Abstract
Our previous studies confirmed that
An epidemiological investigation showed that 246 million people suffered from type 2 diabetes mellitus and were tormented with its complications throughout the world, and it was expected that this number would increase to 380 million by 2030 if the disease would not be controlled in time. 1 Diabetic nephropathy is one of the most common and severe complications of diabetes, and the primary cause of disability and death in diabetic patients. 2 The pathogeny of type 2 diabetes mellitus is hidden and about 5% of the patients have complicated with the renal damage when they are diagnosed with type 2 diabetes mellitus; after the occurrence of the renal damage for a few years, the glomerulus, renal tubule, and renal interstitium are almost damaged; the persistent proteinuria indicates that the patients’ conditions may be irreversible in diabetic patients with the renal damage. 3 The complications will significantly lower the quality of life of the patients, and also significantly increase the cost and the difficulty of treatment, 4 so that the early prevention and treatment of diabetic nephropathy are particularly important.
In recent years, the prevention and treatment of diabetic nephropathy with traditional Chinese medicines have aroused wide attention of domestic and foreign experts.
5
In this study, the protective effect of CCPW on the renal tissue of diabetic rats was investigated. Rats in the normal group were in good spirits and moved agilely, and their hairs were shiny; those in the model group presented listlessness and acted slowly, and their hairs were dry and yellow; the general conditions of rats in CCPW-treated and losartan-treated groups were improved to some extent compared with those in the model group. As shown in Table 1, compared with that in the normal group, the body weight of rats decreased significantly (
Effects of
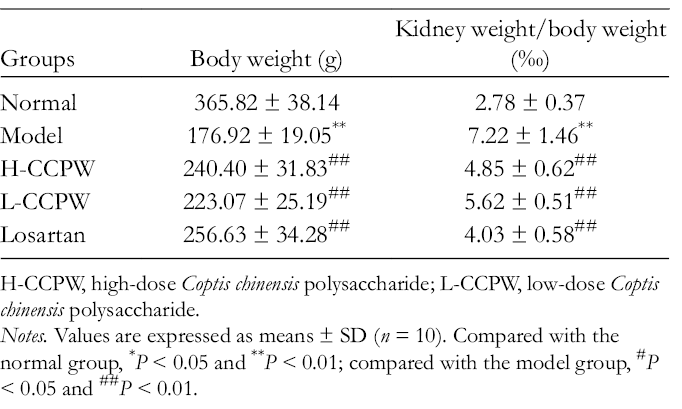
H-CCPW, high-dose
Compared with that in the normal group, the 24-hour urine protein content in the model group increased significantly (

Effects of
The kidney tissue structure of rats in the normal group was clear, without obvious pathological change; the vacuolar degeneration of renal tubular epithelial cells, glomerular sclerosis, and obvious hyperplasia of mesangial cells and matrix of rats were found in the model group; compared with those in the model group, the pathological changes were improved to some extent in H- and L-CCPW- and losartan-treated groups, as shown in Figure 2.

Effects of
Diabetic nephropathy is one of the most serious complications in patients with diabetes and its pathogenesis has not been fully clarified now.
10
A large number of studies have shown that oxidative stress is a key link in the pathogenesis of diabetic nephropathy, and some products with oxidative activity, such as autoxication glucose, glycosylated protein, prostaglandin, and polyols, significantly increased in the long-term hyperglycemia.
11
Xu et al
12
reported that Danshen injection could play a role in the improvement of diabetic nephropathy by lowering the oxidative stress level in the body, showing a potential benefit of the antioxidant treatment to diabetic nephropathy. SOD, CAT, GSH-Px, and MDA have been considered the main indexes to evaluate the antioxidant ability of body. SOD is one of the most important antioxidant enzymes to scavenge free radicals and can protect cells from the oxidative damage by scavenging O2−.
13
CAT is widely distributed in various tissues and can quickly remove the toxic metabolites in cells to protect the body.
14
GSH-Px can catalyze hydrogen peroxide to be decomposed into water and oxidized GSH (GSSG), thereby reducing the content of hydrogen peroxide in the body, to protect cells from the oxidative damage, and maintain the structural and functional integrity of the cells.
15
MDA is a product of lipid peroxidation and its level can reflect the extent of lipid peroxidation in the body.
16
Compared with those in the normal group, the SOD, CAT, and GSH-Px activities were significantly reduced (
Effects of

