Abstract
Hospitals face significant challenges in implementing sustainability practices to mitigate operational impacts in the post-pandemic era. This study aims to comprehensively analyze the existing literature on hospital sustainability practices and identify gaps to guide future research. A total of 62 articles published from 1988 to 2023 in the WOS and Scopus databases were systematically reviewed. The study presents sustainability performance metrics aligned with the triple bottom line (TBL) framework and highlights the complex of interactions between environmental, social and economic dimensions within the hospital setting. The findings are organized into four thematic areas: services continuity, sustainability systems and technologies, sustainability strategies for quality value, and waste minimization in hospitals. This comprehensive analysis reveals key gaps in the literature and proposes relevant directions for future research. From a theoretical standpoint, the study contributes to the contextual relevance and methodological rigor in sustainability research in healthcare. From a practical perspective, it offers a foundational framework for practitioners to better understand sustainability concepts and their implications for healthcare performance. Policymakers and regulators can also benefit form these insight to develop more effective policies aligned with Sustainable Development Goal 3 (SDG3).
Plain language summary
Hospitals are under growing pressure to reduce waste, save energy, and improve care while recovering from the challenges brought on by the COVID-19 pandemic. This study looks at 62 research articles published between 1988 and 2023 to better understand how hospitals are trying to be more sustainable. The researchers found four key areas where hospitals are focusing their efforts: keeping essential services running smoothly, using new systems and technologies, creating strategies to improve quality through sustainability, and reducing waste. The study also looks at how different factors—economic, social, and environmental—interact in complex ways when hospitals try to be more sustainable. It highlights what’s working well, what’s not, and where more research is still needed. This research helps hospital staff, managers, and policymakers understand how sustainability can improve healthcare and how to design better policies that support long-term improvements in health services. The findings are also relevant for supporting global health goals like Sustainable Development Goal 3 (good health and well-being).
Keywords
Introduction
Sustainability practices in hospitals are attracting significant attention but the aspects and interactions remain a critical point. Previous research showed that the implementation of these practices was fragmented due to ignorance and concerns about additional costs (Alboliteeh et al., 2023; Aliakbari Nouri et al., 2019; Sahal Alharbi et al., 2020). In addition, sustainability is rarely integrated into the initiative planning process at hospitals, hindering the development of effective strategies (Nagariya et al., 2022; Rodriguez et al., 2020; Vainieri et al., 2020). This fragmentation is a serious problem because of the difficulty of achieving holistic sustainability goals, which include environmental, social, and economic aspects.
Previous research showed that hospitals faced regulatory pressure and demand from stakeholders to reduce environmental footprint (Badanta et al., 2025). This pressure has intensified since hospitals are among the largest waste generators and significant resource consumers (Borges de Oliveira et al., 2022; Mehra & Sharma, 2021). The environmental impacts, such as carbon emissions and medical waste, can also have far-reaching consequences, including adverse impacts on the health, and well-being of surrounding communities (Krüger et al., 2017). Therefore, hospitals need to engage in sustainability initiatives in response to institutional and social pressures, as well as to fulfill accountability (Andrades et al., 2021; Migdadi & Omari, 2019). These efforts often conflict with the reality that hospitals have yet to establish a cohesive strategy for the widespread adoption of sustainability practices (Olawumi & Chan, 2019; Wang & Juo, 2021).
Based on the description above, several analyses have examined aspects of sustainability in hospitals. However, existing research is only focused on specific areas. In this context, McGain and Naylor (2014) offered a systematic review of hospital sustainability practices but the analysis was limited to environmental aspects such as waste recycling and renewable energy. Social and economic aspects were not addressed, such as the active role of stakeholders as catalysts to drive sustainability initiatives. This partial method reduces sustainability to mere environmental efforts and ignores the complexity and interdependence between environmental, social, and economic aspects in hospital context.
Pasqualini Blass et al. (2017) attempted to map the measurement of environmental performance in hospitals. However, the proposed framework does not specify an operationalizable measurement mechanism, increasing the difficulty of translating the concept of sustainability into concrete actions. For example, there is no clear guidance on the integration of environmental performance indicators in decision-making processes or resource allocation. In addition, the variations in operational context between hospitals were not considered, and this affected the effectiveness of implementation. Migdadi and Omari (2019) identified best practices in green operations strategies in hospitals. Even though this research successfully categorized the strategies into waste, electricity resources, non-hazardous waste, and emissions management, the social and economic aspects of the analysis were not considered. For example, the impact of these strategies on staff welfare or operational costs was not discussed in depth. Furthermore, an evaluation framework was not provided to measure the long-term effectiveness of the proposed strategies.
Lennox et al. (2020) conceptualized the sustainability method and impact through narrative summaries. Therefore, this research does not provide a structured framework for practical application. Mostepaniuk et al. (2023) reported significant challenges such as the lack of long-term data and reliance on secondary data that is unable to capture real-time dynamics. Even though important issues were identified, the synthesis did not follow a specific framework because the results were fragmented and lacked clear guidance in addressing sustainability challenges in hospitals. The diversity of sustainability practices remains poorly mapped, despite the important role hospitals in the healthcare industry. In general, sustainability initiatives are rarely integrated holistically into the planning process, hindering the development of effective strategies (Nagariya et al., 2022; Rodriguez et al., 2020; Vainieri et al., 2020). Despite efforts to promote environmentally friendly practices, the lack of comprehensive research and a deep understanding of social and economic aspects remains a major obstacle (El Khoury et al., 2023).
Considering the results, this result seeks to understand the concept of sustainability holistically by integrating the three dimensions of Triple Bottom Line (TBL) of people, planet, and profit in the context of hospitals. The method is balanced with the UN SDG-3, which emphasizes sustainability as a prerequisite for healthy living and well-being (Baeyens & Goffin, 2011). Valuable insights are provided into the current state of affairs through Systematic Literature Review (SLR), a comprehensive framework as well as future research directions regarding sustainability practices. To achieve this goal, the following research questions are proposed:
What is the current state of research on sustainability practices in hospitals?
What are the key metrics for measuring sustainability performance in hospitals?
What are the emerging themes in sustainability practices in hospitals?
What are the future research directions for sustainability practices in hospitals?
The systematic analysis is the first literature review to synthesize and summarize research by incorporating the three dimensions of TBL in hospital context. Therefore, this research makes a theoretical contribution to filling the literature gap with significant practical implications. Decision-makers are guided in the healthcare sector to implement and deliver sustainable healthcare services. In addition, this research provides academics with a summary of thematic topics as teaching and learning resources and offers a reference point for others. The results show that sustainability practices will improve operational health, service quality, and environmental performance, enabling organizations to gain a competitive advantage.
Multidimensional Discourse on Hospital Sustainability
Sustainability has become a crucial issue in evaluating the integrity and success of organizations in the modern era. Mehra and Sharma (2021) emphasized that organizational performance was assessed from economic, social, and environmental dimensions. This paradigm shift has attracted the attention of stakeholders, including in the healthcare sector. Sustainability in hospitals is becoming a relevant topic (Alboliteeh et al., 2023; Aliakbari Nouri et al., 2019; Canales et al., 2021; Sahal Alharbi et al., 2020) but the diversity has not been comprehensively mapped. Even though sustainability plays an important role in the healthcare industry, implementation often faces challenges, such as a lack of integration in the planning process and an in-depth understanding of sustainability aspects.
According to Hussain et al. (2018), sustainability practices should be reflected through planned synergies in operational activities and resource use to achieve an optimal balance between economic, social, and environmental aspects. However, the implementation of this synergy faces new challenges after the COVID-19 pandemic. World Health Organization (WHO) report in 2021 suggested that the pandemic led to a significant increase in medical waste production, while hospitals were known to be high consumers of energy and materials. The combination of these factors creates additional pressure on sustainability efforts in the healthcare sector. Li et al. (2024) found that Internet of Things (IoT) technology could improve operational efficiency, monitor real-time resource usage, and reduce waste through an integrated management system. Therefore, the integration of IoT technologies could be an effective solution to address the challenges of waste management and high resource consumption in hospitals.
