Abstract
Background
The prevalence and determinants of antenatal care (ANC) dropout in Ethiopia were studied. However, the results were inconsistent and showed considerable variation. Hence, this meta-analysis aimed at estimating the overall prevalence of ANC dropout and its predictors in Ethiopia.
Methods
A comprehensive search of published studies was done using different international databases such as such as PubMed, DOJA, Embase, Cochrane Library, Google Scholar, and the institutional repository of Ethiopian universities were used to search for relevant studies. Data were extracted using Microsoft Excel spreadsheet, and exported to STATA v17 for analysis. A random effect model was used to estimate the overall national prevalence of ANC dropout. Fixed effects model were used to compute the pooled adjusted odd ratios (AOR) with the corresponding 95% confidence intervals (CIs). I2 test was used to assess heterogeneity of the included studies. Egger's tests was used to check for the presence of publication bias.
Results
A total of 7 studies were included in this systematic review and meta-analysis with 11,839 study participants. The overall pooled prevalence of ANC in Ethiopia was found to be 41.37% (95% CI =35.04, 47.70). Distance from the health care facility (AOR = 2.93, 95% CI = 2.75, 3.11), pregnancy complication signs (AOR = 2.97, 95% CI = 2.77, 3.16), place of residence (AOR = 1.79, 95% CI = 1.31, 2.26), educational level (AOR = 1.79, 95%CI = 1.37, 2.21), and age group (30-49) (AOR = 0.61, 95% CI = 0.45, 0.78) were significantly associated with ANC dropout.
Conclusion
Based on this review and meta-analysis, 41% of Ethiopian women dropped out of ANC visits before the minimum recommended visit (4 times). Hence, to reduce the number of ANC dropouts, it is important to counsel and educate women during their first prenatal care. Issues of urban–rural disparities and noted hotspot areas for ANC dropout should be given further attention.
Introduction
Antenatal care (ANC) is the care provided for a pregnant woman that can play a great role in the improvement of health of the women in getting ready for labor and in recognizing the warning signs of pregnancy and childbirth. Dropping out of ANC is defined as ceasing to receive the service before at least 4 ANC visits. 1 ANC is one of the approaches to reduce newborn mortality and maintain maternal health by guiding women to access more maternal health services and prepare for their newborns. 2
In 2017, around 810 women died every day from preventable causes related to pregnancy and childbirth. 94% of all maternal deaths occur in low- and lower-middle-income countries. Despite an apparent global improvement, between 2000 and 2017 maternal mortality dropped by about 38%. 3
In 2016, at the beginning of the Sustainable Development Goals (SDGs) era, pregnancy-related morbidity and mortality rates remain unacceptably high. While substantial progress has been made, countries need to consolidate and increase these advances, and to expand their agendas to go beyond survival, with a view to maximizing the health and potential of their populations. The SDGs target a global maternal mortality ratio not greater than 70 maternal deaths per 100,000 live births by 2030. 4
Women in low-resource setting countries including Ethiopia were prone to high rates of maternity care dropout as well as other maternal continuum of care issues. 5 In Ethiopia, only 32% of women had 4 or more ANC visits and 64% of women had at least 1 ANC visit, while about 32% of women did not receive ANC at all throughout the duration of their pregnancy. 6
ANC visit dropout was high in low-income countries. The sub-Saharan region was one of the African regions with a high dropout rate from ANC. In the region, about 30% of pregnant women among all births in the region did not use the services. 7
Although maternal health care utilization, including ANC has improved in Ethiopia, the majority of women do not attend the minimum recommended number of ANC visits required. 8 Low health care utilization is caused by a variety of factors, but it is clear that poor quality of services and poor treatment by providers are among the reasons why many women do not access newborn and maternal health care services. 9
In Ethiopia, different studies were conducted on the prevalence of ANC dropout and lie between 33.39% 10 and 56.49%. 11 Different factors affect the dropout of ANC services utilization were being far distance, not developing a pregnancy danger sign, not satisfied with ANC service, having no formal education, employment status, marital status, didn’t inform about institutional delivery, place of residence, age group, current pregnancy planned/supported, and presence of professional advice during ANC visit.5,6,10–15
As Health Sector Transformation Plan 2 (HSTP 2) come to the end, which aimed to promote maternity care, with an emphasis on ANC to improve maternal and newborn health outcomes. 16 Therefore, it is important to assess the overall magnitude of ANC dropout and its determinant factors to produce evidence for decision making for planners and program evaluators. Even though there have been numerous studies conducted on the prevalence and determinant factors of ANC dropout in Ethiopia, the results have been inconsistent and varied.
