Abstract
Background
Even though colostrum discarding hurts child health, little is known about the extent of the problem and its contributing factors in Southern Ethiopia. This study aimed to determine the prevalence of colostrum avoidance practices and associated factors among mothers of children aged less than 12 months in Jinka town, South Ethiopia.
Methods
A community-based cross-sectional study was conducted at Jinka Town from March 1 to 30, 2020. A total of 420 mothers having children less than 12 months of age were selected by systematic sampling technique. The data were collected by using pretested interviewer-administered and semi-structured questionnaires. The data was entered using EPI DATA 3.1 and exported to SPSS version 23 for analysis. Descriptive statistics, binary and multivariable logistic regression analysis were done. Adjusted odds ratio with 95% CI at a p-value < 0.05 was estimated to identify statistically significant variables with colostrum avoidance practices.
Results
The prevalence of colostrum avoidance practice was 9.8% [95% CI: (6.9–12.5)]. Delayed initiation of breastfeeding [AOR = 9.08(95% CI 4.16–19.83)], lack of breastfeeding counseling [AOR = 2.33(95% CI 1.11–4.87)], home delivery of index child [AOR = 2.48 (95% CI 1.16–5.27)] and poor knowledge on breastfeeding [AOR = 4.55(95% CI 1.95–10.63)] were factors associated with colostrum avoidance practices.
Conclusion
Colostrum avoidance practice among mothers of children aged less than 12 months in Jinka town was high. Delayed initiation of breastfeeding, lack of breastfeeding counseling, home delivery, and knowledge of breastfeeding practice were factors associated with colostrum avoidance practice.
Background
Breastfeeding is considered a proven child survival strategy, and the World Health Organization (WHO) recommends newborns be put on the breast within an hour after birth. 1 It provides immense immunologic, psychological, social-economic, and environmental benefits. 2 It also significantly reduces a child's risk of developing obesity, type 2 diabetes mellitus, and related chronic non-communicable diseases. 3 Moreover, colostrum feeding promotes a child's intellectual development. 4 Furthermore, it promotes effective suckling, successful establishment, and maintenance of breastfeeding throughout infancy. 5 However, in different countries including Ethiopia, a significant proportion of mothers are deprived of colostrum for their newborn.6–8
Colostrum is the first milk that is produced in the first few hours after delivery. It is thick, sticky, and clear to yellowish in color. It comprises proteins, vitamin A and maternal antibodies vital to the newborn's nutrition till lactation is fully established. 9 It is the low-volume concentrated form of the nutrient supply system, which suits newborns with the premature digestive systems. It has a laxative effect which facilitate the passage of the baby's first stool, meconium. This helps to prevent neonatal jaundice by clearing excess amount of bilirubin, which is produced in large quantities at birth.10,11 Colostrum feeding is associated with a reduced risk of otitis media, gastroenteritis, and respiratory illness, necrotizing entero-colitis, obesity, and hypertension. 12 Contrary to these advantages, colostrum is considered heavy, thick, dirty, toxic, and harmful to children's health, and therefore in some societies, a portion of colostrum is discarded.
Globally, colostrum avoidance is practiced in many countries; In Uttarakhand, India 92% of mothers discarded colostrum, In Nepal 16.5%, In Pakistan 27.9%, and Burkina Faso 16% of mothers deprived of colostrum for their infants.13–16 In Ethiopia, colostrum discarding is the common nutritional malpractice. In Afar 35%, in Debre Tabor 25.6% in Raya kobo 13.5%, in Axum 6.3%, and Motta town 20.3% of mother reported that they discarded colostrum.17–21 Factors contributing to colostrum avoidance identified by previous studies were: home delivery, failure to attend ANC, lack of post-natal care, late breastfeeding initiation, and poor knowledge of optimal breastfeeding.19,20,22
Globally, more than 4000 infants and young children die because they do not get colostrum within the first hour after birth. 23 Among women in developing countries who do not give colostrum feeds, most of them avoid colostrum feeding based on cultural beliefs that range from no nutritional value for infants to harmful to the infant's health. 24 Every day, 3000–4000 infants die in the developing world from diarrhea and acute respiratory infections because they were receiving inadequate amounts of breast milk in their feeding and were deprived of colostrum. 25 A study carried out in the Afambo district, Afar found that children who were colostrum avoided had 2.34 times increased likelihood of being underweight when compared to those children who were fed colostrum. 26
A wide range of dangerous newborn feeding practices was familiar in Ethiopia even after the implementation of infant and young child feeding guidelines. 27 The Government of Ethiopia has been devising different strategies including generating of health extension program and working in collaboration with Non-Governmental Organizations (NGOs) in the areas of IYCF.28,29 WHO and UNICEF recommend that children should initiate colostrum within the first hour of birth, However, in Ethiopia, about 27% of the infant had not started colostrum within one hour of birth.30,31 Although colostrum avoidance harms child health, little is known about the extent of the problem and its contributing factors in Southern Ethiopia particularly in the study area. As there are diverse cultural practices among Ethiopian communities, evidence generated by this study will assist in developing context-specific interventions to halt colostrum avoidance practice and promote optimal IYCF practice. Therefore, this study aimed to assess the prevalence of colostrum avoidance practices and its associated factors among mothers of children aged less than 12 months in Jinka Town, Southern Ethiopia.