Several previous research showed that the integration of green practices in hospital operations significantly improved environmental performance (Benzidia et al., 2021; Wu, 2021) The results reported the role of advanced technologies such as big data analytics and artificial intelligence (AI) in improving sustainability practices. Furthermore, Vasileiou et al. (2024) explored the integration of Green Lean Six Sigma (GLSS) in healthcare, stating that professionals recognized the potential for increased efficiency and reduced waste through sustainable practices. The concerns about limited resources and the need for comprehensive training were also stated. Dion and Evans (2024) proposed a strategic framework for energy-efficient hospital management, emphasizing the importance of green initiatives and corporate governance in reducing operational costs and environmental impact.
Jovy-Klein et al. (2024) provided a comprehensive forecast of smart hospitals by emphasizing the transformative potential of AI and digital technologies in shaping the future of healthcare. In 2042, smart hospitals will leverage AI to improve operational efficiency, patient-centered care, and sustainability practices while overcoming challenges such as staff shortages and ethical considerations. Additionally, Badanta et al. (2025) emphasized the role of healthcare institutions in promoting sustainability, advocating actions such as sustainable food systems, waste management, and healthcare pollution reduction.
Despite the progress, the implementation of sustainable practices faces various challenges. Cowie et al. (2020) identified several key barriers such as financial constraints, regulatory complexity, and resistance to change. There is also a debate on the most effective metrics to measure and compare sustainability performance between healthcare facilities. This discussion has resulted in two different views. Some research are in line with the standardized sustainability reporting framework specific to the healthcare sector. Meanwhile, others support a more flexible and contextual method (Haq et al., 2022; Polese et al., 2018). These divergent views show the need for further research to develop strong sustainability assessment tools widely applied in hospitals. Collectively, the sustainability discourse in hospital context has evolved from a narrow focus on environmental impacts to a more comprehensive method. This includes economic viability and social responsibility, in line with the triple bottom-line framework. The development shows the potential for hospitals to reduce environmental footprint and improve operational efficiency without compromising the quality of healthcare services.
Method
Design
The research articles were selected based on Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) framework (Moher et al. (2009). PRISMA method has advantages over traditional literature review. The method adopts a well-defined process for literature review and selection criteria. Following these guidelines, relevant literature has been collected and analyzed. In this research, the analysis of empirical and theoretical evidence from articles has been peer-reviewed to reduce the possibility of bias.
Search Process and Outcomes
The review process started with article identification. The main sources of literature used in the analysis were Web of Science (WoS) and Scopus databases. These databases (i) provided literature searches with a wide geographical and thematic coverage. (ii) covered diverse fields in the social and natural sciences and (iii) were widely used in academic research (Álvarez Jaramillo et al., 2019; Fahimnia et al., 2015; Parmentola et al., 2022). In addition, search phrases were developed based on discussions with the research team, whose expertise spans the fields of sustainability, public sector management, accounting as well as project and operations management. Keywords used to extract articles related to sustainability in hospitals were (i) ESG AND hospital, (ii) health AND ESG performance, (iii) health AND sustainability performance, (iv) social performance AND hospital, (v) economic performance AND hospital, (vi) environmental performance and hospitals.
The search effort was conducted in February 2023 with no specific limitation on the year of publication. The period of 1988 to 2023 was selected for a more comprehensive coverage of the evolution of sustainability practices in hospitals. This period allows for tracking significant changes in regulation, technology, and sustainability priorities as well as identifying long-term trends. Collectively, the search identified 5,336 documents that were further filtered based on the established inclusion and exclusion criteria.
Inclusion Criteria and Validity
The subsequent step screened the publications based on inclusion and exclusion criteria (1) Dissertations, books, technical reports, and conference proceedings were excluded and only articles were selected, (2) Articles belonging to the subject areas Business, Management and Accounting; Environmental Science; Economics, Econometrics, and Finance, and (3) Articles published in English. To overcome the challenges arising from the wide period, additional inclusion criteria were applied. Articles from the early years (1988–2000) were included after meeting rigorous methodological standards and were relevant to the current sustainability context. Furthermore, articles from the most recent period (2010–2023) were prioritized due to the reflection of current sustainability practices and hospital operational challenges. The complete inclusion and exclusion criteria applied in this study are summarized in Table 1.
Inclusion and Exclusion Criteria.

The next stage is to manually check all articles in the Scopus and Web of Science databases to ensure that there are no duplications or inconsistencies. To avoid subjective bias, two other research review the manual process and verify the results. In the event of disagreement, the articles are re-evaluated until a consensus is reached. The overall screening process is reported in Figure 1. The final collection consists of 62 articles that were screened based on the search-related area and assessed for feasibility through a full-text review.

Diagrammatic view of the selection process based on Moher et al. (2009).
Data Extraction
According to Durach et al. (2017), a standardized data extraction form was used to obtain data from 62 articles to minimize the occurrence of bias in the research. The standardized data extraction form contains specific (author, publication date, and title) and general information (research objectives, methods, results, research context, and journal) for coding.
Synthesis
The next step was to verify the titles, authors, journal names, and publication years in the cleaned list of articles and ensure the matching of the content. NVivo software was used to facilitate data coding and organization to systematically analyze the 62 selected articles. This process started with uploading all articles to NVivo through imported data from Mendeley, followed by initial code development based on TBL framework. Coding was carried out manually by two independent research to ensure reliability. Subsequently, the extracted data were triangulated with each other according to the methodology recommended by Durach et al. (2017) to strengthen the consistency and validity of the results. The analysis was centered on sustainability practices in hospitals covering the three dimensions of TBL. NVivo identified relationships between themes and emerging patterns, with the visualization capabilities to enhance data interpretation. From each theme, existing assumptions about sustainability practices were critiqued in depth to develop new knowledge.
Results and Analysis
This section analyzes the descriptive results of the 62 sample articles, including annual publication trends, methods, theoretical frameworks, journal distribution, and theoretical lenses used.
What is the Current State of Academic Research on Sustainability Practices in Hospitals?
Publication Over Time
The systematic literature review reported that academic attention to sustainability in hospitals was reported in 1988. Generally, publications on this topic showed a significant increase from the late 1990s to 2023, with distinct phases reflecting the evolution of sustainability research in healthcare.
The initial phase of 1988 to 2005 showed a relatively low and fluctuating level of publication, indicating that the sustainability of hospitals was still in the early exploratory stage. In 2008, an increase marked a turning point, leading to increased recognition of the topic in the scientific community. This increase coincided with a strengthening of global environmental awareness penetrating the health sector. Badanta et al. (2025) observed that the phenomenon was partly driven by stringent regulatory pressures on hospital institutions.
Furthermore, there was a decline in publications from 2011 to 2016. Li et al. (2024) stated that this period was a consolidation phase where research focused on deepening methodological methods rather than expanding the volume. The decline in publications also reflects a shift in research priorities after the 2008 global financial crisis.
The years 2017 to 2023 were characterized by exponential growth in publications, placing hospital sustainability as the main research focus in academic literature. This significant increase is driven by rapid technological advances, dynamic developments in sustainability policies, and the implementation of environmentally responsible healthcare. Influential works during this period include Abdul Rahman et al. (2020), Atia et al. (2020), Bem et al. (2019), Canales et al. (2021).
The latest trends show significant publication growth. Jovy-Klein et al. (2024) identified the development of a new focus in the form of integrating AI with sustainability practices. This shows that this field of research has entered a more complex phase of evolution. The integration of cutting-edge technology has made a significant contribution to optimizing the effectiveness and efficiency of sustainable practices in the operational context of hospitals.
Figure 2 illustrates the trajectory of publications over the past decades, showing a quantitative increase in the number of research. The trend in publications also provides a substantial qualitative evolution in the conceptualization of hospital sustainability from an environmental to an integrated method.
