Abstract
Aim:
The aim of this study was to assess outcomes of biological (nonvascularized fibula grafts and extracorporeal irradiated autologous bone grafts) methods used for reconstruction of intercalary defects after resection of femoral diaphyseal tumors.
Materials and Methods:
This study included 28 patients who had undergone intercalary resection in femoral diaphyseal tumors between 2011 and 2016. The mean follow-up period was 24 months (range 12–57 months).
Results:
The mean union time for diaphyseo-diaphyseal union was 10.5 and 11 months in nonvascularized fibula group and extracorporeal radiotherapy (ECRT) group, respectively. The mean union time for metaphyseo-diaphyseal union was 6.5 months in both nonvascularized fibula and ECRT groups. Six patients had distant metastasis, and one patient had local recurrence. The mean Musculoskeletal Tumor Society score was 28 at the last follow-up. Two patients had surgical site infection in the nonvascularized fibula group. Implant failure was found in one patient of the ECRT group requiring revision surgery. Three patients had nonunion (two from the nonvascularized fibula group and one from the ECRT group).
Conclusion:
The present study indicates that the biological reconstruction modalities provide good functional outcomes in diaphyseal tumors of femur. Nonvasularized fibula and ECRT-treated autografts reconstruction provides good results, and union timing is comparable. The outcomes of the current study are promising as compared to the results in the reviewed literature. The reconstruction method depends on the resources available at the oncological center and the conversance with the method of the treating surgeon.
Introduction
Limb salvage has now become the primary mode of treatment due to improved imaging modalities, effective response to chemotherapeutic drugs and regimens, and advances in reconstructive surgery. Multimodality therapy has increased long-term survival rates of patients with chemotherapy-sensitive tumors (Ewing sarcoma and osteosarcoma) to 60%–70%. 1 –6 Tumors involving the diaphysis of the bone require intercalary resection and reconstruction. Various reconstructive options have been reported, which can be used to reconstruct the large osseous defects after a wide excision has been done. These are massive bone allograft, vascularized autologous fibula grafts, the combination of both, nonvascularized fibula grafts, intercalary prosthesis, and extracorporeal irradiated autologous bone grafts. Each technique has its advantages as well as limitations. 7 –31,32 –35 The most commonly encountered complications are fractures, nonunion, and infection. 32 –39
Nonvascularized fibula autografting procedure can be performed by an orthopedic surgeon without microvascular dissection in a routine surgical setup. 25 Second, the nonvascularized autograft incorporation rates are better than allograft. The availability of fibular autograft with minimal complications makes it a useful biological reconstruction modality in treating intercalary defects. In major countries across the globe, there is significant scarcity of bone bank, and it makes a relatively less common modality of reconstruction. The complications associated with nonvascularized fibula are risks of infection, nonunion, delayed union, fracture, and donor site morbidity. Extracorporeal irradiated autologous bone graft and reimplantation is an acceptable modality of reconstruction of defects created by removal of diaphyseal tumors. According to the published literature, this method is oncologically safe and avoids the complications associated with the use of massive allografts. Extracorporeal irradiated autologous bone graft is a size-matched bone and helps in fixation and union with the host bone. 40 The complications and problems associated with the extracorporeal irradiated autologous bone graft are nonavailability of radiation centers, risks of infection due to long surgical hours, nonunion, delayed union, and fracture. In this study, we used two different methods for the reconstruction of intercalary defects after the resection of femoral diaphyseal tumors: nonvascularized fibula grafts and extracorporeal irradiated autologous bone grafts. The aim of our study was to analyze oncological and functional outcomes using these different reconstruction methods.
Materials and methods
We studied 28 patients who had undergone intercalary resection for malignant femoral diaphyseal tumors between 2010 and 2016. The clinical profile, treatment modalities, and outcomes were reviewed retrospectively from the hospital medical records. The mean follow-up period was 24 months (range 12–57 months). The following details were recorded: demographic data (patient age at operation, gender, tumor site, and histological diagnosis), a disease at presentation, surgical details (length of bone defects, operation time, total blood loss, and reconstruction details), adjuvant therapy (chemotherapy and radiotherapy), postoperative complications (nonunion, fracture, implant failure, or infection), the time required for bone union, oncological outcomes, and functional outcomes. Resection of the tumor was performed in all cases, and reconstruction was done using biological methods after magnetic resonance imaging evaluation (Figure 1). Functional outcomes of the reconstructed limb were assessed using the Musculoskeletal Tumor Society (MSTS) scoring system. There was a follow-up protocol for reviewing the patient at 2 weeks postoperatively for suture removal, followed by adjuvant chemotherapy according to the histopathological reports. Then, the patients were followed up every month for a year. A computed tomography thorax and bone scan was performed at every 6-month follow-up for the initial 2 years and then every year for next 3 years. The osteotomy union was assessed using a plain radiograph. The radiograph of the affected extremity was performed at 1-month interval at every follow-up till bone union was achieved. Patients were provided physiotherapy, and proper rehabilitation protocols were followed. Quadriceps exercise and ankle pumps were started, and the patients were immobilized with plaster of paris and brace until bone union was achieved. The patients were followed up to evaluate the healing of the osteotomy, functional recovery, potential complications due to graft as well as due to tumor (local recurrence and distant metastasis) and then every 3 months thereafter.

