Abstract
Objective:
The aim was to compare the fracture strength of Molar endocrowns fabricated from different all-ceramic materials and various preparation designs.
Materials and methods:
Ninety extracted human molar teeth were root canal treated and randomly divided into three groups according to the all ceramic materials used for fabrication of the endocrowns (
Results:
The Lithium Disilicate endocrowns recorded the higher mean fracture strength for 4.5 mm occlusal thickness and 2 mm radicular extension at 3770.28 N and 3877.40 correspondingly. The High translucency zirconia endocrowns at conventional 2 mm thickness showed the highest mean fracture load (3533.34 N). Even though polymer infiltrated ceramic endocrowns displayed comparatively lesser fracture load; they recorded the predominantly favorable fractures.
Conclusions:
Increased occlusal thickness showed a significant improvement in fracture strength of lithium disilicate and polymer infiltrated ceramic molar endocrowns. Although the 2 mm radicular extension had the substantial enhancement of fracture strength in high translucency zirconia, it resulted in more unfavorable failure types.
Keywords
Introduction
The rehabilitation of Root canal (endodontically) treated teeth (ETT) is considered being completed only with the timely and adequate restoration of the tooth. Apart from providing a coronal seal, it is required to restore the esthetic and functional needs of the patient. Conventionally ETT is restored with endodontic post and full veneer crowns. This method exhibits multiple clinical challenges like unfavorable C factor, predisposing for canal perforation, and root fractures. 1 Moreover, the endodontic post has limited applicability in dilacerated and short root canals. In this context, Bindl and Mörmann suggested the monolithic ceramic endocrowns as an alternative to conventional post retained full veneer crown. 2 The endocrowns (EC) are one-piece ceramic restoration; deriving macro-mechanical retention from the internal wall of the pulp chamber and micro-retention with adhesive cementation. 3 The major advantage of EC is the reduced interface between various materials like a post, luting cement, radicular dentin, and indirect restoration. These interfaces of materials with a different modulus of elasticity are reported to be the locus of stress concentration and subsequently leading to root fractures. 4 Sedrez-Porto et al. 5 reported that the EC may perform similarly or better than conventional treatments.
The success and longevity of EC depend on accurate tooth preparation design and selection of appropriate ceramic. 6 The earlier research reports are contradictory regarding the effect of occlusal thickness on the fracture resistance of EC. Mörmann et al. 7 reported the high fracture load values of bonded crowns with thick occlusal dimensions, while Tsai et al. 8 and Zhu et al. 9 recommend 1.5 mm thickness to prevent the bulk fracture. The clinician frequently encounters the ETT with larger coronal tooth structure destruction. Hence, the applicability of EC protocol in the ET with larger coronal tooth structure loss needs further evaluation. Pissis et al. 10 recommended a 5 mm pulpal chamber cavity for the adequate retention of EC, Chang et al. 11 also used the 5 mm central retention cavity in their study to assess the stress distribution and failure probability of EC crowns. Hence ETT with larger occlusal deficiency was incorporated with 2 mm intra-radicular extension to gain approximately 5 mm of retention area.
The Lithium disilicate (LD) ceramics are preferred in EC fabrication due to the enhanced mechanical strength, strong bonding strength to the tooth structure, and superior esthetic appearance. 12 Recently wide-ranging ceramic materials are developed with different mechanical and esthetic properties to improve the clinical performance and to satisfy the patient esthetic demand. The High-Translucent Zirconia (HTZ) was introduced to eliminate the persistent shortcomings like bone-white opaqueness and fracture of a porcelain veneer. The HTZ with higher flexural strength (600–800 Mpa) 13 and improved optical properties, is a suitable material for EC fabrication. The resin-based ceramic materials were developed to attain the combined mechanical properties of ceramic and polymers, besides attaining compatible modulus of elasticity to dentin. 14 This polymer infiltrated ceramics (PIC) comprises 86 wt% ceramic and 14 wt% polymer. The mechanical properties in bulk are reported with a flexural strength at 130 MPa, fracture toughness at 1.4 MPa, and Vickers hardness similar to enamel. 15
Considering the varied biomechanical behavior of these ceramic materials, comparing the fracture resistance of the EC fabricated from these materials is essential. The influence of Preparation depth and occlusal thickness to the fracture resistance of EC fabricated from various ceramic material is an important research question that needs further investigation. The purpose of this in vitro study was to assess the effect of occlusal thickness, radicular extension, and various ceramic on the fracture resistance of endocrowns in the molar region. The null hypotheses tested were that the fracture resistance and failure type would not be influence by the occlusal thickness, radicular extension, or by the ceramic materials.
