations may lead to drawbacks to draw conclusions beyond the studied settings.
Conclusion
This study found that nurses’ engagement in CPD activities is low. Financial constraint, lack of information on Professional Development sessions, time constraint related to family commitments and Lack of CPD resource hindered nurse's engagement CPD. Continued enforcement, regulation, and support of CPD programs, as well as proper selection of sensitive training topics may be advocated to improve engagement in the program.
Implication for Practice
Continuing professional development in nursing is essential for maintaining up-to-date knowledge, enhancing clinical skills, and improving patient outcomes. It enables nurses to meet regulatory requirements, stay competent in evolving healthcare systems, and pursue advanced roles or specialization. Continuous Professional Development also fosters professional growth by supporting career progression, leadership development, and improved interdisciplinary collaboration. Ultimately, CPD ensures that nurses provide safe, effective, and culturally competent care, while remaining accountable to professional and ethical standards.
Supplemental Material
sj-docx-1-son-10.1177_23779608241307447 - Supplemental material for Nurses Engagement on Continuing Professional Development Programs and its Barriers in Selected Hospitals in Addis Ababa, Ethiopia
Supplemental material, sj-docx-1-son-10.1177_23779608241307447 for Nurses Engagement on Continuing Professional Development Programs and its Barriers in Selected Hospitals in Addis Ababa, Ethiopia by Meaza Wehabe, Tigistu Gebreyohannis Gebretensaye and Ketema Bizuwork in SAGE Open Nursing
Supplemental Material
sj-docx-2-son-10.1177_23779608241307447 - Supplemental material for Nurses Engagement on Continuing Professional Development Programs and its Barriers in Selected Hospitals in Addis Ababa, Ethiopia
Supplemental material, sj-docx-2-son-10.1177_23779608241307447 for Nurses Engagement on Continuing Professional Development Programs and its Barriers in Selected Hospitals in Addis Ababa, Ethiopia by Meaza Wehabe, Tigistu Gebreyohannis Gebretensaye and Ketema Bizuwork in SAGE Open Nursing
Footnotes
Acknowledgment
The authors acknowledge the study participants for their participation in the existing of this study. Additionally, the authors thank The Addis Ababa university College of Health Sciences, School of Nursing and Midwifery, Ministry of Health and study institutions for the providing of necessary computational facilities.
Authors’ Contributions
MW, TG, and TB conceived the idea and prepared the proposal. All were involved in the data collection, analysis, and write-up of the research findings. TG prepared the final draft of the manuscript. All authors subsequently reviewed, read and approved the final draft of the manuscript.
Availability of Data and Materials
The datasets generated and/or analyzed in the current study are available with the corresponding author on reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Consideration
Ethical approval Ref: No SNM/008/018/2022 was obtained from Addis Ababa University, College of Health Science, School of Nursing and Midwifery Institutional Review Committee. Study objective, benefits, and potential discomforts were discussed, and written consent was obtained. Respondents’ information was kept confidential and is not used for other purposes other than the study purpose.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.