Methods
This systematic review and meta-analysis were conducted according to the guidelines of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020. 17 The Population, Exposure of Interest, Outcome (PEO) technique from the 2017 JBI Guideline was used to define the inclusion and exclusion criteria. 18
Search Strategies
A comprehensive search of studies was conducted using distinct databases such as PubMed, DOJA, Embase, Science Direct, Cochrane Library, African Journals Online, Google Scholar, and Web of Science. In the beginning, studies were comprehensively searched using the full title (“The prevalence and associated factors of antenatal care service dropout in Ethiopia”) and keywords (“prevalence,” “magnitude,” “incomplete,” “discontinuation,” “antenatal care dropout,” “determinant factors,” “associated factors,” “predictors,” and “in Ethiopia”). Boolean operators “OR” or “AND” were used in combination or independently to connect these keywords and to establish the search terms. Besides, reference lists of all included studies were considered to find other missed studies. Additionally, institutional repository from Mekelle, Jima, Addis Ababa, and Bahir Dar Universities was used to search important literatures.
Criteria's of Eligibility
To establish the inclusion and exclusion criteria for this systematic review and meta-analysis, the authors used the PICO technique, which mainly involves Condition, Context, and Population (CoCoPop) questions for prevalence studies.
Inclusion Criteria
Study area: Studies conducted in Ethiopia.
Study setting: Studies conducted in rural or urban settings and at health institutions or community-based settings.
Study design: Cross-sectional, cohort, and case–control studies that reports either the proportion or prevalence or magnitude and associated or determinants factors or predictors of ANC dropout.
Studies with the outcome of interest published in English language for the sake of clarity, and simplicity of interpretations were included.
Time: No limitation was made for the time of publication and all studies conducted in Ethiopia were included.
Exclusion criteria
Qualitative studies that couldn’t provide a quantitative evidence for the pooled estimate and studies that have a different outcome of interest were excluded. Besides this, studies with different operational definitions and measurements of ANC services dropout were excluded from this systematic review and meta-analysis.
Data Extraction
Two authors (GS and TM) separately extracted the data from the included studies using a piloted data extraction Microsoft Excel spreadsheet. The spreadsheet includes the first author's name, publication year, study year, study design, study area, study setup, sample size, response rate, and the proportion of ANC dropout. When there was any discrepancy between the reviewers, the differences were resolved through discussion and reevaluation of each studies.
Quality Assessment of the Studies
Joanna Briggs Institute (JBI) Critical appraisal checklist was used to assess the methodological quality of the included studies.
19
The 2 authors individually ranked the quality of the included studies (GS and TM). There are 9 parameters in the tool and are as follows:
Was the sampling frame appropriate to address the target population? Were study participants sampled appropriately? Was the sample size adequate? Were the study subjects and the setting described in detail? Was the data analysis conducted with sufficient coverage of the identified sample? Were valid methods used for the identification of the condition? Was the condition measured in a standard, reliable way for all participants? Was there an appropriate statistical analysis? Was the response rate adequate, and if not, was the low response rate managed appropriately?
Each item was evaluated as either low or high risk of bias. A composite quality index was grouped and the risk of bias was ranked as low (0-2), moderate (3 or 4), or high. Articles with low and moderate risks of bias were considered for this systematic review and meta-analysis.
Measurement of the Outcome of Interest
The major outcome of this systematic review and meta-analysis was the proportion of pregnant women whose ANC services dropout in Ethiopia. The secondary outcome variable was determinant factors of ANC dropout, which were estimated using a pooled adjusted odds ratio (AOR) with 95% confidence intervals (CIs). ANC services dropout was considered when the pregnant mothers did not complete full recommended visits during their pregnancy (a minimum of 4 visits for normal pregnancy).10–13,15,20
Statistical Methods and Analysis
The extracted data from Microsoft Excel spreadsheet were imported to STATATM 16 statistical software for analysis. To begin, the Higgins I-squared statistic (I2) and the Cochran Q-test were used to assess the presence of statistical heterogeneity among the included studies. As a result, significant heterogeneity [I2 = 97.6%, P value .001] was found. Therefore, a random effects model using the DerSimonian–Laird method was used to estimate the pooled prevalence of ANC dropout. The AOR and 95% CIs were constructed from the included studies. The pooled AORs were computed using a fixed effect model.
Subgroup analyses and heterogeneity: To identify potential sources of heterogeneity between the included studies, subgroup analyses were conducted based on geographic regions and year the study was conducted.
Publication bias: The presence of publication bias was assessed using statistical methods such as Egger's and Begg's tests, and the results of Egger's regression test indicated that no publication bias between the included studies (P value > .05). A P value of .233 and .114 for Begg's and Egger's tests, respectively, implied that a small study effect was less likely.
