Abstract
“Dietary behavior change in individuals with cardiovascular disease is recommended to modify risk factors, and is particularly relevant for individuals with a history of stroke.”
Introduction
An estimated 7.2 million American adults are community-dwelling stroke survivors, 1 most of whom experience secondary and chronic conditions, including overweight/obesity (70%), 2 type 2 diabetes (28-37%), 3 hypertension (58%), 2 and heart disease (75%). 4 Clinical guidelines put forth by the American Heart Association, 5 the American Diabetes Association, 6 and The Obesity Society 7 recommend at least 150 minutes of weekly moderate-intensity aerobic activity and following a healthy dietary pattern (e.g., DASH diet, Mediterranean diet) to manage these conditions among individuals with cardiovascular disease because physical activity and consuming a healthy diet, independent of each other, can result in cardiometabolic improvements in body composition, glucose and lipid metabolism, and blood pressure management.8-10
Despite the ample research that confirms the benefits of physical activity on cardiometabolic health among stroke survivors, 11 no systematic review has examined dietary behaviors, which we define as habitual and routine activities necessary for accessing, selecting, and preparing healthy foods for consumption, among stroke survivors. In contrast, published reviews have examined post-stroke nutritional status, nutritional supplementation, and nutritional insufficiency in response to swallowing difficulties, particularly among survivors in acute care and survivors within 6 months post-stroke.12-15 However, those findings do not generalize to community-dwelling survivors without swallowing difficulties and survivors more than 6 months post-stroke. Thus, there is an obvious knowledge gap regarding dietary behavior intervention and dietary outcomes among community-dwelling stroke survivors.
Recommended dietary patterns for stroke survivors include the DASH- and Mediterranean-type diets, both of which emphasize vegetable, fruit, and whole grain consumption.5,6 Despite clinical recommendations to follow a healthy dietary pattern, 52% of community-dwelling stroke survivors report consuming less than 1 fruit and 1 vegetable serving daily. 2 Additionally, >50% of community-dwelling survivors report functional disability, 16 including difficulty accessing and preparing healthy foods due to impairments affecting physical (e.g., balance, hemiplegia), cognitive (attention, memory) and psychological (fatigue, motivation) function.17,18 These stroke-related impairments make grocery shopping, preparing and cooking food, and following recipes difficult, which pose additional barriers to consuming healthy foods. Thus, stroke survivors need interventions that improve dietary behaviors, including adhering to healthy dietary patterns and overcoming functional barriers to accessing and preparing healthy foods.
Therefore, the purpose of this investigation was to identify studies that implemented dietary behavior interventions and reported dietary outcomes in community-dwelling adult stroke survivors, summarize dietary interventions and outcomes, and identify research gaps for future study. To achieve this purpose, we conducted a scoping review. A scoping review is a valid approach to evidence synthesis in circumstances where systematic reviews are not appropriate, and can be used to describe existing research approaches on specific topics and to identify knowledge gaps; 19 this approach is appropriate for achieving this investigation’s intended purpose. The knowledge gained from this review may be used to inform future dietary behavior intervention, research, and clinical practice, and improve the health and well-being of community-dwelling stroke survivors.
Methods
To perform this scoping review, we used the methodological framework proposed by Arksey and O’Malley (2005),
20
which consists of 5 phases: (1) identify the research question, (2) identify relevant studies, (3) select relevant studies, (4) chart data, and (5) collate, summarize, and report results. The research questions of interest were: 1. What are the characteristics of dietary behavior interventions for community-dwelling stroke survivors? 2. What dietary outcomes are measured? 3. What dietary outcomes were observed?”
We adhered to the PRISMA checklist for systematic reviews and meta-analyses extension for scoping reviews; the registered review protocol can be accessed online (https://osf.io/skdph).
Data Sources and Search Strategy
The search was conducted by the principal investigator (RRB) on January 1, 2021, through February 1, 2021, in the PubMed/MEDLINE (1966-present) database. Article titles were screened using the following search terms: (“stroke” or “stroke recurrence” or “recurrent stroke” or “stroke survivor” or “stroke survivors”) and (“secondary prevention” or “lifestyle intervention” or “lifestyle interventions” or “lifestyle” or “secondary” or “recurrence” or “recurrence prevention” or “health promotion” or “diet” or “dietary” or “fruit” or “vegetable”). The database searches were limited to English language articles dated between 2000 and 2021, and filtered to include only articles that report data from clinical trials, randomized controlled trials, and systematic reviews. A follow-up search was conducted on June 30, 2022, to identify additional articles published after the initial search between February 2021 and June 2022.
