Abstract
Diabetes mellitus (DM) is a complex metabolic disorder characterized by abnormal glucose metabolism, which is accompanied by alterations in energy metabolism, intestinal bacterial metabolism, amino acid metabolism, lipid metabolism, nucleotide metabolism, and others. However, intestinal flora metabolism plays a fundamental role in host metabolism; they are complementary to each other and help maintain homeostasis, thus ensuring the normal operation of the host metabolic system. This suggests that a holistic analysis method would be of great use in the study of the overall metabolism in patients with DM. With this in mind, this review summarizes the mechanism of intestinal flora metabolism regarding the occurrence of DM and assesses the effects of drug treatments on the intestinal flora of patients with diabetes. Based on these results, we combined intestinal flora metabolism with host metabolism to evaluate the necessity and the advantages of holistic metabonomics analyses in the treatment of DM and its complications.

According to the International Diabetes Federation, the number of people with diabetes mellitus (DM) in the world will reach 642 million by 2040. Diabetes and its complications are a serious threat to human health and can also negatively influence numerous social and economic factors. Although there are many treatments for this disease, the occurrence of diabetes and its complications is still very common. It is suggested that an imbalance in the intestinal flora is closely related to the occurrence and development of metabolic diseases such as DM. 1,2 Intestinal bacteria can produce a number of secondary metabolites, including amino acids and fatty acids, and most of these secondary metabolites can act on specific receptors and participate in regulating the normal physiological processes of the host. 3 -6 The state of the symbiotic metabolic network between the intestinal flora and the host also shows that it is necessary to study the occurrence and development of DM using holistic analysis methods. Metabonomics is a technique used for analyzing the differences in metabolic profiles in body fluids under different conditions. Moreover, this approach could be used to comprehensively analyze the effects of a disease on any biological system. As such, metabonomics provides a good technical platform for metabolic research regarding DM.
Mechanisms Underlying Intestinal Flora Metabolic Disorders
The dynamic balance between the intestinal flora and host physiological function indicates that metabolic disorders of the intestinal flora may lead to the occurrence of host diseases. 7 Studies have confirmed that an intestinal microbial imbalance can induce inflammation, 8 obesity, 9 insulin resistance, 10 and other metabolic diseases, including diabetes. 11 However, the unified mechanism by which an intestinal flora imbalance affects DM has not been fully elucidated. The possible mechanisms include alterations in short-chain fatty acids (SCFA), anti-inflammatory response, and intestinal mucosal permeability (Figure 1).

The mechanisms underlying intestinal flora metabolic disorders affecting diabetes mellitus (DM). Intestinal flora is involved in the development of DM mainly through different pathways, such as short-chain fatty acids produced by its own metabolism, changing the abundance of anti-inflammatory bacteria, and intestinal mucosal permeability.
Intestinal Flora and Short-Chain Fatty Acids
SCFA are mainly produced via digestible sugars, such as dietary fiber, starch, and oligosaccharides, and fermented by beneficial bacteria present in the colon, including lactic acid bacteria and Bifidobacteria. 12 Acetic acid, propionic acid, and butyric acid are all relatively abundant within the human digestive system. Butyric acid is the main energy source of colonic mucosal epithelial cells. It can inhibit the growth and reproduction of pathogenic microorganisms and increase the number of beneficial microflora, thereby improving the intestinal microflora balance. Moreover, relevant studies have shown that ingesting butyric acid-producing or acetic acid-producing bacteria can effectively prevent and control diabetes. 13
