Abstract
We herein review and analyze the diagnosis, treatment, and outcome of a severe infection caused by a human bite. A 68-year-old man was bitten on the forearm by a 3-year-old child. Rapid progression of infection, severe local and systemic poisoning, and diverse clinical manifestations were observed at presentation. Based on the medical history, physical signs, imaging examinations (X-ray films, color Doppler ultrasound, and computed tomography), laboratory examinations, and multidisciplinary consultation, the patient was diagnosed with gas gangrene or gas gangrene-like changes. Twenty-four hours after the injury, an emergency amputation was performed (open amputation with wound closure after 1 week). After the operation, the patient was sent to the intensive care unit for isolation and further anti-infection and anti-shock treatments. His condition gradually improved after treatment and he was discharged without further complications. Bacteriological and pathological examinations indicated
Introduction
Human bites are relatively frequent but very rarely cause severe infections, especially with severe systemic symptoms. In emergency cases, however, it is important to consider this possibility and initiate early anti-infection and active anti-shock treatments when necessary. Surgical treatment should follow life-saving, limb-preserving, and function-preserving principles. In 2018, our hospital admitted a patient whose right forearm had been bitten by a 3-year-old child. The infection was initially undetected but then rapidly progressed to severe systemic poisoning requiring limb amputation. The infection was controlled under isolation in the intensive care unit (ICU), and the patient gradually recovered. The reporting of this study conforms to the CARE guidelines. 1 All patient details have been de-identified in this manuscript.
Patient information
A 68-year-old man was admitted to the hospital with a superficial, roughly 4-cm right forearm bite delivered by his 3-year-old grandson 24 hours earlier. The limb appeared swollen and cyanotic, and the patient reported general discomfort for 4 hours prior to admission. At the time of the injury, the lesion was neither washed nor disinfected. Roughly 16 hours after the injury, the patient developed swelling and pain in the distal right upper extremity. He visited a local clinic and was diagnosed with “gout arthritis” without laboratory confirmation and was given nonsteroidal anti-inflammatory treatment. Despite treatment, he reported gradual worsening of the swelling and pain of the limb, purpura around the wound and right hand, and systemic symptoms including weakness, palpitation, and cold sweats. He then visited the emergency department of our hospital seeking further treatment.
Clinical findings
At presentation, the patient was experiencing acute pain and was in shock as evidenced by hypotension, a rapid pulse, and cold sweats. His upper limb exhibited flaky plaques, swelling, and weak iliac artery pulsation. Dopamine was immediately administered to maintain his blood pressure, and both laboratory and imaging examinations were conducted. Because of the patient’s complicated condition, the attending doctor reported the situation to the hospital duty officer to organize staff for multidisciplinary medical treatment. During the observation period in the emergency department, the swelling and ecchymosis of the patient’s limb continued to expand and rapidly progress. Examination of the upper right limb by a surgeon revealed crepitus of the subcutaneous soft tissue. A puncture examination of the primary lesion revealed gas bubbles in the subcutaneous tissue with edema. The patient was administered anti-infection treatment in the emergency department, but this did not alleviate the condition, and his limb lesions continued to expand (Figures 1 and 2) concomitant with deterioration of consciousness.

Condition of the right upper limb. (a) The condition of the right upper limb at presentation to the emergency department. The 4-cm superficial bite wound was accompanied by local flaky plaques, swelling, and severe pain. (b) After 3 hours of anti-infection treatment, the local condition was aggravated.
