Abstract
Study Design
cross-sectional survey.
Objectives
To evaluate AO Spine members’ practices and comfort in managing metastatic and primary spine tumors, explore the use of decision-support and patient assessment tools, and identify knowledge gaps and future needs in spine oncology.
Methods
An online survey was distributed to AO Spine members to query comfort levels with key decisions in spinal oncology management, utilization of decision frameworks and spine oncology-specific instruments, and educational material preferences.
Results
Responses were obtained from 381 members across 82 countries. Most respondents were orthopedic spine surgeons (62%) or neurosurgeons (36%), with 42% performing 100-200 spine surgeries per year. Extradural primary and metastatic tumors were managed by 84% and 95% of respondents, respectively, with survival and frailty assessment tools used for both. While most surgeons felt comfortable determining when emergency surgery was needed (81% for primary and 82% for metastatic tumors), nuanced decisions about surgical timing were more challenging. Surgeons also noted challenges in tailoring the oncologic surgical plan to what the patient could safely tolerate. There was a strong desire for guidelines on tumor-related spinal pain (85%), treatment timing (85%), stabilization (85%), and glucocorticoid use for symptomatic extradural metastatic tumors (77%). Interest was high for classification systems for spine tumor pain (65%) and stabilization decisions (80%).
Conclusions
Additional support is needed in decision-making regarding surgical timing, patient selection, and tailoring treatment invasiveness to life expectancy and frailty. Surgeons seek further guidance to prevent neurologic deterioration and optimize recovery. Guidelines and classification systems were highly coveted for daily practice.
Keywords
Introduction
Most spine surgeons will encounter and treat patients with spinal tumors during their career, however, comfort levels managing these tumors vary markedly. Currently, the 3 main indications for spine tumor surgery include: (1) curative intent (typically for primary tumors), (2) stabilization, and (3) decompression of the spinal cord or nerve roots (typically for metastatic tumors). Patients can present in emergent and elective settings, and appropriate diagnostic evaluation of primary and metastatic tumors plays a key role in treatment outcomes. While many spine surgeons may not focus their practice and research on tumors of the spine, most spine surgeons should understand how to appropriately evaluate, diagnose, and treat spinal tumors and when to refer for expert multidisciplinary evaluation.
The AO Spine Knowledge Forum Tumor (KF Tumor) is a multidisciplinary group composed of seventy spinal oncology experts with global representation and a mission to generate and translate knowledge about spine tumors. KF Tumor aims to improve the lives of patients with spinal tumors by studying, decreasing, and preventing disease- and treatment-associated symptoms, improving tumor control, and optimizing treatment decisions and care pathways. The group’s knowledge generation efforts include identifying critical knowledge gaps, conducting prospective and retrospective multicenter studies and developing instruments to improve patient assessment and research. Knowledge translation efforts include disseminating the currently available information about spinal tumors to clinicians, trainees and patients, utilizing targeted education programs, treatment recommendations and decision support tools.