Sensitivity analysis: To assess the effect of a single study on the overall prevalence of ANC dropout, sensitivity analysis was done using a random effects model.
Results
Search of studies through different international databases and the institutional repository of Ethiopian universities, a total of 265 published and unpublished studies were identified. The endnote reference manager was used to screen studies that were obtained and the duplicate studies were removed. Then, following the removal of 178 researches based on title and abstract screening, 19 complete papers were obtained. Finally, this study analysis contained 7 studies that met the inclusion criteria (Figure 1).
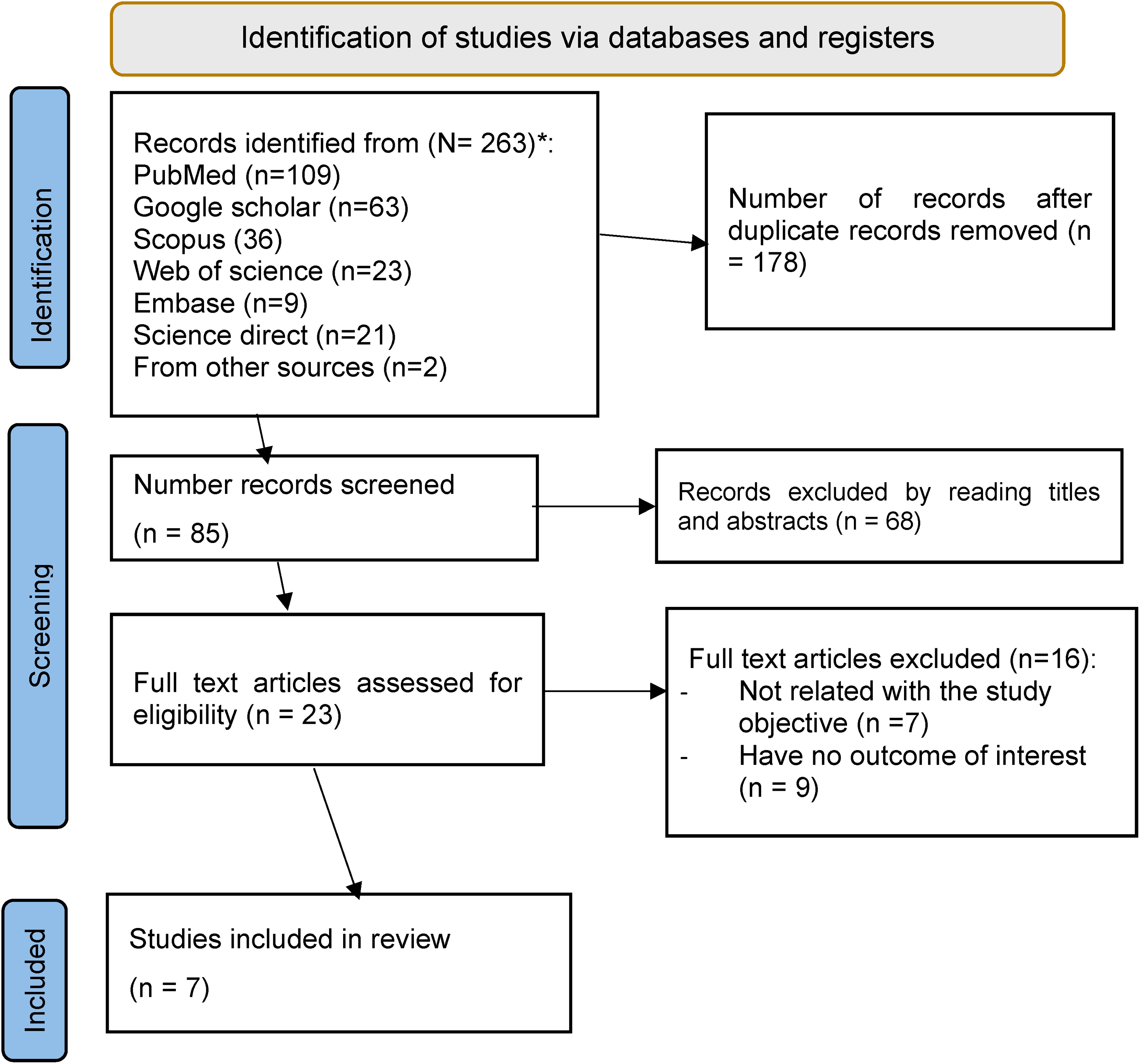
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 flow diagram describing the selection of studies for systematic review and meta-analysis.
