Abstract
Avalanche burial occasionally precipitates pulmonary edema, yet its pathogenesis remains poorly understood. Two male back-country skiers (aged 39 and 53 years) were completely buried for 30 min and 20 min, respectively, by the same avalanche, and immobilized in a right-lateral posture without safety devices. They arrived 2 h post-extrication, conscious but hypothermic (32.4 °C and 34.2 °C, respectively), tachycardic, tachypneic, and hypoxemic (SpO2 88% and 83%, respectively). Chest radiography and computed tomography demonstrated extensive infiltrates or ground-glass opacities confined predominantly to the gravity-dependent right lung and no cardiomegaly. C-reactive protein and N-terminal pro-B-type natriuretic peptide values were within normal limits, and transthoracic echocardiography showed preserved biventricular function. Low-flow oxygen and passive rewarming corrected hypoxia and hypothermia; the pulmonary infiltrates resolved within 24 h, permitting discharge without sequelae. Classical mechanisms, such as negative-pressure pulmonary edema from airway obstruction, hypoxia-induced left ventricular failure, and edema secondary to regional hypoxic pulmonary vasoconstriction, do not fully explain the unilateral dependent pattern observed. We propose that excessive sympathetic nervous system activation and fluid distribution changes caused by extreme emotional stress, cold exposure, systemic hypoxia, whole-body compression by snow, and head-down posture led to an excessive cardiac load increase, resulting in gravity-enhanced cardiogenic edema despite normal intrinsic cardiac function. These cases suggest a previously unrecognized hemodynamic pathway for avalanche-related pulmonary edema. Awareness of cardiac overload as a potential contributor may refine field triage and postrescue management. Additional clinical and experimental studies are warranted to validate this hypothesis and inform preventive strategies.
Introduction
Avalanches are a major cause of fatal mountain accidents in Japan and worldwide. 1 The primary causes of avalanche-related fatalities include asphyxiation and trauma, with hypothermia being a contributing factor. 2 There are several published case reports of pulmonary edema occurring after avalanche burial,3–6 and it is considered a potential cause of death in avalanche victims. 3 Proposed mechanisms for the development of pulmonary edema following avalanche burial include negative pressure pulmonary edema due to upper airway obstruction,3,5 hypoxia-induced left heart failure, 7 and pulmonary edema secondary to hypoxic pulmonary vasoconstriction and pulmonary hypertension. 3
In this report, we describe 2 patients who developed predominantly right-sided pulmonary edema after complete avalanche burial. Drawing on their clinical findings, we discuss the potential mechanisms of avalanche-related pulmonary edema and explore potential pathophysiological pathways based on their clinical findings.
Case 1
A 39-year-old man with no medical history engaged in backcountry skiing. He ascended a snow-covered mountain slope in a line formation with other group members. He carried an avalanche transceiver but no other avalanche safety devices. At an altitude of 1400 meters, he was caught in an avalanche that came down on his left side, and his entire body was buried in snow with him on his right side. He was buried in the avalanche, and the weight of the snow prevented him from moving at all. Thirty minutes later, he was found via the transceiver and dug out by other members who had been caught in the same avalanche. He had quickly covered his mouth with both hands to create an air pocket and prevent his airway from becoming blocked. He remained conscious throughout the burial. He arrived at our hospital 2 hours after being rescued. The depth of the burial was unknown.
Upon arrival, the patient was alert, with a core body temperature of 32.4 °C, blood pressure of 133/65 mm Hg, heart rate of 140 beats/min, respiratory rate of 36 breaths/min, and oxygen saturation (SpO2) of 88% on room air. Breath sounds were clear bilaterally, and there were no contusions, tenderness, or signs of trauma. No medical intervention was provided until transport to the hospital, and rewarming was performed using a warm fluid infusion and external warming after arrival at the hospital. Chest radiography revealed sharp costophrenic angles and decreased radiolucency, predominantly in the right upper lung field, extending into the right lower field, and no cardiomegaly. Chest computed tomography revealed infiltrative shadows suggestive of pulmonary edema, predominantly in the right upper lobe, extending to the right lower lobe and slightly into the medial aspect of the left upper lobe (Figure 1). No fractures or organ injuries were observed. Laboratory tests showed leukocytosis and elevated creatine kinase (CK) levels, but the C-reactive protein (CRP) level was within normal ranges, and N-terminal pro-B-type natriuretic peptide (NT-proBNP) levels were not elevated (Table 1). Transthoracic echocardiography demonstrated normal cardiac function. The pulmonary artery pressure was not measured.
