Abstract
Many head trauma patients who present with prolonged post-concussion symptoms do not meet the American Congress of Rehabilitation Medicine (ACRM) diagnostic criteria for mild traumatic brain injuries (mTBI). This population has not been extensively studied and its clinical characteristics are currently uncertain. A retrospective chart review was conducted to explore the symptomatic differences between mTBI and non-mTBI head trauma patients presenting at a concussion clinic with chronic post-concussion symptoms (PCSx). Patient information was extracted from 161 charts, of which 128 subjects met the ACRM criteria for mTBI (ACRM + PCSx), while 33 did not (non-ACRM + PCSx). These two groups were compared for demographic variables and symptomology. This study found that 20.5% of subjects presenting with chronic post-concussion symptoms do not meet ACRM criteria. No symptom-specific differences were found between the two populations in any of the categories tested. These results show that chronic post-concussion symptoms are similar in both mTBI and non-mTBI head trauma patients in the general population, suggesting a need for further research focusing on this group.
Keywords
Introduction
Mild traumatic brain injuries (mTBI) or concussions account for approximately 80–90% of all TBIs. 1 The American Congress of Rehabilitation Medicine (ACRM) criteria, one of the most commonly used diagnostic criteria for mTBI, defines mTBI as a traumatically induced physiological disruption of brain function, manifested by at least one of the following: (a) any period of loss of consciousness (LOC), (b) any loss of memory for events immediately before or after the accident, (c) any alteration of mental status (AMS) at the time of the accident (e.g., feeling dazed, disoriented, or confused) or (d) focal neurological deficit(s) that may or may not be transient. mTBI is differentiated from more severe TBI with the requirements of LOC to be approximately 30 min or less, an initial Glasgow Coma Scale (GCS) of 13–15 assessed after 30 min and post-traumatic amnesia (PTA) not greater than 24 h. Patients who are diagnosed with mTBI may still have negative CT and MRI scans. 2 Although most patients recover from a mTBI within weeks,1,3 a notable proportion of individuals with mTBI (up to 56%) continue to have prolonged symptoms.4–7 The constellation of physical, cognitive, and emotional symptoms commonly seen after a mTBI are collectively referred to as post-concussion symptoms. If the ICD-10 or DSM-IV criteria are used for these patients, they can be further classified as having “Post-concussion Syndrome” (PCS) or “Post-Concussional Disorder” (PCD) respectively. In this study, we do not use ICD-10 or DSM-IV criteria and look at post-concussion symptoms (hereafter termed PCSx).
In Hamilton, Ontario, a concussion clinic specializes in the management of patients referred for prolonged post-concussive symptoms. Interestingly, it was observed here that a subset of the head trauma population report an array of post-concussive symptoms despite not meeting ACRM criteria for mTBI. To date, there is limited research exploring this group of patients from the general population and their clinical outcomes. This population is often excluded from the studies8,9 or sometimes grouped together with trauma controls.4,10 Clinically, this population often goes unnoticed and does not receive appropriate care. This further adds to the challenges of acute identification and management of mTBI populations. 11
We hoped to investigate whether there are any differences between the chronic symptomatology of head injured patients who sustain a mTBI according to ACRM criteria (ACRM + PCSx) and those who do not (non-ACRM + PCSx). We hypothesize that there will be differences in the reported symptomatology between the two populations, particularly in cognitive and emotional domains. Our secondary purpose is to determine the percentage of referred patients suffering from chronic post-concussive symptoms who do not meet ACRM criteria (non-ACRM + PCSx) for mTBI. We hypothesize a significant proportion of patients with chronic symptoms presenting to the concussion specialty clinic have not sustained a mTBI according to ACRM criteria.
Methods
Consent and confidentiality
This study was approved by the Hamilton Integrated Research Ethics Board, through which the waiver of consent was obtained.
Data collection
Using convenience sampling, patient records from a concussion clinic in Southern Ontario were retrospectively analyzed. All subjects were referred to the clinic for chronic post-concussion symptoms following a suspected mTBI. Data collection was limited to patient records with an initial consultation between January 1st, 2015, to December 31st, 2017. Data was extracted and recorded onto a data collection form (Appendix A) which included the following: demographic information, medical history, current medication(s) and mTBI-related information (ACRM criteria information, mechanism of injury, other systemic injuries sustained at the time of injury, therapies to treat systemic injuries, and symptoms following injury).
