Abstract
Recent advances in microfabrication technologies and advanced biomaterials have allowed for the development of in vitro platforms that recapitulate more physiologically relevant cellular components and function. Microengineered vascular systems are of particular importance for the efficient assessment of drug candidates to physiological barriers lining microvessels. This review highlights advances in the development of microengineered vascular structures with an emphasis on the potential impact on drug delivery studies. Specifically, this article examines the development of models for the study of drug delivery to the central nervous system and cardiovascular system. We also discuss current challenges and future prospects of the development of microengineered vascular systems.
Introduction
The traditional paradigm of tissue engineering involves the combination of isolated patient cells and extracellular matrix proteins to produce an implantable substitute for damaged tissue. In particular, vascular tissue-engineering pursuits include the development of cell-based vascular grafts1,2 and vascularized tissue implants.3–6 The introduction of microfluidic devices has broadened the traditional scope of tissue engineering to include microengineered tissue systems that attempt to reproduce relevant organ physiology. Microfluidic devices offer replicable and cost-effective platforms7,8 on which to study disease states and conduct preliminary drug screening and toxicology studies.9–12 Microfluidics have also been extended to point-of-care devices for patient-specific diagnoses.13–16 In this review, we will overview the key physiological components necessary for accurate in vitro vascular recapitulation and discuss the state-of-the-art microengineered technology available for the study of vascular systems. In vitro models of brain microvessels and arterial lining will be discussed with particular emphasis on the ability of these models to be used for preliminary drug studies.
Vascular Physiology in Relevance to Drug Discovery and Disease
The design of reliable in vitro tissue systems requires an in-depth understanding of the in vivo physiology being recapitulated. Arteries and capillaries are distinguished by several key physiological differences ( Fig. 1 ). Arteries are thick walled, consist of three distinct layers, and are elastic to facilitate the circulation of blood from the heart to target tissues ( Fig. 1A ). Capillaries are thin walled and consist of an endothelial cell monolayer supported by pericyte cells. This thin monolayer of cells facilitates efficient oxygen delivery, nutrient delivery, and waste removal from target tissues ( Fig. 1B ). In both vascular systems, the relative cellular and extracellular components work together to maintain vascular functionality. Development of more physiologically relevant in vitro models to study vasculature has been a rising priority in drug discovery. In the arterial disease atherosclerosis, plaques can occur from the accumulation of foam cells, immune cells, platelets, extracellular matrix (ECM), and fats at damaged endothelial sites. 17 To ensure physiological relevance to arterial vasculature, these components must be taken into consideration in the development of an in vitro model for atherosclerosis.18–22 Notable components that have been studied include endothelial cells, ECM, and platelets.21,23,24 The study of capillary disease manifestation, formation, and maintenance is also significant in the context of drug delivery. For example, the development of drugs for central nervous system (CNS) disorders is particularly challenging because of the specialized capillary microvessels of the blood-brain barrier (BBB; Fig. 1C ). The contributions of several relevant cell types, collectively called the neurovascular unit, are necessary for proper BBB function. Thus, the decision to exclude a component from a simplified in vitro model must be seriously considered in the context of each particular study.