Characteristics of Selected Studies
A total of 7 studies were included to assess the pooled prevalence of ANC service dropout and its associated factors in Ethiopia.10–15 A total of 11,839 pregnant women were considered in this meta-analysis. In each study, the methods of data collection were through face-to-face interview using a pretested, interviewer-administered questionnaire. The included study’s publication year ranged from 2020 to 2022. Two from Amhara,12,13 1 from Tigray, 10 and 1 from Oromia 15 regions and 3 of them were nationwide studies5,11,14 based on Ethiopian demographic and health survey data. All studies were cross-sectional studies and have a low risk of bias (Table 1).
Shows a Descriptive Summary of Studies Included in This Systematic Review and Meta-Analysis.

Abbreviations: CB, community based; CS, cross-sectional study; IB, institutional based.
The Pooled Prevalence of ANC Service Dropout
The overall pooled prevalence of ANC dropout in Ethiopia was found to be 41.37% (95% CI =35.04, 47.70) (Figure 2). The I2 test was computed to look at study heterogeneity, and the results showed that there was a substantial amount of variation between the studies (I2=97.6%, P value = .00). The pooled prevalence of ANC dropout was computed using a random effects model with the DerSimonian–Laird method.

Forest plot showing the pooled estimate of antenatal care (ANC) dropout in Ethiopia.
Subgroup Analysis
