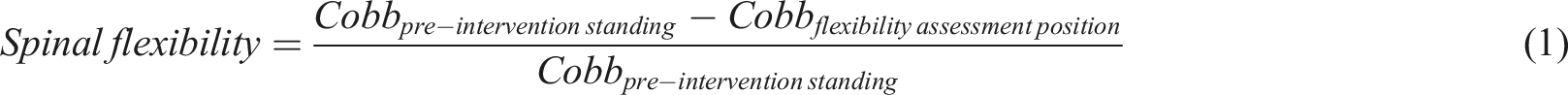Abstract
Study Design
Systematic Review and Meta-analysis.
Objectives
This systematic review and meta-analysis aimed to: (1) synthesize the prevalent application ratios of 2 radiographic spinal flexibility assessment methods in AIS patients treated with PSF or bracing; and (2) quantitatively evaluate the accuracy of these methods in predicting post-intervention correction outcomes.
Methods
A systematic search was conducted across 5 electronic databases: CINAHL, Embase, Ovid, PubMed, and Web of Science. Meta-analyses were performed to investigate the accuracy of the spinal flexibility rate in predicting the post-intervention correction rate in AIS patients treated with PSF surgery or bracing, using RevMan 5.4.1 software.
Results
The results of 31 studies, involving 1868 AIS patients, showed that the side-bending method was utilized more frequently than the fulcrum-bending method in both treatments. Meanwhile, the spinal flexibility evaluated by the fulcrum-bending method may provide a more accurate prediction of post-surgical correction compared to the side-bending approach, particularly for main curves. For the bracing treatment, only a few studies have preliminarily reported good capability of the side-bending method in predicting the initial in-brace correction.
Conclusions
This review quantitatively assessed the clinical application ratio and effectiveness of side-bending and fulcrum-bending radiographs in predicting post-intervention curve corrections in AIS patients undergoing surgical or bracing treatments. The results of the current review supported to adopt the fulcrum-bending approach for AIS patients undergoing PSF surgery with main thoracic curves, and the side-bending approach for those with thoracolumbar/lumbar curves. For patients receiving bracing treatment, further research is still needed to confirm the clinical value of the side-bending method.
Keywords
Introduction
Adolescent idiopathic scoliosis (AIS) is a complex spinal deformity affecting 1% to 3% of children aged 10 to 16 years. 1 It is diagnosed with the Cobb angle of the spinal curve exceeds 10° in the coronal plane. 2 For scoliotic curves between 20° and 45°,3,4 the conservative bracing treatment is commonly prescribed 5 to minimize the risk of curvature progression6,7 and to avoid surgery. 8 For AIS patients with Cobb angles greater than 45°, spinal surgery is needed, 9 with posterior spinal fusion (PSF) as the preferred treatment option for most cases.2,9
Spinal flexibility is a critical parameter in both conservative and surgical treatments of AIS, in terms of predicting the initial in-brace correction and progression in AIS patients,3,4 and the surgical correction in PSF surgery.2,10 It is calculated as follows:
11
where
Various methods have been used to assess the scoliotic curvature flexibility of patients with AIS. Common clinical physical examinations included Sit and Reach Test, 12 Lateral Bending Test, 13 and Trunk Rotation Test, 14 to assess treatment outcomes.15-19 To predict the post-intervention correction, imaging techniques with greater reliability and accuracy are required, including the radiographic methods of traditional X-ray 20 and the EOS stereo-radiography system, 21 and the radiation-free imaging techniques of ultrasound imaging. 22 The testing positions in these methods are diverse, encompassing unassisted positions of supine, 23 supine/prone with lateral side-bending, 24 and prone 25 ; and externally assisted positions of supine, prone, side-lying, or erect, via manual traction, 26 mechanical pushing, 27 the use of a fulcrum, 28 or suspension. 29
So far, the radiographic-based assessment of scoliotic spinal flexibility remains the dominant method, particularly for the side-bending and the fulcrum-bending methods. 20 The side-bending method, introduced by Moe, J. H., 30 has long been regarded as the “golden standard” for the spinal flexibility assessment. However, with the improved surgical curve correction using the pedicle screw instrumentation system,31,32 the side-bending approach appears to no longer estimate the effects of surgical correction accurately. 33 Recently, there has also been growing attention to use the side-bending method to assess the spinal flexibility of AIS patients with moderate curvature undergoing bracing treatment.34,35 However, its application remains limited, with its predicting effects in these patients remained inconclusive. Meanwhile, the Fulcrum-bending radiographic method, as introduced by Cheung and Luk, allows for a simple and accurate assessment of spinal flexibility without requiring patient’s effort. 28 Its application has increased in recent years, with some studies suggesting that it could predict the post-operative curve correction better than the side-bending approach in AIS patients undergoing PSF surgery.36-38 However, 1 previous study found that none of the supine, side-bending, push-prone, or fulcrum-bending methods could accurately predict the curve correction in main thoracic and thoracolumbar/lumbar curves. 23 Controversy still remains regarding the preferred assessment method in clinical practice.
Several reviews have synthesized the predicting value of various spinal flexibility assessment approaches in AIS patients. He, C. and Wong, M. S. 39 provided a qualitative comparison of existing methods for estimating post-surgical correction, but did not specify the involved surgical techniques. In contrast, Khodaei, M. et al 20 focused solely on PSF surgery, and investigated the distribution and predicting capability of various radiographic methods in AIS patients. However, neither review offered precise data on the method differences or detailed clinical advice for selecting the best assessment method for AIS patients based on different curve locations and severities.
Therefore, a research gap still exists in the quantitative comparison of the predicting accuracy of post-intervention curvature correction between the side-bending and fulcrum-bending methods. There has also been limited evidence for AIS patients with different curve locations (eg, proximal thoracic, main thoracic, and thoracolumbar/lumbar curves 40 ) and curve magnitudes (eg, moderate and severe curvatures). Additionally, with the increasing usage of the fulcrum-bending method in recent years, the usage distribution or application ratio of this method should also be reinvestigated to update the information. Filling these research gaps could help synthesis the existing evidence and guide the future clinical practice for AIS patients with different conditions.
To the best knowledge of the authors, this systematic review and meta-analysis is the first study to quantitatively analyze and compare the accuracy of the fulcrum-bending and side-bending methods in predicting the actual correction rate after intervention in AIS patients receiving bracing and surgery treatments. It aimed to: (1) explore the application ratio/proportion of the side-bending and the fulcrum-bending approaches; and (2) quantitatively assess the accuracy of the side-bending and the fulcrum-bending method in predicting the actual post-intervention correction outcomes, in AIS patients who underwent PSF or bracing treatment.
Methods
The protocol of this systematic review and meta-analysis was registered on the International Prospective Register of Systematic Reviews (PROSPERO) 41 with a registration ID: CRD42022363674. The review was conducted following the guideline of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses 2020 statement (PRISMA2020). 42
During the information processing, 2 reviewers (Y.Y. and T.M.) conducted the eligibility assessment, data extraction, study quality assessment, and the evaluation of the quality of evidence independently. In cases of evaluation disagreement, 2 reviewers did separate reassessments and discussions until the agreements/conclusions were reached.
