Abstract
Background:
Urinary tract infections are the primary factors that cause mortality and morbidity in patients with underlying comorbid conditions and are responsible for most hospital admissions worldwide.
Objectives:
The study aims to identify the common bacterial uropathogens and determine their antimicrobial susceptibility pattern, including multidrug-resistant/extensively drug-resistant bacteria.
Methods:
The descriptive cross-sectional study was conducted among inpatients provisionally suspected of urinary tract infections in the medical ward of Koshi Hospital, Biratnagar, Nepal. Samples were inoculated in a cystine lysine electrolyte-deficient medium, and pure growth of significant bacteria was further subjected Gram staining, biochemical identification, and antimicrobial susceptibility testing as per laboratory standard procedure and Clinical Laboratory Standards Institute guidelines, respectively. Descriptive and inferential statistical analysis was performed to analyze the outcomes and a
Results:
A total of 305 patients urine specimens were examined, of which 251 (82.29%) samples resulted in significant bacterial growth in the culture.
Conclusion:
Introduction
Urinary tract infections (UTIs) and antimicrobial resistant (AMR) have become major public health problems worldwide, posing substantial health complications and socioeconomic burdens to society. 1–3
Methodology
The selection criteria for variables were determined based on their relevance to the research objectives and their potential outcomes. The primary outcome variable was to determine prevalent uropathogens and their drug-resistant profiles from collected urine samples. The evaluation was carried out using standardized antimicrobial susceptibility testing following recent Clinical and Laboratory Standards Institute (CLSI) guidelines.
Sample size calculation and sampling techniques
Sample size calculation was done by application of sensitivity of gold standard from a previous study 14 applying, 5% margin of error and 95% confidence level, and a prevalence of 25.24% estimated from a previous study conducted by Joshi et.al. 9

The required sample size is 292. Adding extra 15 (5%) samples to overcome some unlabeled, mislabeled, leaked containers, contaminated samples, or non-clean catch midstream urine. Therefore, our sample size was estimated to be 290 + 15 (5% of 290) = 305.
Data collection techniques
Data were collected in a data collection tool referring to the inpatient’s case sheets and laboratory reports including culture, and sensitivity test of urine samples of participant. Female participants were informed to clean their peri-urethral area with soap and water then cleanse the area applying sterile gauze to collect 5–10 ml of freshly voided midstream urine using sterile and wide-mouthed plastic bottles with a tight cap. Then the collected midstream urine specimens were transferred to the medical microbiology laboratory of Koshi Zonal Hospital. Most of the urine samples were processed within 2 h, and about (0.1 g) of boric acid was used as a preservative and refrigerated at 4°C if the transport of the specimens was delayed.
Ethical considerations and patient consents
Ethical approval was obtained from the Institutional Review Committee of Purbanchal University College of Medical and Allied Science (PUCMAS) (Ref no IRC/014/2020). The study was undertaken during the COVID-19 pandemic surges up period and involves analysis based on routine laboratory culture and sensitivity tests on clinician’s references. Therefore, verbal informed consent was obtained by the researcher and clinical staffs following brief explanation and clarification of objectives and purpose of study.
Laboratory proceeding for urine culture, bacterial identification, antimicrobial susceptibility tests, and quality control
Urine culture was preceded by applying a semi-quantitative method on CLED (HiMedia, India) agar plates with an Andrade indicator. The inoculating loop that possesses standard dimension was calibrated to ensure the volume of urine adjusted in a loop (0.001 ml) for inoculation of a urine sample. The samples were mixed properly so that bacteria remain uniformly suspended before inoculating in CLED. The samples were inoculated to CLED agar and incubated for 24 h at 37°C.