Despite making significant inroads to knowledge generation and translation, there remains ineffiencies and a lack of insight into what and how clinicians want to learn. To gain a better understanding of the current state of spine oncology knowledge among the AO Spine community, AO Spine members were surveyed regarding their comfort with decisions and surgical techniques necessary to treat patients with primary and metastatic extradural bone tumors and intradural tumors of the spine. The AO community was also queried regarding their needs in spine oncology knowledge generation, the success of AO Spine knowledge translation efforts, and the needs and preferences for future knowledge translation topics and methods. The results will be used to direct future research and educational efforts.
Methods
Survey Design and Distribution
A needs assessment survey was developed by JIL and IL. The survey was created using SurveyMonkey Inc (San Mateo, CA) and consisted of 6 sections: general demographics, baseline information on spine tumors, evaluation and treatment of patients with extradural primary spinal tumors, evaluation and treatment of patients with extradural metastatic spinal tumors, evaluation and treatment of patients with intradural spinal tumors, and general concluding questions (the full questionnaire is included in Supplemental Appendix SI).
Questions were presented in various formats, including single and multiple-choice, open-ended questions, and Likert scales. Branching logic was applied to select questions as necessary. The 91-item survey was distributed to members of the AO Spine community, the world’s largest society of international spine surgeons (https://www.aofoundation.org/spine), between January 26, 2024, and February 29, 2024. AO Spine members were invited to participate via an email containing a link to the questionnaire. The survey targeted surgeons who opted to receive emails from AO Spine, including over 16 000 members. All responses were anonymous.
A chi-squared test was conducted to evaluate whether the proportion of responders to each question, segmented by tumor type (extradural primary spinal tumor, extradural metastatic spinal tumor, and intradural tumor), differed significantly across categories of annual surgical case volumes. Statistical analyses were performed using SPSS, version 30 (IBM Corp., Armonk, NY). A
Results
Demographics
Demographics.
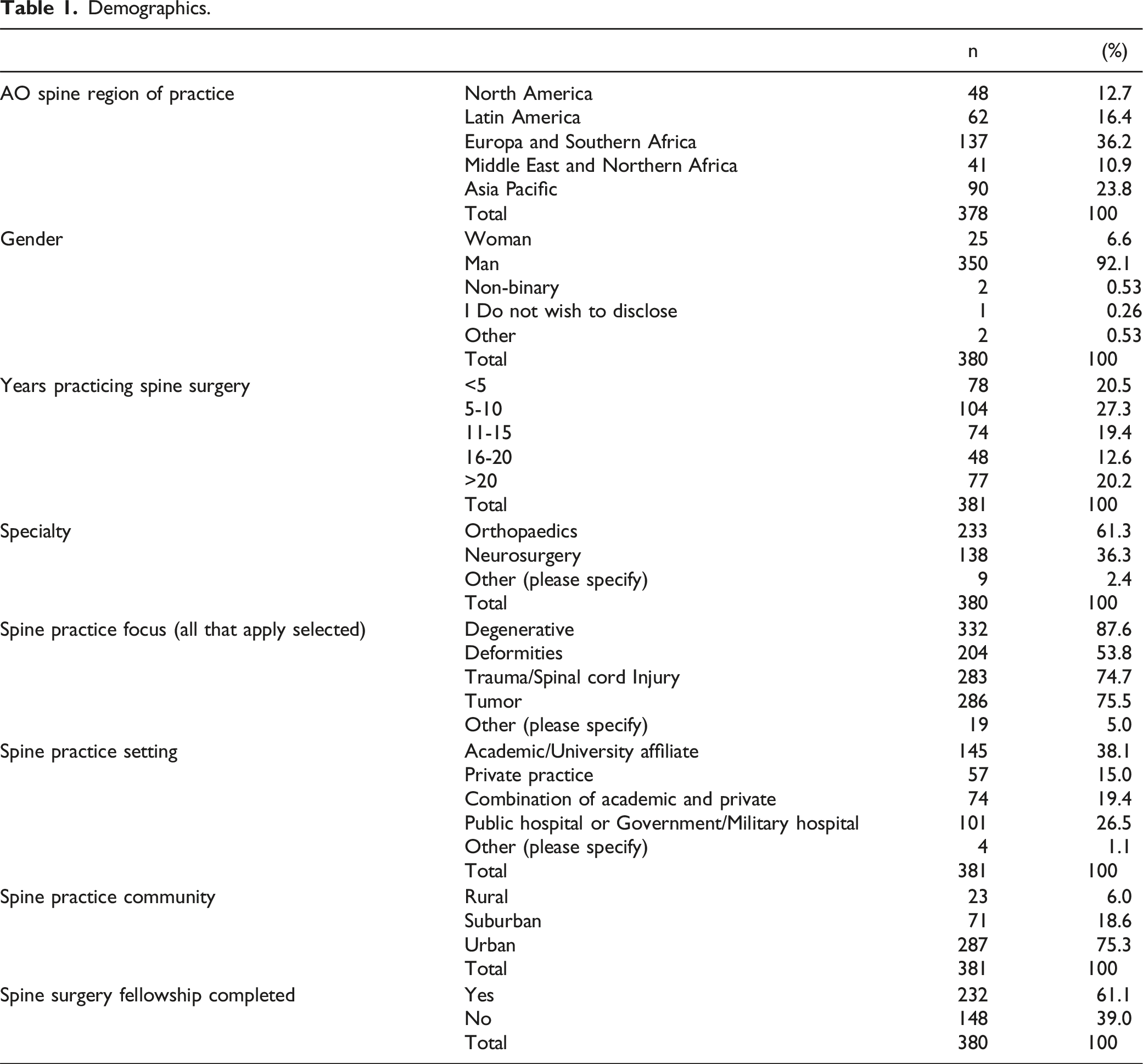

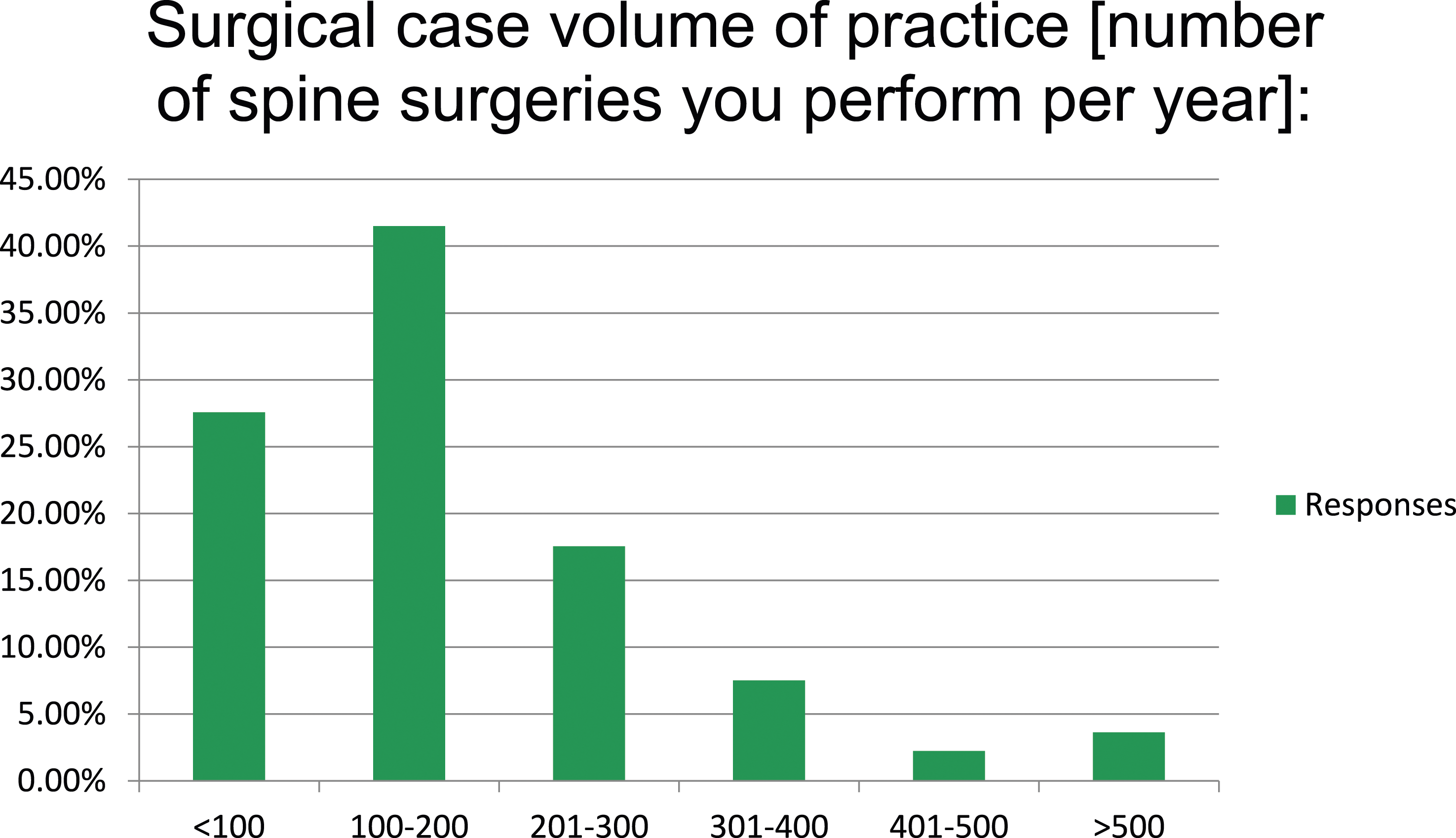
Surgical spine case volume per year (n = 359).
Extradural Primary Tumors
Practice Volume
The majority of respondents treated 1 to 5 extradural primary tumors per year (n = 183, 55%; Figure 2). Twenty-two respondents (6.6%) reported treating more than 20 primary tumors per year, with 7 of these surgeons treating more than 40 per year (Figure 2). Of the 45 respondents from the AO Spine KF Tumor, 4 reported treating over 20 primary tumors per year and 2 of those reported treating more than 40 per year.