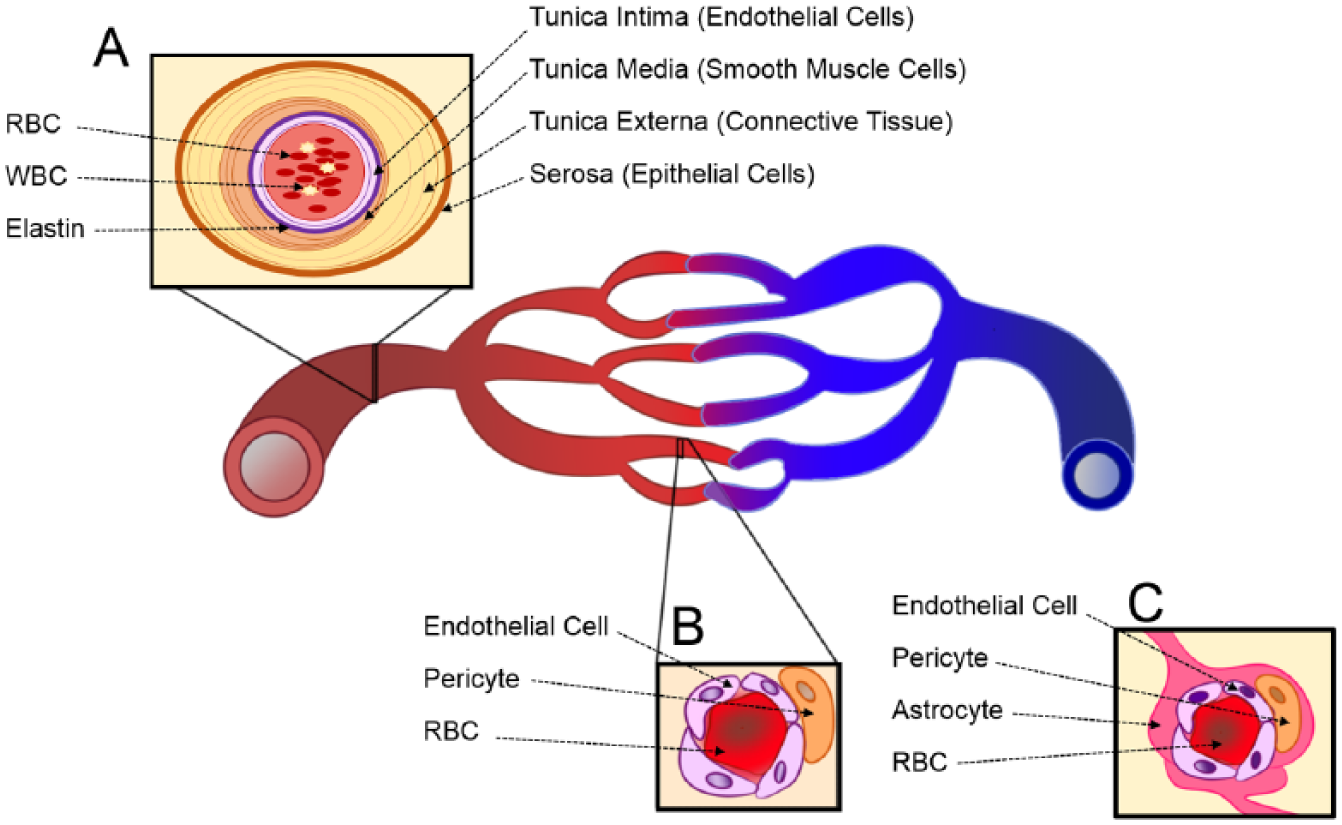
Schematic illustration of vascular systems: (
State-of-the-Art Microengineered Technologies
Drug development is time-consuming and risky. Only 1 in every 10,000 drug candidates make it to market and those that do take well over a decade to develop. 7 The need for animal in vivo verification in determining suitable drugs for clinical trials has remained unchanged. Meanwhile, a rise in in vitro profiling for drug candidates reflects the need to develop suitable in vitro models for various diseases. 25 An abundant pool of microfabrication techniques is being applied for the development of microengineered tissue systems, including photolithography,26–28 micromachining,29–31 three-dimensional (3D) printing,32–34, paper printed devices,35–37 thermoforming,38–40 and wire/needle-based molding. 41 With these technologies, microengineered tissue models can incorporate ECM scaffolds that provide more physiologically relevant microenvironments for cells and tissues.42,43 These approaches provide more cost-effective methodologies for evaluating drug efficacy than time-consuming animal tests, in which drug candidates are evaluated for an extended period of time before being dropped from the study. 44 A high-throughput solution with physiological accuracy would then be desirable for identifying unsuitable drugs, which can reduce the number of animal tests, saving cost and time. Although in vitro technology does not fully recapitulate the complexity of an in vivo system, it remains attractive as a cost-effective alternative to highly variable in vivo studies.