Article Selection Criteria and Process
Eligibility criteria for article consideration were selected a priori and included: (1) a study sample of community-dwelling stroke survivors, (2) study interventions must clearly address dietary behaviors, (3) a dietary outcome must be reported, and (4) articles must have been peer-reviewed. Articles without a dietary outcome, whose intervention focused on nutrient or food supplementation or medication management, or whose intervention indicated “health behavior” or “lifestyle modification” intervention without a clear mention of dietary intervention were excluded. The principal investigator screened the titles and abstracts of all articles identified by the database search. In situations where systematic reviews were consistent with the eligibility criteria, the individual studies identified within the systematic reviews were hand searched and screened for eligibility. All articles that passed the title and abstract screening were reviewed in full by the primary investigator. In cases where it was not clear if the article met all review criteria, another team member arbitrated.
Data Charting
A standardized excel form was developed to extract study characteristics such as publication year, study location, study sample and design, intervention content and format, intervention dose, and dietary outcome measures used. Where a randomized controlled trial (RCT) was conducted, the methodological quality was assessed using the Physiotherapy Evidence Database (PEDro) scale, which scores 10 items (score range: 0 to 10) and scores <6 are considered to have low methodological quality. 21 The Oxford Center for Evidence-Based Medicine 2011 Levels of Evidence was used to grade study design. 22 The principal investigator and another team member independently extracted study characteristics from articles that met eligibility criteria.
Data Analysis and Synthesis
The study team reviewed and synthesized data from the extraction charts to identify similarities and differences across selected studies and to identify research gaps relevant to dietary behavior intervention in community-dwelling stroke survivors.