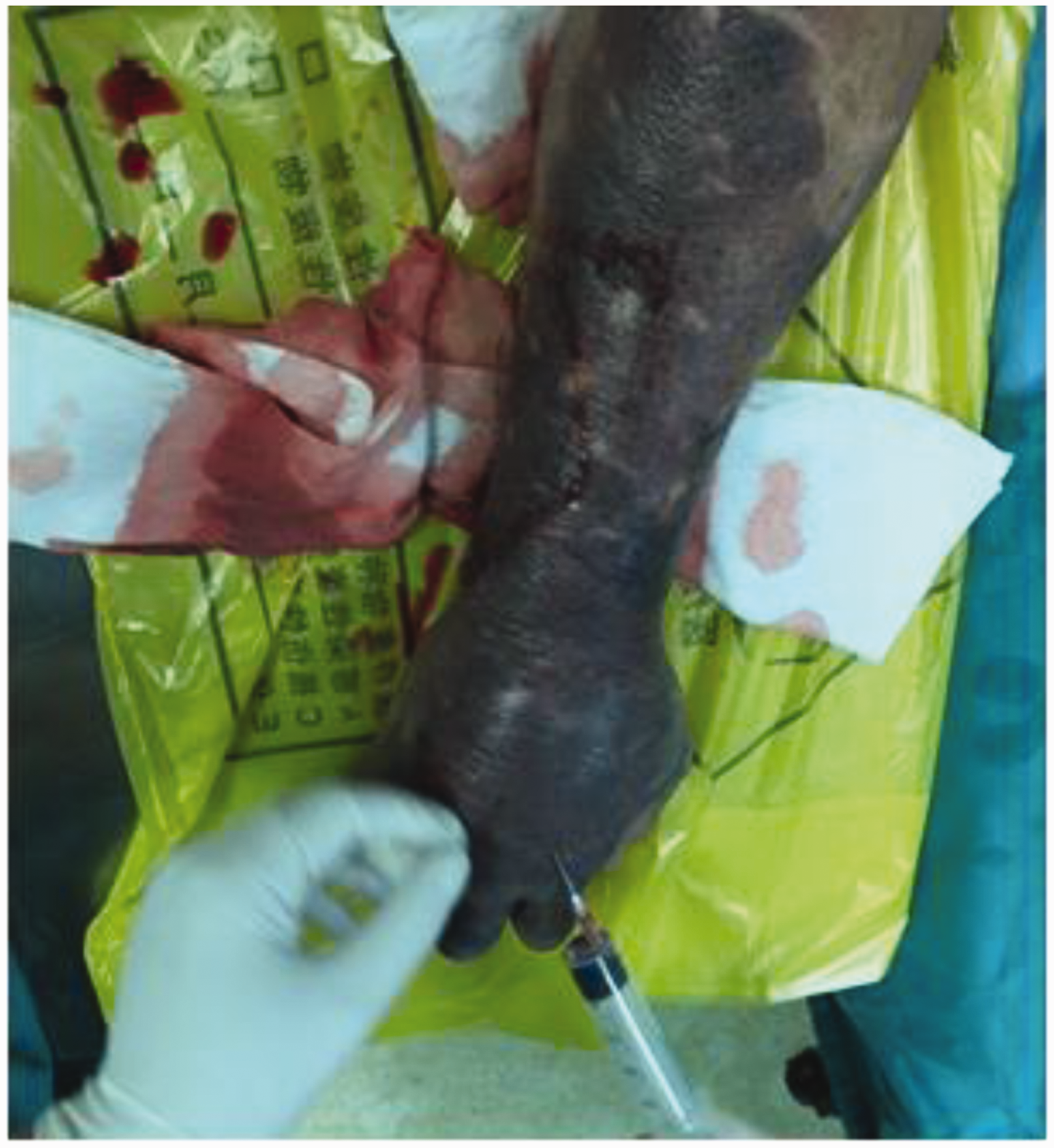
Preoperative condition of the right arm. Swelling and ecchymosis progressed rapidly, involving the entire forearm, and the soft tissue in the right upper limb showed subcutaneous crepitus. Large numbers of gas bubbles were withdrawn from the main lesion, but no fluid was extracted.
Diagnostic assessment
The patient’s emergency laboratory examination results were as follows: white blood cell count, 4.85 × 109/L; hemoglobin (HGB) concentration, 70 g/L; platelet (PLT) count, 36 × 109/L; C-reactive protein concentration, 68.35 mg/L; and procalcitonin concentration, 48.960 ng/mL. Blood coagulation was normal. X-ray and computed tomography examinations revealed a large volume of gas in the soft tissue of the right hand and forearm (Figure 3). Smear examination of the bite wound showed a large number of Gram-negative bacilli. Therefore, we considered this to be a case of gas gangrene-like infection.
