Abstract
Inverted papilloma is a rare and benign tumour. It affects the nasal cavity and paranasal sinuses, has a high rate of recurrence and is associated with malignant transformation. Only few cases of a poorly differentiated carcinoma arising from inverted papilloma have been reported, none of which in the nasopharynx. We report a case of a 37-year-old female, who presented originally in 2012 with inverted papilloma of the nasal septum which was surgically resected. Nasopharyngeal biopsy from 2014 was reported as carcinoma in situ and treated with local endoscopic resection. Three years later she presented with a solitary lesion of the right Eustachian tube opening, confirmed as invasive poorly differentiated carcinoma. Imaging revealed T4 N2b M0 malignancy with skull base and prevertebral space invasion, likely extension into right temporal lobe and malignant adenopathy. Although rare, malignant transformation of inverted papilloma in unusual places should be considered during workup and monitoring of patients.
Introduction
The ectodermal Schneiderian mucosa can give rise to a variety of distinct types of sinonasal Schneiderian papillomas. Classified due to their patterns of growth, papillomas with endophytic growth are named inverted papilloma (IP), papillomas with exophytic growth as fungiform and a third group as cylindrical cell papillomas (sometimes known as oncocytic).1,2 In terms of anatomic localisation, Schneiderian septal papillomas are believed to remain on the septum with very limited malignant potential, whereas papillomas of the lateral wall may involve sinuses, floor and roof of the nasal cavity and the nasolacrimal apparatus and are known to be associated with squamous cell carcinomas (SCCs). 2 The main clinical problems associated with IPs include local bone destruction, a high rate of recurrence (between 28% and 74%) and associated malignant transformation. 3 They can develop synchronously or occur after previous resection of an IP, that is, metachronously.
Only few cases of a poorly differentiated carcinoma arising from IP have been reported, none of which in the nasopharynx. We report a case of this rare lesion, which was initially confirmed to be a carcinoma in situ arising from a septal Schneiderian papilloma, but about 6 years later returned as an invasive poorly differentiated carcinoma of the nasopharynx (Figure 1).

