Abstract
This study tested the effect of issuing return-to-activity advice on activity intentions at Day 2 and Day 10 days post simulated mild traumatic brain injury. One hundred and twenty-eight volunteers were randomly allocated to one of two groups who received (n = 65) or did not receive standardized post-injury advice (n = 63). To prime the simulation, the participants read a mild traumatic brain injury vignette about a person who is concussed while playing sport. Then the participants role-played the injured person and reported activity intentions for three activity types (cognitive, physical and restful) twice, once for each time frame (i.e. Day 2 and Day 10). The advice was to rest for the first 24–48 h and then gradually resume normal activities. There was no significant group by activity-type interaction (p > .05) at Day 2. When both time frames were considered, there was no significant group × time frame interaction for any activity type or any item, except for an increase in non-manual (clerical) work and weight training at Day 10 compared to Day 2 in the group with the advice. In general, the intentions for all activity types were consistent with the recovery advice (i.e., rest then increasing activity), even when the advice was not given. However, at Day 10, cognitive and physical activity levels were still expected to be lower than usual (pre-injury), and many participants were uncertain about the concept of cognitive rest. These factors, along with individual patient circumstances, should be taken into account in rehabilitation planning.
Keywords
Mild traumatic brain injury (mild TBI) is a significant health problem world-wide. 1 Mild TBI can result from a minor head injury that produces a short-term disruption of brain functions. 2 Common causes include a blow to the head from an accident, fall or assault. In Australia between 80% and 90% of the 23,000 TBI hospital presentations were for mild TBI. 3 The remainder are classified as moderate or severe head injury.3–5 However, hospital records greatly underestimate the real incidence of mild TBI, particularly in sport. Mild TBI in sport remains largely underreported with an estimated 25% of all people with mild TBIs having no contact with the health care system.2,6
Although 80 to 90% individuals will be symptom-free after mild TBI within days to weeks,7,8 the recovery trajectory is not fully understood.9,10 The acute effects of mild TBI typically include disorientation, confusion, brief loss of consciousness (≤30 min), and post-traumatic amnesia. In the acute post-injury period (approximately 24 to 72 h after the event) postconcussion symptoms can appear.11,12 These symptoms can impact cognitive, somatic, or affective functioning and include headache, fatigue, and difficulty concentrating.5,13 By 10 to 14 days, the postconcussion symptoms should be fully resolved, and most people will have returned to pre-injury functioning.11,12,14 However, some people continue to report postconcussion symptoms beyond the usual recovery time frame and sometimes much longer, 15 and this has raised questions about why this occurs, and how to help more people achieve a full recovery.
There are many factors that affect mild TBI recovery and several models have been proposed to identify these factors. These models describe how pre-, peri- and post-biopsychosoical factors can contribute to mild TBI outcomes.16–18 For example, the models posit that the recovery course could be impacted (worsened) by factors such as whether the individual has a positive pre-injury psychiatric history, co-incident injury, or is compensation-seeking for their injury. The relative contribution of these recovery factors and their potential interactions is the subject of ongoing research, as is the identification of new factors.
Attention has recently turned to the role of physical and cognitive rest and activity in the post-acute period where there can be the possibility of delayed symptom onset, and how this could be contributing to mild TBI outcomes. Questions have been raised about how long people should rest after their injury and, if activity is to be resumed, how this process should occur.8,19,20 In 2001 the International Concussion in Sport Group (CISG) was formed 21 to provide guidance on the clinical management of mild TBI in sport. Since its formation, this body has produced a number of statements that address the issue of return to sport after concussion, including the return to contact or collision sports (e.g., McCrory et al.14,22). There are also publications that describe the consensus process used by the CISG23 and summaries of the changes, 24 and there is a published infographic for the latest advice. 25
Briefly, the current graded return-to-sport protocol from the CISG, which has been extracted to apply to non-sporting mild TBI injury by health professionals, is for a short period of cognitive and physical rest (not more than 48 h), followed over the next week or so by a gradual and progressive return to activity that is below symptom-exacerbation thresholds. 26 The program is advanced as tolerated and each advance towards the return-to-usual activities would normally occur 24 h after the last advance. There is some guidance on activity intensity and type, particularly for physical activities. Full resumption of sport is recommended only after clearance from an appropriate health care professional. This check, and the initial rest period are considered important to avoid the risk of death or serious incapacity via the second impact syndrome. 27 However, questions may still remain about the scope of such advice and the physical activities it covers, as well as whether the principles can or should extend to cognitive or “restful” activities (such as sleeping).
It is not yet clear how clinicians, athletic trainers and patients interpret and implement post-injury rest and return-to-activity advice and how best to disseminate the guidelines,28,29 but there is some evidence that interpretations and practices differ. 30 For example, a recent study of more than 1000 secondary school and collegiate athletic trainers found variation in the implementation of a return-to-learn strategy, which is a variant on the graded return-to-sport advice. 31 Less is known about how patients or the general public might implement this advice. There have been some simulation studies on this issue in which people are asked to report which physical activities they would modify after concussion. These studies have generally shown an intention to reduce physical activities, 32 and that factors such as the injured person’s sex and sports participation do not alter intentions, whereas a prior head injury does. 33 If the general intention to take rest is followed by an intention to resume physical and cognitive activities by about day 10 post-injury, this would be broadly consistent with a notion of graded return to activity, 26 but this has yet to be shown.
