Abstract
A man attacked by a pet zebra suffers multiple bite wounds to his right arm and generalized trauma after being dragged to the ground and pinned by the animal. He was transported to the emergency department (ED) by the local emergency medical service (EMS) with a tourniquet in place for nearly 60 min. The man's injuries included extensive soft tissue damage, an open fracture and dislocation of his right elbow, and a soft tissue injury to his right ear. His clinical course was complicated by severe necrosis of the soft tissue of the right forearm requiring transhumeral amputation just above the condyles. Ongoing infection and the development of phantom limb pain complicated his recovery.
Introduction
Zebras (subgenus Hippotigris) are African equines, easily recognized by their iconic white coat with bold black stripes. They share the equine family with horses and donkeys. Zebras are known for their small size and aggressive behavior and have been resistant to domestication even though humans and zebras have shared habitats since time immemorial. 1 Their emblematic stripes are thought to serve as a deterrent for flies and for camouflaging their individual presence in large groups. 2
Keeping exotic animals, such as zebras, in captivity is known to be dangerous to one's physical safety. 3 Zebras have shown to be very territorial of their home range, especially of their female harem.4,5 This behavior increases the risk of a caretaker being exposed to harm such as what transpired in this case. While this article's authors could not find an exhaustive database on the occurrence of zebra attacks, they seem to appear rarely. In the United States, only one case report was discovered in the medical literature 6 , and thirteen unique incidents were reported in nonmedical literature after an exhaustive search of academic and nonacademic literature. Only one other case report from South Africa was identified. 7
With limited data on zebra attacks, information had to be gleaned from their close cousin, the horse. Equine oral flora resulting in bite wound soft tissue infections include bacteria from the Actinobacillus, Pasteurella, Staphylococcus, Streptococcus (including group B strep), Neisseria, and Yersinia species as well as from Bacteroides fragilis, Campylobacter ureolyticus, Escherichia coli, Prevotella melaninogenica, and Pseudomonas aeruginosa. 8
Case Report
On a winter afternoon in the United States, a 72-year-old right-hand-dominant man was attacked by a pet male zebra inside an enclosure during a routine feeding of the male and other female zebras. The man's past medical history included type 2 diabetes and renal transplant on immunosuppressant medications. The zebras are raised on a private farm to eventually be sold for profit. The attacking zebra was known to be aggressive, but the incident was reportedly not intentionally provoked. After feeding the male zebra, the man turned away to nourish the females in the herd. Almost instantly he felt a bite and a tugging of his right arm and was slammed aggressively to the ground, experiencing multiple forceful kicks to his body. He even reported the zebra slamming his body against his. Eventually, he was able to free himself from the animal and call for medical assistance. The man knew that he had sustained severe injuries and that the animal would likely be aggressive toward first responders. Arriving law enforcement officers had to fatally shoot the male zebra to secure the scene after the animal repetitively became aggressive toward them.
Upon arrival to the ED, the man's initial vital signs included a blood pressure of 160/90 millimeters of mercury (mm Hg), a heart rate of 111 beats per minute, 16 respirations per minute, and an oxygen saturation of 98% on room air. A tourniquet established by EMS just above his right elbow was removed after being in place for 54 min, with minimal bleeding ensuing. The initial primary survey demonstrated a traumatic injury to the right ear and a deformed right elbow and forearm, with a large open wound exposing muscle and adipose tissue (Figure 1). The patient complained of new numbness and weakness in his right hand. A physical exam revealed an absent right radial artery pulse and the existence of an ulnar arterial pulse by Doppler ultrasound in the presence of a fracture and dislocation of this right elbow. Radiographs of the right forearm demonstrated an open fracture of the proximal radial neck and coronoid process, as well as a dislocation of the elbow joint (Figure 2). In addition, the right-elbow radiographs revealed a fracture of the ulnar styloid.