Information Sources
The systematic literature search was conducted from inception to September 2022 in the following electronic databases: CINAHL, Embase, Ovid, PubMed, and Web of Science. In the search procedure, medical topic headings (MeSH) and keywords containing textual terms relevant to the scope of this research were used. 43 The literature search was conducted using the following keyword phrases and subject headings: (idiopathic scoliosis OR scoliotic) AND (bracing OR brace OR spinal fusion OR spondylodesis OR spondylosyndesis) AND (flexibility). To supplement the search results, the references and citation lists of relevant studies were manually searched. 42 After completing the manuscript, 1 more recent literature search following the same procedure was conducted in November 2024, to screen and identify if there were any newly published studies that fulfill the inclusion and exclusion criteria of this review.
After excluding the duplicates, the title and abstract were preliminarily screened for relevance. Studies relevant to spinal flexibility assessment methods, posterior spinal fusion surgery, or bracing treatment in AIS patients were identified for full-text retrieval.
Eligibility Criteria
The inclusion criteria were as follows: (1) patients with AIS and the mean age when under treatment should not be older than 18 years old; (2) patients with AIS who underwent the PSF or bracing treatment; (3) the study contained the side-bending radiograph and/or the fulcrum-bending radiograph as the assessment method for the spinal flexibility rate; (4) the study contained radiography parameters both before/pre- and after/post- the intervention; and (5) the study provided the original data or the mean & standard deviation (SD) of the pre-intervention flexibility rate and the post-intervention correction rate.
The exclusion criteria included: (1) the study was a case report, case series, review, or abstract; (2) the study contained several kinds of scoliosis illnesses and had no single group of AIS patients; and (3) patients received the previous treatment which might affect the results of the PSF or bracing intervention.
Data Extraction, Quality Assessment and Data Synthesis
The data collected from eligible studies to acquire information regarding the homogeneity of the study were: (1) paper’s general information (first author, year of publication, and study design), (2) participants’ baseline information (sample size, mean age at treatment, gender, and curve type), (3) utilization of the assessment method of the spinal flexibility rate, (4) received treatment, and (5) original data (Cobb angle measured before and after the treatment) or mean & SD data on the flexibility rate and the correction rate. Data were extracted for both pre-intervention and post-intervention.
According to the result of the eligibility evaluation, all included studies were observational studies. Therefore, the Newcastle-Ottawa Scale (NOS) quality assessment tool was used to investigate the potential bias in the studies and the quality of research for eligible papers, which is 1 of the most frequently employed approaches for assessing the risk of bias (ROB) in observational research. 44 Three categories were included in the assessment tool as selection, comparability, and outcome. This assessment tool employs a “star system” for scoring each article. The quality of articles was classified according to the number of stars that the article received with the following criteria: low quality (0 to 3 stars), moderate quality (4 to 6 stars), high quality (7 to 9 stars).
