Abstract
Human immunodeficiency virus (HIV) and tuberculosis (TB) co-infection in Nigeria are medical conditions of public health importance because they double the country’s and its citizens’ burden. Several management measures, including artificial intelligence (AI), are crucial for properly diagnosing and preventing these diseases. This study explores the role of AI in managing HIV and TB co-infection in Nigeria. A comprehensive literature search strategy was developed using the keywords “HIV,” “TB,” “co-infection,” “artificial intelligence,” and “Nigeria” across six electronic databases: PubMed, Google Scholar, Cochrane Library, Web of Science, ResearchGate, and African Journals Online. The review focused on articles published between January 2014 and December 2022 to capture recent advancements and trends in AI applications in managing HIV and TB co-infection. Approximately 23%–26% of people with HIV in Nigeria are infected with both TB and HIV. People living with HIV in Nigeria are 26 times more likely to develop TB due to their weakened immune systems. The Early Warning Outbreak Recognition Systems is an AI system used for TB detection that is in practice in Nigeria. However, findings showed that AI models, including deep learning, machine learning, Computer-aided detection, Fuzzy cognitive maps, and Logistic regressions, the Twin model could be helpful in the accurate management of HIV/TB co-infection in Nigeria compared to traditional models, for example, inaccurate classification of radiographs and detection of HIV drug resistance. Despite the importance of AI toward managing these diseases, Nigeria faces challenges, including the unavailability of skilled personnel and AI experts, and the poor quality of the IT infrastructure, which are barriers to integrating AI into healthcare in the country. Strategic collaboration between the Nigerian government, digital health agencies, and healthcare organizations is crucial to implementing AI effectively for the treatment of HIV and TB co-infection in Nigeria. By embracing AI, Nigeria can revolutionize its healthcare system, improve patient outcomes, and address public health challenges such as HIV and TB co-infection.
Plain language summary
• Nigeria has a significant load of HIV/TB co-infection, worsening public health challenges.
• Approximately 23% of people with HIV in Nigeria are infected with both TB and HIV.
• AI models, including deep learning (DL), machine learning (ML), Computer-aided detection (CAD), Fuzzy cognitive maps (FCMs), and Logistic regressions, are helpful in the accurate management of HIV/TB co-infection.
• By embracing AI, Nigeria can revolutionise its healthcare system, improve patient outcomes, and address public health challenges such as HIV and TB co-infection.
Introduction
Tuberculosis (TB), caused by
TB and HIV co-infection refers to the simultaneous presence of both pathogens in an individual. This dual burden presents complex challenges in terms of diagnosis, treatment, and overall disease management.
5
HIV-induced immunosuppression severely compromises the body’s ability to contain
Nigeria is undergoing a pivotal public health challenge due to the double burden of HIV and TB, which is reported as one of the highest coinfections globally. 1 HIV infections drastically weaken the immune system, making individuals more prone to TB, which is a leading cause of death among individuals living with HIV. 1 From 2021, the prevalence of TB among people living with HIV (PLHIV) in Nigeria has been estimated at approximately 25.8%. 8 The co-infection of HIV and TB enhances the challenges in the healthcare system of Nigeria, escalated by restricted healthcare resources, financial burden, advanced levels of poverty, and overpopulation, all of which promote TB transmission.9,10 The healthcare system has difficulty managing both conditions effectively, as it requires long-term treatments and continuous monitoring for potential drug interactions, especially with the growing incidence of drug-resistant TB. 11
Despite continuous efforts to improve healthcare, there are still some challenges in diagnosing and ensuring treatment. Standard diagnostic methods, such as sputum microscopy, often fall short for HIV-positive patients, who may have no symptoms. 12 Moreover, many healthcare facilities face a shortage of resources, obstructing timely diagnosis and proper treatment. Addressing these issues demands inventive solutions that can be useful for Nigeria’s current healthcare system and assist in delivering proficient care. 13
Artificial intelligence (AI) is transforming healthcare globally by helping with diagnostic clarity, predictive outcomes, and clinical management, especially in managing infectious diseases. 14 AI encompasses various technologies such as machine learning (ML), deep learning (DL), and natural language processing (NLP), which allow computers to analyze data, recognize patterns, and make informed predictions. 15 In the healthcare field, AI applications cover diagnostic imaging, patient monitoring, drug discovery, and personalized treatment plans. 15 AI introduces significant opportunities in infectious disease management, where rapid assessment and decision-making are vital.16,17 For HIV and TB co-infection, AI-assisted tools can elevate diagnostic accuracy, identify at-risk populations, and assist healthcare providers in formulating individualized treatment strategies. 16 By analyzing extensive clinical and sociodemographic data, AI can help in the early detection of TB in HIV-positive patient and suggest treatment outcomes based on their medical histories. Promoting AI’s capability in Nigeria to minimize dependence on specialized staff and expedite diagnostic processes could greatly improve healthcare delivery, particularly in resource-limited settings. 16
Despite the advancement of AI in disease management, developing countries, including Nigeria, are lagging in implementing this advancement in their healthcare system. Moreover, only a few AI experts are present in Nigeria, and there are limited studies on the importance of AI in managing HIV and TB co-infection in Nigeria. This present study tried to explore the role of AI in managing HIV and TB co-infection in Nigeria to give more insights for policy making. Key objectives of this study include investigating the current and potential uses of AI to enhance diagnostic accuracy and treatment options, assessing the incorporation of AI in Nigeria’s healthcare system for infectious disease management, and identifying challenges such as infrastructure barriers and ethical issues while offering strategies for effective AI implementation. Considering the urgent healthcare challenges in Nigeria, it is believed that AI could be a game-changer in effectively managing co-infection. By exploring how AI can improve diagnostic capabilities, treatment monitoring, and health outcomes, this study will highlight how Nigeria can improve AI technology to strengthen its response to the HIV/TB epidemic.