Clinical trials have found that taking acetic acid, propionic acid, and butyric acid at the same time in patients with normal blood sugar levels can help effectively control body weight, promote fasting fat oxidation, increase resting energy consumption, reduce fasting blood sugar, and improve glucose and lipid metabolism. 14 SCFA are involved in the development of DM based on their ability to mediate a reduction of the intestinal anti-inflammatory response and weaken the activity of the SCFA receptor. 15 Additionally, considerable evidence indicates that short-chain fatty acids and bile acids produced by intestinal flora play a role in regulating glucose homeostasis. 16 Increasing the production of SCFA in the host is also beneficial due to their antiobesity and antidiabetic effects. 17 -19 Acetic acid, butyric acid, and propionic acid can also help prevent insulin resistance. 20 Additionally, the intestinal microflora can regulate the metabolism and secretion of bile acid, thereby affecting its metabolism and further participation in the process of DM. 21 For example, acetate promotes metabolic syndrome by mediating the microbiome-brain-β-cell axis. 22 Furthermore, succinic acid produced by microorganisms has been reported to improve glucose metabolism by activating gluconeogenesis in the intestines of mice. 23
Intestinal Flora and the Inflammatory Response
Type 2 diabetes is considered a low-grade inflammatory disease. Studies 24 have shown that inflammation and lipopolysaccharide levels are elevated in patients with type 2 diabetes, and some researchers have speculated that a decrease in anti-inflammatory related bacteria can accelerate the occurrence and development of DM. 25 Biological disorders caused by microbial dysregulation can increase chronic inflammatory conditions, 26 and lipopolysaccharide (LPS), a component of Gram-negative bacteria of the genus Proteus, can induce the release of a series of inflammatory factors and help promote the development of DM. 27 Intestinal microorganisms increase the permeability of the intestinal mucosa, allowing endotoxin to enter the blood, inducing chronic metabolic endotoxemia, and further inducing inflammation of the body. 28 Overaccumulation of LPS can lead to chronic metabolic endotoxemia, which, studies have found, can lead to obesity, diabetes, and insulin resistance. 29 The abnormal increase of conditional pathogens, such as Proteobacterium, can lead to a disease state via the above mechanism of action. In addition, Escherichia coli is an intestinal mucosal bacteria associated with low-grade inflammation 30 and can produce a substance very similar to insulin, which interrupts insulin signaling by binding to insulin’s target cells, thus promoting diabetes. At the same time, studies have shown that Clostridium leptum can reduce inflammation induced by regulatory T cells by inhibiting the production of LPS. 31 Additionally, butyric acid can promote the repair of the intestinal mucosa and its functional recovery and can inhibit the formation of inflammatory cytokines, thus playing an important anti-inflammatory role. 32 -34
The Intestinal Flora and Intestinal Mucosal System
The intestinal flora can regulate the permeability of the intestinal mucosa, thus promoting the occurrence and development of DM. 35 Intestinal tight junction proteins are closely related to the permeability of the intestinal mucosa, which is an important structural basis of the intestinal mucosal barrier. The destruction of the tight junction structure can lead to an increase in the permeability of the intestinal wall, further inducing inflammation and multiple organ dysfunction. 36 Studies have also shown that the expression of intestinal tight junction proteins is decreased in diabetic rats, while the resulting increase in intestinal permeability leads to immune and inflammatory responses, which further destroy pancreatic β cells. 37
In addition, 7 markers in the Kyoto Encyclopedia of Genes and Genomes pathway that are enriched in patients with type 2 DM were also found to be associated with oxidative stress resistance, which may indicate that the intestinal environment of these patients can stimulate bacterial resistance toward oxidative stress. Moreover, intestinal flora can act on the intestinal immune system, and the dysregulation caused by microbial flora disorders can effectively reduce the immune response. 38
Reconstruction of the Intestinal Flora for the Treatment of Diabetes