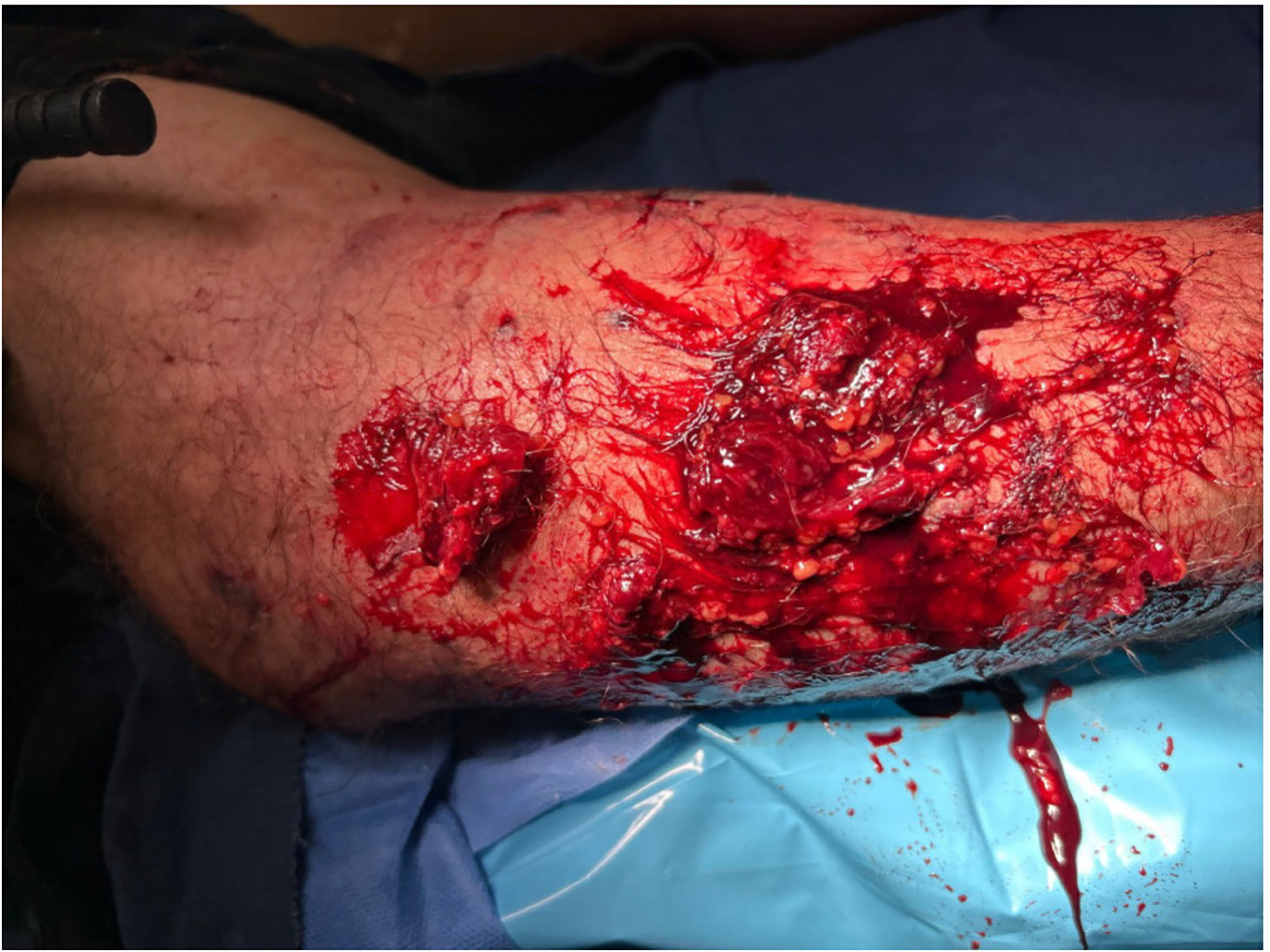
Open wound right forearm.