To identify the source of heterogeneity for the pooled prevalence of ANC dropout, subgroup analysis was conducted by place of region and year of the study conducted. The pooled prevalence of ANC dropout was significantly higher among studies conducted at national level (47.04%, 95% CI = 37.86, 56.22). However, the study conducted in Tigray region had the lowest prevalence of ANC service dropout 33.39% (95% CI = 29.45, 37.34) (Figure 3).

Subgroup analysis for the pooled prevalence of antenatal care (ANC) dropout by geographical regions of Ethiopia.
Additionally, we carried out a subgroup analysis according to the year the studies were done. As a result, the pooled prevalence of ANC dropout was higher for those studies conducted in 2019 and after (44.34%, 95% CI = 34.05, 54.65) when compared with those studies conducted before 2018 (37.35%, 95% CI = 28.60, 46.10) (Figure 4).
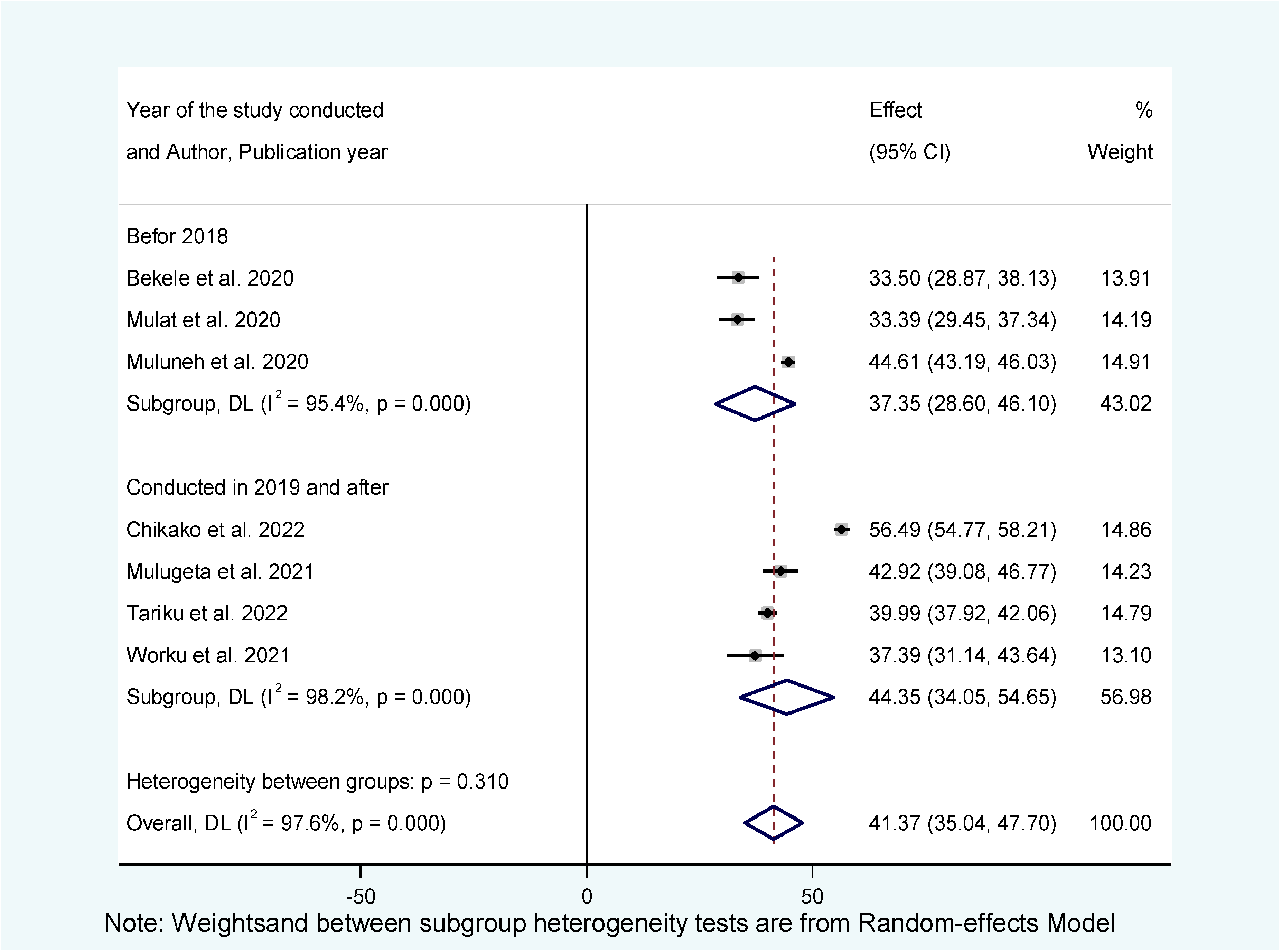
Subgroup analysis for the pooled prevalence of antenatal care (ANC) dropout by year of the study conducted in Ethiopia.
Small study effect: Using Egger's regression test, publication biases among the included studies were evaluated, and the results showed that there was no small study effects among the included studies as the nonstatistical significant result (P value = .114).
Sensitivity analysis: A sensitivity analysis with a random effects model was done to examine any outliers on the overall estimate of the pooled prevalence of ANC dropout and it showed that there was no single study influence (Figure 5).
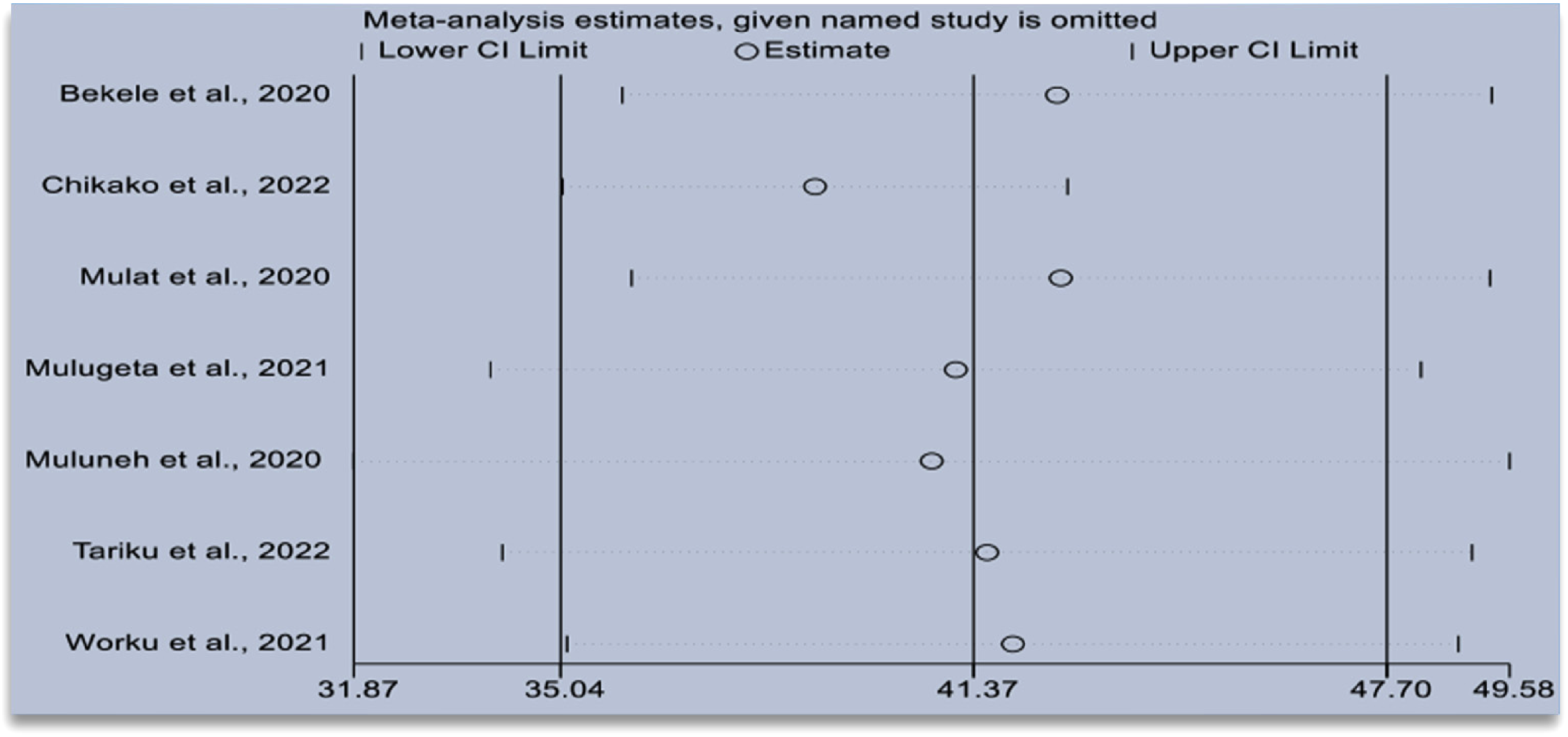
Result of sensitivity analysis of antenatal care (ANC) dropout in Ethiopia.