Meta-analyses were performed using RevMan 5.4.1 software provided by the Cochrane Collaboration. Continuous variables were expressed as the mean difference (MD) and the SD. For studies that only provided the original data on the Cobb angles, the required mean value and SD in the flexibility rate and the correction rate were calculated by 2 reviewers (Y.Y. and T.M.). If subgroups in 1 study contained the mean and SD values of the aforementioned target data, the data from these subgroups were combined into a single group when applicable. Statistical significance was defined as a probability of P = 0.05 in the overall effect Z test. Given the diversity of the included studies and their non-randomized study designs, a high level of heterogeneity was anticipated. Therefore, the random-effects meta-analysis approach was selected in the meta-analysis. 45 The I2 test was used for heterogeneity measurement. According to Cochrane handbook, 45 I2 values of 0% to 40%, 30% to 60%, 50% to 90%, and 75% to 100% were represented as not be important, moderate heterogeneity, substantial heterogeneity, and considerable heterogeneity, respectively. Publication bias was not reported according to the advice from the Cochrane Handbook, 45 as it was demonstrated that there was insufficient proof of the effects of publication bias in non-randomized studies.
Studies were divided into 2 primary groups based on the 2 types of treatment (ie, PSF and bracing) that AIS patients had undergone for data synthesis. In each study group, the secondary categories were the types of measured curves that were described in articles: proximal thoracic, main thoracic, and thoracolumbar/lumbar curves. In each curve category, meta-analyses were conducted according to the different time points of measuring correction rate: (1) immediate correction rate (measured within 4 weeks post-intervention); (2) follow-up correction rate (measured beyond 4 weeks post-intervention). In the category that the number of studies included was not enough for a meta-analysis, the narrative language was used for qualitative outcome synthesis.
The quality of evidence of the included studies was assessed by the “Grading of Recommendations, Assessment, Development and Evaluation (GRADE)” approach. 46
Results
Literature Searching
In the 5 databases of CINAHL, Embase, Ovid, PubMed, and Web of Science, a total of 1891 articles were identified from the beginning until September 2022. After removing the duplicated 926 items, the full texts of 111 of the remaining 965 records were retrieved for further analysis. After eliminating 11 items for which the complete texts were unavailable, 100 full-text articles were assessed for inclusion eligibility. The reasons for exclusion included no utilization of the side-bending or fulcrum-bending methods (n = 32), no pre- and post-intervention radiographs (n = 15), and no mean and SD data on the flexibility rate or the correction rate (n = 24). One additional study was added after the reference/citation searching. One additional study fulfilling the inclusion/exclusion criteria was identified during the more recent literature retrieval that was conducted in November 2024. Finally, a total of 31 studies met the inclusion criteria and were included in this review. Figure 1 displays the flowchart of the study review and selection process. PRISMA 2020 Flowchart for the inclusion process of the studies in the systematic review and meta-analysis. Note: CR, correction rate; FBR, fulcrum-bending radiograph; FR, flexibility rate; SBR, side-bending radiograph.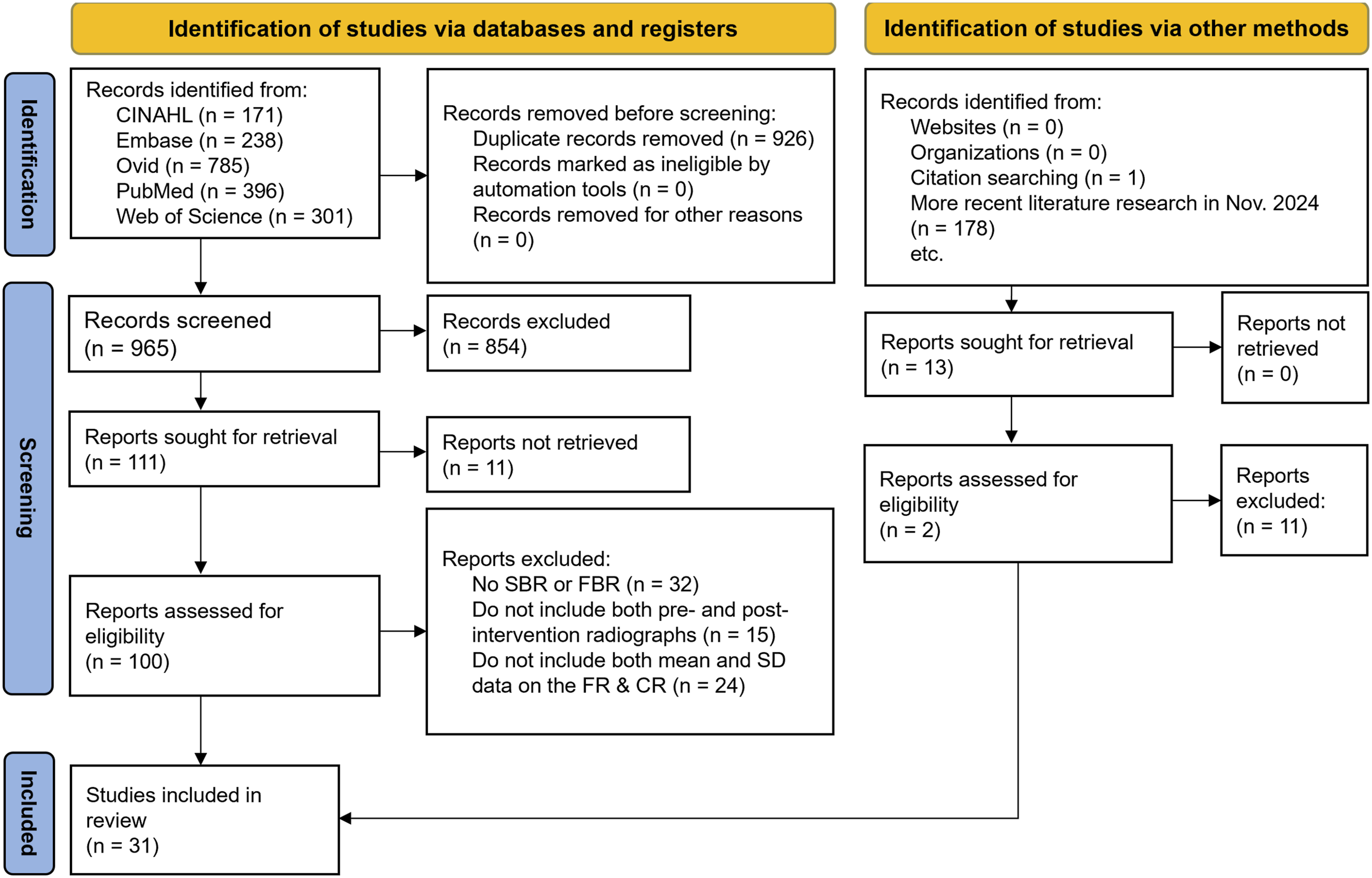
Study Characteristics
Study Characteristics of the Included Studies (n = 31).
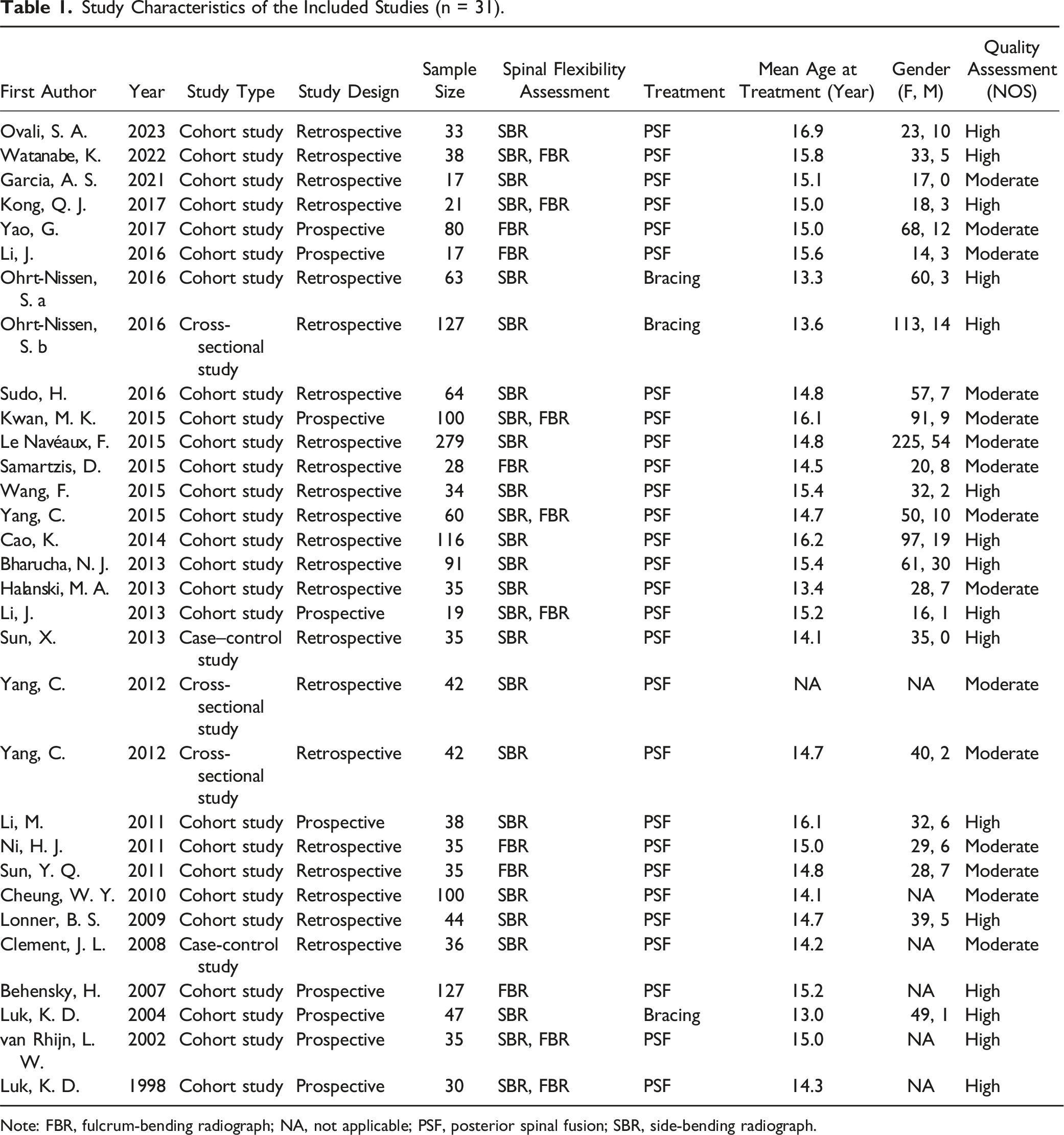
Note: FBR, fulcrum-bending radiograph; NA, not applicable; PSF, posterior spinal fusion; SBR, side-bending radiograph.
Due to the limited number of articles included in the categories of proximal thoracic and thoracolumbar/lumbar curve-relevant studies, 2 fulcrum-bending studies that included 46 AIS patients were excluded from the meta-analysis. Therefore, a total of 1822 patients from 29 studies were included in this meta-analysis. The side-bending method was used in the PSF studies at a percentage of 78.6% (22/28), while the fulcrum-bending method was used at a percentage of 46.4% (13/28). Seven PSF studies contained both the side-bending and the fulcrum-bending methods in their research (25%, 7/28). All 3 bracing-related studies used the side-bending method as their spinal flexibility assessment method (100%, 3/3).