Methods and Materials
Study Setting, Design, and Period
A community-based cross-sectional study was conducted in Jinka Town, South Omo Zone from March 1 to 30, 20202 which is situated 755 Km away from Addis Ababa and 525 Km from Hawassa. The Town has an estimated population size of 31226 living in 6 kebeles (the smallest administration unit in Ethiopia). Out of the total population, 15582 are males and 15644 are females. Out of all female population, 6076 are women in the reproductive age group (15–49 yr). About 997 of the total population are accounted for by children less than one year of age. The Town has 1 hospital, 1 health center, and 6 health posts providing health services including maternal and child health care. The town also has 12 private clinics and 13 drug vendors. 32
Source Population
All mothers of children aged less than 12 months in Jinka Town, South Omo Zone.
Study Population
All mothers of children aged less than 12 months in the selected kebeles of Jinka Town during the data collection period.
Eligibility Criteria
Sample Size and Sampling Technique
In this study, the sample size was determined by using the single population proportion formula. Considering the prevalence of colostrum avoidance practices of 20.3% obtained from a previous study conducted in Motta Town,
21
95% confidence interval, the margin of error of 4%, and 10% non-response rate. The following single population formula:
A systematic sampling technique was employed to select the study participants. From a total of 6 kebeles of Jinka Town 4 Kebeles were selected by lottery method. To obtain the sample size from each selected kebeles proportional allocation to sample size was done. First, the numbering of all households of selected kebeles with mothers of children aged less than 12 months was conducted, and then a systematic sampling technique was applied for selection of the study participants. Finally, every Kth = 2 mother from each household of the selected Kebele was identified until the required sample size was fulfilled and the starting household was selected using a lottery method. At the time of the survey, from each household unit, one eligible mother who had a child aged less than 12 months were selected.
Study Variables
Dependent variable
Colostrum avoidance practices
Independent variables
Socio-demographic factors: age of the mother, educational status of the mother, educational status of father of index child, marital status, religion, ethnicity, occupation of the mother, household's wealth status, family size, and sex of the index child. Maternal health service utilization: ANC visit, BF counseling during ANC visit, place of delivery of index child, mode of delivery of index child, and postnatal care. Breastfeeding history: delayed initiation of BF and prelacteal feeding practices. Knowledge: mother's knowledge of BF. Maternal health-related factors: medical conditions and breast problem
Operational Definition and Terms
Data Collection Procedure and Data Quality Control
A structured interviewer-administered questionnaire was used to collect data from mothers of a child. The questionnaire was constructed by adapting from previous literature.13,18–20,22 The questionnaire was initially prepared in English and then translated into the Amharic version (local language) by different a fluent speakers of both languages and then to English to check its consistency. The data were collected by four trained diploma nurses who are fluent speakers of the local language and supervised by two BSc public health professionals. A face-to-face interview technique was conducted at the study participants’ houses.
The questionnaire was pretested before the actual data collection on 5% of the sample size in a nearby Town, Key Afer to check clarity and consistency of the data collection instruments. The collected data were checked for the consistency, completeness, and relevance on a daily during the entire data collection by the supervisors and principal investigator.