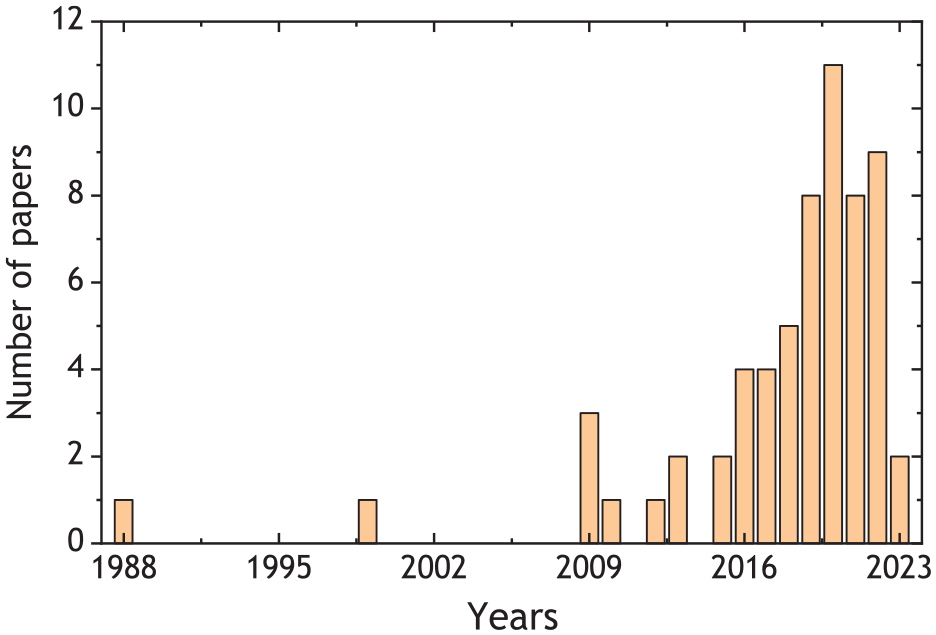
Research output over time.
Research Methods
Analysis of methods shows the diversity of approaches used in hospital sustainability research. The distribution of research methods is illustrated in Figure 3. From the 62 articles reviewed, case research dominates with a proportion of 27.42%, indicating a preference for exploring the implementation of sustainability practices in specific contexts. This in-depth method allows for a more comprehensive understanding of the unique dynamics influencing the adoption of sustainability in real-life situations. According to Vasileiou et al. (2024), this method has limitations in the generalization of the results.

Proportion of methods employed by the sampled articles.
Quantitative methods such as surveys (19.35%), archival (8.06%), and experiments (3.32%) were used to test statistical relationships and measure the impact of sustainability initiatives. The low use of experimental methods reflects the practical challenges of implementing experimental designs in complex hospital environments. Meanwhile, qualitative methods (17.74%) play an important role in exploring aspects that are difficult to measure quantitatively, such as stakeholder motivation and implementation barriers.
The distribution of these methods shows important gaps in current research. The limited number of mixed-methods (6.45%) and longitudinal research, as emphasized by Jovy-Klein et al. (2024), hinders a comprehensive understanding of sustainability practices. In addition, the low proportion of experimental research reports the need for a more rigorous method to evaluate the effectiveness of sustainability interventions in hospitals.
Journals of the Sampled Articles
The sampled articles were published by 42 journal publishers. These journals cover the fields of sustainability, environmental management, socioeconomics, business ethics, and technology. Figure 4 shows that the journal “Sustainability” and the “Journal of Cleaner Production” are the two main sources publishing the most articles related to this topic. The two journals play an important role in supporting and promoting research on sustainability in the health sector. This distribution pattern shows the importance of the topic in the realm of sustainability and reports a representation gap in certain journals.

Most productive journals on sustainability in hospitals.
The dominance of publications in journals focused on sustainability reflects an important phenomenon identified by Vasileiou et al. (2024), namely the segregation of academic discourse in which the perspectives of health are still not optimally integrated. Journals such as Health Care Management Review have made relatively limited contributions, indicating significant opportunities to integrate sustainability perspectives into the mainstream of health management research.
The multidisciplinary nature of the topic is evident from the diversity of journals publishing related articles. However, the uneven distribution shows academic “silos” affecting cross-disciplinary knowledge transfer. According to Badanta et al. (2025), the integration of perspectives from various disciplines is essential for developing a holistic method for hospital sustainability. Publication gaps in certain journals offer strategic opportunities to broaden the scope of literature and enrich the discourse with more diverse perspectives.
Theoretical Lenses
Analysis of sample articles shows the diverse theoretical frameworks used. This diversity reports the complexity of the phenomenon of sustainability, which requires perspectives from various disciplines to be understood comprehensively. TBL is the dominant framework used to evaluate the balance between the economic, social, and environmental dimensions in hospital sustainability practices (Aliakbari Nouri et al., 2019; Migdadi & Omari, 2019; Rodriguez et al., 2020). Jahani Sayyad Noveiri and Kordrostami (2021) using Fuzzy DEA models to evaluate the efficiency and sustainability performance of health systems from economic, social, and environmental dimensions.
Several research use this theory with Intuitionistic Fuzzy Cognitive Map (IFCM) method to build a causal model of a sustainable supply chain (Mirghafoori et al., 2018). This method provides a decision-making framework to manage supply chains sustainably. Meanwhile, Institutional Diffusion Theory (Kennedy & Fiss, 2009), Legitimacy theory, agency theory (Bai, 2013; Couto et al., 2022), environmental sustainability theory (Pasqualini Blass et al., 2016), social construction theory (Aubry et al., 2014), theory of change (ToC; Ryan-Fogarty et al., 2016), economic theory (Pantzartzis et al., 2017), competing values theory (Aubry et al., 2014), social justice theory (Cai et al., 2017), performance management theory (Palozzi et al., 2018), strategic management theory (Palozzi et al., 2018) and stakeholder theory (El Khoury et al., 2023; Seifert & Guenther, 2020) are used to analyze sustainability practices from institutional and stakeholder perspectives.
Even though theoretical diversity enriches understanding, critical analysis shows significant fragmentation in the use of the theories. Several research apply theories in isolation without adequate integration, reflecting gaps in understanding the complex interactions between the various dimensions of sustainability. However, the available empirical evidence is still limited in reporting the real impact of applying the theories in sustainability practices. Future research needs to develop a more integrated theoretical framework by combining various perspectives to provide a more holistic understanding of hospital sustainability. A multi-theoretical method that bridges the gap between the environmental, social, and economic dimensions strengthens the conceptual foundation of research in this field.
What Are the Key Metrics for Measuring Sustainability Performance in Hospitals?
In answering the second research question, this review identifies the sustainability performance metrics used by hospitals. The metrics are categorized into three dimensions, namely economic, environmental, and social, in line with TBL method. In the economic dimension, metrics such as sustainable funding, Affordability of Technology, cost-effectiveness, and return on investment (ROI) are used to assess financial performance. In the environmental dimension, the main focus is on reducing carbon emissions, medical waste management, and energy efficiency. Meanwhile, in the social dimension, patient satisfaction, staff engagement, and employee welfare are important indicators. The use of these metrics provides a comprehensive framework for integrating sustainable practices into hospital operations.
Economic Performance
This review identifies four main categories in the context of hospital economic sustainability, namely sustainable funding, affordability of technology, cost-effectiveness, and Return on Investment (ROI). The categories reflect the key aspects necessary to ensure the sustainable financial performance of hospitals. Sustainable funding (Bem et al., 2019; Couto et al., 2022) emphasizes the importance of long-term funding to maintain hospital operations. The affordability of technology (Benzidia et al., 2021; Farah et al., 2020) focuses on the ability of hospitals to adopt cost-effective and sustainable technologies. Cost-effectiveness (Atia et al., 2020; Stevanovic et al., 2019) measures efficiency and resource allocation, while ROI (Curtis & Roupas, 2009; Roh, 2019) assesses the financial impact of sustainability initiatives. These four categories are interrelated and form a comprehensive framework for evaluating the economic performance of hospitals. Table 2 shows the results of a review focusing on the economic performance of hospitals.
Economic Performance Metrics in Hospitals Identified in the Literature.