Determinants of ANC Service Dropout in Ethiopia
To identify significant determinant factors of ANC dropout, 21 variables were extracted from the included studies. Finally, 5 variables (distance from the health care facility, educational level, place of residence, pregnancy complication signs, and age group) were identified as significant determinants of ANC dropout.
The influence of distance from the health care facility on ANC dropout was assessed using the findings of 4 studies.10–13 In this meta-analysis, women who travel more than 1h to reach the health institution were 2.55 times more likely to have ANC dropout than their counterparts to [AOR = 2.93, 95% CI = 2.75, 3.11] (Figure 6).
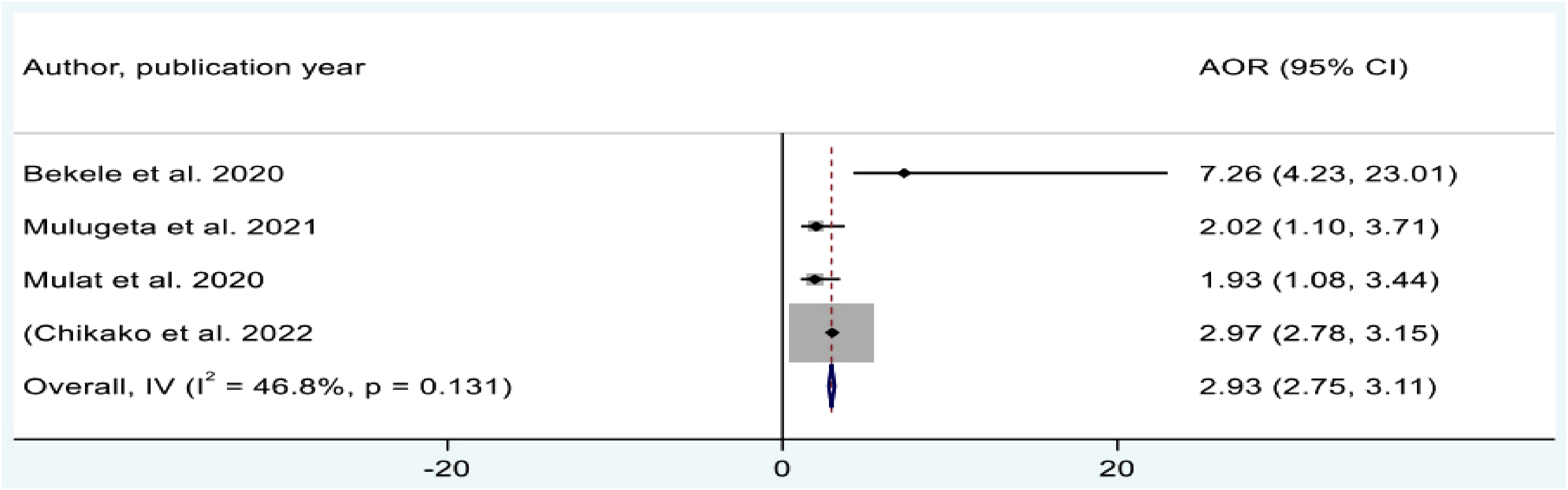
Forest plot showing the pooled odd ratio for the association between distance from the health facility and antenatal care (ANC) dropout in Ethiopia.
The pooled effect of place of residence on ANC dropout was assessed using 2 studies.11,14 In this study pregnant women from rural areas were about 1.6 times more likely to have ANC dropout compared to women from urban areas counterparts (AOR = 1.79, 95% CI = 1.31, 2.26) (Figure 7).

Forest plot showing the pooled odd ratio between place of residence and antenatal care (ANC) dropout in Ethiopia.