Data Processing and Analysis
The collected data was coded and entered by EPI DATA 3.1 and exported to the statistical package for social science (SPSS) version 23.0 for analysis. Then data cleaning, editing recoding, and management were carried out. Descriptive statistics; mean, standard deviation, and proportion were done. The wealth index of participant's households was computed by the principal component analysis (PCA). Assumptions for factor analysis were checked. Finally, household wealth status was ranked into three categories (poor, middle, and rich). Binary logistic regression analysis was employed to examine the statistical association between the colostrum avoidance practices and independent variables. Variables that have p-value < 0.25 during bivariate analysis were entered into the multivariable logistic regression to identify statistically significant variables. The model goodness of fit was tested by Hosmer-Lemeshow statistic which is not significant P-value = 0.264. Multi co-linearity test was carried out to see the correlation between all multivariate independent variables using collinearity statistics which is tolerance > 0.1 and variance inflation factor < 10. An Adjusted odds ratio (AOR) with 95% CI at a p-value < 0.05 was estimated to identify statistically significant variables. The data were presented by tables, frequencies, and graphs.
Results
Socio-Demographic Characteristics of Mothers and Children
Four hundred twenty mothers having children less than 12 months of age were interviewed in this study, with a response rate of 98.4%. The mean age of respondents was 26.86(SD ± 5.06) years. About 183 (43.6%) of the respondents had a primary level of education. A majority of the respondents; 314(74.8%) were unemployed in occupation. About 247(58.8%) of fathers of index children had a secondary level of education and above. Around half of the children, 228(54.3%) were males (Table 1).
Socio-Demographic Characteristics of Mothers of Children Aged Less Than 12 in Jinka Town, South Ethiopia, 2018/19 (N = 420).

The Prevalence of Colostrum Avoidance Practices among Mothers
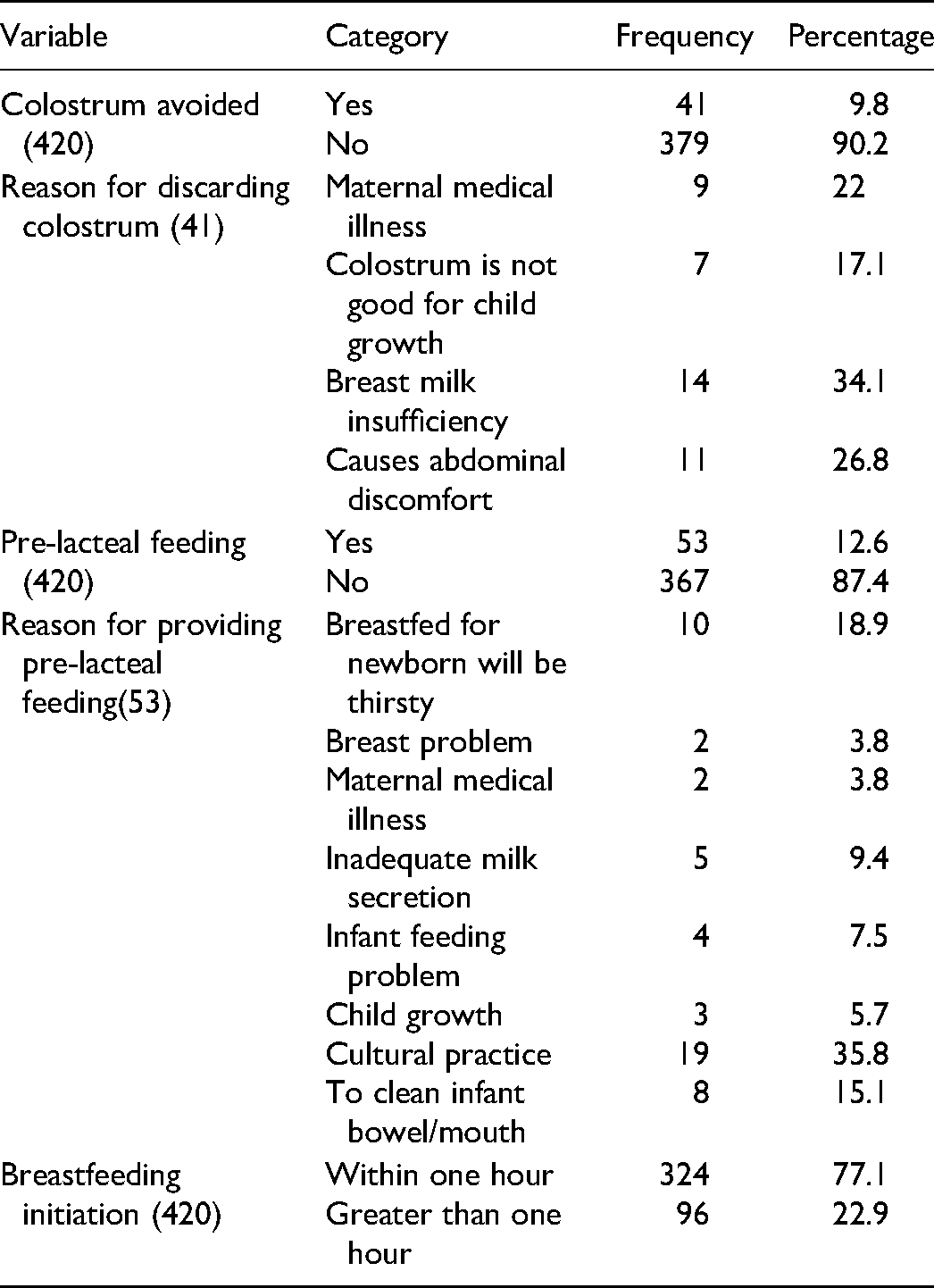
The prevalence of colostrum avoidance practices in this study was 41(9.8%) (95% CI: 6.9–12.5). The main reasons for colostrum avoidance were breast milk insufficiency 14(34.1%). Regarding of the total respondents; 53(12.6%) were practicing prelacteal feeding. A major reason for prelacteal feeding was cultural practice 19(35.8%). Three hundred twenty-four (77.1%) of mothers initiated breastfeeding within one hour (Table 2).
Colostrum Avoidance Practices among Mothers of Children Aged Less Than 12 Months in Jinka Town, South Ethiopia, 2018/19 (N = 420).
Maternal Health Care Service Utilization and Obstetric Characteristics
