Abstract
Background:
Short-lasting hyperglycaemia occurs frequently in prediabetes and poorly controlled diabetes mellitus leading to vascular damage. Pituitary adenylate cyclase-activating polypeptide (PACAP) has been shown to play a protective role in vascular complications of diabetes; moreover, antioxidant effects of PACAP were also described. Therefore, we hypothesized that PACAP exerts protective effects in short-term hyperglycaemia-induced vascular dysfunctions.
Methods:
After short-term hyperglycaemia, acetylcholine-induced and sodium nitroprusside–induced vascular relaxation of mouse carotid arteries were tested with a myograph with or without the presence of PACAP or superoxide dismutase. Potential direct antioxidant superoxide-scavenging action of pituitary adenylate cyclase-activating peptide was tested with pyrogallol autoxidation assay; furthermore, the effect of pituitary adenylate cyclase-activating peptide or superoxide dismutase was investigated on hyperglycaemia-associated vascular markers.
Results:
PACAP administration resulted in reduced endothelial dysfunction after a 1-h hyperglycaemic episode. PACAP was able to restore acetylcholine-induced relaxation of the vessels and improved sodium nitroprusside–induced relaxation. This effect was comparable to the protective effect of superoxide dismutase, but PACAP was unable to directly scavenge superoxide produced by autoxidation of pyrogallol. Endothelial dysfunction was associated with elevated levels of fibroblast growth factor basic, matrix metalloproteinase 9 and nephroblastoma overexpressed gene proteins. Their release was reduced by PACAP administration.
Conclusion:
These results suggest a strong protective role of PACAP in the vascular complications of diabetes.
Keywords
Introduction
Diabetes mellitus is the most frequent cause of severe vascular disorders worldwide. 1 Prediabetes and poorly controlled diabetes mellitus are characterized by frequent hyperglycaemic episodes. Large clinical trials have confirmed that strict blood glucose control shows strong correlation with a reduction in the vascular complications of diabetes.2,3 In a new longitudinal study, cardiovascular burden was associated with higher fasting plasma glucose values. 4 Even a short-term hyperglycaemia is able to cause endothelial dysfunction of the vascular wall of healthy subjects5,6 or of diabetic patients. 7 Therefore, investigation of potential mediators that are able to prevent hyperglycaemia-induced vascular dysfunctions is of major importance.
Pituitary adenylate cyclase-activating poly peptide (PACAP) discovered in 1989 8 is a neuropeptide with two biologically active forms, PACAP1-38 (dominant form) and PACAP1-27. Due to high structural similarity between PACAP and vasoactive intestinal peptide (VIP), PACAP is classified as a member of the VIP-secretin-growth hormone–releasing hormone (GHRH)-glucagon superfamily.9,10 PACAP exerts its effects through G protein-coupled receptors, namely, through the PACAP-specific PAC1 receptor, and through the VPAC1/VPAC2 receptors, which transmit the effects of both PACAP and VIP. PACAP has been remarkably conserved throughout evolution indicating essential roles of the peptide. In the vasculature, these receptors are mainly found in the smooth muscle cells of arteries and arterioles but are also expressed on the endothelial cells.9,11 Previously, PACAP has been shown to play a protective role in various diabetic complications such as diabetic nephropathy 12 or retinopathy. 13 Minor direct antioxidant effects of PACAP were found only in high concentrations in an in vitro system, 14 but PACAP is able to increase the antioxidant capacity after injuries. 14 For example, PACAP enhanced antioxidant activity in traumatic brain injury in mice. 15 In intestinal ischemia/reperfusion, PACAP treatment decreased malondialdehyde levels (an indicator of oxidative stress), while it increased that of superoxide dismutase (SOD) and reduced glutathione. 16 In addition, a decrease in the biological antioxidant potential has been described in PACAP-deficient mice during ageing or in relation with tissue injury, indicating the role of endogenous PACAP in increasing the antioxidant capacity.17,18
PACAP plays direct protective effects on endothelial cells. In cell cultures, it has been shown that PACAP protects against oxidative stress and enhances the barrier properties of cerebral microvessel endothelial cells.19,20 Therefore, PACAP could be a potentially protective peptide regarding vascular complications of diabetes, which vascular dysfunctions are, at least partially, caused by oxidative stress. 19
In this study, we hypothesized that PACAP exerts protective effects in hyperglycaemia-induced dysfunctions in relaxation of carotid arteries. Both endothelium-dependent and endothelium-independent vasodilation ability of the vessels were tested following 1-h incubation with high-glucose (HG) solution. We also investigated the protective effect of PACAP on vascular dysfunction caused by this HG stress. For positive control, we applied both SOD and catalase (CAT), as SOD is an enzyme responsible for converting the free radical superoxide anion into hydrogen peroxide, which is then neutralized by CAT into water. We also aimed to analyse underlying mechanisms of PACAP-induced protection. Therefore, in addition to vasomotor experiments, potential direct antioxidant actions of PACAP were tested in vitro with spectrophotometry. Diabetic hyperglycaemia promotes vascular complications with abnormal angiogenesis. 21 It has been suggested that vascular dysfunction coinciding with elevated levels of many angiogenic growth factors may point to their malfunctioning due to oxidative stress and/or protein glycation at the factor and the receptor levels. Therefore, the effects of PACAP on hyperglycaemia-associated angiogenic vascular markers were also measured with protein array analysis.
