Abstract
A 74-year-old man was attacked by a wild boar while on his way home from his farm in the daytime in winter 2017 on the rural Izu peninsula. He did not provoke the boar; however, hunters were hunting animals in the mountains near the farm around the same time. The boar bit his left leg, and the man fell to the ground. The boar continued biting the man’s left leg, and the man delivered a few kicks to the boar’s face with his right leg. The boar then bit his right foot and ran away. The man was taken to a hospital, and a physical examination revealed 3 bite wounds on his left leg and right foot. The wounds were irrigated with sterilized saline and closed with sutures under local anesthesia. He received antibiotics and a tetanus toxoid booster. The next day, his wounds were found to be infected, and pus was drained from them. After these treatments, his wounds healed successfully. Animal bite wounds are frequently contaminated. Accordingly, in addition to early proper wound treatment, close observation of the wound is required for both the early detection of any signs of infection and early medical intervention, including appropriate drainage of pus and irrigation as necessary.
Introduction
Wild boars (Sus scrofa) exist worldwide. Their breeding period in most areas lasts into the winter season. They reach maturity in 2 years and live for approximately 10 years. 1 In Japan, there are 2 kinds of wild boar: Sus scrofaleucomystax (Japanese wild boar), which is the main species of wild boar in Japan, and Sus scrofariukiuanus (Ryukyu wild boar), which can only be found in the Okinawa prefecture. The height of an adult Japanese wild boar ranges from 100 to 170 cm, with a shoulder height of 60 to 90 cm, corresponding to roughly the thigh level of an adult human. Their weight ranges from 80 to 220 kg. Both male and female boars have tusks in the mandible and maxilla that are sharpened by rubbing against each other (Figure 1). Male tusks grow to up to 15 cm in length. Japanese wild boars can reach running speeds of 40 km/h from a standing start and can jump over 1 m in height. They are polyphagous and eat root vegetables, nuts, insects, and worms. They breed once a year.
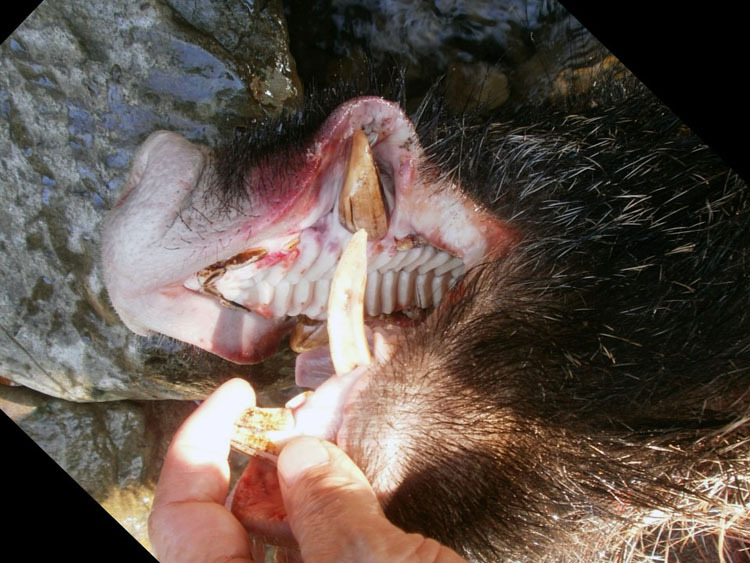
The tusks of a Japanese wild boar. Boars have tusks at the mandible and maxilla.
Recently, these boars have begun to explore human properties looking for food waste to eat or crops to forage. This behavior increases the risk of wild boar-induced trauma to humans living in certain areas of Japan. Kobe City has reported a number of human victims of boar attack every year.
