Abstract
Online self-learning became widespread after the onset of the COVID-19 pandemic, and during this period, learners’ self-leadership became an important measure of their competency. This study aims to verify the validity and reliability of the tool by translating the Abbreviated Self-Leadership Questionnaire (ASLQ) into Korean. Through web-based surveys, 286 nursing students from two university nursing colleges participated in the study. Cronbach’s α, correlation, and confirmatory factor analyses were used to verify the nine-item ASLQ. The factor loading values ranged from 0.378 to 0.892. The ASLQ model fit had a comparative fit index of 0.944, root mean square error of approximation of 0.093, and standardized root mean residual of 0.069. The ASLQ showed a statistically significant positive correlation with the original self-leadership, emotional intelligence, and self-efficacy questionnaires. Additionally, structural, convergent, and criterion validity were also evident. The reliability of the ASLQ was 0.846 for Cronbach’s α (the three sub-dimensions were 0.836, 0.732, and 0.734). This study verified the validity and reliability of the ASLQ and confirmed that it could be used to measure the self-leadership of nursing students at a time when self-leadership is crucial.
Introduction
Self-leadership refers to the process of self-direction and motivation required to form one’s own behavior to improve overall performance, cognitive self-evaluation, and self-influence (Neck & Houghton, 2006; Neck & Manz, 2013).
Additionally, social change has led to the evolution of the definition of self-leadership, which is now essentially defined as the process of controlling and creating one’s own behavior (Ioannis, 2019). Those with high self-leadership ability have the competence to manage their behavior and have a high likelihood of coping with stress (Avcı & Kaya, 2021).
Generally, the nursing curriculum involves a relatively high level of stress throughout learning and training (Smith & Yang, 2017); nursing students generally experience a higher level of stress than other major students for reasons, such as arduous exams, additional tasks, and time pressure (Smith & Yang, 2017; Yagajeyanthi et al., 2022). In addition to managing stress, nursing students require self-leadership skills to adapt to the clinical environment, overcome problems, and address future situations (Kwon & Choi, 2020). To prevent the spread of COVID-19, social distancing policies were implemented worldwide, and face-to-face classes were replaced entirely with online classes (J. Park et al., 2022). Owing to the pandemic, online teaching methods have continued longer than anticipated, that is, lasting over 2 years. The interaction between professors and students has deteriorated because of the improper application of traditional teaching strategies in a new learning environment with extended online classes (D. J. Lee & Kim, 2020). As in other major fields, self-leadership is essential in this environment. Thus, nursing students’ levels of self-leadership must be assessed.
Previous studies have examined the quality of self-leadership for nursing students, which is related to their self-efficacy, social support (S. Y. Lee et al., 2019), emotional intelligence (EI) (J. I. Kim, 2018), problem-solving ability, critical thinking skills (M. Y. Kim, 2017), professional self-concept (Dong & Choi, 2016), major satisfaction (Wang et al., 2016), clinical performance (Dong & Choi, 2016), nursing professionalism (H. J. Park, 2015), and academic achievement (J. I. Kim, 2018). Among them, EI strongly influences self-leadership. A positive mediating effect was identified in the relationship between EI and constructive cognition in sub-areas of self-leadership (Vann et al., 2017). Self-leadership refers to the ability to learn through training (Kum et al., 2019), resulting in grade advancement. Thus, systematic strategies and efforts are required to develop nursing students’ self-leadership skills (Won & Cho, 2013). In addition to self-leadership, there are some instruments that can measure characteristics similar to EI, self-efficacy, problem-solving ability, and critical thinking. The revised self-directed questionnaire comprises several questions, making it necessary to validate the abbreviated self-leadership scale with nine items. In particular, no reliable tool has been identified to measure the self-leadership levels of nursing students.
Therefore, we attempted to verify the validity and reliability of the Korean version of the Abbreviated Self-Leadership Questionnaire (ASLQ) using a psychological measurement validity design, to ensure the efficacy of the self-leadership tools essential to nursing students.
Methods
Design
This methodological, descriptive, and correlational study psychometrically validates the Korean version of the ASLQ.