The intestinal flora is an extremely complex micro-ecosystem, and under normal circumstances, the intestinal microorganisms can regulate energy metabolism, protect the body, and provide nutrients via the secretion of enzymes and synthesis of metabolites. However, external conditions, including diet, can promote intestinal flora disorders, which lead to the occurrence of chronic metabolic diseases, such as diabetes, via a series of mechanisms. 39 At present, drug regulation of intestinal microorganisms has been proposed as an effective way to treat DM. 40 The latest studies, performed both in vivo and in vitro, regarding drug metabolism by intestinal microorganisms published in Nature have shown that drugs can be metabolized by specific bacteria when they encounter intestinal microorganisms. At the same time, researchers have used gain-of-function mutants to show that bacteria without specific functional gene fragments cannot metabolize these drugs. In contrast, these bacteria can resume their metabolic functions after the replacement of these fragments. On this basis, researchers have performed gene enrichment analysis to explore genes involved in the metabolism of diltiazem and found individual differences in the metabolic capacity toward this drug, suggesting that genetic factors may partly explain differences in the intestinal microbial metabolic capacity among individuals. The results of this prior study provide a basis for the rational regulation of individual microbiomes to alter the microbiome-host interaction so as to maximize the efficacy of specific drugs. 41
Drugs for Improving the Intestinal Microflora
Chinese medicinal compounds
Traditional Chinese medicines (TCMs) are typically composed of 2 or more medicines. Each drug is compatible with the other, and each plays a coordinated therapeutic role. A large number of studies have shown that TCM compounds can confer their therapeutic role by influencing the composition and structure of the intestinal flora. Huang-Lian-Jie-Du-Decoction 42 includes 4 herbs: Huanglian (Coptidis Rhizoma), Huangqin (Scutellariae Radix), Huangbo (Phellodendri Chinensis Cortex), and Zhizi (Gardeniae Fructus). Experiments have shown that this compound can significantly improve the hyperglycemia and inflammation occurring in diabetic mice. In addition, this study also confirmed that the intestinal flora composition of these DM mice changed after the application of this compound, including an increased number of SCFA-producing bacteria and anti-inflammatory related bacteria, such as Parabacteroides, Blautia, and Akkermansia, and a reduced amount of conditioned pathogenic bacteria (eg, Aerococcus, Staphylococcus, and Corynebacterium). This compound was also shown to improve the intestinal flora balance in type 2 diabetes rats.
The main components of Xiexin Decoction are Dahuang (Rhei Radix et Rhizome), Huangqin (Scutellariae Radix), and Huanglian (Coptidis Rhizoma), and studies have shown that Xiexin Decoction can significantly reduce blood sugar levels, improve lipid metabolism disorders, and play an anti-inflammatory role in type 2 DM rats. 43 At the same time, the composition of the intestinal flora in type 2 DM rats treated with Xiexin Decoction was significantly altered, especially regarding the number of SCFA bacteria and anti-inflammatory related bacteria. On this basis, researchers have suggested that the balance of important microbial flora in the intestine is closely related to the indicators of DM. The patient with DM obviously showed abnormal lipid and energy metabolism, insulin resistance, and obesity. 44 -46
The Linggui Zhugan (LGZG) formula mainly contains 4 components: Fuling (Poria), Guizhi (Cinnamomi Ramulus), Baizhu (Atractylodis Macrocephalae Rhizoma), and Gancao (Glycyrrhizae Radix et Rhizoma). 47 Clinically, this prescription is often used in the treatment of obesity. Comparing type 2 diabetes model mice with mice treated with LGZG, researchers found that treatment with LGZG could affect the richness and diversity of the intestinal flora in the feces of these mice, and this mainly involved an increase in the relative abundance of certain bacteria, such as Bacteroidetes and Lactobacillus, and a reduced abundance of Oscillospira and Helicobacter. In addition, this compound was found to improve obesity and reduce serum glucose and lipid profiles. Accordingly, the researchers speculated that these observations might be closely related to the impact this compound has on the gut microbiota.