Results
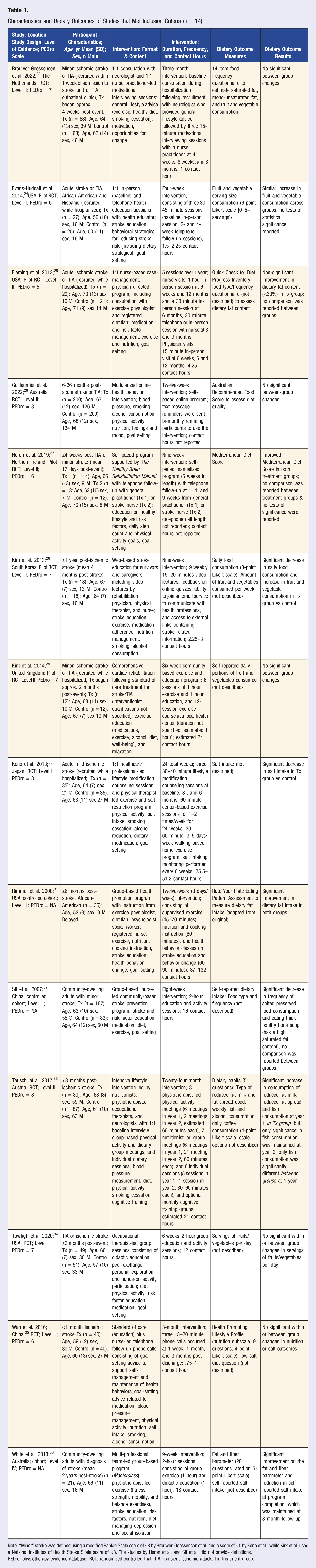
The search strategy resulted in 757 potentially relevant citations. Seven systematic reviews were included that produced an additional 97 individual citations, resulting in a total 854 citations. Following abstract and title screening and removal of the 7 systematic review citations, 740 citations were removed that did not pass the screening process and 47 duplicate citations identified across the systematic reviews were removed. Of the remaining 60 citations that underwent full review, 32 were excluded because no dietary behavior intervention was described. Fourteen additional citations were excluded that did not report a dietary outcome or the dietary behavior intervention was poorly described (see Supplementary Material Table for excluded studies). This resulted in 14 citations that met criteria for inclusion in this scoping review.23-36 The flow of citations through identification to final article selection is illustrated in Figure 1. The 14 included articles and abstracted study characteristics, intervention characteristics, dietary measures, and dietary outcomes are presented in Table 1 and summarized below. PRISMA flow diagram. Flow diagram illustrating the number of articles included and excluded at each step of the review process. Characteristics and Dietary Outcomes of Studies that Met Inclusion Criteria (n = 14). Note: “Minor” stroke was defined using a modified Rankin Scale score of ≤3 by Brouwer-Goossensen et al. and a score of ≤1 by Kono et al., while Kirk et al. used a National Institutes of Health Stroke Scale score of <3. The studies by Heron et al. and Sit et al. did not provide definitions. PEDro, physiotherapy evidence database; RCT, randomized controlled trial; TIA, transient ischemic attack; Tx, treatment group.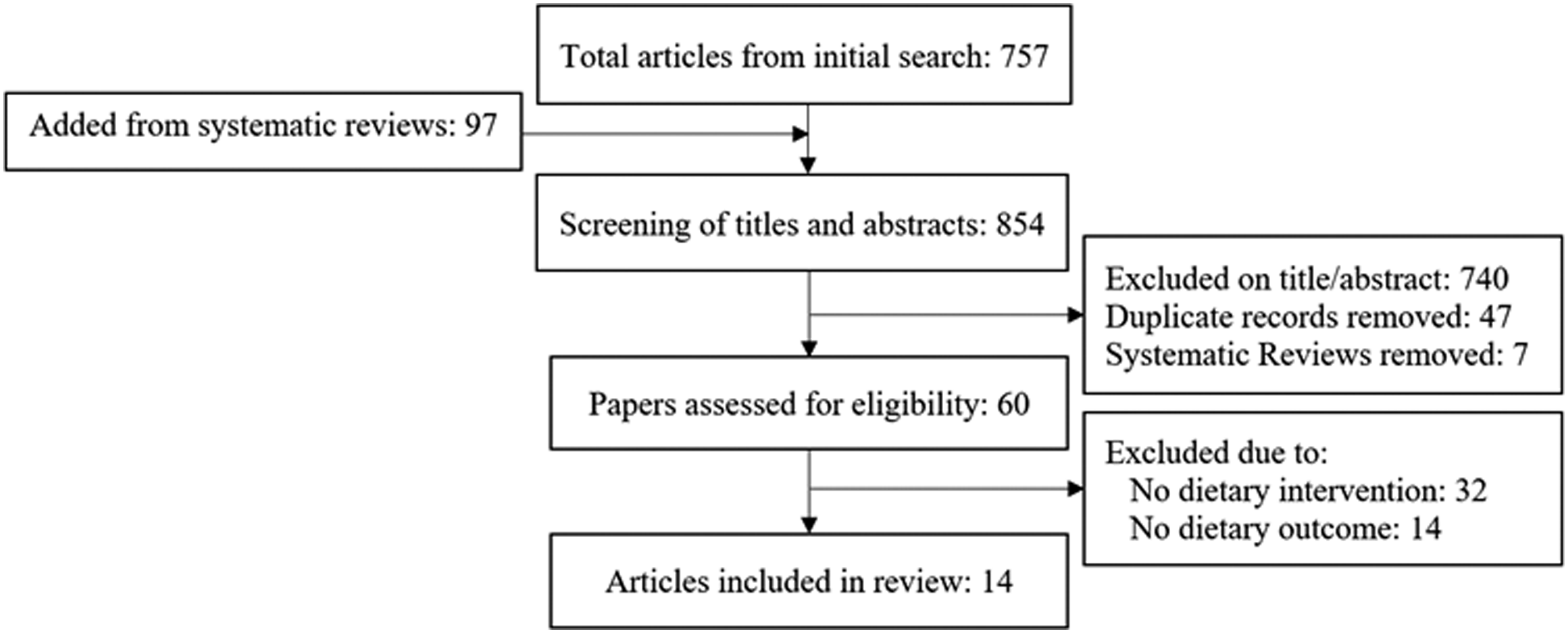
Study Characteristics
Location
Four studies were conducted in the United States, 4 studies were conducted in Asia (China, South Korea, Japan), 4 studies were conducted in Europe (Northern Ireland, United Kingdom, Austria, The Netherlands), and 2 studies were conducted in Australia.