Methodology
Study design
This is a narrative review using the Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) 2020 guidelines. 18 See Figure 1.
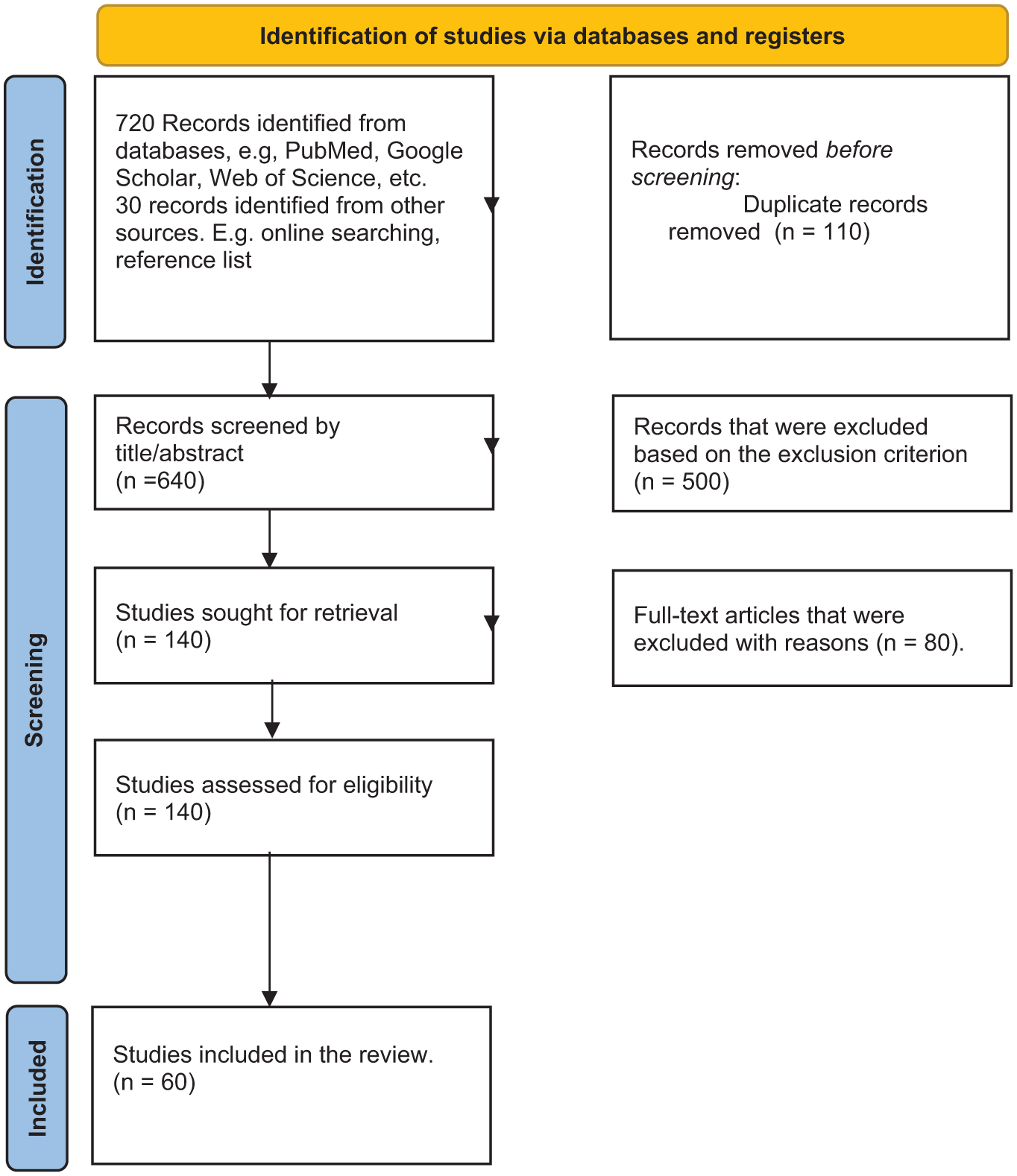
PRISMA flowchart.
Search strategy
A comprehensive literature search was conducted across six electronic databases: PubMed, Google Scholar, Cochrane Library, Web of Science, ResearchGate, and African Journals Online between January 2014 and December 2024 A comprehensive search strategy was developed using the keywords such as “HIV,” “TB,” “co-infection,” “artificial intelligence,” and “Nigeria.” and specific study’s objectives. All the articles were searched across the databases for relevance. For example, articles that discussed the “applications of AI in the management of TB and HIV co-infection” were only searched. Articles that did not discuss any of the study’s objectives were avoided.