Methods
Animals
The 8- to 10-week-old male mice on Balb/C background (total n = 31) from the Colony of the Department of Immunology and Biotechnology of the Medical School, University of Pecs, Hungary, were used in this study. Mice weighed 26.75 ± 0.44 g at the day of the experiment. In all experimental interventions and procedures, both the general regulations and the special rules of the permit obtained from the University of Pecs Ethical Committee for the Protection of Animals in Research (BA02/2000-15024/2011) were strictly followed. All procedures were in accordance with the main directives of the National Ethical Council for Animal Research and those of the European Communities Council (86/609/EEC, Directive 2010/63/EU of the European Parliament and of the Council).
Surgery
Common carotid arteries were isolated using a surgical microscope (Olympus SZX7; Olympus, Inc., Japan) under anaesthesia induced by intraperitoneal 81.7 mg/kg ketamine and 9.3 mg/kg xylazine administration (ketamine: Gedeon Richter Plc., Budapest, Hungary, xylazin: Eurovet Animal Health B.V., Bladel, The Netherlands). The proximal and distal ends of the isolated vessel segments were ligated; the vessel was excised between the ligations and then transferred to refrigerated Krebs solution. Carotid arteries from both sides were used. From one mouse, four vessel rings were obtained. After the removal, mice were sacrificed with an intraperitoneal injection of pentobarbital (100 mg/kg; Ceva Sante Animale, Libourna, France).
Measurement of isometric force of isolated arteries
After removal of the vessel segments, they were quickly transferred into ice-cold (~4°C) physiological Krebs solution [NaCl: 119 mM, KCl: 4.7 mM, KH2PO4: 1.2 mM, NaHCO3: 25 mM, Mg2SO4: 1.2 mM, CaCl2 × 2H2O: 1.6 mM, ethylenediaminetetraacetic acid (EDTA): 0.026 mM, glucose: 11.1 mM]. NaCl and KCl were obtained from VWR International (Radnor, PA). All other chemicals and drugs were purchased from Sigma–Aldrich (St Louis, MO). The arteries were dissected into 2-mm-long rings. Each vessel ring was positioned between two tungsten wires in the organ chamber of the myograph in 5-mL Krebs bath solution. The diameter of the wire was 0.04 mm. The bath solution was continuously oxygenated with a gas mixture of 95% O2 and 5% CO2 (Linde, Repcelak, Hungary) and kept at 36.9°C ± 0.1°C during the whole experiment.
Isometric contraction forces were measured with a four-chamber system, a DMT 610M Wire Myograph (Danish Myo Technology, Aarhus, Denmark). LabChart 8 (AD Instruments, Dunedin, New Zealand) and Myodaq 2.01 (Danish Myotechnologies, Denmark) software were used for data acquisition and display. Before the start of the experiment, normalization was performed on the vessel rings with the Myodaq 2.01 software (Danish Myo Technology A/S) according to Mulvany and Harpern, 22 and to our previous study, 23 and then the rings were allowed to stabilize for 60 min.
Pharmacological agents and experimental protocol
As shown in Figure 1, at the beginning of the experiments, the functional integrity of the vessels was verified with viability tests. To study the endothelium-dependent [acetylcholine (Ach)-induced] and endothelium-independent [sodium nitroprusside (SNP)-induced] relaxation ability of the vessels, first the vessels were pre-contracted with 60 mM KCl. When the contraction reached the plateau phase, 50 µL of increasing doses of either Ach or SNP were administered to the bath solution to reach final concentrations of 10−9 to 10−5 M. After this viability test, the chambers were washed out before a 1-h incubation period with Krebs solution. For the four vessel rings obtained from the same mouse, we used four different incubation solutions: (1) a control Krebs solution, (2) a Krebs solution containing 30 mM glucose, (3) a solution where 10−8 M PACAP1-38 was administered to the Krebs solution containing 30 mM glucose and (4) a solution where combination of SOD and CAT (120 and 200 U/mL, respectively) was administered to the Krebs solution containing 30 mM glucose. PACAP1-38 was always administered twice during the incubation period: one dose at the beginning of the incubation period to reach a final concentration of 10−8 M and another similar one after 30 min.