Study design, level of evidence, and methodological quality
Eleven studies utilized a RCT (5 self-described as pilot trials, 6 non-pilot trials) design, 2 studies utilized a controlled cohort design (1 used a delayed treatment control group), and 1 study utilized an uncontrolled cohort design, which are consistent with Levels 2, 3, and 4, respectively, of the Oxford Center for Evidence-Based Medicine 2011 Levels of Evidence. 22 For the eleven RCTs, the PEDro scores for ten studies were ≥6, indicating good methodological quality. 21 Generally, studies lost points due to lack of participant blinding, lack of interventionist blinding, and absent or unreported group randomization.
Sample size
Sample sizes averaged 159 (range: 70–400) participants in the non-pilot RCTs and 32 (range: 24–52) participants in the pilot RCTs; sample sizes in the controlled cohort studies were 35 and 190 participants, and 21 participants were included in the uncontrolled cohort study. Treatment group sizes averaged 79 (range: 35–200) participants in the non-pilot RCTs and 18 (range: 12–27) participants in the pilot RCTs; treatment group sizes in the 2 controlled cohort studies were 35 (i.e., delayed treatment control group study) and 107 participants.
Participant Characteristics
Eligibility
Five studies limited recruitment to individuals with transient ischemic attack (TIA) or minor ischemic stroke, 4 studies limited recruitment to individuals with TIA or stroke without mention of stroke severity (2 studies limited entry to ischemic stroke, 2 studies did not specify stroke type), 3 studies limited recruitment to ischemic stroke only, and 2 studies did not specify stroke type or severity. The recruitment timeframe relative to stroke occurrence varied across studies: 5 studies recruited participants during their acute hospitalization, 6 studies recruited participants within 6 months post-stroke [i.e., ≤1 month (1 study), ≤3 months (2 studies)], ≥6 months (2 studies)], 1 study recruited participants ≤1 year, and 2 studies reported that community-dwelling stroke survivors were eligible to participate without specifying time since stroke. Only 4 studies reported the average time elapsed since stroke (i.e., 17 days, 2 months, 4 months, and 2 years).
Age, sex, and race
The average age of participants across studies was 64 (range: 50–71) years; the average age of participants was 50–59 years in 3 studies, 60–69 years in ten studies, and 70–71 years in 1 study. The average proportion of males across studies was 63% (range: 55%–83%); only 2 studies were predominantly female (58% and 74%). Only 3 US studies and 1 Australian study reported racial/ethnic demographic information; 2 studies were specifically intended for racial/ethnic minority groups (i.e., African-American and Hispanic), and 1 study occurred in a diverse demographic area (i.e., Los Angeles, California).
Intervention Characteristics
Description of interventions and interventionists
Six studies were self-described as stroke prevention programs, 5 studies as lifestyle intervention, and 1 study each as health promotion, stroke education, and comprehensive cardiac rehabilitation programs. Seven studies reported that interventions were led by multidisciplinary teams, including physicians, nurses, exercise physiologists, dietitians, physical therapists, and occupational therapists; 5 studies included more than 2 healthcare professionals while 2 studies included only 2 healthcare professionals. Five studies were led by a single healthcare professional; 2 of which were led by a nurse, 1 was led by a nurse or a physician; and 1 was led by an occupational therapist. The 1 remaining study did not specify the interventionist’s qualifications.
Format
Six studies provided treatment through in-person, group-based sessions, 1 of which also provided one-on-one sessions. Two studies provided treatment through an initial in-person session followed by telephone follow-up. One study strictly used telephone sessions to provide treatment. One study also provided treatment using in-person sessions, but group vs one-on-one treatment format was not specified. One study provided one-on-one treatment, but in-person vs telephone intervention was not reported. Three studies were self-paced interventions; 1 study utilized an intervention manual with telephone follow-up sessions and 2 studies utilized the internet to deliver educational sessions.