2
The victims include those with wounds not only directly inflicted by boars but also those induced by falling after being attacked by boars. The maximum number of incidents reported annually between 2007 and 2014 was 76 in 2010 (2007: 2; 2008: 1; 2009: 2; 2010: 76; 2011: 21; 2012: 18; 2013: 27; and 2014: 66), with 26.6±29.1 (mean±SD) casualties per year based on reports from Kobe City. The number of victims did not decrease despite the legalization of hunting wild boars, perhaps due to human-generated feeding or leaving unharvested fruit in farm fields. Wild boar attacks on humans have been reported by the mass media in Japan, and these reports are summarized in Table 1,
3
(and
We herein report a case of bite wounds sustained by a human after a Japanese wild boar attack.
Case Presentation
A 74-year-old man was attacked by a wild boar while on his way home from his farm in the daytime in winter 2017 on the rural Izu peninsula. He did not provoke the boar; however, hunters were hunting animals in the mountains near the farm around the same time. The boar bit his left leg, and he fell. The boar continued to bite the man’s left foot, and the man delivered a few kicks to the boar’s face with his right leg. The boar then bit his right foot and ran away. A nearby person called an ambulance, and the injured man was transferred to our hospital. Upon arrival at the hospital approximately 1 hour after the accident, he was alert with a blood pressure of 110/96 mm Hg, a heart rate of 82 beats/min, a respiratory rate of 20 breaths/min, and 99% of SpO2 in room air. A physical examination revealed 3 bite wounds on the left leg and right foot (Figure 2). The wounds were irrigated with 5 L of sterilized saline applied with essentially no pressure, and the wounds were closed with sutures under local anesthesia. The wound closures had some gaps between the edges. The patient received a prescription of 1125 mg/day of amoxicillin/clavulanate for prophylaxis against infection and a tetanus toxoid booster. He did not receive any prophylactic injection for rabies because there have been no reports of rabies infection in any animals, including humans, in Japan since 1957, presumably due to the requirement established in 1950 that dogs be vaccinated by their owners.