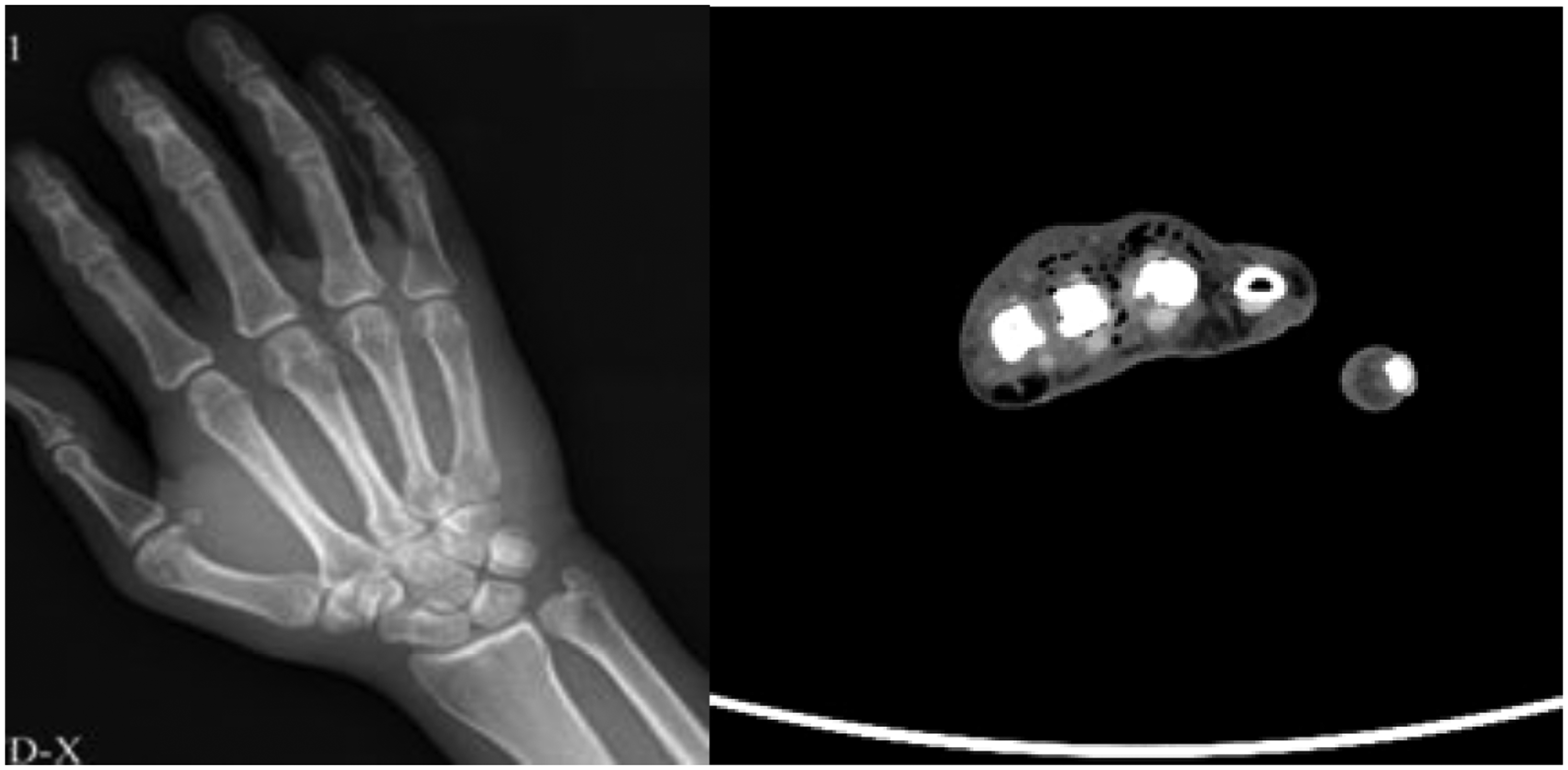
X-ray and computed tomography findings. A large volume of gas was present in the soft tissue of the right hand and forearm.