Content
All studies provided multimodal intervention, which addressed ≥2 behavioral risk factors for recurrent stroke. All studies addressed diet/nutrition (e.g., fruit, vegetable, salt, fat consumption; healthy dietary pattern), twelve addressed exercise/physical activity (e.g., aerobic physical activity, resistance training, balance), 6 addressed smoking cessation, 5 addressed medication management, and 5 addressed alcohol consumption. Additional intervention content included incorporating goal setting or action planning (7 studies) and utilizing hands-on learning activities (e.g., cooking demonstrations, grocery shopping; 3 studies).
Duration, frequency, and contact hours
Interventions ranged in duration from 4 weeks to 24 months [i.e., 4–8 weeks (4 studies), 9 weeks (3 studies), 12 weeks (1 study), 3 months (3 studies), 24 weeks, 12 months, and 24 months). Intervention sessions occurred approximately once weekly in 7 studies and 1 to 3 times per week in 2 studies. In the remaining 5 studies, frequency of intervention sessions occurred approximately monthly (3 studies), every 2 months (1 study), or was self-determined (1 study). The total number of intervention contact hours was approximately 1–12 hours in 6 studies, 16–24 hours in 4 studies, 25.5–51.2 hours in 1 study, and 87–132 hours in 1 study; contact hours were not reported in 2 studies.
Dietary Outcome measures and Results
Dietary outcome measures
Dietary-related assessment measures varied across studies, and all studies used self-report measures. Seven studies utilized a validated, standardized dietary assessment or diet-related questions from a standardized assessment. The other 7 studies used individual questions or food frequency questionnaires to describe dietary outcomes, however, these studies did not describe the sources from which questions were obtained.
Seven studies assessed general patterns of dietary consumption rather than consumption of specific food groups or dietary components (e.g., fat, salt). In contrast, fruit and vegetable consumption and salt intake were assessed in 4 studies each and fat intake was assessed in 2 studies.
Dietary outcome results
Improvement in dietary outcomes was reported in 8 studies. However, statistically significant between-group differences were reported in only 3 studies; among the 5 other studies, significant improvement in both treatment and control groups occurred in 2 studies, between group comparisons were not reported in 1 study, within and between groups comparisons were not reported in 1 study, and 1 study consisted of a single cohort so no between group comparison was possible. The remaining 6 studies reported no improvement in dietary behavior within or between groups.
Among the 8 studies that reported dietary improvement, 6 studies reported ≥16 contact hours, 4 reported improved patterns of dietary consumption, 3 reported improved salt intake; 2 reported improved fruit and vegetable consumption, and 1 reported improved fat intake.
Discussion
This scoping review identifies several knowledge gaps of the current stroke literature regarding dietary behavior interventions and how these interventions modify dietary outcomes. Below, we summarize these gaps and suggest considerations for future research.
Study Characteristics
The majority (11 of 14) of studies were RCTs. RCTs are the gold standard for studying causal relationships because randomization eliminates much of the bias inherent of other study designs, which could lead to consistent over- or underestimations of treatment effects. 37 The 3 remaining studies were non-randomized and of cohort design, 2 of which contained a control treatment group. A control group is necessary for limiting the possibility of bias and gaining a proper understanding of the true effects of an intervention. The pilot nature of several of the RCTs (smallest trial included 12 participants in the lifestyle intervention) also limits the ability to control for potential confounders important to the interpretation of dietary behavior interventions, including age, gender, culture, etc. Further, PEDro scores indicate that the majority of the RCTs were considered of good methodological quality. Overall, these data indicate that although the included studies may not have been adequately powered or controlled to evaluate the effect of the lifestyle intervention, they may be useful in planning future trials to assess the effects of dietary behavior interventions in stroke survivors.
Participant Characteristics
Important participant characteristics (i.e., stroke type, severity, and latency) were not reported by most studies, making the ability to accurately compare studies and interpret study results difficult. Several studies restricted recruitment to TIA or minor ischemic strokes, which limits the generalizability to more severe ischemic stroke or those of hemorrhagic origin. Similarly, there was an over-representation of interventions with eligibility limited to the acute stroke recovery phase (<6 months post-incident), and even among the 5 studies with eligibility to include survivors with chronic stroke (≥6 months), 1 study had a mean stroke latency of <6 months. Overall, only 4 studies specifically reported the mean time elapsed since stroke.