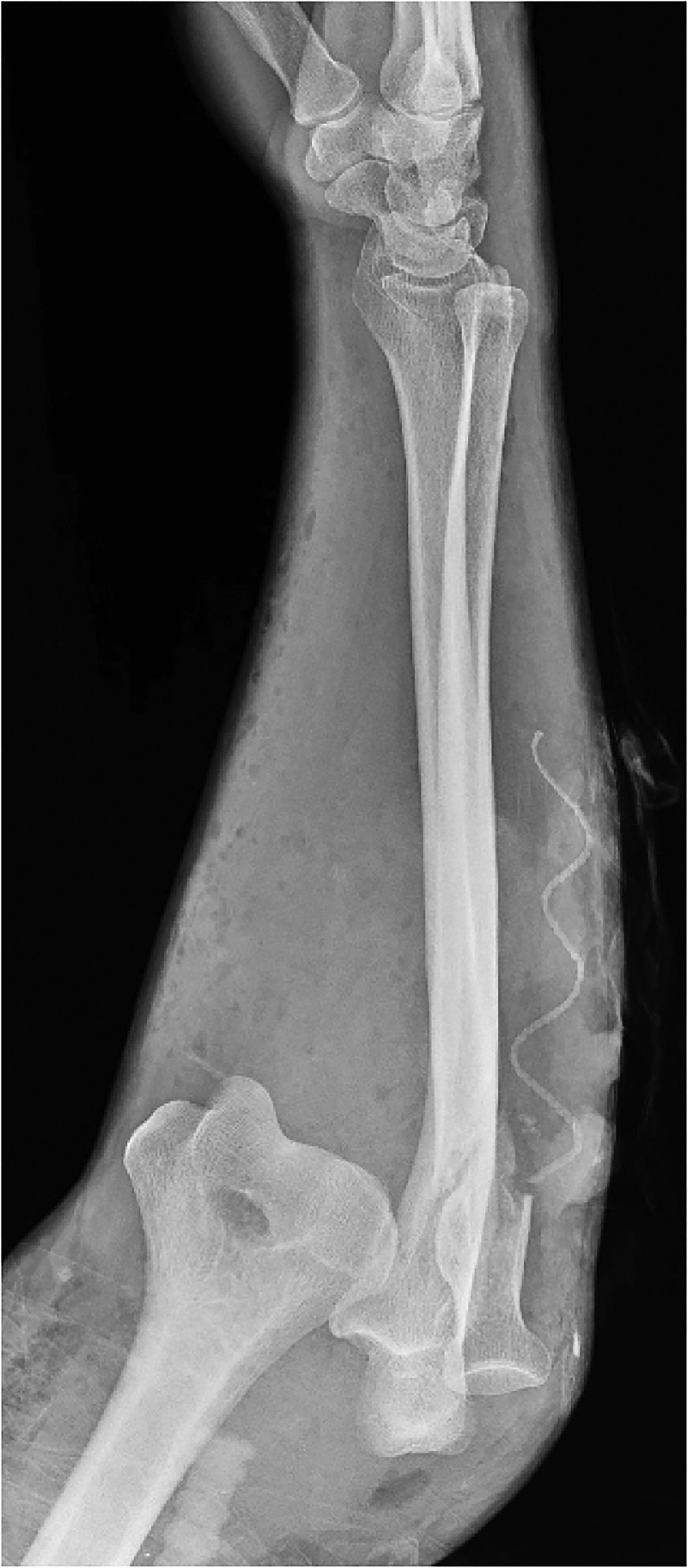
Styloid fracture and elbow open fracture/dislocation.
Pain control was obtained using a single dose of 0.5 mg of intravenous (IV) hydromorphone, and procedural sedation was performed in preparation for an elbow reduction. Post reduction, palpable pulses were noted in both the radial and ulnar arteries, but the patient had limited movement of his right hand. The wounds were thoroughly irrigated in the ED, a wet-to-dry dressing was applied, and the injured extremity was stabilized in a long arm fiberglass splint. An initial IV dose of 4.5 g piperacillin-tazobactam was administered based on the presumed polymicrobial nature of the equine bite wound. The patient also received a 1L bolus of lactated Ringer’s to volume resuscitate the patient while in the Emergency Department. The patient was started on trimethoprim-sulfamethoxazole (TMP-SMX) due to his history of renal transplant and immunosuppression on tacrolimus. No rabies vaccination or immunoglobulin was given, but tetanus vaccination was updated. The plan was for further evaluation of the wound in the operating room (OR) the next morning.