Therapeutic intervention
Open amputation
The surgeon performed a fish mouth incision in the skin 5 cm proximal to the lesion, entered the limb layer by layer, revealed important vascular nerves and disconnected them, ligated the blood vessels, cut the bone at the upper part of the humerus, and trimmed the stump. The proximal muscles responded to electrotome stimulation. The muscle was sutured to cover the end of the bone. The wound was not sutured but was wrapped in a large amount of sterile wound dressing. After the operation, the patient was sent to the ICU of the Infection Department for isolation treatment under endotracheal intubation. Dissection of the amputated limb section caused a large amount of malodorous gas to escape. The lesions were necrotic and dark purple, and some tissues had dissolved (Figure 4).
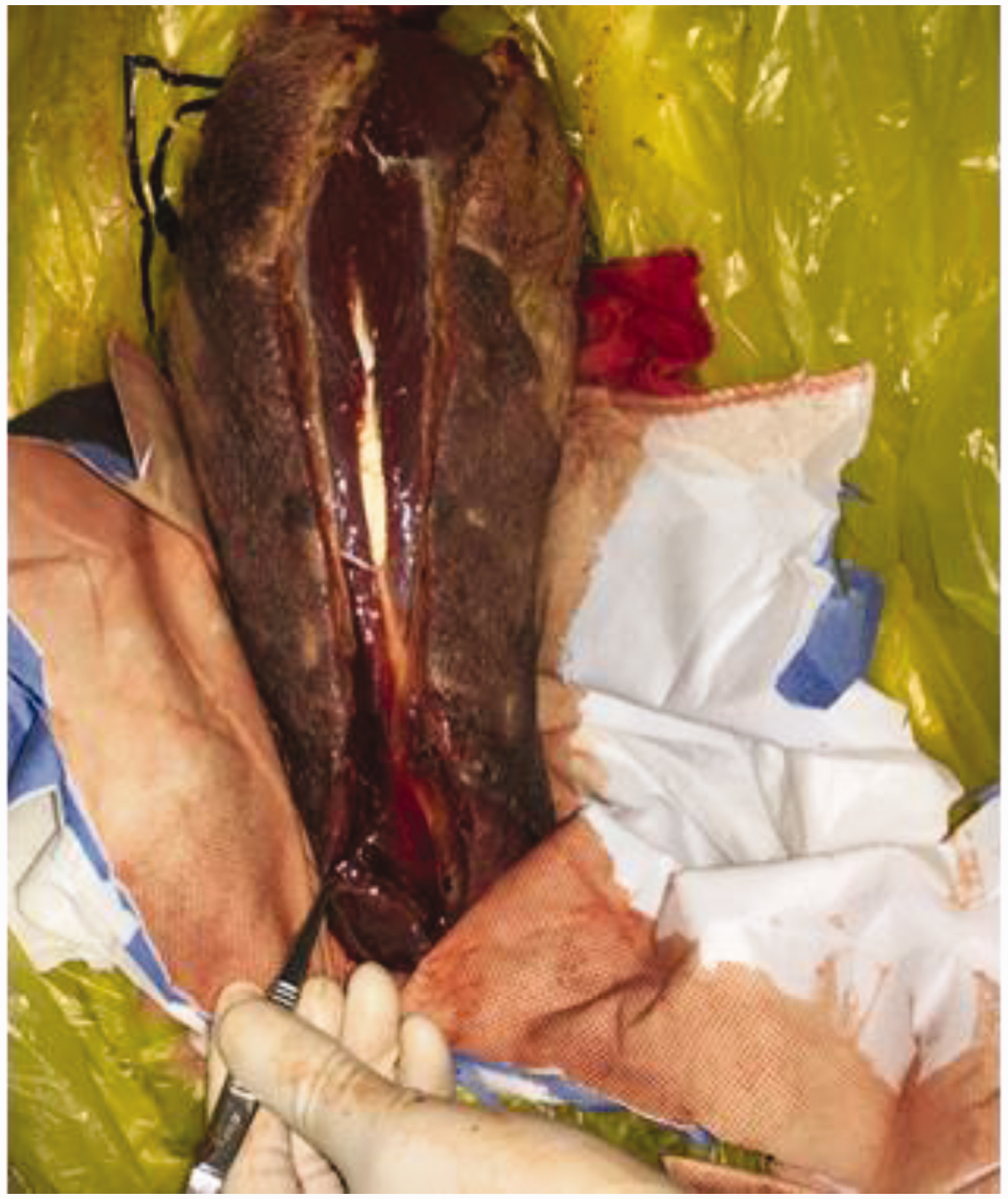
Condition of the residual limb. A large amount of malodorous gas escaped, the lesions were necrotic, and some tissues had dissolved.