T1-weighted magnetic resonance imaging of femur showing diaphyseal osteosarcoma of femur in pediatric patient (white arrow showing the extent of disease).
Results
Patient demographic data and study characteristics were analyzed. There were 18 males and 12 females with a mean age of 20 years (range 9–45 years). The histological diagnosis was Ewing sarcoma (n = 20) and osteosarcoma (n = 8). Four patients had a pathological fracture at presentation. The diaphyseal tumor involving femur was resected in all cases, and the specimen was sent for histopathological review; for assessing the extracorporeal radiotherapy (ECRT) group, the soft tissue was sent for calculating the percentage of necrosis. All 28 patients received neoadjuvant and postoperative chemotherapy, and seven patients received radiotherapy along with the chemotherapy. The mean length of the bone defect was 16 cm (11–19 cm). The fixation methods include locking plate in 28 patients. The union time at both metaphyseal–diaphyseal and diaphyseal–diaphyseal ends was recorded in all the groups. The mean union time for diaphyseal–diaphyseal union was 10.5 months and 11 months in the nonvascularized fibula group and theECRT-treated autograft group, respectively (Table 1). The ECRT was performed with 50-gray radiotherapy for 30 min duration (Figures 2 and 3). The average surgical time in the nonvascularized fibula group was 4.5 h and 5.5 h in the ECRT group. The mean blood loss in both groups was 500 ml. The reconstruction modality used in both groups was long locking plate fixation systems made of medical-grade stainless steel material. The mean union time for metaphyseal–diaphyseal union was 6.5 months in both the nonvascularized fibula group, and the ECRT group (Table 1), and the function was assessed (Figure 4). In total, 19 (70%) patients were free from disease, 5 (18%) had died, 3 (7%) were alive with disease, and 1 patient (3%) was lost to follow-up (Table 2). Five patients with pulmonary metastasis underwent metastectomy: two patients in the ECRT group and three in the nonvascularized fibula group. Three patients had pulmonary metastasis at presentation in the nonvascularized fibula group. One patient in the nonvascularized fibula group had local recurrence and underwent subsequent amputation. Postoperative complications included surgical site infection (SSI), nonunion, and implant failure. One patient in the nonvascularized fibula group with SSI required wound wash and debridement at frequent intervals and underwent amputation for the persistent infection. Another patient with SSI in the nonvascularized fibula group was treated successfully with debridement and antibiotics. One patient in the ECRT group had implant failure at 16 months in the postoperative period (Figure 5). This patient underwent resurgery, and reconstruction done with a nonvascularized fibula graft with anterior plate fixation. There are three cases of nonunion, two in the nonvascularized fibula group and one in the ECRT group. In all these patients, autologous bone grafting was done, and all nonunion healed uneventfully. Using the MSTS functional scoring system, the mean score was 28 and was similar in both groups.
Outcomes of the current study and review of literature.


Intraoperative clinical image showing extracorporeal irradiated autologous bone graft reconstruction and fixation with locking plate method (black arrow osteotomy sites).

Postoperative radiograph showing extracorporeal irradiated autologous bone graft reconstruction and fixation with locking plate method.