Quality Assessment Results
Quality of the Included Studies (n = 31).
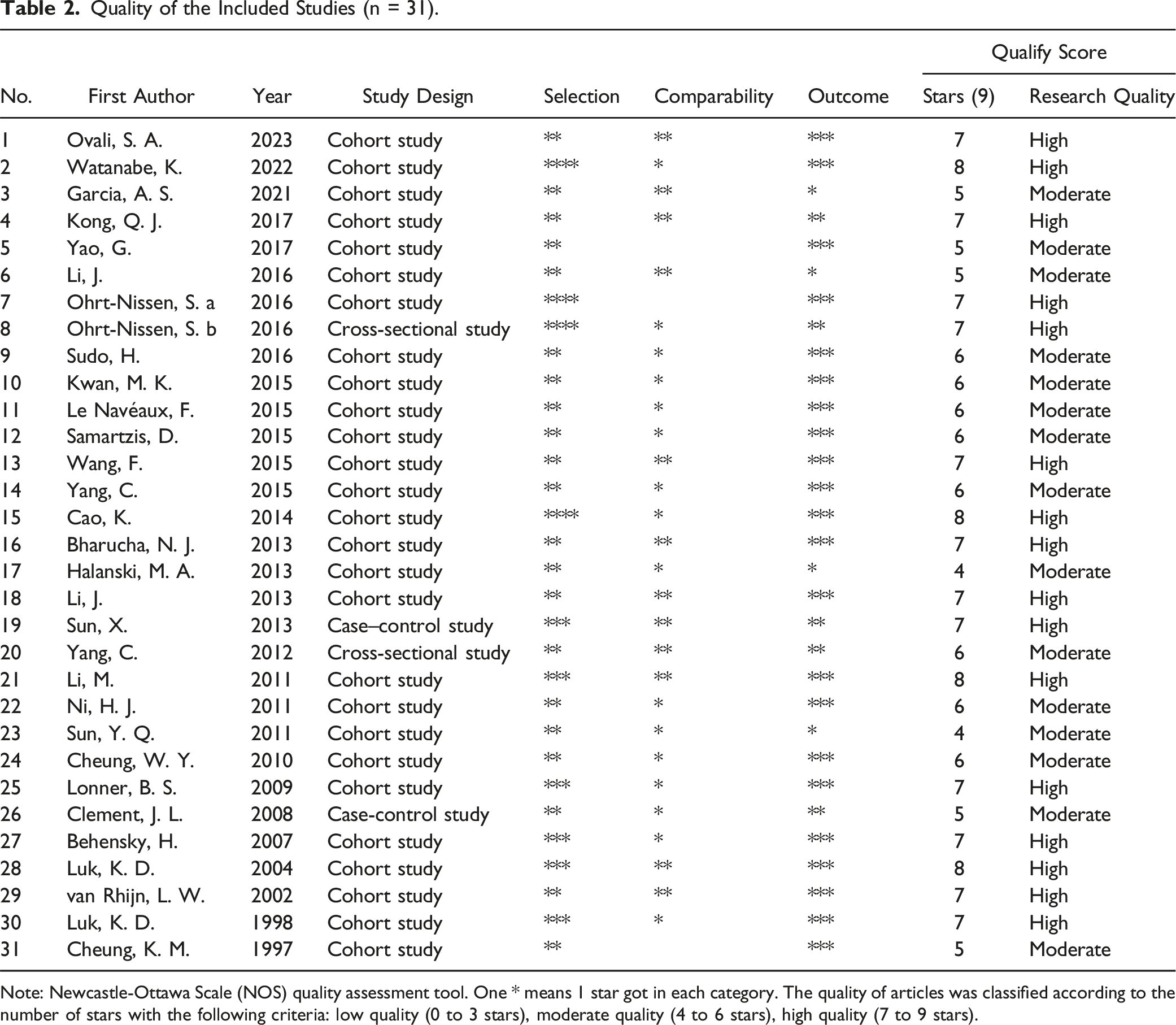
Note: Newcastle-Ottawa Scale (NOS) quality assessment tool. One * means 1 star got in each category. The quality of articles was classified according to the number of stars with the following criteria: low quality (0 to 3 stars), moderate quality (4 to 6 stars), high quality (7 to 9 stars).
Clinical Outcomes
Primary Findings
Figure 2 summarized the primary outcomes of the meta-analyses for included studies, including (1) the comparison of the flexibility rates assessed by the fulcrum-bending and the side-bending methods; (2) the predicted value of the fulcrum-bending and side-bending methods for main thoracic correction after the PSF surgery. The specific information on the meta-analysis for each outcome was reported in Supplemental Material 2. The primary outcomes of the meta-analyses for included studies. Note: This figure was produced according to the outcomes from the meta-analyses which were produced by the RevMan 5.4.1 software provided by the Cochrane Collaboration. The specific information on the meta-analysis for each outcome is in Supplemental Material 2. ◆: Pooled mean difference; error bar: 95% confidence interval. FB, fulcrum-bending radiograph; MT, main thoracic; SB, side-bending.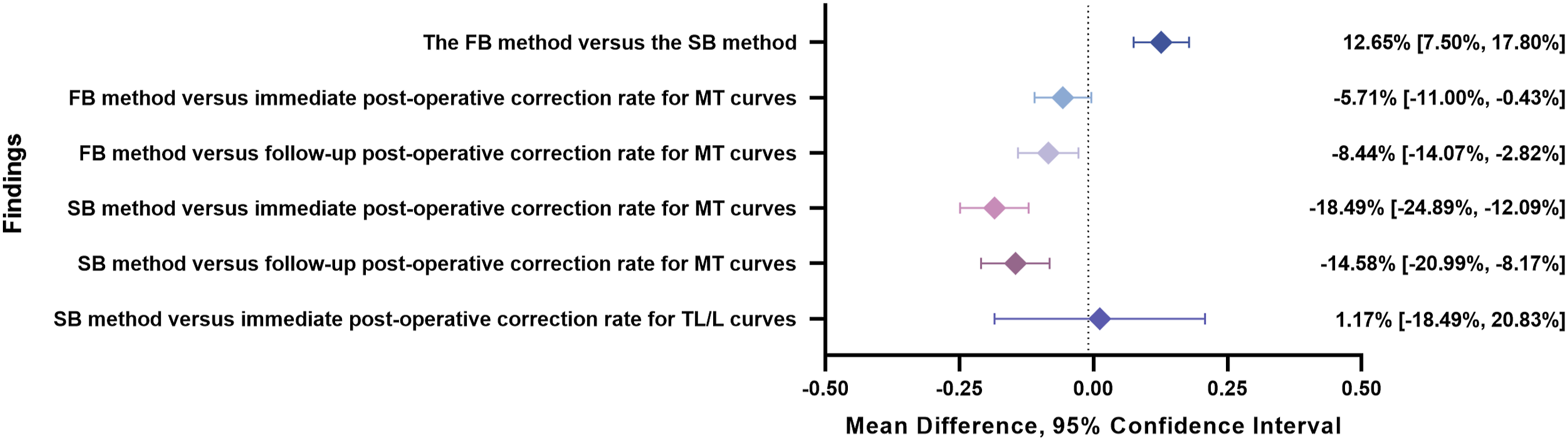
PSF Studies.