Study selection
A total of 750 articles were identified from the selected databases and other sources, 640 articles were screened by title and abstract, 110 duplicates were removed, 500 records excluded (not relevant, wrong population/topic), 140 full-text articles assessed for eligibility, 80 articles were excluded with reasons: not meeting inclusion criteria, (
Inclusion criteria
This study included:
Only original research articles were selected, including cross-sectional studies, case series, systematic reviews and meta-analyses, cohort studies, and randomized controlled trials (RCTs).
Articles that focus on the application of AI in HIV and/or TB management in Nigeria or other African contexts with relevance to Nigeria.
Studies written in the English language.
Exclusion criteria
Excluded from this study were:
Studies not written in the English language. This is because of the difficulty in translation, which can create a bias, as some findings might be lost in translation.
Publications before 2014 were excluded to avoid outdated information.
Editorials, opinions, short communications, and conference abstracts without full abstracts.
Data extraction and analysis
Data extraction was conducted independently by two authors using a structured and standardized template. Extracted variables included the first author, year of publication, study design, examples of AI models applied in HIV/TB co-infection contexts, their potential applications, and reported challenges or barriers to implementation. Owing to considerable heterogeneity in study designs, AI applications, and outcome measures, a meta-analysis was not feasible. Consequently, a narrative synthesis was undertaken to systematically present and compare the key findings across the included studies.
Results
This study identified a total of 60 studies that investigated the role of AI in managing HIV and TB co-infection in Nigeria.11–73 A high burden of HIV/TB co-infection persists in Nigeria.20,21 Confirming TB in HIV-positive patients in Nigeria is challenging due to the limitations of diagnostic tools. Sputum smear microscopy, widely used in low-resource settings, has lower sensitivity in HIV-infected individuals, leading to prolonged and failed diagnoses. 22 These diagnostic challenges increase the risk of TB transmission and aggravate HIV/TB comanagement. The implementation of molecular diagnostic tools, such as GeneXpert MTB/RIF, has improved diagnostic rates, but access remains constrained to urban centers due to the high costs and operational challenges. 19 These limitations lead to delayed diagnosis and initiation of treatment, especially in remote areas where TB incidence is high. 22
Currently, the AI systems used for TB detection in practice in Nigeria are the Early Warning Outbreak Recognition Systems (EWORS). 41 EWORS efficiently identify, but are not limited to, hot spots of TB, help in selective screenings, and thereby efficiently strengthen healthcare surveillance. 41 In the rural areas of Nigeria, ML and DL models of AI analyze population movements, infection rates, and weather conditions, and then predict infection trends and detect hot spot regions of infections. 41
AI-powered tools such as computer-aided detection (CAD), ML, DL, fuzzy cognitive maps (FCMs), and logistic regressions (LR) are now being recognized as transformative solutions in enhancing the accuracy of co-infection screenings. Detection of infection through computer-based diagnostic tools can analyze clinical images with high accuracy, enabling the detection of subtle changes that otherwise escape identification. 31 FCMs can enable both experienced and novice physicians to screen coinfected patients through their ability to interpret complex data and find disease patterns from even uncertain data. 32
DL models utilize artificial neural networks (ANNs) to interpret medical images since most of the patients tend to have abnormal radiological images, and other data, and help in making an accurate diagnosis to improve TB detection in HIV patients, addressing the limitations of traditional methods. For example, the inaccurate classification of radiographs and the detection of HIV drug resistance, AI models such as the Twin model for finding active cases efficiently harness local data and predict disease incidence at the community level. Thus, AI can reduce the healthcare burden by allowing data-informed planning and decision-making. 41
Predictive models such as Gradient Boosting Machines (XGBoost), ANN, and Bayesian networks (BNs) are important tools used in addressing HIV drug resistance. Drug resistance can lead to treatment failure, increased healthcare costs, and poorer outcomes for patients. ML is highly effective in identifying genomic patterns of resistance, enabling earlier and more accurate predictions. 26 For instance, some ML models have been developed using viral genotype data, while others incorporate epidemiological and virological datasets to forecast resistance trends. AI is also transforming the detection of TB drug resistance. 26
AI’s applications extend to disease monitoring and outbreak prediction. AI platforms can analyze large epidemiological datasets, such as surveillance data, historical health records, and environmental factors, to predict disease outbreaks and track trends. For example, ML algorithms have been used to predict outbreaks of influenza and COVID-19, identifying potential hotspots and helping healthcare professionals plan effective responses. These models are context-specific, accounting for variables such as weather patterns, population density, and socioeconomic factors such as access to healthcare.28,29
More recently, new AI approaches have been tested for TB and HIV/TB management. A study used a Fuzzy Preference Ranking Organization METHod for Enrichment Evaluations (PROMETHEE) multicriteria decision approach to evaluate latent TB diagnostic tests and demonstrated its effectiveness in balancing accuracy, cost, and applicability in low-resource settings. 72 Similarly, a large-scale comparative analysis of the WHO’s global TB dataset applied multiple machine learning models to investigate TB incidence and HIV/TB co-infection patterns across different regions, including Africa. This study demonstrated that random forest (RF) and XGBoost models provided the highest predictive accuracy and robustness for large epidemiological datasets. 73
