Abstract
The present study was conducted to determine the effect of corynoline (COR) against sepsis-induced acute lung injury (ALI) in Wistar rats. Results of the study suggested that COR causes significant inhibition of lipid peroxidation (malondialdehyde) together with inhibition of oxidative stress (superoxide dismutase, catalase, glutathione peroxidase, and myeloperoxidase). The level of various proinflammatory (tumor necrosis factor-alpha, interleukin-8, and migration inhibitory factor) was also found to be reduced in COR-treated rats after sepsis. The protective effect of COR was further substantiated by the histopathology of lung tissue, where it improves the architecture of alveolar spaces. In western blot analysis, COR causes significant inhibition of nuclear factor kappa-light-chain-enhancer of activated B cells activation in the lung tissue homogenate. Our results demonstrated that COR was able to prevent the progression of ALI in rats via inhibition of inflammation and oxidative stress.
Sepsis is defined as a deregulated host response to infection which results in organ dysfunction. As per the estimate, alone in the United States, it is responsible for over 1 million cases each year. 1 The lung is the most vulnerable organ to sepsis after the direct or indirect injury, and more than half of the total patients develop acute lung injury (ALI) or acute respiratory distress syndrome. 2,3 The presence of pulmonary edema, arterial hypoxemia, and perivascular infiltration of inflammatory cells, such as neutrophils, eosinophils, lymphocytes, plasmacytes, macrophages, and mast cells are the clinical feature of ALI. 4 -6 The bacterial infection of the blood is another cause of ALI; however, the exact mechanism has not been fully understood until now. 7,8 Therefore, the clinical modalities to treat ALI are only supportive and offer symptomatic relief to the patient such as anti-inflammatory and antibiotic agents. 9 Therefore, the developments of new agents that can improve the condition of ALI are worth to be investigated.
Corynoline (COR) is an isoquinoline alkaloid obtained from Corydalis bungeana Turcz mainly found in the region of Northeast Asia and has been customarily used to take care of inflammation and influenza. It has been reported to possess diverse properties, such as anti-inflammatory 10 and hepatoprotective activities. 11 Recently, the effect of COR has been investigated in lipopolysaccharide (LPS)-induced ALI, where it protects mice from lung injury by activating nuclear factor erythroid 2-related factor 2. 12 On the other hand, the effect of COR on lung injury induced by cecal ligation puncture (CLP) procedure in mice has not been investigated till now. The surgical perforation of the ligated cecum of animal results in immediate and constant drainage of cecal bacteria into the peritoneal cavity to generate an intense immune response induced by polymicrobial infection. This causes overproduction of proinflammatory cytokines. These cytokines lead to the recruitment of leukocytes, tissue damage, and multiple organ failure. It is the most frequently used model because it closely resembles the progression and characteristics of human sepsis. 13 Therefore, in the present study, we intended to investigate the effect of COR in ALI in rats induced by CLP.
Experimental
Animals
Adult male Wistar rats (160-180 g) were obtained from the institutional animal house and kept in polypropylene cages in strict hygienic conditions with the 12 hours of light and dark cycles.
Chemicals
The chemicals used in the present study including COR were purchased from Sigma Aldrich, USA unless otherwise stated.
Experimental Groups
The rats were divided into 4 distinct groups depending on the treatment as follows:
Group 1: Sham
Group 2: CLP
Group 3: CLP + COR (50 mg/kg)
Group 4: CLP + COR (100 mg/kg)
Before CLP surgery, the CLP + COR group received COR by intraperitoneal injection daily for consecutive 3 days, while the rats in sham and CLP groups were given an equivalent volume of olive oil. After 18 hours of the CLP model, the rats were killed, and bronchoalveolar lavage fluid (BALF) and blood were collected for biochemical estimation.
Induction of Sepsis
The animals were anesthetized by an intraperitoneal injection by a mixture of 10 mg/kg xylazine and 100 mg/kg ketamine hydrochloride; a midline laparotomy was performed, and the cecum was exposed, ligated, and punctured 12 times with a 20-gage needle. The cecum was replaced in the abdomen, and the incision was closed. Another group of rats was subjected to midline laparotomy and manipulation of the cecum without ligation and puncture (sham operation). Finally, 1 mL of saline was administered subcutaneously for resuscitation. Control operated mice underwent the same surgical procedures, but the cecum was neither ligated nor punctured. After surgery, animals were put back to their home cages with free access to food and water.