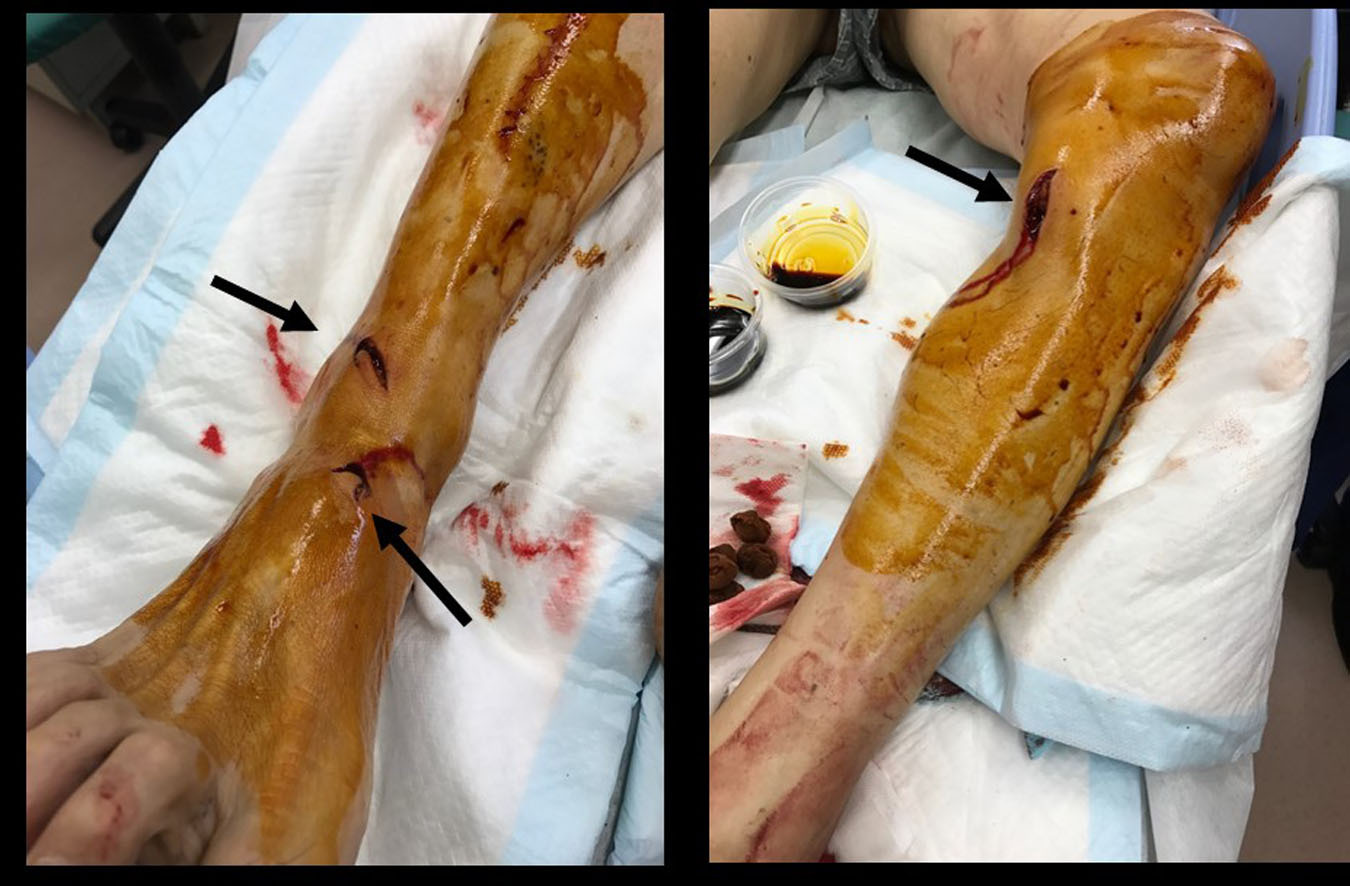
The patient’s bilateral legs on arrival. The photograph shows 3 bite wounds on the left leg and right foot, which were sanitized with iodine. The 2 bite wounds on the right foot are observed to be 5 cm apart from one another, which matches the boar’s tooth marks.
The patient returned for a reevaluation the next day, at which point his wounds were found to be infected. Pus was drained, and the wound was irrigated again. A culture examination was not performed because it was a holiday. After these treatments, his wounds improved, and the same antibiotic was continued. The wounds ultimately healed after 16 days.
Discussion
To our knowledge, this is the first medical report in English concerning bite wounds from a wild boar in Japan. We summarized the findings from the present and previous non-Japan–based English-language cases in Table 2.
1
,4–8 (and
Summary of injuries induced by wild boars in the English language literature
N/A, not applicable; I, irrigation; A, amoxicillin + clavulanic acid; P, primary closure.
Boar tusks can cause deep lacerations or lethal penetrating wounds. Given their depth, the wounds in the present case were probably induced by these tusks. Victims can also experience bone fractures when they fall or while delivering blows after initially being attacked by a boar. 9 Fortunately, the present case did not involve such injuries.
Most attacks occur within the species’ native range, typically in rural areas. Victims are commonly adult men traveling on foot and alone, 9 as was true for the present case. Attacks are most frequent during the winter months, during breeding and farrowing time, and during daylight hours when humans work, 9 similar to the present case. Most incidents happen under nonhunting circumstances and appear to be unprovoked. Wounded animals fighting back were the chief source of attacks in hunting situations. 9 Given the presence of hunting near the farm in the present case, an irritated boar might have been the culprit; however, it is also possible that the boar was provoked because it was the breeding season.