1
Surgical extradural primary spine case volume per year (n = 335).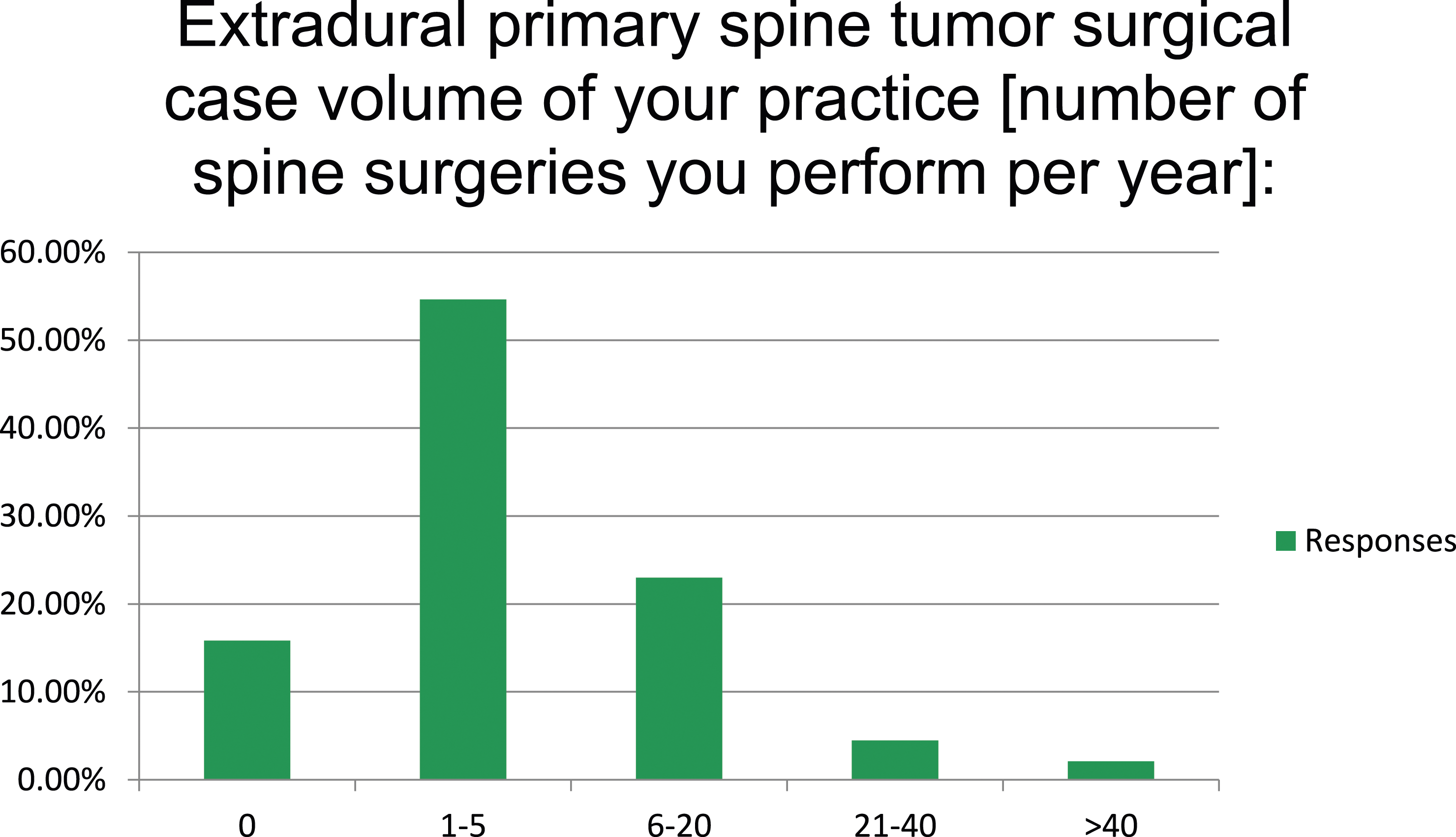
Patient Evaluation/Decisions
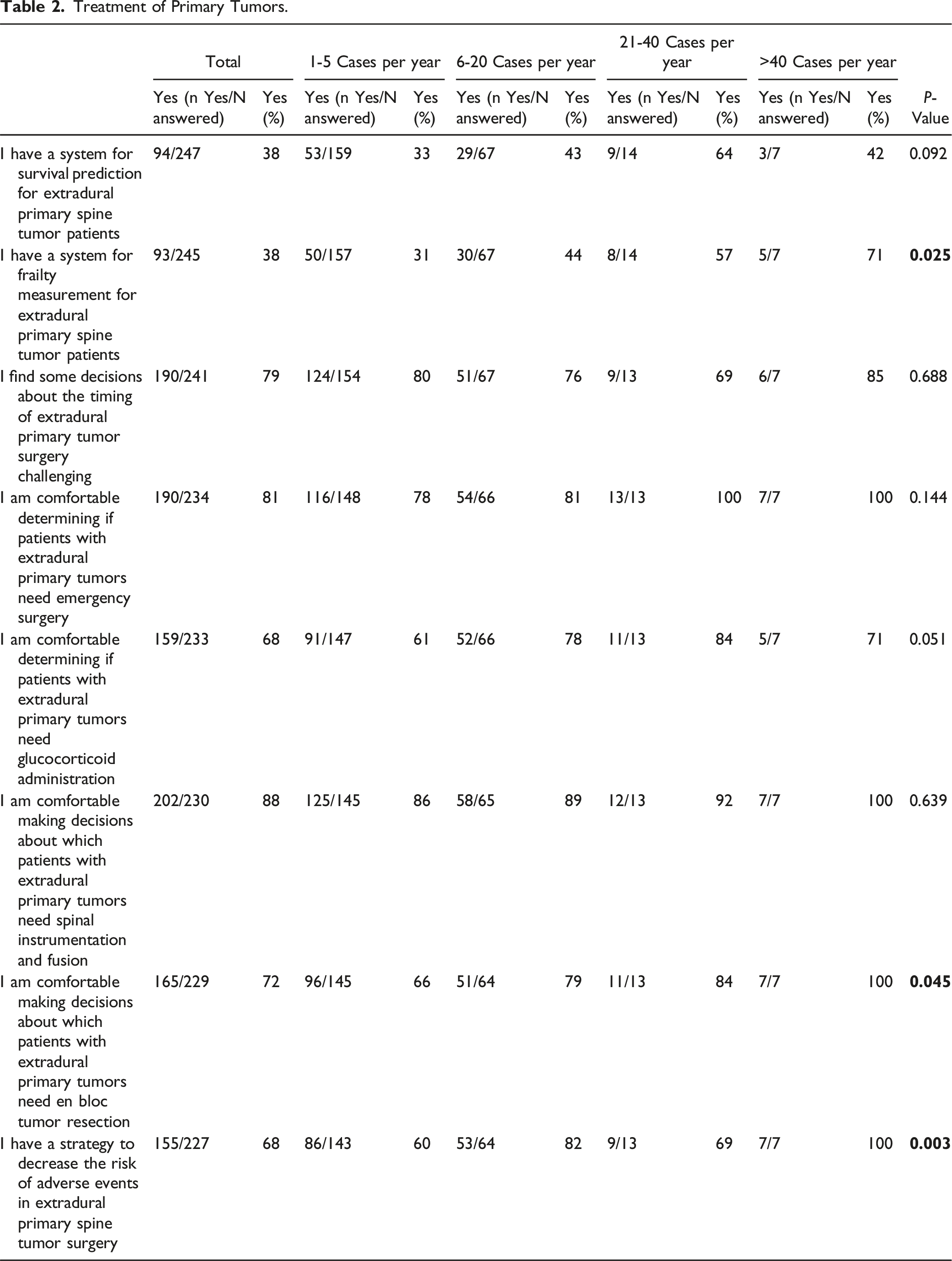
Treatment of Primary Tumors.
Techniques
Despite the relatively low volume of primary tumor surgeries across most practices (Figure 1), 88% of respondents (n = 202) felt comfortable instrumenting the spine, and 72% (n = 165) felt comfortable performing an en bloc resection (Table 2). The majority of the respondents (n = 155, 68%) use strategies to reduce the risk of adverse events, including collaboration with plastic surgeons, patient evaluation and treatment by multidisciplinary care teams, utilization of minimally invasive surgical (MIS) techniques, vancomycin powder, surgical navigation, electrophysiological monitoring, preoperative tumor embolization and nutritional optimization (Table 2).