Timeline from initial presentation of IP to diagnosis of invasive carcinoma.
Case
A 31-year-old woman was referred to our hospital following surgery for an endonasal tumour. Suffering from worsening right nasal obstruction, rhinorrhoea and bleeding for approximately 5 months, she had visited a local hospital and had been taken to theatre for removal of, what had appeared to be, a viral papilloma on the right side of her nose. Biopsy at that time confirmed high-grade dysplasia carcinoma in situ presumably arising from within a Schneiderian IP. A physical examination was unremarkable, and a flexible rhinoscopy did not show any abnormalities on the left side and a difficult view on the right, which rendered it impossible to identify the base of the lesion. The rest of her medical history was unremarkable, and she was on no regular medications.
A computed tomography (CT) following her initial presentation revealed a soft tissue mass filling the right nasal cavity with opacification of the right maxillary, frontal and ethmoidal sinuses and thinning of the medial wall of the right maxillary sinus (Figure 2).
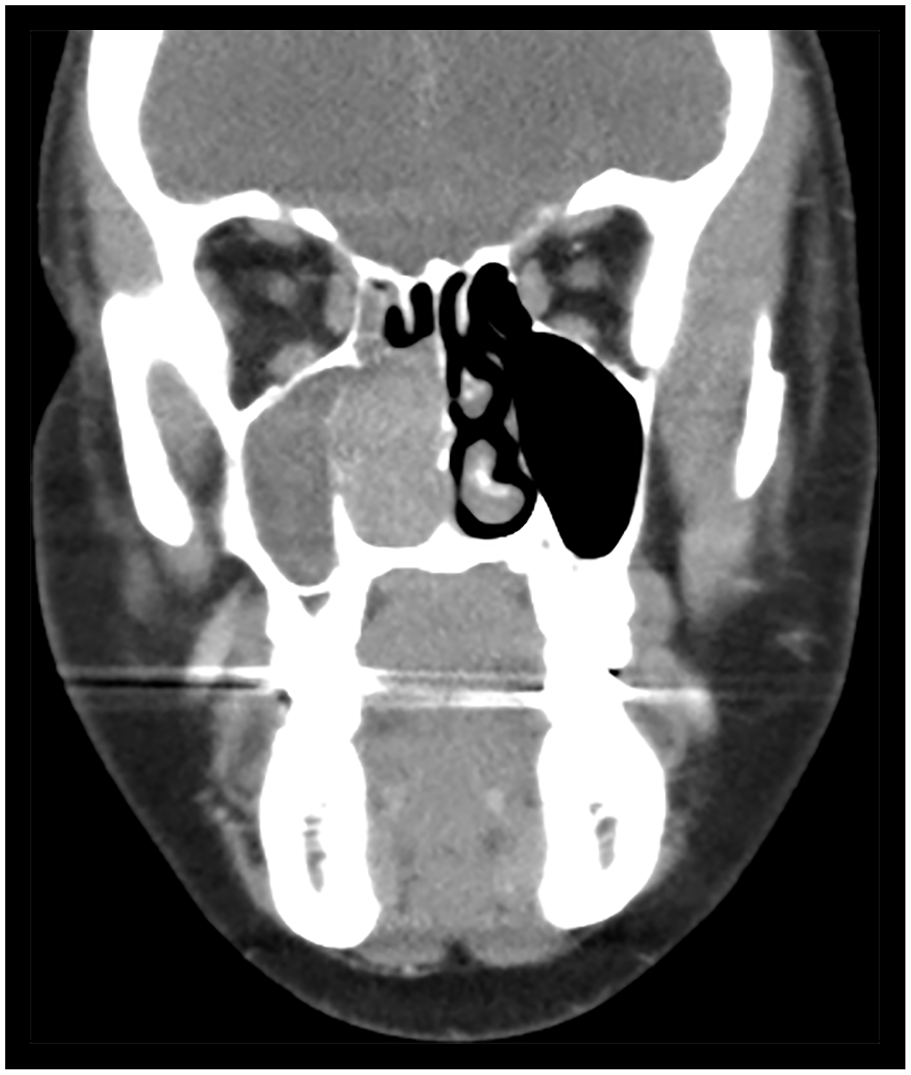
Coronal computed tomogram with contrast showing initial carcinoma in situ involving the right septum.
She was taken back to theatre approximately 6 weeks following her initial surgery for further endonasal full thickness resection of the site of origin, right middle meatal antrostomy, uncinectomy and limited anterior ethmoidectomy. Biopsy of the right nasal septal lesion showed a papillary carcinoma in situ, compatible with an origin in a Schneiderian papilloma (Figure 3(a)). Because of difficult histology and inconclusive margins, close clinical surveillance was advised. Over the following 2 years the patient had two further endonasal resections with no evidence of recurrence. However, 2.5 years after her initial surgery she presented with new symptoms of bloodstained nasal discharge and a follow-up rhinoscopy demonstrated evidence of a skip lesion in the nasopharynx. Surgery confirmed an extensive exophytic papillomatous lesion arising from the posterior nasopharyngeal wall and extending into the fossa of Rosenmüller, which was subsequently resected endoscopically (Figure 4). Biopsy demonstrated a lesion with features, again, of a nasopharyngeal carcinoma in situ arising from a Schneiderian papilloma, followed by a CT scan that showed post-surgical changes but no evidence of invasion. Over the next 3 years the patient was followed up closely with 3- to 6-monthly clinic visits and two further biopsies, all unremarkable, until she presented with right-sided hearing loss, otalgia as well as bloody discharge from the back of her throat. A right myringotomy with grommet insertion was performed in addition to biopsy of a solitary exophytic lesion of the right Eustachian tube orifice, which turned out to be an invasive poorly differentiated carcinoma with some squamous features (Figure 3(b) and Figure 5).

Haematoxylin and eosin–stained tissue sections. (a) Carcinoma in situ within inverted sinonasal papilloma at 200× magnification. (b) Invasive squamous cell carcinoma at 40× magnification.

Endoscopic view of the nasopharynx. Recurrence of carcinoma in situ arising in Schneiderian papilloma from the posterior nasopharyngeal wall and extending into the fossa of Rosenmüller. This was 2.5 years following the initial presentation.

Endoscopic view of the post-nasal space. Recurrence of an invasive poorly differentiated carcinoma at the right eustachian tube orifice 6 years after the initial presentation.
CT and magnetic resonance (MR) imaging revealed a T4 N2b M0 malignancy centred in the right post-nasal space with skull base and prevertebral space invasion, likely extension into the medial part of the right temporal lobe and malignant adenopathy (Figure 6). Due to the extensive invasion of the cancer the patient was offered 6 weeks of palliative chemotherapy in form of paclitaxel (40–45 mg/m2/week) and carboplatin (100 mg/m2/week) with subsequent radiotherapy (70.2 Gy at 1.8 Gy/fraction/day for 5 days/week) to achieve a period of local control.