Mircroengineered Vascular Systems
Microvasculature Platforms for Drug Screening: The BBB
The BBB poses a significant challenge to CNS drug delivery by restricting the permeability of molecules from systemic circulation via a variety of specialized endothelial cell processes. Exposure to soluble cues from astrocyte cells induces increased expression of tight junction proteins between neighboring endothelial cells, resulting in limited paracellular diffusion of solutes. Direct interaction with pericyte cells causes the brain endothelial cells to have a decreased number of fenestra and pinocytic vesicles and to exhibit a specialized portfolio of cell surface receptors, culminating in a restriction of transcellular permeability.45–48 These specializations lead to significantly decreased permeability of the brain endothelium to circulating molecules. To promote the efficacy of systemically administered drugs, it is essential to assess the degree to which a drug candidate can effectively cross the BBB in the drug development process.
In vitro models of the BBB provide a cost-effective platform for high-throughput screening in the early stages of pharmaceutical studies. To be a predictive model, an in vitro model of the BBB would ideally recapitulate several key in vivo properties: physiologically relevant shear rates, acceptable barrier confluence indicated by transendothelial electrical resistance (TEER) measurements, relevant expression of tight junction molecules leading to restricted paracellular permeability, physiologically relevant cellular architecture, and functional expression of critical cell surface receptors. More importantly, an in vitro BBB model with these key features must be highly controllable, repeatable, robust, and easy to fabricate with standard methods. Several in vitro tissue systems have been developed for use as platforms to assess the ability of novel drug candidates to cross the BBB.48,49 In particular, microfluidic models have demonstrated promise for use in the fields of drug development and disease study. The following sections compare microfluidic models to other available in vitro BBB models and discuss the challenges preventing widespread adaptation of microfluidic models for use in drug screening and toxicology studies.
The simplest in vitro BBB models are static transwell cultures in which relevant cell types are cultured on the surfaces of a semipermeable porous membrane. These models are easy to culture and readily facilitate TEER measurement with commercially available devices. Transwell cultures can be monocultures of endothelial cells, co-cultures of endothelial and astrocyte cells, or tricultures of endothelial, astrocyte, and pericyte cells. Transwell models are currently the most widely used in vitro models of the BBB because of their ability to accommodate multiplexing for high-throughput study. However, they lack several components of an ideal drug-screening model discussed above. Specifically, static transwell designs do not allow for the direct interaction of cell types or the incorporation of relevant shear flow rates. 49 A subset of static culture systems, such as spheroids and Matrigel angiogenesis assays, 50 fall under the category of microtissue culture systems. These systems allow for detailed examination of direct cellular interaction on relevant length scales but do not easily facilitate TEER measurement or flow incorporation.