Materials and methods
Ninety extracted human sound mandibular molar teeth with approximately similar dimensions were used in this study. They were extracted for periodontal or prosthodontic therapeutic reasons, stored in distilled water until the preparation for the study. The inclusion criteria for the sample teeth were lack of caries, restoration, cracks, or previous endodontic treatment. The institutional ethical review board had approved this study protocol (SRC/ETH/2018-19/089).
Root canal treatment
All teeth samples were root canal treated following conventional protocol. Root canal shaping was finalized with ProTaper Next X2 file (ProTaper, Dentsply Maillefer, USA). The root canals were disinfected with 5 ml of each 1% NaOCI, followed by distilled water irrigation, dried with the paper points. At the conclusion, root canals were obturated with gutta-percha master cone with sealer (AHPlus, DentsplyMaillefer, USA). The coronal access was filled with a temporary filling (Cavit, 3M ESPE, Seefeld Germany) and stocked at 37°C, 100% humidity for 1 week.
The ETT samples were randomly distributed into three groups comprising 30 samples according to the material used for the fabrication. The Group I sample were proposed to be restored with Lithium disilicate (IPS Emax Press, Ivoclar Vivadent, Schaan, Lichtenstein) ceramic, Group II by Polymer infiltrated Ceramic (Vita Enamic, Vita Zahfabric, Bad Säckingen, USA) and Group III with Highly translucent Monolithic zirconia (Ceramill Zolid HT +White, Amann Girrbach AG, Herrschaftswiesen Koblach Austria). Subsequently, teeth samples from each group were divided into three subgroups (
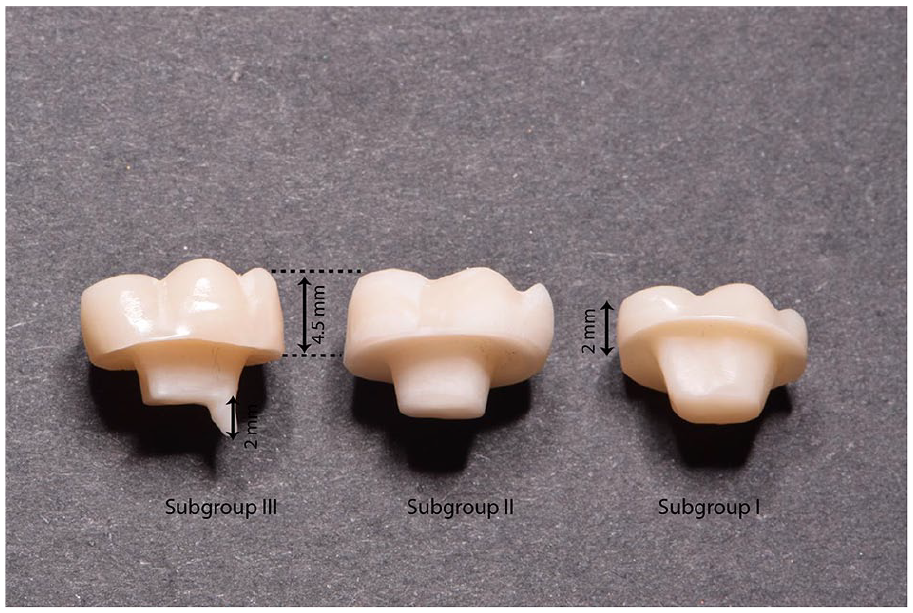
HTZ endocrowns with different occlusal thickness and radicular extension.
Teeth preparation
The ETT were embedded vertically within non-shrink epoxy resin until 1 mm below the cementoenamel junction using silicone mold. The occlusal surfaces were reduced to the pre-defined extent of 2 mm and 4.5 mm according to the subgroups, by verifying with a graduated periodontal probe. The occlusal reduction was accomplished with Tapered Round-end Diamond Bur (856-016, medium coarse, Brasseler, Savannah, GA, USA). The retentive pulp chamber was refined by removing all the undercuts with a tapered diamond bur (856F, Hager & Meisinger GmbH, Neuss, 96 Germany); the uniform taper of 8° was standardized with the parallel milling machine (Bravo, Mariotti, Forli FC, Italy). Average pulp chamber height (retention area) post reduction was 5–5.5 mm for Subgroup I, corresponding values for Subgroups II and III was 3–3.5 mm. The radicular extension was prepared into the distal canal with 2.00 mm depth and 0.9 mm width with pre-calibrated endodontic post drill (Fibrekleer, Pentron clinical, oranage, CA, USA) with a silicone rubber stopper.
