Abstract
Primary anaplastic large cell lymphoma of the trachea is a very rare tumor. Diagnosis is often missed for a long time because the presentation often resembles that of obstructive airway disease. A 24-year-old non-smoker male presented at an outpatient clinic complaining of gradual development of stridor and shortness of breath over a recent period of four weeks. Imaging workup revealed a large lobulated, soft tissue, mildly enhancing, eccentrically placed intraluminal proximal tracheal mass, which showed extension outside of the tracheal lumen in the peritracheal fat. The patient underwent surgery. A biopsy of the resected mass reported anaplastic large cell lymphoma. Post-operation, the patient underwent chemotherapy consisting of four cycles of CHOP (cyclophosphamide, doxorubicin, vincristine and prednisolone). Follow-up imaging showed non-visualization of the mass. Primary lymphoma (anaplastic large cell lymphoma, which is a rare type of non-Hodgkin’s lymphoma) of the trachea is a rare tumor. Early curative resection with post-operative chemotherapy has a favorable outcome, as in our case.
Introduction
Primary neoplasms of the trachea are quite rare, accounting for 2% of all respiratory tract tumors and 0.1%–0.4% of all malignancies. The most common primary tumors of the trachea are squamous cell carcinoma and adenoid cystic carcinoma. Primary tracheal non-Hodgkin’s lymphoma (NHL) accounts for only 0.2%–3% of all tracheal tumors. Anaplastic large cell lymphoma represents 2% of NHLs.1-3 Tracheal tumors may be silent for a long time, until the tumor occludes 50%–75% of the luminal diameter. The tumors may mimic other conditions such as asthma or chronic obstructive pulmonary disease, making early diagnosis a challenge. The symptoms at presentation usually relate to airway obstruction, that is, cough, hoarseness, hemoptysis, shortness of breath and stridor.4,5 We present a case of primary tracheal anaplastic large cell lymphoma in a young male, who underwent an excisional biopsy and chemotherapy resulting in complete remission of the disease. The rationale behind this case is always to think beyond obstructive airway disease if a young non-smoker patient presents with signs of airway obstruction.
Case presentation
The case was a 24-year-old male who presented at an outpatient clinic complaining of gradual development of stridor and shortness of breath over a recent period of four weeks. He had no other comorbid conditions and his past history was also insignificant for any other medical issues. There was no history of cigarette smoking. In a general physical examination, he was fully alert with good body habitus. He was having visible respiratory distress with an audible expiratory wheeze. On chest auscultation, both lungs revealed comparable air entry. Initial baseline workup showed the following: hemoglobin (10.7 g/dl), white blood cell count (8.8 x 109), platelets (272 x109/L), creatinine (1.0 mg/dl), total bilirubin (0.6 mg/dl), SGPT (12 U/L), SGOT (26 U/L). The patient then underwent contrast enhanced computerized tomography (CT) of the neck and chest region. This showed a large lobulated, soft tissue, mildly enhancing, eccentrically placed intraluminal proximal tracheal mass, which showed extension outside of the tracheal lumen in the peritracheal fat. The mass was abutting the lower pole of the right lobe of the thyroid gland (Figure 1). There was greater than 50% occlusion of the tracheal lumen at this level. The mass was showing homogenous enhancement without any internal areas of necrosis or calcifications. No mediastinal or hilar lymphadenopathy was seen. On the basis of the above findings, a differential diagnosis of adenoid cystic carcinoma, lymphoma or a germ cell tracheal tumor was made, given the patient’s young age. His further lab workup was done for a germ cell tumor, and revealed that his beta-human chorionic gonadotrophin (B-HCG) and alpha-fetoprotein (AFP) were within normal limits (0.88 IU/mL and <0.100 mIU/mL, respectively). His lactate dehydrogenase (LDH) level was borderline elevated at 550 IU/L. It was planned that the patient would undergo an open thoracotomy with resection of the lesion. Intraoperatively, a large mass, which was lobulated in appearance, was seen in the trachea causing luminal narrowing, and it was completely resected. Intraoperative frozen sections and a follow-up full-specimen biopsy revealed anaplastic large cell lymphoma (Figure 2). The patient then underwent a bone marrow biopsy, which proved negative, to exclude lymphomatous involvement.

CT chest showing a large lobulated, soft tissue, mildly enhancing, eccentrically placed intraluminal proximal tracheal mass, which showed extension outside of the tracheal lumen in the peritracheal fat.