We collected data from charts on thirty-seven different symptoms (Appendix A). We later organized these symptoms using a modified version of Rivermead Post-Concussion Symptoms Questionnaire (RPQ) checklist template (Appendix B). 12 This modified RPQ checklist had only 15 of the 16 symptoms found in the RPQ as “Frustrated or impatient” was not captured. To ensure that all the included subjects had chronic PCSx, we required them to have 3 or more symptoms from the checklist listed in Appendix B (not including the “Others” category) and required the initial head injury to precede symptoms by at least 4 weeks. In this study, we focused on PCSx in general and did not use DSM-IV or ICD-10 to label patients as having PCS or PCD.
Following data collection, collection forms were screened according to predefined inclusion and exclusion criteria. Data from subjects who met the eligibility criteria were inputted into two electronic databases (Excel and SPSS), where data auditing and analysis were performed.
Inclusion and exclusion criteria
Participants were included if: (a) the initial consultation date was between January 1st, 2015 to December 31st, 2017 (b) age 19–55, (c) trauma occurred under any of the injury conditions specified by the ACRM (the head being struck; head striking an object; or the brain undergoing an acceleration/ deceleration movement, such as whiplash, without external trauma to the head), (d) presented with at least three or more symptoms (Appendix B excluding “Others”), (e) GCS score of 13–15, if available,
Participants were excluded for the following: (a) Do not meet one or more of the inclusion requirements, (b) moderate or severe TBIs, (c) insufficient or incomplete information to diagnose or rule out a mTBI, (d) had positive Head CT scan (hemorrhages or abnormalities), if available, (e) positive focal neurological sign due to a secondary pathology, determined by our clinician, (f) had a time delay of <30 days between the injury and initial assessment (to ensure that only chronic PCSx patients were included).
Following screening for the inclusion and exclusion criteria, the participants were later categorized into ACRM + PCSx and non-ACRM + PCSx groups. Participants in the ACRM group had at least one of the following symptoms immediately following head trauma: (a) LOC less than 30 min, (b) PTA < 24 h, (c) AMS evident by the presence (feeling dazed, confused, or disoriented) or presence of focal neurological signs at the time of injury. Thus, subjects in the non-ACRM groups had no LOC, PTA, signs of AMS or focal neurological signs immediately following the head trauma. If sufficient ACRM-related information was not available, charts were excluded from the study. All included participants had at least three chronic symptoms from the modified RPQ checklist listed in Appendix B (not including the “Others” category).
Statistical analysis
Before data collection, the sample size was calculated using G* Power Software 3.1. A total sample size of n = 88 was calculated using a significance level of α = 0.05 and power (1-β) = 0.8. Baseline patient demographics were analyzed using descriptive statistics. Quantitative analysis of a descriptor was not performed when more than 20% of data was missing. Data from patients was inputted into two electronic databases (Excel and SPSS), where data auditing and analysis were performed.
Pearson's Chi-square test (χ²) was used to compare each symptom category between the two groups. Fisher's Exact Test was used only when at least one of the cells in a chi-square contingency table had an expected frequency of less than 5. The uncorrected statistical significance level was set at p < 0.05. No correction for multiple comparisons was performed. All statistical analyses were performed using IBM SPSS Statistics Version 23.0.
Results
Participants
A total of 508 patient charts were reviewed for eligibility. 161 (31.6%) met inclusion criteria, while 347 (68.3%) patients were excluded. Of the 161 patients included, 128 (79.5%) met ACRM criteria while 33 (20.5%) were categorized as non-ACRM patients (Figure 1).
