Abstract
Currently, there is a paucity of available treatment strategies for oxidative phosphorylation disorders. Coenzyme Q10 (CoQ10) and related synthetic quinones are the only agents to date that have proven to be beneficial in the treatment of these heterogeneous disorders. The therapeutic efficacy of CoQ10 is not restricted to patients with an underlying CoQ10 deficiency and is thought to result from its ability to restore electron flow in the mitochondrial respiratory chain (MRC) as well as to increase the cellular antioxidant capacity. At present, however, there is no consensus on the appropriate dosage or therapeutic plasma level of CoQ10, and this information will be required before CoQ10 can be utilized effectively in the treatment of mitochondrial disease. The following review will outline our current knowledge on the use of CoQ10 in the treatment of MRC disorders and primary CoQ10 deficiencies.
Introduction
The mitochondrial respiratory chain (MRC; Figure 1) is located in the inner mitochondrial membrane and consists of 4 enzyme complexes: complex I (NADH: ubiquinone reductase; EC 1.6.5.3), complex II (succinate: ubiquinone reductase; EC 1.3.5.1), complex III (ubiquinol: cytochrome c reductase; EC 1.10.2.2), and complex IV (cytochrome c oxidase; EC 1.9.3.1;). 1,2 The MRC together with complex V (adenosine triphosphate [ATP] synthase; EC 3.6.3.14) synthesizes ATP, the energy currency of the cell by the process of oxidative phosphorylation. 1,2 In addition to existing as discrete entities, recent studies have indicated that the MRC enzymes can also exist as supercomplexes within the inner mitochondrial membrane consisting of aggregates of complexes I, III, and IV; complexes I and III; and complexes III and IV. 3
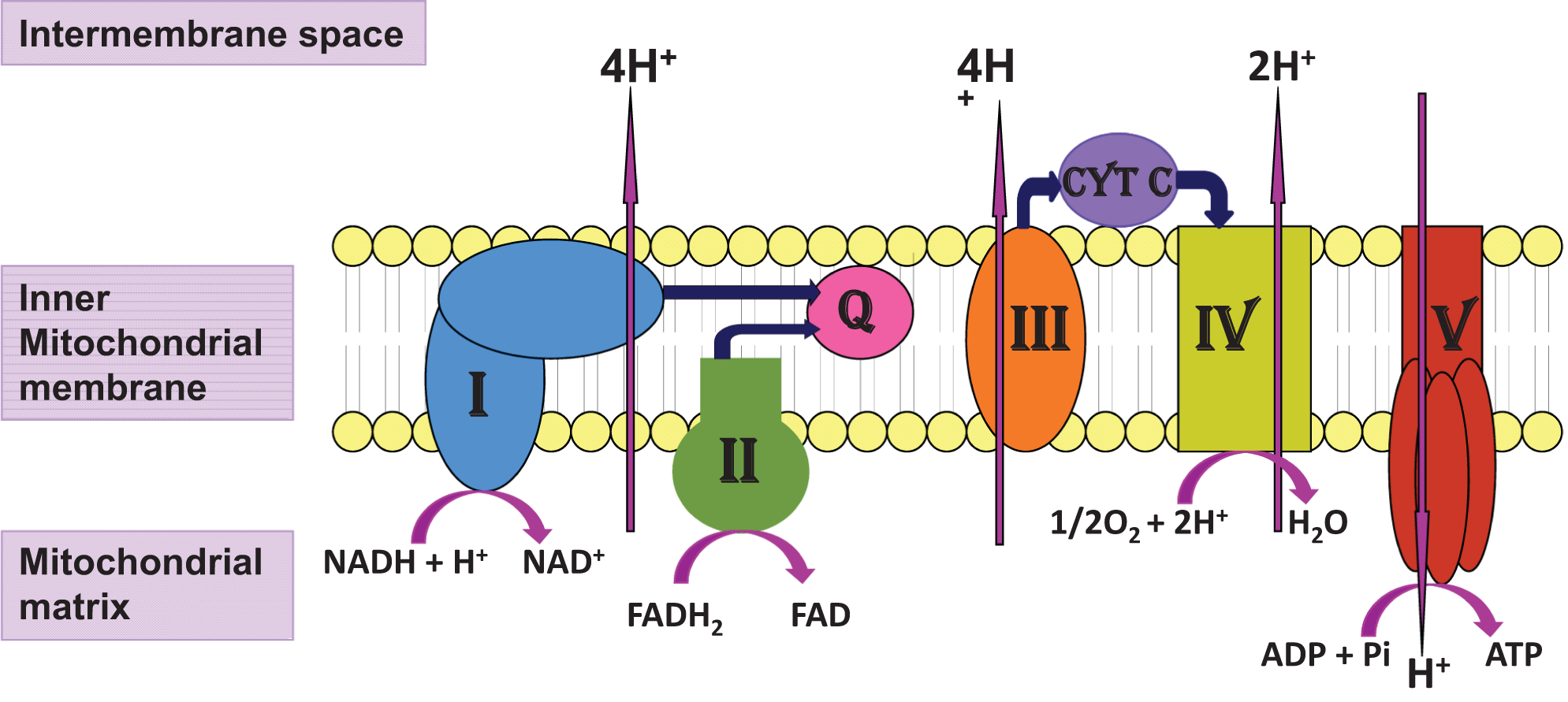
Mitochondrial respiratory chain (MRC).