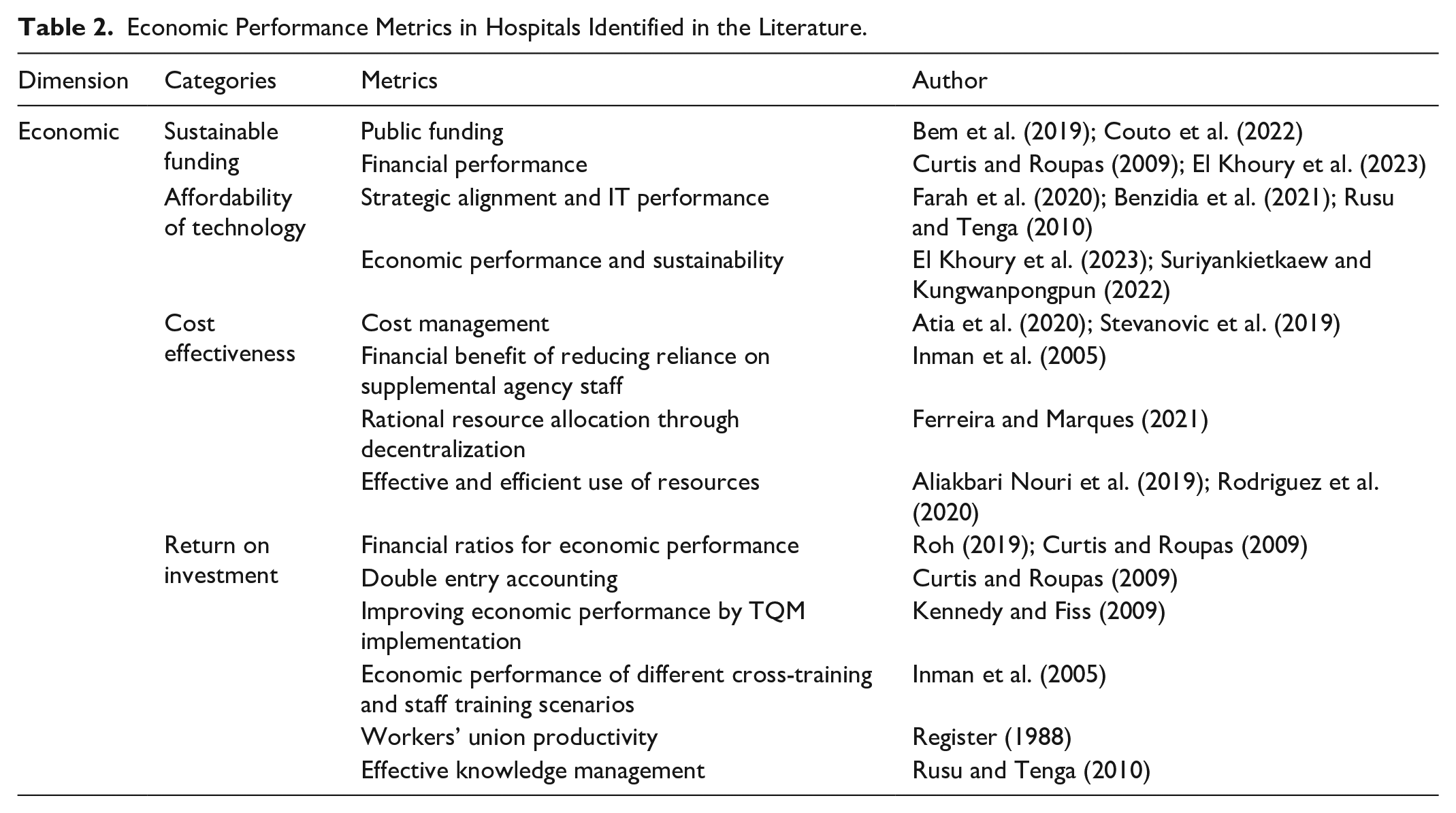
Analysis of current literature shows that the metrics in the categories of sustainable funding, cost-effectiveness, and affordability of technology are interrelated in achieving the economic sustainability of hospitals. In the sustainable funding category, the metrics of public funding (Bem et al., 2019) and financial performance (Curtis & Roupas, 2009; El Khoury et al., 2023) are key to ensuring long-term stability. Public funding ensures that hospitals have a consistent source of funding, while financial performance measures the ability to manage resources efficiently. In the cost-effectiveness category, the metrics of cost management (Atia et al., 2020; Stevanovic et al., 2019) and efficient use of resources (Aliakbari Nouri et al., 2019; Rodriguez et al., 2020) play an important role in optimizing resource allocation. This efficiency reduces operational costs and supports sustainable funding by ensuring that limited resources are used optimally. In the category of affordability of technology, the strategic balance and IT performance metric (Farah et al., 2020; Benzidia et al., 2021) show that renewable energy management systems and advanced diagnostic tools can improve operational efficiency. This technology reduces long-term costs and contributes to ROI by increasing productivity and service quality.
Measurement tools such as financial ratios and balanced scorecards (Aliakbari Nouri et al., 2019; Sherman et al., 2020) are important in assessing the economic performance of hospitals. A balanced scorecard allows the integration of financial and non-financial metrics into a holistic reporting system. Sophisticated methods, such as fuzzy DEA (Jahani Sayyad Noveiri & Kordrostami, 2021) are used to measure operational efficiency by considering the uncertainty and complexity of hospital systems. The implementation of Total Quality Management (TQM; Kennedy & Fiss, 2009) also contributes to improving economic performance by enhancing service quality and operational efficiency. However, challenges remain, such as the lack of exploration of innovative metrics including social return on investment (SROI). This shows the need for a more holistic method of measuring the economic sustainability of hospitals, specifically in the face of contemporary challenges such as the COVID-19 pandemic (Haq et al., 2022).
The implementation of economic sustainability metrics, such as sustainable funding, cost-effectiveness, and affordability of technology, has significant practical implications for hospitals. First, hospitals can develop integrated reporting systems to monitor economic performance in real-time and ensure optimal resource allocation. Second, investment in cost-effective technologies improves operational efficiency and contributes to ROI and long-term financial resilience. Third, a holistic method that combines financial and non-financial metrics, such as fuzzy DEA, and SROI, can help hospitals measure the impact of sustainability more comprehensively. In the face of contemporary challenges such as the COVID-19 pandemic, the integration of metrics is becoming increasingly important to ensure the financial and operational resilience of hospitals. Generally, the framework supports the achievement of financial goals and ensures that sustainability practices are implemented effectively and sustainably.
Environmental Performance
In the context of hospital environmental sustainability, this review identifies six main categories, namely legal, organizational, and individual readiness, technology support, management and political support, capacity building, and policy. These categories reflect the key aspects necessary to ensure the sustainable environmental performance of hospitals. For example, in the legal category, compliance with standards (Alsawaf & Albadry, 2022; Seifert & Guenther, 2019) and environmental regulation control (Sherman et al., 2020; Stevanovic et al., 2019) are the basis for ensuring the compliance of hospitals with environmental regulations. In the technology support category, metrics such as technical implementations (Alsawaf & Albadry, 2022; Borges de Oliveira et al., 2021) and technical efficiency (Borges de Oliveira et al., 2021; Stevanovic et al., 2019) focus on the adoption of environmentally friendly resource efficiency. Table 3 presents the main elements contributing to environmental performance.
Environmental Performance Metrics in Hospitals Identified in the Literature.