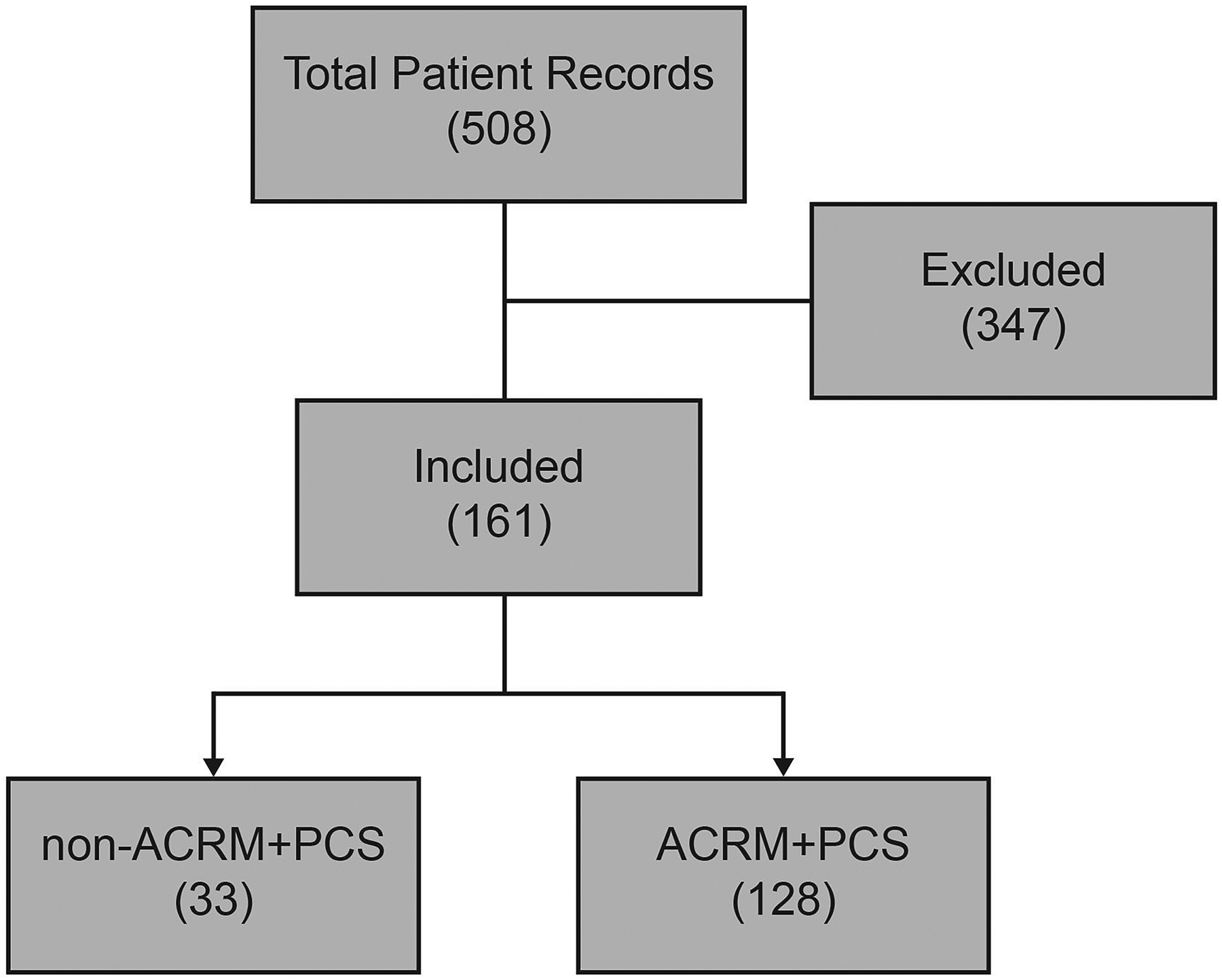
Flow chart of patient selection process.