The MRC disorders are a heterogeneous group of multisystemic diseases that develop as the result of mutations in either nuclear or mitochondrial DNA. 2 Once believed to be rare, inherited disorders of the MRC are now thought to represent one of the more commoner groups of inborn errors of metabolism with a birth prevalence of 1 in 5000. 4 The treatment of MRC disorders is extremely difficult and in general woefully inadequate with no overall consensus on appropriate therapeutic strategies. 5 To date, coenzyme Q10 (CoQ10) and its analogues are among a small group of agents that have been reported to offer some therapeutic potential in the treatment of MRC disorders.
Coenzyme Q10
Coenzyme Q10 is a small lipophilic molecule consisting of a benzoquinone nucleus and an isoprenoid side chain (Figure 2), which is synthesized by all cells apart from red blood cells, and shares a common biosynthetic pathway with cholesterol. 6 Coenzyme Q10 serves as an essential electron carrier within the MRC, transferring electrons derived from complexes I and II to complex III and therefore allowing a continuous passage of electrons within the chain, which is essential for the process of oxidative phosphorylation. In addition to its role as an electron carrier, CoQ10 functions as a lipid-soluble antioxidant, protecting cellular membranes and plasma lipoproteins against free radical–induced oxidation. 7 The antioxidant function of CoQ10 is attributed to its fully reduced ubiquinol form. 7 Other functions of CoQ10 include membrane stabilization and modulation of gene expression. 8,9 In view of all these functions, a deficiency in CoQ10 status could conceivably contribute to disease pathophysiology by causing a failure in mitochondrial energy metabolism, compromising cellular antioxidant capacity as well as adversely affecting membrane stability and gene expression. A deficiency in CoQ10 status can result from either a genetic defect in the CoQ10 biosynthetic pathway, known as a primary deficiency, or as the result of a mutation in a gene not directly involved in CoQ10 biosynthesis, known as a secondary deficiency. 10
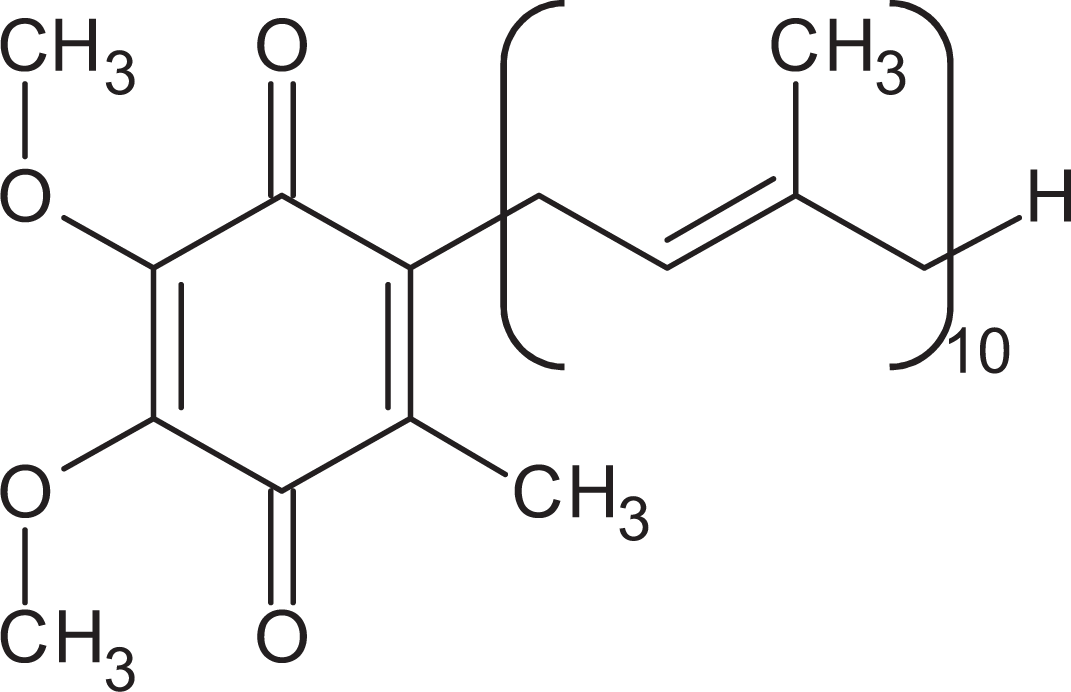
Structure of coenzyme Q10 (CoQ10).
Primary CoQ10 Deficiencies
The first reported cases of CoQ10 deficiency in the literature described 2 sisters born to unrelated parents who presented with recurrent rhabdomyolysis, seizures, and mental retardation. 11 On assessment, the muscle CoQ10 status of these patients was found to be approximately 3.7% of mean control values indicating the evidence of a primary defect in CoQ10 biosynthesis, as yet however, the genetic cause of this defect has yet to be elucidated. Since this time, well over 150 patients have been reported with CoQ10 deficiency, although there are no precise epidemiological data for the overall incidence of this condition. 12 Coenzyme Q10 deficiency appears to have a particularly heterogeneous clinical presentation, although it can be divided into 5 distinct clinical phenotypes: encephalomyopathy, severe infantile multisystemic disease, nephropathy, cerebellar ataxia, and isolated myopathy. 12 In most cases, the family history indicates an autosomal recessive mode of inheritance; and to date, mutations in 9 genes involved in the human CoQ10 biosynthetic pathway have been reported (PDSS1, PDSS2, COQ2, COQ4, COQ6, COQ7, ADCK3, ADCK4, and COQ9). 13,14
Secondary CoQ10 Deficiencies
