Abstract
Primary tracheal synovial sarcoma is a rare malignancy and is usually found incidentally. Tumours can present with cough, dyspnoea, stridor and intermittent haemoptysis. The diagnosis is challenging because it is rare, and the symptoms may mimic other diseases of airway obstruction. A previously well 53-year-old man presented with an eight-month history of cough. He had a history of minimal haemoptysis a few months prior to presentation. Spirometry showed an obstructive pattern, and a computed tomography scan of the thorax revealed an intraluminal tracheal mass. This case highlights that a thorough initial evaluation, including spirometry, leads to an earlier diagnosis and successful treatment of this rare sarcoma.
Introduction
Primary tracheal synovial sarcomas (SS) are rare. The symptoms are non-specific and often related to the tracheal pathology. We report a 53-year-old man with primary tracheal sarcoma who presented with a chronic cough and minimal haemoptysis. Chest radiograph was normal. Spirometry showed an obstructive pattern, and a computed tomography (CT) scan of the thorax revealed an intraluminal pedunculated mass in the trachea. Biopsy of the tracheal lesion confirmed the diagnosis, and the patient was treated successfully with radiotherapy.
Case report
A 53-year-old man, a social smoker, presented with a chronic cough. He had an episode of minimal haemoptysis a few months prior to presentation. He had an eight-month history of intermittent cough, which he attributed to a prior chest infection. There were no constitutional symptoms. He had no significant past medical history, in particular no history of pulmonary tuberculosis or exposure to tuberculosis.
Clinical examination, blood investigations and chest radiograph were unremarkable. Spirometry revealed reduction of airflow during forced expiration consistent with an intra-thoracic obstruction.
He underwent a CT scan of the thorax which showed a mass in the trachea (Figure 1(a) and (b)). Bronchoscopy revealed a pedunculated mass, which was highly vascular in the trachea. There were no abnormalities distal to the mass.
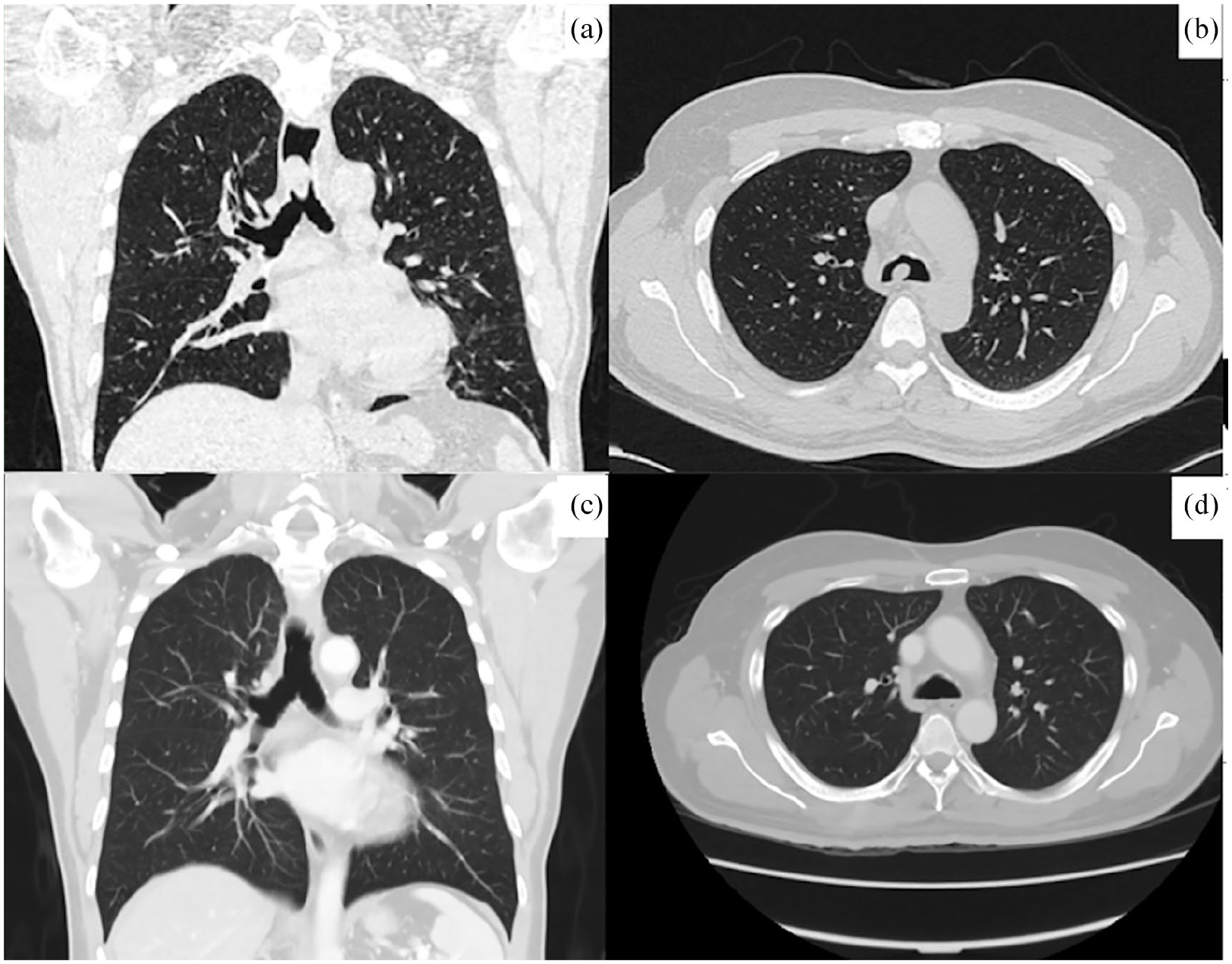
Computed tomography (CT) imaging: (a) coronal view and (b) axial view demonstrating the pedunculated mass in the distal trachea, and (c) and (d) post radiotherapy.