Determination of MDA, SOD, CAT, GPx, and MPO
The concentration of malondialdehyde (MDA), superoxide dismutase (SOD), catalase (CAT), glutathione peroxidase (GPx), and myeloperoxidase (MPO) was determined using the kits obtained from Jiancheng Bioengineering Institute, Nanjing, China, according to the manufacturer’s instructions.
Weight of Lungs
The lung wet/dry (w/d) weight ratio was determined to assess the lung edema. The fresh right middle lobe was measured using an electronic scale and then dried in an oven at 85 °C for 48 hours until the weight remained constant. Dry weights were measured, and the w/d ratios were calculated.
Inflammatory Cell Counts in BALF
The BALF was concentrated by centrifugation (1000 rpm, 10 minutes at 4 °C), and the cell pellet was resuspended in 0.5 mL phosphate-buffered saline (PBS). Total cell count in the BALF was determined with a hemocytometer. A differential leukocyte cell count was performed using 10 µL of the cell suspension, which was transferred to a glass slide and stained with Giemsa stain.
Protein Concentration in Lung BALF
The protein concentration in BALF was determined by the bicinchoninic acid (BCA) protein estimation kit (Beyotime; Haimen, China).
Measurement of Cytokines
Tissue from the lungs was homogenized for enzyme-linked immunosorbent assay (ELISA). Homogenization was performed in ice-cold homogenate buffer, containing 10 mM 4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid (pH 7.9), 10 mM potassium chloride, 2 mM magnesium chloride, 0.1 mM ethylenediaminetetraacetic acid, 1.0 mM dithiothreitol, and 0.5 mM phenylmethanesulfonyl fluoride. The homogenates were centrifuged at 3000×g for 15 minutes at 4 °C. The supernatants were subsequently stored at −70 °C until ELISA was performed for the determination of macrophage migration inhibitory factor (MIF), tumor necrosis factor (TNF)-α, and interleukin (IL)-8 according to the manufacturers’ instructions.
Hematoxylin-Eosin Staining
The lung tissues were embedded in paraffin wax, sectioned into 5 µm pieces, and stained with hematoxylin and eosin (H&E). The pathologic changes in the lung tissues were observed under a light microscope (DP73; Olympus, Tokyo, Japan). Four pathologic processes were assessed and scored on a scale of 0 (normal) to 4 (maximal): (1) alveolar congestion; (2) hemorrhage; (3) leukocyte infiltration or aggregation of neutrophils in airspace or the vessel wall; and (4) thickness of the alveolar wall/ hyaline membrane formation.
Western Blot
Total proteins were extracted from lung tissues using ice-cold radioimmunoprecipitation assay lysis buffer. Dissolved proteins were collected and centrifuged at 12 000 rpm for 5 minutes at 4 °C. The BCA protein assay (Sigma Aldrich, USA) reagent was used to estimate the concentration of total protein. Equal amounts of denatured protein (25 µg in each lane) were separated by 12% sodium dodecyl sulfate-polyacrylamide gel electrophoresis, electrotransferred onto a polyvinylidene difluoride membrane (Millipore Corp, Billerica, MA, USA), and probed with primary antibodies (1:1000 in 1% bovine serum albumin [BSA]/Tris-buffered saline, 0.1% Tween 20 [TBS-T]; Cell Signaling Technology, Danvers, MA, USA) overnight at 4 °C. The membranes were then washed twice for 15 minutes each in TBS-T and incubated with horseradish peroxidase-conjugated goat antimouse or antirabbit antibodies (1:10 000 in 1% BSA/TBS-T; Santa Cruz Biotechnology, Inc., Dallas, TX, USA). After extensive washing, the proteins were detected immediately by the enhanced chemiluminescence reagent (Amersham Pharmacia Biotech, Tokyo, Japan). The relative expression ratio was determined with the density of the band of the protein of interest to that of a β-actin reference band using the software UN-SCAN-IT gel version 6.1 (Silk Scientific, Inc., Orem, UT, USA).
Statistical Analysis
All experiments were performed in triplicate. The data were represented as the mean ± SD. Statistical analysis was carried out using SPSS for windows by one-way analysis of variance followed by the Bonferroni post hoc test. Statistical significance was expressed as *P < 0.05.