DL models, especially the bidirectional long-short term memory (LSTM) and the LSTM+ convolutional neural network (CNN), can detect the intricate patterns of the data of HIV and TB co-infection. 32 Thus, being better able to sort diverse data, AI can efficiently assist in mass screening programs, enabling early detection and promising better resources. 32 ML models, such as RF and support vector machine (SVM), and DL -based CNN models offer reliable personalized treatment planning and drug resistance monitoring in patients co-infected with HIV and TB. 35 An AI model based on a DL program can outperform all other conventional detectors when used for identifying resistant mycobacteria to all the currently first-line four anti-TB drugs, namely isoniazid, rifampicin, pyrazinamide, and ethambutol. 38
Discussion
HIV/TB co-infection in Nigeria
Nigeria has a significant load of HIV/TB co-infection, worsening public health challenges. A 2021 UNAIDS report predicts that around 23% of people with HIV in Nigeria are infected with both TB and HIV, escalating the risk of fatality due to the combined effect of both infections. 16 The high incidence is driven by the overlap of social and economic risks, such as poverty, congested living conditions, and inadequate healthcare access, which increases exposure to TB among HIV-positive individuals. 17 The risk of rapid TB progression in HIV-positive individuals places a major load on Nigeria’s healthcare system, where insufficient supplies often limit efficient integrated care. 19 Socioeconomic factors are important determinants of HIV/TB co-infection rates in Nigeria. Higher poverty and poor living conditions increase sensitivity to TB, which spreads through airborne droplets. 19 The healthcare infrastructure is particularly challenged in remote areas, where diagnostic facilities are often inaccessible or too costly for the underprivileged population. 20 These issues contribute to the spread and persistence of co-infection, as the healthcare accessibility gap and insufficient resources make early diagnosis and continuous treatment difficult. Patients in remote areas face high costs of transportation and prolonged wait times, making reliable healthcare less convenient.
The treatment of HIV/TB co-infection includes multifaceted dosing regimens with risks of adverse interactions between antiretroviral therapy (ART) and TB medications. Drug-resistant TB variants, including multidrug-resistant TB (MDR-TB), add to these challenges by requiring longer, more rigorous treatment, which can strain medical resources and be costly for patients. 20 Treatment adherence is critical to prevent drug resistance, yet tough to sustain due to adverse effects and the need for regular assessment, which is limited in many healthcare facilities. These factors lead to higher treatment rejection rates, especially in remote or under-resourced regions. 21 Nigeria’s National Tuberculosis and Leprosy Control Programme (NTBLCP) has executed strategies to deal with HIV/TB co-infection in line with global recommendations, highlighting the importance of early diagnosis and integrated treatment. The implementation of GeneXpert MTB/RIF at some HIV treatment centers has boosted TB detection rates, improving the ability to quickly identify and manage coinfected patients. 22 In addition, the NTBLCP encourages isoniazid protective therapy (IPT) for individuals who are positive for HIV without active TB, seeking to decrease TB occurrence in the susceptible group by preventing inactive TB from advancing to an active state. 10
Despite several advancements, many voids remain in Nigeria’s HIV/TB management approach. The validation and generalizability of AI models in Nigeria and other African settings remain major challenges, as highlighted in recent work on ML-based prediction of HIV treatment continuity, where authors note that generalizability may be limited due to differences in data quality and health system structures across settings. 74 Access to rapid diagnostic tools, such as GeneXpert, is restricted in rural regions where the load is often highest. The lack of trained healthcare professionals, poor infrastructure, and inconsistent drug supply further limit the efficacy of these strategies. Enlarging strategies such as IPT and improving adherence programs are essential, but are obstructed by financial limitations and operational issues. 17 There is a growing focus on digital health solutions, such as AI-assisted diagnostics, which may offer an affordable approach to improving TB diagnosis and assessing compliance, particularly in resource-limited settings. 17
Applications of AI in the management of TB and HIV co-infection
TB and HIV significantly impact each other, creating a complex health challenge. It was revealed that People living with HIV (PLWH) are 26 times more likely to develop TB due to their weakened immune systems. 23 Diagnosing TB in HIV patients is difficult, leading to TB being undetected in up to 46% of HIV patients at the time of death. 15 This highlights the need for innovative diagnostic solutions. One of the main challenges is the difficulty in obtaining sputum samples from HIV patients, a key diagnostic method for TB. 15 This has led to reliance on imaging techniques such as chest X-rays. However, interpreting X-rays can be challenging in individuals with advanced HIV.
AI-assisted tools have shown great promise in overcoming these barriers. For instance, a study in South Africa utilizes a TB diagnostic algorithm in chest X-rays to help clinicians detect TB in HIV patients. This AI-assisted technology had a mean accuracy of 0.79 (95% confidence interval [CI] 0.77-0.82), while physicians with experience in diagnosing TB in people living with HIV had a mean accuracy of 0.65 (95% CI: 0.60, 0.70) in the same cases. 24 In another study, DL techniques were utilized to classify radiographs that had TB, and they achieved 82.09% detection accuracy. 25 These advancements demonstrate the power AI has to revolutionize TB diagnostics, particularly for vulnerable populations.