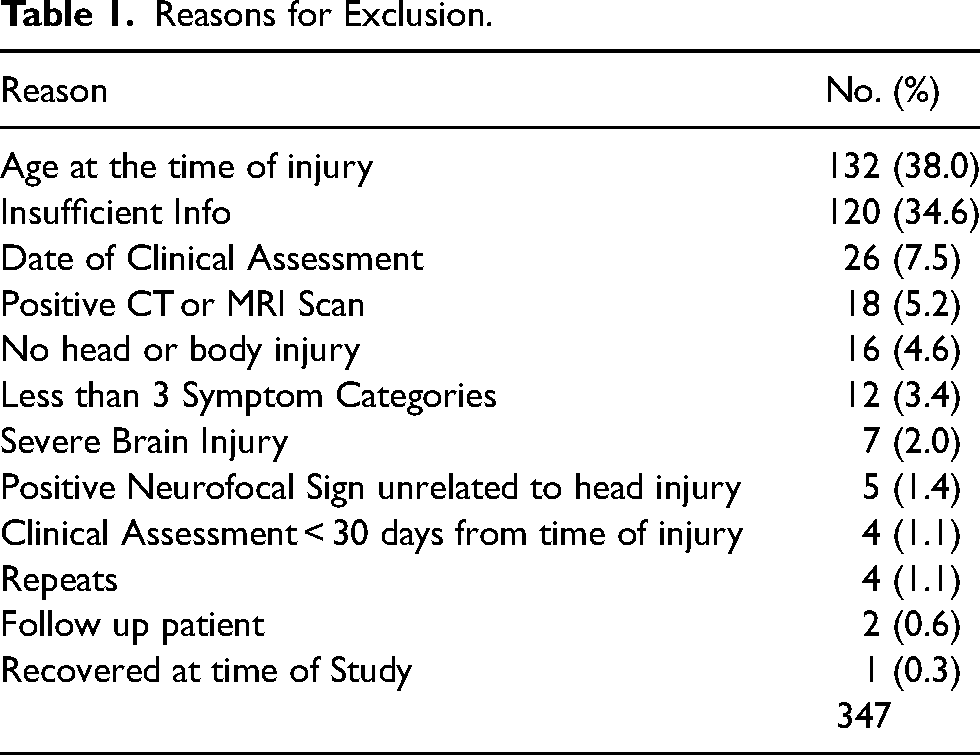
The most common reasons for exclusion were age at the time of injury (38.0%), insufficient information (34.6%), date of clinical assessment (7.5%), positive CT or MRI scan (5.2%), and no head or body injury (4.6%) (Table 1).
Reasons for Exclusion.
Demographics
The ACRM + PCSx and non-ACRM + PCSx head trauma groups had no significant difference in age, sex, history of substance abuse, and the duration of delay between the injury and first clinical assessment (Table 2). The differences in education, pre-existing psychiatric conditions, systemic injuries, previous concussions and the duration of delay between the injury and primary treatment were not assessed due to a large amount of missing data (>20% of any group). The most common mechanism of injury for both groups was motor vehicle accidents. Sports injuries and blunt trauma were more common in non-ACRM group, whereas falls were more common in the ACRM group.
Patient demographics by injury group.
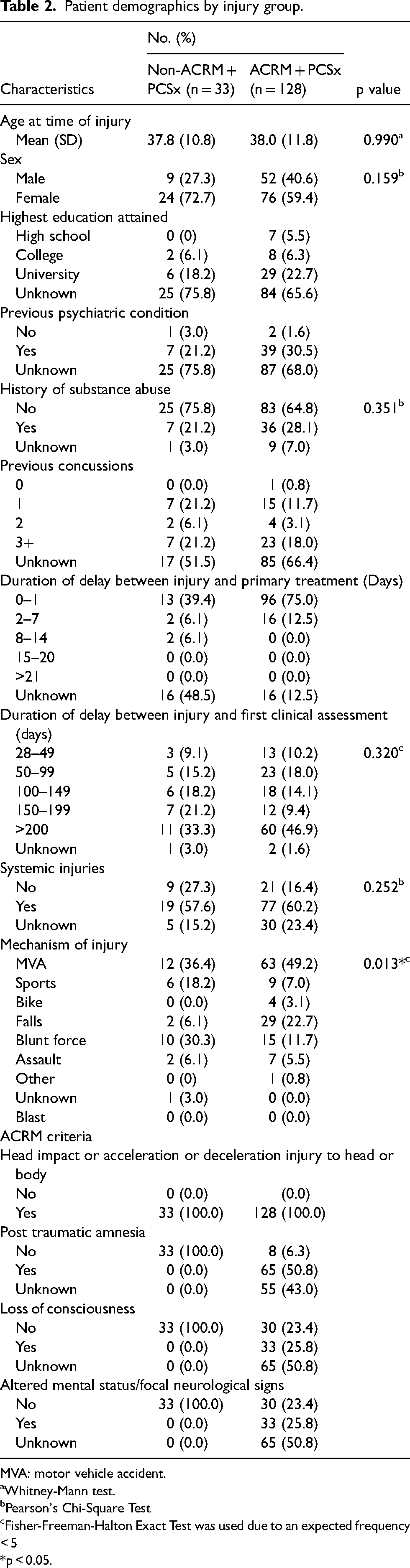
MVA: motor vehicle accident.
aWhitney-Mann test.
bPearson's Chi-Square Test
cFisher-Freeman-Halton Exact Test was used due to an expected frequency < 5
*p < 0.05.