Extradural Metastatic Tumors
Practice Volume
In contrast to primary tumors, many respondents in this cohort (most of whom perform 6-20 cases per year; Figure 3) reported operating on more than 40 metastatic extradural tumors annually. Among the 45 AO Spine KF Tumor members, nearly half (20) reported treating more than 20 patients with metastatic spinal tumors per year, with 12 treating more than 40 per year. Of those treating more than 40 per year (n = 36), around one third (n = 12, 33%) were from the AO Spine KF Tumor group, which is similar to the results for primary tumors. Surgical extradural metastatic spine case volume per year (n = 335).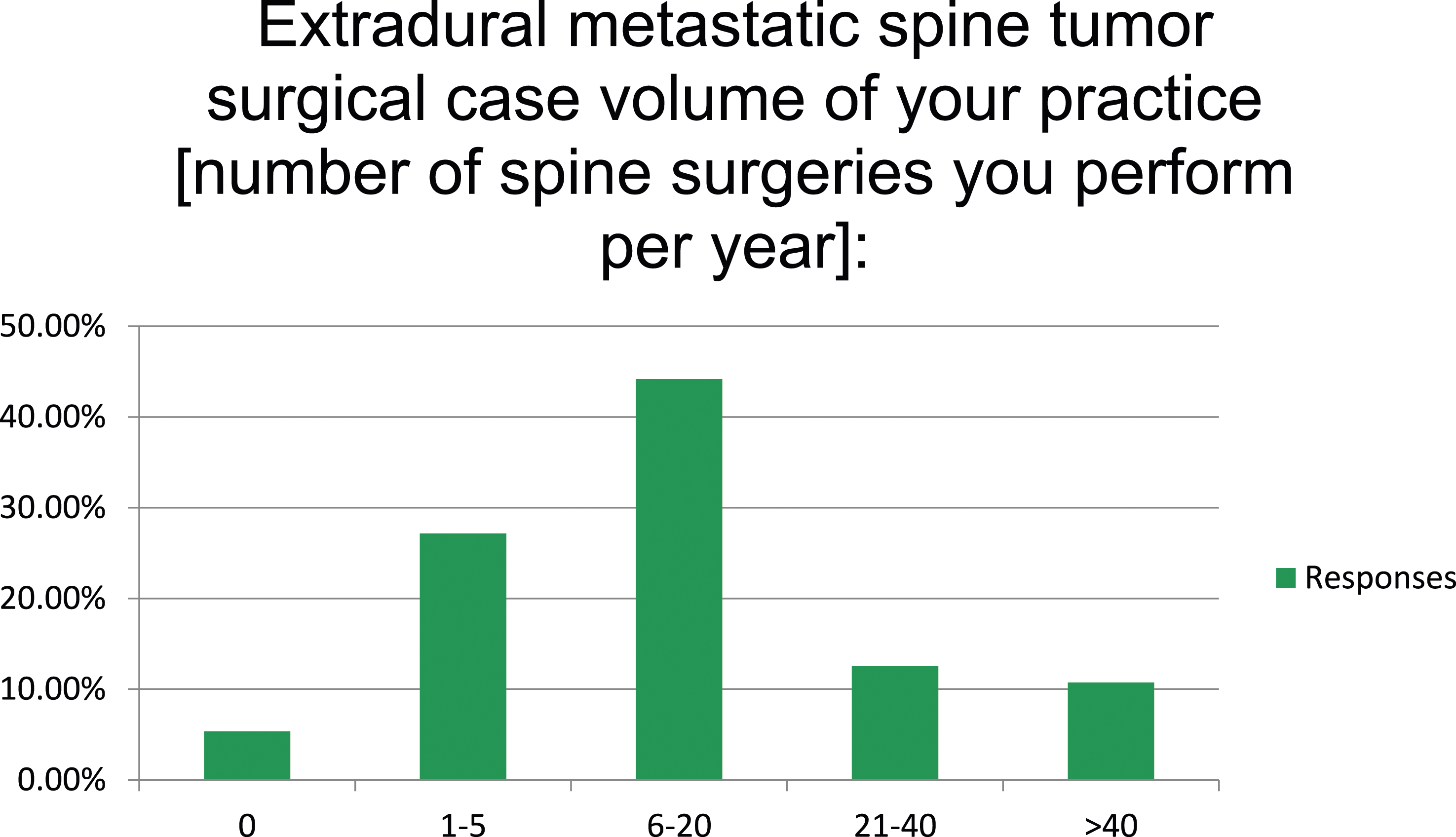
Patient Evaluation/Decisions
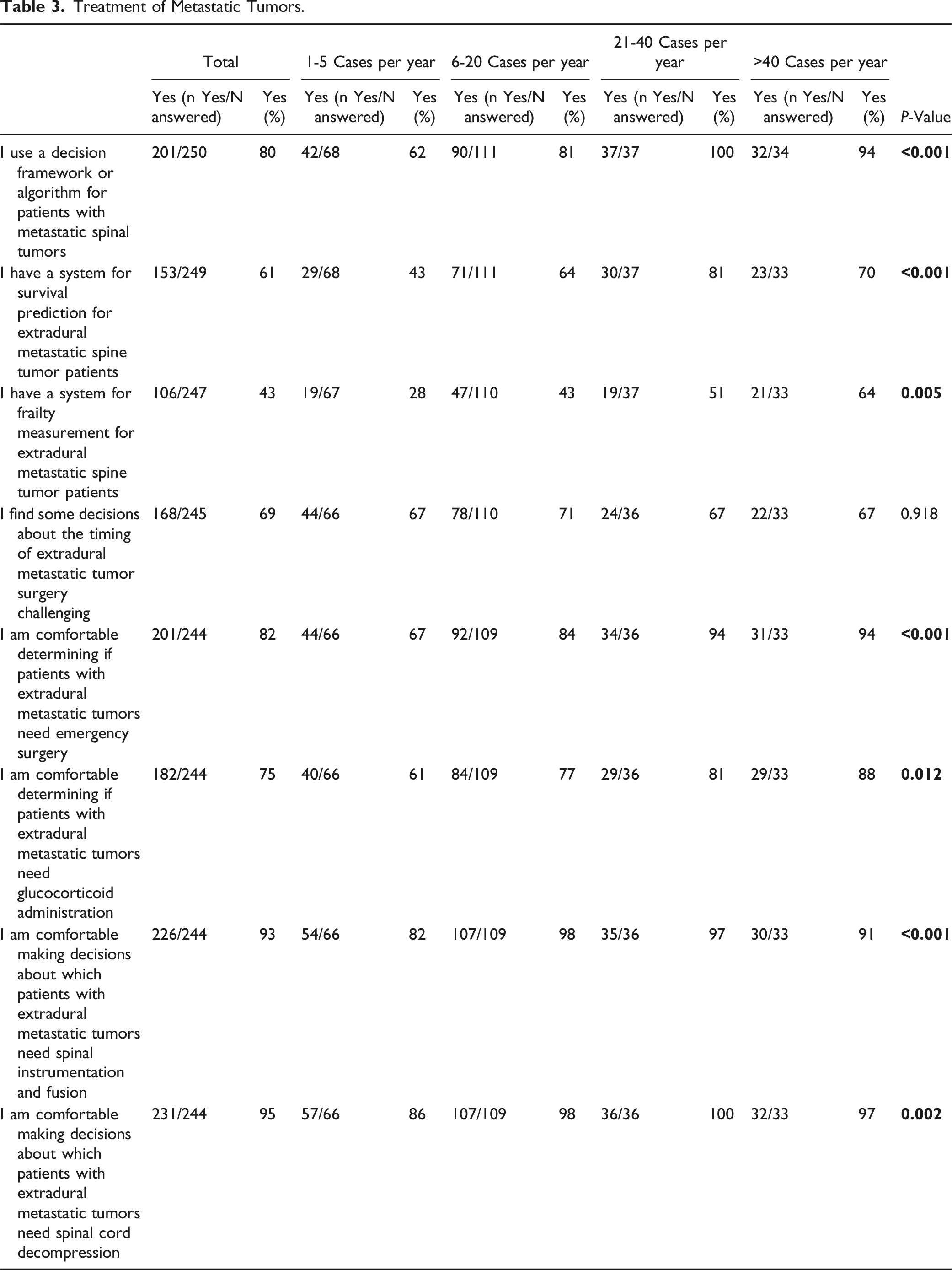
Treatment of Metastatic Tumors.