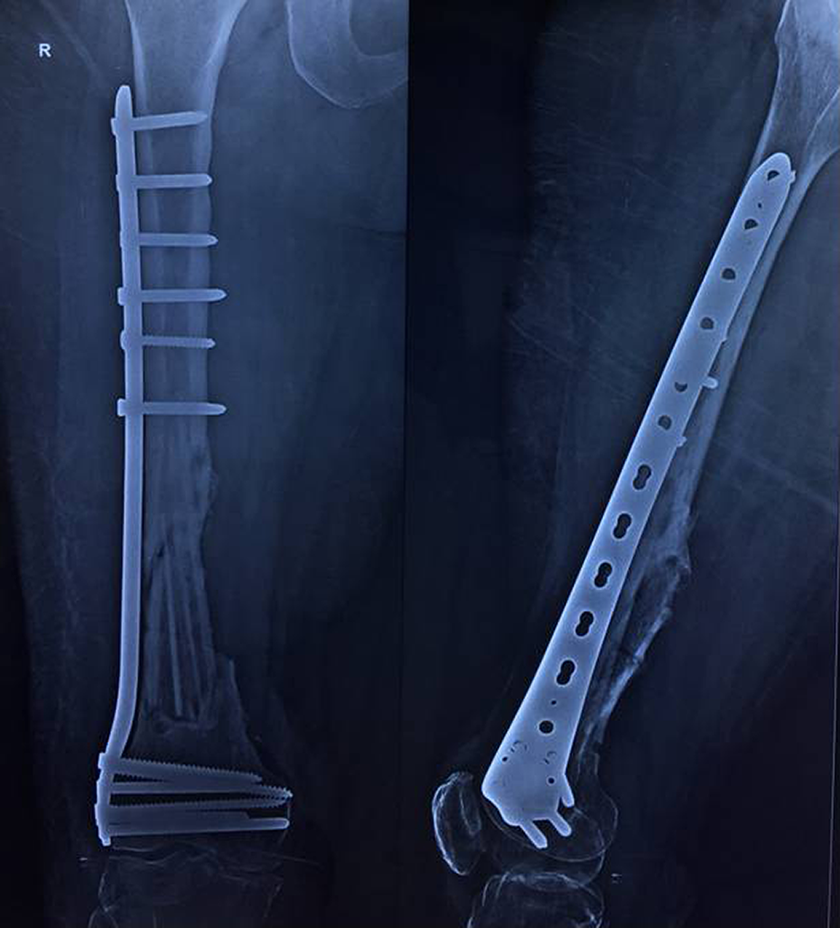
Postoperative radiograph showing use of the nonvascularized fibula in intercalary defects after resection of the femoral diaphyseal tumor.
Oncological outcomes.

ECRT: extracorporeal irradiated autologous bone grafts; NED: no evidence of disease; AWD: alive with disease.
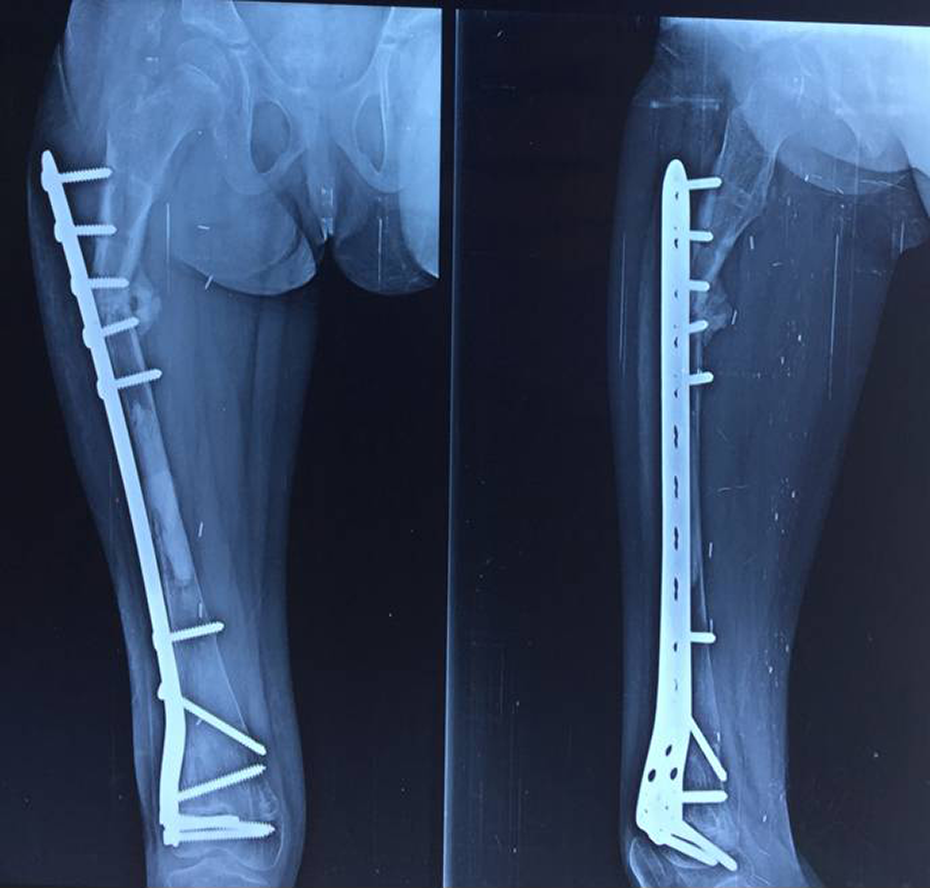
Radiograph showing implant failure and nonunion at the proximal metaphyseo-diaphyseal region following extracorporeal irradiated autologous bone graft.