Results
Effect of COR on Lipid Peroxidation
The effect of COR was investigated on the level of MDA (Figure 1). Result suggests that the level of MDA was found elevated in CLP-treated rats as compared with sham. In the COR-treated rat, the level of MDA was reduced significantly.
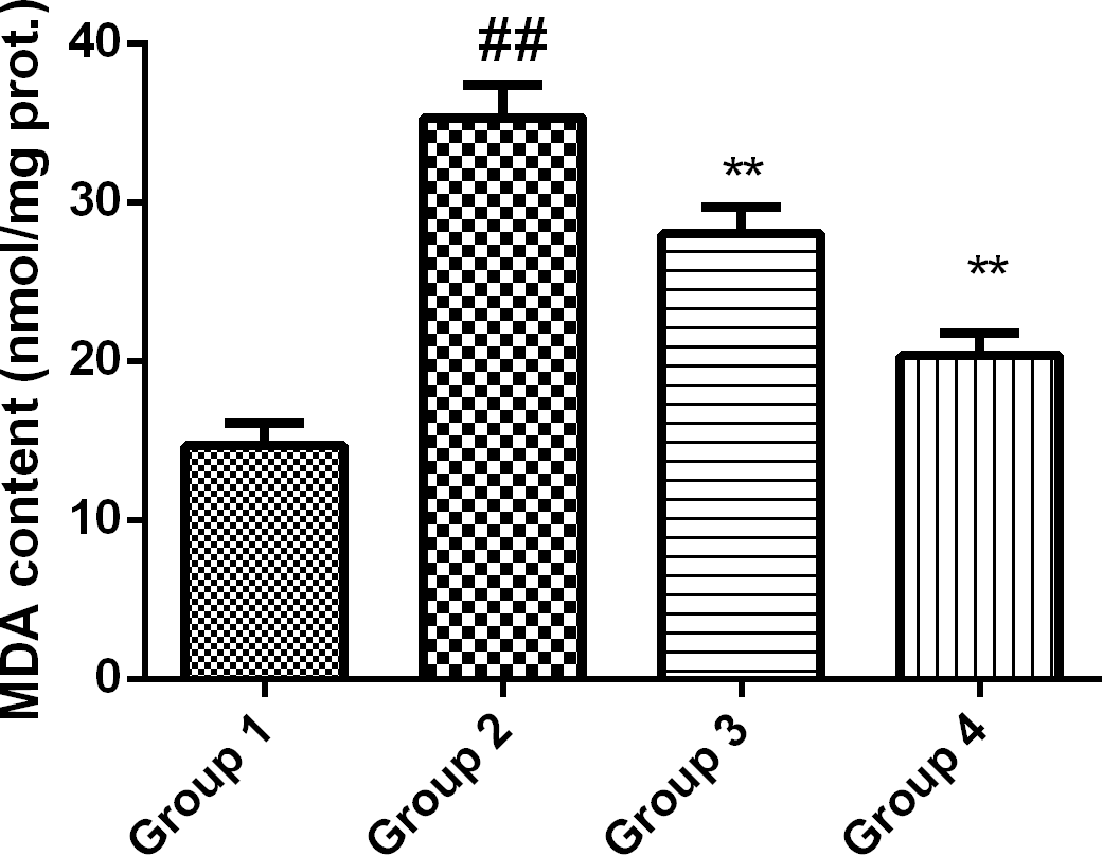
Effect of corynoline on the malondialdehyde (MDA) depicting lipid peroxidation. Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on Lung Weight Ratio
As presented in Figure 2, the effect of COR was investigated on the ratio of w/d lung weight ratio. The ratio of w/d lung was found elevated in the CLP group as compared with the control. The ratio was significantly restored near to sham in the COR-treated group in a dose-dependent manner.