A study developed a rapid method to detect gene mutations responsible for TB resistance, achieving highly precise accuracies ranging from 78% to 89%. 27 These predictive tools help clinicians design effective treatment regimens for patients with drug-resistant strains of TB and HIV, improving outcomes and reducing the risk of further resistance. 27 Predictive models can analyze genomic and epidemiological data to identify trends in drug resistance, enabling clinicians to adjust treatment plans proactively. In a study, researchers developed AI tools to detect mutations in TB gene sequences responsible for resistance, providing accurate and rapid results to inform treatment decisions. 26 These capabilities can be expanded to optimize treatment regimens for co-infected patients, taking into account the complexities of managing both TB and HIV simultaneously. 26
AI is increasingly being used to optimize treatment plans for HIV patients. Personalized treatment plans can account for individual factors such as drug resistance profiles, comorbidities, and lifestyle. 27 AI algorithms are adaptive and capable of tailoring recommendations to changes in a patient’s condition over time. For example, one study used patients’ medication adherence data and treatment plans to develop personalized reminders for patients, which improved patient outcomes and adherence rates. 28 Another study used genetic and clinical data from patients to identify genetic markers related to treatment response, which was used to develop optimized treatment plans for each individual. 28 These advances show how ML can enhance patient care by analyzing large datasets to uncover correlations that might otherwise be missed through traditional analysis. 28 This adaptability makes AI an invaluable tool for managing public health crises and guiding resource allocation.
In addressing TB/HIV co-infection in Nigeria, AI has shown promise in forecasting epidemic trends and informing public health policy. A study focused on developing prediction models for TB/HIV co-infection successfully used both past and present cases to predict future cases, providing valuable insights for policymakers.14,23 These models are used to allocate resources effectively, design intervention strategies, and plan public health campaigns. By utilizing AI’s predictive capabilities, healthcare systems can better address the complex epidemics of TB and HIV, thereby improving patient outcomes and reducing disease burdens. 23 Figure 2. A visualization workflow showing the management of HIV/TB using an AI algorithm.

A visualization workflow showing the management of HIV/TB using an AI algorithm.
AI’s utility is not limited to individual patients but extends to larger public health challenges. Its ability to process large datasets quickly and accurately makes it essential for identifying patterns and trends that inform healthcare strategies. For example, AI can help predict potential hotspots for TB or HIV outbreaks, ensuring that diagnostic tools and resources are deployed where they are most needed. 29 This capability is especially valuable in regions with limited access to healthcare, where targeted interventions can make a significant impact. AI and ML are improving the fight against TB and HIV co-infection. By improving diagnostic accuracy, optimizing treatment plans, predicting outbreaks, and addressing drug resistance, these technologies have the potential to offer solutions to some of the most pressing challenges in managing these epidemics in Nigeria.
Potentials of AI for HIV and TB co-infection management in Nigeria
Several studies have reported that diagnostics based on AI tools have dramatically improved the battle against the burden of HIV and TB co-infection.29,33,34,37,40,41,54 In low-resource settings such as Nigeria, with fewer laboratory facilities, a shortage of expertise, and high disease burdens, AI-based diagnostics can provide a central contribution. For example, AI-powered operators are better able to store large and diverse data, better able to detect intricate patterns, and are more accurate in making diagnoses. 33 When AI operators were compared with radiologists, AI proved itself to be a high-performance detector, giving results of as high as 85% and when radiologists used AI as a helping hand, their work accuracy improved by 11%. 33 AI proved its transformative role in healthcare in low-resource settings by increasing efficiency and decreasing cost. It processed real-time data, scheduled appointments, tracked medical records, analyzed radiological data, optimized clinical decisions, bridged diagnostic gaps, and even made predictions about disease burdens when it was used in Africa. 34
ML models, such as RF and SVM, and DL-based CNN models accurately and timely identify the specific mutations associated with the development of drug resistance, thus enabling timely and targeted therapy adjustments.