Overall, the incidence of secondary CoQ10 deficiencies appears to be more common than that of primary CoQ10 deficiencies, 10 being a common feature among diseases, such as MRC disorders. 10,12,15,16 Furthermore, it has been suggested that a deficit in CoQ10 status may be a good predictor of an MRC deficiency. 17 Indeed, a CoQ10 deficiency has been reported in patients with a range of MRC disorders originating from mutations either in mitochondrial DNA such as Kearns Sayre Syndrome or nuclear DNA such as mitochondrial DNA depletion syndrome. 16,18,19,20 A CoQ10 deficiency has been detected in plasma/serum 18,19,21 as well as in muscle 15,17 in these patient groups. The cause of the CoQ10 deficiency in MRC disorders has yet to be fully elucidated, but it may result from the oxidative degradation of CoQ10 as a consequence of the increase in oxidative stress that is associated with MRC dysfunction 22 or just be a reflection of generalized mitochondrial impairment. 16 The decrease of plasma/serum CoQ10 levels in patients may also reflect an increased utilization or requirement by the MRC defective tissue(s)/organ(s) as well as liver impairment, as this is the major site of synthesis for circulatory CoQ10. 23 Furthermore, since the enzymes involved in CoQ10 synthesis are thought to exist in a superenzyme complex closely associated with the MRC in the inner mitochondrial membrane, an incomplete or abnormal MRC may adversely impact on the structural formation of the CoQ10 superenzyme complex resulting in impaired CoQ10 biosynthesis. 24
Treatment of Primary CoQ10 Deficiency
A primary CoQ10 deficiency is unique among MRC disorders in that it is potentially treatable if oral supplementation is commenced with high-dose CoQ10 during the early stages of the disease with clinical improvement being reported in all forms of this condition. 25 However, treatment protocols for CoQ10-deficient patients have not yet been standardized, and results have varied between studies. 25 Although muscle symptoms associated with CoQ10 deficiency appear to improve in most cases upon CoQ10 supplementation, cerebral symptoms are generally less responsive to treatment. 12 This is illustrated in patients with the ataxic presentation of CoQ10 deficiency who show a variable response to CoQ10 supplementation. Four patients with mutations in the ADCK3 gene have been reported to show improvement following CoQ10 supplementation with stabilization of the cerebellar ataxic features, reduction in myoclonus, improvement in speech, and ataxic symptoms. 12,26 In contrast, no improvement in symptoms have been reported in 7 patients carrying mutations in the same gene. 27,28 Furthermore, 11 patients with cerebellar ataxia and CoQ10 deficiency of undefined molecular cause also failed to show any sign of clinical improvement following CoQ10 supplementation. 29,30 In addition, despite almost complete amelioration of muscle symptoms, cerebral symptoms in patients with the encephalomyopathic phenotype again showed a variable response to CoQ10 treatment. 11,31,32 The reasons for the refractory nature of the neurological sequelae associated with a CoQ10 deficiency are as yet unknown and may be a consequence of irreversible damage prior to supplementation, the retention of CoQ10 in the blood-brain barrier (BBB) itself or simply reflect poor transport across the BBB. Animal studies have indicated that CoQ10 can be transported across the BBB following high-dose supplementation. 33,34 However, it is uncertain whether the degree of CoQ10 uptake demonstrated in these animal studies would be sufficient to replenish the cerebral levels of this quinone in a deficiency state.
Patients who develop renal dysfunction as the result of a CoQ10 deficiency appear to respond well to high-dose CoQ10 supplementation if treatment is initiated early in the course of diseases, with progressive recovery of renal function and decreased proteinuria being reported. 35,36 In contrast, CoQ10 supplementation was reported to be unsuccessful in inducing the recovery of renal function once chronic renal failure had developed. 37 In order to exploit the “window of opportunity” whereby organ dysfunction may be amenable to CoQ10 treatment, supplementation at birth has been suggested for siblings of CoQ10-deficient patients. 38
