Abstract
Hepatic stellate cells (HSCs) are professional lipid-storing cells and are unique in their property to store most of the retinol (vitamin A) as retinyl esters in large-sized lipid droplets. Hepatic stellate cell activation is a critical step in the development of chronic liver disease, as activated HSCs cause fibrosis. During activation, HSCs lose their lipid droplets containing triacylglycerols, cholesteryl esters, and retinyl esters. Lipidomic analysis revealed that the dynamics of disappearance of these different classes of neutral lipids are, however, very different from each other. Although retinyl esters steadily decrease during HSC activation, triacylglycerols have multiple pools one of which becomes transiently enriched in polyunsaturated fatty acids before disappearing. These observations are consistent with the existence of preexisting “original” lipid droplets with relatively slow turnover and rapidly recycling lipid droplets that transiently appear during activation of HSCs. Elucidation of the molecular machinery involved in the regulation of these distinct lipid droplet pools may open new avenues for the treatment of liver fibrosis.
Tuohetahuntila M, Molenaar MR, Spee B, et al. Lysosome-mediated degradation of a distinct pool of lipid droplets during hepatic stellate cell activation. J Biol Chem. 2017; 292:12436-12448.
Disturbances in lipid metabolism are fundamental to a number of highly prevalent pathologies such as metabolic disease, coronary artery disease and liver fibrosis. Due to their poor water solubility, excessive lipid accumulation that occurs during these diseases results in lipid deposition at undesired locations of an organism. Under physiological conditions, neutral lipid accumulation is tightly regulated in lipid droplet (LD) organelles. Lipid droplets are composed of a hydrophobic core consisting of neutral lipids, such as triacylglycerols (TAGs) and/or cholesterol esters (CEs), surrounded by a phospholipid monolayer containing cholesterol and a number of specific proteins. The most characteristic LD proteins belong to the so-called perilipin family that consists in mammals of 5 genes (Plin1-5). 1 Furthermore, the LD proteome is enriched in lipid-metabolizing enzymes and proteins involved in membrane traffic, such as specific Rab proteins. Typically, LD proteins have hydrophobic segments that are compatible with a phospholipid monolayer and a hydrophobic core, such as amphipathic α-helices or hydrophobic hairpin structures, whereas transmembrane proteins are mostly excluded from LDs.
Almost all eukaryotic cells have the capacity to synthesize LDs, although LDs in different cell types can vary considerably in size, lipid content, protein composition, and in the enzymes involved in synthesizing and degrading the different lipids.2,3 Some cells form LDs in response to free fatty acids (FAs) or cholesterol stress, whereas others continually contain LDs as storage compartments for various lipids. Examples of these latter “professional” lipid-storing cells are adipocytes, which possess one large central LD predominantly containing TAG, and steroid hormone–producing cells, such as Leydig cells in the testis and adrenal cortex cells, which contain multiple CE-filled LDs to provide an ample supply of cholesterol. The focus of this comment lies on yet another example of a specific lipid-storing cell—the hepatic stellate cell (HSC). This cell type, residing between the sinusoidal endothelial cells and the hepatocytes in the so-called space of Disse of the liver, stores a large part of the vitamin A reserve of the body in the form of retinyl esters (REs) in multiple relatively large LDs. Interestingly, HSCs are also the cells responsible for the deposition of extracellular matrix proteins, such as collagens, during liver fibrosis. During the transition of the retinoid-storing state, the so-called quiescent state, to the secretory or activated state, HSCs gradually lose their retinoid-filled LDs. As the retinoid-storing and the collagen-secreting phenotypes of HSCs seem mutual exclusive, interfering with the LD metabolism is considered to be a potential way to prevent HSC activation and hence attenuate liver fibrosis and subsequent cirrhosis. We therefore set out to unravel the pathways involved in LD formation and breakdown in HSCs during activation. This is not trivial as eukaryotic cells possess multiple genes coding for acyltransferases to synthesize neutral lipid, and likewise, many genes for lipases/esterases, acting on the surface of the LDs or after transport of (part of) the LDs to the lysosome in a process called lipophagy.