Quality control
Strict measures were followed from the pre-test to the post-test phase. The questionnaire was pretested in 15 patients with symptomatic bacteriuria at Koshi Zonal Hospital. All the laboratory tools and reagents were validated before the experiment. Quality control of each agar plate prepared was checked by incubation of the plate in the incubator after preparation. The American Type Culture Collection (ATCC) strains were used to check the efficacy of various prepared biochemical for microbe identifications. For correct interpretation of disk diffusion tests, at first, the thicknesses of MHA were maintained approximately 4 mm as well as pH was adjusted to 7.2–7.4 before preparation based on the manufacturer’s instructions. Freshly prepared media were tested using control species of bacteria (i.e. known organisms to check its indicators performance). For validation of Gram staining kits
Case definition
MDR/XDR and pan drug-resistant
MDR bacteria are defined as bacterium resistant to at least three or more categories of antibiotics of different groups. XDR organisms are designated as a bacterium resistant to at least one antimicrobial category of all groups but remains susceptible to fewer (one or two) antimicrobials. Pan-drug resistant (PDR) organisms are known as drug-resistant acquired by bacteria to almost all the commercially available antibiotics. 18
Data processing and analysis
The collected data were entered in MS Excel 2019 to record all relevant information such as patient’s demographic details, comorbidities, and culture and sensitivity test report following the outcomes. Descriptive statistics were calculated to summarize the characteristics of the study population and key variables. Frequencies and proportions were used to describe categorical variables, whereas measures of central tendency (mean, median) and dispersion (standard deviation) were used for continuous variables. Bivariate analysis was conducted to explore the relationships between the independent variables and the outcome variable of interest MDR/XDR profile. Chi-square tests were performed to assess associations between categorical variables, such as age, gender, diabetes, hypertension, and multiple antibiotic therapy, with the MDR/XDR profile. Multivariate analysis was conducted using binary logistic regression to examine the independent effects of the variables on the MDR profile while controlling for potential confounding factors. The crude odds ratio (COR) and adjusted odd ratio (AOR), 95% CI, and
Results
Demographic data and baseline characteristics of the patients
A total of 305 patients participated in our study, of which the majority of participants were female (69.8%) as compared to male (30.2%). The mean ages of the participants were found to be 43.94 years (SD ± 19.11). Most patients were married (79.7%). The most common comorbidity was diabetes mellitus (27.2%) followed by hypertension (13%) as illustrated in Table 1.
Demographic baseline data and characteristics of participants (

While going through routine microscopic examination of urine specimens, our results showed that the majority of UTI-suspected patients (75.2%) had pyuria (pus cell ⩾5/HPF). Some degree of microscopic hematuria (>5/HPF) was present in 8.19% of patients and 43.9% of patients had high epithelial cell cast >5/HPF. The results are summarized in Table 2.
Routine urine test parameter results (
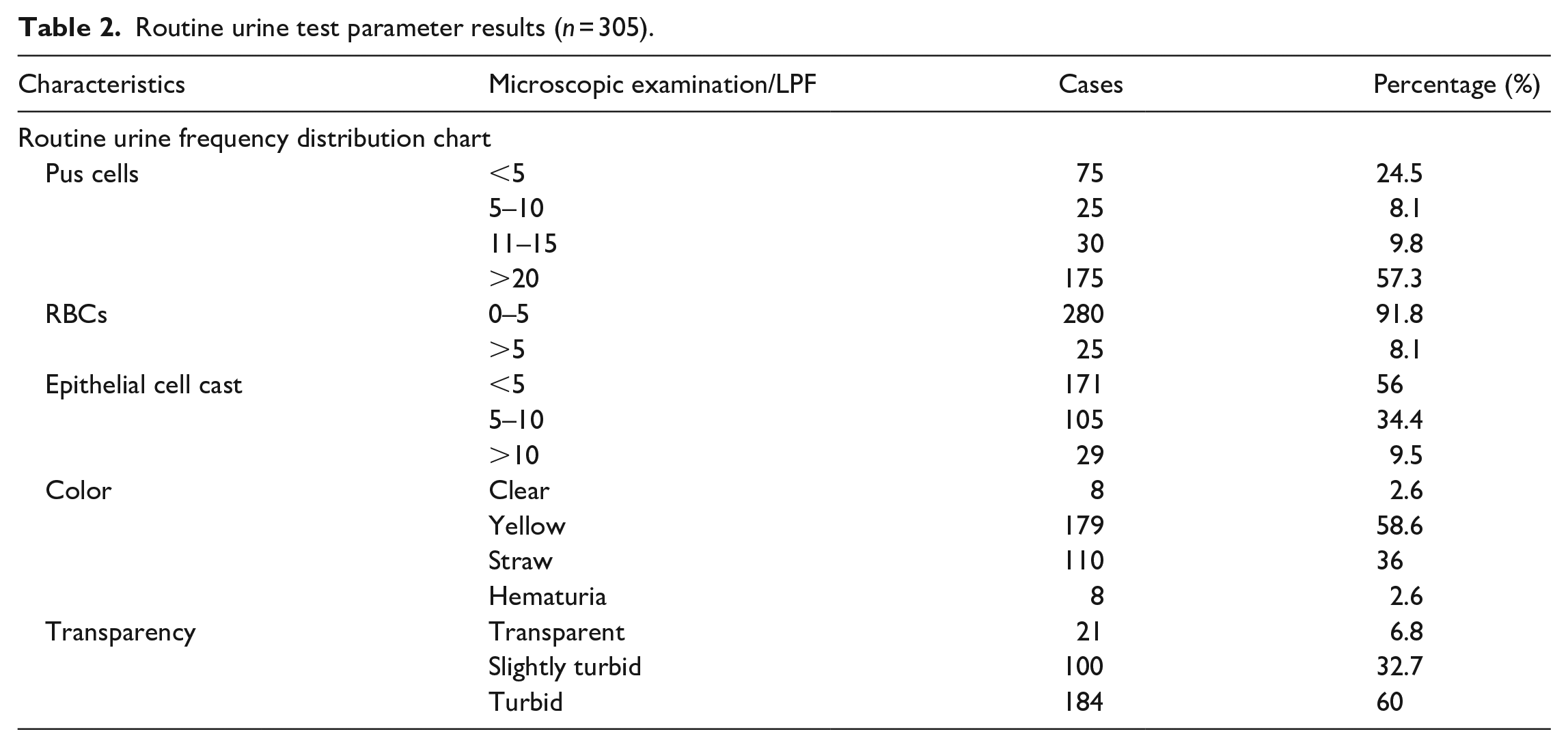
Out of a total of 305 samples processed for urine culture and sensitivity, 54 (17.70%) showed no growth. About 251 (82.29%) samples revealed growth in the culture.