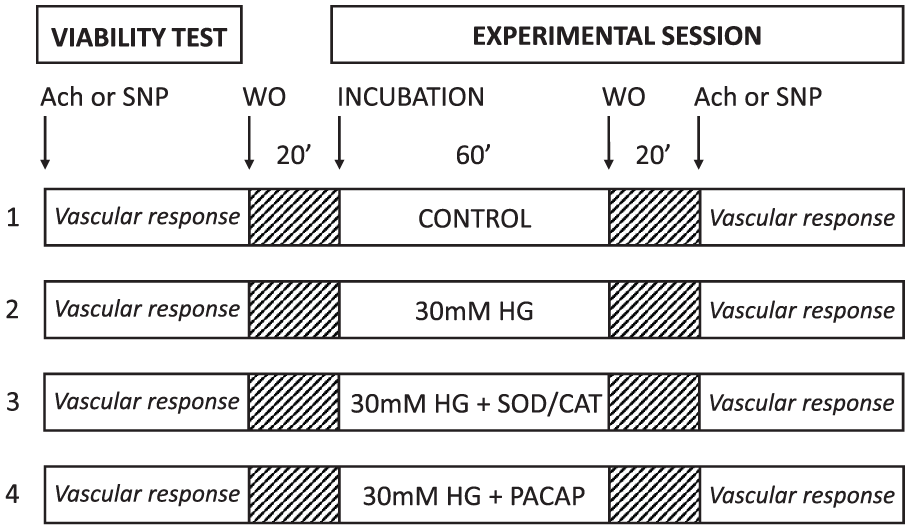
Demonstration of our experimental protocol. Vascular responses of carotid arteries investigated in several sets of experiments. In all cases, a viability test was performed before starting an experimental session. We used four different incubation solutions: CONTROL – a control Krebs solution, 30 mM HG – a Krebs solution containing 30 mM glucose, 30 mM HG + SOD/CAT – a solution where combination of SOD and CAT (120 and 200 U/mL, respectively) was administered to the Krebs solution containing 30 mM glucose, 30 mM HG + PACAP – a solution where 2 × 10−8 M PACAP1-38 was administered to the Krebs solution containing 30 mM glucose and WO – washout.
Following the incubation, the four chambers were washed out again with fresh Krebs solution. During the measurement period, vascular responses of the vessels were tested again in a similar fashion as described above. Thus, we verified that no change in vascular responsiveness developed due to the 1-h control incubation. After the administration of each dose of a specific substance, the isometric force was registered.
All drugs were dissolved in distilled water. When only the solvent (distilled water) was applied, there was no significant change in isometric force. In the beginning of the incubation period, vessels of the control group received also 50 µL of distillated water.
Calculations
Changes in the relaxation activity were calculated according to the following formula: (Fdrug/Fmax) × 100, where Fdrug is a force obtained with the vasorelaxant agent (Ach or SNP), and Fmax is maximal vasoconstriction obtained with 60 mM KCl in that specific group. Calculations were made separately for each administered drug (and dose) and group of mice.
Measuring direct superoxide-scavenging activity of PACAP
Both the classic 24 (at pH 8.2) and the improved 25 (pH is modified to physiological pH 7.4) pyrogallol autoxidation methods were used to determine superoxide-scavenging activity of PACAP. Pyrogallol can autoxidize in solutions to produce superoxide anion radicals. The reaction is detected by a spectrophotometer; the absorbance reflects the generation of superoxide radicals, where lower absorbance indicates higher inhibition of radicals.24,25 Absorbance changes were measured by spectrophotometry (JASCO V630). For the classic assay, 200 µM pyrogallol was dissolved in 50 mM Tris-HCl buffer at pH 8.20 with 1 mM Na2EDTA. Rate of auto-oxidation was determined from the changes in absorbance measured at 420 nm (A420). For the improved assay 250 µM pyrogallol of a 60 mM pyrogallol solution (dissolved in 1 mM HCl) was mixed right before the measurement with 50 mM Tris-HCl buffer containing 1 mM Na2EDTA at pH 7.4, and A325 is measured. Both assays were performed at room temperature (24°C). Inhibition of the absorbance changes was measured after the administration of different doses of PACAP1-38 (2 × 10−8, 10−7, 10−6 and 10−5 M) to the pyrogallol solution. The initial dose was chosen based on our prior functional experiments and then we increased the dose to reveal any possible superoxide-scavenging effect of PACAP.