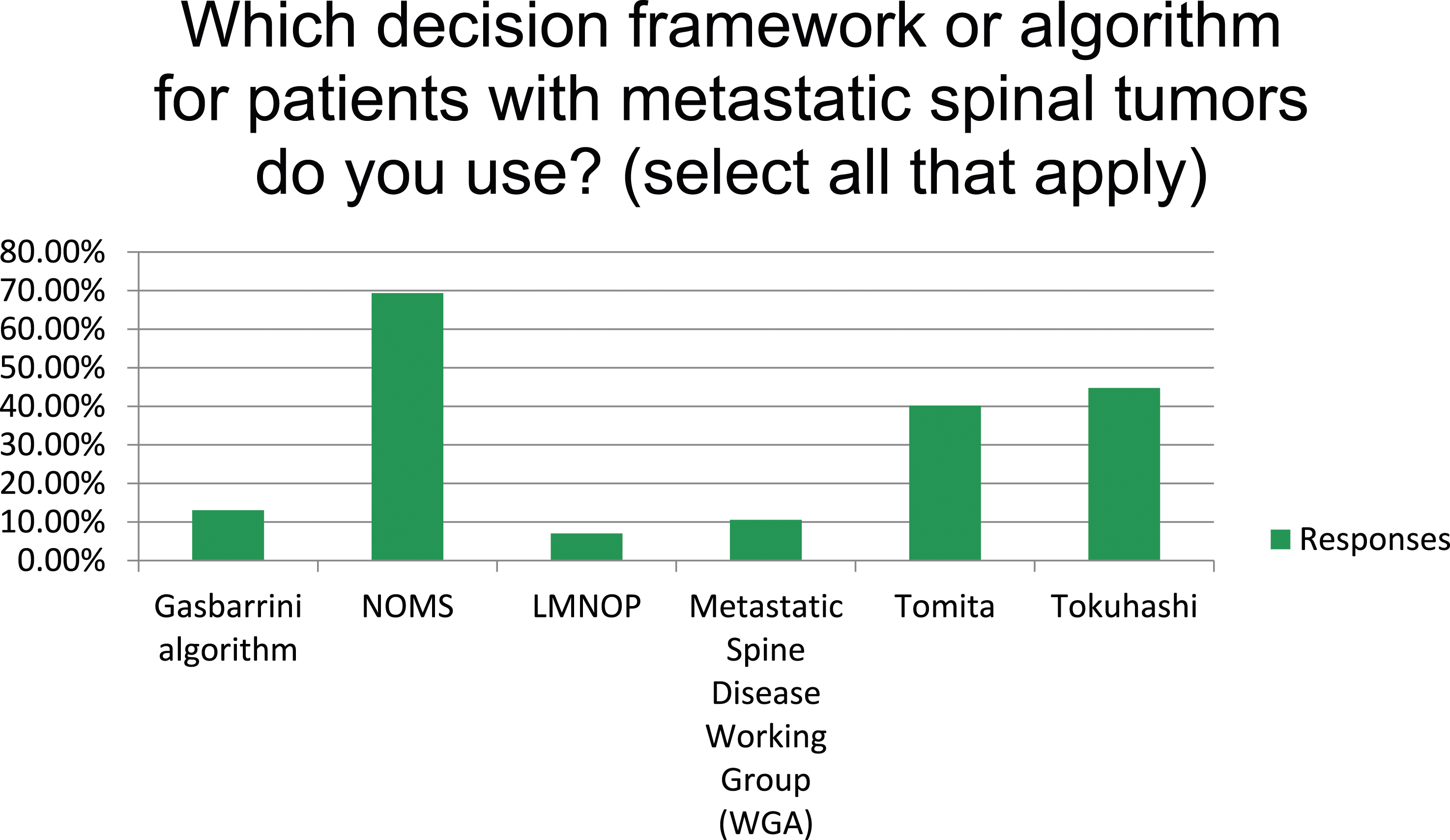
Metastatic spine decision frameworks (n = 199).
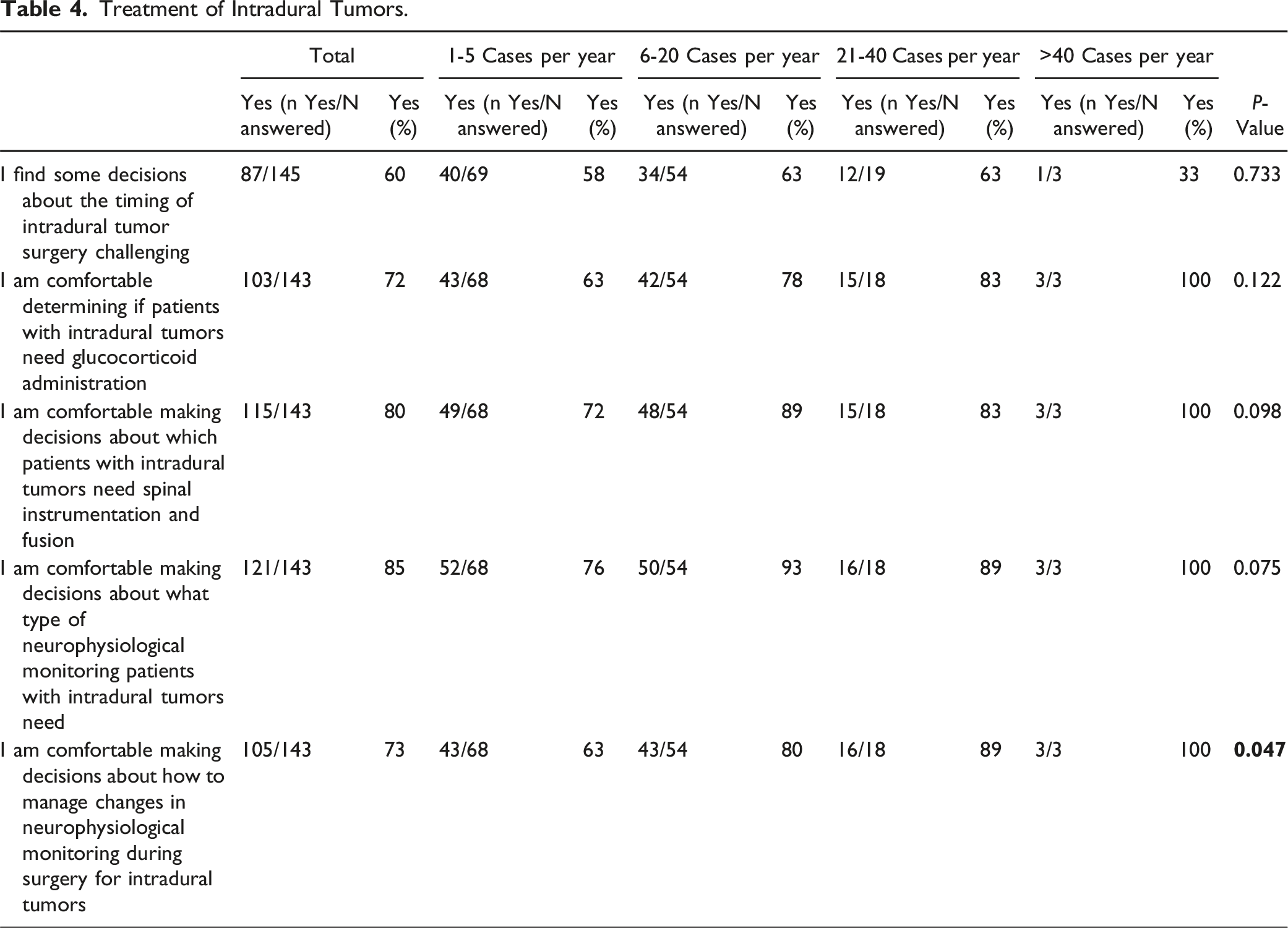
Treatment of Intradural Tumors.