35
RF and SVM models have been found to possess high accuracy in predicting resistance to first-line anti-TB drugs based on
AI helps in identifying pathways, either genetic or molecular, involved in HIV and TB co-infection, their interplay, and their subsequent impact on developing resistance to therapeutic modalities, thereby providing the basis for developing effective drugs and managing drug resistance. 36 MLA, by analyzing gene expressions and genetic variations, predict the pathogenic mutations, emerging gene-disease links, and patient outcomes, and make personalized treatment strategies more effective. 38 By using imaging data and genetics, AI has promising potential in recognizing drug-resistant mycobacterial strains. DL can differentiate drug-sensitive strains from drug-resistant ones. Models of DL, such as SVM and CNNs, have 91.1% accuracy for analyzing CT-based images to find resistant strains. Similarly, DL models such as deep learning–based models for Antimicrobial Resistance prediction (DeepAMR) and Heterogeneous Graph Attention Network for Antimicrobial Resistance prediction (HGAT-AMR) can identify resistant bacteria with 94%–99% accuracy. While these models detect resistance to first-line drugs, other models, such as wide and deep neural networks, aka WDNNs, can detect mycobacteria with resistance to multiple drugs or MDR-TB that show resistance to even the second-line drugs; streptomycin, etc. 39 These models also help in the optimization of treatment and management of drug resistance in HIV and TB coinfected patients and significantly reduce hospital morbidity and mortality. 40
This study found that predictive modeling, for example, ANN, and BN have been proven to forecast treatment outcomes and disease progression, with models demonstrating strong performance in TB–HIV settings. 54 In Nigeria, where more than 40% of TB cases remain undetected, delayed diagnosis continues to hinder effective disease control and treatment outcomes. AI can effectively help in case findings and predicting infection trends. 41 AI-driven models use community data in active case finding (ACF), and this is of particular importance in overpopulated areas where the chances of getting overlooked and undetected by traditional methods remain high. By leveraging local data, AI models can predict new ACF areas and also the locations of undetected cases. 41 ML and DL models aid in the allocation of resources and the better maintenance of healthcare surveillance. 29 AI’s vast capabilities make it efficient in inspecting, monitoring, and inferring large databases that include environmental data, health data, patterns of mobility, and trends of various infections. 29 AI aids in developing early warning systems and alerting healthcare systems for timely interventions. AI analytics thus make it possible to improve the effectiveness of public health strategies by giving comprehensive yet accurate guidelines on real-time public health interventions, including vaccination campaigns and disease-specific advisories. 29
Public health strategies in Nigeria that are informed by AI analytics can significantly improve public health interventions and patient outcomes. Applications of AI, such as predictive modeling of disease outbreaks that include Explainable AI, make transparent predictions, support transparent decision-making systems, resource allocations, and optimize health system responses. 43 AI can help in the personalization of public health strategies that are of central importance in Nigeria, which has having high disease burden in the face of healthcare disparities. 44 In low-resource regions such as Nigeria, where TB is continuously on the rise, more so in combination with HIV, AI can significantly enhance healthcare access.
This study also found that AI has the potential to decrease healthcare disparities. It can accurately identify the ailments that affect certain ethnic and racial groups differently from others, and thus can efficiently make accurate diagnoses by considering social determinants of health. For example, a study by O’Connor showed that DL models, when used for the identification of Knee arthritis in black patients, showed that only pain made 40% disparities. 46 Similarly, another study showed that by using robust systems of data collection and data analysis, AI can reduce the disparities in the healthcare system by identifying the disparities in the health system’s quality, access, and outcomes among various groups, including geographic location, socioeconomic status, gender, race, and ethnicity. 47 Table 1 summarizes the AI applications for HIV/TB management with their accuracy, cost, and scalability.
Comparative analysis of AI algorithms in HIV/TB management.

AI, artificial intelligence; ANN, artificial neural network; ART, antiretroviral therapy; CNN, convolutional neural network; HIV, human immunodeficiency virus; MDR-TB, multidrug-resistant TB; ML, machine learning; PLWH, people living with HIV; RF, random forest; SVM, support vector machine; TB, tuberculosis.
Multisectoral challenges and barriers to implementing AI in Nigeria
The integration of AI into Nigeria’s healthcare system, especially for managing HIV and TB, is hindered by multifaceted challenges that remain insufficiently explored. A major concern is the ethical dilemma surrounding the use of nontransparent, or “black box,” AI models. While global discourse increasingly emphasizes the need for explainability and accountability in AI systems, these issues are further intensified in Nigeria due to limited digital literacy among healthcare professionals and widespread public skepticism toward automated decision-making processes. 59 The unavailability of skilled personnel, AI experts, and the poor quality of the IT infrastructure are barriers to the integration of AI into healthcare in Nigeria. 48 A multidisciplinary team involving clinical scientists, data scientists, and subject matter experts with AI skills, innovation managers, and AI experts to provide training and the resources to facilitate the training is an important element in the adoption of AI into clinical practice. There are few healthcare professionals in the world, including Nigeria, with the talent for both medical and technology knowledge, and who are open to understanding how the two domains meet the patients’ needs. 49
In addition to infrastructure and financial constraints, local implementation barriers extend to socio-cultural resistance, which is often overlooked. A novel insight from this study is the mistrust toward AI-based diagnostics in certain Nigerian communities, where health technologies are sometimes viewed with skepticism, particularly when they circumvent traditional, human-mediated care. This highlights the critical need for community engagement, education, and the participatory design of AI tools to ensure cultural acceptance and trust in their use. 59