TCM extracts
Previous studies have shown that polyphenols (EPE3k) and flavonoids from Enteromorpha prolifera extracts can reduce fasting blood sugar levels, regulate insulin release, and improve insulin resistance. 48 It is suggested 49 that intestinal microflora are closely related to the occurrence of DM, and studies have confirmed that Alpinia oxyphylla extracts (AOE) can reduce blood sugar and improve kidney damage in diabetic mice by altering the composition of intestinal microorganisms. 50 This conclusion is consistent with AOE increasing the abundance of Bacteroides, Phytophthora, and Akkermansia and reducing Helicobacter levels. Experiments 51 have also shown that polyphenol extracts from Herba Dendrobii loddigesii can increase the proportion of Bacteroides to Firmicutes and decrease the abundance of E. coli, and these 3 types of bacteria are related to low-grade inflammation of the body. In addition, these extracts can increase the abundance of Akkermansia muciniphila, suggesting that the mechanism of action for this compound in the treatment of DM is likely related to the regulation of different bacterial abundances. Studies have also shown that corn silk polysaccharide can increase the number of beneficial bacteria, such as Lactobacillus and Bacteroides, in the intestinal tracts of diabetic mice, reduce blood sugar levels, and increase the insulin sensitivity index, suggesting that corn silk polysaccharide can restore the balance of intestinal flora and could be used to treat diabetes. 52
Metformin and Lactobacillus acidophilus supplementation
Metformin, an antidiabetic drug commonly used in western medicine, is widely used clinically for treating patients with diabetes. Recently, it has been reported that metformin significantly alters the composition of the intestinal microflora and the concentration of intestinal SCFAs, which are likely related to its effect on DM. 53 -55 The clinical data 56 regarding patients with DM also revealed that the combination of metformin and Chinese herbal preparations improved hyperlipidemia and reduced blood sugar levels in these patients, suggesting that the role of Chinese herbal preparations is related to the enrichment of beneficial bacteria in the intestinal tract, including the enrichment of SCFA-producing bacteria, Brauderia, and fecal bacteria.
Lactobacillus acidophilus is a common probiotic bacteria, and research has confirmed 57 that it can improve the symptoms of type 2 diabetes by regulating the intestinal flora. This conclusion is supported by the following observations: L. acidophilus treatment can also alter the expression of genes related to glucose and lipid metabolism. Moreover, L. acidophilus 58 supplementation can reshape the gut microbiota by increasing the prevalence of SCFA-producing bacteria and reducing the relative abundances of Gram-negative bacteria, which are related to the inflammation reaction. Therefore, L. acidophilus is a strong candidate for the treatment of diabetes (Table 1). Overall, the effect of drugs and other treatments on the intestinal flora in patients with DM is mainly achieved by improving the composition and diversity of the intestinal flora.
Influencing the Intestinal Flora of Patients with DM.

DM, diabetes mellitus; SCFA, short-chain fatty acids.
A Holistic View Regarding the Treatment of Diabetes
In terms of improving the intestinal flora imbalance occurring during diabetes, both TCM and western medicine can only treat diabetes by acting on different individual targets. In addition, the Chinese Diabetes Society issued in 2018 the “Guidelines for the Prevention and Treatment of Type 2 Diabetes in China (2017 edition),” clearly indicating that metabolic surgery can effectively improve body weight and blood sugar levels. At the same time, this approach can help control blood lipid levels, blood pressure, and other metabolic indicators, helping to alleviate the symptoms associated with diabetes significantly. However, metabolic surgery has certain short-term and long-term risks, especially in the Chinese population; therefore, demonstrating the effectiveness and safety of this approach still requires further evaluation.
In fact, the metabolic pathways of patients with diabetes have been altered prior to the occurrence of different histopathological changes. As such, the related differential metabolites might serve as potential biomarkers for the occurrence and development of DM. 67 This suggests that there is a certain limitation in the use of a single target to treat diabetes. With this in mind, a holistic approach is necessary to understand the metabolic mechanisms of diabetes fully. In recent years, emerging methods in metabonomics can be used to comprehensively analyze the changes and regularities of endogenous metabolites after an external stimulation or disturbance. 68 Among these, nontargeted metabonomics technology can be used to obtain the whole metabolomic information of an organism. This approach is mainly used to search for metabolites with obvious changes between experimental and control groups and to identify the chemical structure of the metabolites, with such results helping to explain the relationship between such metabolites, the involved metabolic pathways, and the state of the organism. 69 This technique is also conducive to the discovery of new metabolites and metabolic pathways and is important for the development of biomarkers for disease diagnosis and research involving disease pathology (Figure 2).