Several techniques can be used to incorporate shear stress in an in vitro device. Cone plate viscometers can be added to transwell culture systems 49 or cells can be seeded on a substrate for use in a parallel plate flow chamber. 51 The Janigro Laboratory has designed several iterations of a novel dynamic in vitro BBB device using hollow polypropylene fibers to mimic microvessels. Although this model reports the most physiological TEER values to date (1000 Ω·cm2 compared with 2000–4000 Ω·cm2 for in vivo BBB) and has been successfully used in studying transendothelial trafficking of immune cells, 52 many literature sources deem it unsuitable for high-throughput pharmacological studies. Reasons cited include the large number of cells needed to load the device, the necessity of specific technical skills to establish the model, and the inability to conduct nondestructive microscopy.53,54
Recent advances in microfabrication techniques have allowed for the development of microtissue engineered BBB models capable of incorporating flow. Microfluidic models provide distinct advantages by allowing for nondestructive microscopy of cellular interactions on relevant length scales in the presence of physiologically relevant shear rates. In addition, by downsizing the device setup, microfluidic devices require fewer cells and reagents, translating into better cost efficiency. In the most common microfluidic configurations, cells are cultured on semipermeable membranes at the interface of two microchannels made from polydimethylsiloxane that are supplied with media flow. 55 These models have been redesigned and altered to include electrodes for TEER measurements.54,56 Several variations of this general device structure have been published. 53 Prabhakarpandian et al. 55 developed a model with two side-by-side compartments separated by regularly spaced (3 µm) pillars in which RBE4 endothelial cells seeded on the apical side are exposed to astrocyte-conditioned media on the basolateral side to simulate the presence of astrocyte cells and induce the expression of relevant tight junction proteins. Incorporating platinum electrodes for TEER measurements, Griep et al. 56 proposed a similar device by seeding hCMEC/D3 endothelial cells on a semipermeable membrane between two microchannels. This approach reported physiological barrier changes in TEER measurements in response to mechanical stimuli in the form of flow administration and biochemical stimuli in the form of tumor necrosis factor–α (TNF-α) administration. 