In many contexts, it has already been demonstrated that the notion of prescribing rest is conceptually complex and subject to multiple interpretations. 34 Yet, the recovery advice issued for concussion, at least for individuals who present to hospital, may include a generic instruction to “rest” and then gradually return to normal activities. 35 Thus it is possible that patients have varying interpretations of what it would mean to rest for concussion, and which behaviors they should change. This study aimed to examine how people would interpret CISG-type advice for concussion by measuring their rest and activity intentions for simulated concussion. It aimed to explore people’s intention to undertake specific behaviors at Day 2 and at Day 10 post-injury, on the assumption that if the advice is effective a change should be evident over this period and potentially for physical and cognitive activities. On the other hand, without this advice people might over- or under-estimate the nature or extent of the “rest” they should take. This study had two research questions. Firstly, if people in a concussion simulation are given standardized post-injury advice based on the GISG recommendations, does this lead to measurable differences in their Day 2 (post-acute) activity intentions for specific behavior types (cognitive, physical and restful), compared to when no advice is given? Second, is the response pattern consistent with a graduated return to activity (that is, do people plan for reduced activity in the first 24 to 48 h and a return to their pre-injury function by Day 10?), and if so, does this occur for all activity types (e.g., physical and cognitive activities)? Thus, compared to a “No Advice” condition, when CISG-type advice was given we expected that at Day 10 there would be a planned increase in cognitive and physical activities compared to Day 2, and a planned decrease in restful activities from Day 10 to Day 2.
Method
Participants
Participants were recruited from the Queensland University of Technology and the general public. Recruitment was via social media advertising (32.0%), email (22.7%), snowball sampling (i.e. through someone they knew) (18.8%), or other means (26.6%) such as the display and distribution of on-campus recruitment material (e.g., fliers).
A total of 145 participants completed the online study. Seventeen participants were excluded; for example, if they entered the study twice (see Figure 1). The final sample comprised 128 volunteers, aged between 17 and 75 years (M = 32, SD =15), most of whom identified as female (80.5% of the sample), resided in Australia (96.9%), spoke English as their first language (91.4%), had completed secondary school (86.7%), and were either attaining (or had attained) a post-secondary school qualification (82.0%) (for example, an undergraduate degree). About half of the sample (approximately 45%) reported engaging in contact sport, and about 10% of the sample had at least one lifetime TBI.
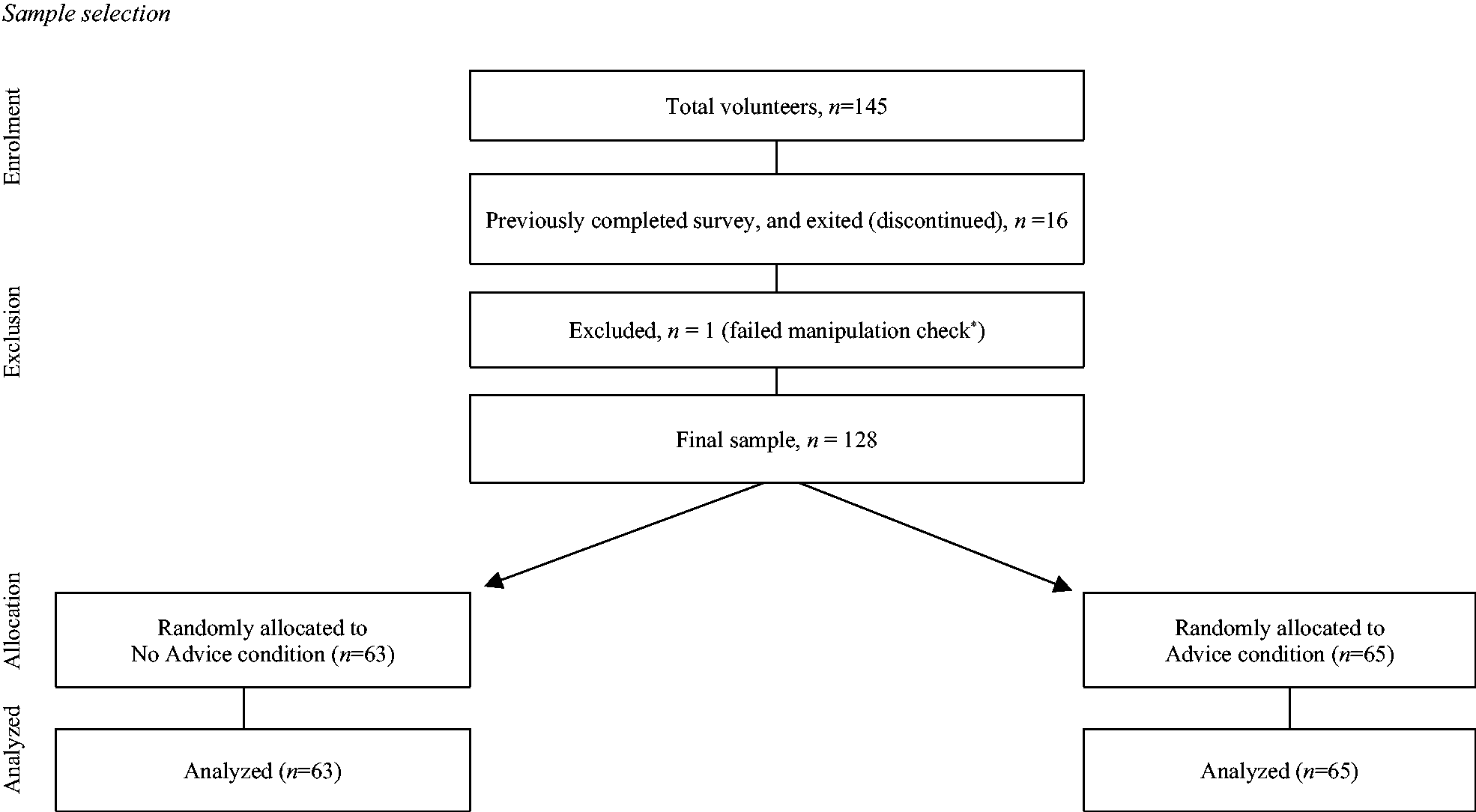
Sample selection. *The excluded participant failed open-ended questions on the post experimental questionnaire and failed the embedded instructional manipulation check.
Materials
Pre-experimental demographic questionnaire