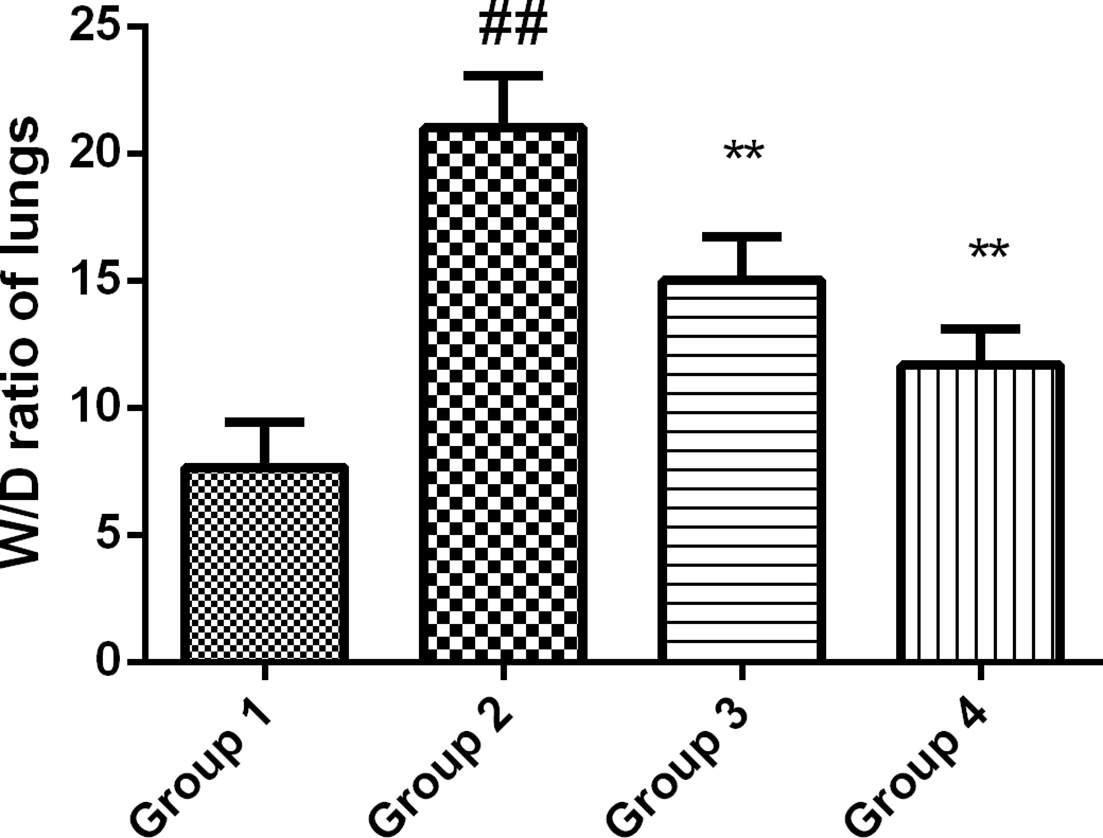
Effect of corynoline on the wet/dry (w/d) lung ratio of rats. Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on Proinflammatory Cytokines
The level of various proinflammatory cytokines was measured in various treatment groups. As presented in Figure 3, the level of TNF-α, IL-8, and MIF was found elevated in the CLP-treated group as compared with the sham. However, the level of these cytokines was reduced significantly by pretreatment of COR as compared with CLP.

Effect of corynoline on the cytokines (A) tumor necrosis factor-alpha (TNF-α), (B) interleukin-8 (IL-8), and (C) migration inhibitory factor (MIF). Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on Protein in BALF
As presented in Figure 4, the level of protein in BALF was found elevated in the CLP-treated group. However, the protein concentration was found reduced significantly in the COR-treated group as compared with the sham.

Effect of corynoline on the concentration of protein in bronchoalveolar lavage fluid (BALF). Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on the Inflammatory Infiltrates
The level of various inflammatory infiltrates was investigated into BALF, and results are presented in Figure 5. The level of these infiltrates was found to increase in the CLP-treated group. However, the level of these infiltrates was found significantly reduced in a dose-dependent manner in the COR-treated group.

Effect of corynoline on inflammatory infiltrates, (A) total cells, (B) neutrophills, and (C) lymphocytes. Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on Oxidative Stress
In the next instance, the effect of COR was investigated on oxidative stress biomarkers (Figure 6). The level of SOD, GPx, and CAT was found to decrease in the CLP-treated group together with an increase in MPO activity as compared with sham. However, the level of these biomarkers was found restored near to normal in the COR-treated group.

Effect of corynoline on oxidative stress, (A) superoxide dismutase (SOD), (B) catalase (CAT), (C) glutathione peroxidase (GPx) and (D) myeloperoxidase (MPO). Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on the Histopathology of Lung Tissues
As shown in Figure 7, lung tissues of the sham group showed normal architecture with no alteration in the tissue histopathology. Whereas as compared with sham, tissues from the CLP group showed typical pathologic changes, such as infiltration of inflammatory cells into alveolar space, interstitial edema, and pulmonary congestion. On the other hand, as suggested by the histopathological score, the pathologic changes were significantly reversed in the COR-treated group.