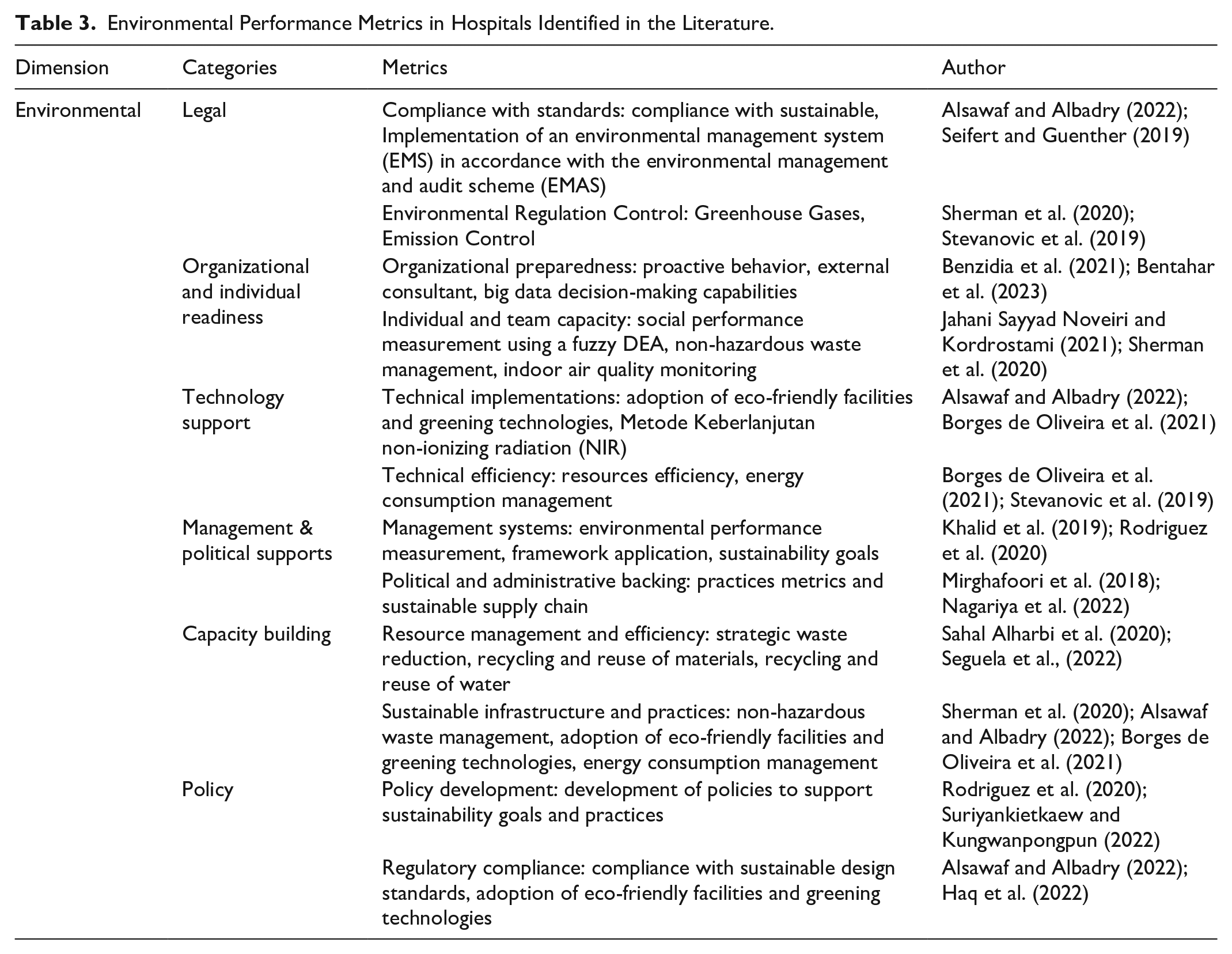
Analysis of current literature shows that metrics in the categories of technology support, capacity building, legal, organizational, and individual readiness, management and political supports, as well as policy, are interrelated in achieving hospital environmental sustainability. In the legal category, compliance with standards (Alsawaf & Albadry, 2022; Seifert & Guenther, 2019) and environmental regulation control (Sherman et al., 2020; Stevanovic et al., 2019) are the foundation for ensuring compliance with regulations. This compliance reduces legal risk and supports management by building stakeholder trust. In the organizational and individual readiness category, preparedness (Jahani Sayyad Noveiri & Kordrostami, 2021; Sherman et al., 2020) showed that readiness and individual capacity were essential in adopting sustainability practices. For the technology support category, the adoption of eco-friendly facilities (Alsawaf & Albadry, 2022) and energy consumption management (Borges de Oliveira et al., 2021) play a key role in reducing environmental impacts, such as carbon emissions and medical waste. In the capacity building category, resource management and efficiency (Sahal Alharbi et al., 2020; Seguela et al., 2022) as well as sustainable infrastructure and practices (Sherman et al., 2020; Alsawaf & Albadry, 2022) support optimal infrastructure development. In the policy category, development (Rodriguez et al., 2020; Suriyankietkaew & Kungwanpongpun, 2022) and regulatory compliance (Alsawaf & Albadry, 2022; Haq et al., 2022) ensure that hospitals have a clear framework to support sustainability initiatives. The interrelationship among these categories is reinforced by the balance of legal compliance and policy development with technology support and capacity building. Meanwhile, organizational readiness and management support contribute to the effective implementation of the initiatives. The challenges include the lack of exploration of innovative metrics holistically integrating social and environmental impacts.
The implementation of environmental sustainability metrics has significant practical implications. First, hospitals can adopt integrated environmental management systems to ensure compliance with standards and improve operational efficiency. Second, investment in environmentally friendly technologies, such as renewable energy systems and medical waste management reduces environmental impact and supports long-term cost savings. Third, strengthening staff capacity and clear policy support ensures the effective implementation of sustainability practices. In the face of challenges such as climate change and the COVID-19 pandemic, the integration of these metrics ensures the environmental and operational resilience of hospitals. This framework supports the achievement of environmental goals and sustainable operations.
Social Performance
In the context of the social sustainability of hospitals, this review identifies four main categories, namely ethical, behavioral, cultural, and stakeholder. These categories reflect the key aspects needed to ensure the sustainable social performance of hospitals. For example, in the ethical category, the metrics of social accountability (Aliakbari Nouri et al., 2019) and community engagement (Rodriguez et al., 2020) are the basis for ensuring that hospitals are socially responsible and actively engaged with the community. In the behavioral category, employee perception of TQM adoption (Kennedy & Fiss, 2009) and cross-training nurses (Inman et al., 2005) focus on staff behavior and participation in supporting sustainability practices. Table 4 presents the practice metrics showing social performance in hospitals.
Social Performance Metrics in Hospitals Identified in the Literature.

The metrics in the stakeholder, culture, behavioral, and ethical categories support each other in achieving the social sustainability of hospitals. The stakeholder category (Rodriguez et al., 2020; Wongsin et al., 2022; Rodriguez et al., 2020; Suriyankietkaew & Kungwanpongpun, 2022) shows that patient satisfaction and employee well-being are important indicators of social performance. Alboliteeh et al. (2023) emphasized that hospital sustainability started with patient satisfaction and quality care. In the behavioral category, cross-training hospital nurses (Inman et al., 2005; Ilea et al., 2020) and employee perception of TQM adoption (Kennedy & Fiss, 2009) play an important role in increasing operational flexibility and human resource efficiency. Furthermore, cross-training and the adoption of TQM increase labor productivity and create a work environment supporting innovation and continuous improvement. The culture category creates a foundation for learning, growth, and innovation through the metrics of organizational culture for big data (Benzidia et al., 2021) and organizational values (Suriyankietkaew & Kungwanpongpun, 2022). For example, the adoption of modern (Benzidia et al., 2021) and effective information technology governance (Rusu & Tenga, 2010; Borges de Oliveira et al., 2022) can improve the sustainability of hospitals.
The Stakeholder category represents the most complex dimension of hospital sustainability, reflecting a diverse, dynamic and often conflicting ecosystem of interests. Recent research suggests a fundamental tension between improving patient experience (Rodriguez et al., 2020; Wongsin et al., 2022) and optimizing employee well-being (Suriyankietkaew & Kungwanpongpun, 2022). Alsawaf and Albadry (2022) identified that hospitals must balance three interrelated imperatives: patient satisfaction, staff engagement, and operational efficiency-without sacrificing any of them. This dynamic creates a “sustainability trilemma” where decisions that improve one dimension may negatively impact another. For example, cost reduction efforts for economic sustainability may limit resources for staff well-being initiatives, which in turn may affect the quality of patient care.
In the ethical category, social accountability (Aliakbari Nouri et al., 2019) and community engagement (Rodriguez et al., 2020) ensure that hospitals are socially responsible and actively engaged with the community. The relationship between these categories is strengthened by the relationship between strong organizational culture and effective stakeholder engagement to support the holistic implementation of sustainability practices. However, the challenges include lack of exploration of innovative metrics that holistically integrate social and economic impacts through the fuzzy DEA (Data Envelopment Analysis) method (Jahani Sayyad Noveiri & Kordrostami, 2021). A promising method is fuzzy DEA, which enables the measurement of social performance by considering the uncertainty and complexity of hospital systems. DEA can be used to evaluate operational efficiency while considering social impacts, such as patient satisfaction and employee well-being in providing a more comprehensive social sustainability.
What Are the Developing Themes in Sustainability Practices in Hospitals?
This section presents a thematic discussion of the issues addressed by the sample articles in the context of sustainability practices. An interpretive philosophical perspective argues that access to reality can be gained through social construction and shared meaning, reflecting the various problem areas (Willis, 2007). The abstracts and full texts of all selected articles were analyzed thematically using NVivo software to identify developing themes.