Comparison Between the Fulcrum-bending and the Side-bending Methods for Main Thoracic Curves Flexibility in AIS Patients.
A total of 5 studies33,37,38,47,48 providing the flexibility rate data that measured by the fulcrum-bending or side-bending methods were included in the meta-analysis (Supplemental Material 2a). Based on the pooled data from 230 patients, the flexibility rate measured by the fulcrum-bending method was significantly higher than those measured by the side-bending method, with an MD of 12.65% (95% CI: 7.50% to 17.80%, P < 0.001). There was substantial heterogeneity between studies (I2 = 50%).
Accuracy of the Fulcrum-bending Method in Estimating the Immediate Post-operative Correction Rate for Main Thoracic Curves in AIS Patients.
There were ten studies28,38,47-54 presented the fulcrum-bending flexibility rate, and the immediate post-surgical correction rate for main thoracic curves in AIS patients (Supplemental Material 2b). According to the pooled 399 sets of comparable data, the measured fulcrum-bending flexibility rate was significantly lower than the immediate post-surgical correction rate, with an MD of −5.71% (95% CI: −11.00% to −0.43%, P = 0.03). With similar pooled sample sizes, the fulcrum-bending method might show smaller predicting errors than the those of side-bending method (as described in the following section), when comparing the spinal flexibility rate to the actual immediate post-surgical correction rate. Significant heterogeneity between studies was reported (I2 = 82%).
Accuracy of the Fulcrum-bending Method in Estimating the Follow-up Post-operative Correction Rate for Main Thoracic Curves in AIS patients.
The meta-analysis included a total of 6 studies33,37,49,50,52,55 that examined the fulcrum-bending flexibility rate and the follow-up post-surgical correction rate for main thoracic curves (Supplemental Material 2c). The follow-up time ranged from 24 to 52 months. The pooled data from 298 patients illustrated that the fulcrum-bending flexibility rate was significantly lower than the actual follow-up post-surgical correction rate with an MD of −8.44% (95% CI: −14.07% to −2.82%, P = 0.003). Compared to the side-bending method, the flexibility rate that measured using the fulcrum-bending method might show fewer predicting errors in comparison with the actual follow-up correction rate (as described in the following section). Considerable heterogeneity was found between studies (I2 = 82%).
Accuracy of the Side-bending Method in Estimating the Immediate Post-operative Correction Rate for Main Thoracic curves in AIS Patients.
A total of eleven studies28,38,47,48,54,56-62 that provided the flexibility rate as measured by the side-bending method and the immediate post-surgical correction rate were included in the meta-analysis (Supplemental Material 2d). Based on the pooled data from 349 patients, the side-bending flexibility rate was significantly lower than the immediate post-surgical correction rate for main thoracic curves, with an MD of −18.49% (95% CI: −24.89% to −12.09%, P < 0.001). Considerable heterogeneity was presented between studies (I2 = 89%).
Accuracy of the Side-bending Method in Estimating the Follow-up Post-operative Correction Rate for Main Thoracic Curves in AIS Patients.
The meta-analysis included thirteen studies33,57,59-61,63-69 that provided data on the side-bending flexibility rate and the follow-up post-surgical correction rate for main thoracic curves in 1021 AIS patients (Supplemental Material 2e). The follow-up time ranged from 1.5 to 82 months. The pooled data demonstrated that the side-bending flexibility rate was significantly lower than the follow-up correction rate with an MD of −14.58% (95% CI: −20.99% to −8.17%, P < 0.001). Heterogeneity was significant (I2 = 96%).
Accuracy of the Side-bending Method in Estimating the Immediate Post-operative Correction Rate for Thoracolumbar/lumbar Curves in AIS Patients.
The meta-analysis comprised 5 studies57,58,61,62,70 that reported the side-bending flexibility rate and the immediate post-surgical correction rate (Supplemental Material 2f). The side-bending flexibility rate demonstrated a good prediction of the immediate post-surgical correction for thoracolumbar/lumbar curves, according to the pooled data from 96 patients. No significant difference between the flexibility rate and the immediate post-surgical correction rate was found with an MD of 1.17% (95% CI: −18.49% to 20.83%, P = 0.91). Significant heterogeneity was found (I2 = 94%).
Secondary Findings
The results from the systematic review and meta-analysis of a smaller number of studies (1 to 4 included studies) were reported as the secondary findings of this review. It was expected that such results could serve as preliminary and intuitive quantitative evaluations, and may also provide considerable insights for future research and clinical research. While the Cochrane handbook states that 2 studies are adequate to conduct a meta-analysis,
45
however, it should be emphasized that the meta-analyses included in the finite quantity study may have larger potential biases in the clinical results. Figure 3 presented the secondary outcomes of the meta-analyses for included studies. The specific information on the meta-analysis for each outcome was in Supplemental Material 3. The secondary outcomes of the meta-analyses for included studies. Note: This figure was produced according to the outcomes from the meta-analyses which were produced by the RevMan 5.4.1 software provided by the Cochrane Collaboration. The specific information on the meta-analysis for each outcome is in Supplemental Material 3. ◆: Pooled mean difference; error bar: 95% confidence interval. MT, main thoracic; PT, proximal thoracic; SB, side-bending; TL/L, thoracolumbar/lumbar.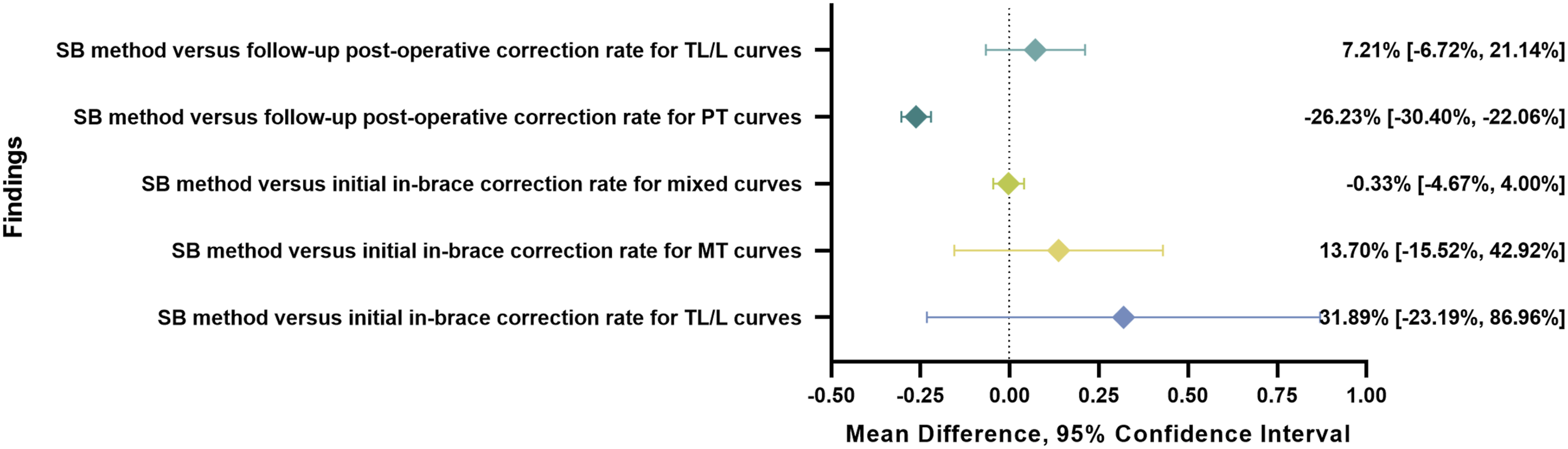
PSF Studies.