Setting and Sample
This study recruited participants from two universities in Suwon and Pochon, Gyeonggi Province, Republic of Korea. The required sample size was estimated using the G*Power program (Faul et al., 2009). The biserial correlational model estimated the required sample size to be 84 with a two-sided test, a significant α of .05, an anticipated power of .80, and an effect size of .25 for the scale’s convergent and criterion validities. The sample size had no criteria for confirmatory factor analysis to evaluate structural validity; however, in the case of less than 40 variables, Singh et al. (2016) recommended a sample size of 200. In this context, a total of 286 nursing students, including dropouts, were recruited. All participants were enrolled in a nursing degree program during the 2021 to 2022 academic year. The eligibility criteria were as follows: age ≥18 years, currently enrolled in a 4-year nursing degree program, and volunteered to participate in the study. The participants were excluded if they had previously received specific leadership training (Linares et al., 2020). Of the 286 questionnaires, 273 valid responses were included in the data analysis, and 13 were excluded owing to incomplete responses.
Measurements
The English Abbreviated Self-Leadership Questionnaire (ASLQ)
Houghton et al. (2012) developed and validated the ASLQ, based on the Revised Self-Leadership Questionnaire (RSLQ) created by Houghton and Neck (2002). This nine-item scale comprises three dimensions with no reverse items: behavioral awareness and volition (BAV, three items), task motivation (TM, three items), and constructive cognition (CC, three items). The responses to the items were rated on a 5-level Likert scale ranging from 1 (strongly disagree) to 5 (strongly agree). Higher scores indicated better ASLQ scores. The alpha coefficient of the ASLQ was 0.73. Confirmatory factor analysis (CFA) produced a 3-factor model with good fit. The nine-item ASLQ is a reliable and valid measure that inherits the nomological network of associations from the original version of the RSLQ (Houghton et al., 2012).
The Korean Revised Self-Leadership Questionnaire (K-RSLQ)
The validated Korean version of the RSQL (K-RSLQ) was used to examine the criterion validity after obtaining written approval from its developers (Shin et al., 2009). The eight dimensions included visualizing successful performance, self-goal setting, self-talk, self-reward, evaluating beliefs and assumptions, self-observation, focusing on natural rewards, and self-cueing. All 35 items were measured on a 5-level Likert rating scale ranging from 1 (strongly disagree) to 5 (strongly agree). Higher scores indicated better RSLQ scores. The coefficient alphas for the Korean 35-item RSLQ ranged from 0.70 to 0.80 (Shin et al., 2009). This study demonstrated a coefficient alpha level of .90 with a range of .60 to .88 across eight dimensions.
The Korean Wong and Law Emotional Intelligence Scale (WLEIS)
The Korean Wong and Law Emotional Intelligence Scale (WLEIS) developed by Wong and Law (2002) was used to examine the criterion validity after obtaining written approval from the developer (H. J. Park & Yu, 2021). This 16-item scale, with no reverse items, comprises 4 operationally defined dimensions: self-emotion appraisal (four items), others’ emotion appraisal (four items), use of emotion (four items), and regulation of emotion (four items). The response items were rated on a 7-level Likert rating scale ranging from 1 (totally disagree) to 7 (totally agree). Higher scores indicated better EI. In terms of reliability, the Cronbach’s alpha coefficient of the Korean WLEIS was .91 (H. J. Park & Yu, 2021), and .90 in this study.
The Korean Self-Efficacy (SE) Scale
The validated Korean Self-Efficacy (SE) Scale was used to examine criterion validity after obtaining written approval from the developers (Hong, 1995). This 23-item scale comprises two dimensions, general efficacy (17 items) and social efficacy (six items), with 16 reverse items. All items were evaluated using a 5-level Likert rating scale ranging from 1 (not at all confident) to 5 (completely confident). Higher scores indicated better self-efficacy. In terms of reliability, the Cronbach’s alpha coefficient of the Korean SE was .86 (Hong, 1995) and .89 in this study.