Symptom differentiation
Headache and poor memory were the most common symptoms in both ACRM + PCSx and non-ACRM + PCSx head trauma groups. There were no statistically significant differences between the symptomology of the two groups (Table 3 and Figure 2). Appendix C shows the differences between the original 37 symptoms captured.
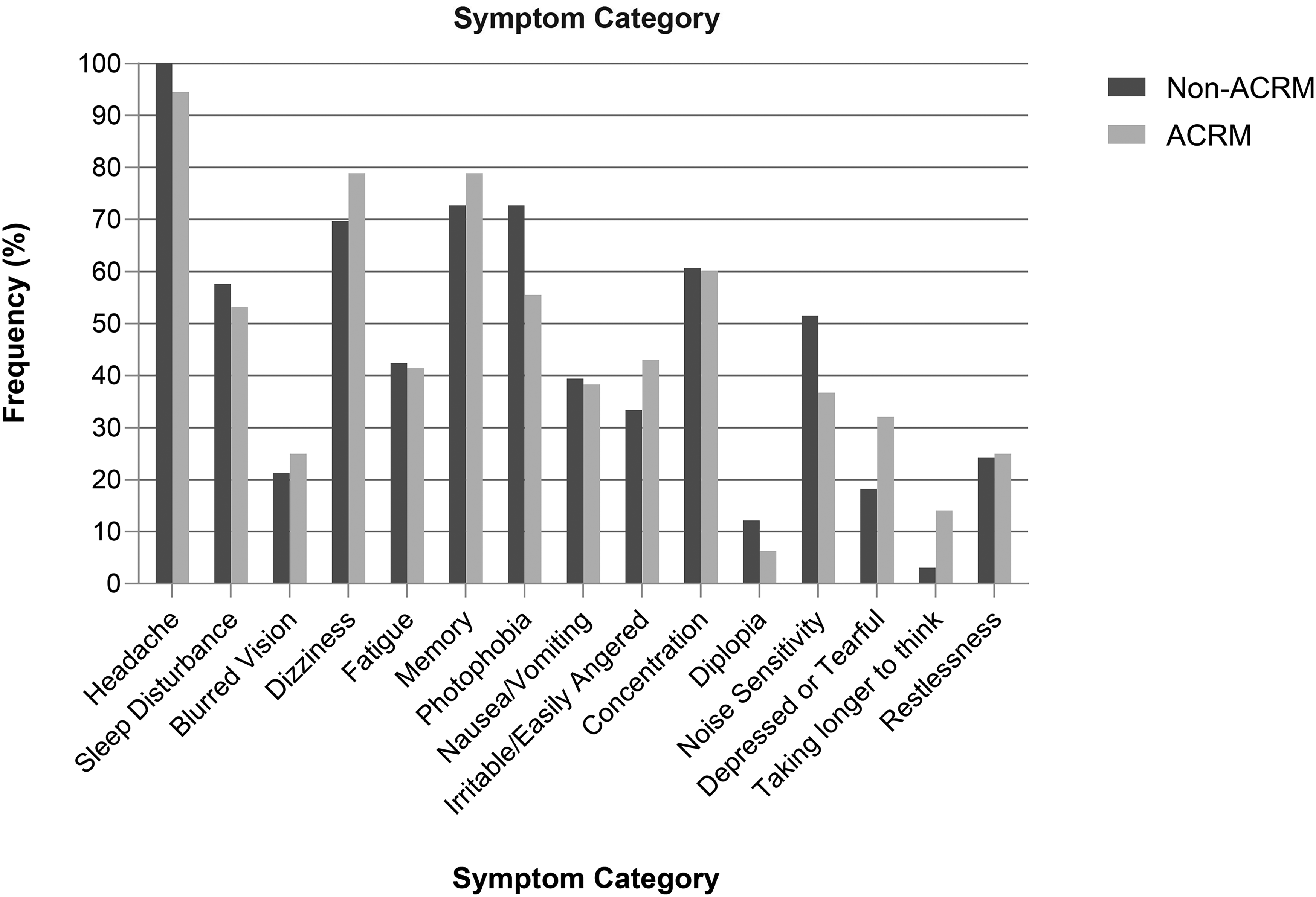
Difference in symptomatology between ACRM + PCSx and non-ACRM + PCSx groups. *Uncorrected p < 0.05.