A questionnaire was administered to check participant eligibility and assess the sample characteristics. An adaptation of the Ohio State University (OSU) Traumatic Brain Injury (TBI) Identification Method (OSU TBI-ID) 36 was included. The OSU TBI-ID is a standardized interview procedure for eliciting an individual’s lifetime history of TBI. The adaptation was that the OSU TBI-ID was administered in an online survey.
Vignette and advice
Vignettes have been used in mild TBI research for more than 30 years (see Mittenberg et al. 37 ). Vignettes allow researchers to control the injury cause (e.g., whether from sport or a fall) and other event parameters (e.g., the duration of posttraumatic amnesia, PTA), which may otherwise vary widely in clinical samples (e.g., PTA duration can vary from none to up to 24 h, yet still meet the mild TBI diagnostic criteria). This study used an adapted vignette from a prior mild TBI simulation study. 38 The vignette depicts a person who is concussed while playing sport (TBIvignettesport). The primary modification was to remove the reference to overnight hospitalization for observation, the time since injury, and to reduce the period of loss of consciousness (LOC) from 15 min to 45 s. It is estimated that 80 to 90% of sport-related concussions do not result in unconciousness, 39 but “lying motionless” is commonly used as concussion indicator. 40 This shortened LOC duration was therefore considered more plausible than the longer duration in the original vignette. A second stimulus, comprising the vignette plus the advice was created by adding a sentence to the end of the vignette: “You are advised to have physical rest and cognitive rest during the first 24 to 48 hours following your injury. Once symptoms disappear at rest, gradually resume or reintroduce your usual activities…” This statement was broadly based on the advice by the CISG 26 and other organizations. 29 Both vignettes concluded with the following instruction: Please indicate which activities you are likely to do: (a) within the first 24 to 48 hours and; (b) 10 days after the injury.
Mild Traumatic Brain Injury Rest–Activity Questionnaire. 41
The Mild Traumatic Brain Injury Rest–Activity Questionnaire (MTBI-RAQ) is a 39-item questionnaire used for establishing rest and activity patterns relative to pre-injury. 41 The items were originally primarily derived from published handouts for concussion patients as activities that should be avoided to improve outcomes after mild TBI. The MTBI-RAQ assesses the amount of change from “before [the injury]” for a specific behavior using a five-point Likert response scale ranging from zero (not applicable – I don’t do this activity) to five (much more than before the injury). Given that this was a simulation study, the response scale was amended to state: “I would do this activity….much more [or less etc.] than before the injury.” The MTBI-RAQ items cover three domains: physical (e.g., jogging, weight training), cognitive (e.g., school/academic tests, puzzles), and restful activities (e.g., sleeping, meditating). The domains are inter-mixed in the questionnaire to decrease response bias. Item- and total-scores for each domain were calculated. In the MTBI-RAQ development study 41 the subscale internal consistencies (Cronbach’s alphas) ranged between 0.75 and 0.92. In this study, the values for cognitive and physical activity subscales were all above 0.90, and above 0.72 for the restful subscale.