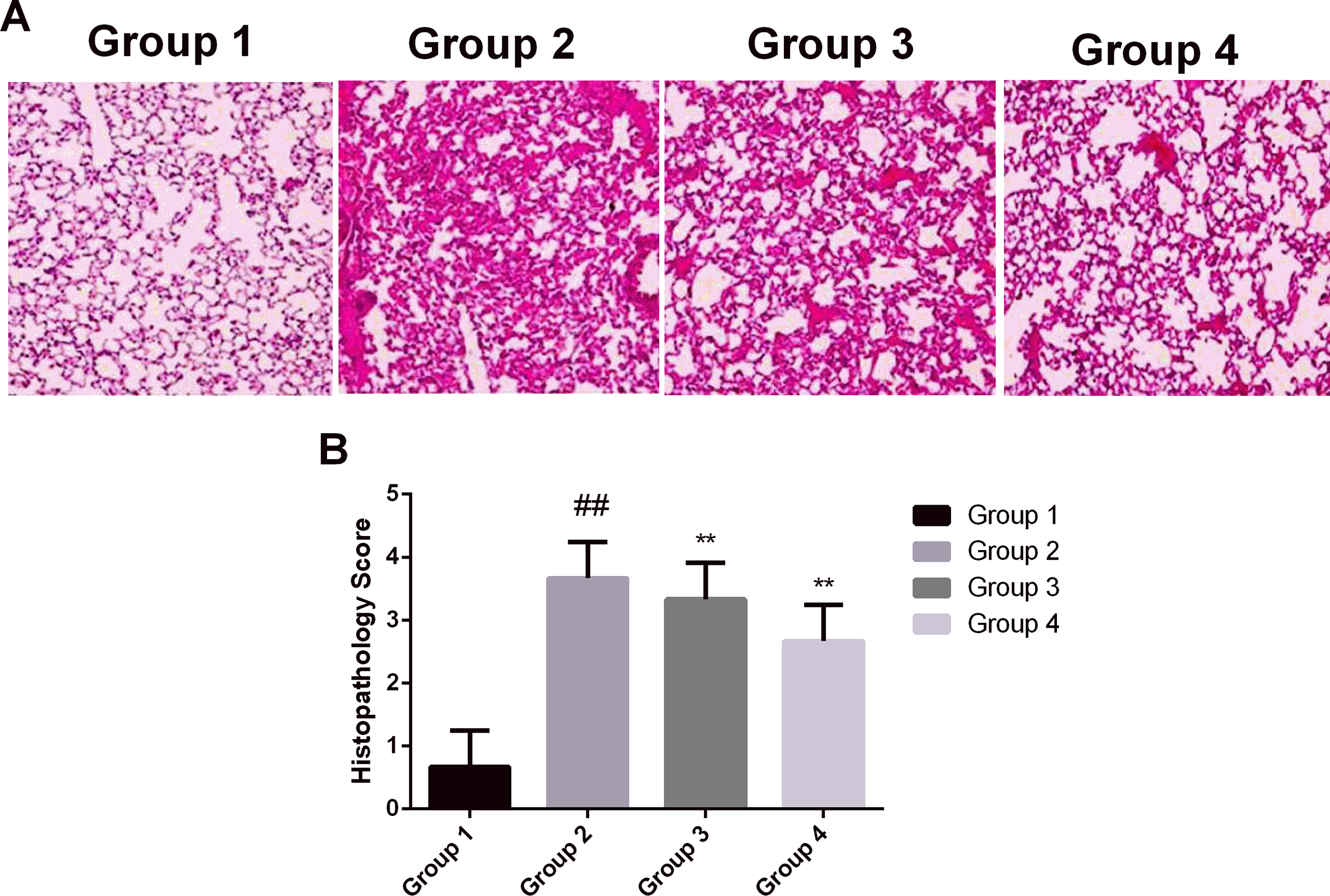
Effect of corynoline on the (A) histopathology of lung tissues and (B) quantitative histopathology score of lung tissues. Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Effect of COR on the Expression of NF-ĸB
The last part of the study was aimed at investigating the effect of COR on the expression of nuclear factor kappa-light-chain-enhancer of activated B cells (NF-ĸB) by western blot analysis. The results are presented in Figure 8. The level of p-NF-ĸB and p-IĸBα was found overexpressed in the CLP-treated group. However, the level of p-NF-ĸB and p-IĸBα was reduced significantly in the COR-treated group in a dose-dependent manner. Moreover, the COR-treated group also showed to inhibit the cytoplasmic level of NF-ĸB and nuclear translocation of NF-ĸB from the cytoplasm.