Angiogenesis-related protein array analysis
To examine the change in angiogenesis-related protein levels, arteries were collected after using the protocol of 1-h incubation and washout without administration of any vasoactive substances. The arteries were then transported to −70°C. For the measurement, proteins were investigated from pooled tissue homogenates by semi-quantitative mouse angiogenesis array kit (R&D Systems, Biomedica, Budapest, Hungary), which can detect expression levels of 53 mouse angiogenesis-related proteins. In these arrays, the sample proteins bind to selected captured antibodies spotted on nitrocellulose membranes. The kits contain all buffers, detection antibodies and membranes necessary for the measurement. The arrays were performed as described by the manufacturer’s protocol. Expression of proteins was measured in all four groups. We used two mice per group and eight mice for one microarray measurement. For both measurements, 16 mice were used. The samples were homogenized in phosphate-buffered saline with protease inhibitors. The nitrocellulose membranes were blocked for 1 h and incubated with reconstituted detection antibody cocktail at room temperature for another 1 h. The membranes were incubated overnight with tissue homogenates containing 200 µg/mL of proteins. After washing with buffer 3 times and adding streptavidin-horseradish peroxidase to each membrane, the plates were spread to a chemiluminescent detection reagent (Amersham Biosciences, Hungary). The membranes were placed facing up to an X-ray film cassette. Developed films were scanned and analysed by densitometry using the Image J software. The array was repeated 2 times and then averaged.
Statistical analysis
All data were collected as single-point measurement, across different groups and doses. Comparison of groups was performed by two-way analysis of variance (ANOVA), while protein array was analysed with one-way ANOVA [post hoc – Fisher least significant difference (LSD)]. Analyses were performed using Sigma Plot 12.5 (Systat, Chicago, IL). Differences were considered to be significant when p values were <0.05. All data are given as mean ± standard error of the mean (SEM).
Results
Protective effect of PACAP1-38 against HG stress regarding Ach- and SNP-induced vascular relaxation
Endothelium-dependent relaxation was tested with the administration of cumulative doses of Ach (Figure 2). As expected, HG incubation reduced the endothelium-dependent Ach-induced relaxation of the vessels (p < 0.05, HG vs control at 10−7–10−5 M). The addition of PACAP1-38 to the HG incubating solution restored vasorelaxation (p < 0.05, HG + PACAP1-38 vs HG at 10−6–10−5 M). Application of SOD/CAT could also restore Ach-induced relaxation impaired by HG (p < 0.05, HG + SOD/CAT vs HG at 10−6–10−5 M). Administration of both PACAP1-38 or SOD/CAT restored relaxation properties to levels corresponding to control (p > 0.05, HG + PACAP1-38 and HG + SOD/CAT vs control).
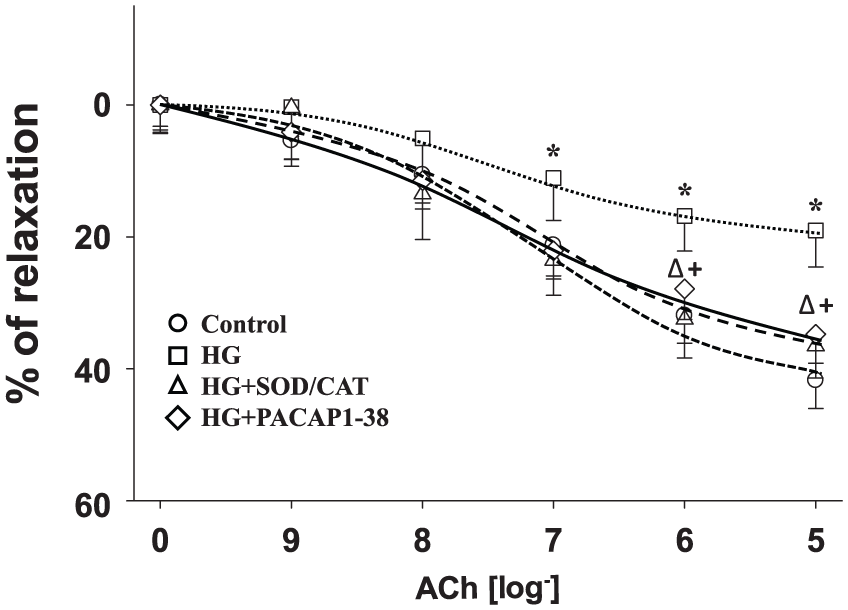
Ach concentration–response curves of isolated carotid arteries after 1-h incubation with a control Krebs solution (Control) or a Krebs solution containing 30 mM glucose (HG) or a solution where combination of SOD and CAT (120 and 200 U/mL, respectively) was administered to the Krebs solution containing 30 mM glucose (HG + SOD/CAT) or a solution where 2 × 10−8 M PACAP1-38 was administered to the Krebs solution containing 30 mM glucose (HG + PACAP1-38).
Endothelium-independent relaxation was tested by SNP administration (Figure 3). HG incubation reduced the endothelium-independent SNP-induced relaxation of the vessels (p < 0.05, HG vs control at 10−8–10−5 M). Both SOD/CAT (p < 0.05, at 10−6–10−5 M) and PACAP1-38 (p < 0.05, at 10−7–10−5 M) improved SNP-induced relaxation response compared to HG; however, relaxation was still significantly reduced compared to control (p < 0.05, SOD/CAT and PACAP1-38 vs control, at 10−6–10−5 M).