Additional participant-relevant characteristics to consider include sex, age, and race. Not surprisingly, males made up the majority of participants and the majority of studies included subjects between the ages of 50–70 years, bringing into question whether results generalize to younger and older participants and females. Further, the geographic area and race/ethnicity represented in these studies was diverse, limiting the ability to determine whether the interventions findings are applicable across all groups of stroke survivors. Only 1 article specifically examined dietary patterns specific to a particular culture, where patients in China were asked about their “consumption of preserved food, cooking methods, additional sauce-serving at meals, eating food with high saturated fat content, etc.” 32 The heterogeneous nature of the reviewed studies with regard to participant characteristics limits the ability to generalize results universally across all populations of stroke survivors.
Intervention Characteristics
Every intervention was multimodal in nature. Though there is a benefit of targeting numerous aspects of unhealthy lifestyle behaviors, it limits the ability to fully understand the direct benefits of dietary behavior intervention. Furthermore, details on the dietary behavior intervention content provided to participants was vague in most studies, with only 1 study specifically including an intervention target for salt intake. 30 This is surprising because studies suggest that 12–41% of stroke survivors are at risk for malnutrition at 6 months and 11% at 16–18 months post-stroke, with limited data beyond the first 2 years after stroke; 12 thus, interventions that include education for meeting specific dietary goals may be important for maintaining a healthy nutritional status in survivors. Only a quarter of interventions included hands-on skill building, which may be especially important in stroke survivors considering the high prevalence of functional disability in survivors due to physical and cognitive impairment that may impede the ability to independently perform dietary behaviors such as grocery shopping and meal preparation.
The interventions, in general, lacked individualization in that all study participants were provided the same dietary information, despite one-third of studies specifying that various components of the intervention were delivered in a 1:1 format. The importance of individualized or personalized dietary advice is becoming increasingly recognized, with dietary strategies varying according to the individual’s personal goals, food preferences, food skills, budget, and food availability. 38 Most interventions were delivered by a multidisciplinary healthcare team, but only 3 studies reported inclusion of a dietitian/nutritionist, therefore, it is unclear whether the study interventionists had the necessary training to provide dietary advice specific to stroke survivors.
There are no clear recommendations regarding intervention dose (frequency*duration) of dietary interventions for stroke survivors. Guidelines for comprehensive lifestyle intervention from the American Heart Association for weight loss among individuals who are overweight or obese recommend that lifestyle interventions should be delivered in at least 14 sessions (i.e., contact hours) over 6 months, incorporate behavior change strategies, and target increased physical activity and reduced calorie intake. 7 If this dose recommendation is considered, only 6 studies met the criterion for contact hours and only 2 studies met the criterion for duration. Of note, half of the studies utilized goal setting and action planning strategies, which are evidence-based behavior change techniques 39 (i.e., behavioral strategies).
Given the variability in intervention characteristics (content, interventionist discipline, contact hours, and duration) and lack of a unimodal dietary behavior intervention, there is no clear implication regarding how interventions should be structured. However, it is noteworthy that most studies utilized multidisciplinary teams and half of the studies reported >14 contact hours and utilized behavioral strategies. Additional research is needed to clarify necessary intervention components for achieving dietary behavior change in stroke survivors.
Dietary Outcome Measures and Results
Only 7 of the studies reported utilizing validated dietary assessments or questions from validated assessments, while the remaining studies did not report the sources from which dietary measure were obtained. Further, all studies utilized self-reported dietary outcome measures. Considering that ∼83% of stroke survivors show some degree of cognitive impairment, 40 the accuracy of previously validated assessments and self-reported outcome measures is unknown. This likely suggests that self-reported dietary outcomes need to be validated for this particular patient population, and more objective measures of dietary assessment may be needed to accurately assess dietary behaviors in stroke survivors.
The outcomes assessed were also heterogeneous, with some focusing on changes in general dietary patterns, and others examining specific food groups or patterns (i.e., fruit and vegetable, salt or fat intakes). Previous studies suggest that suboptimal nutritional status of several key nutrients in stroke survivors, 12 including an excess caloric intake, reduced protein intake, and micronutrient deficiencies (particularly the B-vitamins, vitamin D, and omega 3 fatty acids), may have deleterious effects on metabolic, physical, and psychological functioning in stroke survivors. 12 As such, it appears that a more comprehensive evaluation of dietary behaviors—including dietary intake—in stroke survivors is needed.