Translation, Back Translation, and Content Validity
Written approval was obtained from the developer of the English ASLQ and received the English version of the questionnaire to develop the Korean ASLQ based on international translation guidelines (Fayers & Machin, 2007). Three trained bilingual Koreans independently translated the English ASLQ into Korean for forward translation. The three translations were compared, and any discrepancies were reconciled by a focus group including two nursing professors, a professor of English, and a professor of education. Thereafter, the three translations were retranslated until an acceptable conceptual equivalence of the items and response choices was obtained. Second, two bilingual translators fluent in English and Korean independently translated the Korean ASLQ into English for backward translation. A focus group was conducted comprehensively to resolve any discrepancies in achieving conceptual equivalence and consistency with the English ASLQ. The resulting translation was cognitively assessed to learn students’ vocabulary and thinking patterns, and the translation was identified to be conceptually equivalent among 20 first- to fourth-year nursing students who were excluded from the field test. Based on the first cognitive test, the translation was refined by rewording some items. The refined translation was then cognitively evaluated by 35 nursing students who did not participate in the field test and was finalized after meeting the standards of the alpha coefficient (.80) and test-retest reliability (.87).
Finally, regarding the content validity of the Korean ASLQ, an expert panel of two nursing professors and six nursing instructors evaluated the appropriateness of the nine-item Korean ASLQ on a response scale ranging from 1 (not at all appropriate) to 4 (very appropriate). The average content validity index (CVI) was 0.92, which had high content validity (J. Hair et al., 2000). The Korean ASLQ was administered to 286 nursing students via a field test. The participants completed a questionnaire on characteristics such as sex, age, school year, religion, level of family support, level of academic achievement, aptitude in nursing, perceived adaptation to college life, and satisfaction with college life.
Collecting Data and Ethical Considerations
Online questionnaire responses were collected from a convenience sample of 273 first- to fourth-year nursing students between November 2021 and January 2022. First, the purpose of this study was outlined and willing respondents were recruited through online announcements. All the respondents provided informed consent through an online survey after voluntarily agreeing to participate in the study. In addition, the participants were informed of the purpose of the study and assured that the confidentiality of their responses, autonomy, voluntary participation, and the right to withdraw at any time were guaranteed. The participants were also informed that withdrawing from the study would have no negative consequences.
The participants took approximately 15 to 20 min to complete the online questionnaires. This study was conducted in compliance with the Declaration of Helsinki and was approved by the Institutional Review Board of CHA University (1044308-202109-HR-074-03).
Data Analysis
Data were analyzed using the IBM SPSS software (version 23; IBM Corp., Armonk, NY, USA) and IBM SPSS AMOS (version 24; IBM Corp., Armonk, NY, USA). The Kolmogorov–Smirnov test was used to determine data normality on the ASLQ. Mann–Whitney U and Kruskal–Wallis tests (with Bonferroni multiple-comparison correction) were used to examine the differences in the ASLQ according to the respondents’ characteristics. Ceiling and floor effects were examined using the range and distribution of the participants’ responses to each item. As the ASLQ instrument has already been validated (Houghton et al., 2012), this study examines its structural validity using CFA. To evaluate the confirmatory factor model, model indices and model fit were selected and assessed (Byrne, 2010; Leak, 2011). The criteria of the goodness-of-fit indices include the minimum discrepancy function by degrees of division (CMIN/df) = 4, standardized root mean residual (SRMR) = 0.08, root mean square error of approximation (RMSEA) = 0.10, incremental fit index (IFI) = 0.90 and above, comparative fit index (CFI) = 0.90 and above, and normed fit index (NFI) = 0.90 and above (Noh, 2014; Yu, 2012). For the convergent validity in CFA, a reference value of average variance extracted (AVE) is greater than 0.50 (Song, 2013; Yu, 2012).
The convergent and concurrent validities of the scale were examined using Pearson’s correlation analysis. Test-retest reliability was assessed. The internal consistency reliability of the three dimensions of the Korean ASLQ was calculated using the Cronbach’s α and item-total correlation coefficients.
Results
Differences in ASLQ According to Participant Characteristics
On the participants’ characteristics (N = 273), the mean age was 21.31 years (SD = 2.47). Notably, 207 students (90.5%) were women and first-year students were 97 (35.5%). A total of 191 (70%) students had no religion or a high level of family support (n = 170, 62.3%). Furthermore, more respondents reported moderate levels of academic achievement (n = 169, 61.9%). Approximately half reported high aptitude for nursing (n = 150, 54.9%), moderate adaptation to college life (n = 142, 52.0%), and moderate satisfaction with college life (n = 148, 54.2%) (Table 1).