Procedure
This study was approved by the institutional review board (see Acknowledgements). The experiment was conducted on line using Key Survey (version 8.26). 42 To control for the influences of diagnostic terminology,43,44 the term mild TBI was used in all study materials. The participants read the standardized description of a sport-related mild TBI and they were asked to simulate the injury. Next, the participants completed a validated measure of postconcussion symptoms45–47 to verify plausible simulation (the Neurobehavioral Symptom Inventory (NSI)). 48 Simple randomization was applied to assign participants to one of two conditions (control group (No Advice) or experimental group (Advice)). The participants completed the MTBI-RAQ twice to capture activity intentions for Day 2 and Day 10 post simulated injury, respectively. The MTBI-RAQ was administered with embedded Instructional Manipulation Checks (IMCs), as is recommended for online questionnaires. 49 IMCs appear as a questionnaire items but direct a specific response (e.g., “choose option 3 for this item”). A failure on IMC items was used to assess inadequate effort. The final questions assessed compliance with the study tasks (including the simulation requirements), as is recommended for analogue studies. 50 The study procedure is depicted in Figure 2.
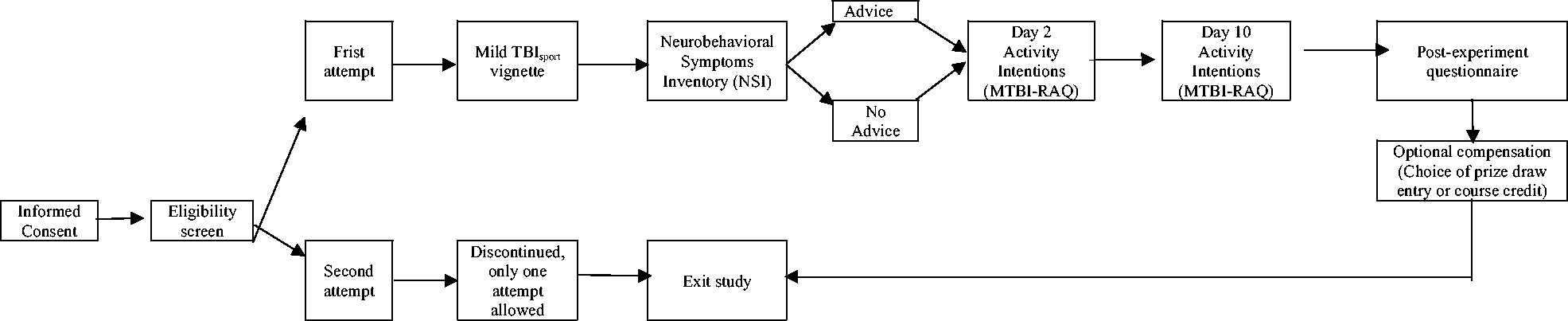
Procedural flow chart.
Statistical analyses
The data analysis was performed using SPSS version 25. Statistical significance was interpreted conventionally (p <0.05), unless otherwise stated. For the main analysis, a series of two-factor, mixed analysis of variances (ANOVAs) were run with one between-groups variable (condition) and one within-groups factor (either activity type with three levels for hypothesis one; or measurement time frame, with two levels, for hypothesis two). The dependent variable was drawn from the MTBI-RAQ and included item or subtotal scores. Effect size statistics and confidence intervals were generated for the comparisons. 51
Results
Preliminary analyses and descriptive statistics
A missing values analysis revealed minimal missing data (0 to 2.30%) and missing values were missing completely at random (Little’s MCAR test, χ2 (2733, N = 128)=2795.44, p = 0.198). A non-imputed data set was used for all analyses. The ANOVA assumptions were met, with minor exceptions. The martial arts item violated two tests of the assumption of homogeneity of variance (Levene’s test and Box’s M test, respectively) so this variable was excluded from further analyses. The background characteristics of the groups were statistically compared (see Table 1). The groups were equivalent, including for proxy measures of concussion risk and exposure (e.g., lifetime history; Table 1). There was no difference in the mean total NSI score for the groups: MNo Advice=30.43 (SD = 15.57); MAdvice=26.79 (SD = 17.64), t(126)=1.235, p = .219. Further, when compared to NSI normative data, the mean scores for the groups were between the 10th and 24th percentile for people with a history of mild TBI, but at or below the first percentile for uninjured individuals. 47
Sample characteristics and group comparisons by allocated condition (N = 128).