Accuracy of the Side-bending Method in Estimating the Follow-up Post-operative Correction Rate for Thoracolumbar/lumbar Curves in AIS Patients.
There were 4 studies57,65,68,71 in the meta-analysis that reported the side-bending flexibility rate and the follow-up correction rate for thoracolumbar/lumbar curves (Supplemental Material 3a). The follow-up time ranged from 24 to 60 months. The pooled data from 229 AIS patients showed no significant difference between the flexibility rate and the actual correction rate, with a mean difference of 7.21% (95% CI: −6.72% to 21.14%, P = 0.31). This suggested that the side-bending method exhibited good predicting capability for determining the actual follow-up correction for thoracolumbar/lumbar curves in AIS patients. There was considerable heterogeneity between studies (I2 = 94%).
Accuracy of the Side-bending Method in Estimating the Post-operative Correction Rate for Proximal Thoracic Curves in AIS Patients.
Two studies33,65 that specifically addressed the proximal thoracic curves, examining both the side-bending flexibility rate and follow-up correction rate data, were incorporated into the meta-analysis (Supplemental Material 3b). The mean follow-up time was 24 months. The pooled data from 154 patients demonstrated that the side-bending flexibility rate was significantly lower than the actual follow-up post-surgical correction rate with an MD of −26.23% (95% CI: −30.40% to −22.06%, P < 0.001). The heterogeneity was considered not important (I2 = 28%). Additionally, 1 study including 7 patients with proximal thoracic curves 62 reported the pre-surgical flexibility rate of 19.60% ± 15.00%, as measured using the side-bending method, and the post-surgical correction rate of 37.30% ± 14.00%. The specific time point for the post-surgical measurement was not provided.
Accuracy of the Fulcrum-bending Method in Estimating the Post-operative Correction for Thoracolumbar/lumbar Curves in AIS Patients.
Only 1 study from Li, J. et al 38 reported data on the pre-surgical fulcrum-bending flexibility rate, as well as the correction rate that measured 1 week post-surgically, for thoracolumbar/lumbar curves. A total of 8 patients were included in the study, with a mean flexibility rate of 68.9% (SD = 14.7%) and a mean correction rate of 83.9% (SD = 7.7%).
Accuracy of the Fulcrum-bending Method in Estimating the Follow-up Post-operative Correction Rate for Proximal Thoracic Curves in AIS Patients.
Only 1 study from Watanabe, K. et al 33 focused on the capability of the fulcrum-bending method in predicting the actual correction measured after 2 years post-surgically for AIS patients with proximal thoracic curves. They found no significant difference between the fulcrum-bending flexibility rate and the post-surgical curve correction. The mean flexibility rate was 44.26% ± 14.27%, and the mean follow-up correction rate was 39.64% ± 15.06%, as calculated by the authors of this review based on the reported data from the study. Watanabe, K. et al indicated that these findings could support the conclusion that the fulcrum-bending method could assess the real proximal thoracic curve flexibility and therefore, had substantial value in predicting surgical outcomes.
Bracing Studies.
Accuracy of the Side-bending Method in Estimating the Follow-up Post-operative Correction Rate for Main Thoracic Curves in AIS Patients.
The meta-analysis included 2 studies72,73 that reported the side-bending flexibility rate and the initial in-brace correction rate from 190 patients with various curve types (Supplemental Material 3c). According to the pooled data, the good predictability of the side-bending method in the degree of initial in-brace correction was observed, with an MD of −0.33% (95% CI: −4.67% to 4.00%, P = 0.88). The heterogeneity was not significant (I2 = 0%).
Accuracy of the Side-bending Method in Estimating the Initial In-brace Correction Rate for Main Thoracic Curves in AIS Patients.
A total of 2 studies73,74 reporting the side-bending flexibility rate and the initial in-brace correction rate for main thoracic curves were included in the meta-analysis (Supplemental Material 3d). The pooled data from 112 patients demonstrated that there was no significant difference between the flexibility rate and the correction rate with an MD of 13.70% (95% CI: −15.52% to 42.92%, P = 0.36). This might indicate a good predictivity of the side-bending method in the initial in-brace correction rate. Considerable heterogeneity was demonstrated (I2 = 97%).
Accuracy of the Side-bending Method in Estimating the Initial In-brace Correction Rate for Thoracolumbar/lumbar Curves in AIS Patients.
Two studies73,74 reporting the side-bending flexibility rate and the correction rate for thoracolumbar/lumbar curves in 84 patients were included in the meta-analysis (Supplemental Material 3e). The analysis showed no significant difference between the side-bending flexibility rate and the initial in-brace correction rate, with an MD of 31.89% (95% CI: −23.19% to 86.96%, P = 0.26). Significant heterogeneity was found (I2 = 99%).
Quality of Evidence
Summary of Quality of Evidence Across the Studies.