The Abbreviated Self-leadership according to Participants’ Characteristics (N = 273).

Note. ASLQ = abbreviated self-leadership questionnaire; M = mean; SD = standard deviation; z by Mann-Whitney test; χ2 by Kruskal-Wallis test with Bonferroni’s multiple comparison.
The mean ASLQ score was higher in participants who had high academic achievement (χ2 = 28.94, p < .001), high adaptation to college life (χ2 = 28.68, p < .001), and high satisfaction with college life (χ2 = 25.53, p < .001). The statistical analysis found that the higher the aptitude for nursing, the higher the ASLQ score (χ2 = 34.48, p < .001) (Table 1).
Structural Validity
Table 2 shows the factor structure of the nine observed variables of the Korean ASLQ, conducted using CFA. The standardized regression weights were statistically significant for all three factors ranged from 0.378 to 0.892 (all p < .001).
Confirmatory factor Analysis of the Abbreviated Self-Leadership Questionnaire (N = 273).

Note. CR = construct reliability; AVE = average variance extracted; CMIN/df = chi-square minimum/degree of freedom; SRMR = standardized root mean residual; RMSEA = root mean square error of approximation; IFI = incremental fit index; CFI = comparative fit index; NFI = normed fit index; Q = question; VIF = variance inflation factor; Q1. I established specific goals for my performance: Q2. I make a point to keep track of how well I am doing at work. Q3. I work toward the specific goals I have set for myself: Q4. I visualize myself successfully performing a task before I do it. Q5. Sometimes, I picture in my mind a successful performance before I actually do a task; Q6. When I have successfully completed a task, I often reward myself with something I like. Q7. Sometimes I talk to myself (out loud or in my head) to work in difficult situations. Q8. I try to mentally evaluate the accuracy of my own beliefs about situations in which I am having problems with Q9. I think about my own beliefs and assumptions when I encounter difficult situations.
Table 2 presents all the indices for the evaluation of the model. The model fit of this instrument was χ2 = 80.16 (p < .001), CMIN/df = 3.34, SRMR = 0.069, RMSEA = 0.093, IFI = 0.945, CFI = 0.944, NFI =0.923, which met all the criteria for the goodness-of-fit indices (Noh, 2014; Yu, 2012).
Convergent and Discriminant Validity
Regarding the convergent validity using CFA, AVE was verified by evaluating values between 0.583 and 0.729, which met the reference value of ≥0.50 (Song, 2013; Yu, 2012; Table 2). In light of the discriminant validity in CFA, all values of AVE were greater than the correlations β2 in the relationship between BAV and TM, between TM and CC, and between BAV and CC (Table 2).
In addition to computing the variance inflation factor (a measure of multicollinearity), the Kolmogorov–Smirnov residual normality test, Durbin–Watson test for autocorrelation, and Breusch–Pagan test for the equality of variances were adopted to evaluate the goodness-of-fit of the regression model. The results supported the model’s goodness-of-fit (Table 2).
Convergent and Criterion Validity
The ASLQ was correlated with the three dimensions of BAV (r = .801, p < .001), TM (r = .815, p < .001), and CC (r = .815, p < .001), which verified the convergent validity (Table 3). The ASLQ score was associated with the EI and SE scores (r = .564, p < .001; r = .415, p < .001), thereby verifying the criterion validity (Table 3).
Convergent Validity and Criterion Validity (N = 273).

Note. M = mean; SD = standard deviation; ASLQ = the abbreviated self-leadership questionnaire; BA = behavior awareness and volition; TM = task motivation; CC = constructive cognition.
Reliability
The internal consistency coefficient alphas (Cronbach’s α) for the three dimensions were 0.836 (BAV), 0.732 (TM), and 0.734 (CC) of the Korean ASLQ. The Cronbach’s α value for the Korean ASLQ was 0.846. The item-total correlation coefficients for the three dimensions exhibited the values of .547 to .630 in BAV items, .401 to .618 in TM items, and .488 to .609 in CC items, which were adequate and reproducible (Table 4).