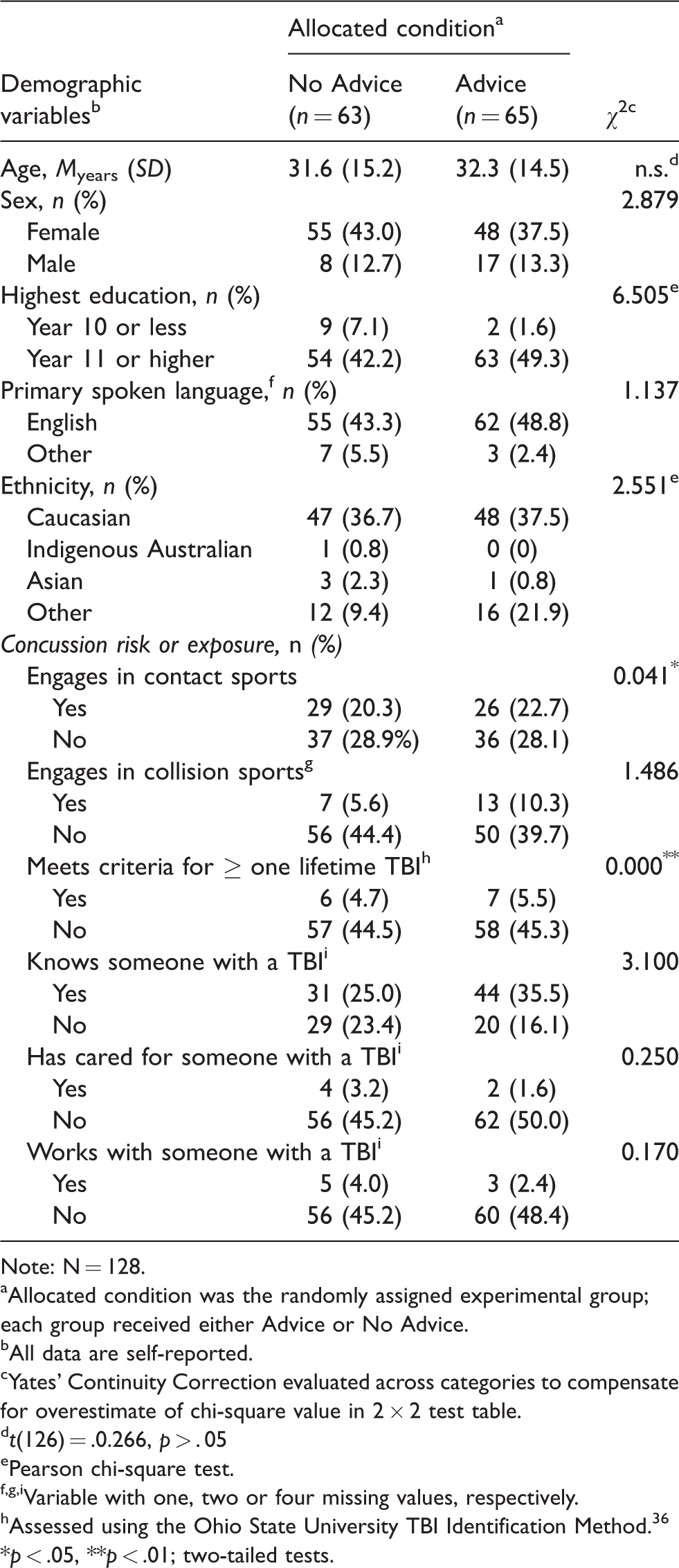
Note: N = 128.
aAllocated condition was the randomly assigned experimental group; each group received either Advice or No Advice.
bAll data are self-reported.
cYates’ Continuity Correction evaluated across categories to compensate for overestimate of chi-square value in 2 × 2 test table.
dt(126) = .0.266, p > . 05
ePearson chi-square test.
f,g,iVariable with one, two or four missing values, respectively.
hAssessed using the Ohio State University TBI Identification Method. 36
*p < .05, **p < .01; two-tailed tests.
Table 2 shows the descriptive statistics for the MTBI-RAQ items and subscales for each group at each time frame. Visual inspection of the data showed that the average scores for MTBI-RAQ physical and cognitive activity items were between one and two (with lower scores for physical vs. cognitive items), indicating an intention to reduce activity from usual, whereas for the three of the six items on the rest subscale the average score was in the order of 3 or 4 (indicating no planned change (score 3), or an increase in the activity (score of 4). There was a trend for higher scores for Day 10 versus Day 2 (physical and cognitive), and at Day 2 the group differences were in the hypothesized direction (e.g., reduced physical and cognitive activity plus increased restful activities with the advice, compared to without it).
Descriptive statistics and two-way mixed ANOVA results for MTBI-RAQ items and subscales.