In addition to the injuries noted previously, the patient also had a right ear hematoma, right nail bed injury, and an age-indeterminate nondisplaced anterior bridging osteophyte fracture of T8 vertebrae. Computed tomography angiography (CTA) of the right upper extremity showed occlusion of the interosseous artery just distal to the origin without any other vascular injuries, presumed to be from recent trauma. Of note, CTA was performed after the reduction in the ED.
The patient's early morning surgery was delayed due to his development of diabetic ketoacidosis, requiring the initiation of an insulin drip. Surgery by late morning revealed significant necrotic muscle tendons as well as severe ligamentous loss in the elbow, leaving it grossly unstable and requiring the placement of internal fixation devices (Figure 3). On admit day 2, his right thumb laceration was repaired and the right ear hematoma was drained. He also developed a new blood loss anemia, requiring two units of packed red blood cells.
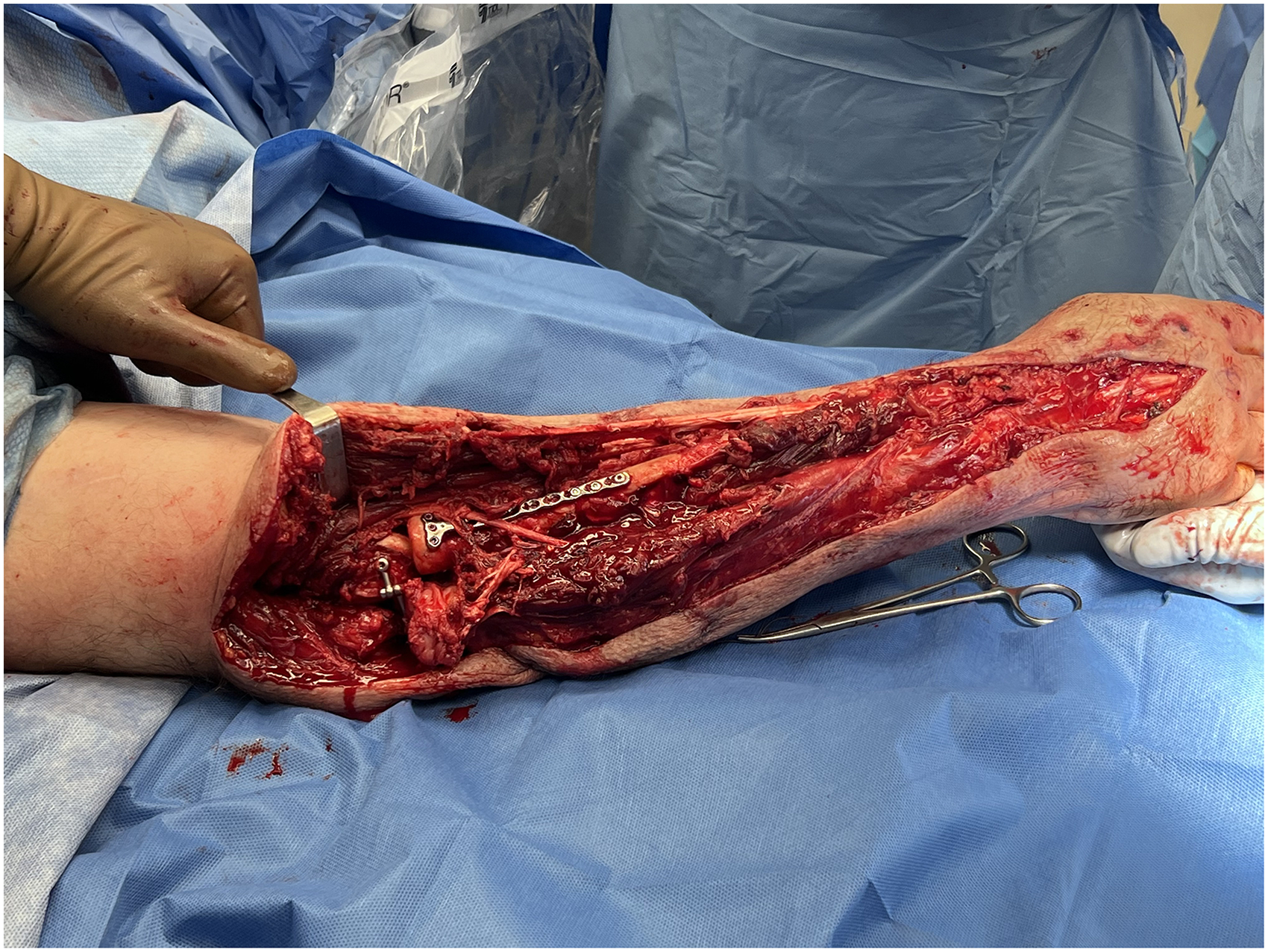
Placement of internal fixation device.