Additionally, 2 studies 11,12 were used to assess the pooled odd ratio for the association between pregnancy complication signs and ANC dropout. Accordingly, pregnant women who had no pregnancy complication signs were 2.88 times more likely to drop out from ANC compared to the counterparts (AOR = 2.97, 95% CI = 2.77, 3.16) (Figure 8).

Forest plot showing the pooled odd ratio b/n pregnancy complication signs antenatal care (ANC) dropout in Ethiopia.
Furthermore, in this meta-analysis, the pooled effects of educational level were assessed by 2 studies.10,14 The results also indicate that women who had no educational level were about 1.79 more likely to drop out from ANC compared to those women who have secondary and above educational level (AOR = 1.79, 95%CI = 1.37, 2.21) (Figure 9).
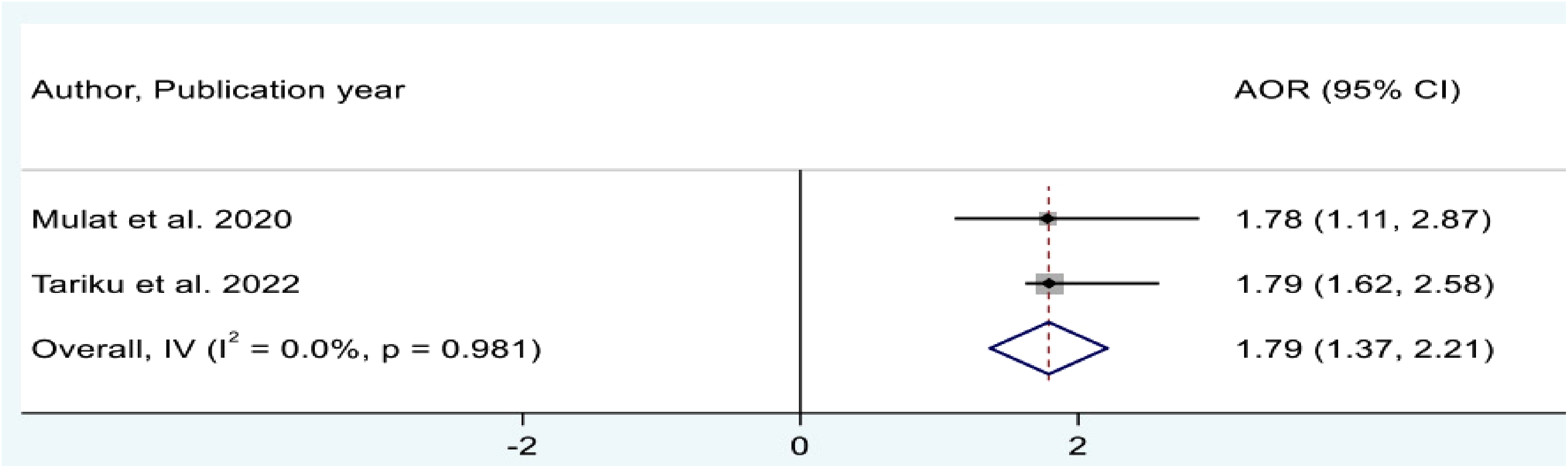
Forest plot showing the pooled odd ratio b/n educational level and antenatal care (ANC) dropout in Ethiopia.
Finally, the effect of age group on the ANC dropout was assessed using 2 studies,14,15 and the likelihoods of ANC services dropout were 39% (AOR = 0.61, 95% CI = 0.45, 0.78) lower among the pregnant women aged 30 to 49 years when compared with the pregnant women aged 15 to 29 years (Figure 10).

Forest plot showing the pooled odd ratio b/n age group and antenatal care (ANC) dropout in Ethiopia.