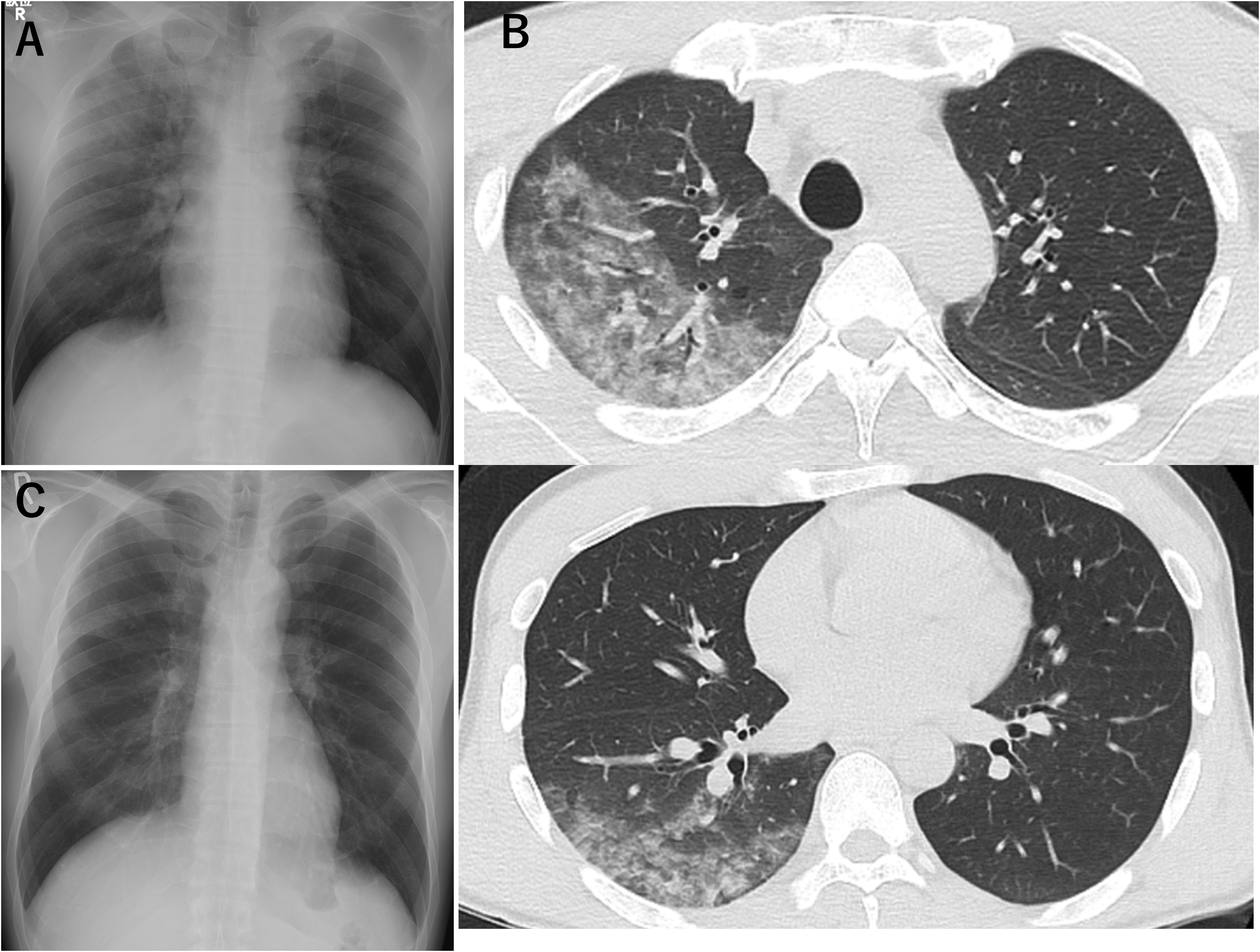
(A) Chest radiograph on the day of admission shows no cardiomegaly, with sharp costophrenic angles and decreased radiolucency predominantly in the right upper to lower lung fields. (B) Chest computed tomography on the same day reveals infiltrative and ground-glass opacities suggestive of pulmonary edema, predominantly in the right upper lobe but involving the entire right lung. (C) Radiographic findings improved in the right lung field on the following day.