Endocrowns fabrication, bonding surface treatment, and adhesive cementation
Materials used in the study are listed in Table 1. ECs from LD ceramic groups were fabricated by the injection technique according to the manufacturer’s instructions. The full anatomical contour wax patterns (Geo classic opak, Renfert, Germany) were made over the teeth samples by a single dental technician. The identical proportion in height from centra groove—pulp floor was confirmed with the digital caliper (fino Pra Ceci caliper; FINO GmbH, Bad Bocklet, Germany). The silicone mold fabricated from the standardized wax pattern was used to replicate the similar occlusal anatomy for all the samples. The wax patterns were pressed with IPS Empress, Programat, EP 5,000 furnace (Ivoclar Vivadent AG Schaan, Liechtenstein) following manufacturers guidelines. The pressed ECs were refined with sandblasting from 100 µm Al2O3 at 1 bar pressure and steam cleaned. Subsequently, washed in an ultrasonic cleaner with distilled water for 10 minutes and were glazed with a single layer neutral shade by firing at 765°C. The endocrowns fabrication from HTZ and PIC were manufactured from Amann Girrbach system (Amann Girrbach AG, Koblach, Austria). The digital impression of the teeth preparations was captured by a laboratory scanner (Ceramill Map, Amann Girrbach AG, Koblach, Austria). The standardized ECs were designed (Ceramill mind, Amann Girrbach AG, Koblach, Austria) at a 2.5% lesser volume for uniform luting cement space; consequently milled with a computer-aided milling machine (Ceramill motion 2, Amann Girrbach AG, Koblach, Austria).
Materials used in the study.

After finishing and polishing the crowns with finishing diamond and rubber polishers (Dialite LD, Brasseler, Savannah, GA, USA), the bonding surfaces of LD and PIC endocrowns were etched with 5% hydrofluoric acid (IPS ceramic etching gel) for 20 and 60 seconds respectively. Post etching, the endocrowns were washed and cleaned in an ultrasonic distilled water bath for 10 minutes. In the end, mono-component silane (Monobond Plus, Ivoclar Vivadent AG, Schaan Liechtenstein) was painted on to the intaglio etched surfaces and allowed to react for 60 seconds, subsequently air-dried. HTZ zirconia endocrowns were prepared with 50 µm Al2O3 air abrasion at 2-bar pressure for 1 minute. Subsequently cleaned in an ultrasonic water bath for 10 minutes.
Enamel surfaces on the prepared teeth samples were selectively etched with 37.5% phosphoric acid (Ultra-Etch, Ultradent Products) for 15 seconds, followed by a water rinse and gentle air-drying. The endocrowns from all the groups were cemented using self-adhesive luting cement (RelyX Unicem2 Automix, 3M ESPE) by applying on to the bonding surface of ECS, and thin layer on to the pulp chamber with extension tip. Excess cement was removed by 2-second tack light curing and a scaler. The ECS were kept under axial static load with 1 kg weight using a specially designed device for 5 minutes. Liquid Strip glycerin gel was applied to all the margins and cured definitively (Elipar S10, 3M ESPE, Seefeld Germany) at 1200 mW/cm² intensity for 20 seconds on each surface. The samples were stored in a humid environment at 37°C for 72 hours before subjecting them to fracture resistance test.
Fracture test, failure and statistical analysis
All the specimens were subjected to 5,000 thermal cyclings (Thermocycler, SD Mechatronik, Feldkirchen-Westerham Germany) in the water at 5° to 55° C, with the dwell time of 30 seconds. The universal testing machine (Instron, Norwood, MA, USA) was used to apply the static load at a crosshead speed of 1 mm/min along the long axis of the tooth (Figure 2). The load was applied using 1.00 mm stainless steel hemispherical tip at occlusal fossa until the fracture. The maximum load at fracture was recorded in newton (N). The failure mode of each specimen was evaluated by observation under the stereomicroscope, 10X magnification (Olympus/DeTrey, Germany). The failure modes were classified according to the fracture pattern.