Symptom comparison between ACRM + PCSx and non-ACRM + PCSx groups.
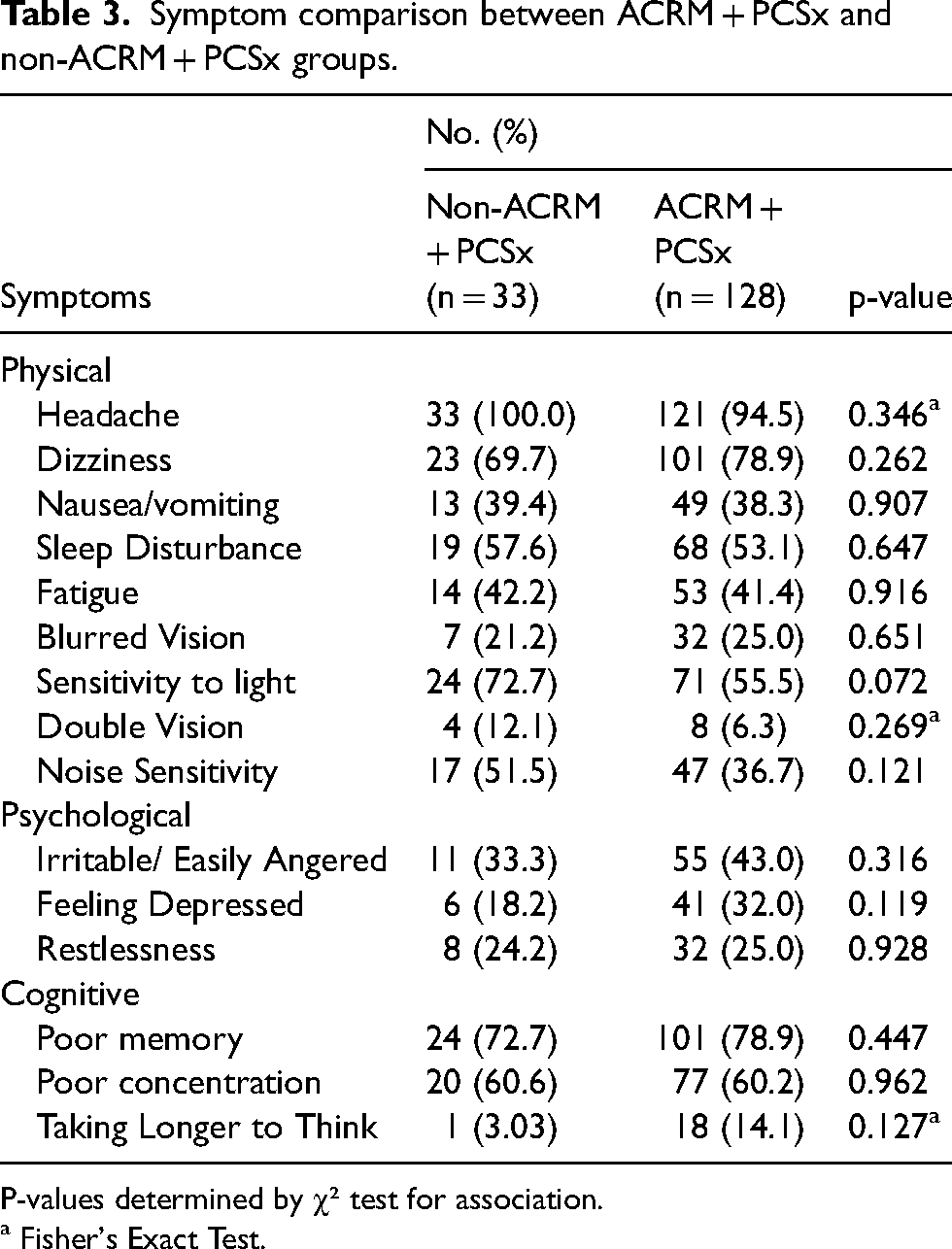
P-values determined by χ² test for association.
a Fisher's Exact Test.