In vitro studies have indicated that the use of modified precursors of the quinone ring of CoQ10 to bypass the enzymatic defect may be effective in treating specific mutations of the COQ6 and COQ7 genes. 39 Studies in yeast harboring the mutant COQ6 gene revealed that treatment with vanillic acid as well as 3-4-hydroxybenzoic acid could restore respiratory growth. 13,14 These compounds may therefore prove efficacious in the treatment of patients with COQ6 mutations and are now being evaluated in mammalian cells. 40 The CoQ10 analogue, 2,4-dihydroxybenzoic acid, also demonstrated some therapeutic potential by its ability to restore CoQ10 biosynthesis in COQ7 mutant human fibroblasts. 42
Treatment of MRC Disorders
At present, there are no standardized therapeutic protocols for the treatment of patients with oxidative phosphorylation disorders, and treatment can vary between specialist centers. An extensive review about the current status of small molecule treatments and clinical trials in mitochondrial patients has recently been published. 41 However, once diagnosed, patients generally receive a “mitochondrial cocktail” containing antioxidants and cofactors for the various constituents of the MRC. The “cocktail” can consist of antioxidants such as vitamin E and C, the flavoprotein precursor riboflavin, and creatine monohydrate to assist in ATP generation. 43,44 Coenzyme Q10 is often a constituent of this “cocktail” because in addition to serving as an antioxidant it can serve to restore electron flow in the MRC. 45 Unfortunately, it has been suggested that patients with complex V deficiencies such as those with the clinical syndrome Neuropathy, ataxia, and retinitis pigmentosa (NARP), which has been associated with increased oxidative stress, may not benefit from CoQ10 therapy. 46 This is because the general blockage of electron flow in the MRC as the result of a complex V deficiency may impede the redox recycling of ubiquinol from CoQ10, which is facilitated by redox exchange with the MRC. A number of small studies have assessed the therapeutic potential of CoQ10 in the treatment of MRC disorders with variable outcomes, 15,18,19,47,48 although evidence of clinical improvement has been documented in a number of these studies with reports of increased strength, 49 accelerated postexercise recovery, 50 and improvement in oxygen consumption. 51 Coenzyme Q10 therapy was also reported to correct pancreatic β-cell dysfunction in patients with mitochondrial encephalomyopathy and lactic acidosis and diabetes mellitus. 52 However, the most consistent finding appears to be at the biochemical level with a decrease in plasma/serum lactate and pyruvate levels being widely reported following exercise 48,51,53,54,55,56,57,58 . In contrast, some studies have shown no evidence of clinical or biochemical improvement in patients following CoQ10 supplementation 59,60 . The failure to elicit a therapeutic effect in these studies may in part be attributable to the dosage or duration of the CoQ10 supplementation employed. However, it has been suggested that patients who show some form of biochemical or clinical improvement (responders) following CoQ10 supplementation may be those patients who harbor an underlying CoQ10 deficiency 19,61 . This is demonstrated in the study by Sacconi et al 15 who reported the evidence of clinical improvement in 7 out of 8 patients with MRC disorder having an underlying CoQ10 deficiency following CoQ10 supplementation, as opposed to clinical benefit being reported in only 1 out of 15 patients with MRC disorder having no evidence of a muscle CoQ10 deficiency. This illustrates the importance of determining CoQ10 status prior to commencing CoQ10 supplementation in order to identify this subgroup of patients who may respond to treatment. An in vitro study by Chan