Effect of corynoline on the expression of nuclear factor kappa-light-chain-enhancer of activated B cells (NF-ĸB) as determined by western blot. Experimental results were presented as mean ± SD. ## P < 0.05 vs Group 1; **P < 0.01 vs Group 2, one-way analysis of variance followed by Bonferroni post hoc test.
Discussion
The sepsis-induced ALI is the major cause of morbidity and mortality worldwide. 14 However, it is difficult to treat due to multifactorial etiology and pose a significant risk to the individual. Thus, symptomatic treatment is the only viable option left. 15,16 Many therapeutic modalities are being currently used to curb the menace of ALI; however, none of them will have a significant impact on the overall survival of patients. Thus, it is worthwhile to investigate new agents/drugs to treat ALI. In the present study, COR showed significant improvement of various biochemical mediators which are known to be involved in ALI. Thus, it could be easily suggested that COR has a protective effect against ALI. Initially, the effect of COR was investigated on the MDA level, which is an important biomarker for lipid peroxidation. Various studies have implicated the importance of lipid peroxidation processes in many organ failures, and more importantly in ALI. Due to their toxic properties, they are deemed to be a causative agent for cellular dysfunction at the site of their origin and far beyond. 17,18 As shown in the results, COR causes a significant reduction of MDA level and thus may exert a protective effect against ALI via lowering the lipid peroxidation. The presence of pulmonary edema is the clinical feature of ALI and can be easily identified by w/d lung ratio in experimental animals. 19,20 In the present study, COR causes a significant reduction of the w/d ratio of lungs. Various studies have implicated the role of polymorphonuclear neutrophils and macrophages in the generation of inflammatory response in ALI patients causing microvascular injury of the lungs. Inflammatory insults, either locally from the lungs or systemically from extrapulmonary sites, damages bronchial epithelium, alveolar macrophages, and vascular endothelium. It results in the increase of protein-rich edema fluid into the alveoli and, consequently, hypoxemia due to impaired gas exchange. 21,22 Accumulating evidence suggests that the concentration of proinflammatory cytokines, such as IL-8, MIF, and TNF-α found elevated in the BALFs from the patients of ALI. 17,18 In the present study, COR causes a decrease in inflammation in CLP rats. It reduces the concentration of cytokines, inflammatory infiltrates, and protein concentration in BALF. Oxidative stress is another clinical feature found in ALI. The development of oxidative stress due to the presence of reactive oxygen species is linked with the presence of proinflammatory compounds. 23 -25 Thus, it is worthwhile to determine the effect of COR on oxidative stress by evaluating the expression of various biomarkers. COR significantly inhibited oxidative stress by increasing the level of SOD, GPx, and CAT together with a decrease in MPO activity. The protective effect of COR against ALI was further confirmed by analyzing the histopathology of lung tissues of rats, where COR showed significant improvement in the architecture of lung tissues. NF-κB is an inducible transcription factor known to regulate the expression of many genes involved in immune and inflammatory responses in ALI. 7,26,27 In our study, COR significantly inhibited the activation and translocation of NF-ĸB in western blot analysis.
Conclusion
Taken together, our data suggest that COR was able to prevent the progression of ALI in rats via inhibition of inflammation and oxidative stress. The protective effect of corynoline against ALI was suggested to be mediated via attenuating the activation of NF-ĸB.
Footnotes
Statement of Informed Consent
There are no human subjects in the article and informed consent is not applicable.
Statement of Human and animal rights
All of the experimental procedures involving animals were conducted in accordance with the Institutional Animal care guidelines of Huazhong University of Science and Technology Union Shenzhen Hospital, Shenzhen, and approved by the Animal Ethical Committee of Huazhong University of Science and Technology Union Shenzhen Hospital, Shenzhen.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