Prediction and diagnosis of metabolic pathways and types in patients with T1DM. The figure shows that the occurrence and development of type 1 diabetes mellitus mainly involves two metabolic pathways: amino acid metabolism and lipid metabolism.
Studies have confirmed that metabolomics analysis methods can be widely used for the detection of biomarkers related to DM, pathogenesis, drug efficacy, early diagnosis, and other processes. 70,71 In combination with PCA and OPLS-DA, Jianping Chen et al analyzed the potential biomarkers in the serum of model and control groups and revealed that Zishen Jiangtang Pill could reverse metabolite levels related to lipid metabolism and suggested that these metabolites were closely related to the occurrence of obesity in relation to DM. 72
Biomarkers can be used to objectively measure and evaluate the physiological, pathological, and other characteristics of an organism.
73,74
Biomarkers can also reflect changes to biological processes subsequent to treatment. At present, the biomarkers related to diabetes mainly include amino acids (alanine, valine, lysine, isoleucine, methionine, etc), organic acids (dimethyl glycine, butane dioic acid, glutaric acid, ornithine, etc), lipids (lyso PI, lyso PC, PG, TG, etc) carbohydrate (
In order to assess the predictive ability of metabolomic data for forecasting the future risk of type 2 diabetes, researchers have collected a large number of metabolite samples and identified a set of the most predictive metabolic markers. These include an assessment of the development of type 2 DM in healthy people during the follow-up period. 78 Based on mass spectrometry-targeted as well as global-untargeted metabolomics, the final results show that 9 metabolites were negatively associated and 25 were positively associated with progression to type 2 diabetes. On the basis of known metabolites, new predictive biomarkers were identified, which play an important role in predicting the occurrence of type 2 DM. This series of studies found a number of potential biomarkers among the metabolites of patients with DM, as assessed via metabonomics. Overall, the tracking and establishment of novel biomarkers is helpful for the study of DM pathogenesis and will also help facilitate the early prevention and treatment of DM (Figure 3).
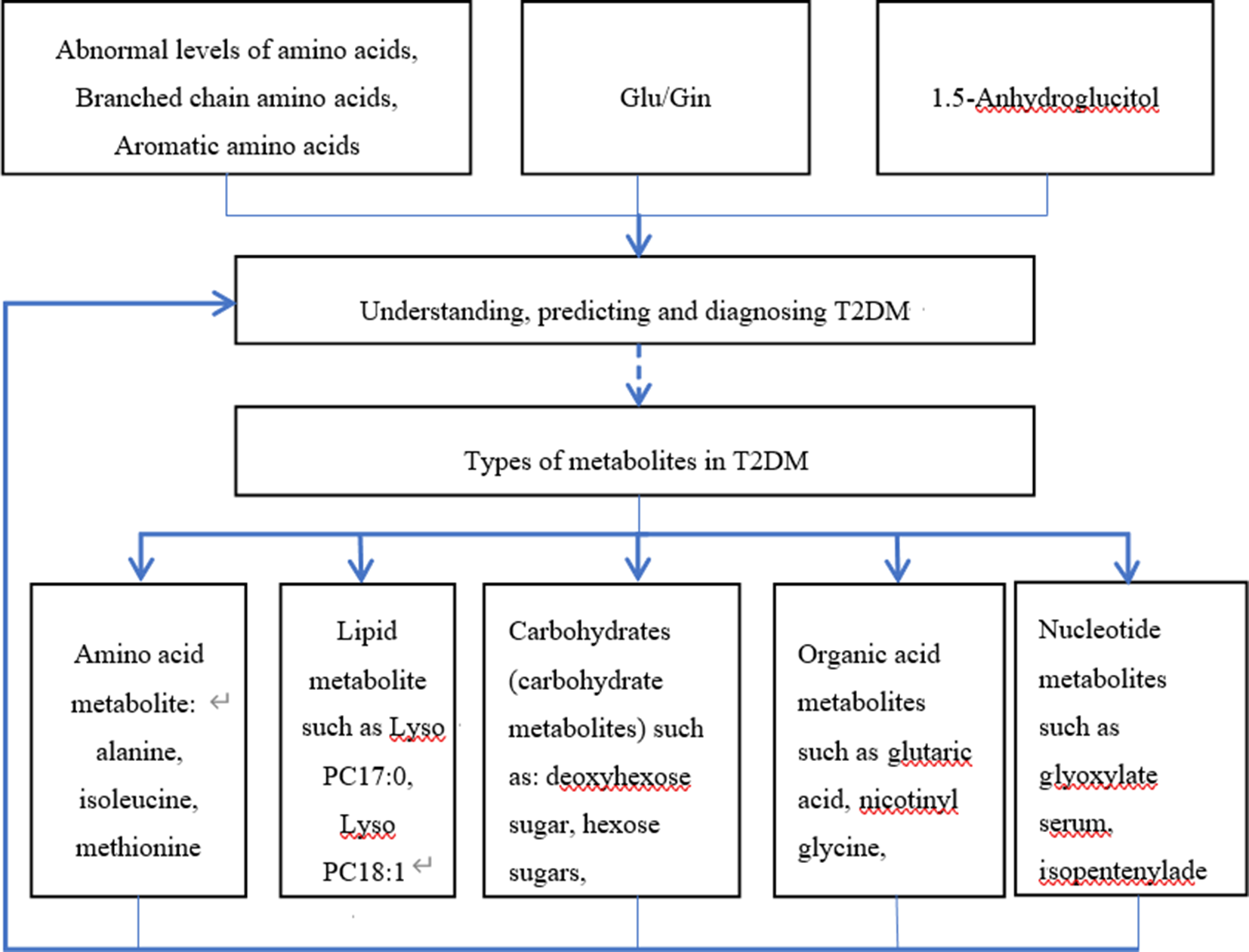
Understanding and predicting metabolic pathways in patients with type 2 DM. The occurrence and development of type 2 DM involve abnormal metabolic pathways, such as amino acid metabolism, lipid metabolism, carbohydrate metabolism, and nucleotide metabolism, which lead to changes in various metabolites within the body. Conversely, these metabolites, which are closely related to the development of type 2 diabetes, can also serve as potential biomarkers for understanding, predicting, and diagnosing this disease.
At present, monitoring the metabolic levels of early-stage indicators has become an important approach toward detecting various diseases. By identifying and quantifying the metabolic markers and regulatory pathways associated with type 2 diabetes, we can better study the mechanism of the metabolic disorders linked to diabetes and help predict the occurrence of this disease.
Discussion