Activated HSCs Have 2 Different Metabolic Pools of LDs
Lipidomic analysis in the presence of deuterated FAs and in combination with various pharmacologic inhibitors and genetic tools revealed that activated HSCs contain 2 different types of LDs: an original pool of preexisting/“original” LDs and a relatively rapid recycling pool of “new” LDs. 4 The “original” LDs, present in quiescent HSCs, are relatively large, contain predominantly TAGs and REs, and are localized around the nucleus. In this state, lecithin retinol acyltransferase (LRAT) is the predominant retinol esterification activity. 5 We reported earlier that quiescent LRAT−/− HSCs synthesize negligible amounts (<2%) of deuterium-labeled RE in comparison with wild-type cells. In addition, we showed that this lack of retinyl ester synthesis activity is accompanied by LDs that were considerably smaller in diameter, suggesting a role for LRAT in LD-size regulation. Although we can only speculate about the exact molecular mechanism that could explain this observation, a remarkable property of LRAT is its FA source during retinyl ester synthesis. In contrast to most neutral lipid-synthesizing proteins (DGAT1, DGAT2, ACAT) that use cytosolic acyl-coA as a FA donor, LRAT uses FAs on the sn-1 position of phosphatidylcholine, the most predominant phospholipid in endoplasmic reticulum (ER) and LD membranes. It is well established that phospholipid metabolism, both via the Kennedy pathway and Lands cycle, is an important regulator of LD size. 6 By consuming the surface area of LDs (phospholipids) and synthesizing its core components (REs), LRAT could potentially increase the surface tension of LDs, a key event in LD fusion, as well as the LD diameter of LDs.
During activation, the “original” LDs are degraded with a halftime of a few days, partly in the lysosome by lysosomal acid lipase, product of the Lipa gene, and partly by an unidentified lipase and a cytosolic RE esterase.
Different types of metabolic LDs are formed specifically on activation of the HSCs. These “new” LDs are made at the periphery of the cells by DGAT1, contain less REs than the “original” LDs, but are enriched in TAGs containing one or more polyunsaturated FAs (PUFAs). The TAGs in the “new” LDs are degraded specifically by adipose triglyceride lipase (ATGL), possibly in combination with the unknown lipase. Turnover of the newly synthesized TAGs is relatively fast. We observed halftimes of less than 8 hours for the removal of the newly incorporated FAs from TAG. From studies with both deuterium-labeled glucose and FAs, we observed that FAs were incorporated not only in “new” glycerol backbones derived from glucose but also in preexisting glycerol backbones, presumably as replacement of an acyl chain released by a lipase (M. Tuohetahuntila, 2015, unpublished observations). This latter mechanism can be used to remodel TAGs as it is very similar to the Lands cycle, known to remodel phospholipids. In these TAGs equivalent of the Lands cycle, ATGL and DGAT1 fulfill similar roles as phospholipase A2 and lysophospholipid acyltransferases in the Lands cycle. This rapid turnover of TAGs in combination with a change in the acyl-CoA pool by a shift from the nonspecific long–chain acyl-CoA synthetases (ACSLs) to the PUFA-specific ACSL4 isoform resulted in a clear remodeling of TAGs, leading to a high percentage PUFA-TAGs in activated HSCs (Figure 1).7,8
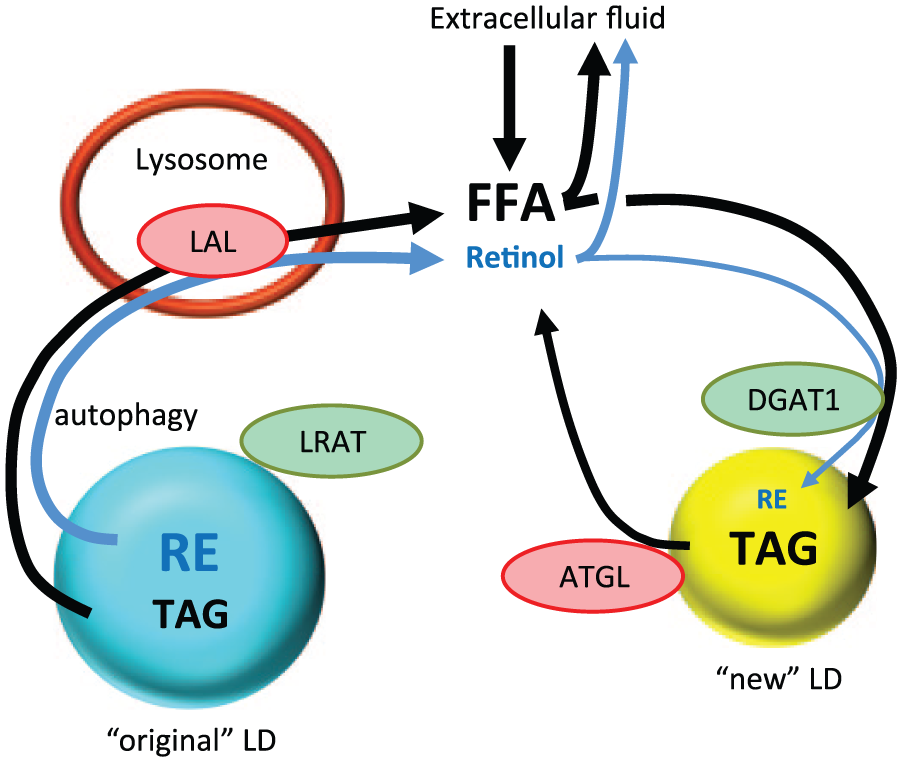
Activated HSCs have 2 different metabolic pools of LDs. Preexisting/“original” LDs are depicted in blue and “new” LDs in yellow. Black arrows show TAG metabolism and blue arrows show retinoid flow. ATGL, adipose triglyceride lipase; DGAT, diacylglycerol acyltransferase; FFA, free fatty acid; HSCs, hepatic stellate cells; LAL, lysosomal acidic lipase; LDs, lipid droplets; LRAT, lecithin retinol acyltransferase; TAG, triacylglycerol; RE, retinyl ester.