He underwent a biopsy of the mass via rigid bronchoscopy, and the histopathological examination (HPE) was suggestive of synovial sarcoma (Figure 2). The patient subsequently underwent eight weeks of radiotherapy without adjuvant chemotherapy. Repeat bronchoscopy and CT of the thorax showed complete resolution of the tumour (Figure 1(c) and (d)). Repeated spirometry showed improvement in the level of airway obstruction (Figure 3). The patient underwent yearly CT scans of the thorax for three years with no evidence of recurrence. He remains well five years after treatment.

Histopathology of the mass showing ovoid to rounded darkly stained nuclei of malignant cells (a). It stained diffusely positive for vimentin (b) and bcl2 (c) and focal positive for CKAE1/AE2, EMA, CD56, synaptophysin and S-100 (d).

Spirometry pretreatment (a) and post treatment (b) shows improvement in the expiratory flow loop.
Discussion
Synovial sarcomas are classified according to the prominent cell type. They can be either epithelioid or spindled, and are further divided into four histological types: biphasic, monophasic fibrous, monophasic epithelial and poorly differentiated. 1 Synovial sarcoma stains positive for cytokeratin, EMA, bcl-2 and vimentin, and negative for S-100, desmin, smooth-muscle actin and vascular tumour markers. 2 They are chemo-sensitive to ifosfamide and doxorubicin, with an overall response rate of approximately 24%. 3
Factors predicting poor prognosis for primary pulmonary sarcoma include tumour size (>5 cm), male sex, older age (>20 years), extensive tumour necrosis, high grade, large number of mitotic figures (>10 per 10 high-powered fields), neurovascular invasion and the SYT-SSX1 variant. 2 Not all synovial sarcomas behave as high-grade tumours. A study on 121 patients with synovial sarcomas attempted to identify both low and high-risk groups. They found the high-risk groups to be those aged ⩾25 years, a tumour size >5 cm and a poorly differentiated tumour. 4
Primary tracheal sarcomas are rare. Due to the presence of mixed histology and a lack of published data on the survival of these patients, there are no clear guidelines for the diagnosis, management and staging of the disease. Patients present with symptoms as a result of the tracheal pathology. Our patient presented with chronic cough and haemoptysis. Spirometry confirmed an intra-thoracic obstruction which prompted us to perform a CT scan of the thorax which confirmed the tracheal lesion. The diagnosis was confirmed by a biopsy of the tracheal lesion via bronchoscopy.
The treatment regime varies according to each case and is based on expert opinion. The optimal treatment appears to be complete resection of the tumour, with negative margins where possible. There are no reported data to support the routine use of adjuvant chemotherapy. Radiation therapy, however, has been shown to improve local control of head and neck synovial sarcomas. 5 In our case, the HPE did not show features of poorly differentiated SS. We discussed treatment options with our patient, and he chose the non-surgical option.
This case highlights the usefulness of spirometry in detecting an intra/extra-thoracic obstruction in a patient with mild symptoms. This report adds to the current literature on the successful treatment of a rare primary tracheal synovial sarcoma.
Footnotes
Acknowledgements
The authors would like to thank all medical personnels for their involvement in the management of this patient.
Authors’ contributions
All authors were involved in literature review, data collection, data analysis and paper write-up.
Availability of data and materials
The datasheets generated and analysed during the study are available.
Ethical approval
Universiti Kebangsaan Malaysia Medical Centre does not require ethical approval for reporting cases or case series.
Informed consent
Written informed consent was obtained from the patient.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