DM is a disease that is characterized by elevated blood sugar levels, involves multiple targets, and presents with complications associated with different cardiovascular and cerebrovascular diseases and microangiopathy. At present, the clinical control of DM and its complications is still not ideal. As mentioned above, it has been summarized that single Chinese and western medicines can have antidiabetic effects, which are conferred by restoring the composition of the intestinal flora. 42,43 These observations could help promote the progress of DM treatments. However, as far as the aforementioned drugs are concerned, they are mostly based on a single target and, as such, play a specific therapeutic role. Complications caused by DM include diabetic nephropathy, diabetic retinopathy, diabetic foot, and other microvascular lesions occurring in different parts of the body. 79 These symptoms cannot be effectively improved by only lowering blood sugar levels. At present, it is considered that diabetes is a kind of clinical symptom with glucose metabolism disorder, which is caused by both genetic factors and environmental factors. The internal factors affecting diabetes include deficiency of the body’s autoimmune system, absolute or relative deficiency of insulin secretion caused by impaired islet b-cell function, and decrease of insulin sensitivity. In recent years, research has found that the intestinal flora, as an important part of the host, can directly participate in various essential metabolic processes within the host. These organisms are interdependent, inseparable, and maintained in a relatively balanced state. 80 Intestinal flora metabolism and host metabolism are complementary to each other and help maintain homeostasis, thus ensuring the normal operation of the host metabolic system. 81
The intestinal flora can produce a variety of secondary metabolites that accumulate in the blood, including various amino acids and fatty acids. In many cases, these secondary metabolites can act on specific receptors, thus playing a key role in the transmission of information. In addition, they can regulate the homeostasis of the host’s internal environment, can participate in diverse physiological and pathological processes, and have a systematic impact on the host. 3 -6 In addition, these secondary metabolites can directly regulate intestinal functions and indirectly regulate the functions of parenteral organs, such as the liver, brain, and kidney. The above literature shows that an intestinal flora imbalance exists in patients with DM, and this imbalance is related to insulin resistance; as such, this imbalance might be closely related to the occurrence and development of metabolic diseases such as DM. 10 This also suggests that restoring homeostasis of the symbiotic metabolic network between the intestinal flora and host could be helpful for the treatment of DM. TCM compounds, including many drugs with different functions, can have a synergistic effect, possibly enhancing their therapeutic effect by acting on multiple targets. 42 Therefore, based on the advantages of multicomponent, multitarget, and multiefficacy of traditional Chinese medicine compounds, it can be surmised that such compounds might provide more comprehensive and systematic improvements for the treatment of diabetes and the complications associated with DM.