Figure 5 present the conceptual framework for sustainability in hospitals, which is built on three interconnected pillars, namely Economic, Environmental, and Social. These pillars support Service Continuity, System and Technology, Sustainability Strategy, and Waste Minimization to achieve Quality Value. The framework also shows two important factors influencing implementation, namely Barriers and Enablers.

Conceptual framework in sustainability in hospital. Source: created by Nvivo.
Continuity Services in Hospital
Continuity services are a crucial aspect in achieving sustainability, specifically in the face of increasingly fierce global competition and ever-higher demands on the quality of health. This concept is closely related to performance management and service quality, which are the main foundations for maintaining operational resilience and patient satisfaction (Mitleton-Kelly, 2011). Additionally, Lee (2020) emphasized that service quality must be continuously improved and carefully measured.
The implementation of effective continuity services is influenced by several key factors. leadership and management commitment to sustainability are fundamental factors that drive organizational culture change and ensure the integration of sustainability practices into hospital operational strategies (Bai, 2013). Aubry et al. (2014) on hospitals in Canada showed that strong leadership was the main catalyst in the successful implementation of an electronic management system to track patients and drug stocks. This system has succeeded in reducing medical errors and significantly improving operational efficiency. The success drives organizational culture change and overcomes resistance to the new system.
Effective information technology (IT) integration is also a significant supporting factor in the implementation of continuity services. A well-integrated IT system improves operational efficiency and helps hospitals monitor resources more effectively (Jahani Sayyad Noveiri & Kordrostami, 2021; Rusu & Tenga, 2010). Hospitals in Singapore have shown the successful integration of IT by adopting IoT system to monitor energy use and medical waste (Li et al., 2024). This system allows the identification of areas that need improvement in energy efficiency and waste management, reducing carbon footprint. Comprehensive training and active staff participation also contribute significantly to successful implementation. Cross-training strategies have proven effective, as reported by hospitals in Sweden that have succeeded in improving service quality and reducing staff turnover (Inman et al., 2005).
The implementation of continuity services faces a variety of complex challenges despite various examples of success. Limited resources are a major challenge, specifically in developing countries with tight budgetary constraints (Ilea et al., 2020). According to World Bank (2022), more than 50% of hospitals in low-income countries have difficulty maintaining basic services due to budget constraints, affecting the implementation of more efficient systems. For example, the healthcare waste management (HCWM) initiative in India failed after the initial phase because local conditions and inadequate infrastructure were not considered (Thakur et al., 2021). However, Seifert and Guenther (2020) stated that some hospitals successfully implemented Environmental Management Systems (EMS) with effective communication and increased staff awareness as keys to success. According to Benzidia et al. (2021), hospitals that successfully overcame barriers to adopting big data analytics and artificial intelligence (BDA-AI) in green supply chains showed high environmental performance through a gradual method and continuous staff training.
The implementation of continuity services is complicated by the complexity of regulations and changing service standards. In addition, regulations on medical waste management and different energy efficiency targets in each country create barriers to system standardization (Pantzartzis et al., 2017; Strotmann et al., 2017). On the technology side, dependence on high-powered medical equipment and fragmented IT systems is a challenge in reducing carbon footprint (Farah et al., 2020). Issues of data security and patient privacy also add complexity, creating a dilemma between innovation and the protection of sensitive information.
A comparative analysis of the success and failure factors of continuity services implementation shows several significant patterns. In this context, the presence of strong leadership is a determining factor in overcoming resistance to change. Benzidia et al. (2021) emphasized the importance of transformational leadership in the adaptation of green supply chain technology. Seifert and Guenther (2020) also stated that comprehensive staff training significantly improved the successful implementation of Environmental Management Systems by addressing barriers related to human resource capacity. Mehra and Sharma (2021) added an important dimension by emphasizing that contextual factors such as technological infrastructure, regulatory support, and economic conditions created striking differences in the implementation of sustainability practices between healthcare facilities in developed and developing countries. Thakur et al. (2021) reported that a gradual method for local conditions led to a higher rate of adoption in healthcare waste management than a comprehensive implementation ignoring the context.
The implementation of continuity services requires a holistic and contextual method considering technical, human, organizational, external, and environmental dimensions. Furthermore, investments in leadership development, comprehensive training programs, and integrated IT systems, as well as effective change management, significantly increase the chances of success. Collaboration with external stakeholders, including policymakers and funding agencies, can also overcome resource, and regulatory challenges in achieving sustainable continuity services.
Sustainability Systems and Technologies in Hospitals
Sustainability systems and technologies are becoming increasingly important in efforts to improve efficiency and reduce environmental impact (Rusu & Tenga, 2010). With rapid advances in IT and AI, this method has evolved significantly, offering innovative solutions and presenting complex implementation challenges.
The integration of Big Data Analytics (BDA) and AI has been proven to improve the environmental performance of hospitals. Benzidia et al. (2021) on 168 hospitals in France showed that BDA-AI technology had a positive effect on internal and external environmental integration, significantly improving performance. BDA-AI enables hospitals to optimize the green supply chain by accurately predicting drug demand, reducing excess stock, and minimizing waste. Similarly, digital learning acts as an important moderator in strengthening the relationship between environmental integration and performance. Despite the provision of substantial benefits, the adoption of technology is often affected by inadequate digital infrastructure.
Jovy-Klein et al. (2024) expanded that AI served as the backbone of smart hospital transformation. The successful implementation depends heavily on the availability of high-quality data, the technical expertise of staff, and consistent support from senior management. Conversely, technology implementation failures are often caused by system interoperability challenges, resistance from medical personnel concerned about reduced professional autonomy, and the lack of a clear regulatory framework for AI in the health sector. The case of hospitals in Scandinavia shows a gradual method of AI implementation, starting with a focused pilot project before full-scale, significantly increasing the likelihood of successful adoption.
Integration methods such as Green Lean Six Sigma (GLSS) are a solution to improve operational efficiency and environmental sustainability. Vasileiou et al. (2024) found that GLSS had great potential to reduce waste, improve service quality, and support environmentally friendly practices. The successful implementation depends on the long-term commitment of management, the participation of staff from various levels, and integration with existing quality management systems. Meanwhile, challenges in the implementation can be overcome by using advanced technologies such as IoT to monitor energy use and waste, and adopting digital-based training programs to improve staff skills (Li et al., 2024; Seifert and Guenther (2020).
As a complement to GLSS focused on process efficiency, a structured method is needed for hospital waste management. Thakur et al. (2021) developed a comprehensive Healthcare Waste Management (HCWM) evaluation framework to assess medical waste management practices. Even though the framework is promising, the implementation of advanced technologies is often affected by inadequate monitoring infrastructure and a lack of standardization, specifically in developing country health facilities. GLSS and HCWM offer systematic methods that can help hospitals integrate sustainability into day-to-day operations.
For the measurement and impact assessment of sustainability systems, several comprehensive methods have been developed. The right evaluation method is needed to measure the implementation of the technology. Pasqualini Blass et al. (2016) proposed a three-phase framework for evaluating environmental performance but the success depends on the availability of accurate data. In this context, Seifert and Guenther (2020) evaluated the effectiveness of EMAS in EU hospitals, which required institutions to conduct periodic environmental audits, transparency of performance reporting, and continuous improvement. EMAS hospitals show significant success in energy savings, waste reduction, and decreased carbon emissions, with implementation supported by a clear regulatory framework and economic incentives for environmental compliance. Jahani Sayyad Noveiri and Kordrostami (2021) complement this method by developing a fuzzy DEA aggregation for sustainability assessment. Therefore, the integration of frameworks, evaluation methods, and advanced technologies such as AI and big data analytics supports the measurement and assessment of sustainability impacts and ensures the achievement of goals without compromising service quality. This integrated method is key for modern hospitals in facing the challenges of efficiency and environmental compliance.
Sustainability Strategy in Hospitals to Create Quality Value
Sustainability strategy in hospitals creates quality value through the integration of practices in daily operations. This strategy aims to reduce environmental impact while improving operational efficiency, service quality, and financial sustainability. Suriyankietkaew and Kungwanpongpun (2022) reported that 20 of 23 strategic leadership practices significantly improved sustainability performance in Thai healthcare organizations, including staff development, good working relationships, and effective leadership. However, the implementation is often affected by hierarchical structures and cultural resistance.