Reliability, Floor Effect, and Ceiling Effect of the Abbreviated Self-Leadership Questionnaire (N = 273).
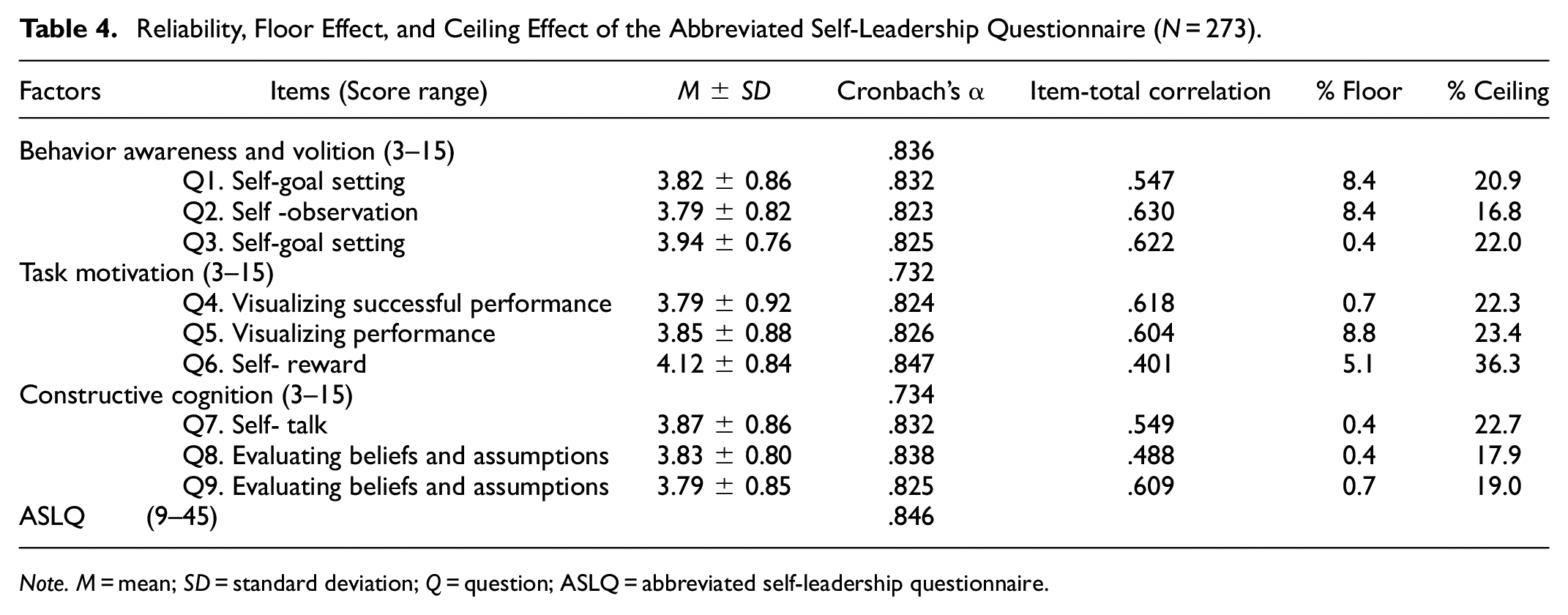
Note. M = mean; SD = standard deviation; Q = question; ASLQ = abbreviated self-leadership questionnaire.
Floor and Ceiling Effects
The distribution of participants’ item responses to the Korean ASLQ was acceptable, except for item 6 (self-reward), which had a high proportion of the maximum scores (36.3%). Seven items did not emerge in high proportions for either the minimum scores (0.4%–8.8%) or the maximum scores (16.8%–23.4%), within an acceptable setting point of 30% (Kane, 2006). This indicates good floor and ceiling effects (Table 4).
Discussion
This study aimed to evaluate the validity and reliability of the Korean version of the ASLQ among nursing students. The discussion section scrutinizes the validity and reliability of the validation.