On day 3 of admission, the patient returned to the OR, where extensive necrotic tissue changes were observed in the extensor and flexor muscles of the forearm. Based on these findings, the decision was made to perform a transhumeral amputation. The patient remained in the hospital for 9 days to allow time for observed healing, evaluation, and treatment by both occupational and physical therapy, as well as finishing his course of broad-spectrum antibiotics, which were expanded to include IV cefazolin as well as tobramycin and vancomycin paste intra-procedure on 3 occasions.
The patient was discharged on a course of TMP-SMX and released to an inpatient rehabilitation center for several days and then to a long-term outpatient rehab facility. As an outpatient, he developed cellulitis at the surgical site and was started on linezolid and piperacillin-tazobactam. During his recovery, phantom limb pain developed but eventually ceased by his 2-month follow-up appointment. During that visit, the man no longer required pharmacologic pain control, and his wound appeared to be healing well.
Discussion
Zebra attacks on humans are rare but can lead to catastrophic injuries and life-changing morbidity.3,6,9 To our knowledge, this is the only case of a zebra attack in the news or in the medical literature resulting in an amputation, and only the third case report of such an attack on humans. Furthermore, this is the only case that was complicated by diabetic ketoacidosis as well. The authors postulate the inciting event was traumatic limb ischemia in the right upper extremity, leading to infarction of the muscle tissue secondary to trauma in a poorly controlled diabetic. The majority of cases in the medical and nonmedical literature involved biting as a mechanism of injury.6,7,9 Both prior case reports involved bite-related injuries to extremities, and both were complicated by infection. While vascular injuries were present in only one of the two previous case reports, ours was the only case to involve a fracture or amputation. The most significant operation in previous literature was limb salvage by revascularization via harvesting of the greater saphenous vein.6,7 The patient did not require amputation. Such an outcome reinforces the old medical adage of “time is tissue.” Getting the patient to definitive care to return blood flow to his dominant arm was delayed due to the patient being in an austere environment and in the presence of an aggressive animal, limiting scene safety to first responders. Maintaining scene safety is always paramount, as failure to do so can cause first-responder injury and can further delay care for the patient. 10 Furthermore, all of these delays also contributed to the tourniquet being in place for nearly an hour, which certainly compounded the ischemic changes seen in the patient. Operative intervention was also further delayed due to the complications of diabetic ketoacidosis. These factors all contributed to the extensive tissue damage seen from infarction that led to eventual amputation, which is unique in the medical literature.
This case was complicated by infection despite early and aggressive antibiotic treatment. This patient was particularly prone to infection due to his immunocompromised state on tacrolimus and being a diabetic, but both other case reports seemed to have struggled from infection as well, even with early and aggressive treatment.6,7 Though the data is limited to only two other case reports, our literature review suggests that treating empirically with broad-spectrum antibiotics for at least Pseudomonas spp. is appropriate since doing so may limit clinical progression to infection in this subset of patients.6,8,11 Our patient was promptly started on prophylactic antibiotics and received cefazolin, piperacillin/tazobactam, TMP-SMX, vancomycin, and tobramycin within the first 24 h of arrival in the ED. Despite this broad antibiotic coverage, the patient did suffer from a cellulitis complication almost 1 week after discharge from the hospital. No signs of infection ever developed during his inpatient stay, so wound cultures were never obtained.