56 Yeon et al. 57 proposed a different model of the BBB in which culture time was greatly reduced. Human umbilical vein endothelial cells (HUVECs) were trapped in microholes via a pressure gradient and incubated with astrocyte-conditioned media for as few as 2 h before drug permeability studies were conducted ( Fig. 2A–C ). Physiologically relevant shear rates were observed, and immunofluorescence staining revealed a slightly discontinuous expression of tight junction proteins. The permeability for several drugs was shown to be comparable with those measured with other conventional methods. 57 Booth and Kim 54 have proposed the most comprehensively characterized microfluidic model to date ( Fig. 3C , D ). In this model, b.END3 brain endothelial cells and C8-D1A astrocyte cells are cultured on either side of an ultrathin semipermeable membrane between two microfluidic flow chambers. Co-culture with astrocyte cells under flow conditions increased the TEER to more than 250 Ω·cm2 after 3 d of culture. Low permeability to tracker molecules was reported and verified by histological staining that showed a continuous membrane. 54 While microfluidic BBB models provide a marked improvement over static culture models, they have yet to see widespread implementation in the drug development process. This can be attributed to a number of factors including technological expertise needed for design and operation of devices, relatively high cost of model establishment, and insufficient multiplexing for high-throughput studies. 53
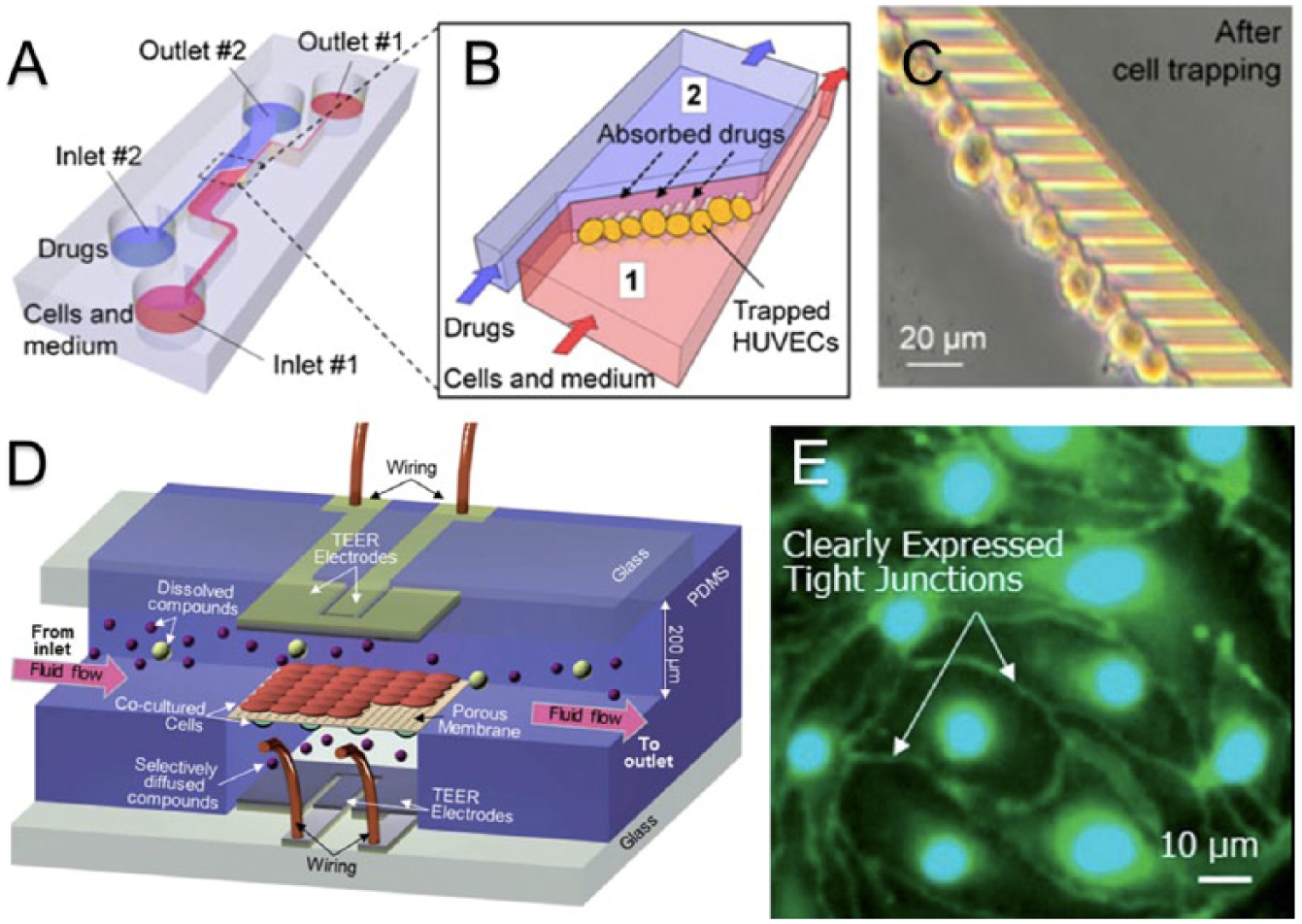
In vitro models of the blood-brain barrier (BBB) for permeability studies. (
(
Microvasculature Platforms for Drug Screening: Arterial Lining
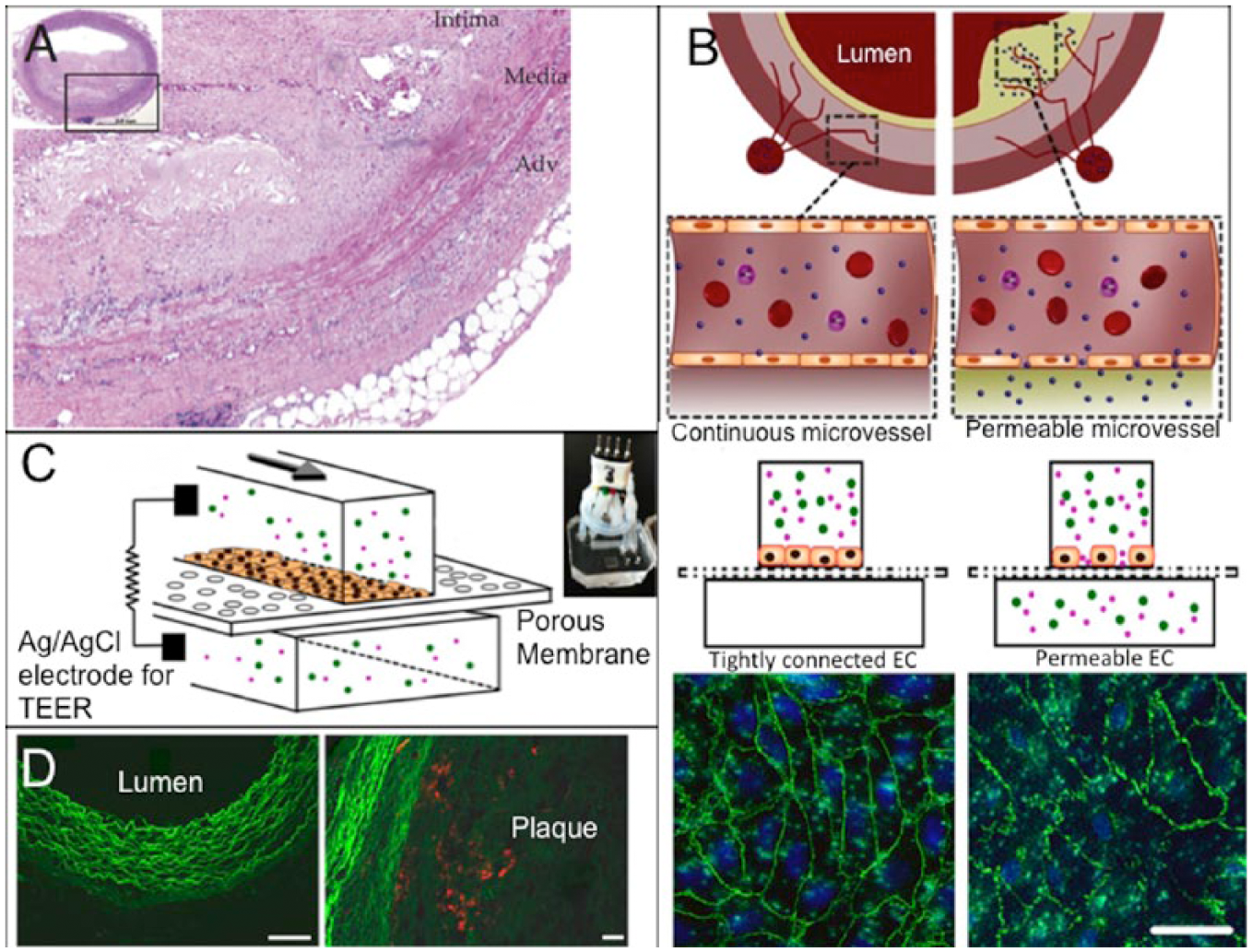
Cardiovascular disease (CVD) accounted for more than 30% of all deaths in the United States in 2010. 59 In atherosclerosis, one of the most common manifestations of CVD, the dysfunctional endothelium causes a chronic inflammatory response, 19 leading to increased endothelial permeability. The subsequent aggregation and introduction of platelets and leukocytes to the dysfunctional endothelium result in intimal thickening and occlusion. 