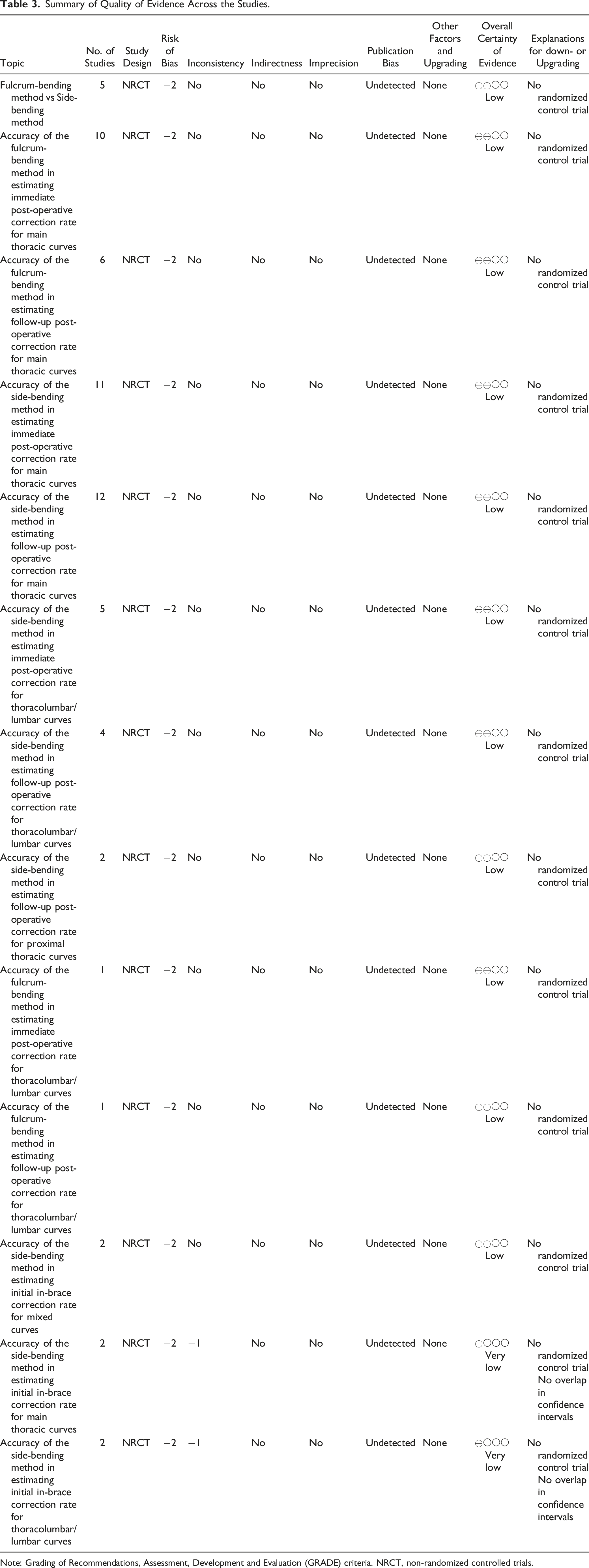
Note: Grading of Recommendations, Assessment, Development and Evaluation (GRADE) criteria. NRCT, non-randomized controlled trials.
Discussion
This systematic review and meta-analysis have investigated and compared the accuracy of the spinal flexibility rates, as assessed by the fulcrum-bending and side-bending radiographs, in predicting the actual curvature correction rate post-intervention in AIS patients who underwent the PSF surgical or bracing treatments. The results supported that the side-bending method has been applied more frequently than the fulcrum-bending method in both PSF and bracing research. The meta-analysis demonstrated that for the main and proximal thoracic curves, the fulcrum-bending method might have better-predicting accuracy both immediately and during follow-up in AIS patients receiving PSF surgery. For thoracolumbar/lumbar curves, the flexibility rate assessed by the side-bending method showed high predicting accuracy for both the immediate and follow-up post-surgical correction rates. In bracing studies, a few studies chose the side-bending method for spinal flexibility assessment, and supported its good capability in predicting the initial in-brace correction for AIS patients.
All included studies showed the moderate-to-high quality of methodologies according to the NOS assessment tool. Based on the GRADE criteria, there was low-quality evidence supporting the accuracy of the fulcrum-bending and the side-bending approaches, in predicting the post-surgical curve correction for AIS patients who underwent PSF surgery. There was low to very-low quality evidence that supported the accuracy of the side-bending method, in predicting the initial in-brace curve correction for AIS patients who underwent the bracing treatment.
The fact that the side-bending method has a longer history than fulcrum bending may be 1 of the reasons why it is more widely used in PSF surgery and brace therapy. Since been introduced in 1972, 30 the side-bending method has demonstrated good predicting ability for the post-surgical correction rate of the traditional non-segmental/segmental instrumentation techniques,75-77 establishing it as the “golden standard” worldwide. In contrast, although the more recent fulcrum-bending method, which was introduced in 1997, 28 has been reported in more recent studies to have less predicting error than the traditional side-bending method with the modern segmental instrumentation techniques,33,37,38,48 it has not yet achieved widespread global acceptance and application. Compared to the side-bending method, which does not require additional manual or auxiliary equipment and is easy for clinicians to master, the result of the fulcrum-bending method is influenced by factors such as fulcrum size. 38 This may affect the prediction results, leading to a lack of trust from clinicians. Similarly, the procedure of predicting initial in-brace correction based on the spinal flexibility have been recently originated from the surgical protocols. 78 The supine position without side-bending was the most commonly used spinal flexibility assessment during bracing treatment, even more frequent than the side-bending method, and the fulcrum-bending method had not yet been utilized. 79 However, so far, no consensus has been reached regarding the most accurate method for bracing treatment. The current meta-analysis indicates that further high-quality studies are still needed to fully understand the clinical value of the fulcrum-bending method in surgical treatment and the side-bending method in brace treatment.
For the surgical treatment of main thoracic curves, the immediate and long-term predicting accuracy of the fulcrum-bending approach was relatively high in AIS patients. In contrast, the predicting ability of the side-bending method should be interpreted with caution, as the results of the meta-analysis indicated that it might underestimate the correction rates more significantly. Compared to lumbar curves, thoracic curves are structurally limited in terms of range of motion due to the influence of the rib cage. 80 Previous studies have also indicated that patients who meet the indications for posterior spinal fusion (PSF) surgery may exhibit relatively rigid curves. 28 Consequently, they may face difficulties in actively and fully side-bending their spine without additional external assistance when assessing the spinal flexibility using the traditional side-bending method. Its limitations relating to the insufficient reliability10,81 and reproducibility10,23,82 have also been noticed in recent years. The above-mentioned issues can be solved by the utilization of the fulcrum-bending method. With the fulcrum in place, the patient’s own body gravity replaces their unstable active effort to passively open the spine. 28 The increased distance between the upper body (specifically the ipsilateral shoulder) and the X-ray table that provided by the fulcrum allows for the maximum application of passive bending force to fully exhibit the potential spinal flexibility. This leads to the results that even with the advanced modern surgical technologies (eg, all-pedicle screw instrumentation system), which have significantly enhanced curve correction in posterior spinal fusion (PSF) surgeries,37,83,84 the fulcrum-bending method still consistently showed smaller predicting errors than the traditional side-bending method. This was also supported by the meta-analysis results of the current review. When considering the time effect, similar to a previous review, 20 this study also observed that the predicting error of the fulcrum-bending approach was smaller over time, comparing with the side-bending method. These findings supported the utilization of the fulcrum-bending method for measuring spinal flexibility in AIS patients with main thoracic curves. Based on the fulcrum-bending assessment results, surgeons can select the surgical fusion with more suitable levels and number of vertebrae. This enables more preservation of motion segments 85 and the potential to save more distal levels,85,86 comparing to the conventional strategies of selecting fusion levels.
For the surgical treatment of thoracolumbar/lumbar curves, the side-bending technique could accurately predict both immediate and long-term post-surgical curve correction. Meta-analyses revealed no significant mean difference between the measured spinal flexibility and the actual post-surgical correction rate. This finding is consistent with the conclusion of a previous literature review. 39 Although a direct comparison between the side-bending method and the fulcrum-bending method for measuring thoracolumbar/lumbar flexibility has yet to be conducted, the side-bending method has shown comparable predictive accuracy to other radiographic-based assessment methods.62,87-89 The previous findings further supported the application of the side-bending method for assessing the flexibility of thoracolumbar/lumbar curves. Its benefits also include ease of use, as it requires no additional equipment, leading and facilitating its extensive application and appreciation by clinicians. For the fulcrum-bending approach, previous studies have reported its ability to accurately estimate the post-surgical correction rate for thoracolumbar/lumbar curves.90,91 However, this systematic review included a limited number of eligible fulcrum-bending research, highlighting the need for additional evidence to further support its predicting capacity.