Furthermore, the integration of a sustainability strategy into hospital operations requires a systematic method. Ryan-Fogarty et al. (2016) reported the success of environmental programs through strong leadership, staff participation, and consistent measurement. Implementation success factors include senior management support, transparent communication, and a gradual method. In contrast, integration failures are due to poor top-down communication, weak monitoring systems, and conflicts of priorities between sustainability goals and short-term operational demands. In complementing the systematic method, Pinzone et al. (2012) emphasized the importance of combining the organizational and architectural levers of hospitals. This is because sustainability strategy must be integrated with the entire structure and processes. Institutions adopting an integrated system method show higher success rates, while partial implementations without considering interconnections between departments often experience coordination barriers and conflicts of interest. As an important component in sustainability strategy, performance measurement and evaluation is a crucial aspect. Khalid et al. (2019) and Aliakbari Nouri et al. (2019) developed balanced scorecard models that integrated environmental dimensions, providing a comprehensive framework for assessment. Challenges in implementing this measurement framework include data collection complexity, lack of metrics standardization, and the difficulty of linking environmental performance to financial and clinical outcomes. Generally, successful hospitals adopt a phased method, starting with measurements in priority areas before expanding to other aspects of sustainability.
As a practical application of the previous measurement framework, Migdadi and Omari (2019) reported the taxonomy of best practices in green operations strategy in hospitals. The research identified effective strategies and reported the implementation gaps due to resource constraints and technical competency limitations. In addition, hospitals in developing countries face additional challenges in the form of limited access to advanced technology, shortage of technical expertise, and competing priorities related to basic healthcare service provision. The success factors in the implementation of a green operations strategy include the availability of relevant technical expertise, adequate supporting infrastructure, and long-term commitment from stakeholders. This taxonomic method complements the balanced scorecard models, providing a more specific operational framework for applying sustainability principles in the daily practice of hospitals.
The adaptability of the sustainability strategy to crises is a crucial factor, as reported during the COVID-19 pandemic. Rodriguez et al. (2020) and Haq et al. (2022) showed that institutions with a mature sustainability strategy integration adapted effectively to disruption. Success factors in the adaptation include resource allocation flexibility, strong digital capabilities, and a cross-departmental collaborative method. Conversely, hospitals positioning sustainability as an “add-on” rather than an integral element experienced significant difficulties in maintaining sustainability initiatives.
To identify key factors in sustainability management, Mirghafoori et al. (2018) developed a causal model based on IFCM. This model is effective in institutions with strong analytical capabilities. However, the implementation is often affected by limited technical abilities and inadequate data infrastructure. Haq et al. (2022) expanded on this understanding through partial least squares structural equation modeling (PLS-SEM), stating the significant contribution of green practices, employee attitudes, and organizational participation to environmental performance. Even though technical factors are important, human and organizational culture are often the primary determinants of the success of sustainability strategy implementation.
In the context of the economic pressures faced by many hospitals, the impact of sustainability strategies on financial aspects is an important consideration. Curtis and Roupas (2009) and Bem et al. (2019) showed the effects of sustainability strategies on financial performance through statement analysis. This research reported that hospitals successfully integrating sustainability strategies comprehensively showed high operational efficiency and long-term cost savings. Roh (2019) complemented the perspective by measuring the economic performance of community hospitals using non-parametric methods. The positive relationship between sustainability practices and economic efficiency was also reported with the challenges in quantifying the indirect value of sustainability initiatives.
The implementation of a sustainability strategy to create quality value requires a comprehensive method in line with the complexity of healthcare organizations. This depends on a combination of strong leadership, systemic integration, consistent measurement, and a supportive organizational culture. The challenges and obstacles faced from limited resources to resistance to change can be overcome through a phased method.
Strategies to Minimize Waste in Hospitals
Strategic efforts to minimize the environmental impact of hospitals are important for global sustainability. In reality, the practice of waste minimization varies between countries, depending on policy priorities and the availability of local resources. Methods such as green development, waste management, and energy efficiency protect the environment and provide competitive advantages through cost savings and a positive image (Borges de Oliveira et al., 2021; Khalid et al., 2019).
Several research showed that consistent hospital waste management was consistently the highest priority in sustainability efforts (Thakur & Sharma, 2021; Seifert & Guenther, 2020; Seguela et al., 2022). In this context, water recycling and energy conservation were reported as crucial aspects. The strategies have the potential to reduce the carbon footprint and offer long-term cost efficiency. However, the implementation faces complex challenges, ranging from financial and technical obstacles to cultural resistance and regulatory limitations.
Water Recycling
Healthcare facilities consume very large amounts of water. This makes water recycling an important issue in hospital sustainability. The Victorian Department of Health, Australia, reported that 20% to 40% of total water use was for sanitation and sterilization in hospitals (Thakur & Sharma, 2021). Even though water recycling was an important agenda, Nagariya et al. (2022) stated that the implementation scored low on hospital sustainability indexes in many countries. These results showed a gap between urgency and practice on the ground.
Several water recycling implementation strategies have been developed to address the issue. The first, second, and third strategies are the construction of water treatment plants for filtering hazardous waste before disposal, the development of rainwater collection systems, and the implementation of recycling systems for non-consumption purposes, respectively (Dhillon & Kaur, 2015). A critical evaluation of recycling procedures is also needed to ensure quality and reduce the risk of contamination (Thakur et al., 2021). Seguela et al. (2022) proved that an effective water conservation strategy could reduce desalinated water consumption, mitigate environmental impacts, and lower hospital operating costs.
Case research of hospitals in several countries showed patterns of success and failure in the implementation of water recycling. Seifert and Guenther (2020) identified top-level management commitment as a key factor, where hospitals with explicit support from executives showed higher success rates. Thakur et al. (2021) reported that hospitals with a dedicated budget allocation for sustainable water recycling infrastructure developed effective comprehensive systems. According to Seguela et al. (2022), institutions with adequate investment succeeded in significantly reducing desalinated water consumption, mitigating environmental impacts, and lowering operational costs.
The analysis showed several main factors for implementation failure. Borges de Oliveira et al. (2021) found that high initial investment costs without calculation of long-term return on investment were often a major barrier, specifically in developing countries. Thakur et al. (2021) stated that several hospitals discontinued recycling programs due to concerns about safety and the risk of nosocomial infections. Furthermore, Seguela et al. (2022) showed that healthcare facilities in remote areas often lacked the expertise to operate and maintain complex water recycling systems. Seifert and Guenther (2020) also emphasized the importance of a long-term systematic method to ensure the success of water recycling programs in hospitals.
Energy Conservation
Energy conservation practices have become an important priority in hospital sustainability but the level of implementation varies across healthcare institutions. Borges de Oliveira et al. (2021) reported that most hospitals, specifically in developing countries struggle to develop the infrastructure for generating energy from renewable sources. This is a significant challenge since healthcare facilities consume 2 to 3 times more energy resources than commercial buildings, as shown in Sint Maarten hospital in Mechelen, Belgium (Stevanovic et al., 2019).
Factors contributing to the successful implementation of energy conservation include the integration of technological solutions with changes in staff behavior. Stevanovic et al. (2019) reported that hospitals that successfully reduced energy consumption by 20% implemented a holistic method combining routine energy audits, staff training, and investment in energy-efficient technology. In Portugal, research on public hospitals showed that top-level management support was a critical factor in determining the success of energy conservation programs (Fonseca et al., 2019).
Several factors have been identified as causes of failed energy conservation implementation. Budget constraints are a major obstacle, particularly due to the high upfront investment in energy-saving technologies. Research conducted in Sao Paulo, Borges de Oliveira et al. (2022) showed that hospitals without a calculation of long-term return on investment ruled out energy conservation initiatives. Thakur et al. (2021) reported that reliance on traditional methods was still dominant, reflecting structural barriers to the adoption of clean technologies. In Western India, Nagariya et al. (2022) stated that the sustainability index of hospitals showed low scores in the implementation of energy and water recycling.