19
The vertical fracture or fracture below CEJ necessitating the extraction of a tooth in clinical circumstances was categorized as unfavorable. The debonded crown, cohesive fracture, or crack within the crown was characterized as a favorable failure (Figure 3). The recorded data were statistically interpreted with SPSS 19 software (IBM Corporation, Armonk, NY, USA). The data distribution normality was confirmed with the Shapiro–Wilk test. The data values were assessed by one-way ANOVA, followed by Tukey HSD tests with

Testing of samples under universal testing machine.

Failure types in tested samples.
Results
Mean (N) fracture resistance for all the groups is enlisted in Table 2. The highest fracture load for a conventional occlusal thickness of 2 mm was recorded by the HTZ group with 3533.34 N, followed by LD ceramic at 2863.62 N, and PIC ceramic with 1598.63 N. The increased occlusal thickness substantially enhanced the strength of LD ceramic (37770.28) and PIC (2685.85 N) EC. However, the HTZ ceramic EC at 4.5 mm had considerably lesser strength at 1066.92 N. The 2 mm radicular extension with a higher occlusal thickness of 4.5 mm was helpful for both LD ceramic (3877.40 N) and HTZ (2951.84) EC. However, PIC groups had a reduced fracture load at 1936.62 N.
Descriptive statistics of Mean (N) fracture resistance recorded in the different groups.

The Shapiro–Wilk test showed normally distributed data (
One-way analysis of variance of fracture resistance at maximum load (N) between the groups.

The mean difference is significant at the 0.05 level.
LD: Lithium Disilicate; PIC: Polymer infiltrated ceramic; HTZ: High Translucency Zirconia.
Tukey HSD post hoc pairwise comparison for fracture resistance at maximum load between the groups.

The mean difference is significant at the 0.05 level.
The overall failures of LD endocrowns were unfavorable (Table 5); especially with the higher occlusal thickness (80%) and radicular extension groups (100%). However, the failures in the PIC groups were predominantly favorable. The HTZ endocrowns with conventional and 4.5 mm occlusal thickness resulted in a greater percentage of favorable failures at 90–100%. Contrarily radicular extension produced largely unfavorable failures at 90%.
Descriptive statistics of the failure modes in different groups.

Discussion
This in vitro study was aimed to assess the influence of preparation design and various all-ceramic materials on the fracture resistance of EC. The results showed a significant difference in fracture load with different preparation designs and between various all-ceramic materials. Hence both null hypothesis of the study was rejected.
The LD ceramic EC demonstrated the highest fracture resistance compared to PIC and HTZ groups at 4.5 mm occlusal thickness (3770.28 N) and radicular extension (3877.40 N). However, the HTZ ceramic EC displayed better fracture resistance at a lesser occlusal thickness of 2 mm with 3533.34 N. Our results of LD ceramic fracture resistance agree with previous studies; Altier et al. 16 reported the higher fracture resistance of LD ceramic EC at 3320.35 N. similar observation of greater fracture resistance of LD ceramic EC was also reported by El Ghoul et al. 17 under axial loading. The results of our study indicate the improvement in the fracture resistance with an increase in ceramic thickness in both LD ceramic and PIC ceramics. These results are consistent with the reports of Tsai et al. 8 who reported the increased fracture resistance of ceramic crowns at higher thickness. Tribst et al. 20 concurred with the observation of enhancement in fracture load with an increase in thickness, they reported 1570 ± 459 N and 1759 ± 378 N for 1.5 mm and 4.5 mm thickness ECs respectively. Mörmann et al. 7 inferred the higher fracture load values with thick occlusal dimensions among the bonded crowns. The results of the 3D Finite element analysis by Dal et al. 21 indicated the lower concentration of stress with a larger height of the EC under axial load. Dissimilarity in crack initiations with different thickness of ceramic may be attributed to enhanced fracture values. The easy generation and propagation of radial cracks within thinner crowns cause catastrophic fractures, while the cone crack mechanism is predominantly observed in thicker crowns. 22 Harvey et al. 23 suggested that the cone-crack fracture of glass-ceramic restorations requires a higher load leading to bulk fracture.