60 Although animal models for atherosclerosis have been used for drug development,61–63 microengineered in vitro vascular systems that can mimic microvessels in atherosclerotic regions ( Fig. 3A ) have started to demonstrate potential for evaluating drug candidates. Estrada et al. 64 were able to replicate atherosclerotic flow conditions to induce endothelial dysfunction. The model featured an elastic membrane on which human aortic endothelial cells (HAECs) were exposed to cyclic strains ranging from 5% to 10% and to oscillatory flow patterns with low shear stresses of approximately 1.3 dynes/cm2, both of which are pertinent in atherosclerosis. 64 Disturbed flow resulted in an increase in cell shape deformation and misalignment of nearly 60% in both cases. Kim et al. 21 developed an endothelialized model that allowed the investigation of the relationship between the permeability of an endothelial monolayer and the nanoparticle translocation across the permeable endothelium ( Fig. 3B , C ). This study focused on a potential pathway for drug delivery to plaque in atherosclerosis by mimicking the permeable endothelium of microvessels surrounding the arterial vessel or penetrating into the plaque.18,58 The device was fabricated through assembling a porous elastic membrane with upper and lower channels. A monolayer of HUVECs was grown onto the porous polymer membrane, and the monolayer permeability was measured using silver/silver chloride (Ag/AgCl)65,66 electrodes on either side ( Fig. 3C ). To mimic the permeable conditions of microvessels residing in atherosclerotic plaques, endothelial cells in the device were exposed to a combination of low shear stresses and the inflammatory mediator TNF-α. In addition, this study used two different nanoparticle types, Cy5.5-lipid-PLGA and Cy7-albumin, to examine the relationship between the endothelial permeability (via the albumin translocation) and the lipid-PLGA nanoparticle translocation in the in vitro microchip and an in vivo rabbit model of atherosclerosis. This work found that the nanoparticle translocation across the endothelial layer was highly dependent on the endothelial permeability in both the in vitro and in vivo models ( Fig. 3D ). Such studies demonstrate the feasibility of microfluidic models for the examination of potential drug delivery mechanisms for CVD.