Discussion
This meta-analysis aimed to assess the pooled prevalence and determinant factors of ANC service dropout in Ethiopia. Accordingly, the overall prevalence of ANC dropout among women on ANC follow-up in Ethiopia was found to be 41.37% with 95% CI (35.04, 47.70). Despite the absence of systematic reviews and meta-analyses undertaken in Ethiopia or elsewhere, we contrasted the current pooled prevalence with a number of primary research conducted aboard. As a result, the prevalence of ANC dropout was higher when compared with the results of primary studies conducted in Nigeria 38.1% 21 and Kenya 29.2%. 22 This variation might be due to the fact that health care providers play a crucial role in Ethiopia by raising awareness of ANC through counseling and education. However, the result of this study was also lower than primary studies conducted in Uganda 55.8% 23 and Nepal 50.47%. 24 This variation could be due to differences in accessibility of health facilities, quality of maternal health services, and lack of awareness about ANC service; as noted in most of the studies included in this systematic review and meta-analysis.5,13,14
In this review, subgroup analysis was done by geographical region and the largest and the smallest pooled prevalence of ANC dropout was reported in a national wide research results, 47.04% (95% CI = 37.86, 56.27) and Tigray region 33.39% (95% CI = 29.45, 37.34), respectively. The low prevalence in the Tigray region might be due to the small sample size of the study used. Additionally, subgroup analysis was done by year of studies conducted and revealed that studies conducted since 2019 had the highest pooled prevalence of ANC dropout 44.35% (95% CI = 34.05, 54.65), compared with studies conducted before 2020. One possible reason could be that the Ethiopian government's emphasis on addressing the low uptake of maternal health services through various measures to improve ANC. 25
Another aim of this systematic review and meta-analysis was to find the most important variables influencing the prevalence of ANC service dropout in Ethiopia. Accordingly, distance from the health care facility, marital status, level of education, place of residence, pregnancy complication signs, and age group were identified as significant determinants of ANC dropout.
This study found that women who travel more than 1h to reach the health institution was more likely to have ANC dropout than their counterparts. This result was supported by studies conducted in Nigeria, 26 South Africa, 27 southern Ghana, 28 and Tanzania. 29 This might be due to the fact that some rural women in developing nations spend more time on their multiple responsibilities, such as care children, gathering water or fuel, cooking, cleaning, and engaging in agricultural work. As a result, they may not be able to travel long distances or use different transportation services to get into the health facilities to access health care services.
This study found that pregnant women who had no pregnancy complication signs were significantly associated with ANC dropout. This study report was supported by study results done in Hadiya zone Ethiopia, 30 South Sudan, 31 Malawi, 32 and low-income and middle-income countries. 33 The possible justification might be due to low attention of health care seeking, and a lack of community access to the health care system.
Furthermore, this meta-analysis revealed that place of residence had significantly associated with ANC dropout. Pregnant women from rural areas had ANC dropout than women from urban areas. This finding is consistent with studies conducted in Ethiopia, 34 Indonesia, 35 and Nigeria.29,36 The possible justification could be due to the less availability of health care facilities in rural areas. And also this study could suggest that urban women may have better access to health care services and have a better understanding of prenatal care than rural women.
In addition, this meta-analysis discovered that women's educational level had significantly associated with ANC dropout. Women who had no educational level were more likely drop out from ANC compared to those women who have primary and above educational level. This finding is consistent with studies report conducted in Enemay district Ethiopia, 37 Pakistan, 38 Nigeria, 39 and Egypt. 40 The possible reason could be the direct relationship between women's education and preference for prenatal care. Those who are more knowledgeable about the importance and appropriateness of ANC services are more likely to take advantage of the recommended number of ANC visits. 41
Finally, women who were in the age group of 30 to 49 years had lower ANC dropout than women in the age group of 15 to 29. The possible justification could be due to the fact that women of older age are more able to make their own health care decisions, which in turn increases the likelihood that pregnant women will use ANC services. This study suggests that early age at marriage has a negative impact on ANC utilization.
Limitations of the Study
Despite the fact that this systematic review and meta-analysis on ANC dropout and its associated factors was the first of its kind in Ethiopia, the limitations listed below should be considered when interpreting the results. Due to the nature of the study design, most of the studies considered were cross-sectional, making it difficult to establish a cause-and-effect relationship. In addition, most of the pooled odd ratios were computed from 2 studies which might be difficult to generalize. Furthermore, the included studies were from 3 regions, which may restrict the generalizability of the findings. And finally, due to the lack of sufficient literature on this topic, we were forced to compare some of our findings with primary studies conducted aboard.
Conclusion and Recommendations
This meta-analysis revealed the pooled prevalence of ANC dropout among pregnant women in Ethiopia was 41.37%. The major determinant factors associated with ANC dropout were distance from the health facility, place of residence, educational level, pregnancy danger sign, and age of women. Hence, to reduce the number of ANC dropouts, it is important to counsel and educate women during their first prenatal care. Issues of urban–rural disparity and locations identified as hotspots for incomplete ANC visits require further attention.
Footnotes
Acknowledgments
The authors would like to thank the authors of the studies included in this systematic review and meta-analysis.
Author’s Contribution
Gizaw Sisay: Conceptualization; formal analysis; methodology; validation; and writing the original draft.
Tsion Mulat: Data curation; methodology; software; writing—review and editing the manuscript.
Data Availability Statement
All the datasets used in this study are accessible in the published article and its additional files.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval and Consent to Participate
Not applicable; since we did not use primary data that needs ethical approval and consent to participate.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