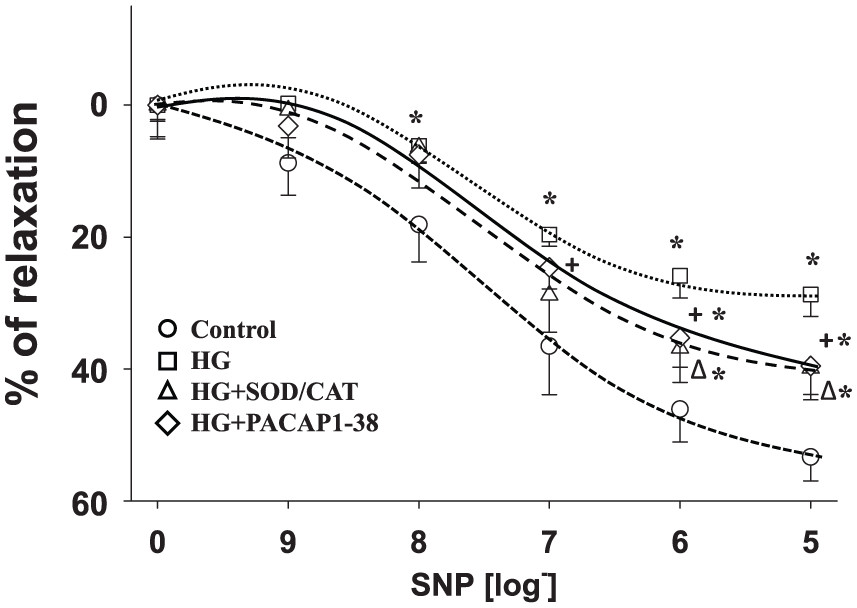
SNP concentration–response curves of isolated carotid arteries after 1-h incubation with a control Krebs solution (Control) or a Krebs solution containing 30 mM glucose (HG) or a solution where combination of SOD and CAT (120 and 200 U/mL, respectively) was administered to the Krebs solution containing 30 mM glucose (HG + SOD/CAT) or a solution where 2 × 10−8 M PACAP1-38 was administered to the Krebs solution containing 30 mM glucose (HG + PACAP1-38).
Superoxide-scavenging effect of PACAP1-38
PACAP1-38 was not effective at inhibiting changes in absorbance at pH 8.2 (data not shown). At pH 7.4, absorbance change was 1.77 ± 0.042 after 5 min in the control condition. Administration of 2 × 10−8, 10−7, 10−6 or 10−5 M PACAP1-38 was not able to change absorbance significantly (at pH 7.4, the changes in absorbance were 1.78 ± 0.054, 1.79 ± 0.073, 1.77 ± 0.038 or 1.73 ± 0.012 for 2 × 10−8, 10−7, 10−6 or 10−5 M PACAP1-38, respectively). Both techniques of superoxide-scavenging assay showed that PACAP1-38 in the observed concentrations is unable to scavenge superoxide produced by autoxidation of pyrogallol.
Effect of PACAP1-38 on the HG-induced rise of angiogenesis markers
To assess the underlying mechanisms of the above-described protective vascular effects of PACAP1-38, we used angiogenesis array kit. In total, 11 proteins were expressed in the vessels, namely, angiopoietin-1 (Ang-1), tissue factor, fibroblast growth factor (FGF) acidic, FGF basic, matrix metalloproteinase 9 (MMP-9), osteopontin, stromal cell–derived factor 1 (SDF-1), endostatin, nephroblastoma overexpressed gene (NOV), platelet factor 4 and serpin E1 (Figures 4 and 5). FGF basic (p = 0.012 HG vs control), MMP-9 (p = 0.003 HG vs control) and NOV (p = 0.032 HG vs control) reacted with a rise to the 1-h HG exposure.