Eight studies reported improvements in dietary outcomes. In general, improvements in dietary behaviors were observed across most outcomes: 80% of studies examining general dietary patterns, 75% examining salt intake, 50% examining fruit and vegetable intake, and 50% examining fat intake. However, statistically significant between-group differences were only reported in 3 studies. It should be noted that many of the pilot trials did not detect an effect of the intervention on dietary outcomes, which could possibly be because they did not control for important confounders. Similarly, the variability across intervention components (including frequency and duration) and the choice of outcome assessment with its corresponding psychometric properties (validity, reliability, responsiveness to change) also likely influence the ability to detect an intervention effect.
Directions for Future Research
Considerations for Future Study Design and Reporting.
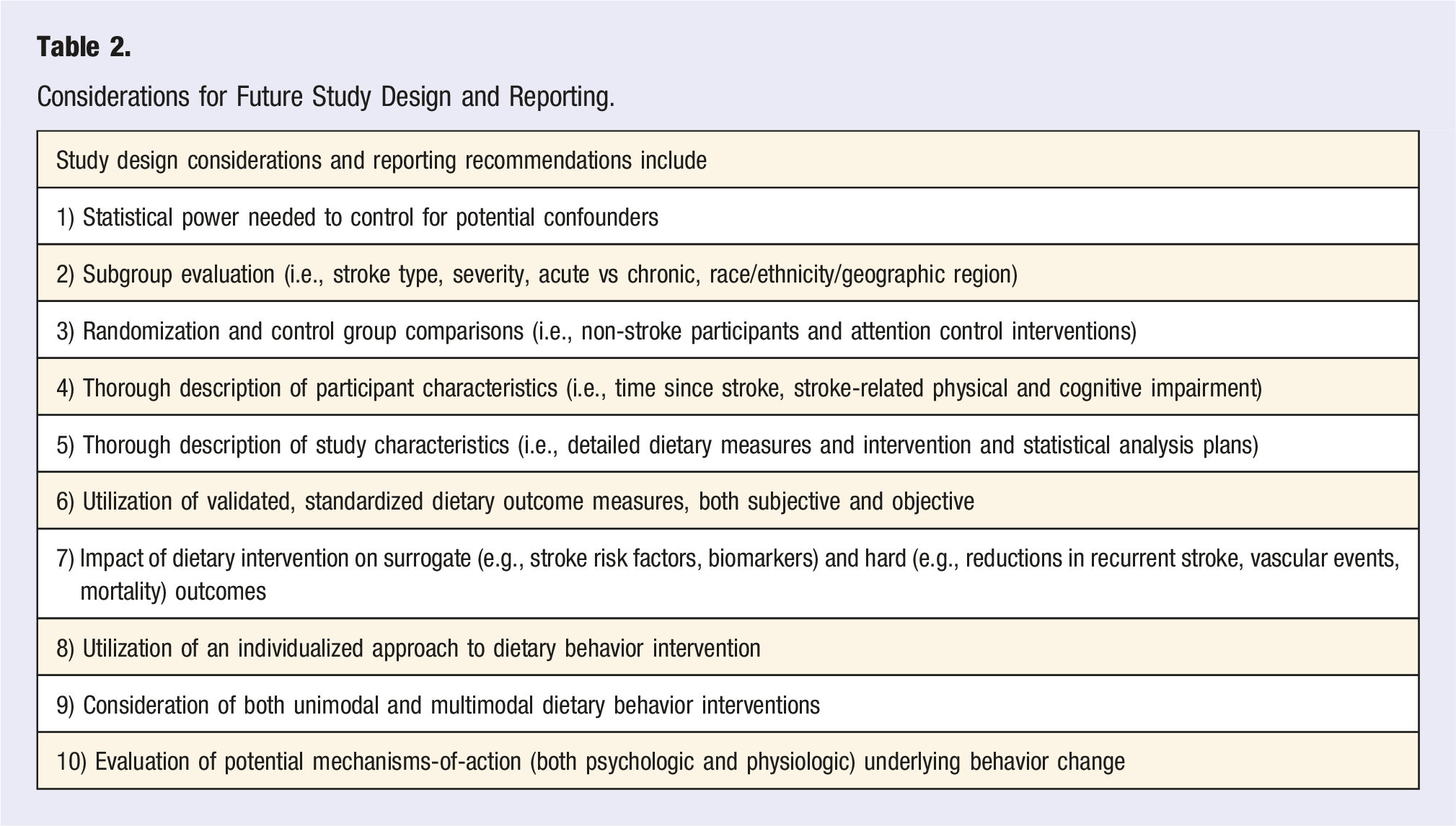
The use of validated, standardized dietary outcome measures is needed in future trials. In patients without cognitive impairment, a 24-hour recall, which when administered by a trained interviewer, is considered the gold standard for dietary assessment. It is suggested that error in recalls can be further reduced by incorporating standardized quality-control procedures (i.e., multiple pass method) and collecting more than one 24-hour recall per person. 41 However, the addition of objective diet measures may be needed when the ability to accurately recall is in question. The addition of doubly labeled water may provide a reference method for evaluating validity of self-reported energy intake in relatively weight stable individuals. Further, technology is allowing for innovative ways to objectively and accurately assess dietary intake, including using digital images and bar-code scanners. 42 In addition to assessing improvement in dietary behaviors, dietary behavior interventions should also include surrogate outcomes (e.g., stroke risk factors, biomarkers) and hard outcomes (e.g., occurrence of recurrent stroke, vascular events, mortality) to assess the impact of dietary intervention on important clinical outcomes of interest.
Finally, the effect of dose (frequency*duration) on outcomes also needs to be explored. While comprehensive lifestyle intervention guidelines recommend 14 sessions over at least 6 months and the use of behavior changes strategies for weight loss among overweight and obese individuals, 7 these guidelines may not be appropriate for dietary behavior change among stroke survivors. A different dose may be required to modify dietary behaviors in stroke survivors because interventions likely need to train survivors how to overcome stroke-related physical and cognitive impairment that make engaging in dietary behaviors challenging.
Limitations