Our study results showed no statistically significant difference (
The PIC endocrowns showed a lower mean fracture load compared to LD ceramic. However, showed a similar trend of enhanced fracture load with an increase in its thickness. The results are concurrent with the outcomes of Sieper et al. 27 Choi et al. 28 reported the lesser fracture strength of PIC endocrowns compared to LD ceramic endocrowns at a similar thickness and enhanced fracture resistance at increased thickness. The PIC materials exhibit elastic-plastic behavior with creep; display the Dugdale cracking model. 29 The increased fracture load at higher thickness is also attributed to crack bridge zone generation and secondary cracking zone formation. An increase in toughness with crack growth (R-curve behavior) stabilize the crack extension. 30 R-curve behavior became more pronounced with an increasing volume fraction of the more ductile constituent phase. Unlike LD ceramics, the radicular extension had a significant reduction of fracture resistance in PIC ceramics with a mean maximum load recorded at 1936.62 N. This could be ascribed to the increased flexing of restoration and leverage action due to higher crown height. The PIC endocrowns are expected to flex more due to lesser flexural strength and lesser elastic modulus (27.26 GPa). This could lead to increased stress on a tooth, restoration, and tooth-restoration interface. 31 Earlier researchers have reported that the thermocycling decreased bond strength of PIC to the resin luting agent. 32 The reduced failure load in the radicular extension group could be due to the combined effect of increased stress concentration and reduced bond strength. Hence most failures in this group were favorable with the debonding of endocrowns.
The HTZ endocrowns at 2 mm thickness showed the highest mean fracture resistance compared to other groups. This finding matches with fracture resistance of monolithic zirconia reported by Sun et al. 33 They observed the doubling of fracture resistance of monolithic zirconia core from 0.6 mm to 1.5 mm thickness. A similar result of higher fracture load in monolithic zirconia was reported by Dartora et al. 34 Although, numerous surface treatments like airborne abrasion, selective etching, primer applications are suggested to improve bond strength establishing a strong and durable bond of zirconia with resin and the tooth structure is difficult. FEA studies indicate the concentration of tensile stress at the cement interface and in dentin. Consequently, increases the risk of failure by detachment. 35 The lesser fracture resistance of HTZ endocrowns at 4.5 mm thickness could be a combined effect of higher leverage due to the increased height of loading, compromised bond strength, and increased stress at the cement interface. KANAT-ERTÜRK et al. 36 also reported the influence of preparation on the fracture strength is limited only for feldspathic ceramic, no influence on zirconia ceramic endocrowns. However, the 2 mm radicular extension of EC in the HTZ crown showed a significant improvement in fracture resistance. Gulec et al. 37 established the least Von-Mises stress and lesser stress on tooth structure in modified endocrowns with Intra radicular extension. Dartora et al. 34 recommended the Greater extension of endocrowns inside the pulp chamber to reduce induced stresses and to increase the fracture resistance. The mandibular molars restored with the endocrown technique with 2- and 4-mm pulp chamber extensions with greater tooth fracture resistance are also corroborated by Hayes et al. 38 The most unfavorable fractures were observed with LD ceramics with the 2 mm and 4.5 mm occlusal thickness. 3D Finite element analysis reports indicate the concentration of an equivalent Von Mises stress at the interface of restorative material and dentin with an incompatible modulus of elasticity. 39 A greater number of catastrophic failures were also observed in the HTZ endocrowns with radicular extension. The higher modulus of elasticity of LD ceramics (95 GPa) and HTZ ceramics (200 GPa) compared to Dentin (18.6 GPa) could be attributed to the increased unfavorable failures in these groups. These findings are also confirmed with conclusions from earlier researchers.36,38
The Clinical implication of our study results includes, both HTZ and LD ceramics could be effectively used as materials of choice for endocrowns fabrication at the Molar region. Although the radicular extensions seem to improve the fracture resistance HTZ endocrowns, predominantly unfavorable failure modes may act as an impediment for its application in clinical practice.
Limitation of the studies comprised of nonperformance of dynamic forces for testing of endocrowns simulating chewing cycles, no artificial periodontal ligament replication around the root during testing. The authors suggest confirming these in vitro study finding with long term clinical studies in intraoral conditions with the presence of the cushioning effect of periodontal ligament and the modulatory effect of saliva.
Conclusion
Within the limitation of this in vitro study, the following conclusions could be drawn: The endocrowns at conventional 2 mm thickness fabricated from HTZ displayed the highest fracture strength. The LD ceramic was second material of choice with marginally lesser fracture resistance, and showing 50% favorable failure modes.
However, in endodontically treated teeth with extensive occlusal deficiency, the radicular extension should not be performed; the endocrowns could be made up of LD possessing the highest fracture resistance or from PIC having more favorable failure modes.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