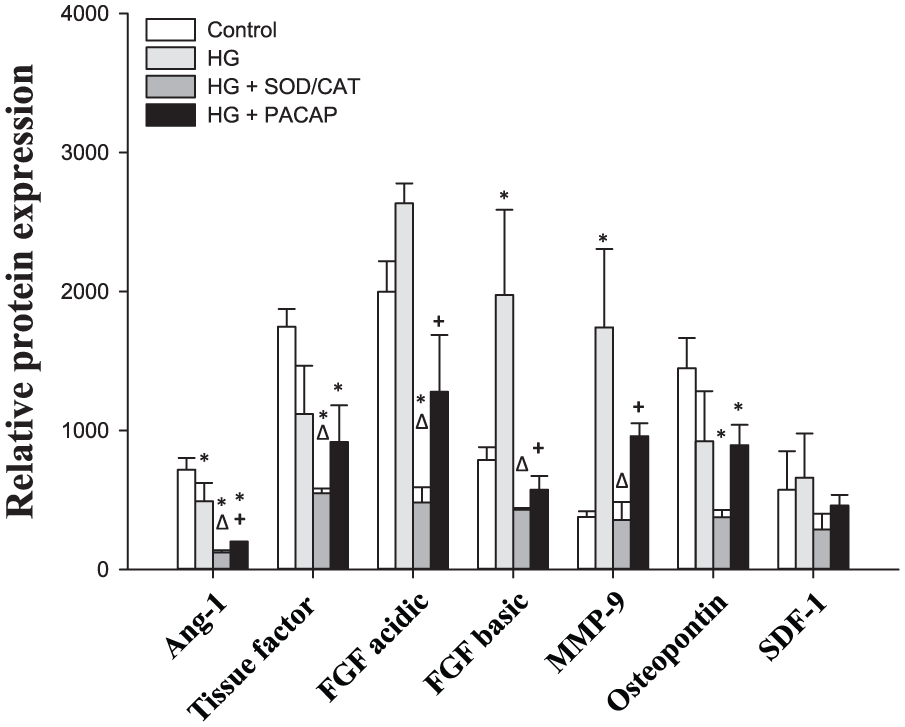
Relative protein expression in carotid arteries, part 1.
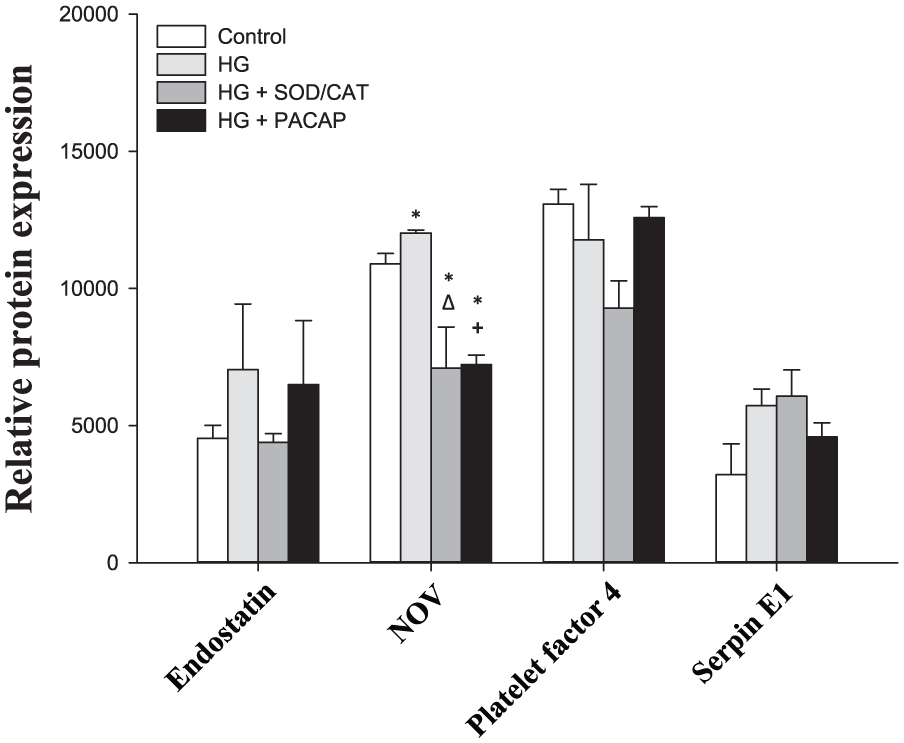
Relative protein expression in carotid arteries, Part II.
Ang-1 declined on HG exposure (p = 0.045 HG vs control), while HG had no significant effect on levels of tissue factor (p = 0.061, HG vs control), FGF acidic (p = 0.082 HG vs control) and osteopoetin (p = 0.108, HG vs control). No treatment could change the level of SDF-1 (p = 0.671), endostatin (p = 0.600), platelet factor 4 (p = 0.130) and serpin E1 (p = 0.091) proteins.
Addition of PACAP1-38 to the HG solution suppressed all increases induced by HG (FGF basic: p = 0.004, MMP-9: p = 0.041 and NOV: p < 0.001 for HG + PACAP1-38 vs HG). Furthermore, levels of Ang-1 and FGF acidic also decreased significantly compared to HG (Ang-1: p = 0.014 and FGF acidic: p < 0.001 for HG + PACAP1-38 vs HG). Addition of SOD/CAT in the presence of HG could also reduce the elevation of the hyperglycaemia markers (FGF basic: p = 0.002, MMP-9: p = 0.002 and NOV: p = 0.001 for HG + SOD/CAT vs HG). In addition, levels of Ang-1, FGF acidic and tissue factor also decreased significantly (Ang-1: p = 0.003, FGF acidic: p < 0.001 and tissue factor: p = 0.038 for HG + SOD/CAT vs HG).