Three hundred eighty (90.5%) of mothers have utilized ANC services for their index infants. Of those mothers who have utilized ANC services 140(36.8%) visit four and above. About 268(63.8%) of respondents had got breastfeeding Counseling. Three hundred twenty-seven (77.9%) of mothers delivered their index child at a health facility. Three hundred fifty-one (83.6%) of mothers gave birth through spontaneous vaginal delivery. Two-third, (65%) of respondents utilized postnatal care. Nearly half 198(47.2%) of infants were birth order of second and third child (Table 3).
Maternal Health Care Service Utilization among Mothers of Children Aged Less Than 12 Months in Jinka Town, South Ethiopia, 2018/19 (N = 420).

Maternal Medical Condition and Breast Problem
A majority (89.3%) of mothers did not face any breast problems following the delivery of the index child. A majority 379(90.2%) of the mothers not faced any medical illness following the delivery of the index child (Table 4).
Maternal Medical Condition and Breast Problem among Mothers of Children Aged Less Than 12 Months in Jinka Town, South Ethiopia, 2018/19 (N = 420).

Maternal Knowledge on Breastfeeding
Of the total respondents, 290 (69%) of mothers know about as there is no need to give prelacteal feeding to the infant and 361(86%) of mothers know about the importance of the colostrum for the infant. Three hundred fifty-two (83.8%) mothers had good knowledge regarding optimal breastfeeding practices while the remaining 68(16.2%) had poor knowledge concerning optimal breast feeding practices (Table 5).
Breastfeeding Knowledge of Mothers of Children Aged Less Than 12 Months in Jinka Town, South Ethiopia, 2018/19 (n = 420).

The Factors Associated with Colostrum Avoidance Practices
In the final multivariable Logistic regression analysis, the time of initiation of breast feeding, BF counseling, place of delivery, and knowledge of breastfeeding practices were significant factors associated with colostrum avoidance practices. Mothers who delayed initiation of breastfeeding were 9.08 times more likely to discard colostrum when compared to mothers who started breastfeeding timely within one hour (AOR = 9.08, 95% CI; 4.16–19.83). Mothers who didn't get breast feeding counseling were 2.33 times more likely to discard colostrum when compared to those mothers who get breastfeeding counseling (AOR = 2.33,95% CI; 1.11–4.87). Mothers who delivered the index child at home were 2.48 times more likely to discard colostrum when compared to mothers who gave birth at a health facilities (AOR = 2.48,95% CI;1.16–5.29). Furthermore, colostrum avoidance practices were 4.55 times higher among mothers with poor knowledge of breastfeeding practices when compared to their counterparts (AOR = 4.55, 95% CI; 1.95–10.63) (Table 6).