For the surgical treatment of proximal thoracic curves, the side-bending method may underestimate the spinal flexibility in patients receiving PSF surgery, while the evidence on the fulcrum-bending approach has been limited. These findings from the current systematic review and meta-analysis are in accordance with a previous systematic review. 20 However, since only 2 side-bending related studies with small sample sizes were involved in the meta-analysis, this finding should be interpreted with caution. For the fulcrum-bending method, similar to the finding on thoracolumbar/lumbar curve studies, only 1 study has reported its promising application prospects in estimating the actual curve correction for proximal thoracic curves for surgically treated AIS patients, 33 making it unavailable to conduct a meta-analysis. Further research focusing on proximal thoracic curves is necessary to provide more evidence.
For the bracing treatment, the side-bending method showed good predicting ability for initial in-brace correction. However, this finding should be applied with caution, as only 3 studies were eligible for the systematic review, and each meta-analysis incorporated only 2 studies. This may explain why some recent studies still chose the conventional supine spine radiographs, without side bending, to assess the curve flexibility.92-94 Although the side-bending method demonstrated certain accuracy in predicting the in-brace correction, more future studies are still needed to strengthen the evidence and identify the optimized protocol for curvatures with different angles, types, and levels in AIS patients.
For future clinical practice of assessing spinal flexibility using the fulcrum-bending or side-bending method, the findings of this meta-analysis and systematic review suggested that: (1) For AIS patients with main thoracic curves and receiving PSF surgery, the fulcrum-bending method could predict the post-intervention correction more accurately; (2) For AIS patients with thoracolumbar/lumbar curves and receiving PSF surgery, the side-bending method appeared to have sufficient predicting accuracy; (3) For AIS patients with proximal thoracic curves and receiving PSF surgery, the fulcrum-bending method may have promising potential, however, further comparisons are still necessary to evaluate the predictive accuracy between 2 methods; and (4) For AIS patients receiving bracing treatment, the side-bending method may be used, while more high-quality research to fully understand its application protocols are still needed.
Future research could consider: (1) investigating the predicted effectiveness of the fulcrum-bending method that applied in surgical AIS patients with proximal and thoracolumbar/lumbar curves; and (2) investigating the application value of the side-bending and/or fulcrum-bending methods for AIS patients who undergoing bracing treatment.
It’s important to point out that this systematic review and meta-analysis have several limitations. The first limitation was the high heterogeneity that existed among the included studies in this review. This might be due to the eligibility criteria of including as much available studies/data as possible, the high variability of the study design, and the objective of each study. Despite this, the meta-analysis results were considered reliable, with rather good control over the type of extracted data and the time point of extraction in this review. The second limitation was the limited number of eligible studies that focused on the utilization of: (1) the fulcrum-bending method for proximal and thoracolumbar/lumbar curves in PSF surgery; (2) the side-bending method for proximal curves in PSF surgery; and (3) the side-bending method in bracing treatment. As a result, most included studies were about surgical interventions (ie, PSF), rather than non-surgical intervention (ie, bracing). Limited by the low quality of evidence and the limited number of eligible studies that related to bracing interventions, the predicting accuracy results on the side-bending methods shall be interpreted with caution. The current evidence did not reject, but may also not be sufficient enough, to recommend the clinical practice of using side-bending method to predict the non-surgical correction for patients receiving bracing treatments.
Conclusions
This systematic review and meta-analysis have qualitatively and quantitatively evaluated the accuracy of 2 common clinical radiographic assessment methods of spinal flexibility in predicting post-intervention curve corrections of AIS patients. Up to now, the side-bending radiography method has been applied more often in clinical practice than the fulcrum-bending radiography method, regardless of whether the AIS patients received surgical or bracing treatments. The quantitative results supported the utilization of the fulcrum-bending method for assessing the spinal flexibility of main thoracic curves, and the side-bending method for thoracolumbar/lumbar curves in AIS patients receiving PSF surgery. Further investigations are still needed to support the use of the fulcrum-bending method for proximal thoracic curves. For patients undergoing bracing treatment, the side-bending method has limited evidence and still needs to be further investigated to confirm its clinical application value.
Supplemental Material
Supplemental Material - Predicting Surgical and Non-surgical Curvature Correction by Radiographic Spinal Flexibility Assessments for Patients With Adolescent Idiopathic Scoliosis: A Systematic Review and Meta-Analysis
Supplemental Material for Predicting Surgical and Non-surgical Curvature Correction by Radiographic Spinal Flexibility Assessments for Patients With Adolescent Idiopathic Scoliosis: A Systematic Review and Meta-Analysis by Yu-Yan Luo, Tim-Mei Hung, Qian Zheng, Hui-Dong Wu, Man-Sang Wong, Zi-Qian Bai, and Christina Zong-Hao Ma in Global Spine Journal
Supplemental Material
Supplemental Material - Predicting Surgical and Non-surgical Curvature Correction by Radiographic Spinal Flexibility Assessments for Patients With Adolescent Idiopathic Scoliosis: A Systematic Review and Meta-Analysis
Supplemental Material for Predicting Surgical and Non-surgical Curvature Correction by Radiographic Spinal Flexibility Assessments for Patients With Adolescent Idiopathic Scoliosis: A Systematic Review and Meta-Analysis by Yu-Yan Luo, Tim-Mei Hung, Qian Zheng, Hui-Dong Wu, Man-Sang Wong, Zi-Qian Bai, and Christina Zong-Hao Ma in Global Spine Journal
Supplemental Material
Supplemental Material - Predicting Surgical and Non-surgical Curvature Correction by Radiographic Spinal Flexibility Assessments for Patients With Adolescent Idiopathic Scoliosis: A Systematic Review and Meta-Analysis
Supplemental Material for Predicting Surgical and Non-surgical Curvature Correction by Radiographic Spinal Flexibility Assessments for Patients With Adolescent Idiopathic Scoliosis: A Systematic Review and Meta-Analysis by Yu-Yan Luo, Tim-Mei Hung, Qian Zheng, Hui-Dong Wu, Man-Sang Wong, Zi-Qian Bai, and Christina Zong-Hao Ma in Global Spine Journal
Footnotes
Author Contributions
All authors contributed to the study conception and design. Study conception and design were performed by Y.Y.L. and C.Z.H.M. Material preparation, data collection, analysis, and interpretation were performed by Y.Y.L., T.M.H., Q.Z., H.D.W., M.S.W., Z.Q.B., and C.Z.H.M. The first draft of the manuscript was written by Y.Y.L., and all authors revised and edited the manuscript. All authors have read and approved the final manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by Department of Biomedical Engineering, The Hong Kong Polytechnic University (grant number: P0034491, P0053711).
Supplemental Material
Supplemental material for this article is available online
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.