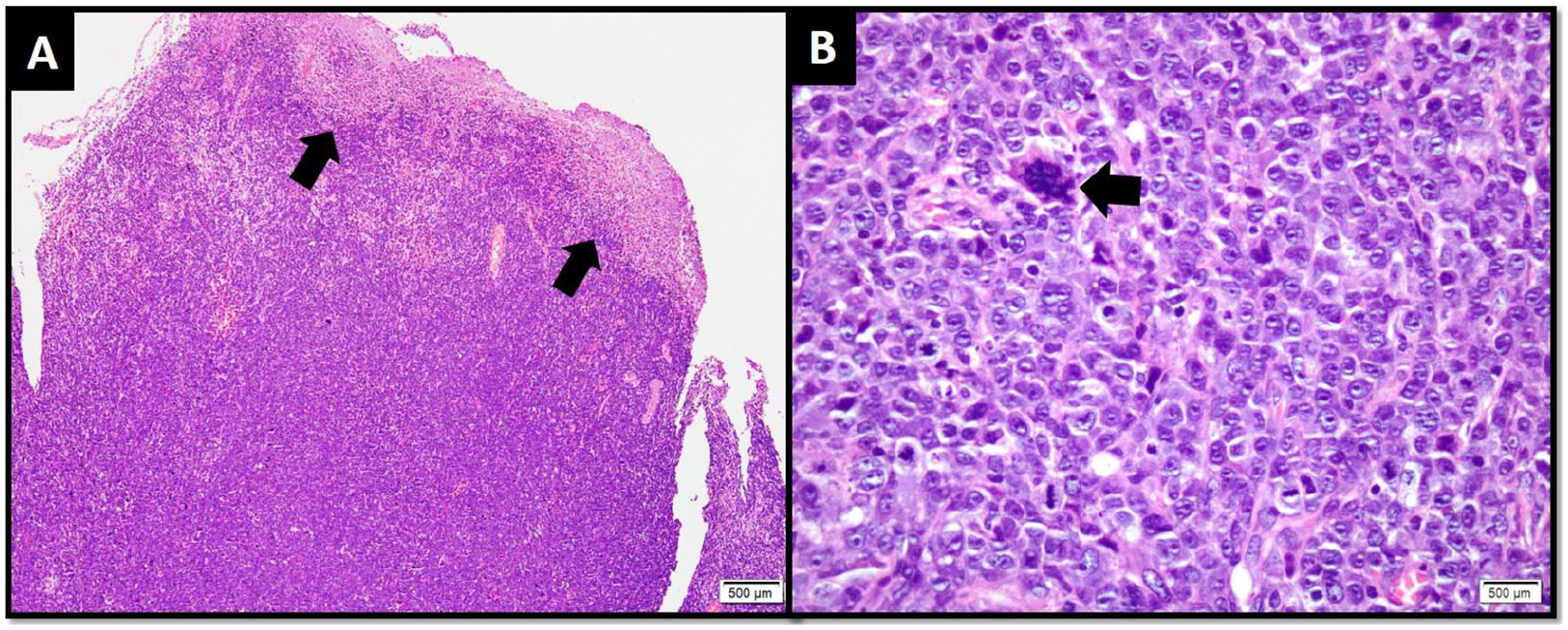
Microscopic examination of the tissue from the tracheal lesion revealed a neoplastic lesion arranged in diffuse sheets of large-sized neoplastic cells. These neoplastic cells demonstrated positive expression for CD45, CD3, CD43, CD30, epithelial membrane antigen and ALK protein immunohistochemical stains. The Ki-67 (Mib-1) index was high. CD20, CD79a, CD15 and cytokeratin AE1/AE3 immunohistochemical stains were negative. Hence, the diagnosis of anaplastic large cell lymphoma, ALK positive, was made.
The patient then underwent chemotherapy consisting of four cycles of CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisone). A follow-up CT evaluation after one month showed non-visualization of the tracheal mass (Figure 3). Mesenteric nodes had also resolved completely in the follow-up evaluation. The patient’s LDH level in the follow-up evaluation was normal as well (324 IU/L). He then underwent follow-up CT at three-month interval and serial LDH levels at regular intervals. The latter also stayed within normal limits.

Status post-surgery and post-chemotherapy. Follow-up CT one month after completion of chemotherapy showed non-visualization of the tracheal mass with visualization of surgical clips in the pretracheal location.
Discussion
The median age of patients with primary tracheal lymphoma is 44 years, with a range of 4–81 years. 6 The symptoms at presentation usually relate to airway obstruction, that is, cough, hoarseness, hemoptysis, shortness of breath and stridor. In a study documenting clinical presentation in 329 patients who had primary tracheal malignancies, difficulty in breathing was the most frequent symptom (71%) followed by cough (40%), hemoptysis (34%), asthma (19.5%) and stridor (17.5%). Hemoptysis is less commonly observed in tracheal lymphomas, the reason being that they predominantly involve the submucosa. 7 They may involve the adjacent structures in advanced stages, causing hoarseness or dysphagia.3,6,7 The young patient in our case presented with difficulty in breathing and stridor.
Diagnostic workup may include either bronchoscopy or radiologic imaging or both. CT is the imaging method of choice. Conventional chest radiographs are of less diagnostic yield in tracheal diseases, as evidenced by the fact that more than half of the tumors are missed on radiographs. Tracheal evaluation can be performed both by conventional CT as well as spiral CT. Spiral CT is superior to conventional CT, because it may allow for the differentiation of mucosal from submucosal masses as well as an assessment of the extent of the tumor and its relationship to adjacent structures.3,6,7 Another advantage of CT is that it allows visualization of concurrent hilar or mediastinal lymph nodes, although none were seen on chest sections in our case. Bronchoscopy has one advantage over CT in that it allows direct visualization of the lesion.
Treatment of tracheal neoplasms may require chemotherapy, radiotherapy or surgery on their own, or any combination of these. NHLs have been reported as highly radiosensitive. Radiotherapy on its own is a standard treatment for stage I to II gastric and non-gastric MALT lymphomas.3,6,7 The surgical option was chosen in our case followed by chemotherapy, resulting in complete resolution of the disease. Prognosis largely depends on the histologic grading, as in all NHLs.
Conclusion
Primary lymphoma (anaplastic large cell lymphoma, which is a rare type of NHL) of the trachea is a rare tumor. Early curative resection with post-operative chemotherapy has a favorable outcome, as in our case.
Footnotes
Acknowledgements
None.
Authors’ contributions
JS: conception, data acquisition and writing up. FK: conception, writing up and critical review. MT: writing up and data acquisition. FJ: language editing and critical review. WA: language editing and critical review. All authors approved the final version.
Availability of data and materials
Available on request from the corresponding author.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethics Review Committee, Aga Khan University.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for his anonymized information to be published in this article.
Trial registration
N/A.