Bivariable and Multivariable Logistic Regression Analysis of Factors Associated with Colostrum Avoidance Practices among Mothers of Children Aged Less Than 12 Months in Jinka Town, 2018/19.
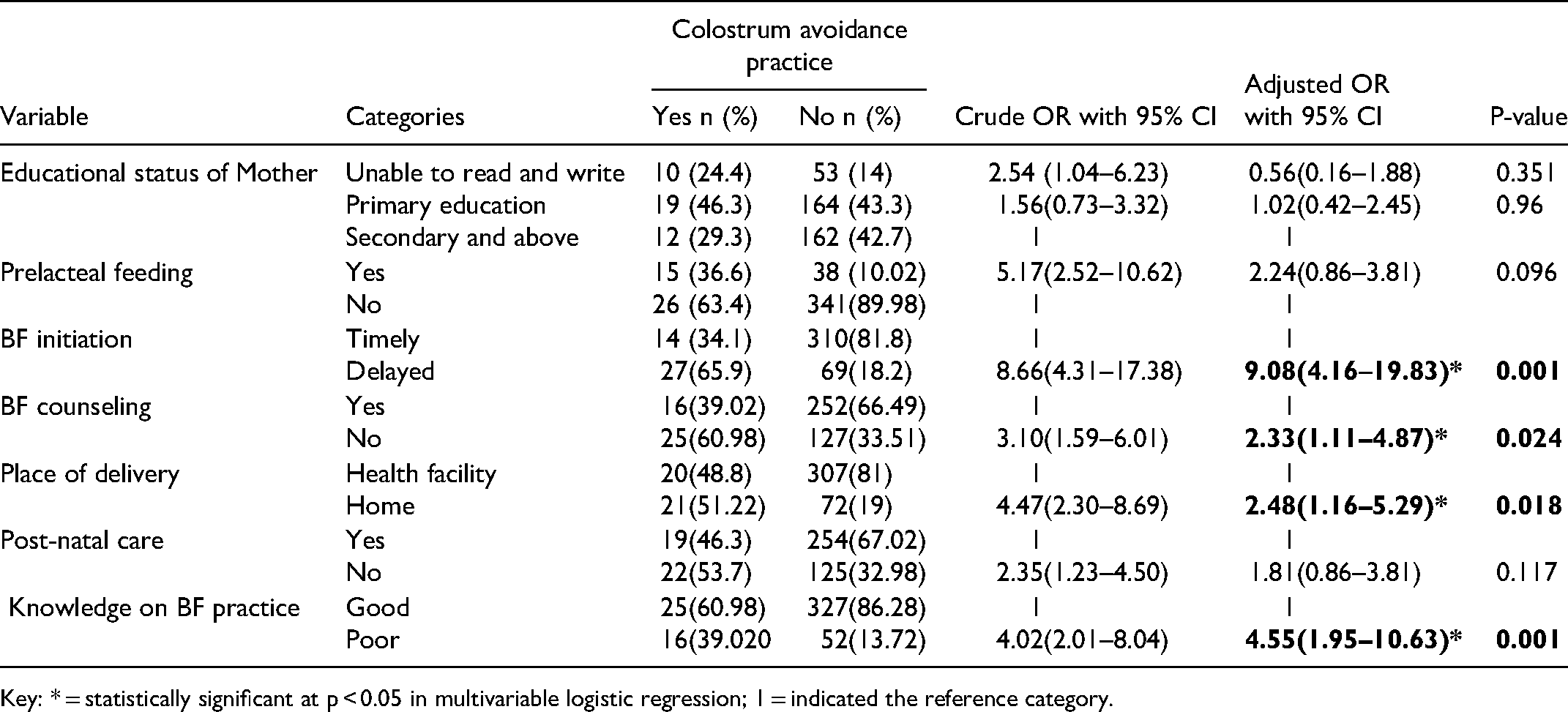
Key: * = statistically significant at p < 0.05 in multivariable logistic regression; 1 = indicated the reference category.
Discussion
This study aimed to assess the prevalence of colostrum avoidance practices and associated factors among mothers of children aged less than 12 months in Jinka town, South Ethiopia. In this study, the prevalence of colostrum avoidance practice was 9.8%. This result is consistent with the studies conducted in Axum town 6.3%, 20 North Wollo Zone 12%, 22 Raya Kobo District 13.5%, 19 and East Wollega Zone 8.8%. 33 However, the finding of this study was higher than the studies done in the Hula district, Sidama Region 3.9%. 34 The difference between these studies might be due to the difference in community attitude towards colostrum feeding among ethnic groups. The other possible reason for this inconsistency of the finding might be the sociodemographic differences among study participants.