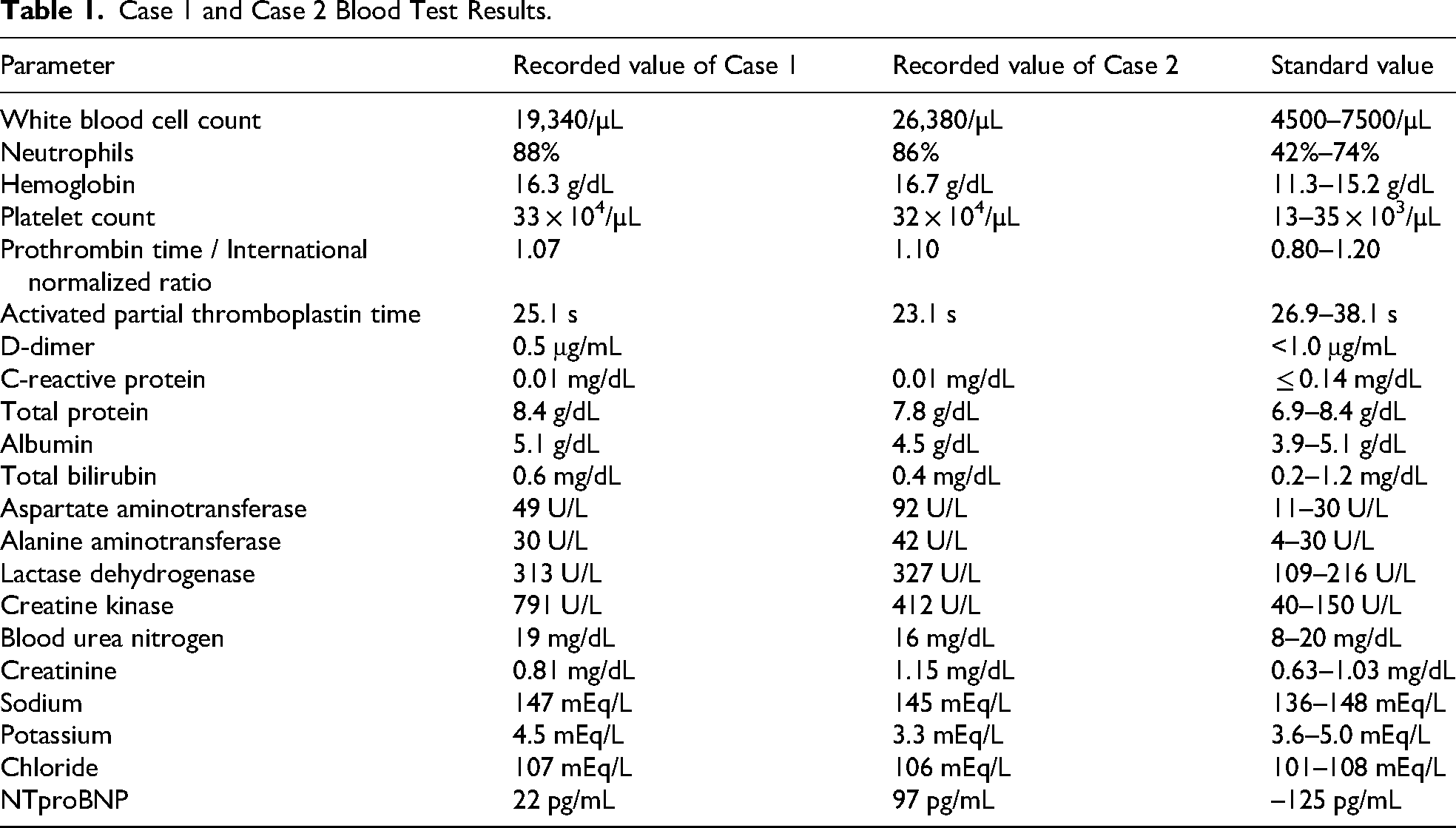
Case 1 and Case 2 Blood Test Results.