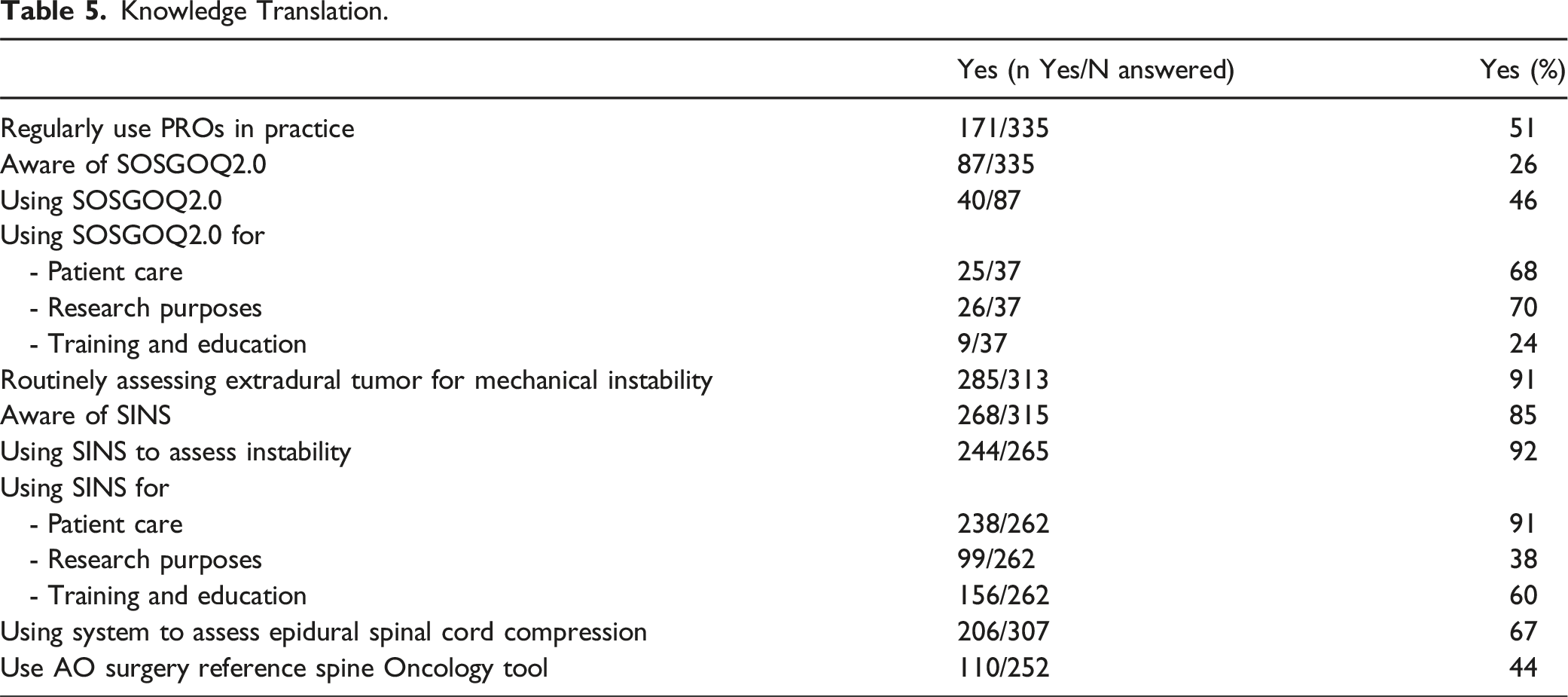
Knowledge Translation.
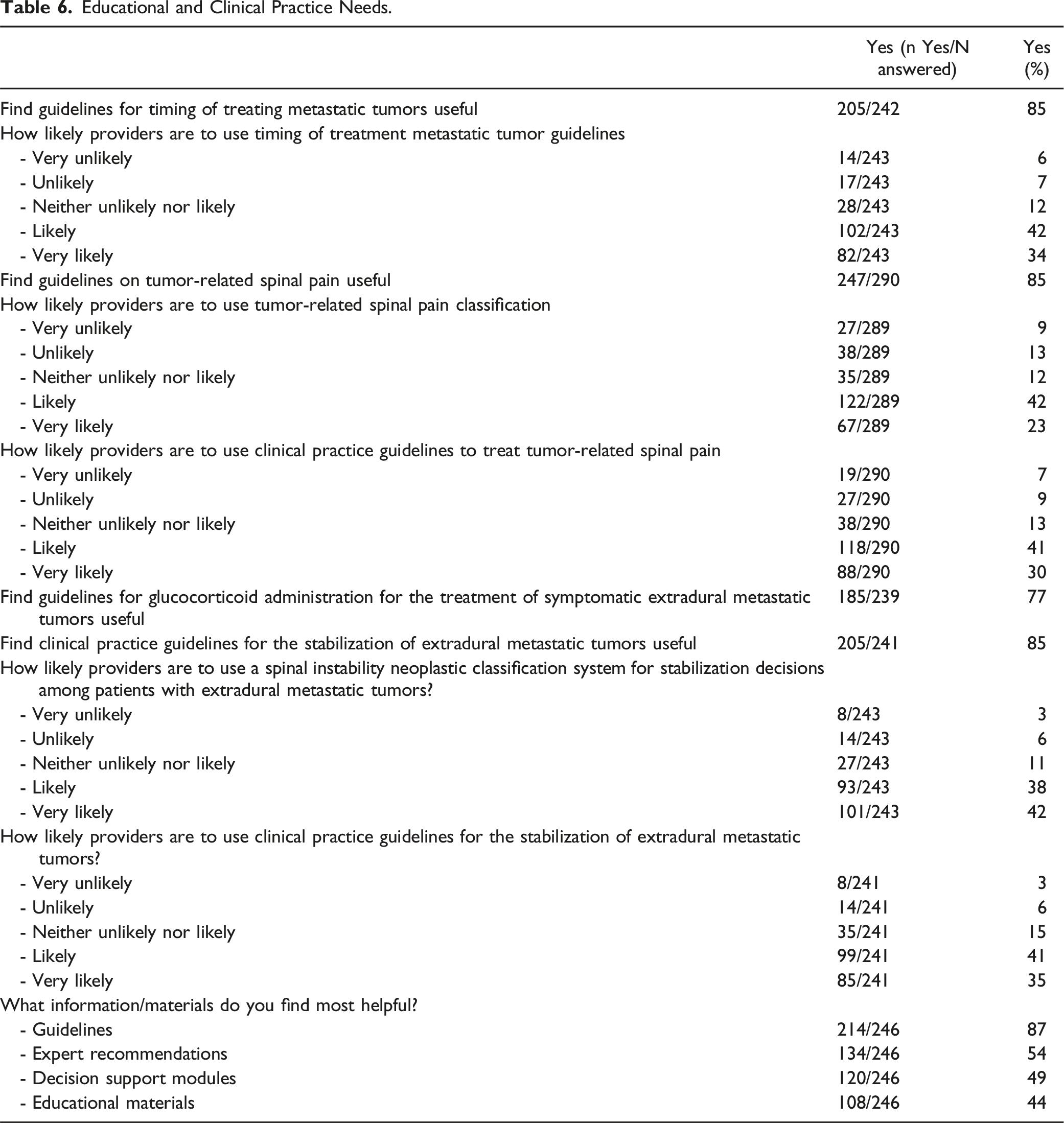
Educational and Clinical Practice Needs.