and colleagues 62 reported that CoQ10 supplementation of hepatocytes with a pharmacologically induced MRC complex I deficiency was able to restore both mitochondrial membrane potential (MMP) and cellular antioxidant status. This indicated the potential of CoQ10 to be reduced by cytosolic DT-diaphorase (NQO1 or NAD(P)H: quinone oxidoreductase) and then bypass the deficiency at complex I, feeding electrons directly into complex III of the MRC to restore MMP. The short-chain synthetic quinone analogue of CoQ10, idebenone, is also thought to display a similar mechanism of action in the treatment of the mitochondrial disorder, Lebers hereditary optic neuropathy, which in general results from an MRC complex I deficiency. 45 However, in vitro studies have demonstrated the potential of idebenone to inhibit complex I activity and therefore, the therapeutic efficacy of this quinone in vivo may be attributable to a metabolite of this drug formed following the administration. 45 Another synthetic quinone, EPI-743, which is also reduced by NQO1 activity has shown some beneficial effects in the treatment of patients with MRC disorders. 63 Although its precise mechanism of cellular action has yet to be fully elucidated, EPI-743 treatment has been shown to replenish the level of the antioxidant, reduced glutathione (GSH), possibly resulting from its ability to facilitate the transfer of electrons between NOQ1 and GSH reductase. 64 In addition to its ability to restore cellular GSH status, the beneficial effects of EPI-743 in the treatment of mitochondrial disease may result from its possible interaction with the transcription factor, nuclear factor E2-related factor 2 (Nrf2), which regulates both the expression of antioxidant proteins and cellular energy metabolism. 63,65
Although a number of small studies and case reports have illustrated the potential benefits of CoQ10 in the treatment of patients with MRC disorder, 25 few controlled clinical trials have been conducted to evaluate its effectiveness. The trials that have been undertaken to date generally included patients with MRC disorder having variable genotypes and clinical phenotypes making it difficult to draw any firm conclusions to the responsiveness of particular groups of patients to CoQ10 therapy 21,48,66,67 . Although 2 trials demonstrated no benefit in any of the outcomes, 61 evidence of improvement in muscle strength 21 and a decrease in plasma lactate levels following exercise 48 was reported. It has been suggested that both the dose of CoQ10 administered and the duration of the study are factors that may compromise the therapeutic efficacy of CoQ10 in clinical trials 21,58 . The paucity of controlled clinical trials that have evaluated CoQ10 in the treatment of mitochondrial disease can be attributed to the difficulties encountered in recruiting sufficient patients and the relatively large expense of conducting such trials. However, phase 3 of a large-scale, double-blind, randomized clinical trial evaluating CoQ10 in the treatment of children with primary MRC disease has been completed, although the results are yet to be published. 42
Absorption and Bioavailability of CoQ10 Formulations
Although all cells of the body apart from red blood cells are capable of synthesizing CoQ10, the body also receives CoQ10 from dietary sources such as meat, fish, and some vegetables, with an estimated intake of 3 to 5 mg per day. 68 In view of its similar physicochemical properties to that of vitamin E, CoQ10 appears to follow an analogous pattern of digestive uptake. Gastric digestion releases dietary CoQ10 from the food matrix, secretions from the pancreas, and bile and then facilitates micelle formation leading to absorption of the solubilized lipid in the small intestine. Coenzyme Q10 is then incorporated into chylomicrons and transported via the lymphatic system into the circulation. 