Discussion
Wide resection of diaphyseal tumors in long bone tumors can create a large intercalary bone defect requiring reconstruction. Reconstruction options include use of segmental allografts, autoclaved autografts, pasteurized and irradiated autografts, intercalary metal implants, and vascularized and nonvascularized fibula grafts. 1 –3,7 –9 Ideal reconstruction method poses a great question to orthopedic surgeons. The choice of reconstruction method depends upon various factors such as patient age, functional demands, durability, complications, and morbidity of the procedure. These factors should be considered while planning for intercalary excision surgery. At present, no studies have been performed for the comparison of results of various biological reconstruction modalities for management of diaphyseal malignant tumors of femur.
Sewell et al. had analyzed the results of tibial intercalary endoprosthetic replacement; implant survival was 63% at 10 years, and the mean MSTS score was 23 (17–28). 41 Villemagne et al. studied the results of 12 children with intercalary segmental reconstruction of long bones after malignant bone tumor resection using primary methylmethacrylate cement spacer interposition and secondary bone grafting. 42 van Isacker et al. compared the results of osteoarticular allografts and intercalary allograft in forearm reconstruction following tumor excision. 43 Tanaka et al. analyzed the results of 19 cases in which reconstruction of the bone defect after resection of a musculoskeletal tumor was performed with the vascularized fibula graft. 44 Reconstructed bone defects were located in the femur in 10 cases (one of inlay graft, one of individual intercalary graft, seven of intercalary graft into treated bone, and one of curettaged bone marrow). The mean follow-up period after surgery was 7.25 years. The mean MSTS score was 98% (93–100%).
Krieg and Hefti had analyzed the results of use of nonvascularized fibula grafts after tumor resection and showed that the mean union time was 9 months (4–10 months) seen in 89% patients 25 (Table 1). The mean union time in the current study was 10.5 months for diaphyseo-diaphyseal union and 6.5 months for metaphyseo-diaphyseal union in the nonvascularized group. Nakamura et al. analyzed six patients with Ewing sarcoma of the mid-shaft femur who were treated by limb-sparing tumor resection and reconstruction with extracorporeal irradiated autologous bone graft with intramedullary cement with a mean follow-up of 41 months 40 (Table 1). The average length of the resected femoral bone was 23 cm (15–32 cm), and the average ratio of bone resection length to total femoral length was 60%. 40 Primary union of the distal and proximal osteotomy sites was achieved in three patients. Function was excellent in all patients with surviving reimplanted bone. 40 The mean union time in the current study for diaphyseo-diaphyseal union and metaphyseo- diaphyseal union was 11 months and 6.5 months, respectively, in the ECRT group. The mean union time for metaphyseo-diaphyseal union was 6.5 months in both the nonvascularized fibula group and the ECRT group.
Krieg and Hefti reported seven fatigue fractures in six patients, with only two requiring treatment. 25 Tanaka et al. in the analysis of the vascularized fibula graft showed that bone union was achieved for 79% of cases. The average period required to achieve bone union was 7.8 months. There were four cases of nonunion and two other complications. 44 The results of Nakamura et al. of the mid-shaft femur-treated reconstruction with extracorporeal irradiated autologous bone graft showed that there was neither infection nor fracture in this series and local recurrence was seen in one patient 40 (Table 1). Delayed union of the proximal osteotomy site occurred in one patient, nonunion occurred in one patient at the distal osteotomy site and was converted to endoprosthetic replacement, and another patient was converted to rotationplasty. 40 Nonunion was found in one patient in the ECRT group in the current study, and autologous bone grafting was done and union was achieved. One patient in the nonvascularized fibula group with SSI required wound wash and debridement at frequent intervals and underwent amputation for the persistent infection. Another patient with SSI in the nonvascularized fibula group was treated successfully with debridement and antibiotics. One patient in the ECRT group had implant failure at 16 months in the postoperative period. This patient underwent resurgery and removal of the implant and reconstruction done with the nonvascularized fibula graft with customized plate fixation.
The economic issues and high cost of treatment of bone sarcoma with logistic and nonavailability of allograft from limited number of bone banks forces the use of allograft a less popular method in developing countries. The prolonged surgery duration for the use of vascularized fibula due to the necessary harvesting of the fibula and the vascular anastomosis theoretically may increase the risk of infection, and secondly, it requires an expert plastic and vascular surgeon for vascular reconstruction. The most suitable or desirable method for reconstruction following removal of diaphyseal tumors in extremity is expected to be easy to perform and economic and provides optimal outcomes at all oncology centers. The use of nonvascularized fibula and ECRT with optimal outcomes and union time makes it a good alternative reconstruction modality.
The limitation of this study was the retrospective nature of it and the limited number of patients.
Conclusion
In conclusion, the presented study indicates that the biological reconstruction modalities provide optimal function in diaphyseal tumors of femur. Nonvasularized fibula and ECRT-treated autografts reconstruction provides good function and union rates. The outcomes of the current study are promising as compared to the results from the reviewed literature. The reconstruction method depends upon the resources available at the oncological center and the conversance with the method of the treating surgeon.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