These considerations and recommendations should be considered in light of limitations and strengths of this scoping review. This review utilized only 1 database, PubMed, for searches. However, because the majority of included articles appeared multiple times in various systematic reviews, it bolsters our confidence that our list is comprehensive and includes relevant articles. The principal investigator performed the article search and screening processes, which is not an uncommon practice given that only 1 reviewer completes these processes in 75–80% of scoping reviews; 43 importantly, predefined inclusion/exclusion criteria facilitated an objective review process. Further, data charting was independently completed by 2 team members using a standardized form to promote accuracy of extracted data, and data analysis and synthesis were performed by the entire study team promoting validity of findings via triangulation 44 across team members. Finally, 14 studies with a known dietary behavior intervention were excluded from this scoping review because they did not meet eligibility criteria. The study and intervention characteristics in those studies (see Supplementary Material Table) did not differ substantively from the characteristics of the included studies such that their exclusion does not affect the findings and future directions reported in this scoping review.
Conclusions
Dietary behavior change in individuals with cardiovascular disease is recommended to modify risk factors, and is particularly relevant for individuals with a history of stroke. Furthermore, secondary stroke prevention guidelines specifically recommend that stroke survivors follow a healthy dietary pattern to reduce recurrent stroke risk; however, there currently are no clear practice standards for dietary behavior intervention post-stroke. Due to a lack of such standards, dietary behavior interventions and outcomes vary across studies and settings, which impedes the ability to conduct meta-analyses of outcomes to inform research knowledge and clinical practice. This scoping review provides several directions for future research to improve the design and testing of dietary behavior interventions and reporting of interventions and their outcomes. Most importantly, however, this review provides support for the efficacy of dietary behavior intervention among community-dwelling stroke survivors, which is important for promoting the health and well-being of this health-disparate population.
Supplemental Material
Supplemental Material - Evidence Surrounding Dietary Behavior Interventions in Community-Dwelling Stroke Survivors: A Scoping Review
Supplemental Material for Evidence Surrounding Dietary Behavior Interventions in Community-Dwelling Stroke Survivors: A Scoping Review by Ryan R. Bailey, Alfonso L. Neri, and Monica C. Serra in American Journal of Lifestyle Medicine
Footnotes
Author’s Note
Data were previously presented as a poster at the American Heart Association EPI|Lifestyle Scientific Sessions 2022 in Chicago, IL, March 2022.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