69 Following absorption from the gastrointestinal (GI) tract, CoQ10 is reduced into its ubiquinol form which is thought to occur in the enterocytes of intestine prior to its entry into the lymphatic system. 70 After release into the circulation, chylomicron remnants are readily taken up by the liver, where ubiquinol is repackaged into lipoproteins, primarily, low-density lipoproteins, and then rereleased into the circulation. 71 In general, tissues with a high-metabolic turnover or energy demand, such as the heart, kidney, liver, and muscle, contain relatively high concentrations of CoQ10, and it is thought that most of this CoQ10 pool is synthesized in such tissues. Approximately 95% of plasma and 61% to 95% of tissue CoQ10 are present in the reduced, ubiquinol form. 71,72 The brain and lungs are exceptions with ≤25% of total CoQ10 being found as ubiquinol. 72 This may reflect the higher degree of oxidative stress in these 2 tissues.
In cases of primary and secondary CoQ10 deficiency, acquisition of CoQ10 from the diet may be insufficient to meet cellular requirements as intestinal absorption of CoQ10 is very limited 71 and supplementation may be a consideration. An important factor to consider which may influence the clinical response to CoQ10 supplementation is the type of CoQ10 formulation employed, as this will have an important bearing on absorption and bioavailability. 40,73
In view of their superior absorption, the use of gel and oil-based formulations of CoQ10 has been recommended in preference to tablets 74 in the treatment of patients with mitochondrial disorders. Recently, a study by Martinefski et al 75 reported that liquid emulsion improved the bioavailability of CoQ10 with respect to solid formulations. Following administration, CoQ10 takes approximately 6 hours to reach its maximal plasma concentration. Subsequently, a second plasma CoQ10 peak is often observed at about 24 hours, which has been attributed to enterohepatic recycling as well as redistribution to the circulation. 76,77 Once administered, the circulatory half-life of CoQ10 has been reported to be approximately 36 hours requiring a 2-week period of cessation of treatment before it returns to its baseline level following 4 weeks of supplementation. 78 There is a lot of debate at present as to whether formulations of ubiquinol have a better absorption from the GI tract than those of CoQ10. It has been estimated that the GI absorption of ubiquinol is 3 to 4 times greater than that of CoQ10. 74,79 However, since upon absorption from the GI tract, CoQ10 undergoes reduction to ubiquinol, the purported superior bioavailability of ubiquinol formulations to that of CoQ10 may in part be attributable to the matrix in which the quinol is encapsulated. Furthermore, there is limited data available from patient studies and no clear indications of dosage compatibility. 40 Interestingly, ubiquinol treatment, in contrast to an equivalent dosage of CoQ10, was reported to increase the CoQ10 status of mitochondria from the cerebrum of a mouse model of CoQ10 deficiency due to a COQ9 mutation. 79 The results of this study may therefore have important implications for the treatment of the cerebral presentations of CoQ10 deficiency.
The efficiency of absorption of CoQ10 formulations has been reported to decrease as the dosage increases with a suggested block of GI absorption above 2400 mg, 74 and split doses have been recommended in preference to a single dose. 80 Dietary fat together with grapefruit juice consumption have been reported to improve the absorption of CoQ10. 74,81 In contrast, ingestion of high-dose vitamin E together with CoQ10 may impede the absorption of CoQ10 resulting in lower plasma levels of the quinone, 82 possibly as a result of competition during the GI absorption process.