Content and Structural Validity
Content validity is generally conducted in two stages: the development of a preliminary measurement tool, including the conceptualization of the construct concept to be measured, and the reflection of the construct concept of the developed tool (E. H. Lee, 2021). This study aims to discuss the content validity of the tool developed in the second stage, which follows a conceptual definition. The CVI should be satisfied if it is 0.78 (Polit et al., 2007). However, some researchers’ recommendations, such as conducting more evaluations than Polit et al. (2007), modifying items with a CVI close to 0.78, deleting items with a low I-CVI, and using more stringent criteria to determine whether the items are appropriate (Beckstead, 2009), have generated controversy in this area. Apart from these controversies, the I-CVI is the most widely used method (Ibiyemi et al., 2019). Madadizadeh and Bahariniya (2023) recommended it to be 0.90 or higher, and the CVI of this study was 0.92 for eight experts, thereby meeting this condition. Structural validity refers to whether the tool being developed appropriately reflects the dimensions of the constituent concept to be measured, and the main verification method used is CFA (De Vet et al., 2011). If existing tools or hypotheses exist, only CFA is conducted without exploratory factor analysis (EFA). Thus, in this study (E. H. Lee, 2021), CFA was performed without EFA, because the original tool had already been developed. Factor analysis requires at least four to ten samples per item; thus, 100 samples are the minimum number required; however, more samples are required to build a stable model (De Vet et al., 2011). The sample size of the present study met these requirements. The indices that represent model fit vary as follows: χ2/degree of freedom, RMSEA, SRMR, comparative fit index (CFI), normed fit index (NFI), and goodness of fit index (Cho et al., 2020). As a result of the CFA, all items were significantly loaded on the designated factors, and the standardization factor loading value was more than 0.50 (J. F. Hair et al., 2014) except for item Q6. This differs from the results of the original version by Houghton et al. (2012). In contrast to Mahembe et al.’s (2017) study, it was found that the factor loading value was less than0.5, in addition to Q6 (When I have successfully completed a task, I often reward myself with something I like) and Q7 (Sometimes I talk to myself [out loud or in my head] to work through difficult situations).
In the EFA study, all nine items had a factor loading of 0.5 or more. Item Q6 had the lowest factor loading in Houghton’s study. This was a question about self-reward, which can be thought of as being influenced by cultural differences. As a sub-method for the standardized factor loading value of the tool, the AVE was higher than 0.50 (E. H. Lee, 2021); hence, Q6 was not excluded. However, confirming this through repeated studies was necessary. Other resulting indicators, including CMIN/df, RMSEA, CFI, and NFI, met the criteria of previous studies. These three factors can be regarded as reflecting the main key elements of self-leadership.
Hypothesis-Testing Construct Validity: Convergent and Discriminant Validity
To verify the convergence validity, the construct reliability (CR) value for the factor load must be greater than or equal to 1.96 (İnkaya & Karadağ, 2021), the AVE value must be greater than or equal to 0.50 (Henseler et al., 2015), and the construct reliability value must be greater than or equal to 0.70 (Gravesande et al., 2019). The value of the factor load for each self-leadership item was 0.50 or more, except for one item (Q6). All the CR values for the factor load were 1.96 or more, and the significance level p value was less than .001. Furthermore, the AVE value for each factor was 0.50 or higher, and the convergent validity was verified at 0.70 or higher for all construct reliability values. In the discrimination validity test, if the AVE obtained between the two factors is greater than the square of the correlation coefficient of each factor, then the discrimination validity is secured between the two factors (G. S. Kim, 2010); hence, this was satisfied, and discrimination validity was supported.
Criterion Validity
Criterion validity refers to the comparison of results obtained using a standardized measurement tool that measures the same constituent concepts as the tool being tested (Mokkink et al., 2010). When creating a short version of a measurement tool already developed, as in this study, the original version may be used as a standardized tool for the abbreviated compliance test (Mokkink et al., 2018), if the correlation analysis result is r ≥ .70, compliance is satisfied (De Vet et al., 2011). In this study, the correlation with the existing tool was .820, and the correlation between EI and self-efficacy was significant, confirming the criterion validity.