Despite facing various challenges, some healthcare institutions have developed innovative solutions. Seifert and Guenther (2020) documented progressive practices in German hospitals validated by EMAS, such as the use of natural ventilation as an effective cost-saving solution to control indoor air quality. According to Rodriguez et al. (2020), private hospitals in Spain integrating a sustainability method into organizational strategy have succeeded in reducing electricity consumption without disrupting clinical services. Wu (2021) reported the optimization of AI technology for green hospital communication systems in China, contributing to better energy efficiency. In Bendigo Hospital in Australia, Royal Children’s Hospital in Melbourne, and Queen Elizabeth Hospital in Hong Kong, Alsawaf and Albadry (2022) emphasized the importance of sustainable design prioritizing energy efficiency as a main principle.
The implementation of energy sustainability faces regulatory barriers, a lack of financial incentives, and cultural resistance to change. An analysis of 168 hospitals in France by Benzidia et al. (2021) emphasized the importance of integrating Big Data Analytics and AI for green supply chains in improving the environmental performance of hospitals. Furthermore, Bentahar et al. (2023) developed a taxonomy of critical factors based on research in French health facilities for the implementation of green supply chains, which classified the methods into reactive, receptive, and proactive. An analysis of three public hospitals in Thailand by Suriyankietkaew and Kungwanpongpun (2022) showed that 20 out of 23 leadership and strategic management practices significantly affected sustainability performance, with energy management being one of the important factors. Borges de Oliveira et al. (2022) also identified five key drivers for sustainability development and management in Brazilian hospitals, with efficient energy resources as a key component in a sustainable hospital physical environment.
Framework of Trends and Proposals for Future Research
A comprehensive review of 62 literature shows a significant growth in research on hospital sustainability and identifies important gaps. A framework was developed to integrate four priority areas for future research.
The most prominent methodological gap in the literature is the dominance of descriptive research to evaluate causal relationships. Future research needs to adopt a more diverse method, especially experimental and quasi-experimental designs, to produce stronger evidence on the effectiveness of sustainability interventions. In addition, there is an urgent need to increase the number of longitudinal research to monitor the progress of sustainability implementation. Vasileiou et al. (2024) and Jovy-Klein et al. (2024) emphasized the importance of longitudinal data to evaluate the long-term impact and sustainability of initiatives. Longitudinal research enables comparisons of implementation across countries, regions, and different economic contexts, providing insights into the contextual factors influencing the success of sustainability practices. A mixed-methods combining quantitative and qualitative data enriches the understanding of the complexity of implementation. For example, a combination of energy consumption data analysis with in-depth interviews on organizational and cultural factors can produce a comprehensive understanding of the enablers and barriers in sustainable energy technologies.
The literature analysis shows limitations in the theoretical foundation of hospital sustainability. Several research are descriptive in nature without a clear conceptual framework. A “multi-theoretical” method should be adopted to integrate theories from various disciplines. Resource-based view, institutional theory, stakeholder theory, and innovation diffusion theory are needed to understand the complexity of implementing sustainability in hospitals. Rahat et al. (2024) identified that these theories were widely adopted and did not understand the complex dynamics of environmental, social, and economic sustainability practices. This observation reported the need for the development of sophisticated and contextual theories for the health sector.
Geographic gaps and theoretical limitations in the literature must be addressed. Current research is dominated by analyses from North America and Western Europe. Expansion to Africa, the Middle East, Asia, and Eastern Europe enriches the understanding of cultural, economic, and regulatory factors in influencing the implementation of sustainability practices. Cross-country comparative research also enables the identification of contextual factors facilitating or affecting hospital sustainability. This review identified a lack of standardization in measuring sustainability performance, which is a significant barrier to comparison and benchmarking. Future research needs to develop a comprehensive measurement framework to integrate the triple bottom-line dimensions with validated and replicable indicators. The development of specific indicators for hospital context is very important, considering the limited applicability of general sustainability indicators to the health sector. These indicators include metrics for resource use efficiency, medical waste reduction, social impact, and economic performance. El Khoury et al. (2023) emphasized the importance of indicators for measuring the trade-offs between various dimensions of sustainability in hospital decision-making.
Related to measurement, research on the quality of information and transparency in hospital sustainability reporting needs to be prioritized. Investigations into reporting standards and guidelines appropriate for the health sector will make significant contributions to practice and policy.
Based on the latest literature, several promising themes were identified for future research. First, the integration of AI and Big Data in hospital sustainability has transformative potential as reported by Jovy-Klein et al. (2024) and Benzidia et al. (2021). Future research needs to explore the development of AI algorithms for the optimization of energy consumption, Big Data applications for the prediction of resource needs, and the impact of AI implementation on the triple-bottom-line performance of hospitals. Second, the concept of a circular economy has developed in various sectors but the application in hospitals is in the early stages. Future research can develop circular business models for hospital supply chains, evaluate medical waste reduction strategies through a circular method, analyze regulatory, and policy barriers, as well as measure the economic and environmental impacts of the initiatives. Third, the experience of the COVID-19 pandemic and the increased frequency of climate-related disasters show the importance of research on hospital resilience, including climate-resilient design and infrastructure, mitigation as well as adaptation strategies for external disruptions, integration of sustainability with contingency planning, and evaluation of trade-offs between operational resilience and environmental sustainability. Fourth, the social dimension of hospital sustainability requires research on the impact of sustainability practices regarding the health and well-being of patients and communities, the equity implications of sustainable technologies, ethical considerations in decision-making, and the development of participatory models to include stakeholders in sustainability initiatives.
The proposed research agenda has significant practical implications for various stakeholders. For policymakers, this research can inform the development of regulations and incentives promoting the adoption of sustainability practices. Meanwhile, for hospital managers, further research should provide empirical evidence and a practical framework for the implementation of effective sustainability strategies. For healthcare practitioners, opportunities must be identified to integrate sustainability considerations into everyday clinical practice.
Conclusion and Limitation
In conclusion, this research made a significant contribution to the understanding of hospital sustainability through a comprehensive systematic literature review of 62 articles. Concerning descriptive analysis, the synthesis showed critical insights into the implementation factors, challenges, and strategic methods shaping sustainability practices in healthcare settings.
The integration of four thematic areas, namely continuity services, sustainability systems and technologies, sustainability strategies for quality value, and strategies to minimize waste, formed a holistic framework that bridged previously fragmented research methods. The results showed that successful implementation across the domains required technological innovation, strong leadership commitment, staff engagement, and balance with organizational culture. A critical examination of implementation barriers showed that many sustainability initiatives failed due to limited resources, technical competence, and organizational resistance.
Based on the description above, the valuable contribution of the review was the identification of interactions between the triple bottom-line dimensions in hospital context. Even though several research focused on environmental aspects, this analysis reported the importance of balancing social impacts and economic considerations for a truly sustainable health system. The synthesis of evidence from various hospital contexts showed that an integrated method consistently outperformed one-dimensional sustainability interventions.
This research presented a future agenda based on identified gaps. Future research could prioritize methodological diversification through longitudinal and experimental designs, strengthen theoretical foundations with multi-theoretical approaches, develop standardized measurement frameworks specific to healthcare contexts, and explore developing themes such as AI integration, circular economy applications, climate change resilience, and the socio-ethical implications of sustainability practices.
For practitioners and policymakers, the results offer actionable insights since (1) sustainability initiatives required integration with core strategic objectives rather than peripheral programs, (2) successful implementation depended on contextual factors evaluated before adoption, (3) potential trade-offs between short-term health priorities and long-term sustainability goals must be addressed transparently, and (4) stakeholder engagement at all levels of the organization was critical to overcoming implementation barriers. This research advanced the understanding of hospital sustainability but the limitations included the interpretive nature of qualitative synthesis and potential variations in thematic categorization. A comprehensive foundation was provided for future research and practice by consolidating existing knowledge, identifying critical gaps, and setting a clear path for developing a more sustainable health system.
Footnotes
Ethical Considerations
This study is a systematic literature review that does not involve direct human participants or intervention. Therefore, formal ethical approval and informed consent were not required. The study was conducted in accordance with ethical standards for scientific publications, ensuring proper attribution of all cited sources and transparent reporting of the review methodology
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors gratefully acknowledge the support from The Indonesian Education Scholarship (BPI), Center for Higher Education Funding and Assessment (PPAPT), Ministry of Higher Education, Science, and Technology of Republic Indonesia, and Endowment Fund for Education Agency (LPDP), Ministry of Finance of Republic Indonesia.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
Raw data is generated in Scopus and WOS. Data obtained supporting the findings of this study are available from corresponding author Melinda Ibrahim upon request by email