Techniques
Regarding treatment of patients with metastatic tumors, 93% of respondents indicated that they feel comfortable instrumenting the spine (n = 226) and 95% feel comfortable performing decompression when there was significant cord compression (n = 231, Table 3). The majority of the respondents (n = 171, 70%, Table 3) use strategies to reduce the risk of adverse events, which include collaboration with plastic surgeons, patient evaluation and treatment by multidisciplinary care teams, utilization of MIS techniques, vancomycin powder, surgical navigation, electrophysiological monitoring, preoperative tumor embolization, and nutritional optimization.
Intradural Tumors
Practice Patterns
Regarding the number of intradural lesions treated each year, many respondents left this question blank, with 140 respondents (42%) indicating they perform zero intradural tumor surgeries per year (Figure 5). This is likely due to the large number of orthopedic spine surgeons (n = 233, 61%, Table 1) who responded, many of whom likely do not routinely treat intradural lesions in their practice. Of those who did reply, only 5 reported treating more than 40 per year, and 21 surgeons reported treating 21-40 intradural tumors each year (Figure 5). Surgical intradural spine tumor case volume per year (n = 335).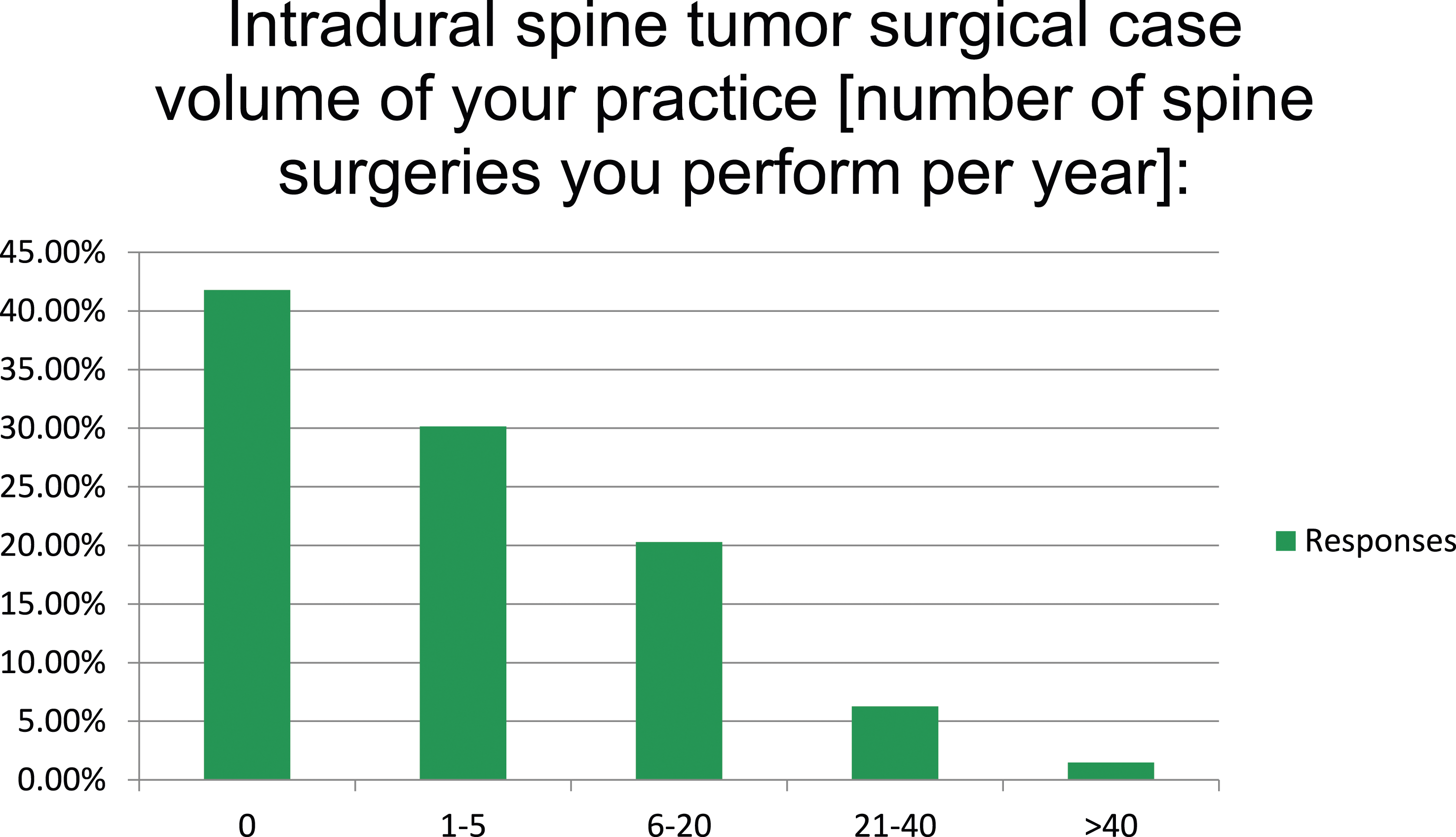
Patient Evaluation/Decisions
Table 4 summarizes key findings in this population. Similar to previous categories, 60% of respondents (n = 87, Table 4) felt that decisions about the timing of surgery could be challenging. Open-ended responses mentioned difficulties in determining when surgery was urgent and establishing overall surgical indications for intradural tumors, particularly when symptoms were mild. Over 70% indicated that they feel comfortable deciding when to administer glucocorticoids in these cases (n = 103, 72%, Table 4).
Techniques
Similar to previous categories, 80% of respondents (n = 115, Table 4) indicated that they feel comfortable deciding which patients require instrumentation. The majority (n = 121, 85%) felt confident in choosing the appropriate type of neurophysiological monitoring, and 73% (n = 121) were comfortable managing changes in monitoring during surgery (Table 4). Stratification by annual treatment volume revealed differences in comfort with decisions about how to manage changes in neurophysiological monitoring. Open-ended responses included questions about the extent of the resection and how monitoring changes influence the extent of resection in various cases.
Knowledge Translation
Table 5 summarizes key findings for Knowledge Translation. SINS and SOSGOQ are instruments developed by the AO Spine KF Tumor.13,14 Practice patterns, respondent awareness, and utilization of these instruments were queried within the broader thematic context.
SINS
Almost all surgeons (n = 285, 91%) routinely evaluate patients with extradural tumors for mechanical instability. The overwhelming majority (n = 268, 85%) are aware of SINS. Nearly all respondents who are familiar with SINS use SINS to assess tumor-related instability (n = 244, 92%), underscoring its utility and its successful integration into clinical practice (Table 5). SINS is widely used in patient care (91%), research (38%), and training and education activities (60%) (Table 5). Respondents noted that they learned about SINS through conferences, publications, and training.
SOSGOQ
Many respondents reported that they regularly use Patient-Reported Outcome tools (PROs) in their practice when evaluating spine tumor patients (n = 171, 51%, Table 5). However, when asked if they were aware of the SOSGOQ2.0 PRO, 74% (n=248, Table 5) were
Educational Material Use and Clinical Practice Needs
AO Surgery Reference
The AO Foundation Surgery Reference is an online resource developed to educate readers about decisions and techniques in spine surgery, with disease-specific modules including primary and metastatic tumors (Spine Tumors (aofoundation.org)). Less than half of the respondents use the spine tumor modules in the Surgery Reference (n = 110, 44%, Table 5), and nearly all comments from those that do not use it reflect a lack of knowledge of its existence.