Test-Retest Reliability, the Reliability (Internal Consistency)
As a result of the reliability analysis, Cronbach’s α, the consistency reliability of the nine items, was 0.846, compared to the 0.73 in the original tool of Houghton et al. (2012). Particularly, item-total correlation is used as a summated rating scale, it should be .30 or higher (Shrestha et al., 2023), and as a result of this study, this criterion was met in all items. This reliability result differed from that of a study that confirmed the validity and reliability of the ASLQ among 400 college students in South Africa (Mahembe et al., 2017). The reliability coefficients for the three abbreviated subareas of self-leadership were slightly lower than the 0.70 threshold; thus, repeated studies on whether differences exist depending on cultural background are imperative.
Nursing students’ self-leadership plays a pivotal role in shaping career adaptation, especially in improving self-directed learning and clinical performance ability. Therefore, it is essential to assess students’ self-leadership levels in the undergraduate curriculum to identify areas that require improvement. Studies by Avcı and Kaya (2021) have shown that self-leadership is closely related to the learned skills of nursing and midwifery students. This finding suggests that developing self-leadership skills can contribute to nursing students’ overall competence. Additionally, the increasing adoption of online self-learning due to the COVID-19 pandemic has highlighted the role of self-leadership as an important measure of learners’ competence and adaptability (Abdelaliem & Elzohairy, 2023; Durnali, 2022; H. J. Park & Kim, 2023). The ability to learn independently and be responsible for the training journey is becoming increasingly important. Therefore, evaluating and fostering the self-leadership skills of nursing students is not only timely, but also essential for preparing nursing personnel for the challenges of modern healthcare.
Implications for Practice and Research
These findings provide important implications for both practice and research in the nursing field. This result highlights the importance of incorporating self-leadership development programs into nursing education. Educational institutions can strengthen the overall capabilities of future nurses by improving nursing students’ self-leadership skills. Implementing targeted self-leadership enhancement programs and curricula in undergraduate nursing courses can help prepare nursing students for the challenges of modern healthcare, especially in the face of increasing online self-learning.
This research highlights the need for a broader multidisciplinary investigation of nursing students’ self-leadership. This will promote a more comprehensive understanding of factors affecting self-leadership and their impact on nursing education and practice. Researchers should consider the role of cultural backgrounds in shaping self-leadership. These surveys can provide valuable insights into developing more effective nursing education strategies and contribute to the continued development of nursing professionals.
Limitations
Nursing students’ self-leadership is generally expected to develop more in the fourth grade of nursing students than in the lower grades. This study also included fourth graders; however, it is worth noting that first, second, and third graders were also part of the research. Including various grade levels could be a limitation to the study. Recent research in this area (Avcı & Kaya, 2021) has shown that self-leadership development varies by grade, highlighting the need for future research focusing more specifically on nursing students.
In addition, this study was limited in that it targeted only nursing students from two universities. In this context, we explored the validity and reliability of ASLQ. However, the generalizability of our findings may be limited. Future studies should consider expanding their sample size to include a wider variety of nursing students to increase the applicability of these findings. A recent study (Nguyen et al., 2023) highlighted the importance of multicenter research in capturing a broader perspective on self-leadership in nursing students.
Conclusions
This study demonstrated the validity and reliability of the ASLQ. Additionally, this study confirmed that the ASLQ could be used to measure nursing students’ self-leadership. The findings also revealed that, first, a curriculum and program that can increase self-leadership while considering the characteristics of nursing students must be developed. In addition, the effectiveness of the improved curriculum and program must be verified. Second, follow-up research is warranted because of the lack of research that verifies the relationship between self-leadership and other factors among nursing students.
Footnotes
Author Contributions
Hye-Ja Park: Data Curation, Formal analysis, Investigation, Validation, Visualization, Writing—Original Draft, Writing—Review & Editing. Sun-Ki Kim: Methodology, Data Curation, Investigation, Project administration, Writing—Review & Editing. Soyoung Yu: Investigation, Supervision, Project administration, Validation, Writing—Original Draft, Writing—Review & Editing.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the CHA University Research Fund of 2021.
Ethics Statement
The protocol and procedures of this study are approved by the Institutional Review Board of *** University (*******-******-HR-***-**). In addition, the study was conducted after receiving prior online consent from all participants to voluntarily participate therein.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