Discussion
This study shows that a significant proportion (20.5%) of patients with chronic post-concussive symptoms referred to a concussion clinic did not sustain a mTBI that met ACRM criteria using retrospective data. Recently, Korley et al. conducted a prospective study recruiting ER patients who had sustained a head injury but did not meet ACRM criteria. 13 This group, which they labeled Head Injury but BRain Injury Debatable (HIBRID), is comparable to our non-ACRM + PCSx group. Korley et al. reported a high incidence of post-concussive symptoms in HIBRID patients (32.7%) at 1-month post-injury. 13 Our study supports these findings and confirms that these post-concussive symptoms can persist in the chronic stages. All patients included in our study were assessed at more than 28 days after injury, with the majority assessed at more than 150 days post injury.
In terms of specific symptomatology, Korley et al. reported that the HIBRID group had a lower incidence of moderate/severe post-concussion symptoms compared to the ACRM groups. 13 The HIBRID group also had a higher incidence of moderate/severe depression compared to trauma and healthy controls but less than the ACRM group. 13 These results contrast with our findings which suggest that there are no significant differences in the symptomatology of mTBI and non-mTBI head trauma groups. It is possible that the symptomatic differences observed during the acute stages by Korley et al. could have resolved with time. Hence, they were not evident in our study, which included participants at more chronic stages. As a prospective study, Korley et al. were able to use the RPQ to look at the symptom severity and not just the presence or absence of symptoms.
One explanation for the similar symptoms seen in both the ACRM and non-ACRM groups is that they both may have suffered a brain injury. It is possible that the non-ACRM population had sustained a low threshold head trauma, resulting in milder brain injuries. Initially, these milder injuries did not elicit any instantaneous symptoms and thus were not captured by ACRM and other current diagnostic criteria.13,14 Nonetheless, these injuries can produce post-concussive symptoms that are essentially indistinguishable from those seen after a mTBI that meets ACRM criteria. In our study, both groups are similar in their demographic variables except for mechanism of injury. However, without further details it is difficult to ascertain whether differences in the mechanism of injury indicate a difference in the severity of head injury. Considering this, a need to incorporate more sensitive testing that can detect milder brain injuries, such as advanced imaging techniques or biomarker quantification, becomes evident.14–16 Early detection and labeling of these sub-threshold mTBIs would help us to provide appropriate care and mitigate long-term consequences.
Another explanation for persisting post-concussion symptoms in both groups is that there may be a common underlying pathophysiology. 17 Neuro-inflammation is a secondary injury mechanism associated with symptoms seen after TBI.18–20 It is also associated with many post-concussion-like symptoms seen in systemic infections and musculoskeletal trauma, such as whiplash and surgery.21–23 The neuro-inflammation hypothesis posits that whenever a trauma occurs, irrespective of the cause, the body launches an immune response that triggers neuroinflammation and can cause post-concussion symptoms through altered brain function.17,20 This could explain the presence of persistent post-concussive-like symptoms in both non-ACRM and ACRM participants. Despite missing data, a high prevalence of comorbid systemic injuries (ACRM: 60.2%, non-ACRM: 57.6%) was observed in both groups, that could also trigger neuroinflammation. While neuroinflammation has been seen objectively in mTBI patients with persistent post-concussion symptoms using single photon-emission computed tomography (SPECT), 24 this has not been investigated in non-ACRM head injury groups suffering from post-concussion symptoms. This suggests a need to investigate the role of neuroinflammation in post-concussion symptomatology in the non-head injured population. 18
Development of post-concussive symptoms following trauma also depends on the presence of various pre- and post-injury risk factors besides the head injury itself. Female sex, pain, previous anxiety and affective disorder, acute post-traumatic stress, higher IQ, history of drug or alcohol abuse, previous head trauma, genetics, personality, and environmental factors are associated with the development of PCSx after trauma.4,25–31 In our study, we were unable to explore these factors in depth due to missing information. However, consistent with the finding that post-concussion symptoms are more common in women, most patients referred for post-concussion symptoms in our study were female (62.1%, n = 100). Despite missing data, there was also a high prevalence of previous concussions in both the ACRM (26.08%) and non-ACRM group (48.4%), which makes both groups potentially more prone to developing similar post-concussion symptoms. To better understand the role of non-ACRM head injuries in causing post-concussion symptoms, future studies may consider comparing patients with no previous history of head trauma.