The most frequent outcome for victims is physical contact and/or mauling. 9 Injuries are primarily lacerations and punctures, with severity ranging from minor to fatal. Most mauled victims experience injuries to only one part of their bodies, with the legs and/or feet being the most frequently injured, 6 similar to the present case. This seems logical, as the average shoulder height of an adult wild boar is 90 cm. Accordingly, an age-associated variation in the types of injuries experienced was noted, with children typically injured in the upper body and adults usually injured in the lower body. 9 In more serious attacks, the animal can knock the human to the ground and then maul the victim. Such victims tend to sustain lethal injuries to multiple parts of their bodies compared with victims who are able to remain standing or upright. Fatalities are typically due to blood loss. Some victims wounded by wild boars die shortly after the attack. For adults with injuries to the lower region of the body, this is typically due to lacerated femoral arteries. 9 In one medical report, a craniocerebral injury resulted in death. 7 In other cases, serious infection or toxemia from the injuries resulted in death. 9
The management of an animal bite wound should start with proper local care of the wound. 1 A tetanus toxoid booster should be administered if the patient has previously been adequately immunized and has not received the most recent dose within the past 5 years. Similar to the present case, the wounds should be washed vigorously and irrigated with water, normal saline, or dilute povidone-iodine solution with high pressure for adequate cleaning to reduce the high inocula of the oral flora of the biting animal. 1 ,10,11 The organisms recovered from domestic pig bite infections include Staphylococcus species pluralis (spp), Streptococcus spp (including Streptococcus sanguis, Streptococcus suis, and Streptococcus milleri), diphtheroids, Pasteurella multocida, other Pasteurella spp, Mycoplasma, Haemophilus influenzae, Actinobacillus suis, Flavobacterium IIb-like organisms, Bacteroides fragilis, and other anaerobic Gram-negative bacilli. 1 There are conflicting data regarding the optimum antibiotic prophylaxis in the treatment of dog bite wounds and very limited data available regarding treatment regimens for other animal bite wounds. 11 Amoxicillin/Clavulanate (Augmentin) is generally considered to be the first-line prophylactic treatment for animal bites, similar to that used in the present case. 11 A meta-analysis of 8 randomized trials showed a benefit with antibiotic prophylaxis in animal bites. 12 However, a Cochrane review of 9 trials found no significant difference in the infection rate between prophylaxis-treated and untreated patients, except in those with bite wounds to the hand. 13 In addition, surgical closure of animal-bite wounds remains controversial, and an evidence-based approach is currently lacking. 1 Only one prospective controlled study concluded that dog bite wounds could be safely sutured. 14 In this report, there were no complications, and the wounds healed without infection after primary closure of the bite wounds. There is no evidence of any similarity in the bacterial flora between dog and boar bites. The present case was complicated by wound infection and treated with first-line antibiotics. This case might have required more irrigation with high pressure to prevent delayed infection. Fortunately, the patient recovered completely with appropriate early drainage.
Several ways of avoiding such attacks or reducing the severity of an attack by wild boars have been suggested. 9 If the animals are near, a person should slowly back away while being careful not to make any sudden or potentially threatening movements. Should the boars begin an aggressive approach from a far distance, an individual should try to outrun them; however, wild pigs can run faster than humans. If a wild boar charges at a close distance, the individual should climb a tree or other elevated object to escape the animal’s reach. If evasion or escape is not possible, one should turn and face the animal and prepare to aggressively fight back with anything at hand. While fighting back, it is important to try to stay upright. A person who has fallen or been knocked down should roll onto the back with the feet facing the animal and start kicking rapidly against the animal’s snout or head.
Conclusion
This is the first known medical report in English concerning bite wounds from a wild boar in Japan. Animal bite wounds are assumed to be contaminated. Accordingly, in addition to early proper wound treatment, close observation of the wound is required for the early detection of any signs of infection and early medical intervention should be performed, including drainage of pus and irrigation as necessary.
Author Contributions: Study concept and design (YY); acquisition of the data (HN, HM); analysis of the data (YY); drafting of the manuscript (HN, YY); critical revision of the manuscript (IT, SK, TI, KJ, TY, KI, and HO); and approval of final manuscript (KO).
Financial/Material Support: This manuscript obtained financial support from the Ministry of Education, Culture, Sports, Science and Technology (MEXT)-Supported Program for the Strategic Research Foundation at Private Universities, 2015–2019.
Disclosures: None.