The 2-pool model described above explains our previous observations in activated HSCs that LDs have an apparently homogeneous lipid composition, are reduced in size, but increased in number, and are localized in cellular extensions. 9 The new model explains the apparent redistribution of LDs without having to assume fission of the LDs and extensive migration to the periphery, by proposing a degradation of the lipid content (both TAGs and REs) of original LDs, concurrent with a rapid resynthesis of TAGs and REs in novel LDs in the cell periphery. In the presence of an inhibitor of RE degradation, lalistat, we could actually observe by live-cell imaging 2 pools of LDs: one with REs in the center of the cell and one without REs in the periphery. 4 The FAs and free retinol required for the synthesis of the new TAGs and REs are partly derived from the “original” lipids (recycling) but came mostly from the external medium.
The mechanism by which one pool is targeted for lipophagy and the other for lipolysis by ATGL remains elusive. Most likely, the presence of specific proteins on the different types of LDs plays a role. The small GTPase Rab7 was found to target LDs to the autophagic pathway in hepatocellular cells. 3 In HSCs, a reactive oxygen species–dependent activation of Rab25 was implicated in lipophagy. 10 In another study, the LD-associated GTPase Rab18 was found to be involved in the degradation of LDs in activated HSCs, although the specific pathway of LD degradations was not addressed. 11 Considering the preference of ATGL for the “new” LDs in activated HSCs, a role of the LD-scaffolding proteins of the Plin family might be anticipated. 1 Activated HSCs are known to lose expression of Plin5 12 and express predominantly Plin2 and 3. 11 Especially, the latter, Plin3, is known to have a preference for newly formed small LDs 1 and may therefore facilitate the degradation of the “new” LDs by ATGL. In contrast, Plin2 is considered to protect LDs against degradation.
It is generally accepted that the function of the “original” pool of LD in quiescent HSCs is the storage of vitamin A. Less clear is the function of its degradation during activation, let alone the formation of the “new” type of LDs. We may speculate that the “original” LDs are broken down to make room for the expanded ER and Golgi and plasma membrane required for the massive collagen synthesis and provide the lipid building blocks for these new membranes and retinoids for cell signaling. The role of the “new” LDs during this membrane remodeling might be to temporarily buffer the FA concentration in the cytosol to prevent the toxic effect of free FAs and at the same time provide sufficient amounts of FAs close to the sites of new phospholipid synthesis. As membrane phospholipids generally contain more PUFAs compared with TAGs, the remodeling of the TAG pool to PUFA-TAGs would fit in this hypothesis. A similar simultaneous breakdown and resynthesis of TAGs are also observed in adipocytes during lipolysis. In this cell type, as in HSCs, DGAT1 was shown to be the major enzyme involved in the resynthesis, presumably to prevent ER stress by high levels of the released FAs. 13 Alternatively, the accumulation of PUFA-TAGs in the dynamic LD pool could function as a transient pool of precursors for the synthesis and secretion of eicosanoids by HSCs. 7
The identification of a number of important lipid-metabolizing enzymes allowed us to investigate the role of lipid metabolism in the activation of HSCs. In general, we found a good correlation between the effect of inhibitors on lipid levels with their effect on activation, showing that relatively large disturbances in lipid metabolism attenuate HSC activation.4,8 As inhibition of TAG and/or RE formation had the same effect as inhibiting their breakdown, HSCs seem to require a dynamic neutral lipid pool for optimal functioning. Understanding the molecular machinery involved in the formation of these distinct LD pools may lead to new targets for the treatment of liver fibrosis.
Footnotes
Funding:
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests:
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Author Contributions
MRM, ABV and JBH wrote the manuscript.