Ethical AI is a serious issue in all industries, especially healthcare, where AI has been slow to develop. 60 Consequently, ethical considerations like human autonomy, ensuring transparency, explainability, and intelligibility, and fostering responsibility and accountability will have to be forfeited as this will not be easy or achievable by most AI systems; for example, some learning models, such as CNNs for radiological image analysis, are neither transparent nor explainable. 60 This can become a sensitive issue in the diagnosis and management of HIV and TB co-infection in Nigeria. 48
Ethical AI deployment requires the integration of fairness, accountability, and transparency into system design. 60 In the Nigerian context, where healthcare disparities are shaped by socioeconomic, ethnic, and geographic factors, AI models must be rigorously evaluated for bias. 71 For example, algorithms trained on data from urban populations may underperform in rural settings, potentially reinforcing existing inequities in care delivery. To mitigate such risks, continuous model evaluation, community-informed development, and robust oversight mechanisms are essential to ensure explainability and prevent algorithmic discrimination. 71
Integration of AI into the healthcare industry in Nigeria has also been limited by the fact that AI is not a single technology but several, encompassing diverse capabilities and applications. 50 Healthcare is unique in comparison with other industries, whereby it relies on public scientific methods to introduce new products and practices, for example, the FDA. Studies have to be conducted on AI and results published and accepted to allow its integration into clinical practice. 48 The financial burden of adopting AI in healthcare extends beyond the initial cost of procuring tools. It encompasses less visible but critical expenses such as data storage compliance, cybersecurity infrastructure, and the training of personnel capable of bridging medical and AI expertise. 49
This study underscores that even pilot implementations often struggle to scale, as healthcare institutions are compelled to prioritize immediate clinical service delivery over long-term digital investments. Moreover, in the absence of a clear return-on-investment framework for AI in public health, funding bodies remain hesitant to support large-scale adoption. 49 AI integration into the healthcare system requires approval from regulatory bodies such as the National Information Technology Development Agency (NITDA), whereby some factors are put into consideration, for example, model risk management, data governance, customer privacy, and supervisory control systems. 51
Healthcare facilities hoping to introduce AI-based applications into their systems should have frameworks designed to address the challenges that the AI model might pose to data integrity and patient privacy. 51 Healthcare facilities ought to have large amounts of data to train and retrain AI models to conduct comprehensive analyses, identify patterns, and make predictions regarding HIV and TB management. 52 AI applications used in healthcare may involve the collection, analysis, and sharing of sensitive patient data, as well as ongoing monitoring of patient response to the different treatment regimens, for example, the use of personally identifiable information and biometrics. 52 This could cause the Nigerian government to be skeptical about integrating it into the management of HIV and TB co-infection, which is sensitive information. Committees in Nigeria that will control these AI-based tools and systems also need to be put in place, and set protocols and procedures by which they will operate. This would require training of these individuals, which the government does not have. 53
Moreover, Nigerian Healthcare facilities cannot afford to pay for AI innovation in healthcare because some AI innovations are very expensive, and healthcare providers in Nigeria have to worry about offering the best care at the same cost and quality of care. 54 As healthcare transitions to value-based payment models, healthcare providers are going to be required to reimburse for AI-based innovations, which are quite expensive. In a few cases where AI innovations have been introduced, they are experimental and therefore bring little return on the investment.48,58
Future directions and recommendations
AI in healthcare encompasses the use of ML algorithms and cognitive technology within medical settings, representing the convergence of humans and ML. 55 It also holds immense public health benefits such as drug and vaccine development, disease surveillance, outbreak response, and health systems management. 56 Studies have highlighted different health applications of AI in low and middle-income countries.57,58 Examples of these are the use of NLP models in epidemiological surveillance and disease prediction, as well as the combination of natural language processing models with expert systems to aid physicians in medical diagnosis. 57 In high-income countries, there has been an integration of AI into their healthcare ecosystems, which has brought about great benefits.
An analysis found that the use of AI applications could save approximately $150 billion on healthcare costs annually by 2026 in the USA. 56 Liang et al. 58 examined the “evaluation and accurate diagnoses of pediatric diseases using AI” at the Guangzhou Women and Children’s Medical Center, which serves as a referral center in Guangdong Province, China. 58 The test applied AI-based technologies with DL techniques using 101 million data points from electronic records of 1.3 million outpatient visits to the medical center. 59
The findings of a study among healthcare workers in Nigeria in 2023 revealed that a significant proportion of the study population had good knowledge of AI, and more than 50% of the respondents believed that AI would complement human efforts rather than replace them. 61 They were also of the opinion that AI could revolutionize healthcare. 61 The study also concluded that Nigerian health professionals exhibited a high level of readiness and enthusiasm for the adoption and implementation of AI innovations. 59 There have been recent trends in African healthcare and AI technologies. This includes advancements in the rapid HIV testing in South Africa, which uses DL algorithms that have been utilized in rural South Africa. 61 Another advancement is the use of AI for diagnosing diabetic retinopathy in Zambia. This yielded significantly accurate results when compared to human assessment. 62