Post-zebra-bite infection seems to be a common trend in all case reports, even with aggressive antibiotic therapy.6,7 Toovey et al documented that the patient experienced a complication of cellulitis, which grew Pseudomonas aeruginosa as well as group B Streptococcus. They were unable to determine if prompt prophylactic antibiotics were started at the outlying hospital prior to transfer to their center. They initially started a 5-day course of twice-daily 750 mg amoxicillin-clavulanic acid followed by a 5-day course of twice-daily ciprofloxacin. They also performed a laceration repair, five hyperbaric oxygen sessions, wound exploration, debridement, and skin grafting. While in the OR, wound cultures were obtained, and they initiated 750 mg amoxicillin-clavulanic acid twice daily for 5 days without any other significant complications or infections. 7
Carlson et al obtained positive wound cultures in the OR upon the patient's initial presentation. These were positive for Pseudomonas aeruginosa, Aeromonas hydrophila, Streptomyces species, Bipolaris species, Enterobacter cancerogenus, and Rhodococcus species. This patient appears to have only initially received oral amoxicillin/clavulanate before culture results on post-op day 3 and eventually received a total of 6 different antibiotics for varying lengths at different times: amoxicillin/clavulanate for 4 days, piperacillin/tazobactam for 3 days, cefepime for 11 days, metronidazole for 48 days, levofloxacin 30 days, TMP-SMX for 30 days, and 1 antifungal, voriconazole, for 50 days. No other clinical signs of infection were ever reported in the case report, though. 6
Being in close proximity to non-domesticated animals, such as zebras, can be dangerous and has led to multiple attacks over the years.9,12,13 At the time of this writing, there does not appear to be an exhaustive private or government-funded database that records exotic animal attacks in the United States. Due to the lack of a centralized reporting system, obtaining definitive data on the prevalence of exotic animal attacks, in particular zebras, proved to be difficult.
Watch groups such as Born Free USA and People for the Ethical Treatment of Animals (PETA) track human-related injuries from exotic animals in the United States. Born Free USA has recorded 662 instances of exotic animals injuring humans, 6 of which were from zebras. This database does not seem to be exhaustive, as we were able to find at least 7 other confirmed cases of zebras injuring humans in the United States that were not included on this list but were aggregated by PETA. These two data sets record a total of at least 13 unique cases of zebras injuring humans in the United States. We also were able to find multiple videos on social media of zebra attacks that do not seem to be in either database, but determining where these videos were filmed proved to be unattainable.9,12,14,15
Only one of the past case reports was from a wild zebra, while all of the incidents reported in the United States involved domesticated animals.6,7,9 Our review of zebra attacks confirmed to be in the United States found biting was part of the zebra attack in all but 4 cases. This proved to be unique to zebras in comparison to other equine attacks, in which biting only represents 3–4.5% of attacks. 11 Due to this seeming to be the most common mechanism of injury in zebra attacks, further research into the normal flora of a zebra's mouth could be an area of further research.
With only two formal case reports published at this time, it is impossible to know the rate at which zebra bites develop infection, so making an evidence-based decision on whether to start prophylactic antibiotics or not is difficult and should be left to the physician's discretion. If the decision is made to start antibiotics, coverage for Pseudomonas spp. is recommended, as this appears to be the only universally cultured microbe from past case reports. Care for all animal bites should focus on early and thorough irrigation and weighing the risks and benefits of primary and secondary healing.16,17 The decision should be made on a case-by-case basis and wounds deemed to be high risk should not be closed. 18 Tetanus should be updated following standard practice guidelines. 16 Rabies infection should be weighed on a case-by-case basis and providers can contact their state health department and the Center for Disease Control and Prevention for assistance with risk assessment. 19 Zebras have been known to carry rabies, but a case report of close observation of an infected zebra yielded no transmission to humans even after high-risk exposure. 20 Rabies vaccination was not provided in this case, as it was deemed to be low risk for transmission.
This case demonstrates the multiple levels of complexity and the need for a multidisciplinary approach when managing a unique and complex exotic animal bite. It also adds to the slowly building body of literature on zebra attacks. This is important as it appears to be in contrast to other equine attacks. This article is not an extensive review of how to manage animal bites, as that is already well established in the literature, but it does review the intricacies of this particular case.16,21
Footnotes
Author Contribution(s)
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