Although hypothermia was successfully corrected in the emergency department, the patient required low-flow oxygen supplementation to maintain an SpO2 of 90%, prompting admission for inpatient observation. By the following day, oxygen supplementation was no longer necessary, and the pulmonary infiltrates had improved, allowing for discharge home.
Case 2
A 53-year-old man with a history of hypertension engaged in backcountry skiing. He was taking an unknown medication for blood pressure control. He ascended a snow-covered mountain slope in the same line formation as the patient in Case 1 when he was caught in the same avalanche from the left side of his body and was completely buried in snow in the right lateral position, similar to Case 1. He carried an avalanche transceiver but no other avalanche safety devices. The weight of the snow prevented him from moving at all. He was rescued 20 min later and arrived at our hospital along with the patient in Case 1. No airway obstruction was observed. The depth of the burial was unknown.
On arrival, the patient was alert, with a core body temperature of 34.2 °C, blood pressure of 184/128 mm Hg, heart rate of 120 beats/minute, respiratory rate of 30 breaths/minute, and SpO2 of 83% on room air. Breath sounds were clear bilaterally, and as in Case 1, there were no contusions, tenderness, or signs of trauma. No medical intervention was provided until transport to the hospital, and rewarming was performed using a warm fluid infusion and external warming after arrival at the hospital. Chest radiography revealed sharp costophrenic angles and infiltrative shadows throughout the right lung field, and there was no cardiomegaly. Chest computed tomography revealed diffuse ground-glass opacities throughout the right lung and slight ground-glass opacities in the left lung, suggesting pulmonary edema (Figure 2). Laboratory findings included an elevated white blood cell count and CK level, while the CRP level was within normal ranges and the NT-proBNP level was not elevated (Table 1). Transthoracic echocardiography revealed normal cardiac function. The pulmonary artery pressure was not measured.
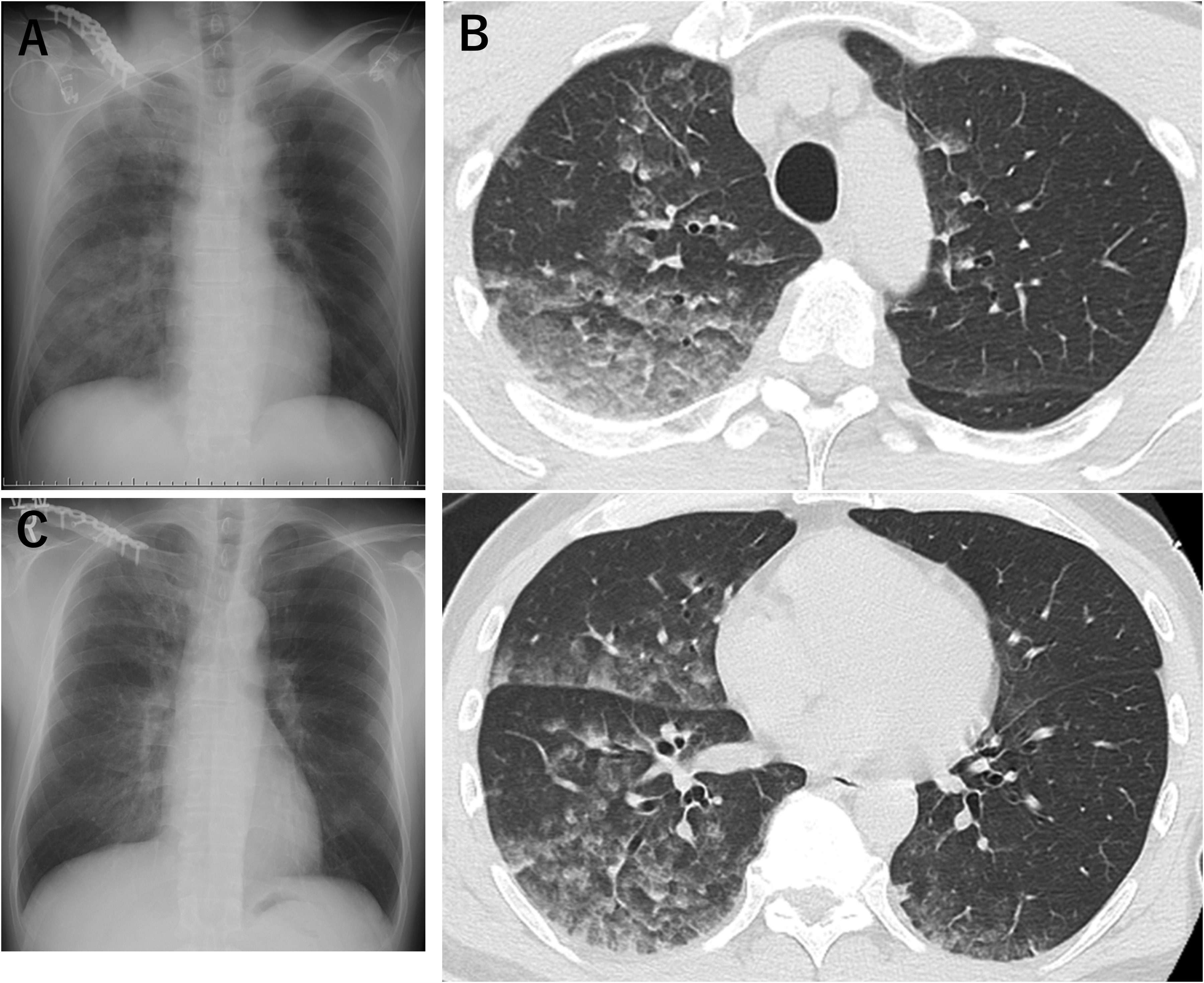
(A) Chest radiograph on the day of admission shows no cardiomegaly, with sharp costophrenic angles and decreased radiolucency predominantly in the right lower and overall right lung fields. (B) Chest CT on the same day shows infiltrative and ground-glass opacities suggestive of pulmonary edema in both the right upper and lower lobes. (C) Radiographic findings improved in the right lung field on the following day.