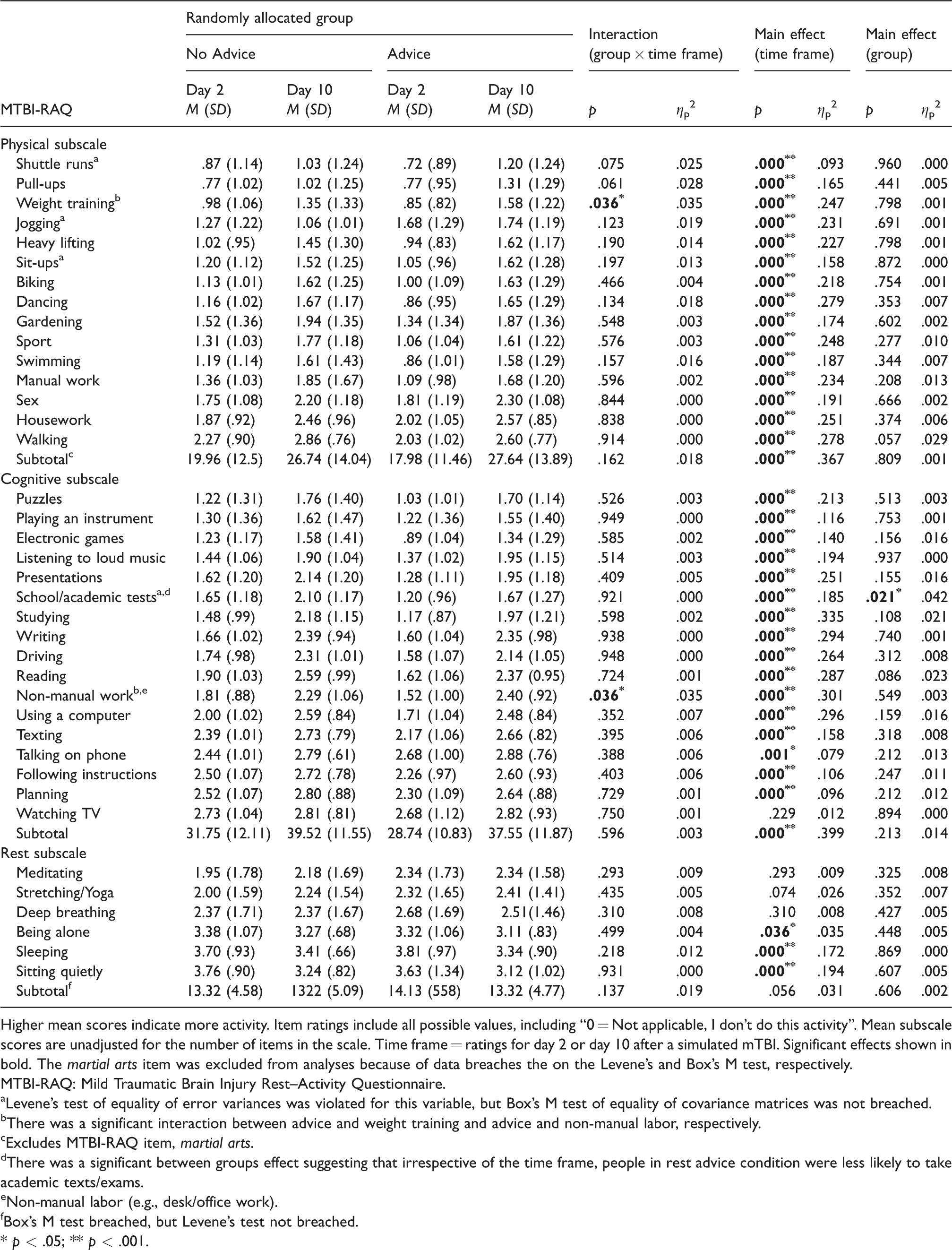
Higher mean scores indicate more activity. Item ratings include all possible values, including “0 = Not applicable, I don’t do this activity”. Mean subscale scores are unadjusted for the number of items in the scale. Time frame = ratings for day 2 or day 10 after a simulated mTBI. Significant effects shown in bold. The martial arts item was excluded from analyses because of data breaches the on the Levene's and Box's M test, respectively.
MTBI-RAQ: Mild Traumatic Brain Injury Rest–Activity Questionnaire.
aLevene’s test of equality of error variances was violated for this variable, but Box’s M test of equality of covariance matrices was not breached.
bThere was a significant interaction between advice and weight training and advice and non-manual labor, respectively.
cExcludes MTBI-RAQ item, martial arts.
dThere was a significant between groups effect suggesting that irrespective of the time frame, people in rest advice condition were less likely to take academic texts/exams.
eNon-manual labor (e.g., desk/office work).
fBox’s M test breached, but Levene’s test not breached.
* p < .05; ** p < .001.
To test the first hypothesis, a mixed ANOVA was used to explore group differences in the Day 2 average score for each activity type (physical, cognitive, restful). Average subscale scores were analyzed to adjust for the unequal number of items in each subscale. (The unadjusted subscale means are shown in Table 2 for comparison.) Despite trending in the expected direction, there was no statistically significant multivariate interaction, Wilks’s Λ = .974, F(2, 125) = 1.655, p = .195, ηp2 = .026 (see Figure 3). Exploratory tests of the main effects found a significant activity type main effect, F(2,125) = 1.61.322, p < .001, but no group main effect, F(1, 126) = .372, p = .541. Post-hoc tests for the activity-type main effect showed that the scores differed significantly from each other (p’s <.05). In order from lowest to highest, the mean MTBI-RAQ subscale score was: physical (M = 1.21; SD = .78), cognitive (M = 1.76; SD = .68), and restful (M = 2.79, SD = 1.03).