ICU isolation and follow-up treatment
The patient was treated under isolation according to the standards for gas gangrene. He received a combination of penicillin, meropenem, and clindamycin for infection and vasoactive drugs to maintain his blood pressure. He developed an intermittent fever after the operation, reaching 40°C. The patient’s infection index, procalcitonin concentration, and C-reactive protein concentration were still elevated for 3 days postoperatively, after which they gradually decreased. Both his HGB concentration and PLT count remained at low levels during ICU treatment. Multi-point bacteriological culture revealed

Wound condition after the first surgery. Three days after the first operation, the exposed stump wound emitted a foul odor and exudate. Local muscle tissue necrosis and a small number of ecchymoses around the wound were also observed.
Follow-up and outcomes
After active treatment, the patient’s vital signs gradually recovered and stabilized. All laboratory indicators, including the HGB concentration and PLT count, gradually recovered to near normal levels. The patient was extubated on the 11th day after amputation and resumed spontaneous breathing. His state of consciousness remained clear. When the wound had healed (Figure 6), the patient was discharged but did not agree to continue chemotherapy for AML and died of blood system disease 2 years later.

Wound condition after the second surgery. Ten days after the second operation, the wound was clean and well-healed.
Discussion
Although bites from children are relatively common, they rarely have such serious consequences in such a short period. In fact, no similar reports were found in the literature. Infections from human and animal bite wounds are usually caused by a mixture of aerobic and anaerobic microorganisms. 2 In this case, the onset was sudden after an initial delay and the disease progressed rapidly, reaching a state of severe systemic toxicity within 24 hours. In such cases, it is very difficult for the attending emergency physician to make decisions regarding diagnosis, prognosis, and treatment.
Surgical exploration of the amputated limb resulted in the release of a large amount of malodorous gas. The muscles near the lesion were dark and inactivated, and some tissues had dissolved. Bacteriologic culture revealed
There are two possible explanations of how the human bite led to
Based on the patient’s condition in the emergency department, we had reason to suspect gas gangrene and treated the patient accordingly. Once gas gangrene has been diagnosed, surgery should be performed as soon as possible.
8
Even if the patient is in shock, surgery should be performed while the shock is being rescued. At that time, we could have chosen either limb salvage surgery or amputation. Postoperatively, partial necrosis was still progressing in the stump, and culture indicated the presence of
Human bite-induced necrotizing fasciitis (gas gangrene-like changes) or sepsis caused by
Footnotes
Ethics statements
Written informed consent was obtained from the patient for treatment and publication of this case report. All patient details have de-identified. Ethics approval was not required because of the nature of this study (case report).
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Natural Science Foundation of Guangdong Province (Nos. 2018A030313640 and 2019A1515012176) and the National Natural Science Foundation of China (No. 81101366).
Author contributions
Study design: Runguang Li. Literature search: Guozheng Zhu, Canjun Zeng, and Runguang Li. Manuscript preparation: Guozheng Zhu, Canjun Zeng, Song Yuan, and Runguang Li. All authors read and approved the final manuscript.