Isolated bacterial frequency distribution from urine culture reports (

Antimicrobial-resistant rates of uropathogens
Antimicrobial-resistant rates were observed against five gram-negative bacteria and two gram-positive bacteria. Based on results represented in Table 4, there was no drug-resistant observed in colistin in all tested four gram-negative bacteria (Resistant rate = 0) except
Antimicrobial resistant rates of commonly tested antibiotics on various uropathogens.

IR: intrinsic resistant; NT: not tested.
“0” indicates that there is no resistant observed among tested isolates.
MDR and XDR uropathogens
Different groups were tested in both gram-positive and gram-negative bacteria to evaluate MDR and XDR profiles. Out of them, altogether
MDR and XDR profile of uropathogens.
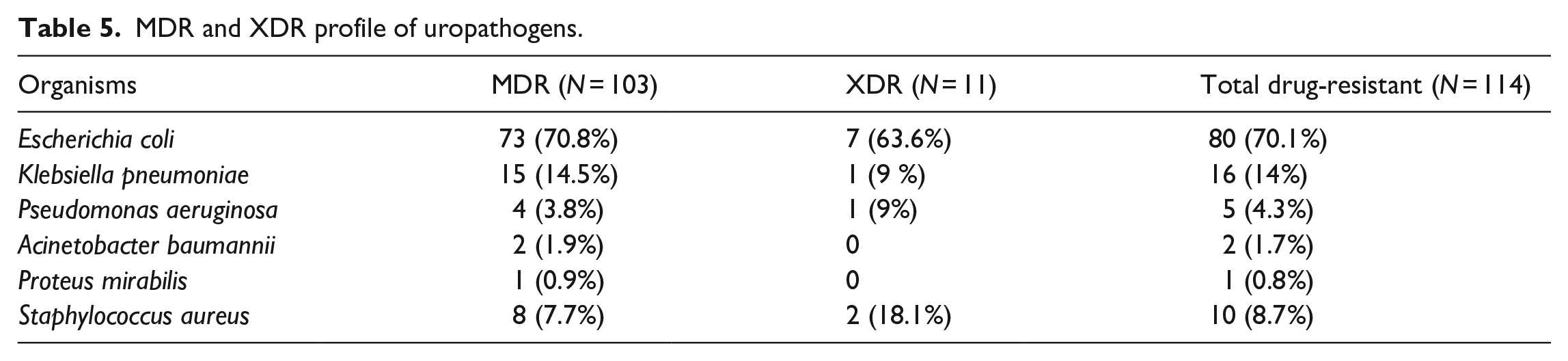
Bivariate and multivariate logistic regression analysis was applied to determine the association between dependent and independent variables. Various independent groups ( gender, age groups, marital status), comorbidities (diabetes mellitus and hypertension) as well as multiple antimicrobial therapies were tested for the outcome of colonization of drug-resistant pathogens. The reference group had an odd ratio adjusted as OR = 1 as shown in Table 6. Based on bivariate analysis independent variables such as diabetes mellitus and combined antimicrobial therapy showed a strong association (
Risk factors associated with the development and colonization of MDR/XDR uropathogens (

COR: crude odd ratio; AOR: adjusted odd ratio; ref: reference in a dichotomous variable; NA: not applicable; CI: confidence interval;
Discussion
UTIs are common worldwide and range from mild symptoms to severe complications. 19 The treatment of UTI is becoming challenging due to the emergence of MDR microorganisms.2,11 In our study, mostly females (69.8%) had UTIs as compared to males. Females are more prone to UTIs because of several reasons including anatomy based on gender that is, shorter urethra, the proximity of the urethra to the anus in females as well as entry of pathogens promoted by sexual intercourse among females with relationship status in sexually active age group, and other factors like estrogen deficiency. 20 Based on our study, diabetes mellitus 83 (27.2%) was the most common comorbidity among patients with UTI. As UTI cases are more prominent in diabetic patients compared to non-diabetics. 21 The reason for this is not well explained, but two hypothetical explanations are supported by published study that is, dysfunction of the urinary bladder and poor prognosis manifested as glycosuria might increase the risk as explained by De Lastours et al. 22 as the bacteria might replicate utilizing the glucose in urine.