H-CCPW, high-dose
The role of inflammation in the occurrence and development of diabetic nephropathy has been closely watched, and the studies have shown that diabetic nephropathy is an inflammatory disease and chronic inflammation is the key factor for its sustained development.
17
TNF-α, IL-6, and hs-CRP contents are often high in patients with diabetic nephropathy. TNF-α is one of the main inflammatory cytokines released by macrophages and can act on other macrophages through an autocrine effect to activate more macrophages further; then, the activated macrophages can release a variety of proinflammatory mediators, leading to the progression of diabetic nephropathy.
18
IL-6 is a cytokine synthesized in fibroblasts, vascular endothelial cells, and activated monocytes, with a variety of biological effects, and can mediate various biological processes, such as inflammation, tissue damage and repair, and host defense, through affecting functions of the cellular immunity and humoral immunity; it also plays an important role in the acute inflammation and synthesis of C-reactive protein (CRP), and at the same time, is a main inflammatory factor to link the local vascular injury with the systemic immune response.
19
In hyperglycemia, IL-6 can promote the abnormal activation and excessive amplification of T and B cells, and the mesangial proliferation; IL-6 can induce the formation of CRP, and the increase of CRP content can further promote the adhesion of monocytes to endothelial cells, thus directly damaging the vascular endothelial cells and then amplifying the vascular injury caused by other inflammatory mediators.
20
As shown in Figure 3, compared with those in the normal group, serum TNF-α, IL-6, and hs-CRP expressions of rats in the model group increased significantly (

Effects of
The activation of JAK2/STAT3 signaling pathway plays an important role in the pathogenesis of diabetic nephropathy, and the hyperglycemia and glycosylated end products can activate the JAK2/STAT3 signaling pathway in diabetes.
21,22
The activated JAK2/STAT3 signaling pathway can further stimulate the synthesis of extracellular matrix and the proliferation of glomerular mesangial cells, eventually leading to the renal injury.
23
On the one hand, oxidative stress can activate the JAK2/STAT3 signaling pathway, the increased intracellular reactive oxygen and lipid peroxidation products in hyperglycemia can induce the phosphorylation of JAK2 and STAT3, thereby activating the JAK2/STAT3 signaling pathway.
24,25
On the other hand, JAK2/STAT3 signaling pathway is also the main mechanism of the mediation of the inflammatory response,
26
that is, JAK2/STAT3 signaling pathway is involved in the transcription and expression of multiple genes associated with the regulation of inflammation, cell proliferation, and fibrosis, thus increasing the expression of hs-CRP, IL-6, and TNF-α.
27,28
Studies have shown that some Chinese herbal medicines can delay the progression of kidney diseases in diabetic rats by suppressing the activation of JAK2/STAT3 signaling pathway.
29
As shown in Figure 4, compared with those in the normal group, p-JAK2 and p-STAT expressions in the renal tissue of rats in the model group increased, showing a significant difference (