Occlusions that can arise from atherosclerosis and progress into thrombosis are part of an essential point of investigation in vascular disease prevention and treatment. Platelets that aggregate to form such occlusions are often exposed to a range of shear rates (greater than 4000 s−1) or chemical factors that can cause activation and occlusion at inflamed sites. 20 Recent approaches using endothelial cells cultured in 3D vascularized microfluidic chips have demonstrated the ability to mimic the dynamics of platelet aggregation. Zheng et al. 24 developed a model that used a patterned collagen gel as a substrate for HUVECs to form a complete vascular network ( Fig. 4A ). The network was used to study angiogenesis and whole blood–endothelium interactions with applications to thrombosis. Von Willebrand factor, a platelet-binding protein that can be released from endothelial Weibel-Palade bodies, in combination with phorbol-12-myristate-13-acetate (PMA), was used in the thrombosis study to stimulate platelet aggregation. Aggregates grew over the course of 250 s to nearly occlude the PMA stimulated vessels while nonstimulated vessels did not form such aggregates. Tsai et al. 23 featured a model using whole blood flowing through bifurcations in microfluidic devices seeded with either HUVECs or human lung microvascular endothelial cells (HLMVECs; Fig. 4B ). 23 In this study, HLMVECs were activated with the inflammatory mediator TNF-α to stimulate the coagulation of the blood, and HUVECs were used in conjunction with a toxin called STX2 to induce hemolytic-uremic syndrome to form thrombotic lesions. These approaches resulted in occlusion formation through platelet aggregation, showing the ability to reproduce multiple types of thrombus formations ( Fig. 4B ). Both studies successfully stimulated thrombotic lesions to form 3D models, helping to elucidate the pathogenesis behind thrombotic complications in vascular disease.