Discussion
This study is the first to demonstrate the ability of PACAP to protect vascular function (as indicated by vasorelaxation) following 1-h HG stress in isolated carotid arteries of healthy mice.
In consistency with previous results, 26 we showed that short-term HG stress reduces endothelium-dependent vasodilation ability of the carotid arteries. In the background of this dysfunction, enhanced superoxide production is suggested as enhanced glycolysis results in increased generation of pyruvate, which is transported into the mitochondria of the cells, and NADH is generated in the tricarboxylic acid cycle. This causes enhanced electron flow through the respiratory chain, which can increase mitochondrial superoxide production. PACAP, similar to the superoxide radical scavenger SOD/CAT, was able to restore Ach-induced vasodilation of the vessels. The protective effect of PACAP was comparable with the protective effect of SOD/CAT, so it was worthwhile to test whether PACAP exerts these positive effects as a direct antioxidant. Pyrogallol autoxidation assay is a classical method to test the superoxide-scavenging ability of different molecules. 24 The assay was originally developed to test/demonstrate the scavenging ability of SOD. As pH is of major importance when testing a possible antioxidant molecule, the improved autoxidation assay 25 included a pH correction to 7.4. This improved method was considered appropriate also for PACAP. According to our study, PACAP seems to be unable to scavenge superoxide anions produced by autoxidation of pyrogallol. Thus, PACAP seems to exert its protective effects by activating signalling pathways acting on its receptor. These results are consistent with the literature. As based on a great number of studies on different cell types (cardiomyocytes, 27 intestinal cells, 16 astrocytes, 28 etc.), it is proposed that the strong protective effects of PACAP against oxidative stress mainly involve not direct, but indirect, antioxidant actions. According to a recent study, PACAP reverses the decrease in the activity of antioxidant enzymes SOD and CAT in ammonium-vanadate-exposed rat lungs. 29 Moreover, a study of Douiri et al. 30 confirmed that PACAP at subnanomolar concentrations induced a dose-dependent increase in both SOD and CAT activities in astrocytes and simultaneously blocked H2O2-evoked inhibition of the activity of these two enzymes.
Endothelium-independent relaxation was examined with the nitric oxide donor SNP. Administration of SNP also induced smaller dilation after 1-h HG stress compared to controls. As a possible explanation for this phenomenon, it has been suggested that hyperglycaemia-induced vascular oxidative stress demonstrated by Bagi et al. 31 can interfere with the bioavailability of NO. 26 According to our results, the addition of SOD/CAT or PACAP to the HG solution could effectively improve SNP-induced relaxation.
The levels of the proteins, FGF basic, MMP-9 and NOV, were increased by a 1-h HG stress. Administration of SOD/CAT alongside with the HG solution markedly decreased the level of these proteins. PACAP together with the HG solution was also able to decrease the level of these markers. FGF basic is synthesized and released by endothelial cells and has an autocrine role. It was suggested that endothelium stores FGF basic capable of autocrine growth promotion both by storing growth factor within the cell and by incorporating it into the underlying extracellular matrix. 32 In a recent study, the role of FGF basic was suggested in type 2 diabetic rats where upregulation of expression of FGF basic proteins were shown. 33 In that study, resveratrol promoted the attenuation of left ventricular diastolic dysfunction by decreasing FGF basic. MMP-9 is a dysglycaemia marker 34 that fits with an early stage of cardiovascular disease as MMPs are synthetized in atherosclerotic plaques, and MMP activity is correlated with unstable angina and plaque rupture. 34 Diabetes mellitus increases vascular MMP activity. 35 MMPs are stored in cytoplasmic secretory granules in endothelial cells, ready for rapid release by angiogenic stimuli. 36 Furthermore, oxidative stress regulates their expression. 34 NOV is an adipocytokine involved in obesity-associated insulin resistance. According to a recent study 37 NOV−/− mice on high fat diet had lower body weight, lower fat mass and improved glucose tolerance and insulin sensitivity. Our data show that FGF basic, MMP-9 and NOV are sensitive vascular markers and are able to indicate already a short-term hyperglycaemia. Both PACAP and SOD/CAT reduced the level of NOV protein below baseline levels. As an explanation of these surprising findings, we suggest that the isolation and the mounting of the vessels (despite the very careful approach of experienced researchers) may induce some low-level damage and oxidative stress (otherwise undetectable). This low-level oxidative stress must have been reduced by the administration of PACAP and SOD/CAT resulting in the fall of angiogenesis-related proteins below baseline.
The very fast change in protein concentrations of angiogenic factors and proteases (FGF basic, MMP-9, FGF basic or ANG-1) in our study implies enhanced protein degradation. Previous findings of the literature also demonstrate a very short half-life (3–30 min) of angiogenetic factors such as FGF or vascular endothelial growth factor (VEGF). 38 Thus, vessels appear to be characterized by very fast angiogenic protein turnover.