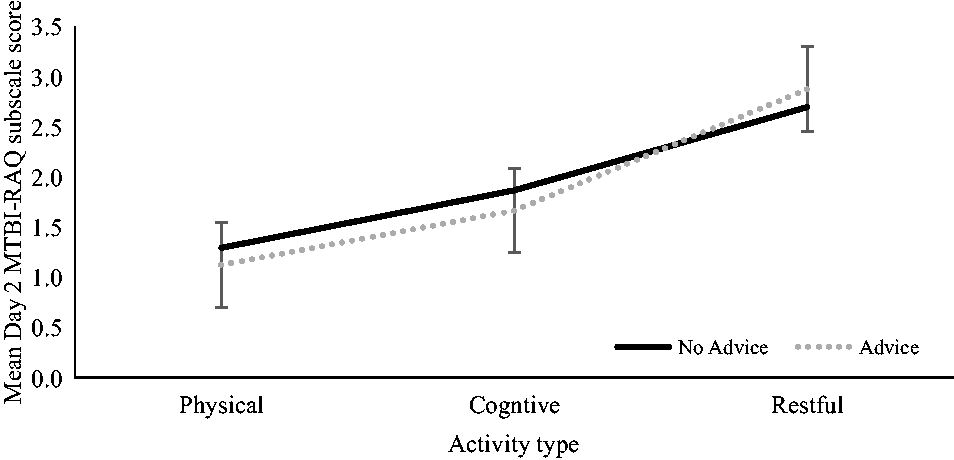
Mean MTBI-RAQ subscale scores by activity type and allocated group (Advice vs. No Advice) with standard error bars.
To test the second hypothesis, a series of mixed (group × time frame) ANOVAs was performed for each activity type and each item. For the subscale analyses, there was no significant multivariate interaction for activity type (see Table 2). For the item analyses, there were only two statistically significant group (Advice vs. No Advice) by time frame (Day 2 vs. Day 10) interactions (see Figure 4). Exploratory analyses of the main effects for all variables showed a significant time frame main effect for almost all variables in the expected direction (i.e. increase in cognitive and physical activities over time, irrespective of group). Of the four variables that did not have a significant time frame main effect, three variables were from the rest subscale: meditating, stretching/yoga, and deep breathing. There was only one group main effect: taking school or academic tests. This analysis found reduced test taking in the Advice versus No Advice group, irrespective of the time frame.
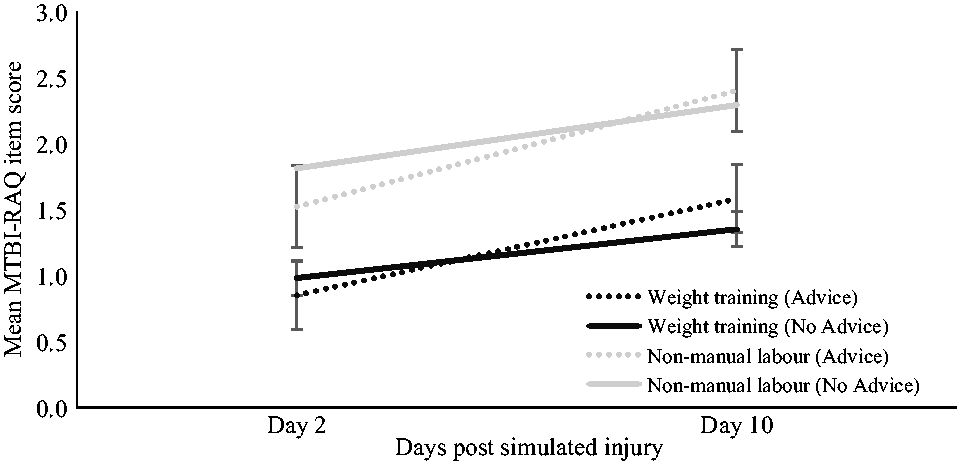
Mean MTBI-RAQ item scores (for two items) by time frame and allocated group (Advice or No Advice) with standard error bars.
Discussion
There is a continuing debate in the literature about the nature and quantity of rest and activity that should be taken after concussion, including questions about how best to communicate this advice to patients.13,14,29,52 This study tested the effect on activity intentions of giving extracted recovery advice, compared to no advice. Mirroring the CISG recommendations, the advice explicitly encouraged a brief period of cognitive and physical rest in the first 24 to 48 h, followed by graded return to usual activities. It was expected that, when compared to controls who received no advice, the CISG-type advice would differentially affect specific activity intentions, including by provoking an initial reduction in activities followed by a return to usual at Day 10.
Contrary to expectations, this study did not find a group (Advice vs. No Advice) by activity (cognitive, physical, restful) interaction for Day 2. Although the data trended in the expected direction, the hypothesis was not supported. People’s rest and activity plans were unaffected by the advice, with both groups proposing to “rest”. They also proposed a significantly greater reduction in physical as opposed to cognitive activity. Some authors have argued that the cognitive rest needs of concussed individuals have been underestimated. 53 It is possible that the participants in this study, also underestimated this need. In this study, the response to an open-ended post-experimental question “what does cognitive rest mean to you?” revealed that many individuals were unsure. When asked to identify the top three activities that would be impacted if they received this advice, a physical activity was often nominated. This could suggest that although a reduction in cognitive activities was proposed by the participants, it was not necessarily viewed as cognitive rest and that the concept itself is subject to misinterpretation. Research on cognitive rest and activity after mTBI is lagging and there is scope to develop this idea so that it can be effectively communicated to patients and subject to further research.