Coenzyme Q10 Monitoring and Dosage
In view of its relative accessibility, clinical monitoring of CoQ10 status is generally based on plasma determinations with an established reference interval ranging from 0.5 to 1.7 μM. However, this will vary between centers. 83 Although the level of plasma CoQ10 is influenced by both diet and circulatory lipoprotein status, it may have utility in identifying both evidence of cellular CoQ10 deficiency 19 and increased tissue utilization and demand. 18 However, in view of the questionable reliability of plasma CoQ10 status to reflect that of cells, blood mononuclear cells 84 and urine epithelial cells 85 may be more appropriate surrogates to determine endogenous CoQ10 status. However, the “gold standard” for the assessment of tissue CoQ10 status is skeletal muscle, and this is commonly used to identify evidence of an underlying CoQ10 deficiency. 86
Currently, there is no consensus on the dosage of CoQ10 or the plasma level required that may prove efficacious in the treatment of patients with a primary CoQ10 deficiency and/or MRC disorders. Coenzyme Q10 supplementation is safe and well tolerated, exhibiting an excellent safety profile with doses as high as 2400 mg/d being used in the treatment of Parkinson disease. 87 Typically, doses in the range 5 to 30 mg/kg/d have been administered to patients with documented low levels of tissue CoQ10 as well as those with a primary CoQ10 deficiency. 25,88,89 In the absence of a demonstrable CoQ10 deficiency, doses of 5 to 30 mg/kg/d may also be used in the treatment of cases of known and suspected mitochondrial disease. 25,78 In Parkinson disease, a plasma CoQ10 level of 4.6 μmol/L was reported to be the most effective in slowing functional decline in patients. 90 An in vitro study using CoQ10-deficient human fibroblasts has shown evidence of an improvement in bioenergetics status/normalization of cellular antioxidant status following 7 days of treatment with 5 μM CoQ10. 91 Furthermore, a recent study by Duberley et al 92 indicated that supplementation with >10 μM CoQ10 may be required to restore MRC enzyme activities to control levels in CoQ10-deficient human neuroblastoma cells. To date, the highest plasma CoQ10 concentration reported is 10.7 μmol/L, using a solubilized ubiquinol formulation 74,83 that may have the potential to show some therapeutic efficacy in the treatment of the neurological presentation of CoQ10 deficiency. These latter in vitro studies indicate that the dosage/plasma level of CoQ10 required to elicit biochemical or clinical improvement may be dependent on the organ of disease presentation.
Discussion/Conclusion
The ability of CoQ10 to demonstrate some beneficial effect in the treatment of mitochondrial disease is thought to rely mainly on its ability to restore electron flow in the MRC and replenish cellular antioxidant capacity. As would be expected, patients with an underlying deficit in CoQ10 status may be more responsive to such therapy. However, factors such as the time of diagnosis, the dosage, and duration of CoQ10 therapy may influence the efficacy of this treatment. Although a number of case reports and small studies have indicated some therapeutic potential of CoQ10 in the treatment of patients with MRC disorders and primary CoQ10 deficiencies, there is as yet no consensus of the dosage or plasma level of CoQ10 required to achieve some clinical benefit and whether this is influenced by the organ of disease presentation. Determination of CoQ10 status in other biological specimens beyond plasma/serum may also be advisable. In this sense, CoQ10 monitoring in blood mononuclear cells 84 or in urine samples 85 may better reflect the cellular uptake of exogenous CoQ10. Furthermore, in view of the purported impermeability of the BBB to CoQ10, monitoring of cerebral spinal fluid CoQ10 levels in preference to those of plasma may be more appropriate in patients with cerebral disease presentations. 93 The possibility arises that the underlying cause of a particular oxidative phosphorylation disorder may dictate the appropriate quinone therapy to implement, whether utilizing CoQ10, a synthetic quinone, or a combination of the 2 in the treatment regime. At present however, this information is not available, and studies aimed at establishing these treatment protocols may improve the therapeutic efficacy of quinone supplementation.
Footnotes
Authors’ Note
The Centro de Investigación Biomédica en Red de Enfermedades Raras (CIBERER) is an initiative of the Instituto de Salud Carlos III.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research and/or authorship of this article: This work was supported by grant from the Spanish Ministerio de Economia y Competitividad PI14/00028 and FEDER Funding Program from the European Union.