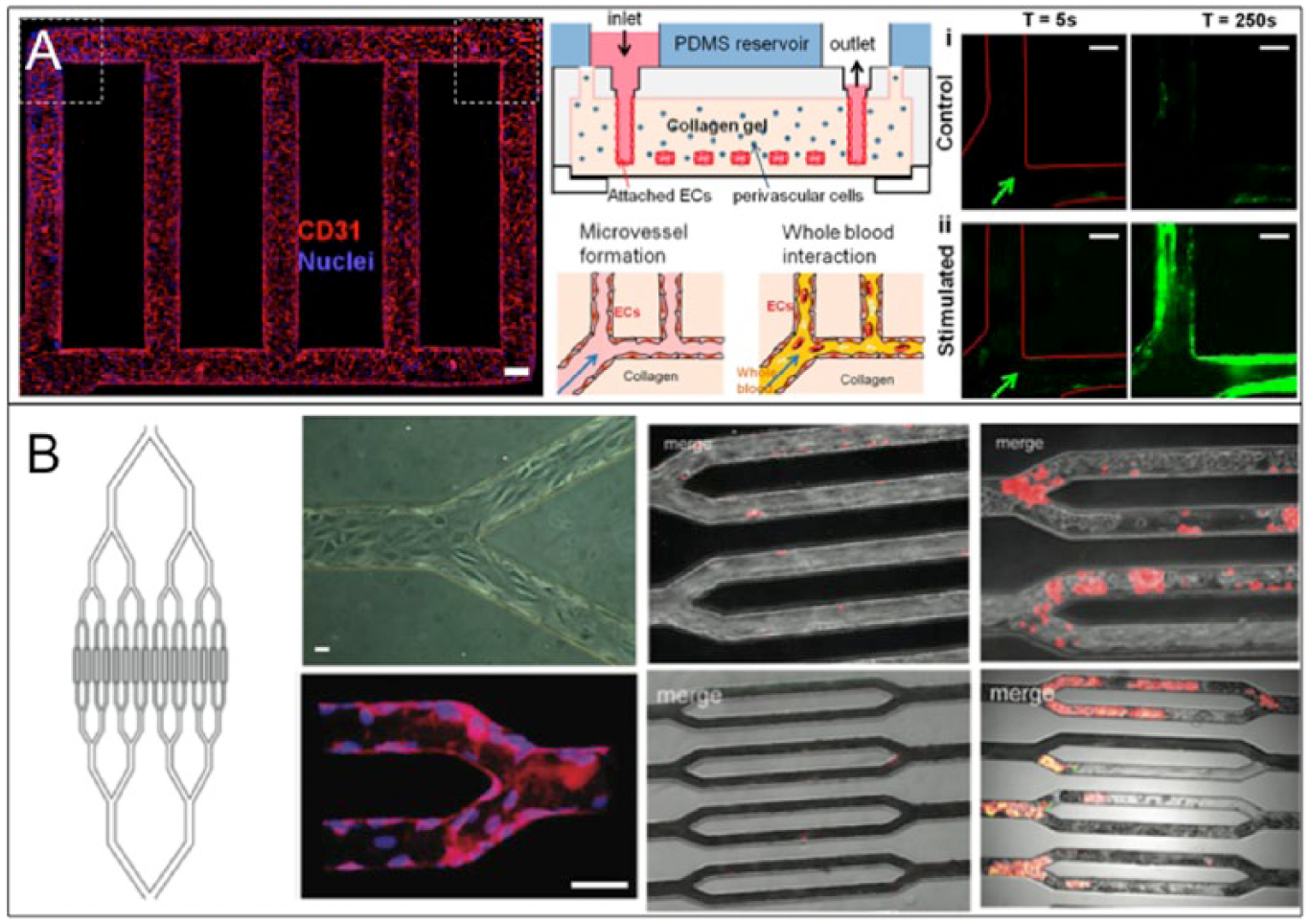
(
Future Prospects
Microengineered tissue systems have demonstrated potential for use in disease- and drug-related studies. In addition, they provide a unique opportunity for detailed examination of phenomena that are hard to observe in vivo. In vitro systems are constantly questioned for their accuracy because of their simplicity compared with the inherent complexity of in vivo models. 67 Recent advances in microfabrication have allowed for the development of more physiologically relevant in vitro systems. These in vitro microsystems can provide a better solution to balance simplicity and physiological relevance. 68 The balanced model systems have the potential to accelerate research toward the successful integration of different microsystems for expanded in vitro studies. Although the idea of integrating multiple in vitro micro-organ systems together is by no means a new one,69–72 the technical limitations preventing implementation of such a system have yet to be overcome. To a degree, microengineered organ systems have been developed to study disease-relevant suborgan systems.73–76 Recent improvements to microfluidic technologies may stir the development of better high-throughput devices that can represent physiological function for greater impact in drug development.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