Effects of
Losartan, an angiotensin Ⅱ receptor antagonist, has a good protective effect against the kidney injury caused by various causes. 30 Studies indicated that losartan had anti-oxidative and anti-inflammatory effects. 31 Wang et al 32 confirmed that losartan could reduce the expression of TGF-β1 by inhibiting the activation of JAK2/STAT3 signaling pathway, playing a role of antimyocardial interstitial fibrosis in rats with diabetic cardiomyopathy.3 4 Therefore, in this study, losartan was selected as a positive control drug to explore the protective effect of CCPW against the kidney injury, and its anti-oxidative and anti-inflammatory mechanism in diabetic rats. The antidiabetic effect of CCPW has been reported. Cui et al 33 confirmed that CCPW had the potential to become an antidiabetic drug because it can inhibit hyperglycemia and improve glucose resistance by increasing glucose uptake. The previous work of our research group also found that CCPW could play a role of anti-type 2 diabetes by reducing the oxidative stress level in the liver tissue of diabetic rats. 8,9 It was further found in this study that CCPW could also reduce the level of oxidative stress in the kidney of diabetic rats and inhibit the inflammatory response, so as to play the role of protection against the kidney injury of diabetic rats. However, the underlying mechanism needs to be further studied.
In conclusion, it is confirmed that CCPW should have a protective effect against the renal tissue injury of diabetic rats, and the effect might be associated with its inhibition on the oxidative stress and inflammation.
Experimental
Animals
Specific pathogen free (SPF) male Wistar rats (Laboratory Animal Center of Jilin University, China) were housed individually in cages at 20°C ± 1°C and in 40% to 70% humidity, subjected to 12 hours light/dark cycle with free access to food and water. The animal experiments were approved by the Institutional Animal Care and Use Committee of Changchun University of Chinese Medicine. All the experimental procedures were performed in accordance with the Regulations for the Administration of Affairs Concerning Experimental Animals approved by the State Council of People’s Republic of China.
Drugs and Reagents
Animal Modeling, Grouping, and Administration
The rats were intraperitoneally injected with STZ (60 mg/kg) to establish a rat diabetes model, and the modeling was regarded as successful when the blood sugar of rats was more than 16.7 mmol/L. According to their body weights, the rats that were successfully modeled were randomly divided into model group, H-CCPW group (300 mg/kg/day), L-CCPW group (100 mg/kg/day), and losartan group (30 mg/kg/day), 10 rats in each group; the other 10 healthy SD rats were randomly selected as normal group. On the second day after the success of modeling, all the rats were administered with the corresponding agents intragastrically once a day, successively for 8 weeks, and the rats in the normal group and model group were given equal volume of normal saline, respectively, in which the body weight and the general condition of rats were observed and recorded.
Determination of Urine Protein, and Serum Scr and BUN
Metabolic cages were used to collect the rats’ 24-hour urine and the urine protein in the 24-hour urine was determined by Coomassie brilliant blue G-250 method. After the administration for 8 weeks, the rats’ blood samples were collected through their abdominal aorta and the serum was separated; BUN and Scr levels in the serum were detected by an automatic biochemical analyzer.
Pathological Observation of Renal Tissue
The renal tissue was fixed in neutral formalin solution (4%), dehydrated by ethanol gradient, cleared with xylene, embedded with paraffin, and sectioned. The samples were stained by hematoxylin eosin (HE) staining for the observation of pathological changes of renal tissue.
Detection of SOD, CAT, and GSH-Px Activities and MDA Content in the Renal Tissue
After the administration for 8 weeks, the rats were killed and the kidney tissue was taken. An appropriate amount of the renal tissue was prepared into 10% kidney tissue homogenate with precooled normal saline. The homogenate was centrifuged at 3000 rpm for 5 minutes to obtain the supernatant and the supernatant was stored in −20°C refrigerator for use. According to the instructions of kits, SOD, CAT, and GSH-Px activities and MDA content in the renal tissue were detected.
Detection of TNF-α, IL-6, and hs-CRP Levels in the Serum
At 24 hours after the last administration, the blood of rats was collected from the rats’ femoral artery for the separation of serum. TNF-α, IL-6, and hs-CRP levels in the serum were detected by ELISA method according to the instructions of kits.
Detection of P-JAK2 and P-STAT3 Expressions in the Renal Tissue by Western Blot
An appropriate amount of the renal tissue was added into the tissue lysis buffer, the lysate was centrifuged at 3000 rpm for 5 minutes to obtain the supernatant, and the protein concentration in the supernatant was determined by bicinchoninic acid (BCA) method. A total of 10 µg protein of each sample was loaded on 12% sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) electrophoresis, and then the transfer membrane was performed; an appropriate amount of p-JAK2, JAK2, p-STAT3, and STAT3 polyclonal antibodies (diluted at a ratio of 1:300) was added onto the membrane after the blocking, respectively, and the membrane was incubated at 4°C overnight and then the second antibody was added onto it; after the chemiluminescence and development of X-ray film, the relative expression of target proteins was calculated according to the gray.
Statistical Analysis
SPSS 15 statistical software was used for the analysis of data and the data were expressed as mean ± SD. One-way ANOVA combined with post-hoc Tukey’s HSD test was used to compare the differences for individual group.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The authors are grateful to the support by Research Program of Jilin Provincial Administration of Traditional Chinese Medicine (No. 2019055), Jilin Province Health and Health Technology Innovation Project (No. 2018J110), and High Level Talent Fund of Changchun University of Traditional Chinese Medicine (No. 2018KJ15).