Computed tomogram with contrast. (a) Coronal view showing malignancy centred in the right post-nasal space with skull base and prevertebral space invasion, likely extension into the medial part of the right temporal lobe and malignant adenopathy. (b) Axial view showing extensive nodal disease.
Discussion
IPs are the most frequent type of Schneiderian papillomas and represent 0.5%–5% of all primary sinonasal tumours. They occur predominantly in male patients, typically peaking around the age of 50 years. According to a review by Barnes (2002), IPs rarely arise from the nasal septum (around 8%), as described in this case, but typically originate from the lateral nasal wall close to the middle turbinate or ethmoid recesses, often extending into the maxillary and ethmoid sinuses, and to a lesser extent into the frontal and sphenoid sinuses. 4 Unilateral nasal obstruction is one of the most common presenting symptoms followed by epistaxis, nasal discharge and anosmia. 5 Complete surgical resection is still the mainstay of treatment for an IP owing to its propensity to local destruction, recurrence and potential malignant transformation.3,6,7 Recurrences in particular can progress without any significant presentation of symptoms. 7 Often occurring early at the original site of the surgery, incomplete local resection is believed to be a major cause for IP recurrences, with a chance of subsequent recurrence lying around 58%.2,8 Varying incidences of carcinomas associated with IPs have been reported in the literature, ranging from 0% to 53%. 6 Types most commonly found are SCCs followed, to a much lesser extent, by verrucous, mucoepidermoid, spindle and clear cell carcinomas and adenocarcinomas. 4 The associated SCCs may arise from the papilloma itself or as separate synchronous lesion with no previous history of resection. A metachronous SCC, however, develops at or near the site of a previously resected benign IP.5,7 Synchronous carcinomas are more common than metachronous, occurring in 61% of reported cases of carcinomas associated with IPs, whereas metachronous carcinomas make up 39%. 4 Mirza et al. reviewed a total of 3058 cases of sinonasal IP, reporting dysplasia in 12% of cases, carcinoma in situ in 3.4%, synchronous carcinoma in 7.1% and metachronous carcinoma in 3.6%. The authors also suggested long-term follow-up to allow early detection of recurrences, and thereby preventing silent and undetected progression of the disease. 7 Interestingly, Lesperance and Esclamado 9 observed that for metachronous carcinomas the mean time from the IP to the SCC onset was 63 months (6 months–13 years). In this patient, we believe that a metachronous nasopharyngeal cancer developed 6 years following initial resection of a benign septal IP. To our knowledge this is the first reported case of a septal IP with subsequent transformation into a poorly differentiated invasive carcinoma of the nasopharynx. Only few similar cases have been described in the literature. Garcia et al. 10 reported a case of a SCC arising from an IP in the maxillary sinus with extension to and involvement of the oral cavity. A retrospective study by Liang et al. 11 looked at medical records from 87 patients with IPs and associated SCCs and found that most tumours were located in the ethmoid region, maxillary sinus or lateral nasal wall, rather than other sides. Similar results were reported by Lobo et al. 12 who showed that in 29 patients with SCCs and associated IPs sites most commonly involved were maxillary sinuses followed by the nasal cavity. Unfortunately, both groups failed to mention more details about these more rare sites, particularly where metachronous SCCs were identified. However, Liang et al. 11 suggested that as much as possible of the tumour should be removed with a safe resection margin to decrease the total number of surgeries necessary for IPs. A study by Sulica et al. (1999) reported 16 cases of Schneiderian-type mucosal papillomas in the nasopharynx and oropharynx. One patient was found to have a separate nasopharyngeal SCC, however, this patient had received radiotherapy for a cancer of unknown primary beforehand. Even though malignant transformation precipitated by radiotherapy was thought to be unlikely, the authors acknowledge that ectopic papillomas harbour a malignant potential. 13 This has to be set in context to the known propensity of the upper aerodigestive tract to give rise to multiple SCCs from an area of epithelium that has been preconditioned by long-term exposure to carcinogens such as tobacco and alcohol.14,15
It could be argued that in our case they were two different pathologies arising at different points in time, however, a simultaneous diagnosis of IP of the posterior septum and persistent carcinoma in situ especially around the posterior septum, choana and nasopharyngeal area implies that they could have been related pathologies. Our patient was a healthy, young woman who presented with an unusual pathology, unlikely to be due to the effects of field cancerization. However, to proof a clonal relationship further genetic testing would be necessary. We acknowledge that no final conclusions can be drawn from a single case presentation. Nevertheless, we believe that the time course as well as the anatomic location of the pathologies allow the presumption that this might have been a metachronous tumour and not a simple association of two separate diseases.
Although rare, malignant transformation of IP in unusual places should be considered during workup and monitoring of patients. Particularly length and frequency of follow-up needs to be planned carefully.
Footnotes
Authors’ note
Poster Presentation at BACO International 2018 in Manchester, UK, on 04–06 July 2018.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Informed consent
Full written informed consent was obtained from the patient in using endoscopic images and radiologic images after discussing the details of the case report contents.
Consent for publication
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