Previous studies have shown that the number and proportion of intestinal flora in patients with DM are different from those in healthy individuals. It is also suggested that the effect of hypoglycemic agents is related to changes in the intestinal flora. In such experiments, most researchers have analyzed the quantity and composition of the fecal flora before and after the administration of a given treatment. Importantly, they found that the intestinal flora of DM patients was different from that of non-DM patients. 82 However, the specific mechanism linking the efficacy of anti-DM drugs and the observed changes in the intestinal flora remains to be further explored. DM is mainly characterized by disorders in glucose metabolism accompanied by complex metabolic disorders, such as those affecting lipid metabolism and amino acid metabolism. So far, some progress has been made in the study of the mechanisms related to diabetes, but these mechanisms and their associated complications have not yet been fully explained. 83 Metabolomics analysis methods, an emerging omics technology, can comprehensively analyze changes in endogenous small molecular substances within the body. At the same time, this method can be combined with LC-MS analysis technology, biomarkers, and other means to explore the related metabolic substances and metabolic pathways involved in DM, so as to better reveal the mechanism of diabetes and its complications. 80
Diabetes, a kind of metabolic disease, its pathogenesis, and pathological state are very complex. So a single treatment cannot fully reveal the complex pathology of diabetes. Therefore, the holistic approach is more conducive to the treatment of diabetes and reveals the complexity of diabetes. On the one hand, based on the symbiosis and interaction of intestinal flora metabolism and host metabolism, a variety of secondary metabolites produced by intestinal flora can regulate the homeostasis of host environment, and the homeostasis of both sides ensures normal operation of host metabolic system. On the other hand, the clinical characteristics of diabetes are the metabolic disorder of carbohydrate, lipid, amino acid, and other substances. The use of metabonomics can bring new solutions to the exploration of pathogenesis, early diagnosis of disease, evaluation of drug efficacy, and elaboration of mechanism of action. 84,85 Many studies have shown suggest that the holistic approach can have certain value in the prevention, diagnosis, and treatment of diabetes. In short, DM is a complex metabolic disorder caused by multiple factors. Numerous studies have shown that improving intestinal flora metabolism as a core pathway can effectively alleviate diabetes. However, it is of great significance to systematically study the metabolic mechanisms underlying DM in terms of the whole organism. Therefore, in future studies, it will be of great significance to explore the metabolites affected by traditional Chinese medicinal compounds in regard to DM and its complications by using metabonomic analysis methods. In this regard, assessing the changes in the intestinal flora will be of great value toward developing effective treatments for DM.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This paper was fully funded by the National Natural Science Foundation of China (Nos. 81774007, 81560806, 81473427, 81173360), the National Key R&D Program of China (No. 2017YFC1703904), the Science and Technology Plan of Qinghai Province (2017-ZJ-922Q), and Education Department of Sichuan Province (16ZA0120).