As in Case 1, although the hypothermia was successfully corrected in the emergency department, low-flow oxygen supplementation was required to maintain the SpO2 at 90%, and the patient was admitted for observation. By the following day, oxygen therapy was no longer necessary, and the pulmonary infiltrates had improved, allowing for discharge home.
Discussion
We encountered 2 cases in which right-dominant pulmonary infiltrates suggestive of pulmonary edema developed after complete burial by an avalanche. Herein, we discuss the potential mechanisms underlying the pulmonary abnormalities observed in these patients.
Several mechanisms have been proposed to explain the development of pulmonary edema following avalanche burial, including negative pressure pulmonary edema due to upper airway obstruction,3,5 hypoxia-induced left ventricular failure, 7 and pulmonary edema resulting from hypoxic pulmonary vasoconstriction and pulmonary hypertension. 3
The patient in Case 1 breathed through a small air pocket of several hundred milliliters created by covering his mouth with both hands, while the patient in Case 2 breathed in a very small space without creating an air pocket. Breathing in this small space may have caused strong negative airway pressure. Hypoxic pulmonary vasoconstriction may lead to regional perfusion heterogeneity, with relative overperfusion in areas without vasoconstriction, which could increase the risk of pulmonary edema. 8 Marked negative airway pressure, in combination with hypoxic pulmonary vasoconstriction, may have precipitated pulmonary edema in the gravity-dependent, highly perfused right lung. However, the upper left (nondependent) lung may have been relatively more compliant, potentially experiencing larger negative pressure swings. In contrast, the dependent right lung may have been less ventilated and therefore more prone to hypoxia. These conditions could favor hypoxic pulmonary vasoconstriction in the right lung. Taken together, these observations may not be fully explained by hypoxic pulmonary vasoconstriction or negative-pressure pulmonary edema alone; therefore, we considered a multifactorial explanation in light of the patients’ circumstances.