Considering the role of various injury and non-injury-related factors in shaping clinical outcomes following trauma, the concept of a single underlying cause seems inadequate.32,33 There is a growing acceptance of the “Biopsychosocial Model,” which stipulates that the complex interactions between biological, psychological and social factors and various unique injury-related and non-injury-related factors are responsible for multiple post-concussion symptoms.31,33–35 Kenzie et al. proposed a model in which four groups of factors interact with each other to affect mTBI injury and recovery.36,37 These include cellular (e.g., axonal injury, neuroinflammation), network (intrinsic connectivity networks), experiential (e.g., psychological, and cognitive symptoms) and social factors (healthcare access and available social supports). These factors are further influenced by injury biomechanics, injury context and personal characteristics (e.g., genetics, age, sex).36,37 Currently, these models provide the most plausible explanation for why mTBI and other non-mTBI groups may have similar clinical presentations. Any trauma that triggers one of these scales, regardless of the cause, may give rise to post-concussion symptoms. Similarly, Iverson proposed the idea of network connectivity. 32 This theory implies that post-concussion symptoms occur together, not because they are all due to a common underlying pathology, but because they are strongly interrelated, each triggering and worsening the next.
Conclusion
This study found that a significant proportion of head trauma patients present with chronic post-concussion symptoms despite not meeting ACRM criteria for mTBI (20.5%). There is no difference in the chronic symptomatology between the patients who meet ACRM criteria and those who do not. Future studies should focus on exploring these populations using emerging techniques that can better detect and evaluate the extent of head injury. They may also consider exploring the role of factors such as previous mTBIs, psychiatric factors and neuroinflammation in the head trauma population that does not reach the threshold for mTBI.
Limitations
The conclusions drawn by the study are impacted by certain limitations. In a retrospective chart review, data is prone to omissions, inconsistencies, and the possibility of recall bias during consultations. Moreover, there is also the problem of incomplete or missing data in patient charts. This prevented us from exploring the role that previous mTBI and psychiatric history may play in influencing post-concussion symptoms, as well as how symptoms at the time of injury relate to those present before the head trauma.
Supplemental Material
sj-docx-1-ccn-10.1177_20597002231173772 - Supplemental material for Do concussed and non-concussed head trauma individuals have similar symptoms? A retrospective chart review of chronic post-concussive symptomatology
Supplemental material, sj-docx-1-ccn-10.1177_20597002231173772 for Do concussed and non-concussed head trauma individuals have similar symptoms? A retrospective chart review of chronic post-concussive symptomatology by Shazia Malik, Rahim Ahmed, Teresa Gambale and Michel P Rathbone in Journal of Concussion
Supplemental Material
sj-docx-2-ccn-10.1177_20597002231173772 - Supplemental material for Do concussed and non-concussed head trauma individuals have similar symptoms? A retrospective chart review of chronic post-concussive symptomatology
Supplemental material, sj-docx-2-ccn-10.1177_20597002231173772 for Do concussed and non-concussed head trauma individuals have similar symptoms? A retrospective chart review of chronic post-concussive symptomatology by Shazia Malik, Rahim Ahmed, Teresa Gambale and Michel P Rathbone in Journal of Concussion
Supplemental Material
sj-docx-3-ccn-10.1177_20597002231173772 - Supplemental material for Do concussed and non-concussed head trauma individuals have similar symptoms? A retrospective chart review of chronic post-concussive symptomatology
Supplemental material, sj-docx-3-ccn-10.1177_20597002231173772 for Do concussed and non-concussed head trauma individuals have similar symptoms? A retrospective chart review of chronic post-concussive symptomatology by Shazia Malik, Rahim Ahmed, Teresa Gambale and Michel P Rathbone in Journal of Concussion
Footnotes
Acknowledgements
We appreciate the support of Dr Shajiullah Khan, Adrienne Atayde, and Sabrina Campbell for helping with the initial study planning and organization. We are thankful to Dr Bill Parkinson for his valuable feedback on data analysis. This work was supported by Dr Benecio Frey, Dr John Bienenstock and Dr Joseph Gabriel at McMaster University, Canada.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