The current concussion advice for return-to-sport encourages a graded return to usual activity that would normally occur after an initial rest period (up to Day 2) and be completed by approximately Day 10 post-injury. A time frame (Day 2 vs. Day 10) by group (Advice vs. No Advice) effect on intended activity was anticipated, but it was only found for two activities. Thus the second hypothesis was not supported. As the exploratory analyses of the main effects showed, the vast majority of activities (cognitive and physical) were proposed to increase over time, irrespective of the advice. This suggests that even without the advice people intended to increase their activity. However, on average, physical and cognitive activities were not back to “usual” by Day 10. This could represent an expectation for a somewhat protracted recovery, and if so, it is consistent with the findings from a prior a cross-sectional study which showed that, on average, athletes allocated more than 20 days for return to sport following concussion. 44 While the potential for symptom exacerbation is obviously a key contributor to individual recovery timelines (as are a host of other factors), it could be important to discuss patient expectations for this timeline early on. This might be especially important if it is medically determined that a realistic rehabilitation goal is to resume usual activities by about Day 10 post-injury.
There were two exceptions to the general trend in the results for activity intentions over time. This study found a significant group (Advice vs. No Advice) by time frame (Day 2 vs. Day 10) interaction for weight training and non-manual work (e.g., office work). This suggests that the advice can support an earlier albeit modest increase in these activities over time than would otherwise have been the case. Given that return-to-work after mild TBI can involve extended absences of up to six months, 8 the advice could potentially support an earlier return-to-work for people in non-manual employment. This could promote better outcomes for mild TBI patients since being “sick-listed” from work is a predictor of worse outcomes. 54 In relation to the finding for weight training, it has been proposed that a combined aerobic and resistance exercise program for concussion with low weights based on individual prescription may be effective for postconcussion symptom reduction. 20 If this proves to be the case, the advice could prime patients to participate in such programs.
This study has a number of limitations. First, this study used a simulation design. Although this approach can be valuable because it allows for tight experimental control, 44 the results may not generalize to real life. On the other hand, the vignette was successful in inducing a degree of postconcussion symptom reporting that is seen in up to 24% of patients and only one percent or less of healthy individuals, 47 and this could suggest that the simulation was effective. Second, this study assessed activity intentions not behavior, and intentions may not be enacted. Third, this study tested an abstracted form of graded return-to-sport advice and the use of this abbreviated and modified form of the advice could be a factor in the results. The full advice includes important elements not captured in this study, such as monitoring for symptom exacerbation. Fourth, this study had two sequential administrations of the MTBI-RAQ, and this could have resulted in inflated Day 10 ratings, simply due to repeat administration. Fifth, the MTBI-RAQ primarily captures physical and cognitive activities that have been suggested as ones that adults should avoid after concussion, and these may or may not represent the behaviors that need the most careful titration for specific individuals. Sixth, this study did not control for the motivational factors that may affect the reported symptoms or activity of specific groups, such as concussed professional athletes or those seeking litigation for concussion. Also it did not directly test the basis for study participants expectations (e.g., whether due to media coverage or concussion awareness programs), but this should be examined in future research. The limited sample size could also have been a factor in the results, especially because some effects were small. Given all of the above reasons, the study findings should be interpreted cautiously.
Despite these limitations, this study is the first of its kind to measure activity intentions post simulated concussion at two critical periods; at 48 h when rest is usually recommended, and at 10 days when usual activities would usually have resumed. 6 Up until now, it was known that people expected to reduce physical activities if they were injured,32,33 but it was not known if or when the activities would be increased, and whether cognitive activities would be viewed similarly. This study has shown that irrespective of whether or not CISG-type advice is issued, people anticipate changing their behavior in a manner that is broadly consistent with the current recommendations for improved recovery; but also that there is room to discuss with patients when the recovery should be complete, and what is meant by cognitive rest. Patient information leaflets, in general, can improve patient knowledge of what to do for recovery, particularly for acute conditions. 55 However, this advice is best viewed as an important element in a scaffolded educational strategy. Ideally, generic advice should be followed up with tailored information that is adjusted for each patient’s individual circumstances.19,52 Based on this study, the framing of advice about post-acute rest and activity for mild TBI recovery should include a check that the advice is appropriate for, and understood by the patient, especially in regards to the recovery timeline and cognitive rest. The athletic trainer or health professional could start by checking the patient’s understanding of what to do, and reinforce this (as appropriate) and explore refinements. This could include consideration of any displacement effects (e.g., how will “down” time be spent, and is the substitution harmful?) and the wider contextual factors affecting recovery.56,57 Future studies with injured individuals are strongly recommended so that their activity choices can be incorporated into a better understanding of how these choices relate to eventual outcomes from mild TBI.
Footnotes
Acknowledgements
The authors thank the School of Psychology and Counselling, Queensland Univerity of Technology (QUT) for funding the gift cards and flyers for this project. This project was approved by the QUT Human Research Ethics Committee (QUT HREC approval ##1700000257) and the QUT health and safety risk assessment process (approval #688).
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