However, hyperglycaemia appears to slow down this rapid protein turnover. Previous reports attributed the glucose-induced increase in basement membrane FGF basic to the enhancement of its release due to increased permeability of endothelial cells. 39 In this case, the existence of slow turnover reservoirs (e.g. the basement membrane) were suggested as an explanation of the lasting vascular consequences of short-term exposure to glucose.
Other studies focusing on the mesangial cells of the kidney reported that in hyperglycaemic media, several proteases (e.g. MMP-9) show significantly lowered activity leading to decreased protein degradation. This occurrence rather contributes to impaired protein turnover and consequent induction of cellular hypertrophy and accumulation of extracellular matrix. 40
Future studies should investigate the effects of glucose exposure on vascular protein turnover affecting angiogenic factors.
Diabetes mellitus patients frequently have postprandial hyperglycaemia in which situations endothelium is directly exposed to HG environment. Endothelial cells are highly susceptible to both proliferating and antiproliferative signals. In the pathogenesis of atherosclerosis, endothelial dysfunction plays a critical role, leading to vascular inflammation, thrombosis, arterial stiffness and impaired regulation of arterial tone and flow. 41 Several studies investigated endothelium-dependent vasodilation to assess the health of endothelium; endothelium-dependent dilation is compromised in patients with coronary artery disease. 42 A connection between some of these endothelium damage-inducing/indicating signals and short-lasting hyperglycaemia was tested in this study. Excessive angiogenesis plays a role in many of the clinical manifestations of diabetes, such as diabetic retinopathy 43 or nephropathy. 44 As abnormal angiogenesis is a key factor of vascular tissue damage in diabetes, it is important to find molecules that can help reduce such trophic effects. A previous study confirmed the role of PACAP and VIP peptides on endothelial cell growth after exposure to a hyperglycaemic environment and suggests the potential involvement of both PAC1 and VPAC2 receptors in inhibiting a harmful proliferative response. 45
In summary, the important findings of this study demonstrate that PACAP administration results in reduced endothelial dysfunction after a short-term hyperglycaemic episode. This protective effect is comparable to the antioxidant effect of SOD. Furthermore, here we reported three vascular markers of short-term hyperglycaemia. Endothelial dysfunction was associated with the elevation of FGF basic, MMP-9 and NOV proteins. Their release was reduced by PACAP administration. These results suggest a strong protective role of PACAP in diabetic vascular complications.
Perspectives
In the future, investigations should focus on the potential mechanisms of the protective vascular effects of PACAP in hyperglycaemia. Since vascular dysfunctions demonstrated by our study correlate with hyperglycaemia-induced free radical production, antioxidant actions of PACAP should be further characterized. Based on the available data in the literature,17,46,47 this analysis of PACAP’s protective antioxidant actions could include investigation of various enzymes (such as glutathione peroxidase, heme oxygenase-1 and peroxiredoxin-2) and that of antioxidant small molecules (such as vitamins E and C, glutathione, sulphides or polyphenols).
In addition, we also plan further investigations to characterize the PACAP-dependent positive vascular effects in diabetic animal models. Such investigations may reveal a potential contribution of PACAP in the prevention and even in the treatment of the chronic vascular complications of type 2 diabetes mellitus that present a major public health burden in modern societies.
Key messages
Pituitary adenylate cyclase-activating polypeptide (PACAP) diminishes 1-h high-glucose (HG) stress-induced endothelial dysfunctions in carotid arteries.
Vasoprotective effects of PACAP are independent of direct superoxide scavenging.
PACAP suppresses vascular markers [fibroblast growth factor (FGF) basic, matrix metalloproteinase 9 (MMP-9) and nephroblastoma overexpressed gene (NOV)] raised by 1-h HG stress.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
This work was supported by Hungarian National Science Research Fund (OTKA) K119759, K115874, 2017-1.2.1-NKP-2017-00002 and GINOP-2.3.2-15-2016-00050 ‘PEPSYS’ (D. Reglodi, A. Tamas); University of Pecs Medical School KA Research Grant (D. Reglodi, A. Tamas); OTKA K108444 (A. Koller); University of Pecs Medical School PTE-AOK-KA-2015-14 (M. Solymar); PTE AOK-KA 2017/13 (M. Balasko); MTA TKI Grant MTA TKI 14016 (D. Reglodi); Bolyai Scholarship (A. Tamas); EFOP-3.6.3-VEKOP-16-15 2017-00008/EFOP-3.6.2-16-2017-00008 project; and FP7 Marie Curie project-Small Artery Remodeling (SmART) ITN (I. Ivic, A. Koller). The present scientific contribution is dedicated to the 650th anniversary of the foundation of the University of Pecs, Hungary.