The finding of this study is also lower than studies done in different developing countries. Uttarakhand, India 92%, 13 Nepal 16.5%, 14 Pakistan 27.9%, 15 Burkina Faso 16%, 16 South Sudan 38.8% 35 and Debre Tabor 25.6%. 18 This difference could be due to the difference in maternal health service utilization between study populations. This could also be the place of residence and difference in maternal educational level. Hence, mothers who reside in the towns would have better access to maternal and child health services.
In this study, Mothers who delayed initiation of breastfeeding were about nine times more likely to practice colostrum avoidance than those who initiated breastfeeding within one hour. This result is consistent with the study done in Raya Kobo District, North Wollo zone, Pakistan, Nepal and Uttarakhand, India respectively.13–15,19,22 This might be due to the fact that when the mother delays initiation of breastfeeding infants suckling activity decreases and which in turn affects or decreases maternal milk secretion due to decreased breast stimulation, which finally made the mother give other food to the infant and discard colostrum. 21
This study showed that mothers who didn't get breastfeeding counseling were 2.3 times more likely to discard colostrum when compared to the mothers who get counseling regarding breastfeeding. Other studies done in Hula District, Sidama Region, and East Wollega Zone showed that breastfeeding counseling during antenatal care improves timely initiation of first breast milk.33,34 This could be due to breastfeeding counseling during the perinatal period may increase the mother's awareness of optimal breastfeeding practices that might decrease colostrum avoidance. But study done in the Axum town revealed that there was no association between breastfeeding counseling during ANC visit and colostrum avoidance practices. 20 This could be due to variation in the utilization of maternal health services among study settings.
In this study, mothers who delivered their index infants at home were 3.48 times more likely to engage in colostrum avoiding practices when compared with those mothers who delivered in a health facility. This finding was consistent with a study done in Raya Kobo district, North Wollo Zone, Pakistan and Uttarakhand, India.13,19,22 This could be due to the fact that mothers, who gave birth at home, were more likely to be exposed to the traditional beliefs that favor colostrum discarding. In contrast, utilizing an institutional delivery would have an added benefit to receiving immediate obstetric care, such as early initiation of breastfeeding which reduces the likelihood of practicing colostrum avoidance.
The odds of colostrum avoidance were 4.55 times higher among mothers with poor knowledge of optimal breastfeeding practices when compared to their counterparts. This finding was supported by other studies carried out in Axum Town, Raya Kobo District, Hula District, and Uttarakhand, India.13,19,20,34 This might be due to the awareness of mothers about breastfeeding practices and the nutritional value of colostrum decreases the likelihood of colostrum discarding.
The limitation of this study was that the information obtained from mothers having children aged less than 12 months is subject to recall bias and also it is difficult to establish a temporal relationship as the study design was cross-sectional.
Conclusion
Colostrum avoidance practice among mothers of children aged less than 12 months in Jinka town was found to be high when compared to WHO recommendations. Delayed initiation of breastfeeding, lack of breastfeeding counseling, home delivery of index child, and poor knowledge of breastfeeding practice were significant factors associated with colostrum avoidance practices of mothers. Awareness creation activities on the nutritional value of colostrum, promotion of institutional delivery, and improving breastfeeding counseling are important interventions to reduce colostrum avoidance practices in Jinka Town.
Footnotes
Acknowledgements
we would like to express our heartfelt appreciation to the Jinka Town health office, data collectors, supervisors and study subjects.
Ethics Approval and Consent to Participate
The study protocol was approved by the Institutional Review Board (IRB) of the College of Medicine and Health Science, Arba Minch University. Based on the approval, an official letter of support was written by Arba Minch University Public Health Department to the Jinka Town health office. At last, data was collected after assuring the confidentiality of responses and obtaining informed verbal consent from the study participant.
Participant Consent
Obtained
Consent for Publication
Not applicable.
Availability of Data and Material
For those who are interested; the datasets of this study could be accessed from the corresponding author up on reasonable request.
Competing interests
The authors declare that they have no competing interests.
Authors’ Contributions
EA and FG designed the study, supervised the data collection, performed the analysis, interpretation of the data and prepared the first draft of the manuscript. GT, MG and ZJW assisted in data interpretation and reviewed the manuscript critically. All authors read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.