We speculate that in the 2 cases reported here, the circumstances created by the avalanche burial led to pulmonary edema with right lung predominance, as evidenced by findings in the gravity-dependent lung, which may reflect increased cardiopulmonary loading. Emotional stress, cold exposure, and body-surface compression by snow are plausible contributors in this context. A head-down posture is a theoretical contributor during avalanche burial in general; however, the burial angle was not documented in our cases, and both patients were described as being right-lateral at extrication, so we cannot infer head-down positioning as a contributor here. Our evaluation was limited to noninvasive clinical assessment and transthoracic echocardiography, and pulmonary artery pressures were not measured. Therefore, compartmental blood-volume shifts were not directly quantified. The splanchnic venous system is considered the body's largest reservoir for unstressed blood volume, and the majority of unstressed blood volume is found there. Additionally, approximately one-quarter of the total blood volume is stored in splanchnic-perfused organs. With sympathetic activation and increased vasomotor tone, this reservoir can redistribute blood centrally, potentially increasing stressed blood volume and cardiopulmonary filling pressures. 9 This sympathetic stimulation is considered one of the causes of acute pulmonary edema, 10 and indeed, rapid increases in cardiac output, central venous pressure, and systemic vascular resistance have been reported with visceral sympathetic stimulation. 11 In these cases, we suspect that emotional stress caused sympathetic nervous system hyperactivity. Cold exposure is known to constrict skin vessels via sympathetic nerve stimulation. 12 While hypoxia alone can cause cutaneous vasodilation, hypoxia has been shown to augment cutaneous (non-noradrenergic) vasoconstriction during prolonged cold exposure. 13 In these cases, the combination of cold exposure and hypoxemia may have exacerbated the condition through an increase in cardiac afterload due to peripheral vasoconstriction. Regarding compression caused by the surrounding snow, an increase in cardiac output has been reported with the use of compression garments, 14 and an increase in venous return due to a decrease in the vascular bed volume caused by compression of the entire body surface has been suggested. In our patients, it is possible that an increase in cardiac preload occurred due to similar conditions. In addition, hypoxic conditions may have exacerbated the above mechanisms by inducing left ventricular dysfunction. 15 Furthermore, it has been reported that a sudden head-down position can cause a rapid increase in right ventricular stroke volume, resulting in a dissociation between right and left ventricular stroke volumes, 16 which can lead to pulmonary edema. Because cephalad–caudal tilt relative to the slope was not recorded, any inference about head-down positioning in these cases is precluded.
The factors contributing to pulmonary edema are multifactorial, and it is possible that a combination of the above mechanisms may have contributed to the presentation of pulmonary edema in our patients. If pulmonary edema is caused by cardiac overload, this could help explain the pulmonary edema occurring predominantly in the lower lungs. Similarly, there is a report of a case of cardiogenic pulmonary edema occurring in the lateral decubitus position with pulmonary edema predominantly in the lower lungs. 17
A clearer understanding of the mechanisms underlying pulmonary edema after avalanche burial may inform clinical management and education. Further research is required in this area. The limitations of this report include the fact that details such as the size of the avalanche, weather conditions, burial depth, buried posture, and conditions surrounding the burial site are unknown. In particular, cephalad–caudal tilt relative to the slope was not recorded, precluding any inference about head-down positioning in these cases. In addition, due to the small number of cases and the unknown oral medication in the patient in Case 2, it may be difficult to generalize the findings to other cases.
Conclusion
We report 2 cases of right-dominant pulmonary edema following complete avalanche burial, with findings localized to the gravity-dependent lungs. In addition to the previously reported pathogenesis of this gravity-induced pulmonary edema, we discussed established mechanisms that may increase cardiac load—sympathetic activation, cold exposure, and body-surface compression by snow. Head-down positioning remains a theoretical consideration in avalanche burial but was not established in our cases.
These 2 cases are consistent with a multifactorial pathophysiology that integrates established mechanisms of avalanche-related pulmonary edema. Detailed clinical and radiological assessments support consideration of this possibility. Improved mechanistic understanding may inform clinical management and education, and further observational and experimental studies are warranted to evaluate these possibilities and clarify the underlying mechanisms.
Footnotes
Ethical Considerations
This case report was conducted in accordance with the institutional ethical standards. Ethical approval was not required for this study because it involved a retrospective description of anonymized clinical cases without identifiable patient information.
Consent for Publication
Verbal informed consent for publication was obtained from both patients, and consent was documented in their medical records. Written informed consent was not obtained in accordance with the institutional policy for nonidentifiable case reports.
Author Contribution(s)
Conceptualization (R.S.); Data duration (R.S.); Formal analysis (R.S.); Writing – original draft (R.S.); Writing – review & editing (R.S., S.Y.).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability
All data generated or analyzed in this study are included in the published article. No additional datasets are available.