In this study, the urine routine microscopy parameters were taken as a marker in prompt diagnosis of UTI as urine culture takes at least 24 h to diagnose the infection. Routine urine examination shows a significant amount of pyuria (75.2%) in most of the participants. These findings are supported by the study conducted in central Nepal which determined the pyuria as a prime marker for suspecting UTI. 23 Concordantly, the rise in epithelial cells in cases of participants also primarily suggests performing cultures for confirmation of UTIs. This conclusion has been supported by a study conducted at the University of Iowa that had shown some efficacy in predicting bacteriuria. 24
In our study,
In this study, the results of the antimicrobial-resistant pattern assessed on different antibiograms demonstrate that two groups of antibiotics (cephalosporin and penicillin groups) show higher resistant rates for all isolates, whereas the polymyxin group remains highly susceptible to the drug-resistant uropathogens. Similar studies conducted in Nepal11,12 and another country32
–34 had revealed a higher rate of resistance among penicillin and cephalosporin group of antimicrobials. Nevertheless, the polymyxin group for gram-negative uropathogens still remains 100% susceptible for most of the severe UTI cases that were influenced by MDR/XDR bacterial strains. The outcomes of treatment effectiveness of this drug were also discussed in several recent studies as well.35,36 The glycopeptides and oxazolidinone group (vancomycin and linezolid) showed great antimicrobial potency among gram-positive bacteria in our study. The study from the USA also showed the efficacy of the broad-spectrum drug tetracycline group, glycopeptides, and oxazolidinones group had superior efficacy with low resistant rates to treat gram-positive uropathogens including methicillin-resistant
The high prevalence of MDR and XDR in our study among gram-negative uropathogens was reported in
Based on the finding of risk factors in our study, the higher incidence of existing comorbidity like diabetes mellitus results in more than twice the greater odds of colonization and development of MDR bacteria as compared to non-diabetic patients. One reason behind it is these types of comorbidity negatively interact with the immune system which leads to develop a greater risk factor for the infection. Similarly, the pharmacokinetics of antibiotics in obese diabetic populations could also lead to suboptimal levels of antibiotic concentrations and increase the risk of antibiotic resistance.44 –46 Moreover, diabetics could acquire the most resistant strain of pathogens due to frequent hospital visits. This finding was supported by a British study on systematic review and meta-analysis that had compiled reports on the high resistant rate of antimicrobials in diabetics patients, particularly in UTIs and respiratory tract infections similar to our findings. 45 Apart from that, our findings also highlight the need for combined antibiotics therapy for the treatment of MDR and XDR bacteria. Patients under combined therapy had lower odds of MDR and XDR bacteria as compared to those who did not receive them. The study conducted in Greece highlights the need for combination therapy to treat XDR infection. 47 Another Japanese study claimed the necessity of combined antimicrobial therapy to combat MDR bacteria. 48
There are several limitations of our study as the study was a single-centered study, which limits the study to be conducted in mass sample size. The use of convenience sampling may limit the generalizability of the findings to a broader population and lack of control over the sample composition. More importantly, the research conducted in low resource country restrains us from conducting molecular assays to evaluate the genes responsible for evolving uropathogens into MDR and XDR bacteria. Despite limitations, our study possesses some strength as these findings are important for reviewing empirical therapy as the study has a prime focus on MDR/XDR strains of uropathogens. Apart from that, documentation of predisposing factors and statistical analysis determines the leading risk factor responsible for the potent carrier and rise in drug-resistant pathogens among admitted patients in a healthcare facility. Therefore, our study recommends the utilization of recent surveillance data and guidelines to optimize treatment outcomes and minimize antimicrobial resistance in healthcare settings.
Conclusion
Footnotes
Acknowledgements
The authors would like to acknowledge all the staffs and clinicians of Koshi hospital for cooperating, assisting for taking history and providing clinical reports and information.
Author contribution
The authors confirm their contribution to the paper as follows: study conception and design: BS, PD, SKM; Data collection: BS, CS, UM; analysis and interpretation of results: PD; Literature review and initial draft: BS, PD, SKM. Critical revision of the manuscript for intellectual content: PD, CS, DPA. All authors reviewed and approved the final version of the manuscript.
Declaration of conflicting interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethics approval
Ethical approval for this study was obtained from Institutional Review Committee (IRC) of Purbanchal University College of Medical and Allied Science (PUCMAS-IRC) (APPROVAL REF NO: IRC/014/2020).
Informed consent
Verbal informed consent was obtained from all subjects before the study.
Trial registration
Not applicable.