There are challenges in the aspect of handling patient information, highlighting the need for robust data protection measures. These challenges are hindering the utilization of digital health to combat Africa’s health issues. 63 Moreover, there is a lack of clear policies for the development of e-health platforms in African countries, including Nigeria. This serves as a significant barrier to the adoption of digital health solutions. 64 There should be strategies aimed at solving infrastructure and technology challenges in Africa. In Nigeria, this will require a great investment in ICT infrastructure and digital skills training for healthcare professionals. There should also be the development of policies and frameworks to enhance the integration of AI-based technologies into health systems. 65 López et al. 66 emphasized the need for AI models to be trained under a comprehensive legal and regulatory framework to ensure they meet the public health system requirements of low and middle-income countries (LMICs). 66
Luo et al. 67 further underscored the need to use secondary health data to overcome barriers to data availability. This could unravel new insights and advancements in medicine. Ibeneme et al. 68 also highlighted the need for the government and all stakeholders to hold meetings to integrate AI and digital health into the healthcare sector in Africa. 68 This recommendation can be utilized by the Nigerian health authorities. There are examples of notable partnerships and initiatives for the adoption of AI in healthcare in Nigeria. These include the collaboration between the African Centre for Economic Transformation (ACET) and the Convergence AI partnership in Accra. The main aim of the collaboration between them is to improve AI research, enhance collaboration, share practices and knowledge, create impact-driven solutions, and improve the advocacy for responsible AI use in Africa. 69 The expertise of both organizations can be utilized to revolutionize innovation and address key challenges confronting Africa. 69 The Nigerian government should therefore facilitate a strong collaboration with ACET and convergence AI in Ghana to improve the AI surveillance system in Nigeria. Another notable collaboration is between LifeBank and Bensh AI. This seeks to use AI to improve patient outcomes in hospitals in Africa. 70 By effectively utilizing the power of AI, the partnership seeks to enhance patient care and streamline hospital operations. 70 The results of a cross-sectional study among healthcare workers in Nigeria in 2023 showed that, despite agreeing that AI would play an integral role in future healthcare, two-thirds of the respondents were of the view that the integration of artificial intelligence in healthcare can raise new ethical challenges. 59 A significant step in the aspect of ethical issues is the European Parliament’s report with recommendations to the Commission on the Civil Law Rules on Robotics. 61
In brief, the rapid advancement of AI in the clinical and biomedical fields is considered a great approach in many communities that may augment professionals in the healthcare system. 61 There is an urgency for the Nigerian health authorities and stakeholders to create more awareness of the importance of AI toward the management of HIV and TB. This awareness can be achieved through webinars, seminars, and social media platforms, including Facebook and Twitter.
Study limitations
Though AI has tremendous potential in the treatment of HIV and TB co-infection, the present review indicates some limitations that could influence its real-world application in Nigeria. Most of the studies reviewed covered high-income countries with well-developed digital infrastructure and, therefore, are limited in their applicability to low-resource countries like Nigeria.15,23,31,57,54 Most of the AI models reported high accuracy based on well-annotated datasets; however, few studies reported validation in African or sub-Saharan settings.33,41,63
Another limitation of this study is that most reports were not well detailed in reporting study design, sample size, and external validation, which complicated an evaluation of their reproducibility and robustness.23,27,35 Interpretability, in turn, which is a crucial aspect for clinical decision-making, was considered in a few studies.43,57 Ethical issues, data protection, and implementation obstacles were not discussed frequently enough despite their high relevance in Nigerian healthcare systems.46,47,61,63 Cost-effectiveness and workforce preparedness were not taken into account at all, although these are decisive in ensuring long-term integration of AI.34,48,49
Again, only a few models were dedicated to the HIV/TB co-infected group, further restricting their applicability to Nigeria’s epidemiologic context.24,54 Moreover, evidence on the deployment of these resources in weak infrastructure-decentralized care settings was extremely sparse. These results underscore the need for locally relevant, context-specific research that proves AI tools in Nigerian clinical environments. Subsequent studies, for example, epidemiological studies, case reports, must tackle obstacles to deployment and include clinicians, patients, and decision makers to guarantee that AI solutions are not just technologically viable but also ethically sound, affordable, and scalable within Nigeria’s healthcare landscape.55,59,65
Conclusion
This study provides a Nigeria-specific perspective on the transformative potential of AI in managing HIV and TB co-infection. Unlike broader global analyses, it contextualizes AI applications within Nigeria’s unique sociopolitical and infrastructural landscape. The study emphasizes the relevance of AI tools, particularly ML, for diagnostic imaging, genomic resistance prediction, and personalized therapy planning in addressing challenges within the country’s constrained healthcare system. AI technologies offer promising improvements in the detection of TB in HIV-positive individuals, prediction of disease trends, drug resistance analysis, and the development of tailored treatment strategies. Moreover, AI can enhance surveillance by integrating diverse data sources, including clinical, environmental, and socioeconomic indicators.
To harness AI’s full potential, the Nigerian government must prioritize investments in healthcare and ICT infrastructure, support digital skills training for healthcare professionals, and establish ethical frameworks for AI use, in collaboration with agencies such as NITDA. Strategic partnerships between government, health institutions, and digital health stakeholders are essential for successful implementation. By adopting AI, Nigeria can significantly strengthen its healthcare system and improve outcomes for individuals affected by HIV and TB co-infection.
Footnotes
Acknowledgements
None.
Declarations
Transparency statement
All the authors have approved the submitted version and have agreed both to be personally accountable for their contributions and to ensure that questions related to the accuracy or integrity of any part of the work, even ones in which they are not personally involved, are appropriately investigated, resolved, and the resolution documented in the literature.
Provenance and peer review
Not commissioned, externally peer-reviewed.
Declaration of generative AI and AI-assisted technologies in the writing process
There is nothing to disclose.