Clinical Practice Needs
When surgeons were asked, “What information or materials do you find most helpful,” and instructed to select 2-3 items from a list of 4 options (guidelines, expert recommendations, decision support modules, education materials), the guidelines option was selected 214 times (87%). Expert recommendations were chosen 134 times (54%), decision support modules 120 times (49%), and educational materials 108 times (44%, Table 6).
Respondents indicated that they would find guidelines for the treatment of tumor-related spinal pain (85%), timing of treatment (85%), stabilization (85%) and glucocorticoid administration for symptomatic extradural metastatic tumors (77%) useful (Table 5).
Over 70% of respondents indicated that they were likely or very likely to use these guidelines in clinical practice (Table 5). The majority of respondents also indicated that they were likely or very likely to use classifications system for spine tumor pain (n = 189, 65%) and spinal instability for stabilization decisions (n = 194, 80%).
Discussion
Overall Findings
Several themes emerged from this survey of nearly 400 practicing spine surgeons worldwide, which evaluated their preferences, practices, and needs. The treatment of spinal tumors, particularly primary spinal tumors, remains a specialized field, with only a handful of surgeons and centers treating a large number of these cases. In this survey, 45 of the respondents were members of the AO Spine Knowledge Forum Tumor, an international group of key opinion leaders in spine oncology. Despite this inclusion, only 22 surgeons surveyed reported treating more than 20 primary tumors per year, and only 7 surgeons more than 40 annually. While there is no universally agreed-upon minimum number of cases per year for treating primary tumors of the spine, this underscores the importance of referring to tertiary centers where specialized surgical teams handle a high volume of such cases. 15 These surgeries are often multidisciplinary in nature and require a coordinated team of providers.
In contrast, many providers queried treated more than 20 and even over 40 metastatic tumors per year. These data suggest that teaching modules, symposia, and educational materials designed for practicing spine surgeons should differ markedly in their overall methods and focus depending on whether the topic is primary tumors or metastatic tumors. Teaching and discussions around
Knowledge Gap Identification
The survey results indicate that most of the surgeons are familiar with the fundamental principles of spinal oncology and are overall relatively comfortable making decisions about emergency surgery, the need for instrumented stabilization, glucocorticoid administration, tumor excision and spinal cord decompression. Stratification by annual spine tumor treatment volume indicated that the integration of measurement and decision frameworks and comfort with some of the more challenging treatment decisions was higher among clinicians who treated a higher number of tumors. Such data may guide educational efforts in specific topics where knowledge was identified to vary based on annual treatment volume. The majority of respondents also expressed a need for additional decision support in making more nuanced real-world decisions about the timing of non-emergency surgery, patient selection, tailoring the extent of surgical intervention to the patients’ survival expectancy and frailty, prevention of neurologic deterioration, and optimization of neurologic recovery potential. Currently the AO Spine KF Tumor focuses on knowledge generation to avoid and treat neurologic deficits, spinal instability, and pain using data from international prospective registries, which will meet the needs of the AO Spine community to provide decision support in real-world treatment of spine tumor patients.
The majority of surgeons use generic survival and frailty instruments to assess patients with primary and metastatic spine tumors. The validity of these generic instruments in the spine tumor population remains to be confirmed. Several survival prediction instruments were developed and validated in the metastatic spine tumor patient population; however, their utilization remains limited.16,17 The limited utilization may be attributable to usability of the instruments and lack of clear understanding about how survival predictions should influence clinical decisions. The AO Spine KF Tumor is currently working to develop survival and adverse event risk assessment instruments for patients with primary and metastatic tumors of the spine; this work will clearly meet the expressed needs of the AO Spine community.
Knowledge Translation
Knowledge Translation was introduced to reduce the gap between research evidence and its application. Knowledge Translation aims to enhance the use and usefulness of research and accelerate uptake by the community. It covers the design and conduct of studies, as well as the dissemination and implementation of findings into health care decision-making and practice. Knowledge generation and translation involve identifying important knowledge gaps, collecting and analyzing data to fill these gaps, disseminating new information to those who can use it, and facilitating its practical application.
Based on the current survey results indicating its pervasive utilization, SINS serves as an ideal example of an instrument developed to address a critical knowledge gap. SINS was created to standardize the assessment of spinal instability and to facilitate referral decisions.13,18,19 It was effectively popularized through educational efforts, and its design has allowed for successful and widespread integration into clinical practice, research and education, with our current survey indicating that over 90% of respondents use SINS.
The SOSGOQ2.0 is a PRO developed by the spine oncology study group to assess 4 domains in patients with spinal tumors. 14 While the SOSGOQ also addressed an important knowledge gap, its utilization is less widespread. This may be due to the more recent development of this instrument compared to SINS, its lower relevance and applicability to daily clinical practice, and limited dissemination efforts, including its unavailability in certain languages. Despite being proven reliable and valid, it remains relatively unknown to many, as demonstrated by the lack of awareness reported in this survey. Similarly, the AO Surgery Reference has launched Spine Tumor modules developed by experts in the field that remain underutilized. Ongoing efforts to raise awareness of these resources are essential.
The overwhelming majority of respondents indicated that they would find guidelines and classification systems useful and that they would utilize them in daily practice. While the development of guidelines requires substantial time and resource investment, they offer crucial decision support in difficult situations where time is critical, and the stakes include shortened survival, long-term disability, pain, and diminished quality of life. The AO Spine community has expressed a strong interest in such guidelines.
Limitations
The key limitations of the current analysis include challenges inherent to survey-based research, such as response bias, accessibility issues, and potential misinterpretation of questions. The high proportion of reported comfort with decisions and surgical techniques may represent response or selection bias, with people who are interested in spinal oncology being more likely to respond to the conducted survey. Some sections had lower response rates than others, which can affect the validity of the conclusions drawn. For example, the intradural tumor section yielded lower response rates than the others, likely reflecting the large number of practicing orthopedic spine surgeons who participated and do not routinely treat intradural pathology. Additionally, synthesizing themes from open-response questions requires qualitative analysis, which may overlook important concepts that were not prominently mentioned. Finally, the survey may have inadvertently omitted important themes that may require future investigation.
Conclusions
AO Spine members commonly treat patients with metastatic bone tumors and intradural tumors, with only a few surgeons treating a high number of patients with primary tumors. The majority of clinicians are comfortable making decisions around the indications for emergency surgery and spinal instrumentation and the administration of glucocorticoids. Respondents indicated the need for better decision support in determining the timing of non-emergency surgery and tailoring surgical invasiveness to oncologic benefit and patient frailty. AO Spine members expressed strong preferene for guidelines that would facilitate real-world decisions in spinal oncology.
Supplemental Material
Supplemental Material - Frontline Voice: AO Spine Member Survey Regarding Spine Oncology Knowledge Generation and Translation Needs
Supplemental Material for Frontline Voice: AO Spine Member Survey Regarding Spine Oncology Knowledge Generation and Translation Needs by Matthew L. Goodwin, Janneke I. Loomans, Ori Barzilai, Nicolas Dea, Alessandro Gasbarrini, Aron Lazáry, Cordula Netzer, Jeremy Reynolds, Laurence Rhines, Arjun Sahgal, Jorrit-Jan Verlaan, Charles Fisher, and Ilya Laufer on behalf of AO Spine Knowledge Forum Tumor in Global Spine Journal
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the AO Spine Knowledge Forum Tumor.
Ethical Statement
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
